Abstract
Introduction:
Shadowing a physician is an observational experience which includes a student observing a licensed healthcare provider caring for patients. Shadowing is commonly done by students before and during medical school, but little is known about the nature or extent of these extra-curricular observational experiences.
Objective:
We hypothesized that shadowing experiences were common yet variable. We investigated the prevalence, nature, and perceived value of medical student experiences with shadowing physicians (both before and during medical school).
Methods:
This survey-based study was non-experimental with a cross-sectional convenience sample of osteopathic medical students about their shadowing experiences before and during medical school. The survey was sent to all matriculated osteopathic medical students (OMS1-4) for the 2017 to 2018 academic year from two medical schools: Philadelphia College of Osteopathic Medicine (PCOM) (1084 total students) and PCOM-Georgia (554 total students). The final survey instrument included three sections: demographics (6 questions), pre-medical shadowing experiences (21 questions), and medical student shadowing experiences (24 questions).
Results:
Respondents (357) identified themselves as OMS1 (96), OMS2 (89), OMS3 (73), OMS4 (95) and other (2, OMS5) with enrollment at PCOM-Philadelphia (242) and PCOM-Georgia (115). Among survey respondents, 339 (95.5%) reported shadowing a physician as a pre-medical student, and 110 (30.8%) reported shadowing (outside of their required clinical rotations) a physician during medical school. Requirements to participate were inconsistent; fewer than 50% of shadowing experiences required Health Insurance Portability and Accountability Act of 1996 (HIPAA) training, proof of vaccination, or purified protein derivative (PPD) documentation. In addition to observation, pre-medical and medical students, respectively, participated in history taking (44 [13%], 47 [42.7%]), physical examinations (45 [13.3%], 44 [40%]) and procedures (13, [3.8%], 20 [18.2%]) during their shadowing experiences. Motivations to participate in shadowing varied between pre-medical and medical student experiences, but both groups mentioned their desire to learn more about a particular discipline, obtain letters of recommendation, and gain patient care experience. Students recommended both pre-medical (273 [80.5%]) and medical school (93 [84.5%]) shadowing to future students.
Conclusion:
Shadowing remains a common and important tool for students to learn about patient care, medicine and careers. The nature of each shadowing experience and participation requirements are quite variable. Measures to ensure patient safety, confidentiality, liability and supervision are inconsistently applied. Promoting guidelines, as well as codes of conduct, for shadowing could serve as a helpful resource for students, academic advisors and supervising clinicians.
Introduction
Shadowing a physician is an experience defined as observing a licensed healthcare provider caring for patients. 1 The goal is to offer an introduction into medicine, a glimpse into a specific medical specialty and the daily responsibilities it might include, as well as give the provider the opportunity to model professional behavior and exemplary care of patients. 1
Physician clinical shadowing is common for undergraduate students hoping to apply to medical school in an extremely competitive application process. 2 In a 2003 study that surveyed pre-medical students attending a small, liberal arts college, 80.20% of them had shadowed a physician on at least one occasion. 3 Why such a common practice among students applying to medical school? Shadowing has been encouraged by pre-medical advisors as a way to show genuine interest in the medical field, as well as to gain an awareness of the day-to-day duties of a clinician. 2 It is generally recommended that applicants applying to medical school shadow a clinician1,2,4 and obtain a letter of recommendation from a clinician. 5 A large number of premedical students apply to both MD and DO schools; 6 shadowing provides an opportunity to learn more about osteopathic medicine. Of the 39 osteopathic programs identified in the Osteopathic Medical College Information Book 2018 to 2019, 22 require letters of recommendation from a physician, one recommends a letter from a physician, and 16 do not specify. Of the 22 which require letters from a physician, three require letters from a DO, eight recommend letters from a DO, and three specifically require a shadowing experience with the specific DO who is writing the letter. 5 Shadowing experiences provide applicants with the opportunity to learn about the field of medicine and to obtain a letter of recommendation.
Shadowing is also common among students who have already matriculated into a medical school. Third year medical students report feeling inadequately prepared for the transition to rotations, and course directors acknowledge the start of the clinical education years is often difficult. 7 As an additional strategy to assist students in their transition to clinical education with real patients, medical schools have established mentoring and shadowing programs for medical students. 8 This opportunity to shadow in specialties of interest during the first 2 years was deemed particularly useful by the medical students. 8 In addition to clinical rotations and formally arranged observational experiences by the medical school, it is likely that medical students participate in independently arranged shadowing experiences without the school administration’s knowledge.
