Abstract
The United Kingdom Office of National Statistics population estimates that 10 million people are aged 65 years and older, of which some would be considered frail. This is conceptualized as a complex progressive loss of physiological and social function. In order to establish and evaluate appropriate services, feedback tools designed for this patient group have begun to take greater importance, which the Acute Frailty Network has been developing using experience-based design. These tools focus on the experience of frail patients in the settings of accident and emergency and the acute medical unit. An analysis of data from 12 hospitals was used to look at the common emotions and comments expressed at the key touchpoints. A total of 609 respondents were used in the analysis, revealing that patients expressed mostly positive experiences. The areas with the most negative emotions and comments were in the domains “being admitted,” “first assessment,” and “preparing to leave hospital.” We would recommend that future quality improvement projects focus in improving the communication standards around the admission and discharge process.
Keywords
Introduction
The Aging Demographic and Frailty
The 21st century has seen a shift in population demographics in Europe; 16% of the population are above the age of 65 years, with a predicted rise to 22% by 2031 (1). The UK Office of National Statistics estimates for 2017 suggests that 10 million people are 65 years and older, with 3 million greater than the age of 80 (2,3). A proportion of this older cohort would be considered “frail” (4), the concept of progressive physiological and social function loss due to complex interactions of physical comorbidities or functional limitations (5). This consequently results in a weakened resilience to events that stress the human body, with an increased risk of morbidity and mortality (6).
Frailty has an established correlation with mortality and morbidity outcomes from hospital admissions. In total, 5% to 10% of accident and emergency (A&E) attendees and 30% of patients admitted to an acute medical unit (AMU) are classified as frail (7). Within the frailty spectrum, those considered severely frail are more likely to die within 3 years compared to the nonfrail, independent of comorbidities (8). Patients admitted with “frailty syndromes” (falls, immobility, new incontinence, and confusion, among others) are at a greater risk of institutionalization, increased admission duration, and disability (9,10).
The Role of Feedback in Health Care Services
The National Health Service (NHS) presently emphasizes patient empowerment to their health management in an approach known as patient-centered care (11). Elderly medicine has seen a drive to promote patient-centered care to improve the quality of life for their patients; their feedback is vital in determining appropriate service redevelopment (12,13). Patient feedback is being accepted as integral to transforming health care services (14). The 2007 Darzi report emphasized the need for the NHS to deliver care that focuses on the patient, of which patient feedback forms an important role (15). There are several ways to collect patient feedback, including surveys, interviews, and focus groups, among others. No specific feedback tool confers an advantage over the others, but different feedback styles can complement one another in shaping health care services (16,17).
Experience-Based Design
Experience-based design (EBD) is one modality for patient feedback to be delivered to health care services and professionals (18). Experience-based design identifies key moments (known as touchpoints) from patient interactions with health care services (19). Experience-based design elevates patient feedback and emphasizes their involvement in co-designing health care services to meet the population needs (20). It has been recognized by the NHS as an effective tool to improve the care delivered to patients (21).
Several studies have analyzed the feedback of patients and their experiences in the acute sector. One study compared patient perspectives on the quality of care in A&E between England and the Netherlands across 6 domains (22). The study noted that England had a greater variation in health care experiences for the general population and elderly individuals in comparison to the Netherlands, although it noted that England had individual departments with the best health care experiences as well. The experience of wait times and perceptions of doctors and nurse are the major differences here, highlighting opportunities for improvement. A report on the NHS emergency department survey in 2016 used feedback from stratified samples of around 45 000 patients of their experience in A&E. It noted that 75% of respondents were confident in the medical staff and 77% felt involved in their treatment. Sixteen percent felt that the medical staff did not explore their concerns, and 27% felt this was partially explored (23).
