Abstract
Background
The relaxing of COVID-19 pandemic restrictions has not seen the return to previous in-person teaching formats. As blended training continues to be used, there is emphasis on the need to better appreciate the expectations, etiquette, and professional code of conduct (“netiquette”) surrounding online learning, especially in light of evidence that poor online professionalism compromises learning and clinical practice.
Objectives
This review seeks to map regnant netiquette guidelines in medical schools that will inform and provide preliminary recommendations for a clinically relevant framework.
Design
This study is a systematic scoping review (SSR).
Methods
Krishna's Systematic Evidence-Based Approach (SEBA)'s Constructivist ontological and Relativist epistemological lens was used to guide this SSR. The SEBA process involves 6 stages, including the
Results
In total, 7941 abstracts were reviewed, 198 full text articles were evaluated, and 83 articles were included. The analysis of the results revealed 4 key domains: (1) current guidelines, (2) manifestations, (3) contributing factors, and (4) implications. This SSR in SEBA highlights variability and gaps in current guidelines and reveals the impact of sociocultural factors on breaches in netiquette. Unsurprisingly, contextual and clinical considerations shape the contributory factors impacting lapses in netiquette and their implications.
Conclusions
Based on the data accrued, this article proposes basic guidelines on netiquette and measures to support their effective employment. This includes curricular adaptations, methods of teaching and enhancing engagement with the students and faculty training. Drawing on prevailing studies, it also recommends methods of assessing netiquette, online professionalism, and the learning environment. Suggestions are also made for future areas of study.
Keywords
Introduction
Observing appropriate digital social norms or netiquette has been far from simple. The online training environment has unique traits, conditions, professional standards, codes of conduct, roles and responsibilities, implicit norms, culture, values, beliefs, and principles1–9 (henceforth netiquette). 10 This environment offers upcoming physicians a unique and regulated learning environment that inculcates them with the requisite knowledge, skills, and attitudes needed for the competent future physician. However, the sudden adoption of netiquette as teaching moved to online platforms to adapt to the COVID-19 pandemic has also compromised learning.11–15 Confounded by unclear program expectations, roles and responsibilities, as well as rules of conduct expected of users, medical students have struggled to adapt to professional, social, and clinical expectations on participation during online teaching. Of note, these struggles have also resulted in unprofessional behavior, 16 compromised interpersonal relationships, 17 disengagement,18–21 and poor learning environments.
Even now, as COVID-19 restrictions have begun to ease and as in-person teaching has resumed, online teaching continues to be employed. To address this gap and sustain online professionalism and etiquette (netiquette) to guide online communication, clinical teaching, and build a conducive online learning environment,22–24 a review of current netiquette guidelines is proposed.
Methodology
We adopt Krishna's Systematic Evidence-Based Approach (SEBA) to guide a wide-ranging review of netiquette guidelines. The constructivist approach25,26 and relativist lens27,28 are best placed to account for the regnant social, cultural, ethical, legal, professional and contextual considerations,29,30 alongside the desired characteristics and expectations set out by professional, organizational and ethico-legal practice that shape netiquette guidelines 31 and how netiquette guidelines are interpreted by the organization and medical students. Furthermore, compliance with netiquette guidelines is contingent upon factors such as the medical student's narratives,32,33 belief systems, 34 competencies, context, experience, goals and motivations, as well as duration of their interactions within the program. 35 These factors affirm the SEBA's ontological and epistemological roots.
A SEBA-guided systematic scoping review (SSR) (henceforth SSR in SEBA) methodically maps existing data, structures the extraction of key characteristics of netiquette, synthesizes and summarizes actionable and applicable information.36–40 This complex process relies on SEBA's 6-stage process which is illustrated in Figure 1.
