Abstract
Background and Objective
Mental health has emerged as a critical public health priority during the COVID-19 pandemic. The purpose of this review was to analyze and summarize existing literature on the effects of the COVID-19 pandemic on the mental health of the general population in Iraq.
Methods
The systematic reviews were conducted in accordance with the PRISMA 2020 guidelines. The review protocol was registered in PROSPERO with the unique identifier CRD42023423291. Searches were performed in PubMed, Scopus,Medline, and Google Scholar in May 2023 for studies published from January 2020 to January 2023. The researchers used the Joanna Briggs Institute to evaluate the quality of the studies. Data from all the included research in this review were collected and synthesized.
Results
This review included data from 11 high-quality studies conducted in Iraq, involving a total of 8,917 participants. Of these participants, 4,860 (54.5%) were female and 4,057 (45.5%) were male. The aim of these studies was to investigate the impact of COVID-19 on mental health. The systematic review yielded important findings regarding the prevalence rates of anxiety, stress, depression, and post-traumatic stress disorder (PTSD). These rates were estimated to be 54.89%, 48.15%, 49.57%, and 31.35% respectively. It is worth noting that various demographic groups in Iraq exhibited elevated levels of stress, anxiety, depression, and PTSD, highlighting the significant burden experienced by individuals. These findings emphasize the wide-ranging effects on different segments of the population, including college students and individuals with a history of COVID-19 infection.
Conclusion
This review highlights the substantial impact of COVID-19 on mental health in Iraq, noting increased levels of stress, anxiety, depression, and PTSD among various groups. The findings consistently showed a significant mental health burden on Iraqis, urging healthcare authorities and policymakers to implement targeted interventions to address these challenges promptly.
Introduction
The coronavirus (COVID-19) pandemic, caused by severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2), has had a significant global impact. In January 2020, the World Health Organization (WHO) declared COVID-19 a Public Health Emergency of international concern. Later, on March 11, 2020, it was officially designated as a pandemic (Cucinotta & Vanelli, 2020). The COVID-19 pandemic has profoundly impacted Iraq, a nation characterized by a prolonged history of political instability, economic hardship, and social unrest. Since gaining independence in 1921, Iraq and its citizens have faced recurring crises, including conflict, sanctions, and internal displacement, which have weakened the country's healthcare infrastructure and social resilience. These pre-existing vulnerabilities have amplified the multifaceted consequences of the pandemic, particularly its psychological toll. The pandemic has intensified mental health challenges in a population already burdened by prolonged exposure to trauma and adversity (Al Janabi & Chung, 2022).
During an infectious disease outbreak, the well-being of the population plays a crucial role in the spread of the disease and its impact on mental health and social interactions (Cullen et al., 2020; Xiang et al., 2020). Psychological factors influence individuals’ adherence to public health measures and their ability to cope with the stress and perceived risk of infection (Bakshi et al., 2021). Research has identified over 60 physical symptoms associated with COVID-19, including weakness, fatigue, impaired concentration, reduced lung function, and mental health issues such as depression, anxiety, post-traumatic stress disorder (PTSD), insomnia, distress, reduced quality of life, and cognitive impairments (Michelen et al., 2021; Sher, 2020).
Several studies have investigated the psychological impact of the COVID-19 pandemic (Alacevich et al., 2023; Daniali et al., 2023; Deng et al., 2021; Kunzler et al., 2021; Mahmud et al., 2023; Mud Shukri et al., 2023; Nochaiwong et al., 2021; Prati & Mancini, 2021; Salari et al., 2020; Santabárbara et al., 2021; Schou et al., 2021; Taha et al., 2023). Recent umbrella reviews and large-scale meta-analyses exploring the pandemic's impact reveal complex patterns in mental health outcomes across different phases, populations, and regions. One umbrella review noted a worsening of symptoms among individuals with eating disorders linked to the social restrictions imposed by COVID-19 (Vavassori & Donzelli, 2024). Another review, which included 72 meta-analyses, found that 37% of healthcare professionals reported experiencing stress, 31.8% reported anxiety, 29.4% reported depression, and 36.9% reported sleep disturbances during the pandemic (Maqbali et al., 2024). Additionally, the latest umbrella review reported an overall anxiety prevalence of 30.4%, with the highest rates observed among patients at 41.3%, followed by students at 30.8%, pregnant women at 30.6%, and healthcare workers at 30.5% (Amini-Rarani et al., 2024).
