Abstract
Study design
The present case report demonstrated a reproducible and low-cost method to planning orbito-zygomatic reconstruction applied to a sequela of facial trauma.
Aim
This study aims to purpose a method to surgical planning orbito-zygomatic reconstruction and demonstrate it in a clinical report.
Method
An 89 years old male patient with severe sequela due to previous trauma surgery was submitted to a reconstructive surgery using cutting guides and mini-plates pre shaped using a stereolitographic printed model with mirroring healthy side.
Results
Computed assisted surgery (CAS) contributed to the advancement of surgical planning and reconstruction in Oral and Maxillofacial Surgery, and trauma-related injuries. Traumatic injuries at the orbito-zygomatic region and midface are challenging and satisfactory three-dimensional reconstruction is not often achieved with conventional techniques; therefore, it strongly benefits from CAS and 3D printing. However, the high costs and technical difficulties can impair the use of new technologies in the public health system of low-income countries.
Conclusion
Hence, the present case report demonstrated a reproducible and low-cost method to planning orbito-zygomatic reconstruction applied to a sequela of facial trauma
Introduction
The introduction of new technologies as Computed Assisted Surgery, and virtual 3D-planning, has been related to the improvement of predictability in the field of oral and maxillofacial surgery.1-3 The use of stereolithographic models allows the surgeons to preview the tridimensional changes in the hard and soft tissue.4,5
One of the most usual functions of 3D printing technology is the use of solid printing material to reproduce some areas of skeletal anatomy. 1 The craniofacial area is one of the most complex structures in the human body, due to its specific and very specialized functions; consequently, the surgical procedures which aim its reconstruction are particularly challenging.1,2,6 The need for symmetry and the importance of facial aesthetics are both factors that increase the difficulty in craniomaxillofacial reconstruction.
The orbito-zygomatic complex (OZC) is the second most traumatized part of the facial skeleton. Its anatomy is related to several laminar bones and noble structures.7,8 When large orbital defects are present in facial trauma the loss of main landmarks can impair the proper reconstruction. The difficulty to restore anatomical volume and shape can lead to catastrophic consequences, as severe enophthalmos, loss of symmetry, diplopia, loss of soft tissue, and esthetical defects.7,9,10
However, in the last years, the improvement of 3D planning and printing is doing better to restore the anatomy of traumatized or tumor-destroyed orbits. One of the most popular uses of these technologies is the mirroring of the healthy side, and printing patient-specific surgical guides, according to the previous planning of the surgeon.1,4,6
Besides its incontestable benefits, those technologies are still expensive and demand a well-trained team. Many oral and maxillofacial services in developing countries do not count with the aid of 3D planning and printing technology, and in consequence, present high rates of post-surgical deformities in orbito-zygomatic fractures. After all, the patients are referred to a well-equipped surgery team several months after the first surgery. The literature in the field of computed assisted surgery and 3D printing in oral and maxillofacial surgery is still incipient, and there is a lack of evidence about the use of these techniques in the treatment of sequelae.2,5
This report aims to present the surgical treatment of a severe sequela of orbito-zygomatic fracture, using a low-cost method of 3D printing to the surgical planning and surgical guides fabrication. The patient’s written consent was obtained for publishing the full case report including clinical information and clinical and radiologic images.
Case Report
An 89 years old, male patient was attended to the department outpatient clinic of maxillofacial surgery referring a previous facial trauma due to a fall from own height, 4 months before the consulting. The patient is also referred to have been submitted to reduction and fixation of the right side orbito-zygomatic complex.