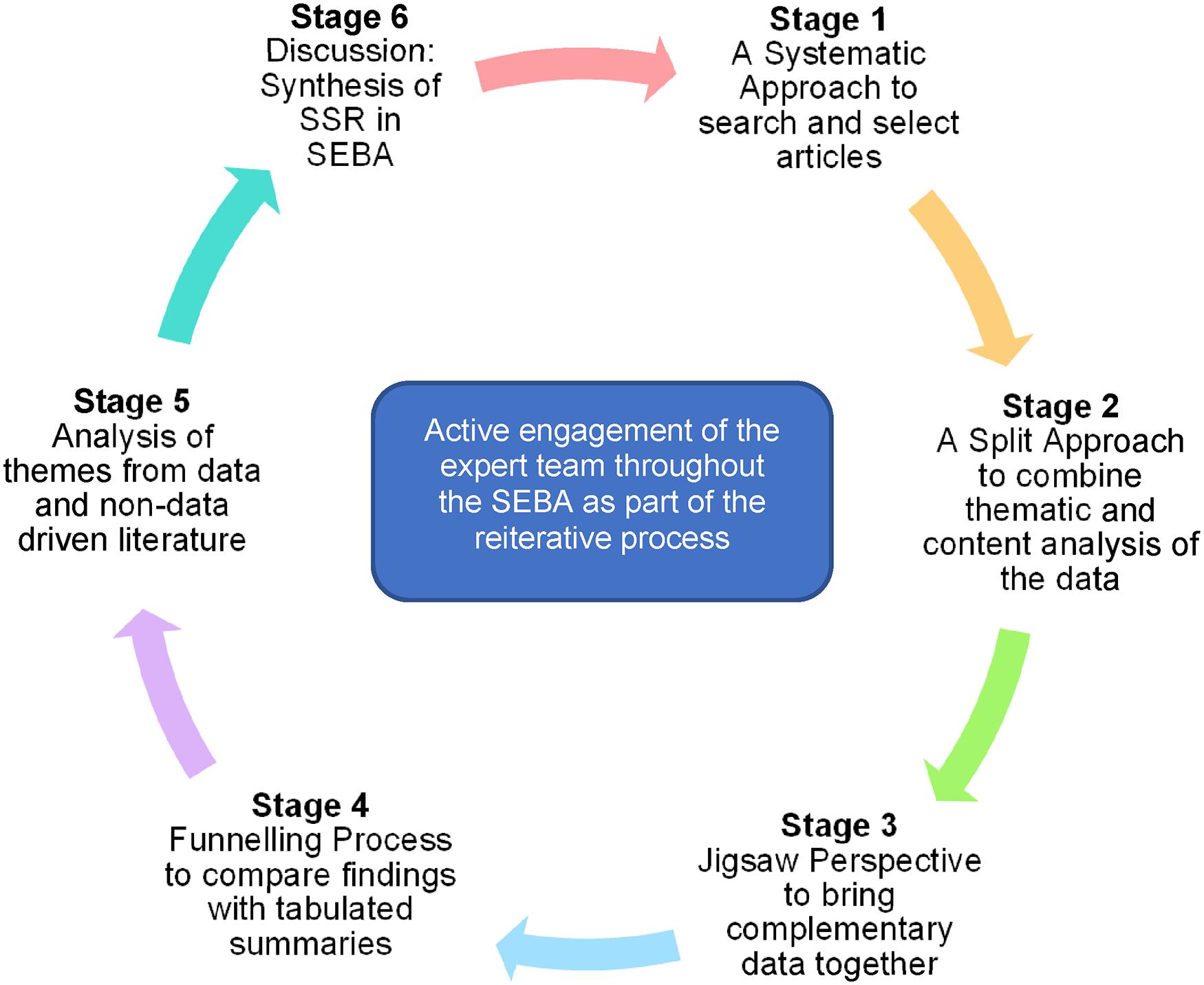
The SSR in SEBA process. Abbreviations: SEBA, Systematic Evidence-Based Approach; SSR, systematic scoping review.