In a study by Chen et al. (2022), fatigue was identified as the primary symptom among individuals with post-COVID-19 complaints, followed by memory problems (Chen et al., 2022). Parlapani et al. (2020) examined a sample of 3,700 individuals from the general population in Greece and found that 35.7% of participants experienced high levels of fear related to COVID-19. In addition, 22.8% exhibited symptoms of depression ranging from moderate to severe, and 77.4% reported experiencing moderate to severe anxiety symptoms. Female participants scored higher than males on these measures, while respondents under the age of 30 reported lower levels of fear and depressive symptoms (Parlapani et al., 2020).
Researchers in Iraq have investigated the physiological and psychological consequences of the epidemic on individuals following the outbreak and subsequent implementation of quarantine measures. Their research has revealed that quarantine measures have had a significant impact on adverse mental health outcomes (Seidi et al., 2021). A quantitative study conducted in Sulaymaniyah examined a sample of 394 elderly individuals. The findings indicated that 20.01% and 19.0% of the participants reported experiencing moderate and severe levels of stress, respectively (Qadr & Ismail, 2023). The responses of inhabitants residing in different geographical areas varied in relation to the global health crisis. For example, individuals residing in southern Iraq displayed a higher prevalence of anxiety, with a recorded percentage of 59.13%. In comparison, residents of the northern and middle governorates exhibited anxiety levels of 45.05% and 43.75% respectively (Karim et al., 2020). The COVID-19 pandemic has had a significant impact on students, resulting in an increase in mental health concerns (Mohammed & Memmedova, 2023). A study conducted by Taher et al. (2021) focused on Iraqi medical students, excluding those from Kurdistan in northern Iraq (Taher et al., 2021). The findings revealed that 70.1% of the participants showed symptoms indicative of mental health issues. Specifically, 25.9% reported experiencing worry, while 23.7% reported experiencing stress. Additionally, 43.0% of the participants displayed potential symptoms of obsessive-compulsive disorder (OCD). Another study conducted in northern Iraq found that 31.6% of individuals who had recovered from COVID-19 fulfilled the criteria for PTSD, and 21.05% of these individuals were identified as having probable depression (Ibrahim et al., 2022).
The COVID-19 pandemic has presented significant challenges to the physical and mental well-being of people globally. Iraq, a country profoundly affected by the pandemic, faces its own unique circumstances due to pre-existing difficulties and the additional burden of COVID-19. During a pandemic, the detrimental impact on mental health often surpasses the number of individuals affected by the physical infection itself (Ornell et al., 2020). Iraq, still recovering from years of conflict and instability, has experienced various social, economic, and political stressors that have unquestionably influenced the mental health of its population (Saied et al., 2023a; Saied et al., 2023b; Saied et al., 2023c). The COVID-19 pandemic has significantly exacerbated pre-existing challenges, intensifying mental health issues and giving rise to new psychological burdens within populations worldwide. In Iraq, a country already grappling with prolonged political instability, economic hardships, and societal stressors, the pandemic has further compounded these difficulties, disproportionately affecting the mental well-being of its general population. Understanding the specific effects of COVID-19 on mental health in this unique socio-political context is crucial for informing public health interventions and policy decisions aimed at mitigating the psychological impact of the pandemic. Despite the global focus on mental health during the COVID-19 crisis, to the best of our knowledge, no comprehensive review has been conducted to evaluate the pandemic's effects on the mental health of Iraq's general population. Such an examination is vital for identifying prevalent mental health conditions, highlighting at-risk groups, and proposing evidence-based strategies to support and enhance the overall health and resilience of the Iraqi population. Therefore, this study seeks to systematically review and synthesize the existing literature to provide an in-depth understanding of the mental health consequences of COVID-19 on Iraq's general population.
Methods
Review Objectives
The main objective of this review was to comprehensively examine and analyze the current body of literature on the effects of the COVID-19 pandemic on the mental health of the general population in Iraq. This review aimed to explore the prevalence of mental health disorders, including anxiety, depression, PTSD, fear, and stress.
Protocol and Registration
The systematic reviews were conducted following the PRISMA 2020 guidelines (Supplemental File 1). The review protocol was registered in PROSPERO with the unique identifier CRD42023423291. The quality of the review was assessed using the AMSTAR-2 checklist, which received an excellent rating (Shea et al., 2017). Ethical approval was considered unnecessary for this review article.
Search Strategy
In May 2023, the researchers searched online databases, including PubMed, Scopus, and Google Scholar, to identify relevant studies. The search strategy employed relevant keywords: (“COVID-19” OR “coronavirus” OR “pandemic” OR “SARS-CoV-2”) AND (“mental health” OR “psychological health” OR “emotional health” OR “mental illness” OR “anxiety” OR “depression” OR “stress” OR “PTSD” OR “trauma”) AND (“Iraq” OR “Iraqi” OR “Kurdistan region”). In addition, the references of all pertinent papers were thoroughly reviewed to ensure a comprehensive search (Table 1).
