Abstract
Background
Rising poisoning incidences worldwide, primarily in developing countries, remain ambiguous due to paucity of data and poison centres. This study evaluates patterns and factors causing poor outcomes in Kiambu County, Kenya.
Methods
A records-based retrospective cross-sectional study of poisoning cases who presented to nine facilities between June 2015 and July 2020 was conducted. The data collected was analysed through descriptive, bivariate, and multivariate logistic regression using STATA version 13.
Results
Kiambu county has a minimum prevalence of poisoning of 3.2%. A total of 434 cases were studied. Most cases (85.5%) resulted from acute exposures, with 75% being intentional. Pesticides (61.1%), paraffin (18.7%), alcohol (6.5%), and pharmaceutical drugs (4.4%) were the primary poisons used. 3.9% didn't fit these categories, while 5.5% remained unknown. Common presentations at admission were vomiting (35.3%) and unconsciousness (21.6%). Pesticides were responsible for 72.0% of deaths. Sequelae occurred in 7.8%, full but delayed recovery in 17.6%, and 6.0% died. The largest cluster of total cases was found in Thika town sub-county. It also contained the primary clusters of alcohol and pesticide poisoning. Being male (AOR 4.577, 95% CI [1.244–16.842]) was significantly associated with adverse outcomes. Regardless of the poison, the majority 78.8% made a full recovery.
Conclusion
Due to the lack of standardized poisoning data tools, patient records lack vital information reflecting the quality of care that the patient received, reflecting a lack of structures to collect, analyse and utilise poisoning data for decision making. This study underpins the need for the establishment of a PC in Kiambu county, Kenya.
Introduction
Poisoning has been defined as a medically undesirable state resulting from over-exposure to an exogenous chemical, 1 and most known chemicals can cause morbidity or mortality with sufficient exposure. 2 In just 16 African countries, it was estimated that unintentional poisoning accounted for 16,500 deaths and 1,128,500 disability-adjusted life years.3,4 Nonetheless, this issue continues to be inadequately characterized in African nations, primarily due to the scarcity of data and the near absence of poison centers (PCs).
Developed countries have well established PCs that provide information on mitigating, detecting, treating, as well as managing hazards. These PCs are equipped with patient management facilities and analytical laboratories which collect population-level data on poisoning in the community. 5 PCs subsequently retrieve and utilize de-identified patient information, which is uploaded into registries, to inform evidence-based decision-making for policy development. 6 For example, in the year 2019, United States of America was reported to have fifty-five (55) PCs, and data from these PCs revealed an alarming 6.4 poison exposures per 1000 of the population and 37.4 per 1000 poison exposures in children. 6 Cumulatively, these PCs documented an alarming 1 poison exposure in every 15 s. 6 To contrast these commendable numbers, the African continent has less than nine PCs, with Kenya having the only documented PC in Eastern Africa. 7
The World Health Organization (WHO) estimated that Kenya had 3.4 deaths per 100,000 in 2004 from unintentional poisoning. 8 This figure does not provide an estimate on the numbers of deaths due to deliberate poisoning, which has been estimated to be higher. 7 There also exists a lack of contemporary data to fully characterize the problem of poisoning in Kenya which is further compounded by the lack of accessible PCs. 9 This poses a significant challenge because, while information on the patterns of poisoning in Kenyan hospitals is limited, such information is crucial for the appropriate management of the rapidly growing scourge of poisoning in Kenya.2,6 We aimed to characterize the poisoning patients seen in Kiambu County, Kenya over a period of 5 years, to determine the outcomes, factors associated with said outcomes and investigate the geographic patterns of poisoning, all information vital in establishing a PC within the county.
Methods
Study design
This was a retrospective cross-sectional study reviewing patient records of those admitted for poisoning in Kiambu county, Kenya over a 5-year period between January 2015 and December 2020.
Study setting
Kiambu County is one of the 47 counties in the Republic of Kenya. As per the 2019 national census it has a total population of 2,417,735 with 49.1% (1,187,146) males and 50.9% (1,230,454) females. The county is 40% rural and 60% urban. It is in the former central province and covers a total area of 2543.5 Km2. Kiambu County borders Nairobi and Kajiado Counties to the South, Machakos to the East, Murang’a to the North and Northeast, Nyandarua to the Northwest, and Nakuru to the West. The county lies between latitudes 00 25’and 10 20 South of the Equator and Longitude 360 31’and 370 15’East. Kiambu is divided into twelve (12) sub-counties: Limuru, Kikuyu, Kabete Lari, Gatundu South, Gatundu North, Githunguri, Kiambu, Kiambaa, Ruiru, Juja and Thika Town. Agriculture is the predominant economic activity in the county and contributes 17.4% of the county’s income. Kiambu also hosts a variety of industries and has an extensive road network feeding one of the major superhighways in the country. Notably, the county lacks a Poisons Centre (PC).
Data sources
The medical records of all the individuals diagnosed with poisoning at the point of admission in all public hospitals in Kiambu county, Kenya.
Eligibility criteria
Inclusion criteria
All persons admitted to the accident and emergency department with a diagnosis of poisoning were included in the study.
Exclusion criteria
Patients not admitted for poisoning and/or patients whose medical records were not available.
Sampling technique
In the study period, there were a total of 36,718 hospital visits in Kiambu county with a diagnosis of poisoning as per the Kenya Health Information System (KHIS) MOH 705 A/B. All level 5 hospitals and 4 out of 12 level 4 hospitals were purposively selected as they had the highest number of poisoning cases in the county. Level 3 and 2 facilities were excluded as these facilities do not have in patient wards to admit poisoning patients. Furthermore, patients at these levels go home with their clinic card and thus these records are not retained at the facility. The sampling frame obtained from the KHIS showed a total of 4747 poisoning cases that were admitted in the 7 selected health facilities in the study period.
Sample size
Using Cochrane’s formula, a sample size of 384 poisoning cases was determined to have the power to detect a minimum prevalence of 50% in a previously not studied population with a power of 95% and margin of error of 0.05.
Definition of poisons
Pesticides: These include organochlorides, organophosphates, carbamates, pyrethrins, synthetic pyrethroids, herbicides, acaricides, rodenticides and any poison that is used for eradication of household and agricultural pests.