At the first evaluation, by the surgical team, the patient presents with significant enophthalmos, and asymmetry, reporting binocular diplopia and eye movements restriction. (Figure 1) A CT scan showed the unsatisfactory position of the orbito-zygomatic complex and increased orbital volume, which was not corrected despite the presence of a titanium mesh previously inserted. (Figure 1) (A) Patient in clinical frontal view. (B) Tridimensional volume rendering of CT scan, demonstrating the orbito-zygomatic fracture. (C) Coronal slice of CT scan showing a blow-out orbital fracture and the difference in the orbital volume between the two orbits. (D) Virtual planning of 3D cutting guides. (E) The stereolithographic model used to support surgical planning.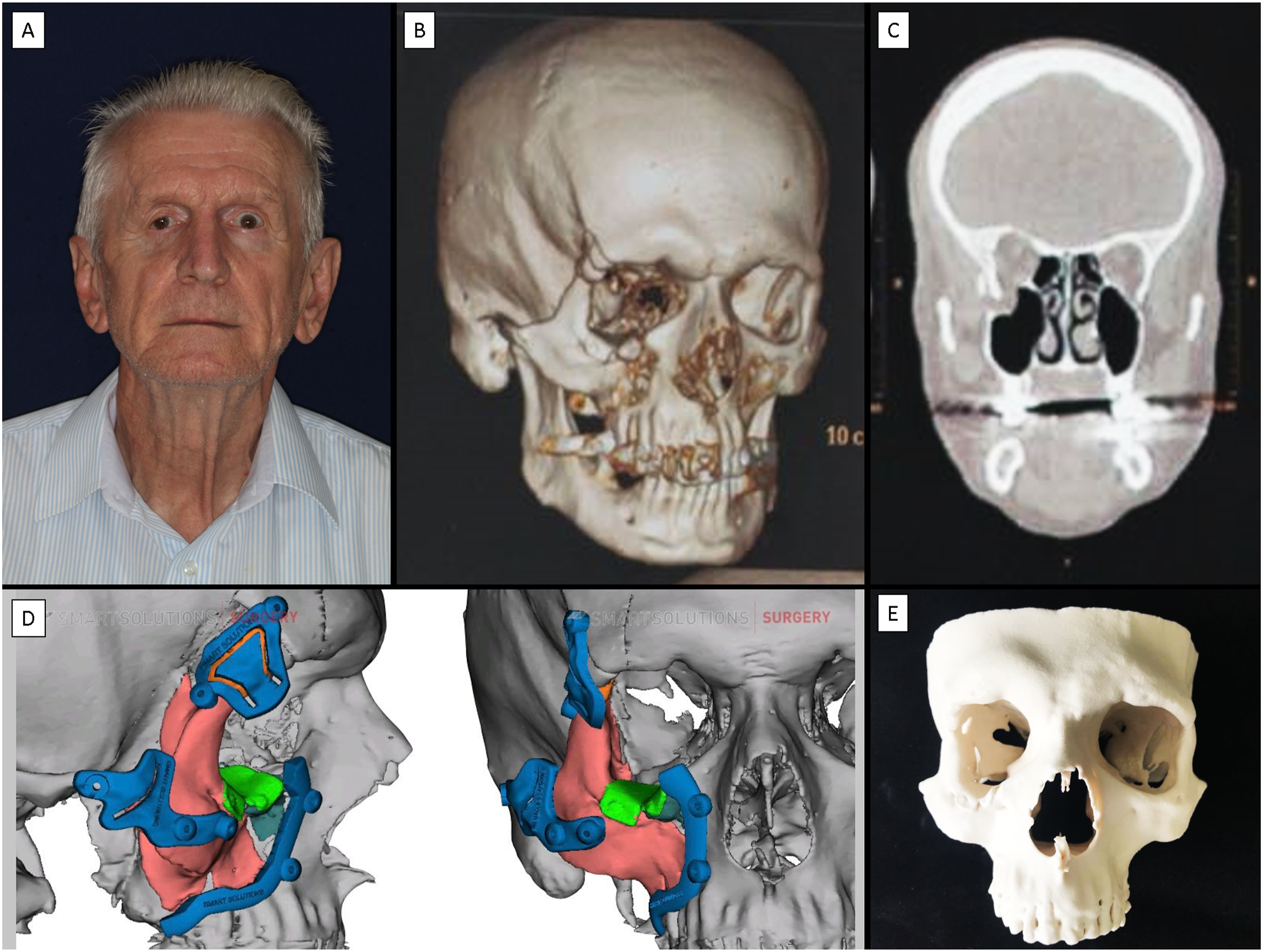
Despite the patient’s advanced age, a new surgical intervention was recommended and performed following the patient’s wishes. To guarantee the correct repositioning of the orbito-zygomatic complex, the surgical team choose to use virtual 3D planning, by mirroring the opposite side and generating a stereolithography model printed in a Objet30 Polyket Fullcure (Stratasys, Minessota, USA) with a translucid resin (Polyjet RGD720), to simulate the osteotomies and develop the cutting guides, the osteosynthesis materials were pre-bent in the 3D model, and not special printing of titanium plates and meshes was demanded. (Figure 1). The total printing time was 60 minutes, 40 minutes for printing and 20 minutes of curing time. The surgical procedure was performed under general