Search Strategy Across Databases for Systematic Review (May 2023).

Eligibility Criteria
This paper reviews studies on COVID-19's impact on mental health in Iraq from January 2020 to January 2023. The review focuses on studies that report on mental health outcomes and contributing factors in the general population of Iraq. The inclusion criteria encompass various study designs, including observational studies, cross-sectional studies, and longitudinal studies.
Several criteria were applied in this systematic review to select relevant and reliable studies. Firstly, studies published in languages other than English were excluded. Secondly, studies that did not specifically examine the impact of the COVID-19 pandemic on mental health in Iraq were omitted. Thirdly, studies that did not report on mental health outcomes or contributing factors were excluded. Fourthly, studies with insufficient data or incomplete methodology were excluded. Lastly, to safeguard against potential bias and unreliable sources, studies published in predatory journals were also excluded.
Data Extraction and Selection Process
The data extraction process followed the PRISMA 2020 guidelines (Page et al., 2021). Two reviewers (first and second authors) independently assessed abstracts and full-text articles using the Rayyan website, based on predetermined inclusion and exclusion criteria. Any discrepancies were resolved through discussion. Data extraction was done using predefined forms in Microsoft Excel. Each study included in the analysis provided information on study design, sample size, gender, population characteristics, and mental health outcomes.
Critical Appraisal of the Included Studies
The researchers used the critical appraisal checklist for analytical cross-sectional and case control studies from the Joanna Briggs Institute (JBI) to assess the quality of the studies in this review. A set of eight questions was gathered to evaluate the quality of these studies. The checklist covered various areas of investigation, including sample inclusion criteria, characteristics of the study subjects, study context, use of valid and reliable measurement tools (with a focus on questionnaire validity and reliability), adoption of standardized measurement criteria, identification of confounding factors, implementation of strategies to address confounding factors, use of valid outcome measures, and appropriateness of the statistical analysis conducted. The responses to the questions were categorized as yes, no, unclear, or not applicable. Each response was assigned a binary value of 1 or 0, based on its alignment with the options yes, no, unclear, or not applicable. Every study included in the analysis received a quality score of 8, and only studies with a quality score below 5 were excluded.
Data Synthesis and Analysis
The data from all the articles included in this systematic review was extracted and aggregated. This included author names, year of publication, age, gender, type of mental health, prevalence of mental health disorders, and their associated outcomes. The researchers obtained this information from the findings of eligible studies and subsequently consolidated the results into a single table.
