Abstract
Introduction
Over the course of the COVID-19 pandemic, personal protective equipment (PPE) has become necessary. According to published research, PPE-related physical impacts were probably underreported during the pandemic.
Objective
To examine the physical burden and perceived stress associated with prolonged PPE wearing among nurses during the COVID-19 pandemic in the United Arab Emirates (UAE).
Methods
This was a cross-sectional retrospective study of 209 nurses working in two hospitals in the UAE. A convenience sampling technique was applied, and the data were collected using an online questionnaire. Data collection was completed within three months (April 2022 to June 2022). The completed questionnaires were analyzed using SPSS version 21. Chi-square statistics was used to test the association of categorical variables at a 5% level of significance.
Results
A total of 209 nurses had a mean age of 38.4 ± 8.7 years. More than 65.1% wore PPE continuously for 4 hrs per day. The most common physical burdens reported were difficulty in breathing (62.2%), excessive thirst (41.6%), and facial itchiness (39.2%). Most participants (95.2%) reported high-stress levels. There was no significant association between the level of stress and the duration of wearing PPE (p = .43 > .05). However, the authors found a statistically significant association between breathing difficulty with face masks and the duration of wearing them (p < .05). In addition, itchiness/rash related to gloves was significantly associated with wearing duration (p < .05).
Conclusion
Findings show that nurses experienced adverse effects from PPE use, which increased with the number of hours of wearing. Further studies with a larger sample size will allow for generalization of the study results.
Introduction/Background
Personal protective equipment (PPE) has become an important subject during the COVID-19 pandemic, owing to the high transmissibility of severe acute respiratory syndrome-coronavirus 2 infections (Galanis et al., 2021). Nurses and other healthcare workers (HCWs) provided care to patients in high-risk care settings, including isolation wards, intensive care units (ICUs), emergency rooms, and general medical and surgical wards (Galanis et al., 2021); therefore, they were obliged to wear PPE (respiratory and eye protection, gowns, and gloves) to interrupt infection transmission.
N95 masks, surgical masks, goggles or face visors, gloves, aprons, and gowns were recommended by the World Health Organization as essential PPE, while alcohol-based disinfectants and soap are advised to maintain good hand hygiene (World Health Organization, 2020). Concerns have been expressed about the rising incidence of occupationally caused adverse effects due to the prolonged duration that HCWs are required to wear PPE while delivering care during the COVID-19 pandemic (Gheisari et al., 2020; Lan et al., 2020; Navarro-Triviño & Ruiz-Villaverde, 2020). It is important to note that various research studies on COVID-19 have been conducted among healthcare professionals in the United Arab Emirates (UAE). Ilesanmi et al. (2021) reported an increased burden of caregiving among nurses in the region. However, to the best of the researchers’ knowledge, there seems to be a dearth of studies on the consequences of prolonged PPE use by healthcare personnel in this region.
Literature Review
A review of the published literature suggests that wearing PPE for an extended period of time increases the risk of skin irritation as well as other symptoms such as burning, discomfort, blisters, skin tears, acne, abrasions, eczema/atopic dermatitis, and allergic responses (Agarwal et al., 2020; Aloweni et al., 2022; Daye et al., 2020; Vidua et al., 2020). In addition to the physical symptoms, nurses practicing in high-workload departments such as Emergency Departments (EDs) and ICUs reported considerable mental burdens, including communication problems, depression, anxiety, isolation, and sadness (Xia et al., 2020). A study conducted in Italy by Vidua et al. (2020) noted that nurses reported facial bruises and falling asleep over workstations due to the constant wearing of PPE. Additionally, Unoki et al. (2021) observed several negative consequences, including pressure ulcers, heat exhaustion, thirst, and inability to use the restroom, in a scoping review of the literature on the impact of PPE among healthcare professionals in ICUs during the COVID-19 pandemic. Similarly, Tabah et al. (2020) in Australia revealed that 49% (n = 211) of healthcare professionals in the ICU experienced at least one negative consequence of wearing PPE in a cross-sectional web-based survey (PPE-SAFE).
Xia et al. (2020) examined the psychological and physical effects of PPE on 279 HCWs in Wuhan, China. According to the authors, 81.8% of the study participants reported face mask-related retroauricular pain as the most common adverse event. The authors also noted chest pain and dyspnea, lightheadedness, and pressure sores on the face around the nose (81%), cheeks (66.5%), forehead (45.1%), and retroauricular areas (43.6%).