Most medical students seem incredibly familiar with shadowing, having had several instances throughout pre-medical and medical education where they were encouraged to participate in some form of physician observation. However, there appears to be a lack of data, especially within the osteopathic medical profession, regarding the prevalence, nature, requirements and motivations for participating in these shadowing experiences. We hypothesized students frequently participated in shadowing experiences before and during medical school, but wanted to better understand the prevalence, nature and perceived value of these shadowing experiences (both before and during medical school). Focusing our attention only on these extra-curricular observational experiences, we excluded all clinical rotations, philanthropic, paid, or research-based experiences. Through survey responses, we collected details regarding the shadowing experience (setting, discipline, required paperwork and pre-requisites, duties, and responsibilities), required clinical or procedural skills, and perceived value in terms of career guidance or professional preparedness.
Methods
This survey-based study was nonexperimental with a cross-sectional convenience sample of first, second, third and fourth year osteopathic medical students that asked about their shadowing experiences before and during medical school. The institutional review board for the Philadelphia College of Osteopathic Medicine (PCOM) approved this study.
Sample
Using PCOM’s email database, an email invitation to participate was sent to all current matriculated osteopathic medical students (OMS) for the 2017 to 2018 academic year. The sample included first, second, third, and fourth year osteopathic medical students from two medical schools: PCOM (1084 total students) and Philadelphia College of Osteopathic Medicine Georgia Campus (PCOM-Georgia, 554 total students). The survey link was emailed and available to students between April 9 and May 8, 2018. The initial invitation to participate was followed by two emailed reminders.
Survey development
After reviewing shadowing programs’ characteristics and outcomes reported by other investigators, 9 survey questions were developed by two investigators (one physician and one fourth year medical student), and revised after soliciting input from three physicians familiar with shadowing and undergraduate medical education. Questions were then uploaded and formatted to SurveyMonkey. After testing by three medical students, two physicians and one administrator, survey formatting and grammar enhancements were applied. The final survey instrument included three sections: demographics (6 questions), pre-medical shadowing experiences (21 questions), and medical student shadowing experiences (24 questions). Questions regarding shadowing experiences addressed setting, discipline, required paperwork and pre-requisites, duties, responsibilities, and perceived value. Students were also provided the opportunity to share any other comments (open-ended response) regarding their shadowing experience before and/or during medical school. Survey participants were instructed to answer questions limiting their shadowing experiences to extra-curricular observational experiences only, excluding all clinical rotations, philanthropic, paid, or research-based experiences.
Analysis
Data (descriptive statistics) from the survey were extracted from Survey Monkey using Microsoft Excel 2016. Responses to open-ended questions were first reviewed by one investigator who identified themes for responses for each of the questions. Responses and themes were reviewed and verified by a second investigator. Responses were then categorized into different themes by one investigator, reviewed, and verified by the second investigator. The statistical analysis was performed using Microsoft Excel 2016 and Statistical Package for Social Sciences (SPSS). Descriptive statistics were initially computed and consisted of percentages and frequencies for two independent groups of shadowing before medical school and shadowing during medical school. Following the descriptive data, χ2 tests were used to evaluate specific hypotheses in regard to differences between categorical groups. Both the goodness of fit and test of independence were utilized depending on the number of categorical variables being examined. The two groups (before medical school and during medical school) were considered independent of one another. A significance value of α = .05 was accepted.
Results
The survey was completed by 357 students: 242 enrolled students from PCOM (22.3% response of 1084) and 115 students from PCOM-Georgia (20.8% response of 554). Respondents identified themselves as OMS1 (98, 27.5%), OMS2 (89, 24.9%), OMS3 (73, 20.5%), OMS4 (95, 26.6%) and OMS5 (2, 0.6%). Medical students identified themselves as female (224, 62.8%), male (133, 37.3%), age 22 to 24 (82, 23.0%), age 25 to 27 (172, 48.2%), 28 to 30 (72, 20.2%), 31 to 35 (23, 6.4%), older than 36 (7, 2.0%), Caucasian (223, 64.8%), Asian (57, 16.6%), African American/Black (18, 5.2%), Hispanic/Latino (9, 2.6%), Indian (10, 2.9%), and Other/Mixed (28, 8.1%). When asked to account for their time between undergraduate training and medical school, responding students reported, “I took no time off between undergraduate and medical school” (76, 14.3%), “I worked (odd jobs or temporary employment)” (143, 27.0%), “I worked (previous career)” (85, 16.0%), “I traveled” (38, 7.2%), “I completed additional course work (graduate or post-baccalaureate studies)” (161, 30.4%) and “other” (27, 7.6%). “Other” responses included spending time with family, military, research, and volunteer experiences.