Pharmaceutical drugs: included prescription and non-prescription medicines.
Alcohol: These included all 1st, 2nd, and 3rd generation alcohols.
Toxidrome: a constellation of clinical signs and/or symptoms specific to a particular chemical or a class of chemicals or drugs. Whether or not a toxidrome was present in the study was based on the clinical signs and symptoms and the assessment of the attending medical professional.
Other: this included systemic and haematological agents, diuretics, drugs, medicaments, biological substances, corrosive substances, alcohols, gases, fumes and vapours that were unspecified.
Data collection
The sampled patient files were distributed proportionately by poisoning cases identified by facility (facility workload). Data were checked for completeness, accuracy and consistency via double data entry for cross-validation. Though 456 files were abstracted, 22 were dropped due to a lack of congruence.
Data analysis
The data were analysed using StataCorp. 2013. Stata Statistical Software: Release 13. Descriptive statistics including average, frequencies and percentages were reported. Bivariate and multivariate logical regression analysis was carried out to deduce factors associated with poisoning. To assess seasonality trends of reported poison cases the line plot of reported cases during the understudied period was used using the Breusch Godfrey LM test for autocorrelation. QGIS Geographic Information System was used to create descriptive maps. The unit of spatial analysis was in different sub-counties of Kiambu county. Heat maps and point maps were used to describe the distribution of the poison and mortality cases.
Ethical considerations
Ethical approval was obtained from Mount Kenya University (MKU/ERC/1737) and the National Commission for Science and Technology and Innovation (License No: NACOSTI/P/21/9127). The research was authorized by Kiambu County Health department.
Results
For 2019, Kiambu County had an incidence of poisoning of 3.73 per 1000 of the population using the 2019 census data.
Sociodemographic characteristics of the poisoning patients
Summary of the sociodemographic characteristics of the poisoning patients and the facilities where the patients were taken to be treated.
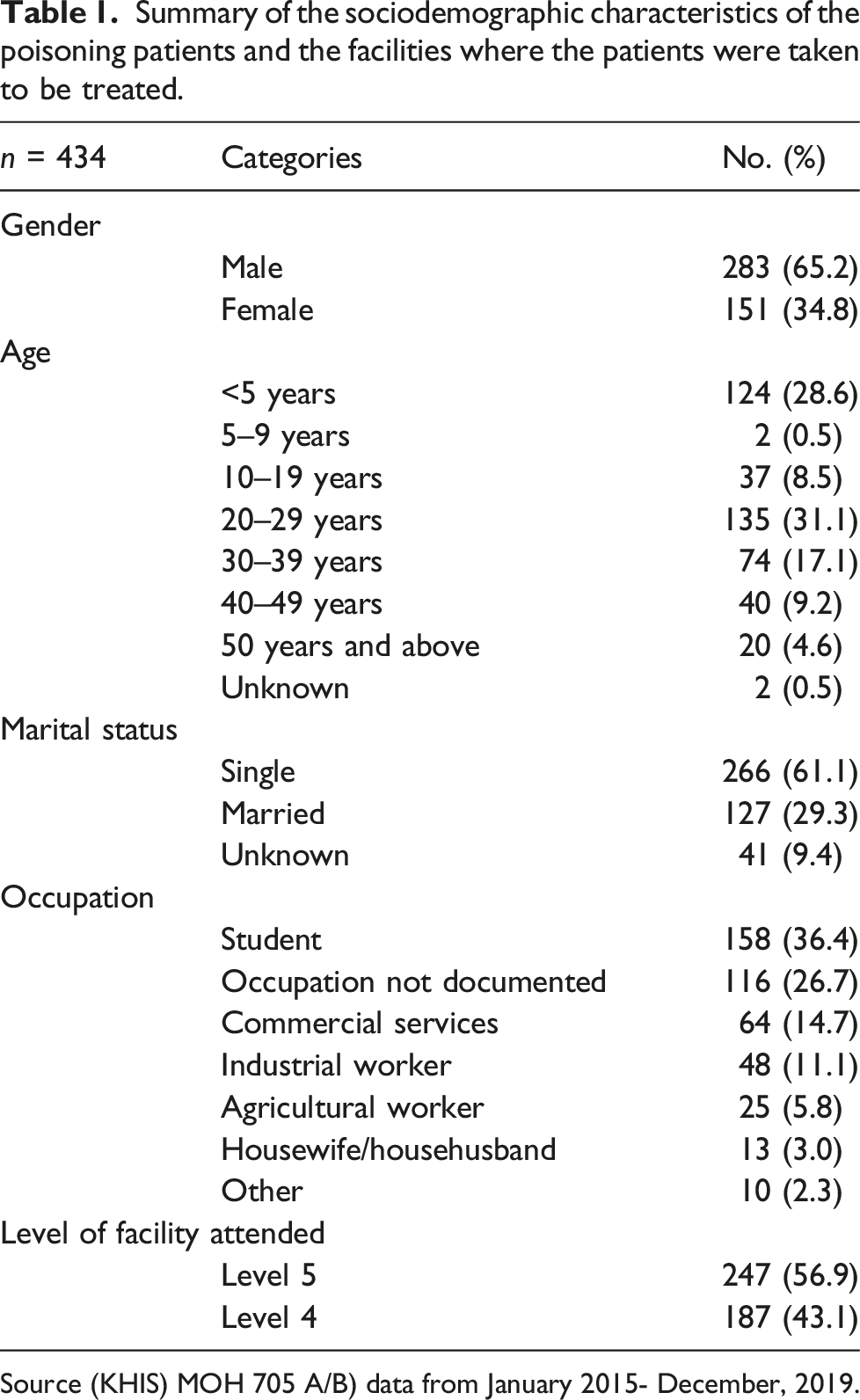
Source (KHIS) MOH 705 A/B) data from January 2015- December, 2019.
