Abstract
Patient characteristics have been linked to prevalence and quality of shared decision-making (SDM) behaviors across diverse studies of varied size and focus. We aim to evaluate the extent to which patient characteristics are associated with patient-rated SDM scores as measured by
Introduction
Shared decision-making (SDM) has been defined as “a process by which clinicians and patients make decisions together using the best available evidence about the likely benefits and harms of each option, and where patients are supported to arrive at informed preferences” (1,2). Shared decision-making has been demonstrated to improve decisional conflict, uncertainty, and knowledge of treatment options among disadvantaged patients (3) and has been suggested as a possible means of reducing health disparities (4). Shared decision-making has been shown to benefit underserved populations “more than those with higher literacy, education, and socioeconomic status” (3). Shared decision-making also improves knowledge and helps form informed preferences among a broader patient population (5). However, existing literature has also shown the prevalence and quality of SDM and related communication constructs to vary according to patient and clinician characteristics (6 –18), as well as organizational and system-level factors, including the extent to which SDM is included in medical training (19).
In studies assessing SDM and patient–clinician communication across patient characteristics, age, gender, race/ethnicity (including race concordance between patients and clinicians), health status, socioeconomic status (including poverty and proxy measures such as educational attainment and employment status), and English proficiency have each been identified as associated with the prevalence and/or quality of SDM. Joseph-Williams’s 2014 systematic review (13) reports age as a barrier to SDM with mixed findings as to whether it is older or younger age that is associated with lower SDM. Forcino et al (7), Tai-Seale et al (20), Xu and Wong (21), Barton et al (14), and Solberg et al (12) support Joseph-Williams et al’s (13) earlier systematic review, with Forcino et al (7) and Tai-Seale et al (20) finding slightly higher SDM reports by older patients, while Barton et al (14), Solberg et al (12), and Xu and Wong (21) find poorer SDM among older age groups. Forcino et al (7) and Tai-Seale et al (20) also identify gender as a significant predictor of patient-reported SDM, with women more likely than men to provide high SDM ratings.
With regard to race and SDM, Cooper-Patrick et al (10) report that African American patients experienced less participatory healthcare visits than their white counterparts, a finding which was moderated by race concordance between patient and clinician. Both Joseph-Williams et al (13) and Solberg et al (12) found poor health status to be associated with poorer SDM. Lower socioeconomic status has also been demonstrated to predict poorer SDM, with proxies including limited educational attainment associated with poorer SDM in studies by Xu and Wong (21), Joseph-Williams et al (13), and Peek et al (15), patient employment associated with higher SDM in the study by Menear et al (6), and receipt of government financial assistance predicting lower SDM in the study by Xu and Wong (21). Poverty itself was associated with lower SDM in the study by Solberg et al (12). Finally, limited English proficiency was associated with poorer SDM in studies by Barton et al (14), Suurmond and Seeleman (18), Mosen et al (8), and Morales et al (9). Because of these previously identified associations between SDM and patient characteristics, each of these characteristics was represented in the current analysis to replicate those prior studies and determine whether those relationships hold in a large California-based sample. As the largest routinely collected generic (ie, not specific to a certain type of medical decision) SDM measurement effort to date, this study has the potential to further elucidate relationships between patient characteristics and SDM in a large and diverse sample.
Given the promise of SDM in improving health outcomes and reducing disparities (3,4), SDM is increasingly emphasized in clinical practice. This emphasis also translates to medical education, where 75% of medical students report training in SDM (23). Efforts to measure SDM have therefore increased (24), demonstrated by the development of
In this study, we aim to (1) replicate existing studies using a large patient survey sample to evaluate the extent to which patient-level characteristics are associated with patient-rated SDM scores as measured by
Methods
Data
This study involved secondary analysis of the 2017 California Patient Assessment Survey (PAS) data set. The PAS is an annual cross-sectional survey conducted by the Pacific Business Group on Health. Our use of the deidentified data set was approved by the Pacific Business Group on Health and deemed exempt from further ethics review by our institutional review board.
Participants
Per the PAS standard sampling procedure, participants included adult (18 years and older) patients with commercial health insurance coverage who received ambulatory healthcare services from one of 153 participating California-based medical groups between January and October 2016.
Survey Administration
The PAS administration procedure invites a random sample of eligible patients to complete the survey through a sequence of survey administration modes, beginning with e-mail invitations to complete the survey online, followed by mailing the survey, and finally offering telephone administration for prior nonrespondents. Questionnaire administration was offered in English, Spanish, Chinese, Korean, and Vietnamese languages. Surveys were administered between December 2016 and March 2017.
Measures
Of the 35 total items in the 2017 PAS, this study includes demographic items in addition to
Measures.