Responses regarding logistics and details of shadowing experiences before and during medical school are presented in Table 1. Students reported they spent time shadowing clinicians before (339, 95.5%) and during (110, 30.8%) medical school. Of those who reported shadowing a DO before medical school (204, 60.2%), the following were identified as reasons for doing so (open-ended responses): curiosity about osteopathic medicine (58, 28.4%), application requirement (56, 27.5%), convenience/familiarity (38, 18.6%), and exploration of differences between MDs and DOs (26, 12.7%). Of those students who shadowed a DO during medical school (62, 56.4%), the following reasons were cited: convenience/familiarity (10, 16.1%), desire to learn how DOs practice medicine (7, 11.3%), coincidence (6, 9.7%), networking (5, 8.1%), desire to differentiate MDs from DOs (3, 4.8%), and program requirement (1, 1.6%).
Logistics: shadowing experiences before and during medical school, response summary (n = 357).

HIPAA: Health Insurance Portability and Accountability Act of 1996; BLS: Basic Life Support; CPR: cardiopulmonary resuscitation; PPD: purified protein derivative.
(1) not all survey respondents answered all questions, (2) many questions allowed multiple responses to each question, (3) responses to free text questions were categorized into one or more themes; therefore, responses to each question, by percent, do not add to 100%.
Percentages in column “Before medical school” are based on those who reported participating in shadowing experiences before medical school (n = 339).
Percentages in column “During medical school” are based on those who reported participating in shadowing experiences during medical school and outside of their required clinical rotations (n = 110).
P <.05. Chi-square tests for independence were performed between groups for each response.
Of those who reported shadowing experiences before medical school included history taking (44, 13.0%), specific elements cited elements included history of present illness (18, 40.9%), chief complaint (4, 9.1%), complete history (4, 9.1%), and miscellaneous conversation (2, 4.5%). Of those who reported history taking to be a part of their medical student shadowing experiences (47, 42.7%), specific elements included complete history (14, 29.8%), miscellaneous conversation (3, 6.4%), and chief complaint (2, 4.3%).
Of those who reported physical examination was involved with their shadowing experience before medical school (45, 13.3%), elements included pulmonary exam (15, 33.3%), cardiac exam (14, 31.1%), verification of abnormal findings (9, 20.0%), vital exam (9, 20.0%), complete physical exam (5, 11.1%), ENT exam (3, 6.7%), musculoskeletal exam (2, 4.4%), abdominal exam (1, 2.2%), and visual exam (1, 2.2%). Of those who reported physical examination was also part of shadowing experiences during medical school (44, 40.0%), specific elements included complete physical exam (8, 18.2%), musculoskeletal exam (8, 18.2%), partial physical exam (4, 9.1%), and pathology exam (2, 4.5%).
Of those reporting performing or assisting with procedures (13, 3.8%) during their shadowing experience before medical school, specific procedures included suturing (4, 30.8%), injections (3, 23.1%), phlebotomy (3, 23.1%), incision and drainage (2, 15.4%), nerve conduction testing (1, 7.7%), ear irrigation (1, 7.7%), and lumbar puncture (1, 7.7%). Of those reporting shadowing experiences during medical school included performing or assisting with procedures (20, 18.2%), specific procedures included various surgical procedures (4, 20.0%), emergency room (ER) procedures (4, 20.0%), injections (3, 15.5%), phlebotomy (3, 15.5%), osteopathic manipulative treatment (2, 10.0%), chest tube placement (1, 5.0%), and autopsy (1, 5.0%).
Among reasons cited for wanting to shadow a clinician before medical school (Table 2), “to learn more about medicine in general” (108, 37.5%), “to learn more about a specific medical specialty/discipline” (47, 16.3%), and “to enhance medical school application” (41, 14.2%) were identified as the most important.
