Abstract
Health-care decisions in the Philippines are widely affected by various factors such as family, community, health-care access, and educational attainment. We designed a questionnaire to evaluate patient views at the University of the Philippines–Philippine General Hospital colorectal multidisciplinary clinic to identify factors that contribute to continued follow-up at the colorectal multidisciplinary clinic. A total of 128 patients, 62% of whom were being treated with curative intent participated in the study. We found that trust in their physicians, presence of family support, and affordability of treatment were factors highly valued by patients consulting at the clinic.
Introduction
Colorectal cancer (CRC) is potentially curable if addressed in a timely manner by both the patient and health-care team (1). Appropriate follow-up improves patient outcomes as patients who have been lost to follow-up after initial work-up and treatment return later with more advanced disease, if at all they come back to their physician (2).
Studies concerning follow-up among cancer patients in developing countries have identified several socio-demographicand disease-related factors that influence patient follow-up (3). Health practices and decisions in the Philippines are similarly affected by the interplay of these factors (4). Identifying patient preferences contributing to continued follow-up is the focus of this study.
Methodology
This study was approved by the University of Philippines Manila Research Ethics Board. It was conducted in the weekly colorectal multidisciplinary clinic (MDC) of the Philippine General Hospital, the teaching hospital of the University of the Philippines. The health-care team in the MDC is composed of medical oncologists, colorectal surgeons, radiation oncologists, and oncology nurses.
A questionnaire was designed to allow CRC patients to identify factors that they felt contributed to continued follow-up at the clinic. The questionnaire was based on reasons commonly elicited by physicians from CRC patients at the clinic during check-up that the latter felt encouraged their continued follow-up. In answering the questionnaire, participants could identify multiple factors if they so wished. Also, patients could enumerate other factors not included in the list.
All adult patients seen at the colorectal MDC were eligible for inclusion in this study. The inability of a patient to self-administer the study questionnaire would not preclude participation since a companion or member of the study team might assist in its administration if the patient so requested. Refusal to participate was the only exclusion criterion.
After informed consent was obtained, patients completed a structured questionnaire on sociodemographic and clinical parameters. Information regarding stage, performance status, and treatment intent were obtained from patient records by the study investigators. Provisions were made for the patient to answer the survey in private within the clinic.
Reasons for refusal to participate included: being too busy, others stated that they were unable to answer due to poor eyesight, and some mentioned that they were unable to read. These reasons were given despite being informed that provisions for assistance in answering the questionnaire were available. Some patients said that they were simply not interested in participating in the study. Descriptive statistics (mean, standard deviation) were employed in the analysis of the data obtained from respondents.
Results
Patient Characteristics
A total of 128 patients were included in the analysis for this study (Table 1). The mean age was 53 years old. Fifty-one percent of the respondents were male. Most were married, and more than 70% reported being unemployed at the time the survey was taken. Disease was most often locally advanced or metastatic at the time of study participation. Notably, clinical staging could still be incomplete at the time of recruitment and were therefore noted as “stage pending.’ Sixty-two percent of patient were being treated with curative intent.
Characteristics of Study Participants.

Factors Contributing to Follow-Up
Respondents identified the 3 most common factors that influence continued follow-up: trust in treating physician, adequacy of family support during treatment, and affordability of treatment at the clinic (Figure 1). The two patients who chose other factors in the questionnaire both identified improved clinic workflow (eg, shorter lines and more organized queuing) as one of the factors contributing to follow-up.
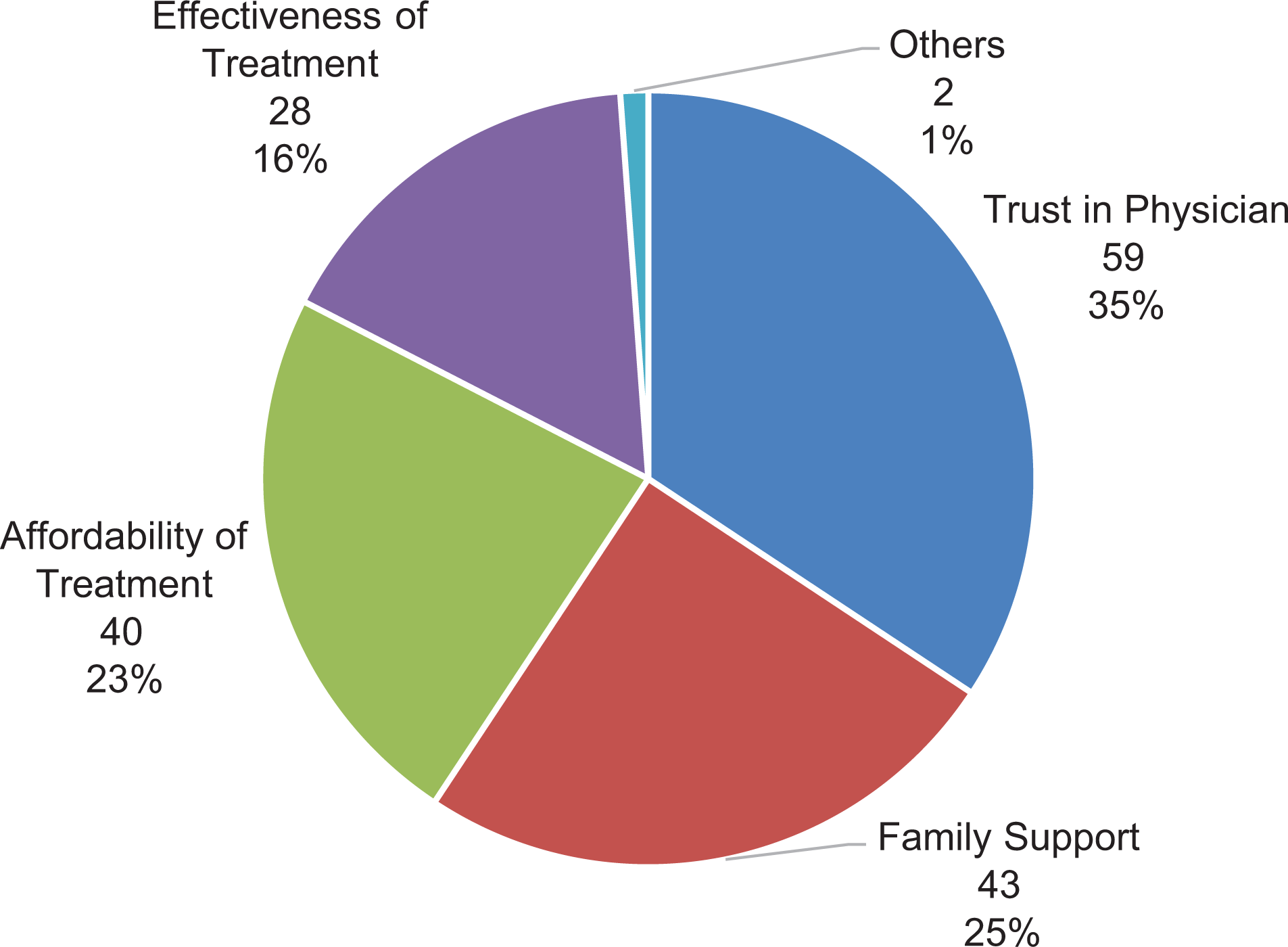
Breakdown of factors identified by patients as beneficial to their continuing follow-up.
Discussion