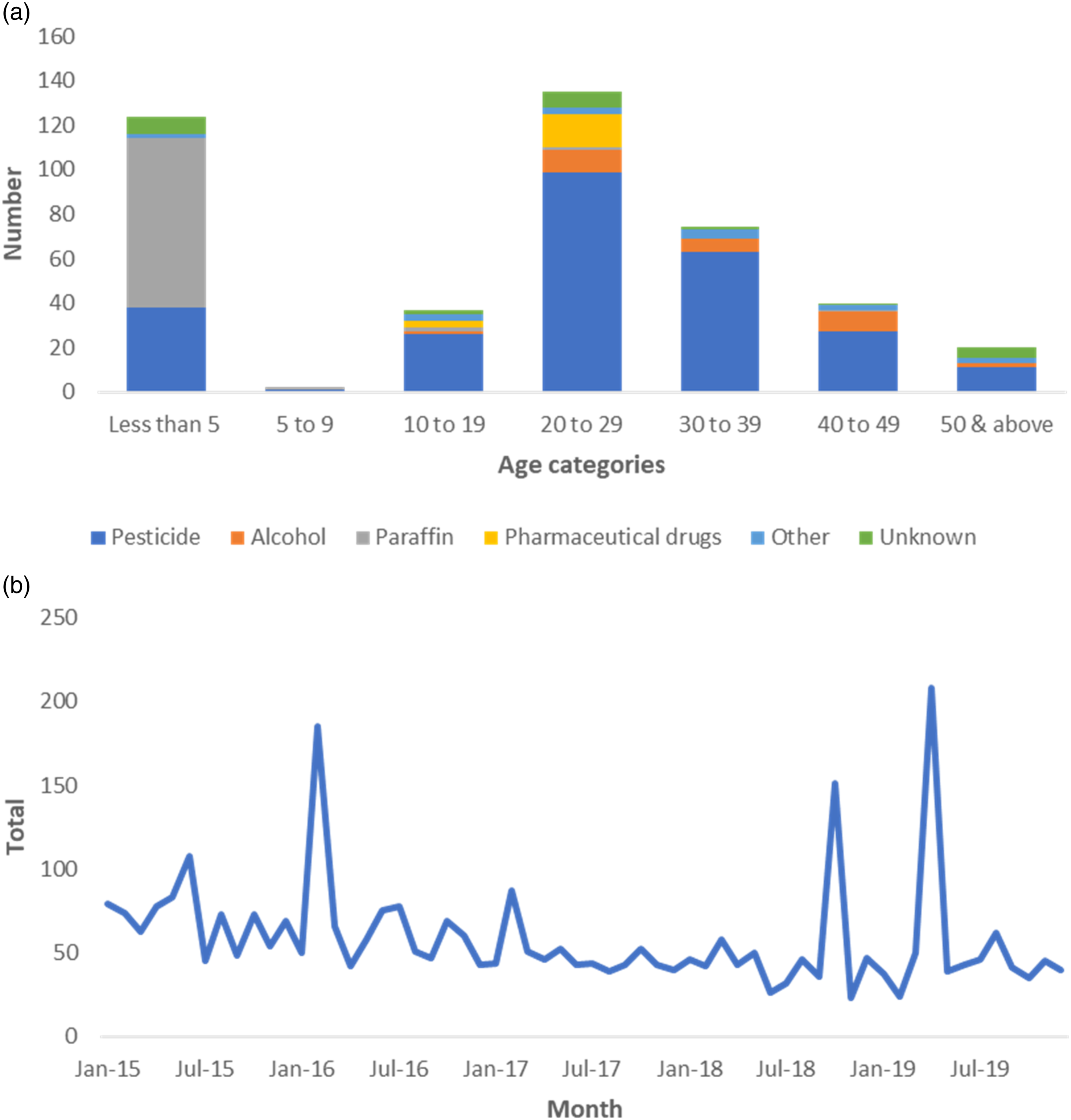
(a): The categorization of poisoning agents based on age groups. (b): The trends of poisoning cases in Kiambu County health facilities as documented in MOH-KHIS.
Trends in poisoning
A total of 36,718 cases of poisoning were reported in KHIS in the 5-year period between 2015 and 2019. After 2015 (8722 cases), there was a steep decrease in the number of cases in 2016 (6378 cases), 2017 (6370 cases) and 2018 (6230 cases). In 2019, there was a spike to 9018. There was no serial correlation between the twelve (12) lags and hence there was no notable seasonality in the trends of poisoning (Figure 1(b)).
Characteristics of the poisonings
Characteristics of the poisoning.
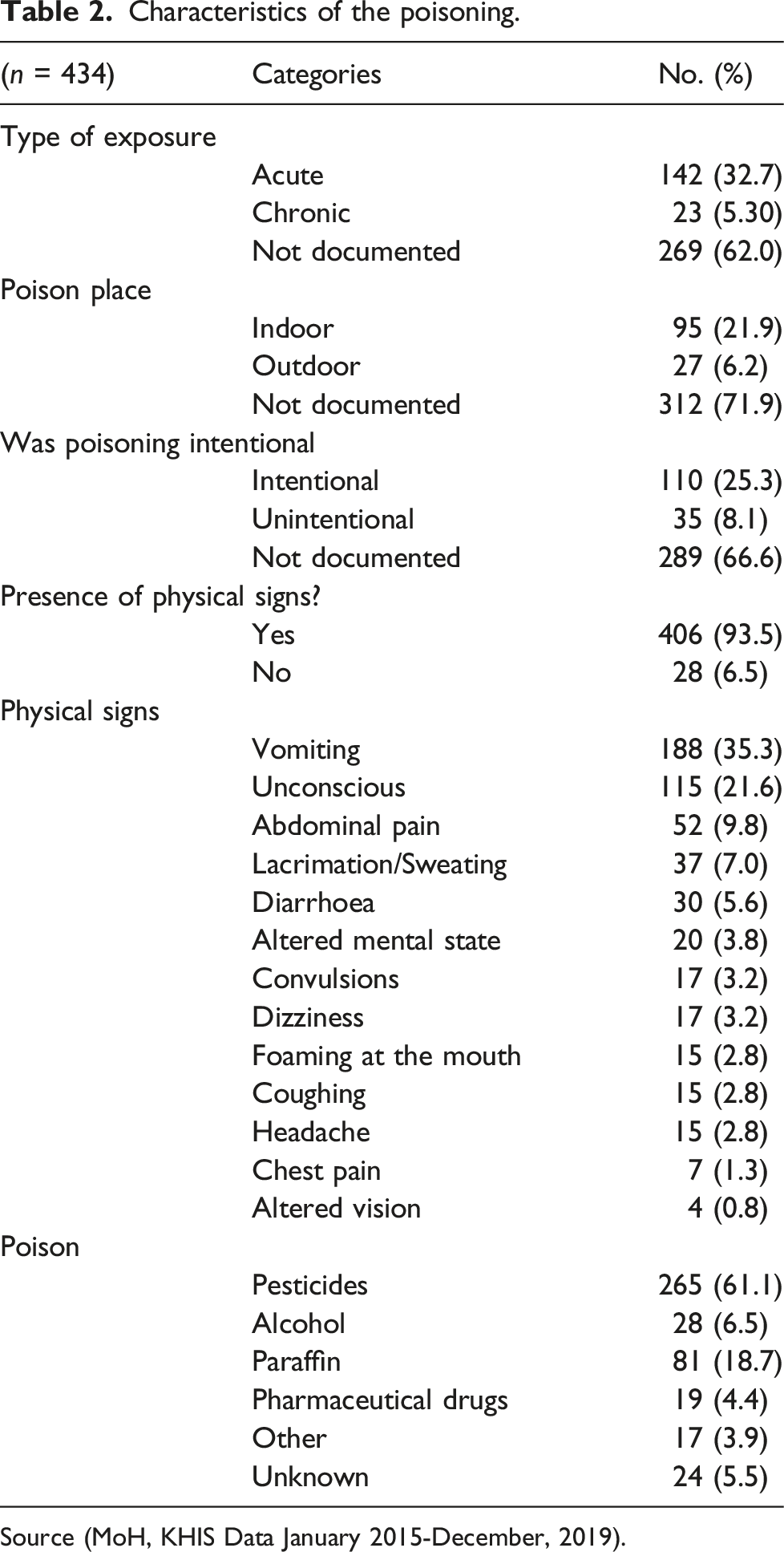
Source (MoH, KHIS Data January 2015-December, 2019).
The most common type of poisoning in this study was due to pesticides (n = 265, 61.1%). Because of the data collection process, 93 (35.0%) entries were explicitly categorized as organophosphates, while the remaining entries (65.0%) were labelled as various brand names or generic terms for insecticides or pesticides. Among the pharmaceutical agents, 1 was identified as a benzodiazepine, 2 as antipsychotics, 1 as a tricyclic antidepressant, 1 as a derivative of warfarin, 4 as nonsteroidal anti-inflammatory drugs (NSAIDs), and 2 as antihistamines. It's worth noting that many of these agents were used in combination, and the rest were too nonspecific to classify.