anesthesia. A combination of surgical approaches was performed to allow the positioning of cutting guides, tridimensional correction, and fixation with stock titanium plates. (Figure 2) (A) Trans operative view of the fractured frontozygomatic area. (B) Cutting guide positioned at the frontozygomatic buttress. (C) Cutting guide positioned at the zygomaticomaxillary buttress. (D) Osteosynthesis plate in position at the frontozygomatic area. (F) Infraorbital rim, (G) zygomaticomaxillary buttress, and (H) in the orbital floor.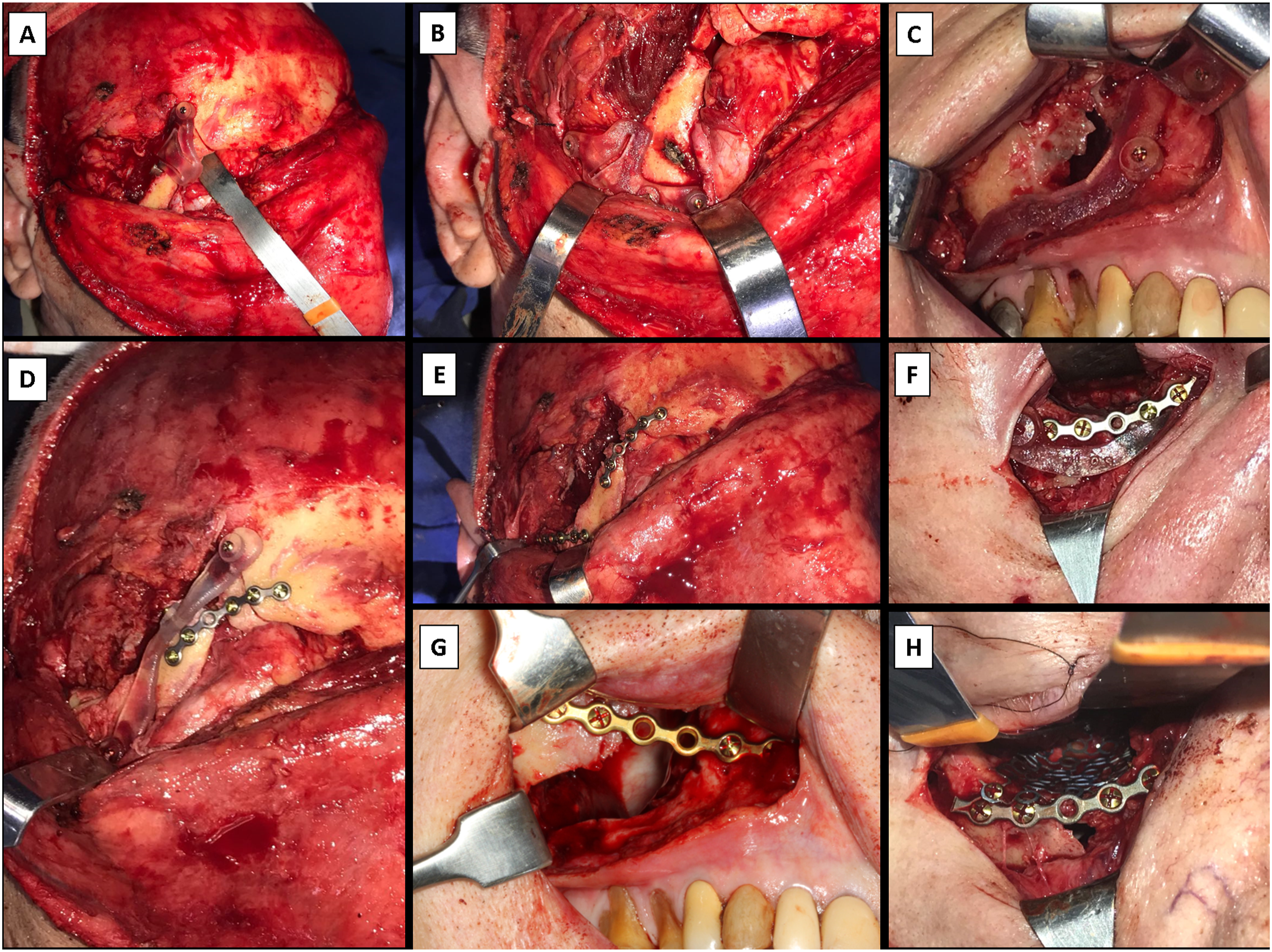
An ophthalmologic evaluation was performed 6 months after surgery, and the visual accuracy was improved by 90% in comparison to pre-operative evaluation. Also, a new CT scan was performed and compared to the mirrored virtual planning with a collision map (Figure 3), showing the accuracy of the reconstruction. (A) Patient in frontal view 6 months post-op. (B) Post-operative CT scan 3D volume, with highlighted osteosynthesis plates. (C) Color map showing the mirroring of heath side for three-dimensional printing. (D) Collision map of the mirrored side with the post-operative result. (A) Patient in frontal view 6 months post-op. (B) Post-operative CT scan 3D volume, with highlighted osteosynthesis plates. (C) Color map showing the mirroring of heath side for three-dimensional printing. (D) Collision map of the mirrored side with the post-operative result.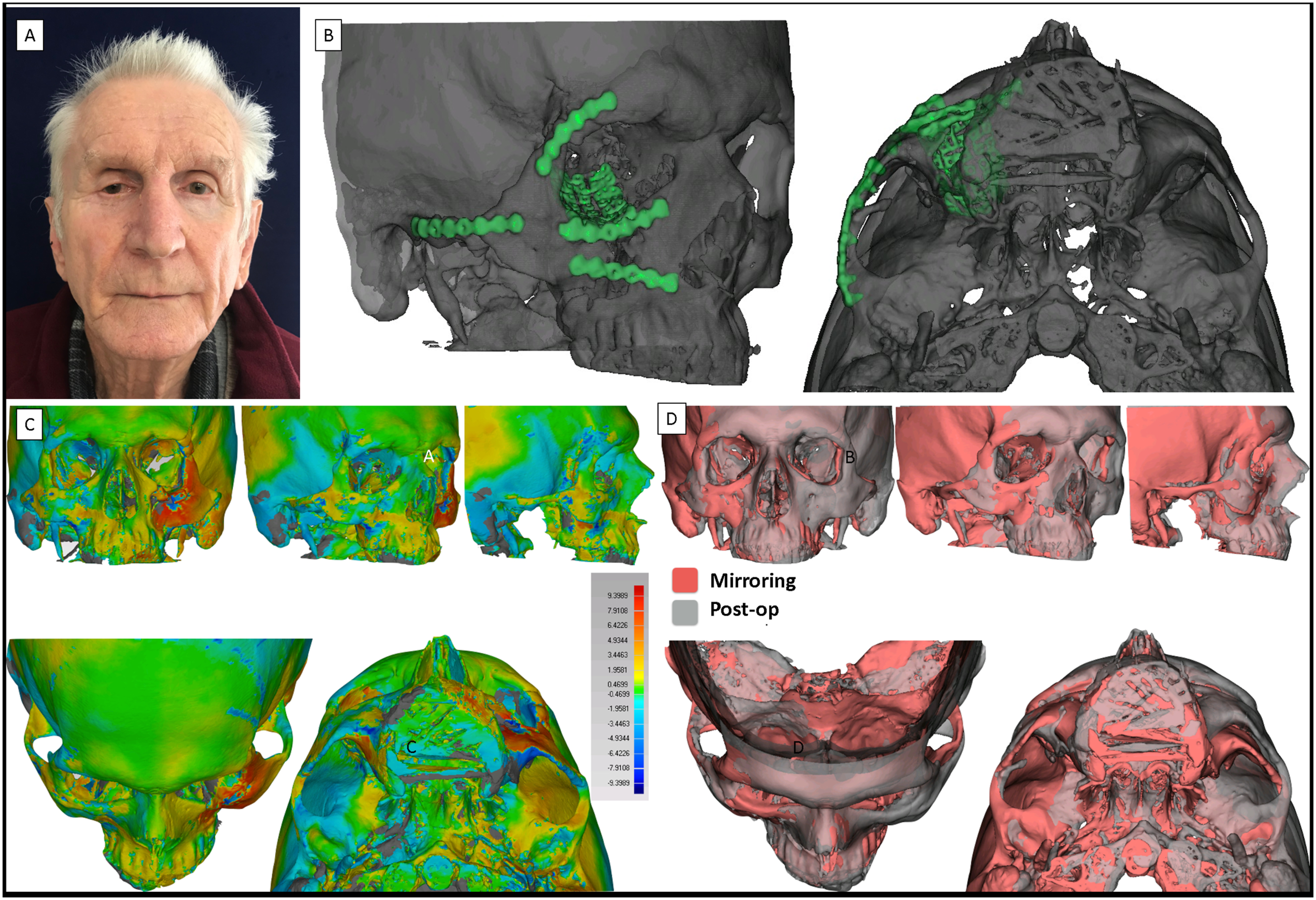

After 2 years of follow-up, the patient presents with good visual accuracy, correct eyeball position, and is satisfied with the facial symmetry.