Trust is imperative to the patient–physician relationship (5,6). This concept was consistent in our study which showed that patient’s trust in their physician had emerged as an important factor behind continued follow-up. Trust serves as bridge between patient and health-care system. The physician's ability to convey competence, honesty, and care contribute to patient trust. Moreover, of these three, the ability to demonstrate care had the largest impact on promoting trust (7).
The effectiveness of the health-care team in educating patients is vital in reinforcing patient trust and consequently, enhancing medical follow-up (8). It has been observed that obtaining information on their condition is a means by which cancer patients cope with their disease (9). A review of patient–physician trust in China has shown that asymmetry in medical information between patient and physician leads to patient distrust in their caregivers (10). The patient’s need for information is highest during the initial stages of treatment. As treatment progresses, the need for additional information diminishes with time, provided that the plan of treatment is unchanged (11).
Family support has been identified by participants as the second most important factor behind continued follow-up. In the Philippines, family is a critical source of financial and social support. This is particularly true when the cancer patient is unemployed. Thus, the cost of care is supported in whole or in part by other family members. Meanwhile, social support translates to providing advice, participating in decision-making, and accompanying the patient to medical appointments. Most patients in this study have advanced-stage cancers necessitating greater family support. A study done in Malaysia, which shares cultural similarities with the Philippines, has shown similar observations (12).
Financial constraints have been identified as a consistent cause of loss to follow-up (3). This observation is consistent with results of this study, wherein patients identified affordability of treatment as vital in ensuring patient follow-up. The cost of cancer treatment and its availability to those who need it continues to challenge cancer care globally (13,14).
Limitation of the Study
The purpose of the study was to identify factors that CRC patients believed promoted their continued follow-up. This study presented the views of a population of patients seen in a public hospital and might not be representative of all Filipino CRC patients. In addition, the questionnaire used had not been validated across different patient demographic groups. A validation study should include a more diverse population and would best be conducted across multiple centers.
The low response rate (<50%) potentially skewed the results of this study. Concerns regarding privacy at the clinic might be one factor contributing to this finding. Another issue would relate to the frantic nature of the MDC. If a patient did not hear his name called out in the clinic, he could miss seeing his doctor. In this context, a survey could serve as an unwelcome distraction. A study conducted in the General Medicine clinic at the University of the Philippines–Philippine General Hospital also reported a response rate below 50%. In that study, the authors identified the emergent nature of a patient’s condition, patients being in a hurry, and frank refusal as reasons why patients did not participate in the study (4). The last two factors mentioned mirror the reasons given by patients who refused to participate in this study. As a remedy, nonresponders could be contacted again later to answer the questionnaire. It would also be informative to obtain a profile of patients, who refused to participate.
Patient follow-up is governed by an interplay between patient and health-care system factors. Patient factors include economic constraints, comorbidities, adverse treatment effects, and lack of motivation for treatment. Health-care system issues meanwhile include inadequate health facilities and services, limited competency of medical staff, resources to improve patients’ adherence rates, long clinic queues, and shortage of physicians (3). This study, although the first to report on preferences of Filipino CRC patients looks only at patient factors, specifically their preferences with respect to the medical care they hope to receive.
It is important to point out that patient’s preferences evolve during treatment. Following a population of patients prospectively and noting why some patients continue to follow-up while others become lost to follow-up will provide more dynamic insight into patient preference and its impact on follow-up.
Conclusion
This study has shown that CRC patients believe that trust in their physician, presence of family support, and affordability of treatment are important factors that underpin follow-up with their health-care provider. It highlights these as areas of focus during interactions with patients. Future studies need to account for the evolving preferences of patients as they proceed with their treatment.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