The poison was ingested orally in the majority of cases. In the rest of the cases, the poison was: inhaled (n = 6, 1.4%); inhalation/skin contact (n = 1, 0.2%); inhalation/skin contact and eye contact (n = 1, 0.2%); injected (n = 1, 0.2%); skin contact (n = 1, 0.2%) and eye contact (n = 1, 0.2%).
The physical nature of the poisons was liquid (n = 141, 32.4%), powders (n = 25, 5.8%), tablets (n = 22, 5.1%) and gases (n = 2, 0.5%), but the physical nature of 244 (56.2%) was unknown. Of the 39 (9.0%) adverse reactions, (n = 28, 71.8%) were due to drugs, and (n = 10, 25.6%) due to food poisoning (the type of drugs and foods were not documented in patient records). The rest (n = 395, 91.0%) were not documented altogether.
Where intention of poisoning was documented, majority of the cases were suicide attempts (n = 110, 75.9%). Of these attempts, majority used pesticides (n = 64, 58.2%), followed by pharmaceutical drugs (n = 44, 40.0%), and the poison used by the rest (n = 2, 1.8%) was unknown. Those who used pharmaceutical drugs also used alcohol (n = 5) and other drugs (n = 14).
The outcomes of the patients based on time-lapse between poisoning incident and presentation at the emergency department, type of poisoning agent and treatments administered.
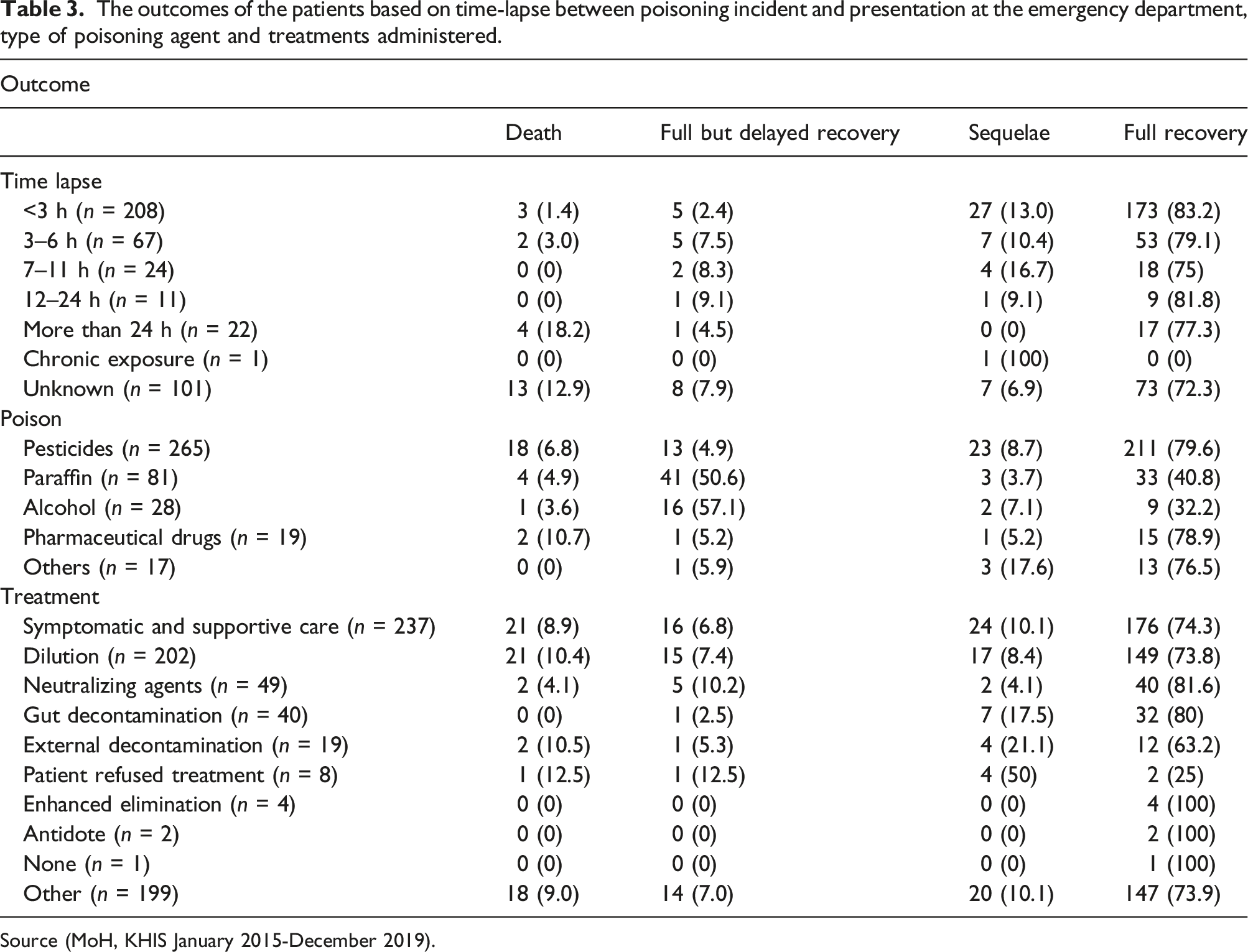
Source (MoH, KHIS January 2015-December 2019).