Only 1 systematic review analyzed the experience of older patients in the emergency department and drew its conclusions from 5 papers (24). Completed in 2012, it noted that older patients generally reported more negative experiences in waiting times and expressed a greater need for physical and psychological support, alongside improving information about their experiences. These papers and surveys identify that more research is needed to understand the experience of the frail older population within the acute sector and identify potential strategies to improve their hospital experience.
The Acute Frailty Network and Integration of EBD
The Acute Frailty Network (AFN) is a large-scale improvement collaborative organization established in 2015 to support frail older people to return home sooner and healthier. Improvement efforts are focused in the initial 72 hours of acute care across, A&E, assessment units, and acute frailty units (25). The AFN emphasizes patient involvement in projects to codesign services and improve the quality of their experience.
To promote patient involvement, the AFN has developed an anonymized feedback tool based on the concept of EBD, which was designed in collaboration with staff and patients at the Leicester Royal Infirmary and Royal Berkshire Hospital. The tool was developed with a target “persona” or example patient in mind—an 83-year-old female normally residing indoors with a carer who lives with them. The tool comprises 8 touchpoints covering the aspects important to patients from admission to discharge. Hospitals can use a paper-based or digital version of the EBD tool to collect patient experience data; the digital version allows automatically generated graphical representation of the data and the ability to group feedback into the specific touchpoints. A summary of the touchpoints is represented in Figure 1.

Diagram showing the 8 touchpoints used in the experience-based design feedback tool.
The majority of hospitals working with the AFN elected to use the EBD feedback tool to collect data on the patient perspective of their services. Although the data have been analyzed at a local level by individual hospitals, it not been aggregated and analyzed from a national perspective. This study could identify common themes across former hospital cohorts that future ones might seek to drive changes early on in their involvement with the AFN program.
Aim
To collate and analyze data from the digital version of the EBD feedback tool used by hospitals that collaborated with the AFN, looking at common emotions and comments expressed by the frail older population.
Method
Participants
This study included 609 participants identified as frail by hospital staff. These participants were nonelective emergency patients discharged from the A&E or the AMU of 12 hospitals who took part in the AFN program.
Procedure
Suitable participants were identified by staff working in the emergency department or AMU. Once the participant had consented, a staff member would complete the EBD tool with the participant or the participant would complete it independently. No descriptive information was collected about the participant. Both web- and paper-based versions of the EBD tool were used depending on resource availability. Tablets were used to collect web-based responses (Figure 2).

Example of the digital experience-based design app interface designed by the Acute Frailty Network.
Analysis
The paper-based EBD responses were scanned and sent to the AFN for inputting into the web-based tool. Following data collation, the information was extracted into Microsoft Excel. The responses at each touchpoint were ranked in order of popularity and placed into Pareto charts. This was repeated for the responses to all touchpoints combined. The percentage of positive, neutral, and negative responses at touchpoints were calculated and displayed graphically. Qualitative comments for each touchpoint were collated and reviewed by the team for commonly occurring themes.
Ethics and Consent
No ethical review was undertaken or required as the work was performed as a service development and evaluation (Table 1).
Number of Responses Provided by Each Site Included in the Study.

Discussion
The data from the feedback tool suggest that patients generally express positive experiences when admitted to A&E or AMU. Graph 1 shows that the domain “dignity and respect” had the most positive emotions expressed at 91.7%, whereas the domain “being admitted” had the lowest number of positive emotions expressed at 69.3%. The domain “first assessment” had 75.9% of respondents express positive emotions, whereas “preparing to leave hospital” had 76.0%.

The proportion of respondents expressing happy, indifferent, or sad emotions across each touchpoint.
The domain with the highest volume of negatively expressed emotions was “being admitted” at 10.8%, which may relate to the disorienting process of admission that patients experience when entering hospital (4); 3.6% of respondents expressed negative emotions in the domain “preparing to leave hospital,” which may represent focal concern for the frail older population on their readiness to return to their home environment (26).
