Abstract
Inadequate provision of medication-related information can lead to nonadherence to treatment. This study aims to investigate patient satisfaction regarding medication-related information provided by healthcare professionals and to identify factors associated with patient experience regarding information. A cross-sectional descriptive study was conducted in October 2023 among 400 patients at a rural private polyclinic in Ben Tre, Vietnam by using a self-administered questionnaire. The key findings of this study showed that over half of the participants expressed overall satisfaction with the information provided (52%), with 57.5% satisfaction on the action and use subscale, and 56.8% satisfaction on the potential problems subscale. Patients aged 41 to 60 (P = .018), those older than 60 (P = .001), those with more than 2 dependents (P = .038), and those receiving information only from nurses (P = .009) were more likely to be satisfied with the information they received. Patient satisfaction with medication-related information received was low. Healthcare professionals should ensure timely and comprehensive communication about medications, particularly regarding potential side effects. While this study primarily focused on satisfaction, the closely related concept of patient experience warrants further exploration in future studies with a more deliberate focus.
Introduction
Nowadays, people are highly concerned with their healthcare, creating a strong demand for information relating to diseases, symptoms, and treatment methods. In this context, healthcare models help to promote the active involvement of patients in the healthcare process, as in the patient-centered care model, representing a significant trend in the medical field. Identifying, understanding, and considering patient priorities are integral parts of patient-centered care, playing a crucial role in improving patient satisfaction, patient experience, and health outcomes.1,2
Medication is one of the most common healthcare interventions, and patients often need comprehensive information about their medications to facilitate making informed decisions about treatment processes. This becomes especially important in the evolving healthcare landscape that emphasizes patient-centered care.3,4 Due to differences in strategies for coping with illness, an individual patient's requirement for medication-related information can vary significantly. 5 Patients are exposed to multiple sources of medication-related information, including healthcare professionals, the internet, family/friends, and social media. 6 However, when a patient receives information from nonhealthcare sources, there is a risk of that information being inaccurate, leading to confusion and impacting treatment outcomes. 7 Insufficient provision of medication-related information, poor patient understanding about medications, and inadequate information communication from healthcare professionals can lead to serious consequences, such as medication errors, improper use, nonadherence to treatment, overdoses, and misunderstandings about the significance of side effects. These issues contribute in turn to treatment failure.8–11
To ensure that patients have sufficient understanding about their medications, there is a responsibility on healthcare professionals to provide comprehensive medication-related information and to ensure patient satisfaction with the information provided. 10 In this context, patient satisfaction and patient experience play an essential role in healthcare services. The main indicator of patient satisfaction is the patient's expectations and their assessment of whether or not they were fulfilled. 12 Subjective factors can affect satisfaction, 13 which can vary throughout populations and circumstances. 14 However, from the viewpoint of the patient, patient experience includes all facets of care, such as clinical quality, communication, emotional support, and participation in decision-making. 15 Experience is a more objective indicator of how well healthcare providers interact with patients than satisfaction.
A positive correlation has been demonstrated between medication adherence and patient satisfaction with medication-related information received. 16 A study conducted in the United Kingdom (2018) reported that 74.4% of inpatients were satisfied with information provided regarding drug “action and use” and 56% of patients were satisfied with information provided regarding “potential problems.” Age, education level, and ethnicity were found to be associated with inpatient satisfaction regarding medication-related information received. 16 A study conducted in China (2019) in patients with systemic lupus erythematosus reported that 67.62% of patients were dissatisfied with the medication-related information they received, especially relating to potential problems (63.63%). 17
In Vietnam, the medication counseling model for outpatients faces numerous barriers to full implementation, despite some studies indicating that the majority of patients have a need for medication counseling.18,19 Information that patients need relates to medication use, indications, drug names, dosage, and side effects. The preferred counseling methods for most patients are face-to-face and telephone consultations.18,19 According to Bui et al (2015), over 50% of patients are willing to pay for counseling services. 19 Although many patient satisfaction and patient experience studies were conducted in Vietnam, these studies were on many different aspects, such as satisfaction with healthcare service quality,20,21 notable aspects of patient's service experience, 22 which not yet thoroughly evaluated drug information factors.