Results
Selection of Studies
The databases and search engines used (PubMed, Scopus, Medline, and Google Scholar) returned 555 articles on May 2, 2023. The references were organized and 58 duplicate articles were automatically removed using a citation manager tool (Mendeley). A final check was then conducted on 497 articles to ensure the accuracy of their titles, abstracts, and full texts. Of these, 422 articles were rejected for not meeting the requirements for inclusion. Additionally, 75 articles were submitted for retrieval, but 54 of them were rejected for not meeting the inclusion criteria. Ultimately, our systematic review included only 11 articles (Figure 1).
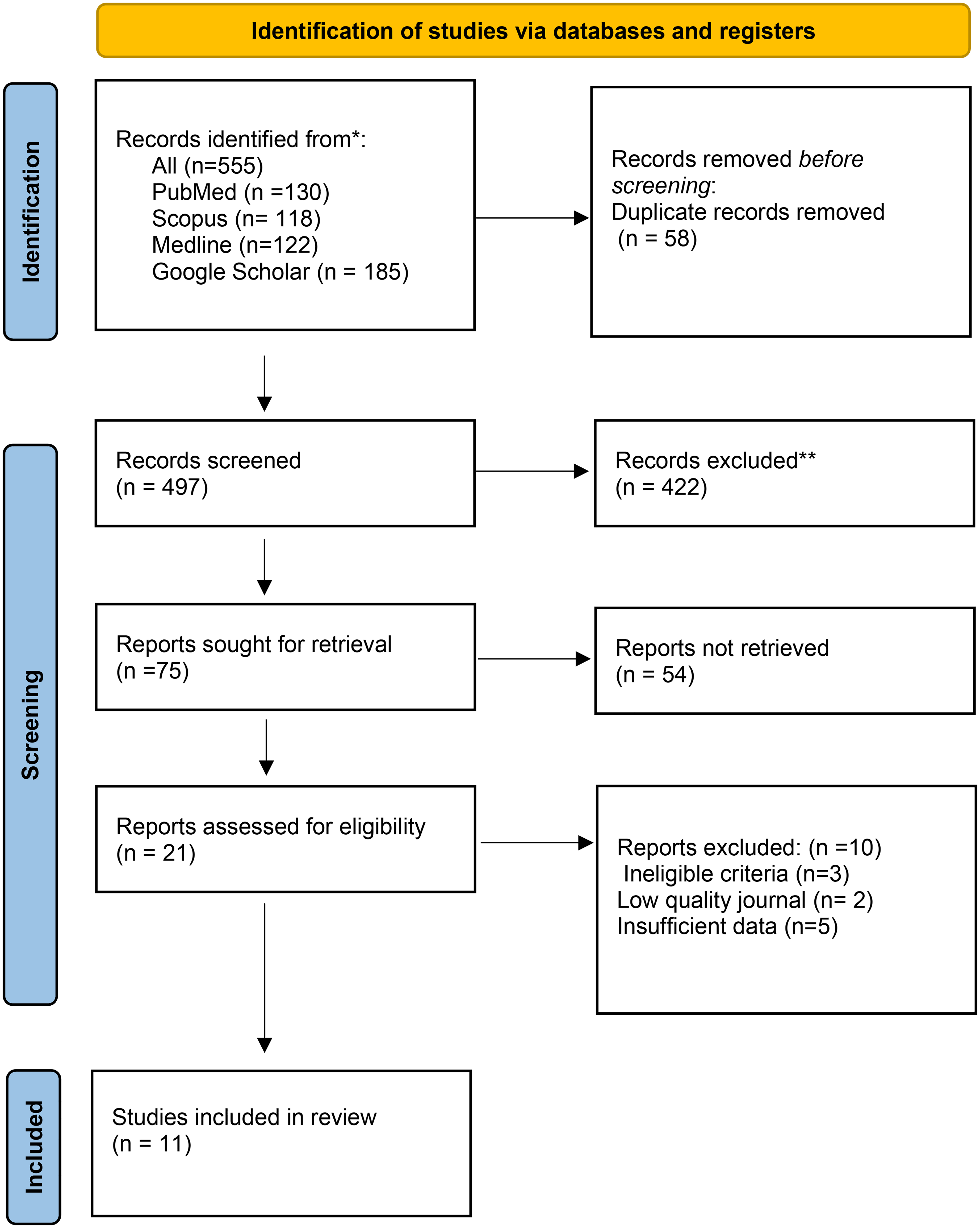
PRISMA flow diagram.
Methodological Critical Appraisal of the Included Studies
The results in Table 2 show no bias in the included studies. Only high-quality studies were included in the review.
The Quality Assessment Conducted on the Articles, Utilizing the JBI Critical Appraisal Checklist.

Note. JBI = Joanna Briggs Institute; Q = question; N = no; NA = not/applicable; U = unclear; Y = yes; Score = the quality assessment score was determined by assigning values ranging from 0 to 8 for each question on the JBI checklist. (Q1) Were the criteria for inclusion in the sample clearly defined? (Q2) Were the study subjects and the setting described in detail? (Q3) Was the exposure measured in a valid and reliable way? (Q4) Were objective, standard criteria used for measurement of the condition? (Q5) Were confounding factors identified? (Q6) Were strategies to deal with confounding factors stated? (Q7) Were the outcomes measured in a valid and reliable way? (Q8) Was appropriate statistical analysis used?
Characteristics of the Included Studies
Among the 11 studies examined, 10 focused on the general population. Two studies specifically targeted COVID-19 survivors (Ibrahim et al., 2022; Mohammad et al., 2023), while one study was conducted among university students (Mohammed & Memmedova, 2023). All articles used a cross-sectional design. Out of the 11 studies analyzed, six of them were published in 2023 (Lafta & Mawlood, 2023; Mohammed & Memmedova, 2023; Mohammad et al., 2023; Saeed et al., 2023; Taha, 2023; Taha et al., 2023), three were published in 2022 (Alrubai et al., 2022; Blbas et al., 2022; Ibrahim et al., 2022), one was published in 2021(Tahir et al., 2021), and one was published in 2020 (Kamal & Othman, 2020). The majority of the studies were published in international journals (Alrubai et al., 2022; Blbas et al., 2022; Ibrahim et al., 2022; Karim et al., 2020; Lafta & Mawlood, 2023; Mohammed & Memmedova, 2023; Mohammad et al., 2023; Saeed et al., 2023; Taha et al., 2023; Taha, 2023; Tahir et al., 2021). The total sample size of the studies included in the review was 8917 participants, with individual study sample sizes varying from 57 (Ibrahim et al., 2022) to 1578 Taha, 2023) participants. Of these participants, 4,860 (54.5%) were female and 4,057 (45.5%) were male. Table 3 provides a comprehensive overview of the study characteristics from all the included studies.
