Abstract
Background:
Posthospital syndrome is associated with a decrease in physical and cognitive function and can contribute to overall patient decline. We can speculate on contributors to this decline (eg, poor sleep and nutrition), but other factors may also contribute. This study seeks to explain how patients experience hospitalization with particular attention on what makes the hospital stay difficult.
Design:
Qualitative interview study using grounded theory methodology.
Setting:
Single-site academic medical center.
Patients:
Hospitalized general medicine patients.
Measurements:
Interviews using a semistructured interview guide.
Results:
We recruited 20 general medicine inpatients from an academic medical center. Of the participants, 12 were women and the mean age was 55 years (range = 22-82 years). We found 4 major themes contributing to the hospital experience: (1) hospital environment (eg, food quality and entertainment), (2) patient factors (eg, indifference and expectations), (3) hospital personnel (eg, care team size and level of helpfulness), and (4) patient feelings (eg, level of control and feeling like an object). We discovered that these emotions arising from hospital experiences, together with the other 3 major themes, led to the patients’ perception of their hospital experience overall. We also explore the role that patient tolerance may play in the reporting of patient satisfaction.
Conclusions:
This article demonstrates the factors affecting how patients experience hospitalization. It provides insight into possible contributors to posthospital syndrome and offers a blueprint for specific quality improvement initiatives. Lastly, it briefly explores how patient tolerance may prove a challenge to the current system of quality reporting.
Keywords
Introduction
The experience of hospitalization is not easy (1 –3). Patients often leave the hospital less able to care for themselves and in a state of health worse than their baseline (1,2,4). This period of potential decline, termed posthospital syndrome, places patients at a higher risk for a range of adverse events, including unsteadiness, readmission, and death (2,5,6). Some of these can be attributed to their illnesses, but that does not explain the entire functional and/or cognitive decline sometimes seen in hospitalized patients. We can make educated guesses based on literature clinical experience about factors that might contribute to this decline: Sleep, nutrition, hospital provider, depersonalization, and mood can all be negatively impacted by hospitalization (7,8). However, other factors may come into play. It has also been shown that health outcomes are positively correlated with metrics that can assess the patient experience, indicating that a crucial part in improving quality may lie in addressing the hospital experience (9 –13).
Currently, the health-care experience is often assessed with surveys. Since their implementation, CAHPS Hospital Survey and Press-Ganey have worked to standardize data reported from hospitals about quality (14). This has allowed for meaningful comparisons across hospitals as well as incentivized accountability and quality improvement (14,15). For example, HCAHPS provides important data about hospital quality and patient satisfaction (14). However, these questions are closed-ended and responses are restricted to a 4-point Likert scale; they only skim the surface of the patient experience. Instead of a question such as “what made it challenging to sleep?” patients are restricted to responding to a yes or no question about if the hospital was quiet (14,15).
As medical professionals, we can speculate on what patients may want improved about hospitalization. Some studies have been conducted about particular areas, such as service handovers and food quality (16 –18). However, this focused approach does not allow for new themes to emerge and instead assumes that the focus area is one which patients would like improved. Others have gone one step further to discuss with patients what they would like to improve (19,20). A limitation of these studies was that participants were interviewed after discharge and thus may not remember everything that occurred during their hospitalization. Qualitative literature on patient-derived areas for improvement is lacking. We conducted this study to gain a better understanding of how patients view their hospitalization with particular focus on the factors that patients feel make their hospital stay difficult.
Methods
Study Design
This was a single-site qualitative interview study. We chose this technique with several thoughts in mind. Qualitative studies are ideal when the primary aim is to gain a deeper understanding of a scenario or phenomenon (21). We chose to implement interviews in order to glean patient-derived data to explain the processes and emotions associated with hospitalization, a technique well supported in qualitative research methodology (21). We anticipated this technique would provide us with the most robust data that we could then use to form a model of the hospital experience that accurately represented the data. We interviewed general medicine patients from June to August 2016 with particular interest in understanding the parts of hospitalization that were difficult for patients.
Participants
Our participants were recruited from an academic medical center located in a large, Midwestern city. The hospital has 585 beds and approximately 29 000 admissions per year. We included inpatients on general medicine teams, who were at least 18 and thought to be within 2 days of discharge. We excluded patients who were unable to speak English or were unable to give informed consent. We included patients from both housestaff and hospitalist Advanced Practice Provider (APP) teams.