To the best of our knowledge, no relevant study has reported patient satisfaction with medication-related information received in the Vietnamese population. Patient demand for medication information continues and evolves over time. 3 However, the amount of time allocated to the exchange of information relating to medications between healthcare professionals and patients is limited. Therefore, the present study aims to explore patient satisfaction with multiple aspects of medication-related information received from healthcare professionals and to identify factors relating to patient satisfaction with this information. Although this study focuses on patient satisfaction, its findings are anticipated to offer deeper insights into the broader patient experience and shed light on ways to enhance the medication counseling process.
Method
Study Setting
This study used a cross-sectional descriptive design with a self-administered questionnaire to recruit patients attending a rural private polyclinic in Ba Tri district, Ben Tre province, Vietnam, between October 1 and 31, 2023. Ben Tre is a province in Vietnam located at the end of the Mekong River ranks 4th in population density. 23 Ben Tre is well-known for its longstanding agricultural economy with 90% of population reside in rural areas. According to health statistics in 2020, Ben Tre province hosts 760 doctors, 496 pharmacists, and 1435 nurses. 24 With an average population of 1.2924 million people, 24 the ratio of specialists per 10 000 population is approximately 5.88 doctors, 3.84 pharmacists, and 11.10 nurses.
Study Population
The study population comprised patients who visited a polyclinic in Ba Tri, Ben Tre, Vietnam. Inclusion criteria included adults aged 18 or older who had received medications at the polyclinic in the past 3 months. Exclusion criteria included patients who were illiterate in Vietnamese or did not agree to participate in the study.
Sample Size
The sample size for the study was determined using the sample size formula implemented in the online software, Raosoft, developed by the Australian Bureau of Statistics. 25 A required sample of 368 participants was calculated, assuming a confidence level of 95%, a 5% margin of error, and a response rate of 58% based on the findings of Twigg et al (2016). 11
Data Collection
The estimated number of patient visits to the clinic in one month was approximately 4650. Each day, the research team conveniently selected 15 patients to invite to participate. In the study period, a total of 465 individuals were selected and invited to the study. Each participant who accepted the invitation was sent a printed questionnaires to complete without supervision. Participation was voluntary and anonymous. Completing the survey took approximately 10 min.
Survey Tool
A printed self-administered questionnaire was developed based on the Satisfaction with Information about Medicines Scale (SIMS) 5 and the Medicine Information Needs for Individuals Questionnaire (MINI-Q). 2 These 2 questionnaires were integrated to form one questionnaire, which was then translated, and adjustments made to adapt the content for use in the context of Vietnam. Specifically, all 17 questions from the SIMS questionnaire were used, supplemented by an additional 6 questions from the MINI-Q questionnaire that did not overlap with the SIMS questions. Thus, the questionnaire constructed by the research team comprised a total of 23 questions (Appendix). Three healthcare experts assessed the content validity of the questionnaire and subsequently, small modifications were made to improve respondent comprehension. For instance, Question 4 “How it works” was changed to “How your medication works or has an effect,” Question 6 was also adjusted from “How I will know my medicine is working” to “How you will know that your medication is working or taking effect.” We summarized lengthy questions without changing the meaning, such as Question 9, which was modified from “If I run out of medication, how to get a further supply” to “How to get a further supply.” The final version of the questionnaire comprised 2 sections.
The first section included patient information such as gender, age group, ethnicity, marital status, occupation, number of dependents, participation in health insurance, chronic diseases, disease characteristics, source of medication information received and income.