Reasons identified as the most important reason for wanting to shadow a clinician before medical school (premedical shadowing).
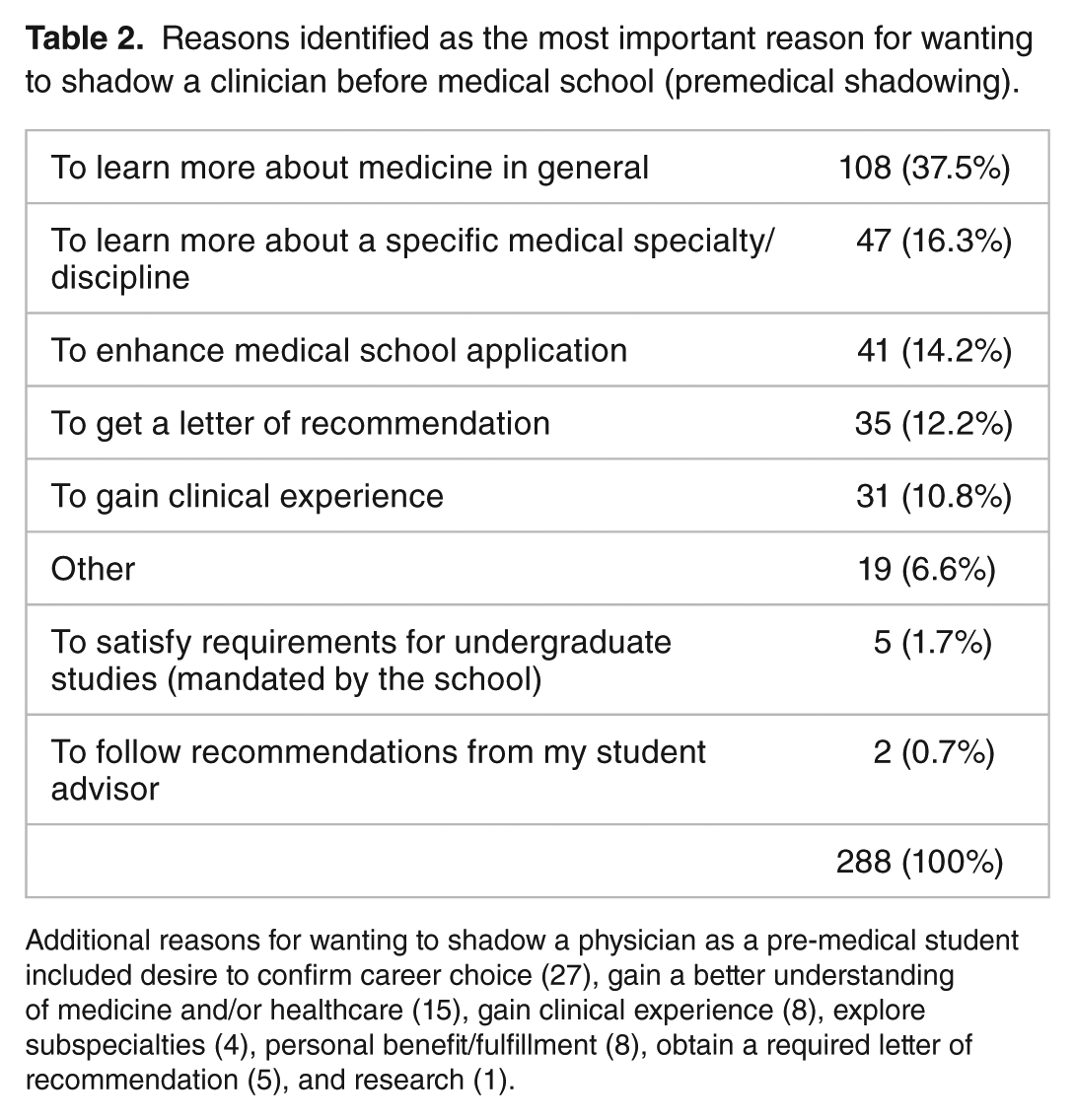
Additional reasons for wanting to shadow a physician as a pre-medical student included desire to confirm career choice (27), gain a better understanding of medicine and/or healthcare (15), gain clinical experience (8), explore subspecialties (4), personal benefit/fulfillment (8), obtain a required letter of recommendation (5), and research (1).