An expert team comprising of a librarian from the National University of Singapore's (NUS) Yong Loo Lin School of Medicine (YLLSoM) and local educational experts and clinicians at YLLSoM, National Cancer Centre Singapore, Palliative Care Institute Liverpool, and Duke-NUS Medical School were recruited to provide a balanced review, ensure transparency and accountability, and oversee all aspects of the SEBA cycle.
Stage 1 of SEBA: Systematic Approach
The review was guided by a PCC (Population, Concept, Context)
41
framework. The PCC framework was employed to guide the primary research question, “
PCC, inclusion, and exclusion criteria applied to database search.

Abbreviation: PCC, Population, Concept, Context.
Independent searches were conducted on PubMed, SCOPUS, ERIC, Google Scholar and Embase databases between September 12, 2021 and January 1, 2022 for articles on online professionalism and standards of practice in online interactions within medical schools, published between January 1, 2000 and December 31, 2021. The review was restricted to papers published after 2000
42
to facilitate a sustainable research process. The full search strategy may be found in
For every 100 articles in a particular database, the medical students, peer-mentor, and senior researcher compared their findings at an online meeting. Sandelowski and Barroso’s 43 “negotiated consensual validation” was used to achieve consensus on the final list of titles to be reviewed. The process was repeated where consensus was again required; interrater reliability was not evaluated.
Stage 2 of SEBA: Split Approach
The “Split Approach”25,42–44 was employed to enhance the reliability of the data analyses. Two groups of researchers independently analyzed the included articles. The first team analyzed the included articles using Braun and Clarke 45 's approach to thematic analysis by identifying common characteristics, creating codes to analyze the rest of the articles, and subsequently categorizing the codes into categories, and the categories into themes that best represent the data. 46 The research team employed Sandelowski and Barroso’s 43 “negotiated consensual validation” approach to determine a final list of themes.
The second team utilized a priori codes and categories derived from Taggar et al’s
47
“
Stage 3 of SEBA: Jigsaw Perspective
The identified themes and categories were viewed as pieces of a jigsaw puzzle. Guided by phases 4 to 6 of France et al’s 52 adaptation of Noblit et al’s 53 7 phases of meta-ethnography, complementary pieces of the jigsaw were combined into themes and categories (Table 2).
Themes and categories.

Stage 4 of SEBA: Funneling
The Funneling Process compared the final themes/categories with the compiled summaries of the included articles to ensure that the data effectively represented current thinking. This process created domains that guided the discussion process in stage 6 of the SEBA.
Results
In total, 7941 abstracts were reviewed, 198 full text articles were evaluated, and 83 articles were included (Figure 2). A further 7 additional articles were snowballed from existing articles to yield a total of 90 included articles. We also reviewed online guidelines of the top 10 ranked medical schools on the Times Higher Education 2022. 54

PRISMA flow chart.
Forty articles were quantitative studies, 14 were qualitative studies, 4 were mixed studies, 25 were descriptive/opinions/proceedings/reviews/perspectives/monographs and 7 were university guidelines. The themes and categories identified overlapped with current guidelines, contributing factors, and their implications. A thematic analysis also highlighted the manifestation of breaches in online professionalism.
Results
The domains identified were: (1) current guidelines, (2) manifestations of poor netiquette, (3) contributing factors, and (4) implications.