Instrument
Based on a literature review, we designed a semistructured interview guide to explore the hospital experience. It contained a variety of open-ended and more direct questions with the goal of obtaining an in-depth view of what patients perceived as important during their hospitalization. The interview process began with asking open-ended questions such as “walk me through your hospital stay. What were some of the major things that happened?” The interviewer made notes and went back to elements of the patient’s story to probe more deeply about crucial elements (as seen in the Supplementary Interview Guide). The interview guide was designed to allow patients to talk through their experience in its entirety and to also steer the conversation if they felt something was crucial to their hospital stay, a process that is well supported in the literature (21). Additional direct questions focused on specific topics such as comfort, meals, hospital workers, and what they felt should be improved were addressed depending on the amount of detail the original open-ended questions solicited. Patients were continuously probed further by questions such as “can you tell me more about that? What was that like? How did that make you feel?” This process was created to reveal patient-generated areas for improvement as well as to assess hypotheses about areas suspected to be difficult. We shared the guide with experts in doctor/patient communication, medical education, and hospital medicine and made adjustments based on their feedback. As the interviews progressed, we adapted the interview guide to explore emerging themes in subsequent interviews.
Data Collection
To perform the interviews, we obtained the team lists and went team by team in a random order to identify eligible patients. Each patient on the selected team list was assigned a number. We then spoke with either a resident or attending physician to identify eligible patients. If there were no eligible patients or the team could not be reached, we moved on to the next team. Using a random number generator, we randomly selected the order in which eligible patients were approached.
After completing 9 interviews, we switched to purposive sampling to ensure a broad age, gender, and racial representation of patients. Specifically, we switched techniques to account for racial diversity in our sample. This was achieved using the process described above, just substituting purposive sampling of eligible participants. We chose to begin with random sampling in order to achieve a diversity of participants and increase the generalizability of our results (22). We then used purposive sampling in order to ensure a diversity of our sample, anticipating that different participant demographics would lead to differences regarding hospital experience, thus providing more diverse, comprehensive data (22).
Patients completed a brief demographic survey. Interviews were audiotaped using a Zoom H4n Handy Recorder and then transcribed verbatim. We began data analysis while continuing to collect data to allow us the chance to explore new themes in subsequent interviews. We reached thematic saturation after completing 12 interviews and completed 8 more interviews before ending data collection (Table 1). We held a larger meeting with experts in physician/patient communication, medical education, and hospital medicine after half of the interviews were complete in order to gain outside opinions about how the analysis was progressing, and we made some adjustments to the interview guide as a result. This study was approved by this academic center’s institutional review board.
Saturation Grid.

Analysis
We used a grounded theory approach to the data analysis and interviewed patients until we achieved thematic saturation (23). Grounded theory does not use a previous theory or model to analyze and interpret data. Rather, it uses the data obtained to develop a model that accurately represents the findings (24). Transcripts were analyzed using NVivo qualitative data analysis software. The transcripts were first analyzed using open coding to identify distinct concepts that appeared in the transcripts. Open coding is a process in which there are no preformed ideas of exactly what the codes will be, they are derived from the transcripts themselves (24). Two of the study team members met on a weekly basis to discuss codes and themes as they were emerging during the interview process. We then developed a code book with codes and definitions and examined the breadth of experiences within each code (Table 2). After open coding was complete, we used axial coding to develop larger themes and concepts that allowed us to develop a framework. We began by organizing similar codes together to assess their relationships. Some were denoted as “daughter” codes within the NVivo software as they were better explained in their association with their “parent” code (Table 2). For example, the original codes “helpful personnel” and “unhelpful personnel” became daughter codes of hospital personnel. After parent and daughter codes were identified we began to look for relationships between codes, organizing codes into subthemes. The relationships, or lack thereof, between subthemes allowed for organization of major themes and areas of overlap between major themes. Our work in the form of major themes and subthemes are representative of substantive-level theory about the patient experience. Each theme and subtheme were derived from the data to represent specific areas of the patient experience (24). We presented preliminary findings to a group of experts (including clinicians and researchers) to further refine our axial coding. To assess for agreement, one investigator identified the chunks of text coded and marked these on an uncoded copy of 3 randomly selected transcripts. Overall agreement was calculated by the number of chunks that had any coding agreement (considered if the coders agreed on at least one code for the chunk) divided by the total number of chunks. Coding agreement was 89%.