Among reasons identified for wanting to shadow a clinician during medical school (Table 3), “to learn more about a specific medical specialty/discipline” (56, 56.5%), “to learn more about medicine in general” (13, 13.1%), and “to gain clinical experience” (9, 9.1%) were reported as the most important.
Reasons identified as the most important reason for wanting to shadow a clinician during medical school (medical school shadowing).
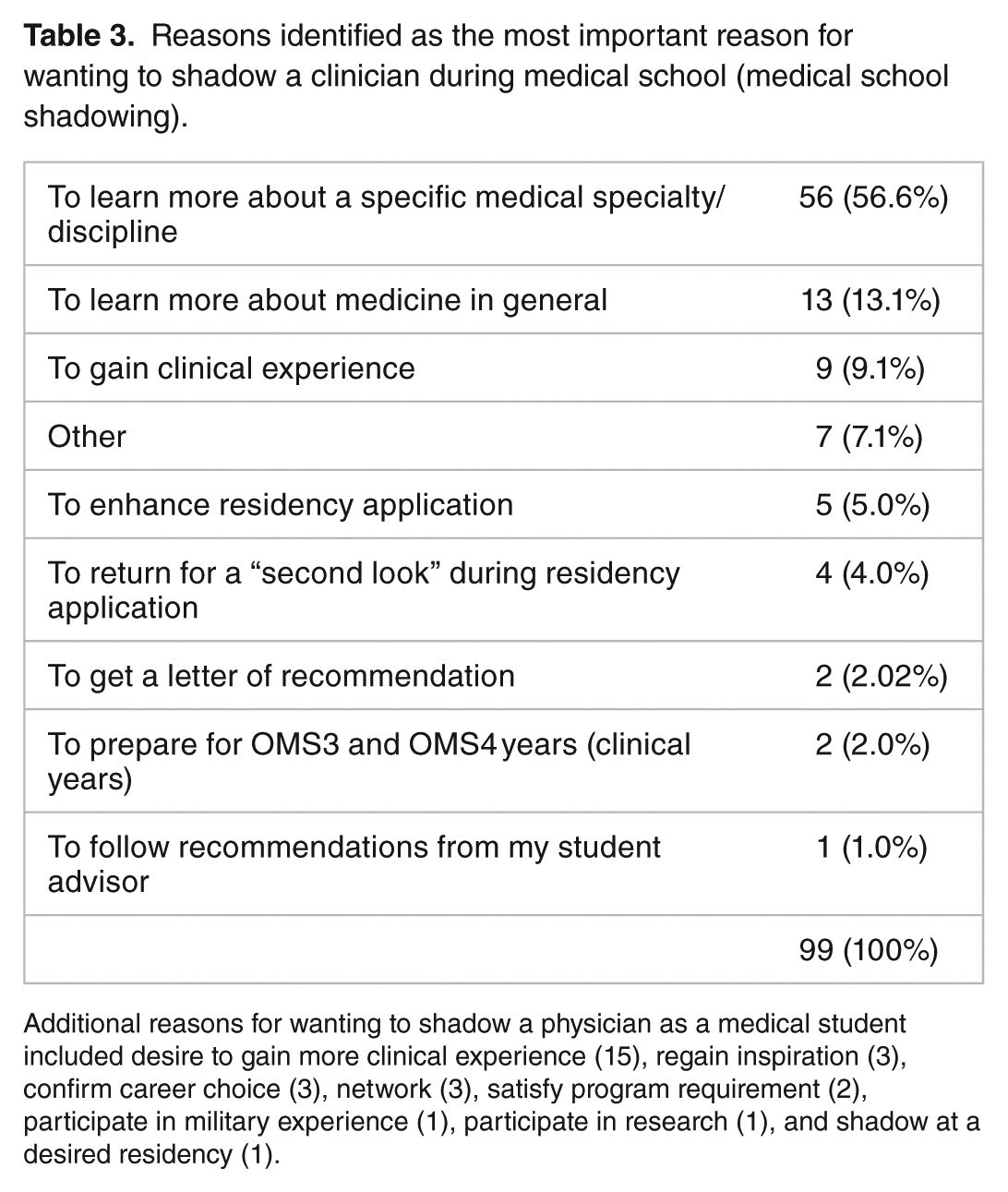
Additional reasons for wanting to shadow a physician as a medical student included desire to gain more clinical experience (15), regain inspiration (3), confirm career choice (3), network (3), satisfy program requirement (2), participate in military experience (1), participate in research (1), and shadow at a desired residency (1).