Domain 1: Current Netiquette Guidelines
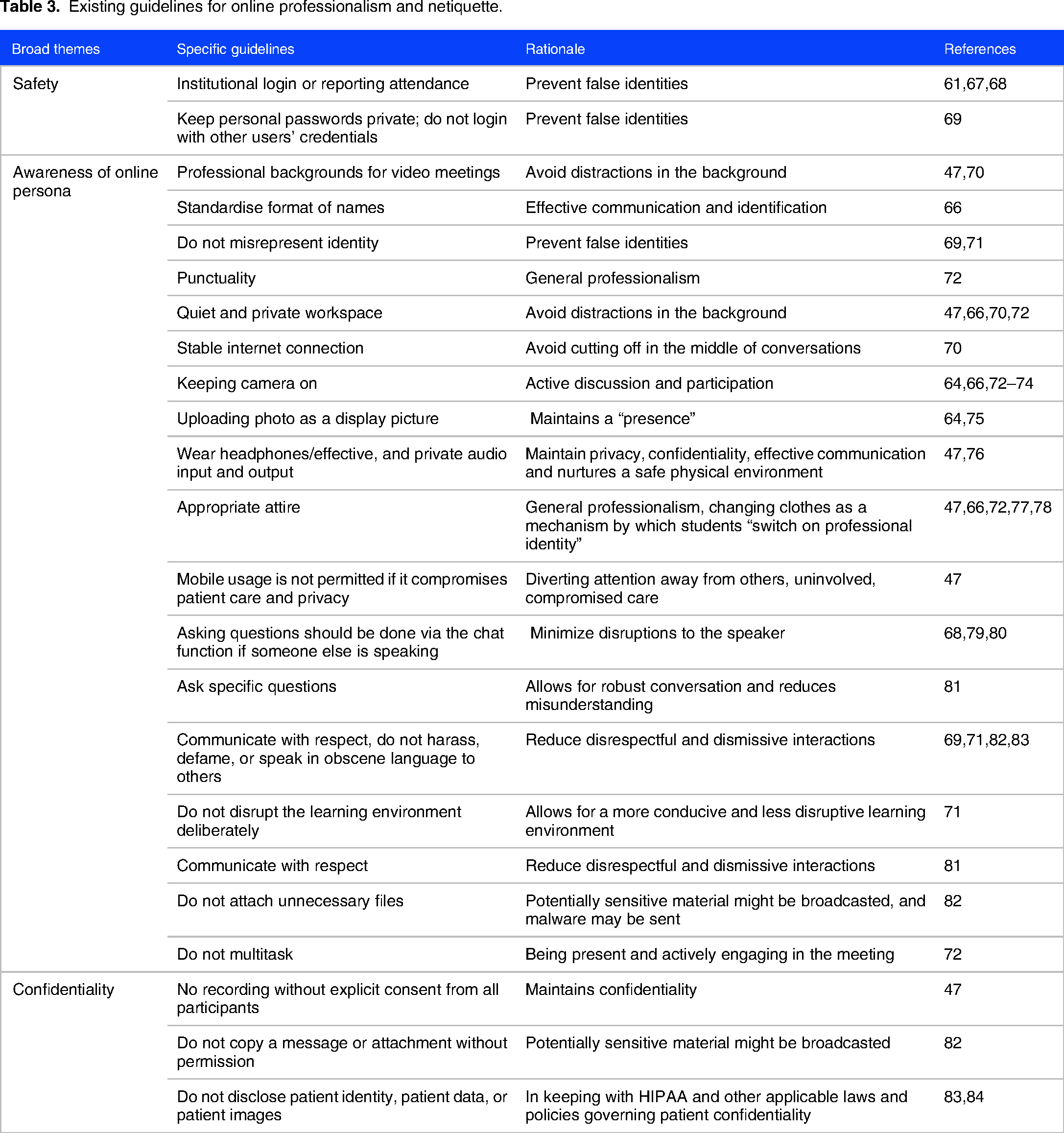
A review of publicly accessible online netiquette guidelines among the top 10 ranked medical schools on the Times Higher Education 2022 list did not reveal any results. 54 Among the 90 included articles,17,47,48,55–62 guidelines varied on key issues, such as confidentiality, safety, and awareness of online personas.63–65 These variations are credited with the rise in breaches in professionalism and standards of practice (Table 3).24,47,66
Existing guidelines for online professionalism and netiquette.