The second section aimed to assess patient satisfaction with medication-related information received, consisting of 23 questions divided into 2 subscales: (i) action and use and (ii) potential problems, with 5 answer options: “about right,” “none needed,” “too much,” “too little,” and “none received.” For each item, responses of “about right” and “none needed” were allocated 1 point, indicating patient satisfaction. Responses of “too much,” “too little,” and “none received” were allocated 0 points, indicating patient dissatisfaction. Questions 1 to 12 formed the action and use subscale with a total possible subscale score ranging from 0 to 12, while questions 13 to 23 formed the potential problems subscale with a total possible subscale score ranging from 0 to 11. The overall satisfaction score represented the sum of scores from all 23 questions across both subscales, and had a possible range of 0 to 23. Patients with an overall satisfaction score above the median were considered satisfied, and conversely, those with an overall score equal to or below the median were classified as dissatisfied. 17 Similarly, for the 2 subscales, the median threshold was chosen to classify participant satisfaction along each subscale. 3
Reliability of each of the scales was assessed using Cronbach's alpha. A Cronbach's alpha coefficient higher than 0.7 and corrected item-total correlations greater than 0.3 were considered to demonstrate the reliability. In fact, the scales of action and use, potential problems were found to have Chronbach's alphas of 0.88 and 0.91, respectively. All corrected item-total correlations greater than 0.3.
Data Analysis