Coding Scheme for Transcript Analysis.

Results
We interviewed 20 patients. The mean age was 55 (range = 22-82); 8 were men; 4 were African American, and there was a wide range of employment and education status (Table 3). Direct, comprehensive chart review was not performed as part of the original study protocol. However, several patients self-reported the reason for their admission during the interview. These reasons for admission reflected a wide range of internal medicine topics such as cystic fibrosis exacerbation, abdominal pain, bowel obstruction, and mechanical fall (Table 3).
Participant Demographics.a

an = 20.
A model representing the patient experience emerged from the analysis (Figure 1). The model consisted of 4 major themes (Table 4): environmental factors, patient factors, hospital personnel factors, and patient feelings. Each major theme was composed of several subthemes. There were also several subthemes that overlapped between major themes. The interaction between the environmental, patient, and hospital personnel themes and subthemes seemed to influence the feelings patients developed throughout their hospitalization and therefore contributed to their perception of their hospital stay overall. In the following paragraphs, we highlight the main themes and selected subthemes.

Patient perceived factors and the patient experience of hospitalization.
Major Themes, Their Subthemes, and Representative Quotes.
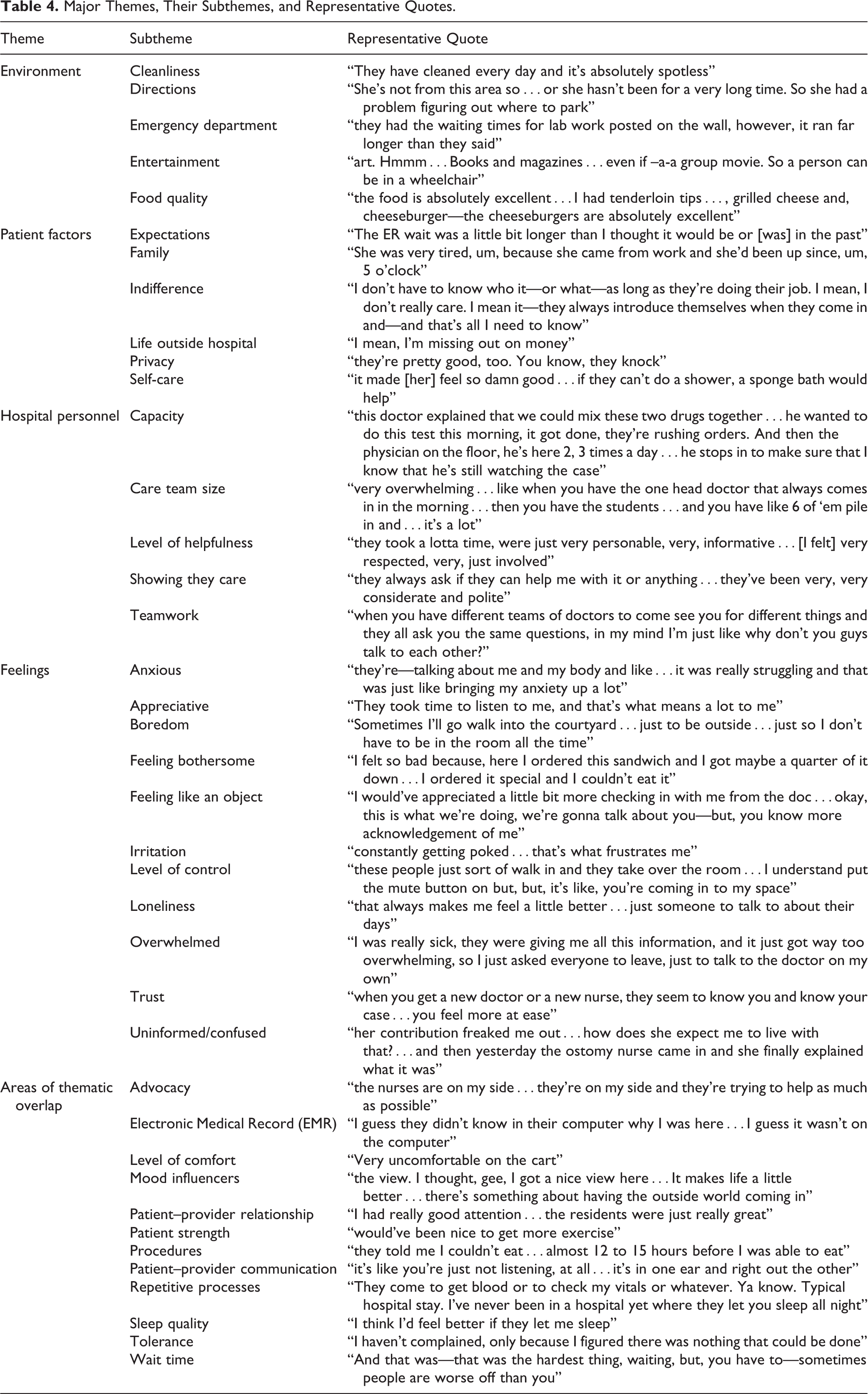
Environment
The first major theme was the hospital environment, which focused on aspects of the hospitalization that were intrinsic to the hospital itself. When discussing the hospital environment with patients, 5 subthemes emerged: cleanliness, directions, emergency department, entertainment, and food quality.
Patient Factors
The second major theme was patient factors. This theme included factors brought to the hospitalization by patients themselves. The subthemes were patient expectations, family, indifference, life outside the hospital, privacy, and self-care.
A commonly discussed subtheme was the concept of indifference. We defined this as when patients did not have a preference about a situation or about how something was done. For example, when asked if they would like more information about their hospital providers, one patient replied, “I don’t have to know—as long as they’re doing their job. I mean, I don’t really care…they always introduce themselves when they come in and—and that’s all I need to know.”
Hospital Personnel
Hospital personnel reflected the attitudes and work of the hospital workers. Subthemes within this theme included capacity, care team size, level of helpfulness, showing they care, and teamwork.