Graph 2 shows the frequency of emotions selected across all touchpoints. The data show that 72.9% of patients expressed positive emotions, while 13.4% expressed negative emotions. The 3 most commonly expressed negative emotions were “confusion,” “worry,” and “unhappiness,” which potentially indicate issues in communication within patient the journey through A&E and AMU. Issues pertaining to communication have been identified in previous studies on patient experience in the acute setting (Graph 2) (27,28)

The frequency of emotions selected by patients across all touchpoints (minimum >10 responses).
In the domain “being admitted,” 69.3% of respondents expressed positive emotions, while 10.8% expressed negative emotions. Graph 3 shows that the most commonly used negative emotions were “confusion,” “worry,” and “frightened.” The negative emotions may reflect issues around communication in the acute setting, which have been identified in previous studies of patient experience in A&E (27). Other studies have also identified communication and psychological support as key themes for improvement in the acute setting (24,29).

The frequency of emotions expressed by patients in the touchpoint “being admitted.”
The domain “first assessment” shows that 75.9% of respondents expressed positive emotions. Graph 4 shows that the emotions “cared for” and “supported” were the most frequently expressed; 5.0% of respondents expressed the negative emotion “confusion” and 4.7% expressed “worry.” Again, this may reflect issues around communication in the acute settings of hospitals. An analysis of the comments left by patients indicated a level of staff unawareness around the patient’s issues and that patients did not feel listened to. Previous systematic reviews across the entire age demographic note communication as a key obstacle to patient satisfaction with services (24,29).

The frequency of emotions expressed by patients in the touchpoint “first assessment.”
The “communication” touchpoint notes that 82.4% of respondents felt their interactions with the medical staff to be positive, with Graph 5 displaying that the most commonly used positive words were “good” and “happy”; 3.4% of respondents used negative emotions about their experiences, with “confused,” “unhappy,” and “misunderstood” being the most prevalent words selected. The comments left by patients suggest that there remain pertinent issues that are not being explored by the staff, potentially due to the time constraints faced in A&E and AMU (30).
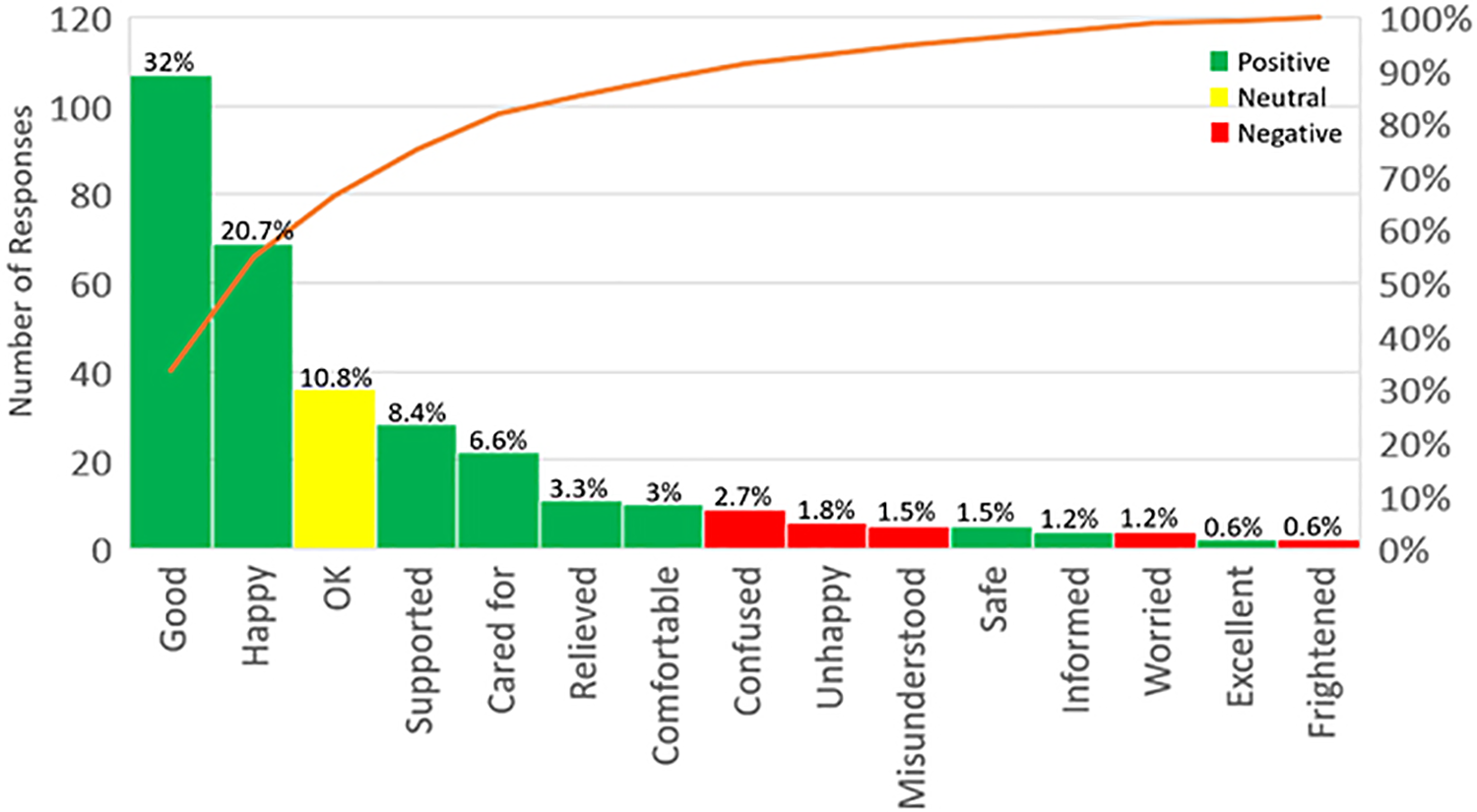
The frequency of emotions expressed by patients in the touchpoint “communication.”