Most cases were admitted for 1–6 days (n = 355, 81.8%) with the rest being admitted for durations as follows: 1–4 weeks (n = 46, 10.6%); less than a day (n = 31, 7.1%) and more than 4 weeks (n = 2, 0.5%). The length of hospital stays for 1 (0.2%) patient was not documented.
Of the complete data (disregarding the “unknown” categories, n = 410), regardless of the course of poisoning, most of the patients made a full recovery (n = 281, 68.5%), 32 (7.8%) had sequelae and 72 (17.6%) had a full but delayed recovery. Death was the outcome of 25 (6.0%) of the poisonings, and of these, 72.0% were due to pesticides.
All cases that were seen received at least one management modality, though multiple treatments were often administered to one patient. Among the 434 patients who received care 237 (54.6%) received symptomatic and supportive care. This was followed by dilution (46.5%); administration of neutralizing agents (11.3%); gastro-intestinal decontamination (9.2%); external decontamination (4.4%) and enhanced elimination (0.9%). Only two received an antidote (0.5%), and eight patients declined any treatment. On top of the aforementioned treatment modalities, 199 (45.9%) received other additional treatments. Four (0.9%) the patients admitted after 24 h died.
Spatial clustering of poisoning cases in Kiambu county
For the total number of poisoning cases, there were a total of seven (7) significant clusters in Kiambu county. The biggest cluster was in Thika town sub-county, followed by a cluster in north-west of Ruiru bordering Juja sub-counties and South-west of Ruiru bordering Roysambu sub-county and another cluster was seen in Kiambaa bordering Westland’s sub-county. A hotspot cluster for mortality was identified in Ruiru sub-county bordering Roysambu sub-county (Figure 2). Distribution of all poisoning cases and mortalities in Kiambu county, Kenya over the 5-year period data from January 2015-December 2019.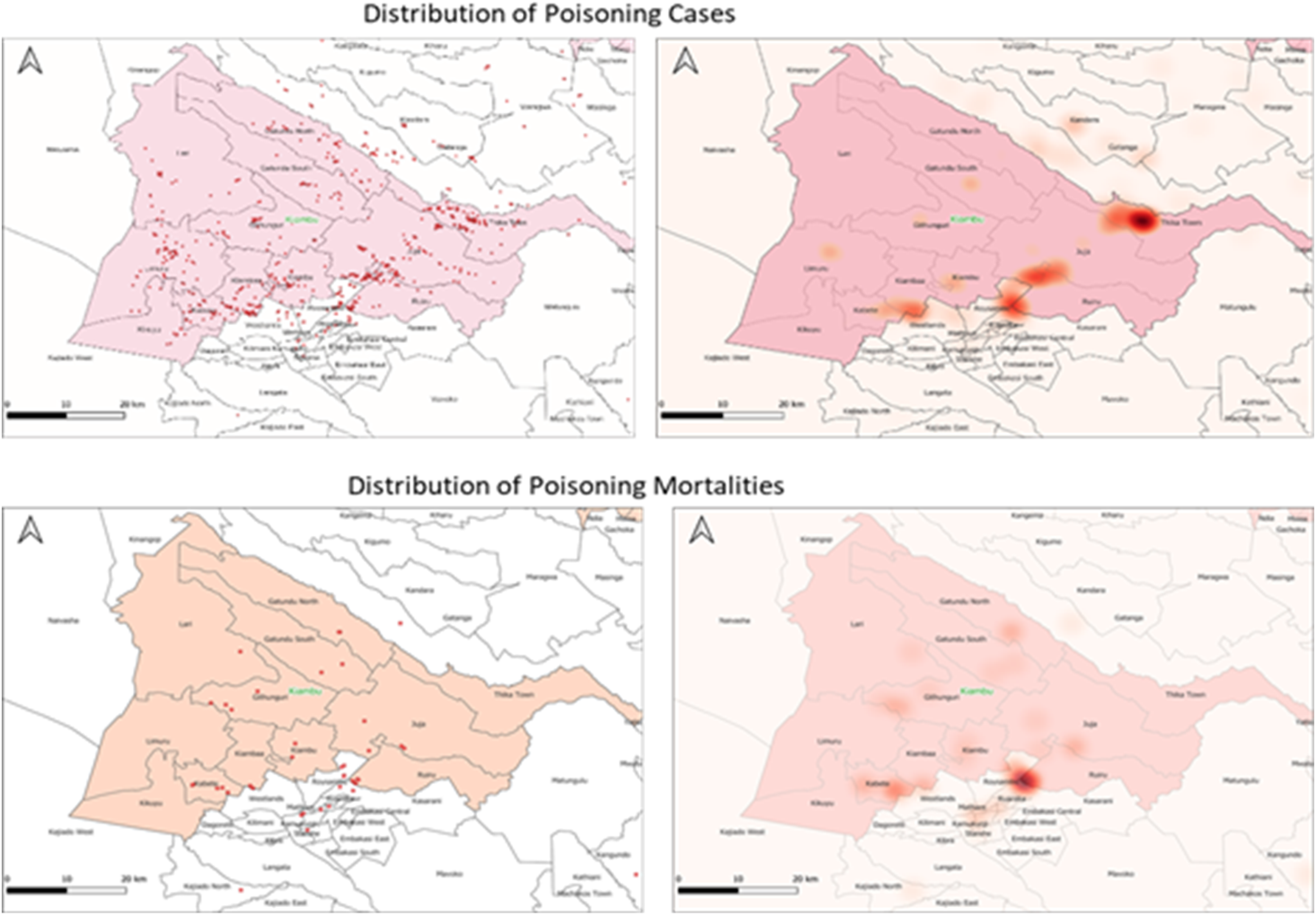
The primary cluster for alcohol poisoning was in Thika town sub-county while the primary cluster for organophosphate was in Ruiru bordering Roysambu sub-county. Pharmaceutical drugs’ primary cluster was found in Juja and Thika town sub-counties, with the pesticide primary cluster being found in the latter Figure 3. Distribution of poisoning cases by poison group in Kiambu county, Kenya over the 5-year period data from January 2015-December 2019.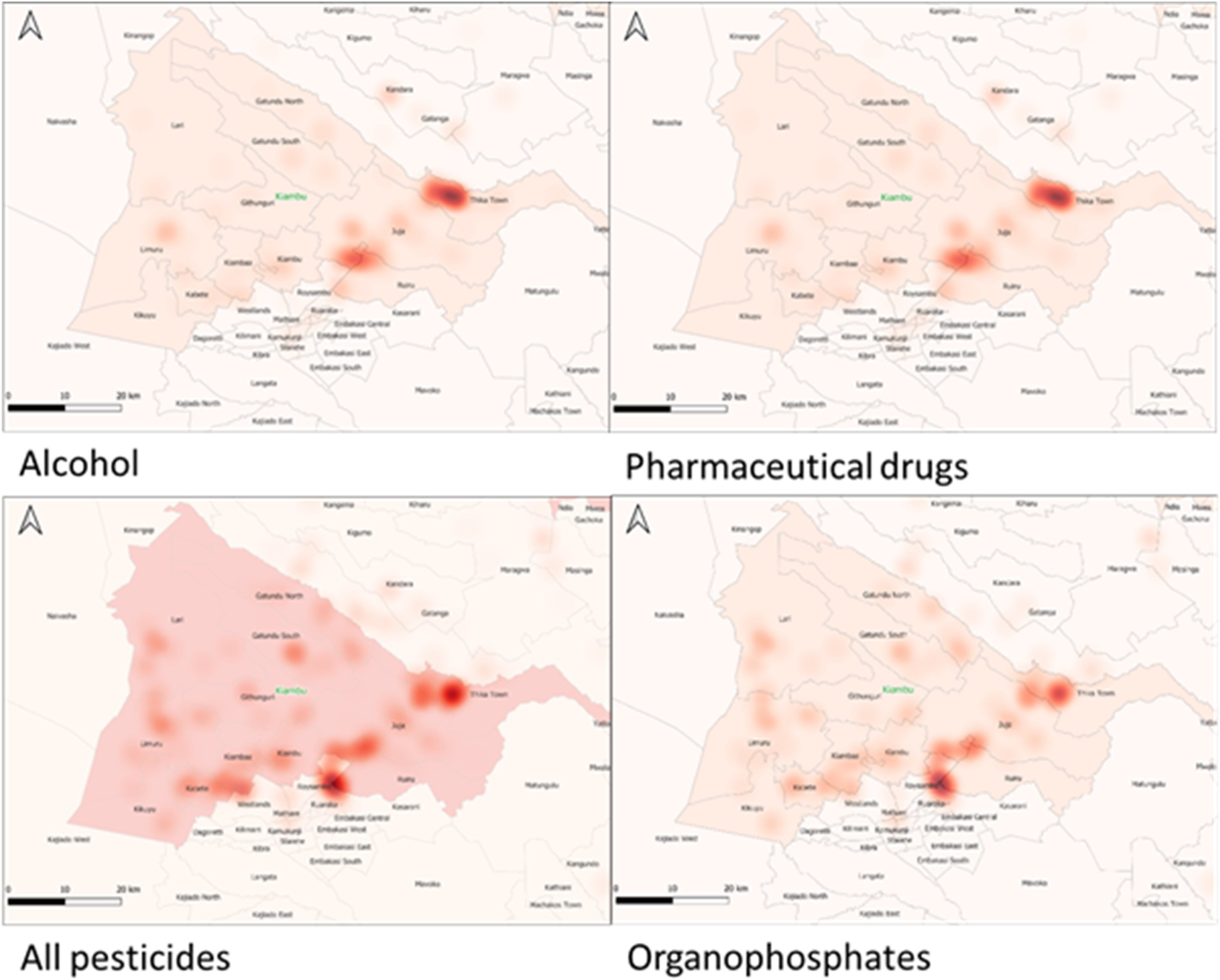
Factors associated with poisoning
The results of the bivariate and multivariate analysis to quantify the relationship between treatment outcome and gender, age, marital status, facility, and the time between poisoning and receiving treatment.