Domain 2: Manifestations
The lapses in netiquette fall into 2 groups—technical and individual lapses (Table 4).
Manifestations of compromised online professionalism and netiquette.

Individual lapses in netiquette included poorly selected and inappropriate learning environments,85,88,90 failure to turn on their videos,59,62,73 poor participation,73,93,95 and a lack of attention during lessons and discussions.75,92–94
Technical lapses included an unstable internet connection85–89 and inadequate and/or inappropriate devices hindering students’ effective participation in online teaching.88,91 Disturbing instances of hackers invading virtual meetings and sharing explicit comments and images, while uncommon, were also reported. 81
Domain 3: Contributing Factors
Aside from a lack of consistent guidelines23,96 and effective assessment tools,97,98 breaches in netiquette include technical gaps, curriculum limitations, poor means of identifying and supporting poorly motivated students,90,99–101 students with mental health issues and behavioral problems,90,101–104 burnout,91,99,102 loneliness,101,105 cynicism, 102 arrogance and frustration, 101 distraction,62,101,106–108 lack of self-discipline, 107 stress and anxiety (Table 5).101,103,105,109–112
Possible contributing factors for reduced online professionalism and netiquette.

Technical lapses result from inadequate facilities,91,127 poor internet access,85–88 limited access to computers,17,85,87,117–120 restrictions in the number of private rooms and conducive online learning environments.85,88,90 Other sources of technical lapses include poor faculty training,85,87,101,105,123–125 skills management,88,117,121 and time limitations.17,129
Domain 4: Implications
While the short-term implications have focused on disrupted and ineffective learning,23,59,73,87,133–137 it is perhaps equally concerning that poor netiquette is also associated with poor tutor-learner relationships,48,62,75,94,95 reduced peer interactions17,95,138 and increased student isolation.95,105,139,140 These concerns platform a tendency toward reduced collegiality,76,139 poor faculty relations105,141 and ineffective guidance, assessment and support of learners.
Stage 5 of SEBA: Analysis of Evidence-Based and Non-data Driven Literature
Almost half the included articles were data-driven while the remaining articles were non-data driven. A unique aspect of the SEBA is that it allows the inclusion of articles such as position, perspective, conference, reflective and opinion papers, editorials, commentaries, letters, posters, oral presentations, forum discussions, interviews, blogs, governmental reports, policy statements and surveys. Two considerations emerged from the analysis of these articles.
First, there were concerns that the non-data-based articles may have introduced bias to the analysis. Themes drawn from the data-driven publications were thus compared with those from non-data-based articles and the similarities between the 2 groups revealed no untoward biases.
Second, there were also questions over the quality of the included articles. While MERSQI and COREQ quality appraisals were carried out, deeper consideration of the data-driven articles were called for. Some articles only discussed the notion of netiquette in passing.12,55–57,59,61,62,70,76,79,80,85,86,90,96–98,100,101,108–110,118,120,121,124–127,134–137
Out of the articles that touched on netiquette, 22 articles discussed netiquette and 6 articles evaluated the issue of lapses in netiquette.
Discussion
Stage 6 of SEBA: Synthesis of Discussion
The “Best Evidence Medical Education (BEME) Collaboration Guide” 142 and the “Structured approach to the Reporting In healthcare education of Evidence Synthesis (STORIES)” 143 were used to guide the discussion.
In addressing its primary research question on “
To this end, we outline a set of recommendations for addressing online professionalism in Table 6.
Baseline expectations for online professionalism and netiquette.

Limitations
Netiquette in medical education is a relatively under-reviewed and novel area in literature which may account for the limited papers considered in this article. Furthermore, our specific focus on the presence of netiquette guidelines available online may have precluded the inclusion of guidelines that are only made available on university intranet systems, accessible to students and faculty.
Due to time, manpower and resource constraints, the exclusion of other health professional literature may have also led to the omission of key ideas potentially transferable to the field of medical education in medical schools. This is especially important, given that there may be a common set of guidelines that involve all healthcare professionals.