Care team size referred to the number of people on the team taking care of the patient. This number was dependent on whether the team was resident or Physician Assistant/Nurse Practitioner based. Feelings toward the care team size varied widely. For example, several patients described large care teams as, “very overwhelming…when you have the one head doctor that always comes in in the morning…then you have the students…and you have 6 of ‘em pile in…it’s a lot.” However, it was also common for patients to enjoy or feel indifferent about having a large care team.
Feelings
Feelings was the theme that included emotions that patients experienced throughout their hospitalization as a result of the interplay between the hospital environment, their personal patient factors, and the hospital personnel. Patients described a wide range of emotions including anxiety, appreciation, boredom, feeling bothersome, feeling like an object, irritation, level of control, loneliness, overwhelmed, trust, and uninformed/confused.
One subtheme frequently discussed was level of control. Patients described frustration due to the minimal control they have over their schedule. Others described their frustration from their lack of personal space stating, “these people just sort of walk in and they take over the room…I understand put the mute button on but, it’s like, you’re coming in to my space.”
Overlapping Subthemes
Several aspects of hospitalization fit within more than one theme. Level of comfort, for example, was not only dependent on the hospital environment but also on the hospital personnel. Another area of immense overlap existed between patients and personnel and included areas such as patient–provider communication.
Another area of overlap was between environment, patients, and hospital personnel. A topic within this area of overlap was patient strength. Some patients described how they felt that being able to move about the hospital, either for exercise or entertainment, played a pivotal role.
A final area of overlap was the concept of tolerance. This subtheme emerged as a combination of patient expectations, hospital environment, and personnel factors. This subtheme describes when patients settled for something because they believed that is the way it is in the hospital, even though they were dissatisfied. One of the earliest examples emerged when a patient remarked, “what do you do?” while describing that the patient in the neighboring room was loud and kept him awake for most of the night.
Discussion
This study aimed to understand the patient experience, paying special attention to aspects of hospitalization that are particularly difficult. We discovered that hospital factors, patient factors, and personnel factors played a role in determining the feelings that patients experienced during their hospitalization. The feelings ranged from anxious, to appreciative, to feeling out of control. The model emphasizes the importance of hospital personnel in setting the tone for patients’ experiences. Patients wanted their care providers to be kind to them. This may seem obvious, yet it reinforces that patients want their providers to demonstrate they care and to know that they are working as hard as they can on their behalf (25).