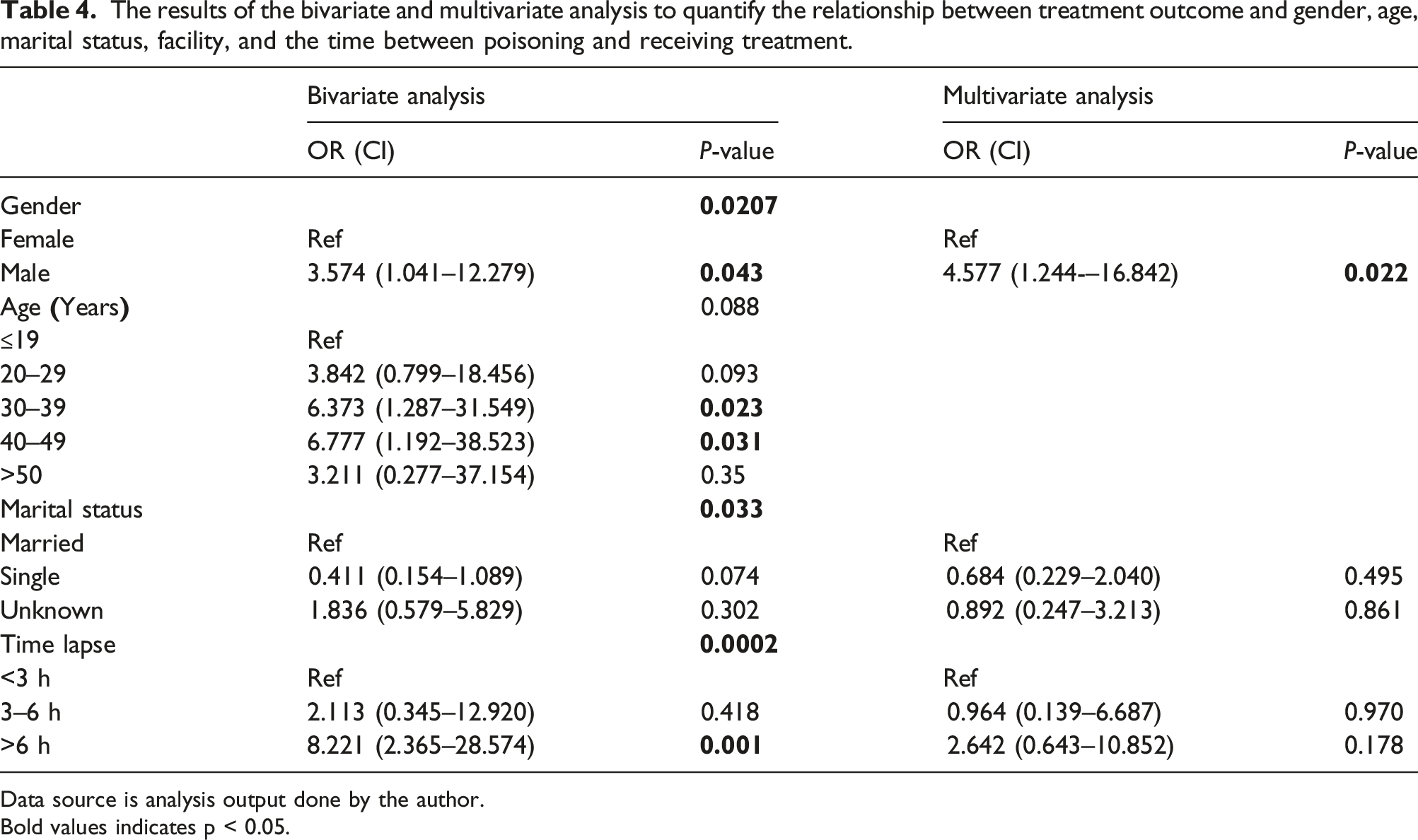
Data source is analysis output done by the author.
Bold values indicates p < 0.05.
The multivariate logic regression model included the dependent variables, gender, marital status, facility, and time to facility. Stepwise regression analysis was used to select the independent variables in multivariate analysis and all these variables were considered potential explanatory variables. Being a male was a significant predictor of the treatment outcome (OR = 4.57, p = .022). There was no statistically significant association between the treatment outcome and the time it took to get to hospital and marital status when we adjusted for the other variables. Table 3 summaries the results of the bivariate and multivariate logistic regression analysis of the factors associated with poisoning. The male patients (p = .043), relationship status (p = .033) and time-lapse to presentation were all associated with poisoning, as shown in Table 4 below.
Discussion
To our knowledge, this is the first attempt to describe the incidence of poisoning in Kiambu County, Kenya. Kiambu county had a incidence of poisoning of 3.73 per 1000 in 2019, higher than the 0.7 per 1000 previously reported in a study conducted in the Rift Valley province of Kenya in 2012. 9 This rise may be due to ease in access to poisoning agents, social behaviour, and the absence of regulating bodies. Furthermore, no seasonality in trends of poisoning cases was found. This contrasts with a study conducted in the Duke Poison Control Centre that examined trends of poisons and affected victims over a calendar year. 10 It was found that pesticide poisoning was predominant in preschool victims during the summer while pesticides affected older adults during the months of spring.
An Ethiopian study found that approximately half the poisoned patients were between 21 and 30 years old. 2 Our findings were similar. This is also corroborated by a hospital-based surveillance study in Tanzania. 11 In the present study, the second most commonly affected age group was children below the age of five, a finding reflected in a 2015 study conducted in Australia. 12 This has been largely attributed to unintentional poisoning as this age group frequently explores their environments by placing things in their mouths indiscriminately. 13
Three-quarters of the poisoning cases in the current study were intentional, in line with studies conducted in Hospital emergency departments in both Shenyang, China and Ethiopia.2,14 We found that many of the poisoning cases were acute exposures, took place indoors and presented with toxidromes. A study in Egypt found that 40 percent (40%) of poisoned cases presented within 6 h to hospital while others presented more than 6 h after exposure. 15 We found that 62.3% of cases in Kiambu County were brought to a health facility within 3 h of exposure, which is a timely response. After arrival, 81.8% of the patients spent 1–6 days in the hospital. This is similar to a study conducted in Iran where the mean duration of hospital admission was 4.66 days. 16 However, this was the average stay for patients admitted to the intensive care unit while our study just looked at in-patient admissions.
Almost a tenth of the cases experienced sequelae 6.0% died. These proportions contrast with a study from the United Kingdom wherein less than 5% of patients experienced serious clinical side effects and mortality rates were less than 0.5%. 17 This may be due to the different poisons used, as in the previous study paracetamol was the most used poison. It may also be due to the UK having established PCs in the form of the National Poisons Information Service, as well as established cadres for clinical toxicologists in their hospitals that can rapidly respond to the cases and improve their outcomes.