Characteristics of Participants in all Included Studies.
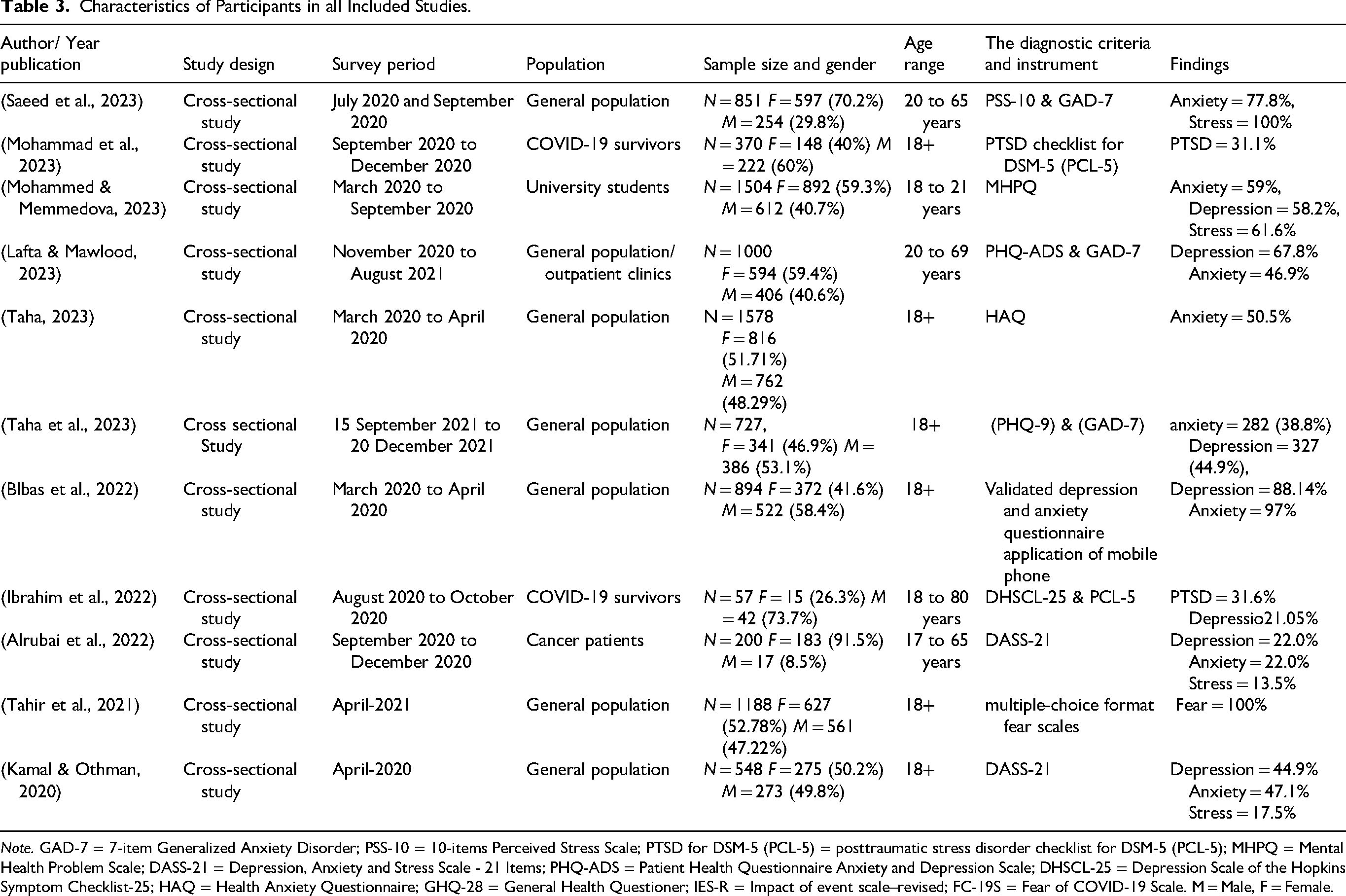
Note. GAD-7 = 7-item Generalized Anxiety Disorder; PSS-10 = 10-items Perceived Stress Scale; PTSD for DSM-5 (PCL-5) = posttraumatic stress disorder checklist for DSM-5 (PCL-5); MHPQ = Mental Health Problem Scale; DASS-21 = Depression, Anxiety and Stress Scale - 21 Items; PHQ-ADS = Patient Health Questionnaire Anxiety and Depression Scale; DHSCL-25 = Depression Scale of the Hopkins Symptom Checklist-25; HAQ = Health Anxiety Questionnaire; GHQ-28 = General Health Questioner; IES-R = Impact of event scale–revised; FC-19S = Fear of COVID-19 Scale. M = Male, F = Female.
