Abstract
Postnatal depression is a critical public health issue with substantial impact on child development outcomes and family functioning. With the additional stressors that arose during the COVID-19 pandemic, the impact on global mental health has been marked. This study aims to examine the change in the prevalence of postnatal depression (PND) in Singaporean women before the onset of the pandemic and during the pandemic period. A single-center observational cross-sectional study was conducted at Kandang Kerbau Women’s and Children’s Hospital (KKH) where women were screened for postnatal depression using the Edinburgh Postnatal Depression Scale (EPDS). High scorers on EPDS (EPDS≥13) were considered probable cases of postnatal depression. The prevalence of high EPDS scorers increased from 4.9% in 2019 to 6.5% in 2021, which was statistically significant (p = .028). The total number of women who received screening for postnatal depression at KKH increased by 42.6% in 2021 compared to 2019, whilst the numbers identified as probable cases increased by 91% over the same period. The prevalence of PND in Singapore significantly increased during the COVID-19 pandemic.
The COVID-19 pandemic has had a drastic impact on public health worldwide, with unprecedented effects on economic, social, and psychological sectors. Singapore was one of the first Asian countries to be affected by the COVID-19 outbreak. To mitigate the effect of the pandemic, numerous preventative measures were implemented, such as business closures, travel and hospital visitation restrictions, and limitations on the size of social gatherings.1,2 The aim of this study was to examine the change in the prevalence of postnatal depression (PND) amongst mothers in the Postnatal Depression Intervention Programme (PNDIP) in Singapore before the onset of the COVID-19 pandemic versus during the pandemic period. This is especially pertinent given that postnatal depression is an important public health concern, with severe adverse impact on child development outcomes and family functioning. 3
Kandang Kerbau Women’s and Children’s Hospital (KKH) is the main public maternity hospital in Singapore and it hosts Singapore’s first postnatal depression early intervention program, PNDIP. It handles about a third of Singapore’s national births annually, representing approximately 12,000 deliveries every year. Women are routinely screened for postnatal depression at their obstetric review at KKH using the Edinburgh Postnatal Depression Scale (EPDS). 4 Women with high scores (EPDS≥13) are considered to have screened positive for PND and are referred for early intervention. We hypothesized that the prevalence rates of PND would be higher during the pandemic period.
Participants were recruited from the KKH Postnatal Depression Intervention Programme (PNDIP) from 2018 to 2021, following live births. Exclusion criteria included those who had been under psychiatric care during the prenatal period as per PNDIP protocol. Women who were below the age of 18 years were also excluded as they are under the management of a separate psychosocial care program in Singapore.
Participants were interviewed and screened individually by trained perinatal mental health case managers/clinical counsellors under the PNDIP, with the Edinburgh Postnatal Depression Scale (EPDS). The EPDS is widely used as a well-validated screening tool for postnatal depression.5,6 It is a 10-item self-reported scale in which each item is scored from 0 to 3, with higher scores corresponding with greater severity. An EPDS total score of <10 is considered a low score, 10–12 borderline, and ≥13 a high score which identifies probable cases of PND. Under the PNDIP care pathway, patients who were identified as high scorers (EPDS ≥ 13) were offered psychiatric intervention with supportive counselling or medication, whereas those with borderline scores (EPDS 10–12) were provided with phone support and monitoring.
Data collected from the PNDIP included the total number of women who received screening, and the number of high scorers (EPDS ≥ 13) for the pre-pandemic year of 2019 and the pandemic year 2021. The year 2020 was excluded as screening was limited due to restrictions on cross-service access during the height of the pandemic. Prevalence of PND was defined by the number of high scorers expressed as a ratio of the total population screened for that year. Prevalence of PND based on socioeconomic status and race were also analyzed. We collected data on (1) housing type (whether public or private), as a proxy measure for socioeconomic status in Singapore, and (2) race (Chinese, Malay, Indian, and others). Data was analyzed using Microsoft Excel (2016 version) for descriptive statistics and chi-square tests, and STAT software version 18.0(Statacorp, College Station, US) for effect size analyses. This study was submitted for ethics review and was granted an exemption by the Centralised Institutional Review Board.
Prevalence of Probable PND (EPDS high score ≥13).