Analysis
Scoring
We used the top score approach to
Patient characteristics: Relationship to collabo RATE top-box scores
We used mixed-effects logistic regression analysis to evaluate the relationship between
We conducted a sensitivity analysis exploring the interaction between patient age and general health status by adding an interaction term to the regression model described above. As this sensitivity analysis resulted in a statistically nonsignificant interaction term (p > .05), we used the original regression specification described above in presenting and discussing our results.
We used Stata 13 software for all statistical analysis. As most missingness on patient characteristic variables was observed in blocks, missing data on any
Patient and provider characteristics: collabo RATE item-level analysis
Replicating the analysis described above using the same fixed and random effects, we conducted mixed-effects logistic regression analysis with top-box scores for each of the 3
Results
Participant Characteristics
We analyzed 31 265 total responses to the PAS, reflecting an overall survey response rate of 29.5%. Majorities of respondents were between the ages of 45 and 64 (61.7%), attended at least some college (81.3%), were white (63.5%), and spoke English at home (86.3%). Table 2 presents full demographic details for survey respondents.
Demographic Profile of Survey Respondents.

a Multiple responses accepted.
Medical Group/Survey Characteristics and Overall collaboRATE Scores
Among the included medical group and survey characteristics, only mode of survey response was significantly associated with
Mixed-Effects Logistic Regression Results: Patient, Provider Characteristics, and
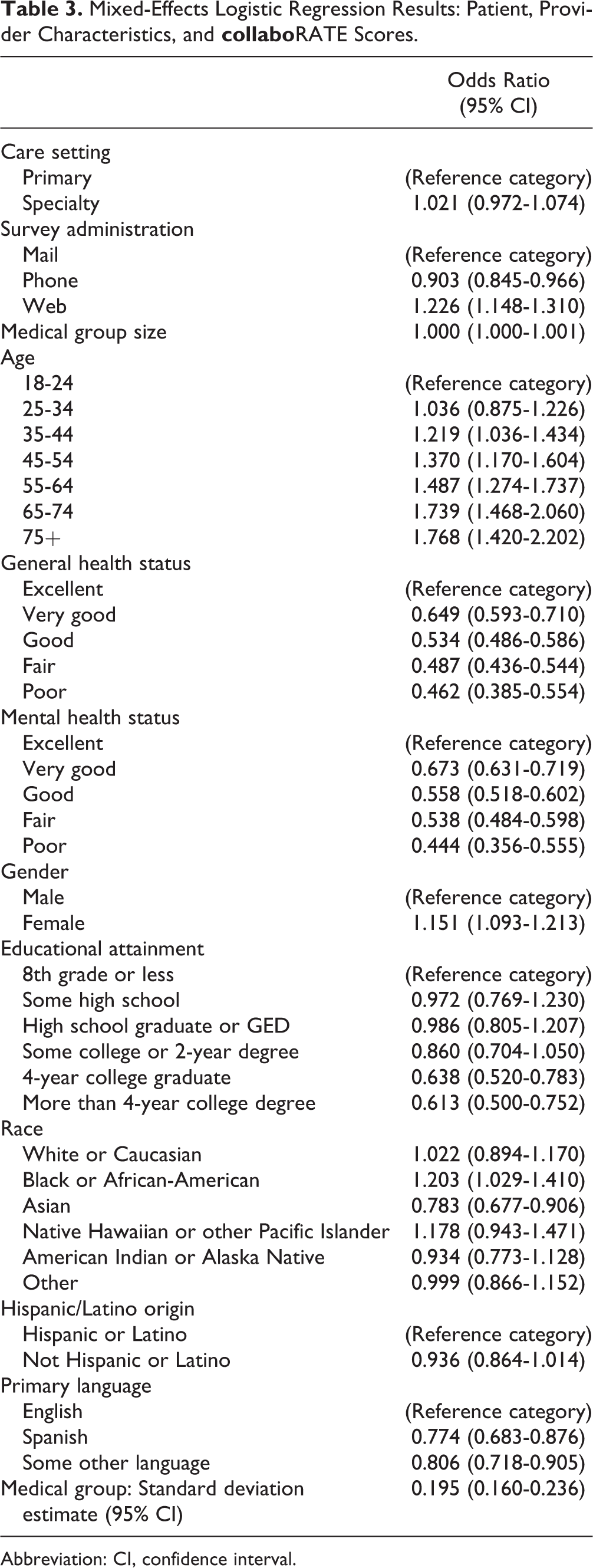
Abbreviation: CI, confidence interval.

