Abstract
Objective:
The aim of this study is to develop a simulation model for the Le Fort partial colpocleisis.
Introduction:
One in 9 women will undergo surgery for incontinence or prolapse by age 80 with 30% of these requiring an additional prolapse surgery. With a success rate of over 90% and recurrence rate of 4.2%, obliterative procedures hold a significant place in the management of pelvic organ prolapse in elderly women who are no longer sexually active. For new trainees, the Le Fort colpocleisis may be difficult to conceptually visualize, requiring the need to develop models as teaching tools.
Method:
A low-cost model was developed using easily available craft supplies to simulate the Le Fort partial colpocleisis with the uterus in situ to treat procidentia. The cost of each model was under US $14 and time to make was approximately 1 hour. The video presents the construction and use of this model.
Conclusions:
The Le Fort partial colpocleisis technique has been in use for over a century. The aging population as well as the high risk of recurrence after prolapse repairs makes colpocleisis an important technique for trainees to master. Simulation models have proven their efficacy as a training tool. This simple model will allow trainees to fully comprehend the steps of this procedure. Using this video, educators can construct a model and use it to orient trainees to the Le Fort partial colpocleisis procedure.
Introduction
As health care advances improve longevity, more women are entering the eighth and ninth decades of their life. It has been reported that 1 in 9 women will undergo surgery for incontinence or prolapse by age 80. 1 Long-term recurrence rates from conventional reconstructive surgeries can be as high as 50% with a reoperation rate for failures as high as 30%.1,2
First described by Gerardin in 1823, obliterative vaginal surgeries have long been used in the management of pelvic organ prolapse in elderly women who are no longer sexually active. It was not until 1877 that Leon Le Fort performed and published the technique for the procedure now known as Le Fort partial colpocleisis. This involves denudement of rectangles in the anterior and posterior vaginal walls which are then sutured together leaving lateral channels for drainage of cervical secretions. 1 The surgery is performed leaving the uterus in place and is an excellent option for elderly patients with multiple medical issues who do not desire vaginal functionality and are not candidates for extensive reconstructive surgery. It can also be an option for recurrent pelvic organ prolapse in patients who are no longer sexually active. Typical success rates vary between 91% and 100% 3 and a recent review found recurrence rates as low as 4.2% with only 2% to 3% of patients requiring reoperation. 2
Although the procedure has been described extensively in text, new trainees may have a hard time comprehending the steps of the procedure through reading materials alone. Two-dimensional pictures are unable to capture the orientation of the prolapsed vagina which can be disorienting for the uninitiated. Previous models have described the technique for Le Fort as well as total colpectomy.4,5 Although these models adequately describe the technique, they do not describe the proximal and distal aspects of the vagina in relation to the uterus or test for patency of vaginal tunnels. The video available below the making and use of a novel, low-cost simulation model to act as a learning aid for surgeons new to the technique of Le Fort partial colpocleisis.
Materials and Methods
To make our model, we purchased easily available craft supplies. This includes pink and magenta felt, an embroidery hoop, fusible bonding web (such as Stitch Witchery), as well as hook-and-loop fasteners. We used Black and White Velcro Sticky coins (4 pairs each) as well as Velcro sticky back tape. The cost of each model was under US $14 and time to make was approximately 1 hour (Figure 1).