Pesticides caused an abysmal 72.0% of the poisoning-related deaths in Kiambu. This is in contrast to the 6.6% rate reported in a study conducted in Pakistan. These deaths could be attributed to late presentation as the ‘ageing’ reaction of organophosphorus-inhibited cholinesterase activity is time-dependent and dictates the therapeutic window.18,19 This is also probably why majority of the late presentations led to death in this study. This could be remedied by the implementation of PCs which deliver antidotes and prevent precious time being lost during referral. Symptomatic management of the toxidrome and dilution were the main treatment modalities used in the present study, in-line with conventional treatment algorithms for patients who have been poisoned to alleviate toxidrome symptoms. 20
Temporo-spatial mapping of poisoning cases revealed Thika town as the most significant cluster. Thika is an industrial town with several workers in this area having direct access to industrial chemicals. Our findings indicate that 36.4% of participants were students. This could explain why Thika Level 5 Hospital reported the highest number of suicide cases as Thika town hosts seven (7) tertiary institutions and high proclivities to suicidal behaviour in students has been previously established. 21 This town possessed a primary cluster for alcohol poisoning. A survey from the National Authority for the Campaign Against Alcohol and Drug Abuse in 2011 revealed that alcohol use was a major concern citing the fact that the alcohol was readily available. 22 It also had a geospatial cluster for pharmaceutical drugs. The use of pharmaceutical drugs for poisoning has been documented in urban areas and developed countries, 13 and hence can be attributed to Thika’s cosmopolitan nature.
Pesticides followed by paraffin and alcohol were the most used poisons in the present study. In a South African study, 34.8% of all the poisoning cases were due to pesticides, consistent with the current study’s findings. 23 Kiambu is an agricultural county, there is ready access to pesticides making it an easy go to in deliberate self-poisoning, which is in-line with a systematic review conducted by the WHO on the global distribution of poisoning with pesticides. 24 Paraffin poisoning was the second most common cause of poisoning and affected mostly the younger age groups. This is akin to another study conducted in Kenya. 25 This has long been attributed due to its resemblance to water and improper storage.
Organophosphate poisoning was concentrated in Ruiru, an agricultural zone with heavy use of insecticides for domestic use, as well as poor sanitation and hygiene that further aggravates the problem of insects and infestations. Ruiru had the second-densest in all poisoning cases and possessed the main mortality cluster. This cluster borders Roysambu, a rural area with low economic status where most farmers may not have the required personal protective equipment when using pesticides, making it a culprit for accidental poisoning. The frequency of substance-related mortality in rural regions has increased over the last decade and there is growing worldwide acknowledgment on the rapidly expanding use of poisons in rural communities. 26 A study conducted on the utilization of poison control centres in a rural setting showed that for every 43.3 calls made to the centre, one hospital admission for poisoning was prevented, 27 which brings forth the utility of its establishment in Kiambu county. An organophosphate cluster was also found in Githunguri where zero-grazing is a dominant activity and acaricides are commonly used to eradicate ticks and hence are readily available.
Our study is not without limitation. In the county, poisoning patient details are captured in patient files without a clear or standard format. The KHIS summary tool gives an aggregate number of all patients poisoned without any associated details and most pertinent variables collected had incomplete data, including occupation, type of exposure, place of poisoning, whether poisoning was intentional or not, and the outcome given the various time lapses. In the instance of intention behind poisoning, 33.3% were not documented. The study was also conducted only in public sector health facilities and mortalities that occurred elsewhere were not taken into consideration.
Conclusion
Sequelae and fatalities from poisoning are minimal in countries with PCs. 28 A robust system of early diagnosis, poison detection and delivery of antidotes can allow clinicians to attend to emergencies promptly and efficiently. A PC also provides a reference point for information gathering and sharing both to the medical personnel and public. Furthermore, clinical toxicologists can harness the information gathered by PCs and guide treatment and management of patients in hospital settings. This study emphasizes the need for establishing well-functioning PCs in developing countries. There is also a need to develop a standardized national tool for the collection of poisoning data. Kenya should also develop a standard poisons management guideline.
Supplemental Material
Supplemental Material - Poisoning patterns and factors associated with treatment outcomes among patients: A case study of Kiambu county hospitals, Kenya
Supplemental Material for Poisoning patterns and factors associated with treatment outcomes among patients: A case study of Kiambu county hospitals, Kenya by James Maina Githinji, Michael Mungoma, Kinara Fossa, Jesse Ngugi, Samwel Ondiek, Prabhjot Juttla, Alfred Owino Odongo, Moses Ndiritu and Magoma Mwancha-Kwasa in Toxicology Research and Application
Footnotes
Acknowledgments
We are indebted to Beate Ringwald and Robinson of LVCT Health for their technical support during the conceptualization and initial stages of this study. The contributions of various people, as well as governmental and commercial entities, made this project feasible. We are grateful to the County Health Management Team and the County Government of Kiambu for supporting the study's inception and granting permission for its members to take part in a variety of capacities. We also appreciate Dr. Francis Makokha, who peer reviewed the manuscript. Special recognition goes to EGPAF, which supported the final stage of writing and submission of the manuscript.
Author Contributions
Dr. James Maina Githinji: Conceptualization, Study design, protocol development, investigation, Resource provision, Project administration, Data curation, writing original draft, and Review editing, Authorizing publication, Corresponding author. Dr. Michael Mung’oma: Conceptualization, researched literature, Study design, resource provision, Data curation, writing original draft, Protocol development, Gaining ethical approval and Review editing. Ms. Kinara Fossa: Data analysis. Dr. Jesse Ngugi: Resource provision. Mr. Samwel Ondiek: Resourse provision. Prabjot Juttla: Wrote the first draft of the manuscript, review and editing. Dr. Alfred Owino Odongo: Final review and editing. Dr. Moses Ndiritu: Final review and editing. Dr. Carolyne Magoma Mwancha-Kwasa: Conceptualization, project administration, Data curation, writing original draft, and review editing.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical statement
Data availability statement
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