Shadowing experiences before medical school increased desire to attend medical school (242, 71.4%), while experiences during medical school increased desire to become a physician (78, 70.9%). Students reported frustrations, such as those included in Table 4 (eg, difficulty finding shadowing opportunities, limited exposure with patients, etc) regarding shadowing experiences before and during medical school. However, students overwhelmingly recommended shadowing before (273, 80.5%) and during (93, 84.5%) medical school for future students.
Motivation and outcomes: shadowing experiences before and during medical school, response summary (n = 357).

(1) Not all survey respondents answered all questions, (2) many questions allowed multiple responses to each question, and (3) responses to free text questions were categorized into one or more themes; therefore, responses to each question, by percent, do not add to 100%.
Percentages in column “Before medical school” are based on those who reported participating in shadowing experiences before medical school (n = 339).
Percentages in column “During medical school” are based on those who reported participating in shadowing experiences during medical school and outside of their required clinical rotations (n = 110).
P <0.05. Chi-square tests for independence were performed between groups for each response.
Discussion
We found shadowing before and during medical school to be common. Like other investigators, 9 we were surprised by the general lack of research and literature regarding shadowing experiences. The majority of students in this study chose to shadow a clinician prior to medical school in order to learn more about medicine in general, and many specifically chose to shadow a DO. Students chose to shadow a DO to better understand osteopathic philosophy, gain insight into the daily practices of a DO, and compare MDs and DOs. The shadowing opportunity provided them with the insight required to make an application decision and likely contributed to their decision to pursue an osteopathic medical education. Consistent with published application resources for osteopathic medical schools, 5 pre-medical students also chose to shadow a DO physician to obtain suggested letters of recommendation or to satisfy osteopathic medical school application requirements. A small number of students reported challenges with meeting this requirement, reporting that they had difficulty finding DO physicians to shadow. The requirement to shadow and obtain a letter from a DO physician is a well-intended mechanism to expose pre-medical students to osteopathic medicine, but the requirement may be a barrier to some students who are unable to find shadowing experiences before medical school.
In terms of primary responsibilities, the majority of pre-medical students reported that their shadowing was purely observational. The remaining stated that they were involved in history taking, performing vitals and physical exam, scribing the visit note, assisting with surgeries or procedures, or performing other tasks. Given the nature of some of the reported responsibilities (suturing, assisting with Cesarean Sections, performing a lumbar puncture, incision/drainage, chest tube placement), it is unclear if pre-medical students fully performed the procedures, assisted in them, or simply observed. Survey respondents likely over-stated their involvement in these procedures, but further study would be of interest. A majority reported shadowing increased their desire to attend medical school, and most recommended shadowing for future pre-medical students.
Shadowing was also common among medical students. Unrelated to structured rotations or clinical exercises, medical students were motivated to shadow a clinician by their desire to learn more about a specific medical specialty/discipline, reporting that medical school clerkships often do not offer enough time to fully experience a specialty. Through open-ended responses throughout the survey, students also reported a desire to explore additional subspecialties not necessarily seen during mandatory rotations. Most shadowing experiences during medical school occurred during the first and second years of training. Medical students found these extracurricular shadowing opportunities through student club contacts, personal connections and networking. Medical school administrators likely do not know the extent or nature of these independently arranged extracurricular shadowing experiences. Medical students seemed very satisfied with their shadowing experiences, reporting that shadowing experiences outside of required rotations greatly enhanced their desire to become a physician. Many believed that their medical school should have had a larger role in facilitating shadowing opportunities, identifying mentors, and integrating the osteopathic philosophy of hands-on care. Students expressed desire for a database of accessible physicians that would help them explore areas of clinical interest. The vast majority (84.5%) of students recommended shadowing to future students during medical school, but many of the comments suggested shadowing should not be required, citing concerns with time management and studying demands.