Patient Characteristics and Overall collaboRATE Scores

Health status was also significantly related to

A,
Gender, educational attainment, race, and primary language were also significantly associated with

A, Unadjusted
Discussion
Key Findings
Even while controlling for patient and survey characteristics, we observed moderate variation at the provider group level as evidenced by the random-effect standard deviation of 0.195. This standard deviation approximately equates to a 95% confidence interval for the probability of obtaining a top
In analysis adjusting for available provider-level characteristics, several patient characteristics were associated with top
Strengths and Limitations
This study has several strengths, including its use of a large data set with SDM ratings from diverse patient populations across California. As a routinely administered survey used for performance measurement purposes, the PAS provides a unique look at routine and large-scale measurement of SDM. However, detailed information on clinicians and provider organizations was unavailable in this deidentified public data set; analysis of medical group characteristics was therefore very limited in this study. Our use of the number of survey responses as a proxy for medical group size assumes proportional sampling which may not have always been operationalized. Additionally, we lack observational data on SDM performance for the sample of clinical encounters rated in this study. We were therefore unable to strictly delineate differences in SDM behaviors across patient characteristics from other potential survey response biases. Finally, the fully California-based patient sample and 30% survey response rate may limit the generalizability of this study’s findings.
Results in Context
Our findings contribute additional insight into the role of patient and provider characteristics in SDM measurement among a large patient sample in a routine survey setting. This study finds evidence confirming existing literature with regard to less SDM reported by patients in poorer health (12,13). Interestingly, this relationship between poorer health and poorer
Our findings also support prior work demonstrating an association between limited English proficiency and poorer SDM (8,9,14,18). Although we do not have data specific to English proficiency in this study, we found that patients who speak a language other than English at home reported experiencing poorer SDM than those who speak English at home.
To our knowledge, this is the first US study to report a significant association between patient-reported SDM and Asian patient race as we observed lower
In contrast to other studies of SDM and clinical communication focused on patients’ racial identities (15,10), we did not find a significant difference in
Additionally, despite existing evidence for better SDM experience among patients with higher educational attainment (13,15,21), our findings depart from that prior literature as they suggest that patients with 4-year college degrees were least likely to give top
Case-mix adjustment is common in healthcare quality measurement and “uses statistical models to predict what each [provider’s] ratings would have been for a standard patient or population, thereby removing from comparisons the predictable effects of differences in patient characteristics that are consistent across [providers]” (29). This adjustment can be useful in provider performance profiling and pay-for-performance systems. Indeed, Paddison et al suggest that case-mix adjustment for performance assessment often has a minimal impact on most provider scores but “may meaningfully improve measurement of performance for practices with less typical patient populations, discouraging practices from ‘cream-skimming’ by avoiding enrolling patients who could be seen as ‘hard to treat’” (30). Incentivizing “cream-skimming” behavior through lack of case-mix adjustment for provider performance measurement threatens to exacerbate the disparities that performance measurement seeks to highlight and ameliorate. Based on our analysis, for provider performance profiling use cases, we recommend adjusting
However, unlike quality metrics based on biomarkers or patient-reported symptoms, SDM is a process that can be highly influenced by, and even dependent on, patient characteristics. Because SDM is defined by the clinician–patient interaction, it is unavoidably influenced by patients’ personal characteristics and dependent on clinicians’ skill in navigating healthcare conversations regardless of those characteristics. In fact, the possibility of “cream-skimming” implies that patient-reported estimates of SDM may hide even further inequities in the quality of SDM across patient groups (30). For this reason, we believe that many measurement use cases, such as quality improvement initiatives, do not require case-mix adjustment. In these situations where case-mix adjustment is not required, we suggest highlighting observed disparities and quantifying potential unobserved disparities in SDM across diverse patient populations to improve attention to inequities in patient experience that can have substantial downstream effects on patient outcomes. Further research evaluating the role of SDM in improving health disparities is therefore advised.
Conclusion
We found significant associations between
Supplemental Material
JPE_Supplemental_materials - Do collaboRATE Scores Reflect Differences in Perceived Shared Decision-Making Across Diverse Patient Populations? Evidence From a Large-Scale Patient Experience Survey in the United States
JPE_Supplemental_materials for Do collaboRATE Scores Reflect Differences in Perceived Shared Decision-Making Across Diverse Patient Populations? Evidence From a Large-Scale Patient Experience Survey in the United States by Rachel C Forcino, Marcus Thygeson, A James O’Malley, Marjan J Meinders, Gert P Westert and Glyn Elwyn in Journal of Patient Experience
Footnotes
Authors’ Note
R.C.F., M.T., A.J.O., M.J.M., G.P.W., and G.E. contributed to design of the work. R.C.F., M.T., A.J.O., and G.E. contributed to the acquisition, analysis, or interpretation of data. R.C.F. drafted the manuscript; M.T., A.J.O., M.J.M., G.P.W., and G.E. critically revised the manuscript. Our use of the deidentified data set was approved by the Pacific Business Group on Health and deemed exempt from further review by Dartmouth College’s Committee for the Protection of Human Subjects (study #31002).
Acknowledgments
The authors gratefully acknowledge Grace Lin, MD, for facilitating PAS data access.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Glyn Elwyn is a developer of the
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
