Abstract
Study Design:
A retrospective study of 26 cases of human bite injuries at the Government Dental and Maxillofacial Hospital (now Maxillofacial unit, Rivers State University Teaching Hospital), Port Harcourt, within September 2011 and August 2016.
Objective:
To analyze the pattern, presentation, management, and complications of human bite injuries in the orofacial region.
Methods:
Information was extracted from hospital records of all victims of human bites to the face between the study period. Facial bites resulting from animals were excluded. Data such as age, gender, time lag between the injury and time of presentation in the hospital, nature and the circumstances of the injuries, site of injuries, and treatment outcomes and complications were collected and analyzed.
Results:
A total of 26 patients within the ages of 18 and 60 years were seen during the period of study. They were all related to fights, which were all resolved out of court. There was a preponderance of females, and the lower lip was the most affected site (p < .05). In all, 14 patients presented within 24 hours of injury and all but 2 (7.6%) patients presented within 7 days of injury. No wound was overtly infected. Treatments of injuries were varied from simple wedge excision and primary closure to complex multistaged procedures and were uneventful with acceptable surgical outcomes.
Conclusion:
Human bite wounds reported in this study were all due to social conflicts without legal redress. Although human bite wounds are considered to be dirty or contaminated but with proper wound debridement, antimicrobial cover and primary or immediate surgical closure results in very favorable aesthetic outcomes in all cases.
Introduction
Human bites to the face constitute a significant proportion of injuries to the face. All parts of the face are involved including the ears, chin, cheek, forehead, and lips. Records from 2 separate studies in the United Kingdom showed that these facial injuries accounted for 84% 1 and 82% 2 of total body bite wounds. In Nigeria, Ugwu 3 , Tabowei and Amaefula 4 , Robsam et al, 5 and Ozinko and Otei and Otei 6 reported that facial human bite injuries accounted for 16%, 26%, 55%, and 83% respectively. Attributable causes in adults are interpersonal conflicts resulting in fights, physical and sexual abuse, robbery, and in children during playing. 7 –9 The severity of the injuries is varied, ranging from simple lacerations to avulsive injuries with loss of vital tissues resulting in both cosmetic and psychological consequences. 10 –12 Port Harcourt city in Nigeria has had its fair share of the problems of urbanization which is characterized by unprecedented growth in population with insufficient basic infrastructures, social, health, and economic equalities. Therefore, there is an increased tendency for family conflicts, strife at places of work, and armed banditry. 13
Human bite injuries carry the risk of being infected with bacteria from the oral cavity and as such are generally considered as dirty or contaminated wounds. This becomes obvious especially when presentation to the hospital is delayed. 14 In an elaborate multicenter study by Talan and colleagues in 2003, bite wound cultured several microbes including fungi. Streptococci especially Streptococci anginosus, which topped the list of isolates, has been implicated in serious brain and visceral abscesses when compared to other S viridians. 15 It is also biologically plausible for transmission of herpes simplex, hepatitis B and C, syphilis, tuberculosis, actinomycosis, and tetanus during bites. A rare case of transmission of HIV 16 and mycobacterium ulcerans 17 disease have been reported in the literature.
Opinions in the literature lean toward primary surgical repair as the treatment of choice for a majority of cases. 9,11,18,19 There is however a place for delayed closure in certain cases where wound infection exists already or there is a high risk of infection. 20
Human bite of the face resulting in partial or total loss of important aesthetic subunits of the face like the ears, nose, eyelids, and lips presents a challenge to the surgeon in 2 major fronts. These are restoration of the structure and function to avulsed facial structures and the resultant introduction of surgical scars which may be unpleasing. Therefore, meticulous planning and implementation of proposed treatment plan is key. This study therefore is an overview of the presentation, management, and prognosis of all the patients with human bite injuries presenting at the Government Dental and Maxillofacial Hospital, Port Harcourt, over a 5-year period.
Materials and Methods
This retrospective study was conducted at the Government Dental and Maxillofacial Hospital, Port Harcourt. Port Harcourt is the capital city of Rivers State in the oil-rich region of the Niger Delta, Southern Nigeria. It is located on latitude 4°46′38.71″ N and longitude 7°00′48.24″ E. Information was extracted from hospital records of all victims with various degrees of human bites to the face between the period of September 2011 and August 2016. Facial bites resulting from animals such as dogs and cats were excluded. This information included age, gender, time lag between the injury and presentation in the hospital, nature and circumstances of the injuries, sites of injuries, details of treatment, and outcome of treatment including complications. Ethical clearance was obtained from the Ethical and research committee, and informed consent was obtained from the patients. Descriptive analysis and Chi-square analysis were done with p < .05 considered as statistically significant with IBM Corp, Released 2012 (IBM SPSS Statistics for Windows, Version 21.0. Armonk, New York: IBM Corp), and the results are presented in Tables 1 and 2.