The feedback from patients in the domain “preparing to leave hospital” notes that 75.9% of patients expressed positive emotions, while 3.6% expressed negative ones. Graph 6 shows that the most common negatively used emotions were “worry,” “frightened,” and “unhappy,” which reflects the concern the frail older population perceive on managing safely at home or being able to rely on the hospital support systems (31). The patient comments note frustration in their lack of involvement on discharge planning and insufficient communication with external care providers.

The frequency of emotions expressed by patients in the touchpoint “preparing to leave hospital.”
The analysis of patient feedback in this study identifies communication as a key barrier to their experience. This reinforces previous studies in the acute setting, which highlights communication to patients as an area for improvement and their perceived lack of engagement in their management plan (27,28). Other studies have also identified psychological support and communication as an issue in the acute setting requiring improvement (24,29). The 2016 Emergency Department Statistical Release from the Care Quality Commission notes that 16% of patients did not feel their concerns were explored or 27% feeling these were partially explored (23). This study on the EBD feedback tool adds further weight to the overall need for clinical services to improve the quality of communication with the frail older population (15).
Reading the comments left by patients across all the touchpoints, communication was a common theme for patients. Many expressed negative experiences of poor communication between themselves, their family, and health care staff and were more frequently expressed at the touchpoints “being admitted,” “first assessment,” “communication,” and “preparing to leave hospitals.” The A&E staff undoubtedly face pressures in providing swift care to all their patients—improving the interactions between staff and patients could potentially reduce the confusion and worry in a patient’s acute admission process (27,31).
Recommendations
Clinicians engaged in service development within the A&E and AMU may wish to review their communication models with the frail older population and evaluate their efficacy. They may look at ways to improve the engagement of the patients and families in their management planning to improve their quality of care. The solutions are likely to be multifaceted, but general suggestions may include simplified leaflets on their condition or discharge planning and environmental changes that result in a lower level of distress expressed by patients on their initial admission (32). A recommendation would be the coinvolvement of patients in designing the solutions, which is a key principle of the EBD approach to redesigning services (18,20). Quality improvement projects should focus on the initial aspects of the admission process for frail older patients in order to improve their experience and quality of service. They may also work on improving patient care and may wish simplifying their discharge processes so that patients can assimilate the information more effectively.