According to Vidua et al. (2020), healthcare professionals have trouble working on PPE for extended periods of time because of headaches, dehydration, and urine retention. Also reports from China and Europe, showed that the extended PPE time has a number of issues (Lan et al., 2020). For example, China has a more distinct winter season, whereas European nations are typically distinguished by their temperate climates, which feature colder temperatures and drier conditions throughout the summer months (Lan et al., 2020). Yokomichi et al. (2021) noted that atopic dermatitis might also be more common in hot, humid settings. One theory to explain this phenomenon is that increased sweating under humid conditions impairs the barrier function of the skin, which promotes cellular turnover, resulting in an increased incidence and severity of atopic dermatitis in susceptible individuals (Kim & Leung, 2018). This retrospective study was conducted to examine the physical implications and perceived stress experienced by nurses during the COVID-19 pandemic.
Methods
Research Questions
What are the types of physical burdens experienced by nurses from prolonged use of PPE?
What is the level of perceived stress associated with prolonged PPE use among nurses?
What is the association between the type of physical burden and hours of wearing PPE?
The convenience sampling technique was used to select the participants.
The Cohen's Perceived Stress Scale (PSS; Cohen et al., 1983) is a validated tool with approved psychometrics and a 10-item scale to assess participants’ perceptions of their degree of stress (Questionnaire 1). Each participant provided feedback on each item on a Likert scale ranging from 0 to 4 (0 = never, 1 = practically never, 2 = seldom, and 3 = fairly). The total PSS score was calculated and categorized as low (0–13), moderate (14–26), or high (27–40). However, as indicated by content validity experts, certain statements were rephrased to better fit the study's aims. Each item's computed Item Content Validity Index score fell between a range of 0.8 and 1, indicating that all of the items were suitable and had high validity. The Score-Content Validity Index was 0.91. The interrater reliability coefficient is 0.92. The participants responded to a Google Form-powered online survey. A brief description of the study's goals and advantages was provided to the participants as part of an introduction to the online survey.
Demographic Characteristics.

Categories for the PSS, Average PPE Wear Time, and Different Types of Masks
The findings indicated that the disposable surgical mask 146 (69.9%) was the most popular face mask worn by nurses during work. However, 63 (30.5%) participants wore a respirator with an N95 filtering facepiece respirator (FFPR). Only 31 (14.8%) nurses reported an average PPE-wearing time of 12 hrs, while the majority of nurses 136 (65.1%) reported an average time of 4 hrs of wearing the PPE. The findings showed that 199 (95.5%) patients reported high levels of stress related to PPE (Table 2).
Categories for the PSS, Average PPE Wear Time, and Different Types of Masks (n = 209).
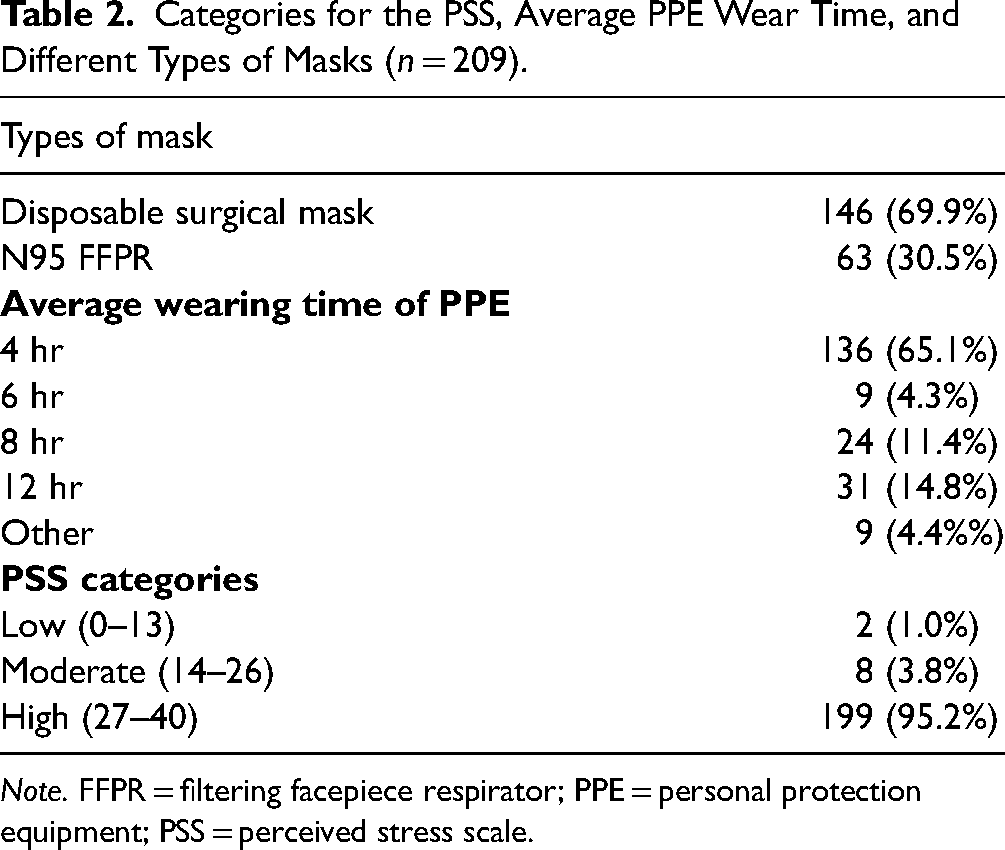
Note. FFPR = filtering facepiece respirator; PPE = personal protection equipment; PSS = perceived stress scale.

Physical burden of a facemask.

Effect of prolonged gloving.