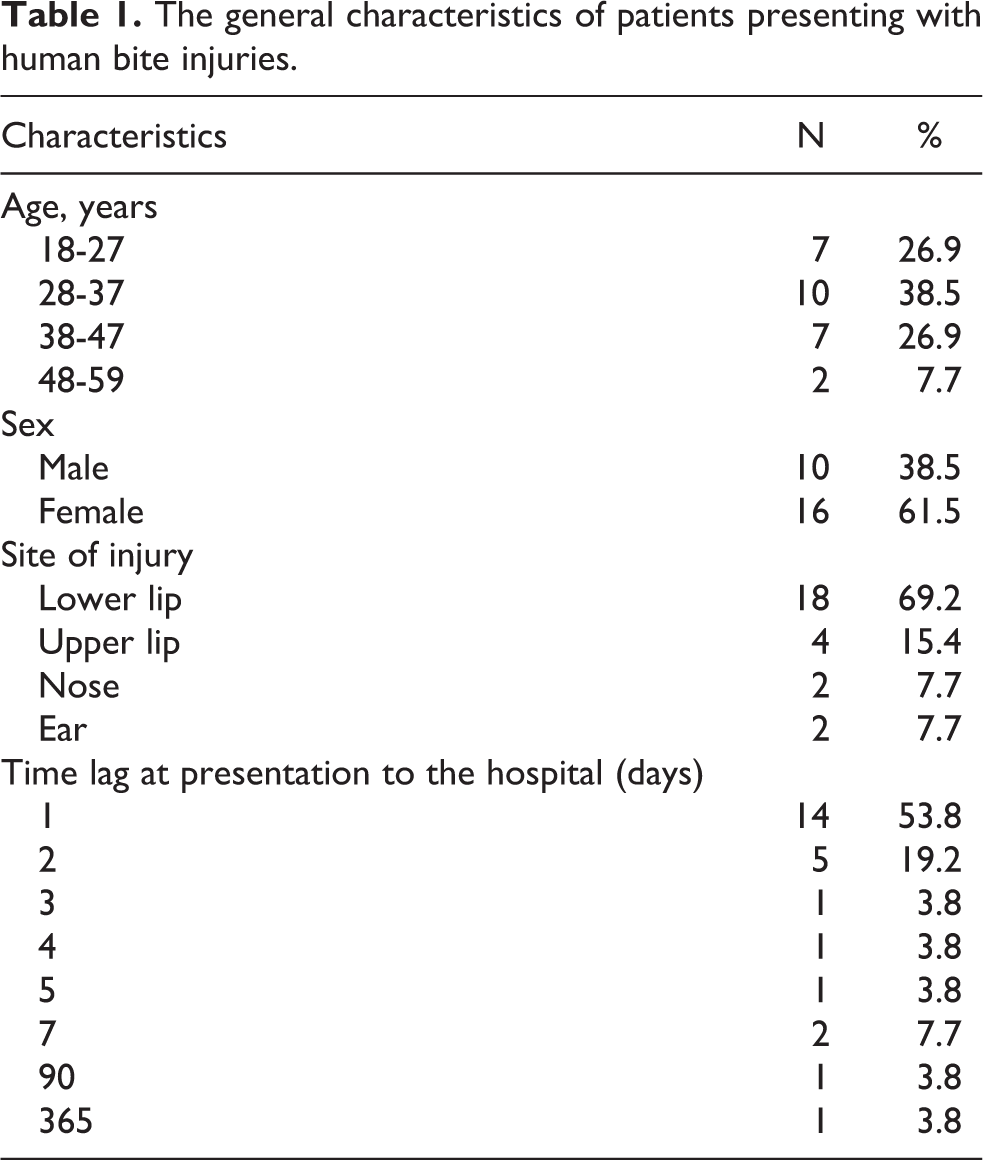
The general characteristics of patients presenting with human bite injuries.
Relationship Between Gender and Age of Presentation, Site of Injury, and Time Difference Between Onset and Presentation.