Data were analyzed using SPSS Statistics version 22.0. Descriptive statistics such as frequency (n) and percentage (%) were used to summarize categorical data. In line with previous studies, 16 univariate analysis, including chi-square test, were used to determine the associations between demographic characteristics (gender, age group, ethnicity, marital status, occupation, number of dependents, health insurance, chronic diseases, source of medication information received, and income) and patient satisfaction with the medication-related information received (overall satisfaction variable categorized as “satisfied” or “dissatisfied”). Variables with a significance of P < .05 were then included in the multivariate logistic regression model using the binary logistic regression with the enter method. For each demographic characteristic, the odds ratio (OR), 95% Confidence Interval (CI), and significance (P) were calculated to estimate patient satisfaction with the medication-related information received. Significance was considered at a threshold of P < .05.
Results
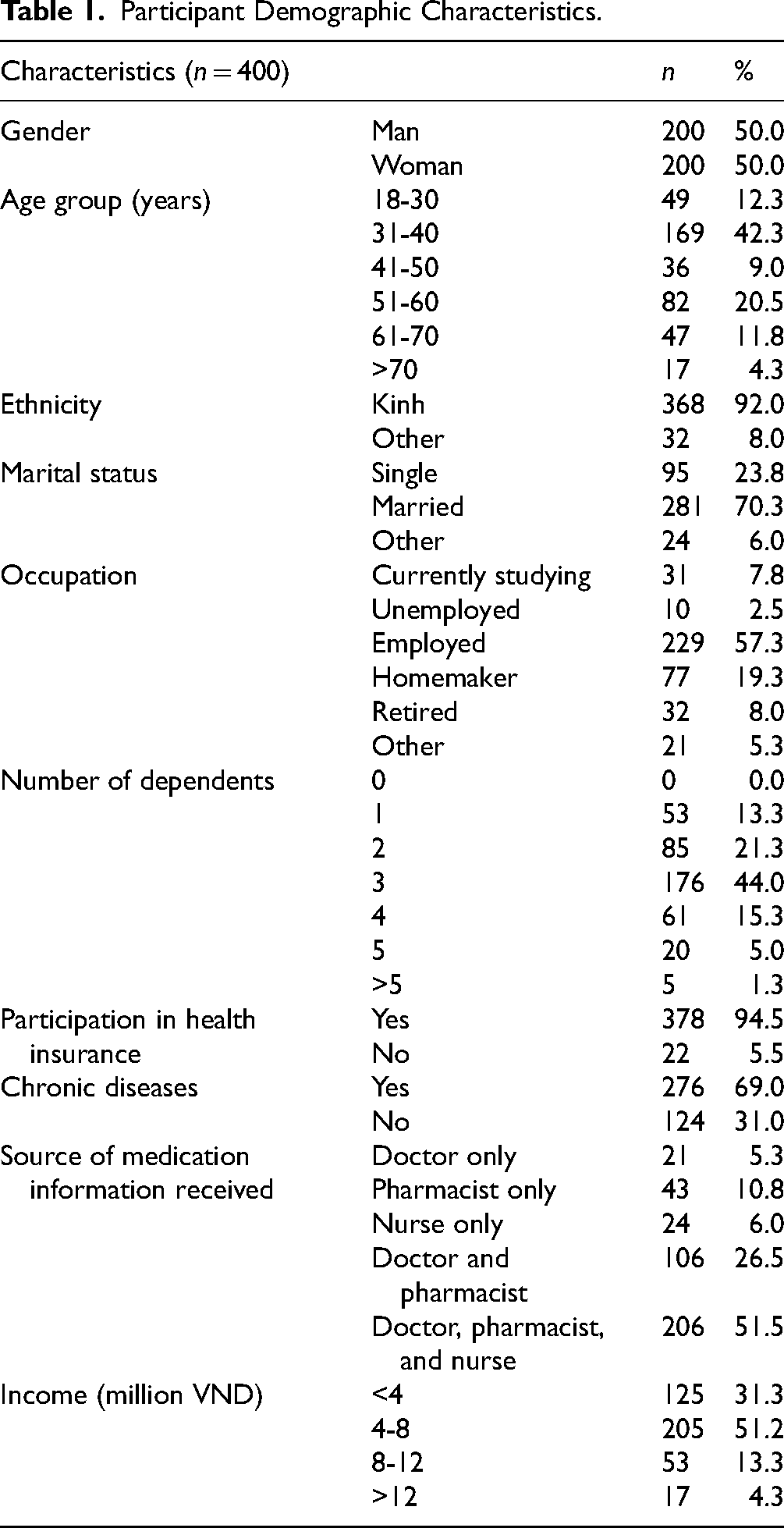
In total, 465 questionnaires were distributed, and 400 valid responses were received, resulting in a response rate of 86%. The majority of participants had health insurance coverage (94.5%), were married (70.3%), and employed (57.3%), as presented in Table 1. Nearly 70% of participants reported having chronic diseases, with gastric-duodenal inflammation and ulceration being the most prevalent (39%) (Figure 1).

Diseases reported by participants.
Participant Demographic Characteristics.
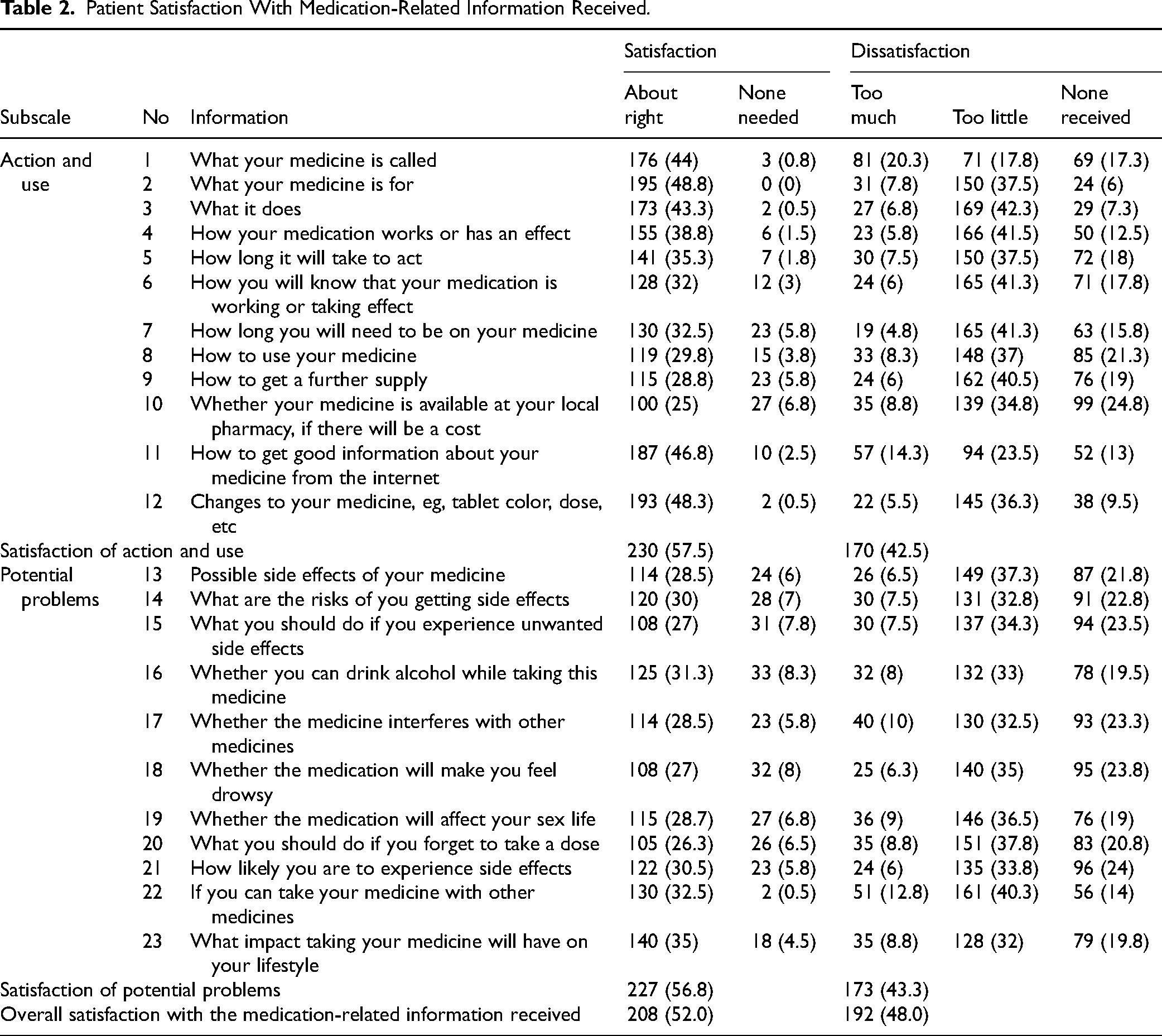