As shown in Table 3, the majority of the nurses (103) reported a high level of stress with an average of 4 hrs of continuous wearing time of PPE. In addition, 25 reported a high-stress level with an average 8 hrs PPE-wearing time. However, the findings showed no significant association between the average PPE-wearing time and the level of stress among nurses (X2 = 7.423, p = .43 and >.05).
Analysis of Association Between Wearing Time of Personal Protection Equipment (PPE) With Perceived Level of Stress.

As shown in Table 4, breathing difficulty was significantly associated with prolonged use of facial masks (p = .00 and <.05). In addition, itching and rashes were statistically associated with prolonged glove use (p = .04 and <.05).
Association of Wearing Time of Facemask and Gloves With Physical Burden.

*p > 0.05
Discussion
Protecting HCWs from infection through appropriate infection prevention protocols is critical. PPE plays a fundamental role in achieving this objective, although the literature is consistent with the fact that prolonged PPE is associated with physical and mental burdens. This study aimed to investigate the physical burden of prolonged PPE, including nurses’ perception of stress during the COVID-19 pandemic. In this survey, more than 65.1% of the nurses said that they continuously wore PPE for 4 hrs each day. Breathing difficulties (62.2%), facial itching (32.1%), indentation and soreness behind the ears, and pressure injuries to the ear (18.2%), nose (22%), and face (23.9%) were among the physical burdens mentioned by the survey participants. These findings are consistent with those of a study conducted in Singapore by Aloweni et al. (2022). The authors stated that 53.8% (N = 592) of participants had PPE-related side effects, which supports the findings from other earlier studies, showing a high prevalence of pressure injuries and acne flare-ups when wearing face masks (Abiakam et al., 2021; Bambi et al., 2021; Chiriac et al., 2020; Han et al., 2020; Yaqoob et al., 2021). According to Han et al. (2020), prolonged usage of masks may cause acne to flare up more frequently due to increased temperature and humidity on the face, secondary to stale air and perspiration.
In the current study, there was a statistically significant association between time spent on gloves and skin itchiness (p < .05). A study by Daye et al. (2020), who assessed the skin issues in HCWs wearing PPE during the COVID-19 pandemic, supports the current findings. Accordingly, scientists have claimed that lichenification, dryness, itching, cracking, burning, flaking, and scabbing are the most common skin issues (Daye et al., 2020). Maintaining skin integrity is crucial for infection prevention because the skin serves as the body's main line of defense against infection. According to Pei et al. (2020), the use of PPE (goggles, masks, and protective garments) can compromise skin integrity. Therefore, attention should be paid to dermatological issues. Atzori et al. (2020) discovered that dryness, irritation, and burning were most prevalent among HCWs. The most frequently affected areas were the bridges of the nose, palms, cheeks, and periocular and perioral regions. In the current study, nasal and facial injuries were reported in 22% and 23.9% of participants, respectively. Furthermore, Daye et al. (2020) found that female HCWs were more likely to have skin issues than male HCWs. However, the authors of the current study did not make connections between incidence and sex.