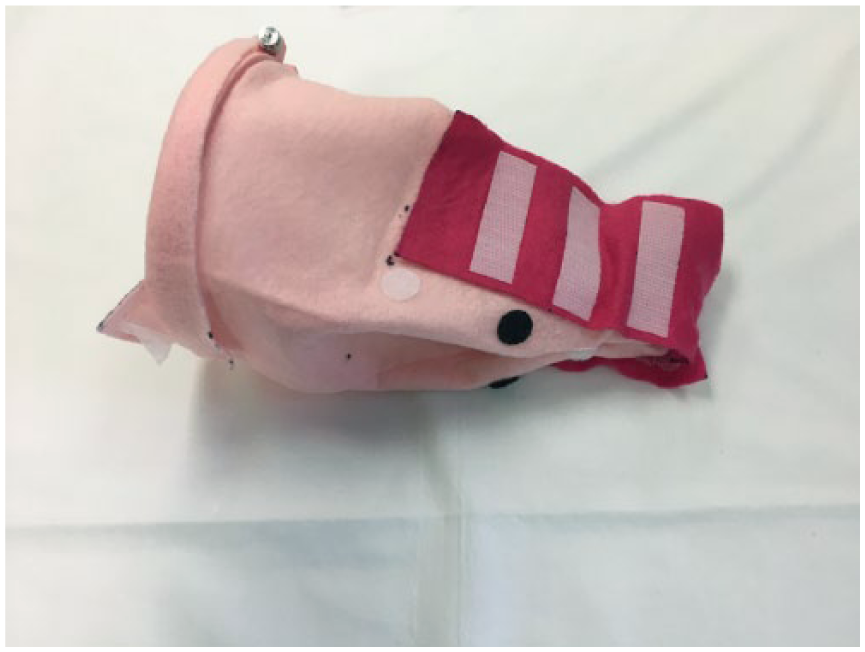
Completed simulation model.
Making the model
We began by cutting the pink felt into a rectangle measuring 46 cm × 39 cm.
Along the 46-cm edge, we marked out 6, 20, 26, and 40 cm and cut slits 5-cm long at each of these points.
We then cut the magenta felt into rectangles measuring 8 cm × 16 cm and affixed them on to the pink felt using Stitch Witchery and a hot iron.
We cut the Velcro tape into strips 7-cm long and attached them to the magenta felt at 3, 7, and 11 cm marks.
The Velcro sticky coins were attached to the pink felt along the magenta felt at 5 cm distances alternating the white and black coins.
The large pink felt was folded and the longitudinal edges were bound together using Stitch Witchery to create a cylinder. The slit ends of the pink felt were bound together to close one end of the cylinder.
Next, the embroidery hoop was attached to the open end of the cylinder.
We cut 2 additional rectangles out of the pink felt measuring 18 cm × 9 cm and used Velcro strips to adhere it to the magenta felt.
Finally, we sutured a bottle cap to the closed end of the pink felt cylinder.
Using the model
In our model, the embroidery hoop acts as the vaginal introitus with the cylindrical pink felt acting as prolapsed vagina and the bottle cap acting as a cervix. The steps of the surgery and the corresponding use of the model are as follows1,4:
Rectangular areas are marked and denuded off the anterior and posterior aspects of the vagina. In the model, the overlaying pink felt simulates vagina that is denuded to reveal the underlying magenta.
The cut edges of the vaginal walls are sown together with interrupted delayed absorbable suture. The sides of the rectangles create the vaginal tunnels. The sequential reapproximation of the Velcro strips acts as the interrupted sutures placed in the suturing of the anterior and posterior vaginal walls, whereas the Velcro coins step in for the creation of the vaginal tunnels.
In a sequential fashion, the model demonstrates creation of vaginal tunnels while simultaneously obliterating the vagina and reducing the vaginal prolapse.
At the end of the procedure, patency of the lateral tunnels is confirmed.
Conclusions
The Le Fort partial colpocleisis technique has been in use for over a century and is an important tool in the versatility of management of pelvic organ prolapse. The advantages of our simulation model include its low cost and the use of easily available materials. Although this model has currently not been validated, we believe that this simple model will allow trainees to fully comprehend the steps of this procedure and have used it for this purpose in our community-based training program. This model is especially useful for orientation of the prolapsed vagina and understanding the basic steps and principal of the partial colpocleisis. Using this video, educators can construct a model and use it to orient trainees to the Le Fort partial colpocleisis procedure.
Footnotes
Acknowledgements
The video was presented at the American Urogynecology Society Annual Meeting in Providence, Rhode Island, USA, on October 6, 2017.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
AG: Project development, Manuscript writing, Video recording & editing
SH: Manuscript editing, Video recording & editing
SK: Project development, Manuscript editing, Video recording and editing
LK: Project development, Manuscript editing, Video editing
Informed Consent
This study did not require any consent as this video did not involve any patients.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