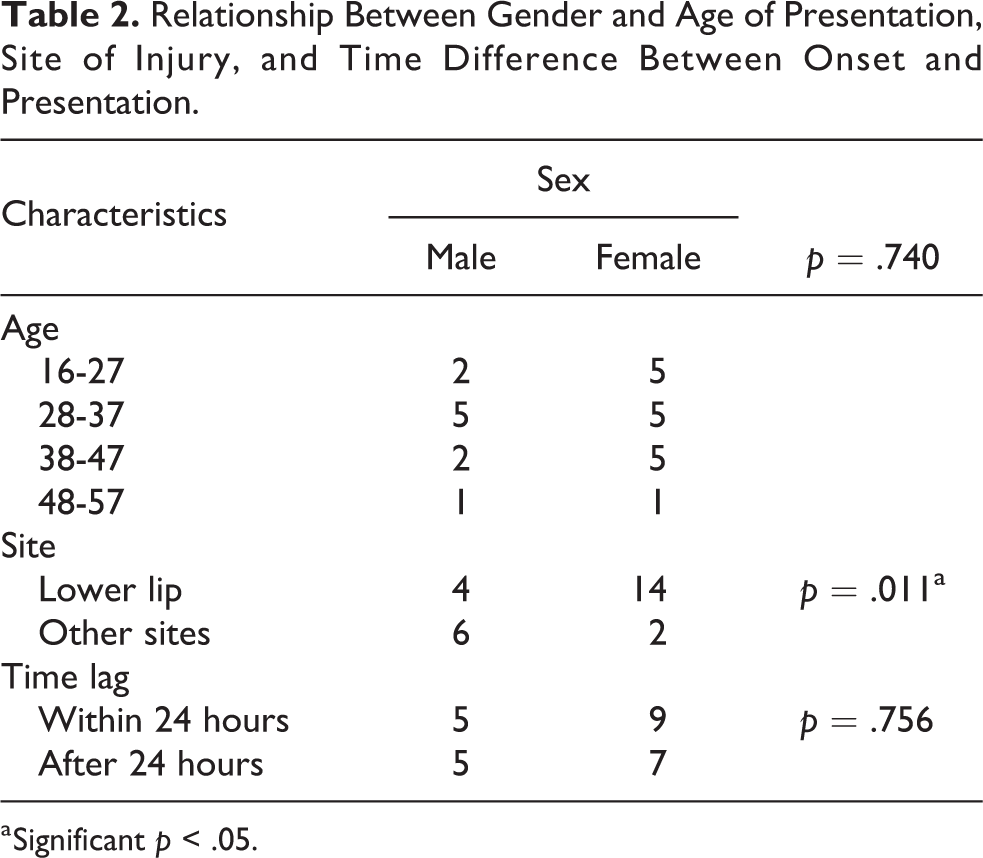
a Significant p < .05.
Results
A total of 26 patients with human bites of the orofacial region were treated in our hospital during the 5-year period of this study. Patient age ranged from 18 to 60 years with a preponderance of females. The male to female ratio is 1:1.6; 18 (69.2%) patients had lower lip bites and 14 (53.8%) presented to the hospital within the first 24 hours of the injury. The general characteristic is shown in Table 1. Of the 26 patients, 25 (96.2%) who presented in the clinic were surgically managed. All lip injuries were surgically repaired by wedge-shaped closure except 1 who received 2-staged Abbe lip switch repair. All ala avulsion was repaired with nasolabial flap. Ear injuries were referred to the plastic units of the same institution. They all had uneventful healing of their injuries, and the outcome of surgery was satisfactory.
Discussion
In this study, more female victims of facial human bites were recorded. This is in agreement with earlier studies reported by Iregbulem 19 and Obuekwe 9 in Nigeria and Shubi et al 21 in Tanzania. It however contradicts other studies by Donkor et al 18 in Ghana and Koesch et al 7 in Kenya, where males were more afflicted.
The victims were aged between 18 and 60 years and there was no predilection for the younger age-group as found in other studies from Tanzania, Zimbabwe, England, and Ghana, 2,18 –20 where alcohol consumption, intake of recreational drugs, music and dancing, or unlawful acts like robberies were common factors implicated in such attacks. The factor most commonly implicated in our study was matrimonial conflicts in mono- or polygamous marriages commonly resulting in fights between man and wife or wife and cowife. Other reasons that were found to be involved included jealousy, unfaithfulness in marriage, disagreements in family matters or at work places, and fights between neighbors. Although few cases related to robbery was reported by Iregbulem 19 and Koech and Chinidia, 7 sexual assault by a rapist has been reported by Donkor and Bankas. 18 These were not features in our study rather all the assailants knew all their victims and the bites were aimed at deforming or as a form of defense. None of the victims in our study asked for legal redress in a competent court of law as compared to Olatan et al, 14 where 4 patients of 54 patients sought the face of the law necessitating pictorial evidence from the attending doctors. This highlights the importance of proper documentation. It is believed that patients in this study would have resorted to indigenous method of conflict resolution negating legal actions. 22
The lower lip (69.2%) was most commonly involved in cases. This was followed by injuries to the upper lip (15.4%) of cases. Lower lip involvement was more frequent in the females (p < .05). The Negroid lips are particularly prominent on the face due to bimaxillary protrusion leading to thicker and more prominent lips, thereby making it easier for the assailant’s teeth to grab unto it. These findings are in agreement with those of Obuekwe who also found the lower lip to be the most commonly involved site. 9 Only 7.7% of cases involved the nose in this study, however, 2 cases of ear involvement was recorded during the period of study. Earlier reports from the same city between a period of 1983 and 1985 by Datubo-Brown 23 showed a predilection for the ear, 10 patients had pinna injuries followed by 8 patients with lower lip injuries in 24 patients who presented with facial injuries.