Similarly, Lan et al. (2020) reported that wearing N95 masks and goggles caused substantial levels of cutaneous irritation. These skin issues may affect the nurses’ quality of life in terms of dermatology. In the current study, 55.5% of the nurses wore an N95 FFPR mask, which also caused pressure injuries to the nose (22%), ears (18.2%), facial rashes, and itching (39.2%). Evidently, other studies have found that using the N95 mask increases the severity of asthma attacks and that doing so causes cognitive impairment that results in serious mistakes when executing tasks (AlGhamri et al., 2013; George et al., 2022). In this study, the wearing time of face masks was significantly associated with breathing difficulty (p < .05).
Regarding stress levels, the majority of nurses (95.5%) reported having a high degree of stress as a result of wearing PPE for an extended period. Similarly, a study of the relationship between PPE and nursing staff stress during the COVID-19 pandemic (Hoedl et al. (2021) revealed that 56% (n = 1404) of nurses who used gloves experienced moderate levels of stress. These data corroborate the findings of this current study. However, there was no statistically significant correlation between stress and the use of face masks, eyewear, gloves, or gowns. This suggests that the stress levels in the study cohort were unaffected by the use of PPE. Similarly, the findings from this study revealed no connection between high-stress levels and longer PPE duration (p > .05). Hoedl et al. (2021) explained that, because nurses are fully aware of the significance of utilizing PPE, as it constitutes the only option to ensure safety for both themselves and their patients. This may explain these findings. The authors further explained that the use of PPE itself was not linked to the stress felt by nursing personnel. This could be due to their knowledge of contagious viruses. The reported issues with using a face mask were breathing difficulties, lightheadedness, and cloudy vision. The researchers believe that the high degree of stress experienced by nurses in the current study may have been influenced by the fact that wearing a facemask continuously for 4 hrs or more is linked to physical symptoms, such as migraines (Ong et al., 2020). This finding suggests the need for nursing management techniques to reduce the impact of PPE. Desai et al. (2020), in a similar analysis, proposed that routine cleaning, skin moisturization with emollients at least an hour before applying facial PPE, proper wearing of facial PPE, and selecting the appropriate sizes could minimize adverse events connected to facial PPE.
Another essential PPE used during the pandemic was coveralls. Findings from the current study indicated that nurses reported physical loads such as excessive perspiration (77.5%), mask soaking (37.8%), difficulty urinating (40.2%), headache (30.1), claustrophobia (12.4%), and skin injury (7.7%). These results are consistent with those of George et al. (2022), who investigated the physiological risks of PPE use among HCWs in central India. According to the authors, the main issues with wearing coveralls or other protective garments during the pandemic were excessive sweating, skin rash with itching, and dry skin. According to the literature, frequently changing protective garments could be an excellent way to solve this issue (Hu et al., 2020). In addition, several PPE users have reported long-term stress, anxiety, and psychological claustrophobia (George et al., 2022).
Ethical Considerations
Two institutional boards, the Research and Ethics Committee at RAK Medical and Health Sciences University, and the Ministry of Health and Prevention Research and Ethics Committee (202213-2022-PG-N, 117-202122-PG-N) granted ethical approval for the conduct of the study. Nurses were informed of the study's goals and advantages and an online poll was used to request their agreement to participate in the study. Each potential participant was expected to click “yes” or “no” to express their consent or otherwise on the consent form, which clearly stated the purpose of the study. The survey form was opened by selecting “yes.” To safeguard the privacy and confidentiality of participants, codes were assigned to each respondent's data-gathering tool.
Footnotes
Acknowledgements
The authors acknowledge the support of the nurse managers in the selected hospitals, as well as the nurses who participated in the study.
Authors Contribution
All authors participated sufficiently and take responsibility for the content, concept, design, analysis, writing, or revision of the manuscript. Mariam Mohamed Hasan: Conceptualized the study, participated in the data collection, and reviewed and edited the manuscript. Rose Ekama Ilesanmi: Conceptualized the study design, provided the resources (instruments) for the data collection, and interpretation, and prepared the initial draft, revision, and editing of the manuscript. Eman Abdelaziz Rashad Dabou: Participated in data acquisition, conducted the formal analysis, data synthesis, and interpretation, and revised the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