Main Results
The present systematic review showed that the COVID-19 pandemic has had a significant negative impact on the mental well-being of the Iraqi population. The included studies evaluated various mental health consequences, including stress, anxiety, depression, PTSD, and other forms of psychological distress (Ibrahim et al., 2022; Mohammad et al., 2023; Mohammed & Memmedova, 2023; Saeed et al., 2023). The results of this systematic review indicate that the overall prevalence rates for anxiety, stress, depression, and PTSD were found to be 54.89%, 48.2%, 49.57%, and 31.35%, respectively (Figure 2).

The overall percentage psychological disorders based included studies. The overall percentage was calculated by combining the percentages reported in all included studies and then dividing by the number of studies.
COVID-19 and Depression
Depression rates were found to be significantly high in multiple studies, indicating a substantial burden of mental health issues across diverse demographic groups during the survey periods. In a study by Lafta and Mawlood (2023), a prevalence rate of 67.8% for depression was reported among 1000 participants from the general population and outpatient clinics (Lafta & Mawlood, 2023). The assessment was conducted using the PHQ-ADS. Furthermore, Mohammed and Memmedova (2023) conducted a cross-sectional study from March to September 2020 involving 1504 university students aged 18 to 21 years, with a majority of female participants (59.3%). Using the MHPQ, the researchers found that 58.2% of the students experienced depression (Mohammed & Memmedova, 2023). Additionally, Ibrahim et al. (2022) identified a prevalence rate of 21.05% for depression among 57 COVID-19 survivors (Ibrahim et al., 2022). The Depression and Anxiety Stress Scales (DHSCL-25) and the PTSD checklist for DSM-5 (PCL-5) were used for assessment. (Ibrahim et al., 2022). Kamal and Othman (2020) found a depression rate of 44.9% in the general population during the early months of the pandemic (Kamal & Othman, 2020). Taha et al. (2023) found that the general population post-COVID-19 infection experienced mild to moderate levels of depression (44.9%) (Taha et al., 2023).
COVID-19 and Anxiety
Anxiety disorders were found to be prevalent in various populations and settings in the reviewed studies, indicating a widespread mental health issue that has been exacerbated by recent global events such as the COVID-19 pandemic. In a cross-sectional study conducted by Saeed et al. (2023) between July and September 2020, 851 participants aged 20 to 65 years from the general population were included, with a majority being female (70.2%). Using the GAD-7 scale, they found a remarkably high prevalence of anxiety, reaching 77.8% (Saeed et al., 2023). Similarly, in a study conducted by Blbas et al. (2022) from March to April 2020, an exceptionally high prevalence of anxiety, reaching 97%, was reported among 894 participants who used a validated mobile phone application for anxiety assessment. This study included a higher proportion of male participants (58.4%), indicating that anxiety was prevalent among both genders (Blbas et al., 2022). Furthermore, Lafta and Mawlood (2023) identified significant anxiety levels (46.9%) among 1000 participants from the general population and outpatient clinics, using the GAD-7 tool (Lafta & Mawlood, 2023). Mohammed et al. (2023) found that a significant number of university students displayed symptoms of anxiety (Mohammed and Memmedova (2023). Taha et al. (2023) reported that the general population experienced mild to moderate anxiety levels (38.8%) after a COVID-19 infection (Taha et al., 2023).
COVID-19 and Stress
Stress levels were consistently high across different demographics in the surveyed studies, indicating the widespread impact of stress-inducing factors such as the COVID-19 pandemic and associated lockdowns. According to Saeed et al. (2023), all 851 participants from the general population reported experiencing stress as measured by the PSS-10 (Saeed et al., 2023). Mohammed and Memmedova (2023) found that 61.6% of the 1504 university students experienced stress (Mohammed & Memmedova, 2023). Kamal and Othman (2020) observed a stress prevalence of 17.5% in a study conducted in April 2020 with 548 participants from the general population, using the DASS-21 (Kamal & Othman, 2020).
COVID-19 and PTSD
PTSD was found to be highly prevalent among individuals who have survived COVID-19, highlighting the significant psychological impact of the ongoing pandemic. In a cross-sectional study conducted by Mohammad et al. (2023) between September and December 2020, a total of 370 COVID-19 survivors participated, with the majority of them being male (60%). By utilizing the PTSD checklist for DSM-5 (PCL-5), the researchers observed that 31.1% of the participants exhibited symptoms meeting the criteria for PTSD (Mohammad et al., 2023). Similarly, Ibrahim et al. (2022) reported a PTSD prevalence of 31.6% among 57 COVID-19 survivors (Ibrahim et al., 2022). This prevalence was determined through the use of the DHSCL-25 and the PCL-5.