More than half of the participants expressed overall satisfaction with the medication-related information received (52%), with 57.5% satisfaction on the action and use subscale, and 56.8% satisfaction on the potential problems subscale. Participants reported that the information provided was “too little” or “none received” with high rate, specifically relating to the “Possible side effects of your medicine,” “What are the risks of you getting side effects” (37.3% and 32.8%, respectively). While the majority of participants rated that the information received was “about right” in relation to “What your medicine is for” (48.8%) and “Changes to your medicine, eg, tablet color, dose, etc” (48.3%) (Table 2).
Patient Satisfaction With Medication-Related Information Received.
Univariate analysis identified 8 variables associated with overall satisfaction with medication-related information received, including gender, age group, ethnicity, occupation, number of dependents, participation in health insurance, chronic diseases, and source of medication-related information received (Table 3). These variables were then included in a multivariate regression model, and the results of this analysis revealed that only 3 variables were significantly associated with satisfaction with medication-related information. Specifically, participants aged 41 to 60 (OR = 1.954; 95% CI: 1.122-3.403; P = .018), those with more than 2 dependents (OR = 1.709; 95% CI: 1.030-2.839; P = .038), and those receiving medication-related information from nurse only (OR = 6.463; 95% CI: 1.605-26.030; P = .009) were more likely to be satisfied with the information they received.
Factors Associated With Patient Satisfaction Regarding Medication-Related Information Received.