Most would agree caring for patients is an honor, and students, before and during medical school, must comply with standards to ensure patient dignity, confidentiality, and safety. However, fewer than 50% of shadowing experiences required Health Insurance Portability and Accountability Act of 1996 (HIPAA) training, proof of vaccination, or PPD documentation. Shadowing pre-requisites were notably inconsistent. Previous investigators have called for the development of protocols, guidelines and codes of conduct for shadowing, 9 and the American Association of Medical Colleges (AAMC) published “Guidelines for Clinical Shadowing Experiences for Pre-Medical Students” in 2016. 1 This AAMC publication emphasizes the observational nature of shadowing. If patient care is provided (including taking a history, conducting a physical exam, or performing procedures), then it is not considered shadowing. We discovered a large number of shadowing experiences, particularly during medical school that had included history taking, physical examination and procedures. By definition, these experiences would not be considered shadowing. Questions regarding consent, confidentiality, safety and liability should be considered. There is clearly great reward for the clinicians and students with regard to shadowing, but do these clinicians follow recommended guidelines or protocols for shadowing? This would be of interest in future study. Based on the results of this study (as reported by students), protocols and guidelines are not consistently applied, and opportunities to improve consistency exist.
This study had a few limitations with opportunities for further research. First, the study was limited to matriculated students at two osteopathic training institutions, and findings may not be generalizable. A national survey of all medical school trainees would be of interest. Second, the survey response rate, although high for a volunteer survey of this nature, did not include the entire student body. Third, differences between groups (ethnicity, for instance) were not investigated. In a larger, more comprehensive study, exploring differences in shadowing experiences between groups would be of interest. Fourth, students were asked to report details of shadowing experiences before starting medical school; this recall bias likely confounded response accuracy. Fifth, the study excluded research and paid positions; these experiences, while not considered observational or shadowing in nature, undoubtedly influence a pre-medical student’s perspective regarding health careers, specific healthcare disciplines and patient care. For instance, medical school applicants often become scribes to learn about healthcare professions, gain clinical experience, and increase chances of matriculation at medical school. 10 Further study of all volunteer, paid, scribe, research and observational experiences would be of interest. Sixth, given the non-observational nature of many of the activities reported by students, further exploration of the extent to which they assisted in these procedures would be of interest. Did the student observe, assist, or perform arthrocentesis, for instance? Did the student exaggerate his or her participation in this procedure? Seventh, the survey was lengthy and lacked redundant questions to evaluate internal consistency of responses. Eighth, we did not conduct interviews or focus groups with study participants, relying instead only on their multiple choice and open-ended answers. Further information would be helpful in better understanding the nature and timing of some of the reported experiences, as well as the motivations to participate in shadowing.
Conclusion
Shadowing is a common strategy to introduce potential medical students to healthcare and to expose medical students to different disciplines and experiences. Although shadowing is traditionally considered limited to observation, pre-medical and medical students are often taking histories, conducting physical exams, and performing or assisting with procedures. Measures to ensure patient safety, confidentiality, liability, and supervision are inconsistently applied for many shadowing experiences. Shadowing is valuable, but students often shadow without clearly defined expectations, direction, and procedures. Establishing safe standards and procedures for shadowing could involve many stakeholders: undergraduate institutions (pre-medical colleges), undergraduate and graduate medical education programs, student organizations, accrediting agencies, patient safety organizations, and clinicians who provide these important shadowing experiences. Reviewing, expanding and increasing promotion of existing guidelines, 1 as well as codes of conduct, for shadowing could serve as a helpful resource for students, academic advisors, and supervising clinicians.
Footnotes
Acknowledgements
We wish to thank the 357 students who participated in this study and provided thoughtful responses to the survey. We also wish to thank all clinicians who take time to provide invaluable shadowing opportunities to pre-medical and medical students.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
EL and SJC provide substantial contributions to the conception and design, subject recruitment, and acquisition of data. EL, SBF, and MBR provided substantial contributions to the analysis and interpretation of data. EL, SJC, and SBF drafted the article, reviewed content critically for important intellectual content. EL, SJC, and SBF addressed reviewer comments, conducted further analysis of data, provided substantial edits to the revised manuscript, and reviewed content critically for important intellectual content. EL gave final approval of the version of the article to be published. EL, SJC, SBF, and MBR agree to be accountable for all aspects of the work ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