Discussion
Three-dimensional printing promoted a shift of paradigm in the medicine and reconstructive surgery field. However, the application of these technologies on large scale faces some impairments as the cost and the demand of a multidisciplinary team, with doctors, computational scientists, and engineering.
In low-income and developing countries the search for cost-effective treatments and resources, most of the time comes over the gold standard technologies.3,4,11 In this case report, we showed how surgeons can aid patients and the surgery team with consolidated technology using the available resources.
Cutting guides has been widely used to plan and perform complex osteotomies, in the field of orthognathic surgery the 3D-printed occlusal guides have been used to define the final position of operating segments, but recently cutting guides also helped in determining the position and fixation since the moment of the first osteotomy to be performed.12-14 In Maxillofacial trauma, the precise spatial restoration of anatomy is challenging, and position guides printed with the assistance of three-dimensional planning can improve the post-operative esthetical and functional results.11,15,16
Hierl et al 9 have shown that preformed meshes can reduce the surgery time by 15 to 30 minutes; however, they performed this investigation using patient-specific implants printed in titanium. Bachelet et al 16 in a similar study, demonstrated in a case series that further than time reduction, pre-shaped meshes also reduce post-operative morbidity
Other authors have been concerned about the cost-effectiveness of printing the implants in titanium. Callaham et al, 11 for example, developed a method to print a bent mold, they simulate a reconstruction in virtual planning, then printed a negative copy of the affected wall, and finally shaped the chosen reconstruction material with the negative This method presents lower cost because do not need to print all the midface or the orbito-zygomatic complex. However, in cases of post-traumatic sequelae or reposition of the entire OZC, like the one presented in this paper, it is useful to shape the reconstruction materials and plan the cutting guides in a complete OZC print.
Using the opposite side as a mirror to reshape the injured orbit is a recurrent technique in the literature, but most authors agree that the most significant disadvantage of this technique is the dependence of an unaffected side,8-10 which is also a concern in our described technique.
Despite the limitations, the purposed technique has been demonstrated to be effective, presenting good results, and it is also reproducible. In conclusion, three-dimensional printing is an alternative to shape and plan both cutting guides and reconstruction materials.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
This study was conducted according to Helsinki declaration rules for ethical standards and consent, and free consent was obtained from patient regarding the rights of image and data. The Ethical Committee of São Paula State University—São José dos Campos have been informed of this case report.