The results from this article have identified general issues around communication with the frail older population, which adds to the previous studies on patient feedback (8,22). Future studies should look to evaluate improvement projects that hospitals have carried out for the older adult services and the perceived impact on their care. This would enable clinicians to determine which service developments provide the greatest impact for older adult care. It may be of interest to look at stratifying feedback and the perceived quality of care between frailty cohorts or between those living in their own homes versus nursing or residential care homes. Qualitative research data such as focus groups and interviews could provide valuable insights on how hospitals could redesign their services to meet the needs of the older adult population.
Strengths and Limitations
The main strength from the study is that the feedback and results are derived exclusively from the frail older population. Previous studies into patient satisfaction have collected views and opinions from an entire age range of users, with a smaller proportion of respondents from the older population (22). This can make it difficult to identify the specific concerns that this individualized subgroup may have that could be different from other age groups. Previous NHS surveys have also sampled from the entire age spectrum with a smaller focus on the frail older population, and the systematic literature reviews have made recommendations for more research into feedback from the frail older population (23,24,29).
A few limitations should be noted when reviewing the results from the analysis. The collated feedback represents a patient’s experience that could be purely based on their admission in A&E, their admission to an AMU, or their experience through both an A&E and AMU. Although the digital EBD feedback tool can be divided into individual hospitals, when collated nationally, there is no ability to distinguish between A&E and AMU. The collated feedback would still be representative of a patient’s acute experience, so it can still be valuable in understanding their experience of an acute care pathway.
The majority of hospitals collected feedback at the start of their collaboration with the AFN to gain an understanding of where patients felt their journey could be improved, before setting out to make those changes. There are a small proportion of hospitals collecting feedback after making improvements, which was included in the collation of the data. We have still used these data to understand the patient perspective of their care in the acute setting.
Conclusion
The data collected by the EBD feedback tool suggest that the acute sector of NHS hospitals provide satisfactory service from the patient perspective, although there remain key touchpoints where patients feel more acutely distressed. The top 3 areas where the most negative feedback was expressed were in “being admitted,” “first assessment,” and “your comfort.” The most 3 most commonly expressed positive emotion across all the touchpoints were “good,” “happy,” and “cared for,” while confusion, worry, and unhappiness were the 3 most commonly expressed negative emotions, albeit to a smaller extent.
Our recommendations from the analysis of the data would be that hospitals looking to improve the acute care of the frail older population should adopt an early focus on raising the standards of communication with this patient group. The key areas to focus on would be at the point of admission, their first assessment, and discharge, as these were the areas where patients felt the most distressed and the highest incidences of negative experiences about communication occurred. Each hospital site is likely to develop its own solution to these issues, although other sites may benefit from sharing the data on both successful and unsuccessful projects, which is exemplified in the breakthrough collaborative approach undertaken by the AFN. We would also recommend continuing to use and analyze patient feedback (through the use of the either EBD tool or individually developed solutions) to help indoctrinate their experience into designing a system that places a greater focus on the patient.
The study performed builds on the previous work by researchers on analyzing the feedback from patients who attend emergency departments. It focuses on a specific subgroup of the frail older population, which has only seen limited analysis from a small number of papers. We would suggest that future work in the feedback of the frail older population considers adding qualitative data such as focus groups and interviews to provide more heterogeneous data for synthesis in the future.
Experience-based design is an effective way of undertaking codesign with patients and carers. It provides staff with a different perspective on the service and transforms improvement plans to ensure that they are patient centered. The power of having an insight into way patients feel using our services cannot be underestimated.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