None of the cases who presented in our center were overtly infected. Our observation is that those who presented late may have been administered some kind of wound treatment and antimicrobial coverage at the nearest primary health center or a patent medicine stores before their presentation to our clinic. In Nigeria, many antibiotics can easily be purchased over the counter such as amoxicillin, amoxicillin–clavulanic acid, the quinolones, and cephalosporins. Incidentally from several microscopy, culture and sensitivity studies, these antibiotics were found to be active against bacteria cultured from human bite wounds in varied degrees. 15,24 In a few of the patients, facial disfigurement was the primary reason for consulting the oral and maxillofacial unit.
Wound resulting from human bites is regarded as contaminated wound owing to exposure to the oral microbes from victim’s oral cavity and from inoculation from assailant’s teeth. However, there may not be frank infection in the early presentation but with delays in presentation, there is edema of various degrees, serous discharge, frank pus discharge, and increasing pain. A case of cervicofacial necrotizing fasciitis of the eyelid was reported in a series by Luksich et al. 25 There is a possibility of transmission of viruses from assailants to victims or vice versa. None of the patient in this series were screened for HIV and hepatitis B and C virus. It has been proposed in earlier work that HIV status of victims and assailants be known. 14
As our institutional protocol, surgical wound care for bite injuries includes debridement with copious irrigation with 0.9% saline solution and/or povidone-iodine solution, removal of tissue tags and granulation tissues, and antibiotic cover. Amoxicillin–clavulanic acid tablets 625 mg every 8 hours and metronidazole tablets 400 mg every 8 hours are our first-line choice of antibiotics for 1 week, then followed by immediate or primary surgical repair. Immunization status of all our patients are not known but they routinely received a booster dose of tetanus toxoid. There is diversity of opinions regarding the timing of surgical intervention to human bite wounds. While some studies concluded that immediate surgical closure of human bite injuries healed uneventfully, a few other studies support delayed primary closure. 9,14,18,20 We recorded a 100% success with primary surgical wound closure. All the cases were treated under local anesthesia with intravenous conscious sedation such as diazepam or midazolam titrated until “Verrill sign” is achieved in a few selected cases. The use of local anesthesia resulted in a significant cost reduction to the patients who could be discharged home on the same day. This is an important consideration as majority of the patients are poor and cannot afford general anesthesia and prolonged hospital stay.
The use of hyaluronidase injection into the wounds in delayed presentation by Baurmash and Monto 26 showed promising successes. Accordingly, wounds were debrided, copious irrigated with various antiseptic agents, wedge of tissue was removed, antibiotics were given, and wound were finally closed primarily in layers. Hyaluronidase is an enzyme that breaks down hyaluronic acid found in the extracellular matrix. Therefore, injection of hyaluronidase to wounds improves diffusion capacity and bioavailability of drugs including antibiotics and local anesthetics. The resultant effects are good pain control both intraoperatively and postoperatively as well as minimizing tissue swelling, tension, and easy manipulation of tissues and good wound healing. 27 The authors find this interesting and therefore would consider this for patients presenting late to the hospital in future studies.
Obtaining satisfactory aesthetics, restoration of functions, and restoring normal anatomic relationship of the defaced facial subunit is key. Therefore, repair of the avulsed subunits of the face is based on employing local flaps abutting or adjacent to the facial defect in small defects. 28 The advantages are good color, texture, and thickness match. The use of the simple wedge-shaped closure was employed when less than a third of the lip was missing, this is also a guide for ala and pinna avulsion. In some of our patients, the outcomes were satisfactory even when there was perceived tension of the wound (Figure 1A and B). Abbe flap was used in a single case for lip repair. With loss of ala, we found the nasolabial flap a better option (Figure 2A-C). The defects presented were not massive enough to use composite flaps. The case of ear avulsion was lost to follow-up.