COVID-19 and Fear
This review identified only one study addressing fear related to COVID-19, specifically focusing on the fear of COVID-19 vaccines. The authors categorized fear into three levels: low, medium, and high. The results showed that 408 participants (34.3%) reported low levels of fear, 674 participants (56.7%) reported medium levels, and 106 participants (8.9%) reported high levels. While all participants exhibited some degree of fear, the distribution across these categories highlights variability in the intensity of fear (Tahir et al., 2021).
Discussion
Magnitude of Mental Health Challenges
The results derived from the 11 included studies in this review provide insight into the psychological implications of the pandemic on the Iraqi population. These studies revealed considerable levels of stress, anxiety, depression, and PTSD (Ibrahim et al., 2022; Lafta & Mawlood, 2023; Mohammed & Memmedova, 2023; Qadr & Ismail, 2023; Saeed et al., 2023). It is worth noting that results of this systematic review indicate that the overall prevalence rates for anxiety, stress, depression, PTSD, and fear were found to be 54.89%, 48.15%, 49.57%, 31.35%, and 100%, respectively. The findings of this review align with global trends, demonstrating significant mental health impacts of the COVID-19 pandemic. For instance, global prevalence rates of anxiety and depression reported by Salari et al. (2020) were 31.9% and 33.7%, respectively, which are lower than those observed in Iraq (54.89% and 49.57%). Similar patterns have been observed in studies from Pakistan (Yasmin et al., 2022), reflecting comparable psychological distress in a region affected by socio-economic challenges. This disparity likely reflected Iraq's unique socio-political context, where ongoing conflict, economic instability, and limited mental health resources exacerbate psychological distress. Additionally, Iraq's PTSD prevalence of 31.35% surpasses global averages, highlighting the compounded burden on a population already exposed to prolonged trauma. These statistics illustrate the psychological distress experienced by Iraqis and emphasize the repercussions of the pandemic on mental well-being. However, more detailed analysis of how these outcomes manifest in specific groups is essential for targeted interventions.
Vulnerable Populations
Certain demographic groups have been identified as being more susceptible to the mental health implications of the pandemic. Specifically, university students, who face pressures associated with academic life, have reported experiencing psychological difficulties (Mohammed & Memmedova, 2023). For example, 59% of university students in the study reported symptoms of anxiety, 58.2% experienced depression, and 61.6% reported stress, highlighting the unique challenges faced by this demographic group during the pandemic. Additionally, elderly individuals, who often deal with isolation and health issues, have expressed feelings of stress (Qadr & Ismail, 2023).
Contextual Factors
Iraq's unique context, which is marked by a long history of conflict, political instability, and economic hardships, has a significant impact on the psychological well-being of its people (Ahmed, 2022; Saied et al., 2023a). The ongoing COVID-19 pandemic has worsened this situation, exacerbated existing mental health problems, and presented new challenges. This interplay between the pandemic and pre-existing social stressors has contributed to heightened rates of mental health issues, as observed in the general population—for instance, 44.9% depression and 47.1% anxiety among individuals surveyed in April 2020 (Kamal & Othman, 2020). Furthermore, the consequences of the pandemic go beyond the transmission of the virus itself, as the burden on mental health exceeds its physical toll (Ornell et al., 2020).
Awareness and Education
Awareness and various other factors, such as the media disseminating false information, limited understanding of COVID-19, and the lack of effective vaccines or pharmaceutical treatments, collectively contribute to the manifestation of symptoms associated with depression and anxiety (Blbas et al., 2022). These factors underline the importance of accurate information dissemination and public education campaigns to mitigate the psychological burden of the pandemic.
Implications for Public Health
The systematic review highlights the importance of addressing the mental health consequences of the pandemic within an academic setting. Effective strategies should include providing easily accessible mental health resources, promoting coping mechanisms, and enhancing mental health and psychosocial support. According to Kamal et al.'s study, interventions that address immediate mental health needs and foster long-term resilience are recommended (Kamal & Othman, 2020). Given the varying prevalence rates of mental health issues, a comprehensive approach tailored to the specific needs of different population segments is necessary. In summary, this systematic review emphasizes the urgent need for comprehensive and targeted interventions to address the mental health challenges brought about by the COVID-19 pandemic in Iraq. The diverse prevalence rates of mental health issues underscore the importance of providing accessible and effective mental health support and resources to mitigate the adverse psychological effects of the pandemic on the Iraqi population.