Discussion
More than half of patients expressed satisfaction on the potential problems subscale in our study, suggesting that patients are interested in multiple aspects of information regarding their medications. However, global studies consistently show the majority of patients to be dissatisfied with the information received about the potential problems associated with their medications.16,26,27 The information gap predominantly exists around potential problems, reflecting a lack of overall focus on these issues by healthcare professionals. 27 Patient satisfaction with the information received and treatment adherence are positively correlated, as patients have varying information needs.5,11 Patients may become nonadherent if healthcare professionals do not provide sufficient information. 27 Therefore, effective disease management, including the provision of medication-related information, is key to ensuring strict adherence to treatment plans and helping alleviate illness. 17 Patient satisfaction focuses on whether patients feel their expectations have been met, but it is only one part of the bigger picture—the patient experience. The patient experience includes not just subjective feelings captured by satisfaction but also objective aspects like the quality of communication, empathy, and access to thorough medication information. To better understand the complex relationship between patients and healthcare systems, future research should explore this broader concept, looking at how effectively patient needs are recognized and met.
Concerning the potential problems subscale, respondents rating the information they had been provided as “too little” or “none received” was most common for items relating to the side effects of medications. One reason for this could be healthcare professionals’ concerns that information about side effects may cause unnecessary fear and nonadherence to treatment.8,28 According to a study by Sieg et al (2022), the majority of patients have a desire to be fully informed about potential side effects, especially those that are frequent and serious. 29 Similarly, a study by Aspden et al (2023) reported the most common theme participants wanted information about as being potential side effects (92%). 2 This underscores the importance of information related to the side effects of medications, especially in the current era of enhanced global pharmacovigilance. 30 Healthcare professionals must provide clear information to patients about the side effects of medications, enabling them to understand, detect, and report side effects to healthcare professionals, and increase confidence in medication use.31,32 The future research should focus on strategies to communicate drug side effects through personal counseling or digital tools to ensure that patients receive clear information, supporting both understanding and global pharmacovigilance efforts.
On the action and use subscale, a significant portion of patients were dissatisfied with the medication information they received, particularly regarding what the medication does and how it works. The reason for this could be that healthcare professionals believe that during brief consultations, they should only provide general and easily understandable information to patients about the reason for taking the medication. It may be believed that when patients understand the reason for using the medication, they are more likely to have a psychological inclination toward better medication adherence. Studies have also shown that patients often do not take their medication due to a lack of understanding of the reason for taking the medication.9,17,33 However, information about the function of the drug and how the drug works is related to specialized knowledge such as pharmacology and pharmacokinetics, making it challenging for patients to understand and requiring patients to have a prerequisite level of medical knowledge to understand.34,35 However, if patients do not know the purpose and name of the medication, they may misuse the medication, use it for the wrong purpose, and reduce the effectiveness of the treatment.8,9 Future studies should explore how providing more detailed information about medication use during consultations affects patient understanding and adherence.
This study found that older patients tended to be more satisfied with the information received about their medication. This finding aligns with numerous global studies3,16,36 and could be explained by older patients often having a better background understanding and a lesser inclination to challenge the authority of a healthcare professional. 16 Additionally, patients with more than 2 dependents were more likely to be satisfied with the medication-related information received, being 1.709 times higher to be satisfied than patients with 2 or fewer dependents. This is consistent with the findings of Matos et al (2022). 26 This underscores the importance of patients receiving support from family members, as those with more dependents may receive better assistance from family members in managing the medication-related information they receive and gaining a clearer understanding, especially in Asian countries, because of cultural features.37,38 A future qualitative study should explore why older patients and those with more than 2 dependents report higher satisfaction with medication information through in-depth interviews on their expectations and perceptions regarding medication-related information.