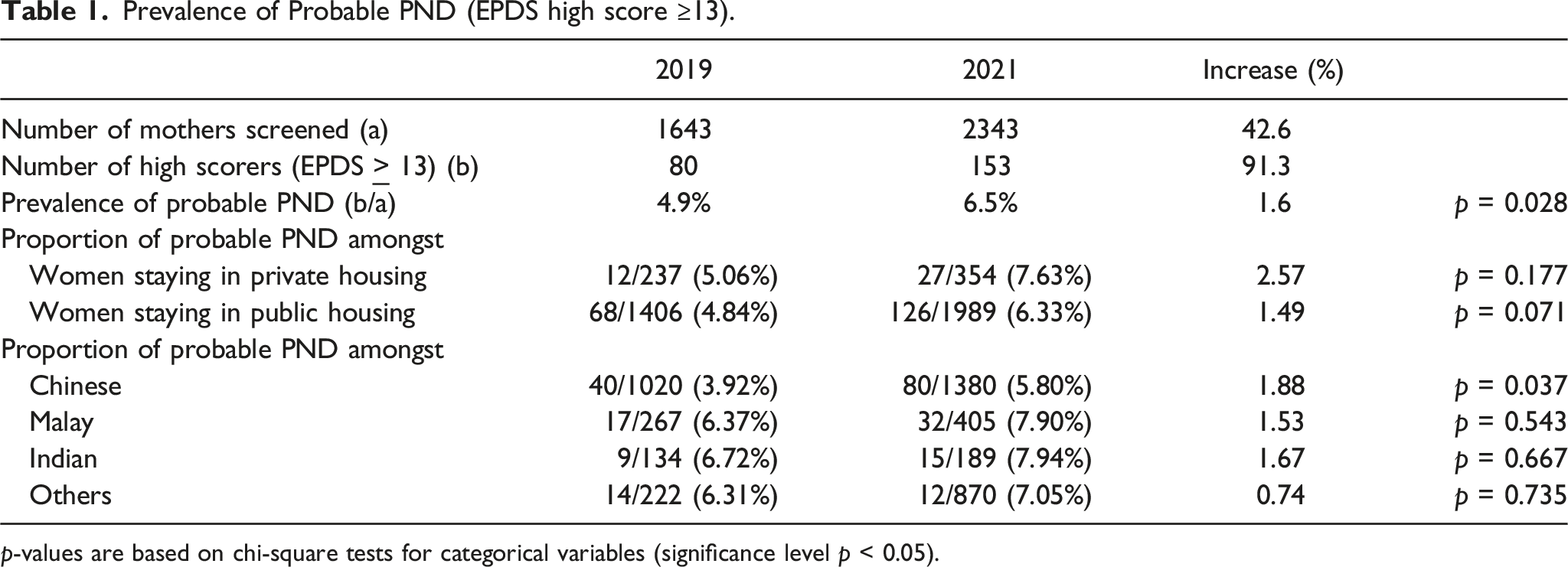
p-values are based on chi-square tests for categorical variables (significance level p < 0.05).
In terms of socioeconomic status, there was a slight increase in the percentage of high scorers in both private and public housing groups between 2019 and 2021. For race, more high scorers were seen across all ethnic groups (Chinese, Malay, Indian, others) in 2021 compared to 2019 (Table 1). However, the increase was statistically significant only amongst Chinese participants (p = .037), who nonetheless remained the ethnic group with the lowest prevalence of PND across both years. Although Indian women had the highest prevalence of PND compared to other races across both years, the difference was not statistically significant (p = .18–.30). This finding differed from that of an earlier PNDIP study, in which Indian women were significantly over-represented among high scorers. 12 A possible explanation for the difference was that a higher proportion of migrant Indian women presented for care at the study public maternity hospital in 2011, with related psychosocial challenges reported in this group. 13 Future research is needed to better understand ethnic and cultural influences on the prevalence development of PND.
The strengths in this study are derived from the relatively large and diverse sample size of the study as a result of the wide population KKH serves in Singapore. Additionally, as the screening was free and part of routine care, our study population is likely to be more representative of the general population, unlike other research populations that might be subject to sampling or selection bias. A key limitation is that we were unable to collect more detailed socio-demographic information (such as parity, past history of depression, substance or alcohol use, or level of social support) that is relevant to examining the risk factors associated with postnatal depression, as the data was extracted from a health service audit. The lack of data during the height of the pandemic in 2020 is also a limitation, although women presenting with symptoms or distress still had access to on-site psychiatric care. However, we believe that this study adds valuable knowledge to the long-term understanding and impact of COVID-19 on maternal mental health, and by extension child development outcomes and family functioning. Our findings suggest that the COVID-19 pandemic and its associated stressors have led to an increase in the prevalence of PND in Singapore, regardless of race or socioeconomic status.
Footnotes
Acknowledgements
We would like to acknowledge the women who participated in the KKH Postnatal Depression Intervention Programme (PNDIP), who shared their information to help inform maternal mental healthcare in Singapore. We would also like to thank Ms Elaine Quah Phaik Ling for her assistance in our data analysis.
Author contributions
KKC, SJU, and NYP prepared the manuscript. YCC led the team of clinical counsellors who conducted the screening for PND; CMY and MSC were part of this team and extracted the data from the PNDIP database. MSC and TEC performed the data analyses. HC led and designed the study, and all authors contributed to manuscript preparation.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval for this study was waived by the KK Women’s and Children’s Hospital Institutional Review Board because the study was conducted with minimal risk to participants and involved examining audit data from an existing clinical service programme. This study was completed in accordance with the Helsinki Declaration.
Informed consent
Written informed consent was obtained from patients for their participation in the PND Intervention Programme.