Strengths and Limitations
This review has several limitations. One limitation is the lack of longitudinal data. Most of the studies analyzed were cross-sectional, which means we can't establish cause-and-effect relationships or observe changes in mental health over time. Additionally, the exclusion of non-retrieved articles may introduce a potential publication bias, as the studies included may not fully represent the breadth of research conducted in Iraq during the COVID-19 pandemic. This bias could result in an overestimation or underestimation of mental health outcomes. The language restriction to English-only studies is another potential source of bias that limits the inclusiveness of this review.
However, a strong point of this study is that it incorporates the most comprehensive systematic review to date on the psychological impact of COVID-19 in Iraq. The use of high-quality, critically appraised studies strengthens the reliability of our findings, and the adherence to PRISMA 2020 guidelines ensures a rigorous methodological approach. Furthermore, the detailed synthesis of data across diverse population groups provides a nuanced understanding of the pandemic's mental health effects in Iraq.
Implications for Practice
The mental health challenges highlighted in this review underscore the urgent need for targeted interventions within Iraq's healthcare system to address the psychological impact of the COVID-19 pandemic. Health practitioners, policymakers, and mental health professionals must collaborate to design comprehensive mental health programs that offer accessible, culturally sensitive support. This includes integrating mental health services within primary healthcare settings to improve reach, reduce stigma, and provide early interventions. Furthermore, specialized training programs for healthcare providers are essential to equip them with the skills necessary to recognize and manage pandemic-induced mental health issues effectively.
Community-level initiatives can also play a critical role, with public awareness campaigns focusing on mental health literacy and stress management. Leveraging digital health tools, such as telepsychiatry and mental health apps, could bridge accessibility gaps, particularly in rural or underserved regions. Additionally, the healthcare system should explore partnerships with local organizations to foster social support networks, which are crucial in a context marked by prolonged conflict and instability.
Conclusion
This review brings attention to the high occurrence of stress, depression, anxiety, PTSD, and other psychological problems within Iraqi society. Drawing on the primary aimed of this review, our findings highlight the urgent need for tailored mental health interventions, particularly for vulnerable groups such as university students, COVID-19 survivors, and the elderly. These insights emphasize the importance of addressing mental health in a culturally sensitive and context-specific manner. Future research should explore longitudinal studies to better understand the evolving mental health landscape post-pandemic, incorporating underrepresented populations and addressing potential biases in study designs. Investigating the effectiveness of intervention strategies, such as community-based mental health programs and digital health tools, could also provide actionable insights for policymakers. Cross-country comparisons could further enhance our understanding of the interplay between cultural, economic, and political factors in shaping mental health outcomes during global crises. Therefore, it is essential for healthcare authorities, politicians, and mental health professionals to quickly recognize these findings and create personalized therapies, support systems, and mental health services that specifically cater to the needs of Iraqis. It is crucial to effectively tackle these mental health issues in order to reduce the long-lasting effects of the pandemic and foster resilience among Iraqis affected by COVID-19. By addressing these gaps and building on the current results, future studies can better inform policies aimed at reducing the long-term psychological toll of the COVID-19 pandemic, fostering resilience, and improving the overall mental health of the Iraqi population.
Supplemental Material
sj-docx-1-son-10.1177_23779608251347847 - Supplemental material for Widespread Mental Health Impacts of COVID-19 on Iraq's General Population: A Systematic Review
Supplemental material, sj-docx-1-son-10.1177_23779608251347847 for Widespread Mental Health Impacts of COVID-19 on Iraq's General Population: A Systematic Review by Sirwan Khalid Ahmed, Darya Rostam Ahmed, Radhwan Hussein Ibrahim, Safin Hussein, Hazhar Talaat Abubaker Blbas, Kochr Ali Mahmood, Karzan Qurbani, Abdulmalik Fareeq Saber and Araz Qadir Abdalla in SAGE Open Nursing
Footnotes
Acknowledgements
The authors wish to acknowledge the insightful comments and constructive critiques provided by the peer reviewers and editors, which significantly enhanced the quality of this research. We extend our profound appreciation to Assistant Professor Dr. Ribwar Arsalan Mohammed, Dean of the College of Nursing at the University of Raparin, for his continuous and invaluable support throughout the duration of this project.
ORCID iDs
Author Contributions
SKA and DRA conceptualization and design, SKA, and DRA write the first draft, SKA, DRA, SH, HTAB, RHI, AFS, KQ, and AQA review the literature and edit the manuscript. All authors read and agreed for the final manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
All relevant data are within the manuscript and its supporting information files.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