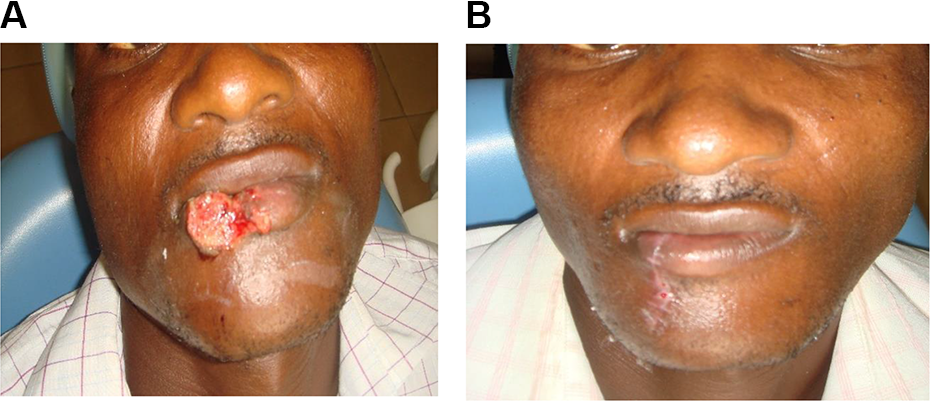
Picture shows loss of lip tissue due to human bite (A) and after simple wedged shaped excision and repair (B).
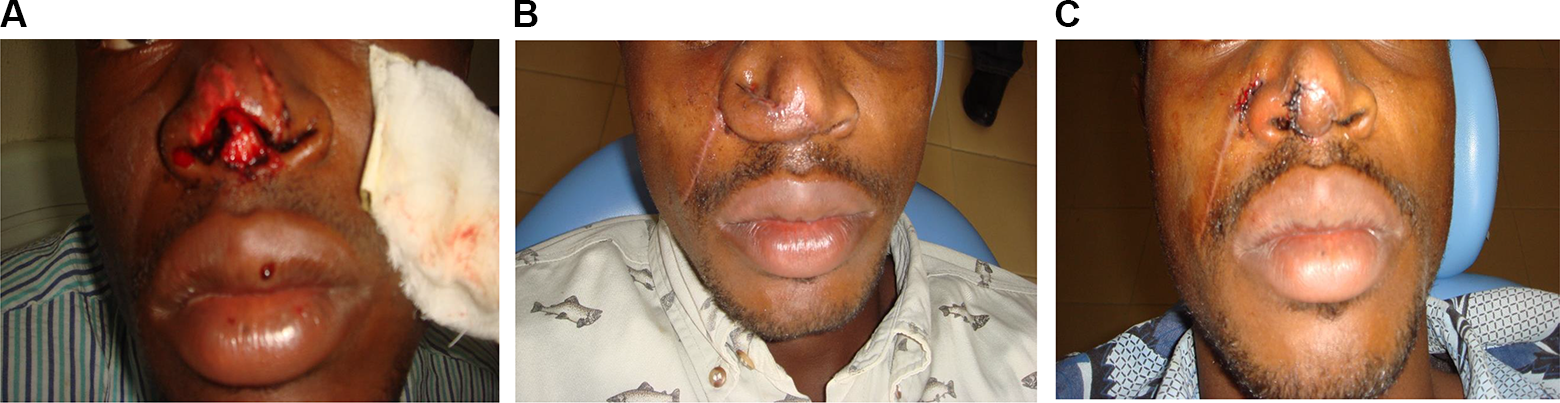
Picture shows loss of ala and septal cartilage repaired with an inferiorly based nasolabial flap (A) before surgery, (B) nasolabial flap in situ, (C) after surgery.
Our study just like many others in the literature reviewed facial human bite wounds paid emphasis on the victims of human bites not accounting for the assailants. The assailant’s medical history relating to immunization status, HIV, and hepatitis B and C infection should be known and documented. This study is from a single tertiary health facility, and our findings may have been representative of Port Harcourt city since the city has another tertiary referral center. However, this analysis provides an insight to a simple approach to human bite injuries and immediate surgical intervention with significant success. In conclusion, the human bite wounds reported in this study were all due to social conflicts without legal redress. Although human bite wounds are considered to be dirty or contaminated but with proper wound debridement, antimicrobial cover and primary or immediate surgical closure resulted in a very favorable aesthetic outcome in all the cases treated. Wedge-shaped closure or the use of local flaps gives better aesthetic outcomes
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