Including articles in or translated into English may have also restricted search results. As most of the data was drawn from North America and the Europe, they may not necessarily be transferable beyond these regions. While we advance a general expert opinion-guided set of guidelines, more context-specific adaptations may be needed to account for local healthcare, education, and sociocultural considerations.
Conclusion
This SSR in SEBA highlights the complex, variable, and multifactorial factors that impact current online professionalism and netiquette guidelines.
In our tabulated recommendations for Online Professionalism and Netiquette (Table 6), we have addressed not only the lack of standardized guidelines or assessment tools, but factors which are determined by sociocultural considerations, such as teaching approaches and support for students. Having said that, this framework will require further adaptation to local social and cultural settings, program nature and goals, student profiles and characteristics, as well as infrastructural considerations, for it to be effective. There is scope to pilot this framework and appraise its intervention for further improvement.
Supplemental Material
sj-docx-1-mde-10.1177_23821205241255268 - Supplemental material for Enhancing Professionalism Online (Netiquette) in Medical Schools: A Systematic Scoping Review
Supplemental material, sj-docx-1-mde-10.1177_23821205241255268 for Enhancing Professionalism Online (Netiquette) in Medical Schools: A Systematic Scoping Review by Donovan Kai Wei Ng, Jonathan Zhen Liang, Ruth Si Man Wong, Vijayprasanth Raveendran, Gillian Li Gek Phua, Warren Fong, Crystal Lim, Jamie Xuelian Zhou and Lalit Kumar Radha Krishna in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-2-mde-10.1177_23821205241255268 - Supplemental material for Enhancing Professionalism Online (Netiquette) in Medical Schools: A Systematic Scoping Review
Supplemental material, sj-docx-2-mde-10.1177_23821205241255268 for Enhancing Professionalism Online (Netiquette) in Medical Schools: A Systematic Scoping Review by Donovan Kai Wei Ng, Jonathan Zhen Liang, Ruth Si Man Wong, Vijayprasanth Raveendran, Gillian Li Gek Phua, Warren Fong, Crystal Lim, Jamie Xuelian Zhou and Lalit Kumar Radha Krishna in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-3-mde-10.1177_23821205241255268 - Supplemental material for Enhancing Professionalism Online (Netiquette) in Medical Schools: A Systematic Scoping Review
Supplemental material, sj-docx-3-mde-10.1177_23821205241255268 for Enhancing Professionalism Online (Netiquette) in Medical Schools: A Systematic Scoping Review by Donovan Kai Wei Ng, Jonathan Zhen Liang, Ruth Si Man Wong, Vijayprasanth Raveendran, Gillian Li Gek Phua, Warren Fong, Crystal Lim, Jamie Xuelian Zhou and Lalit Kumar Radha Krishna in Journal of Medical Education and Curricular Development
Footnotes
Acknowledgments
The authors would like to dedicate this article to the late Dr S Radha Krishna and A/Prof Cynthia Goh whose advice and ideas were integral to the success of this review and Thondy, Maia Olivia and Raja Kamarul whose lives continue to inspire us. The authors would like to extend their gratitude to the anonymous reviewers, Ms. Annelissa Mien Chew Chin, Dr Ruaraidh Hill, and Dr Stephen Mason for their help comments which enhanced this manuscript. The authors would also like to thank Miss Nur Diana Abdul Rahman and Miss Alexia Lee at the Division of Cancer Education, from National Cancer Centre Singapore, for their contributions.
Authors’ Contributions
DKWN, JZL, RSMW and VR were involved in the conceptualization, methodology, and writing of the initial draft. GLGP, WF, CL, JX, and LKRK were involved in the conceptualization, methodology, data curation, investigation, formal analysis, supervision, funding acquisition, visualization, writing of the initial draft, reviewing, and editing.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