Patients received information only from nurses expressed significantly higher levels of satisfaction compared to those who only received information from doctor. This finding is consistent with multiple studies globally.28,39,40 Nurses, providing the closest and longest-standing contact point of contact for patients, may be more approachable and accessible, making it easier for patients to seek information. The experience of patient counseling by nurses is often perceived as friendly/approachable (>99%), instilling trust and reliability (>99%), and providing clear explanations of reasons for medication usage (97%). 28 This may indicate a lack of consensus among doctors, nurses, and pharmacists regarding their perceptions of responsibility in providing information. 27 Studies have emphasized the importance of a multidisciplinary team in providing comprehensive medication-related information to patients. 26 One challenge that may hinder doctors from providing comprehensive information to patients is the limited time available during medical appointments. In Vietnam, the average duration of a doctor's appointment is around 5 min. 41 During medical examinations, physicians need to focus on assessing overall health, signs and symptoms, and providing treatment advice all within a short time frame. This constraint may limit the physician's ability to provide detailed information about any medications prescribed. 42 For pharmacists, providing medication-related information to patients is a fundamental responsibility. The information provided should be comprehensive, comprehensible, and easy to understand to maximize the benefits of the medication. Among all medication information that needs to be conveyed, patients should, at the very least, be made aware of the instructions for use. 9
In conclusion, patients should receive information about their medications at various points in time, including during consultations with physicians, during visits to the pharmacist, and even in follow-up appointments after the treatment course has started. 43 There has been a global rise in popularity of online consultations (telepharmacy), particularly since the COVID-19 pandemic, including in Vietnam. 44 Multiple interactions with healthcare professionals help patients retain and consolidate more information and better understand the most relevant medication-related information. 43
Limitations
This study has several limitations. It was conducted in a single clinic in one province, potentially limiting the generalizability of the results to the entire population. The survey was conducted in the previous 3 months, for a one-month period (October) introducing possible recall bias and participant bias. To reduce response bias, the research team implemented measures such as informing participants that responses would be entirely anonymous and confidential. Language barriers related to the tool may be considered a limitation. To mitigate this limitation, the translation was performed with adherence to published guidelines, and cultural adjustments were implemented to ensure the applicability of the survey content to the research setting of the present study. Finally, the study did not aim to explore differences in patient satisfaction between inpatients and outpatients or among specific disease groups or between patients receiving specific medication types. However, this study represents the first to provide an overall perspective on patient satisfaction with the provision of medication-related information in Vietnam. Other demographic and health-related variables, such as literacy level and type of chronic diseases, may influence satisfaction but were not explored in this study. Future research should examine a wider range of these factors. This study provides valuable insights into patient satisfaction; however, to gain a more comprehensive understanding of the patient experience, future research should explore both subjective and objective aspects of the relationship between patients and the healthcare system.
Conclusion
This study reports levels of patient experience with medication-related information received, across the 2 subscales of potential problems and action and use. Satisfaction on the potential problems subscale was slightly lower than satisfaction on the action and use subscale. Most patients felt that insufficient information was provided relating to the potential side effects of their medication. Overall satisfaction with medication-related information was low. Older patients, those with more dependents, and those receiving information solely from nurse reported higher levels of satisfaction. This study highlights the importance of increasing the duration of interactions between healthcare professionals and patients, and better optimizing the amount and quality of medication-related information provided by healthcare professionals to patients. While factors like literacy level and type of chronic diseases may also influence satisfaction, they were not explored in this study, highlighting the need for future research to examine a broader range of variables.
Footnotes
Appendix
Acknowledgments
We express our gratitude to the Can Tho University of Medicine and Pharmacy and the patients who participated in this study.
Availability of Data and Material
The data that support the findings of this study are available from the corresponding authors upon request.
Author Contributions
Conceptualization: QLDV and VDT; methodology: QLDV and VDT; investigation: MTN and TNYD; resources: MTN, THDQ, and HKNT; writing—original draft: QLDV, VDT, MTN, TNYD, THDQ, HKNT, TTT, and RSD; writing—review and editing: QLDV, VDT, MTN, TNYD, THDQ, HKNT, TTT, and RSD.
Conflicts of Interest
The authors have no conflicts of interest to declare.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
The study was approved by the Institutional Review Board of the Hoa Binh Ba Tri polyclinic, Ben Tre, Vietnam. Participants were informed that taking part in the study was voluntary. Participants gave written informed consent.
Statement of Human and Animal Rights
All procedures in this study were conducted in accordance with the Declaration of Helsinki and the Institutional Review Board of the Hoa Binh Ba Tri polyclinic, Ben Tre, Vietnam.
Statement of Informed Consent
Written informed consent was obtained from the patients for their anonymized information to be published in this article.