In addition to explaining the hospital experience, this model provides insight into possible contributors to posthospital syndrome. Some factors such as lack of sleep or food quality have been studied or suggested as factors that contribute to posthospital syndrome (17,19). This study sheds light on other factors that may also contribute, such as the opportunity for self-care, mood influencers, patient strength, and advocacy. Since patients described self-care activities (eg, showers, essential oils) as calming or making them feel better, improving the ease with which patients can perform these activities may help patients feel better sooner. Patient strength also seems to play an important role. Current literature emphasizes the importance of early mobility in intensive care unit patients (26). Similarly, encouraging appropriate mobility and exercise may prove beneficial not only for physical health but also for patient morale and self-efficacy.
The concept of tolerance was intriguing. We identified tolerance when patients responded to questions with phrases such as “it’s fine.” We ultimately defined it as when patients settled for something because they believed that is the way it is in the hospital, even though they were dissatisfied. Upon hearing these responses early in the interview process, we were uncertain how to characterize them. In order to further investigate, we added probes about what ideal might look like; this allowed patients to offer feedback or suggestions. As we continued to acquire and analyze data indicating that patients did not enjoy certain aspects but did have suggestions on how to improve them, the tolerance concept separated itself from indifference. Where indifference suggests that patients truly do not have a preference regarding a specific topic, tolerance emerged as a concept where patients accept the norm but do have an underlying belief regarding the manner in which something should be done. For example, while discussing staff entering the room at night, one patient stated that “they gotta do that…but you know, that [gets] kinda annoying sometimes.” When probed further about what his ideal night would look like, he suggested that “twice a day” would help him to sleep better. Further probing with a subsequent patient produced this statement: “I haven’t complained, only because I figured there was nothing that could be done.” These responses indicate that patients may have more to say than they initially let on or even realize, and that with the appropriate conversation they may be able to provide suggestions for improvements that may otherwise be undiscovered.
Understanding that patients view hospitalization through a lens of tolerance led us to wonder how well satisfaction surveys truly discern quality. If patients are viewing and assessing their hospitalization through a lens of tolerance, are the data being reported on satisfaction surveys accurately reflecting the patients’ experiences? Our data suggest that sometimes patients are not considering the possibility that things could improve, which may also impact survey results. Moreover, this may suggest that our current method of assessing quality is not well rounded and may need improvements in order to ensure maximal patient-centered improvements.
This concept of tolerance also presents unique challenges when approaching hospital leadership to discuss change. If surveys do not accurately reflect how patients feel, it could prove challenging to convince leadership that change is needed. Additionally, if patients realize they can expect more from hospitalization, they may begin completing surveys based on what their ideal situation would be. This could lead to a decrease in satisfaction scores that would then require a response from hospital leadership. Leadership may be hesitant to explore what ideal would look like for patients. However, we believe that eliminating tolerance and striving for ideal deserve serious consideration and future study.
There are several limitations to this study. First, this was a single-site study with a sample size of 20, which limits the generalizability of our results. Although the sample size and obtained patient demographics make these findings somewhat preliminary, we did achieve thematic saturation and we used both random and purposive sampling to obtain a diversity of participants. Second, our results are qualitative and we are therefore unable to describe them in a quantitative manner. We can say, however, that these are issues present in the hospital and that we should address them. Third, the study was restricted to English-speaking participants only as we did not have the resources to provide translation services. Non-English-speaking patients have their own unique challenges and may have unique stressors related to hospitalization. However, we used a combination of random and purposive sampling to ensure maximum diversity.
One area we did not address in this study is actual posthospital recovery. In other words, we did not follow patients home and reinterview them to understand their recovery. If they experienced posthospital syndrome, how long did it take for them to recover? A future study could address how patients’ posthospital recoveries are impacted by factors such as those identified in this study.
Limitations notwithstanding, this study adds depth to our understanding of the patient experience and provides data that we can use to improve hospital care. Because this was a single-site study, further exploration at an additional site would be a reasonable next step. The implications of these results are numerous. Most markedly, the conceptual model provides a framework from which to draw areas for targeted quality improvement initiatives. For example, future initiatives encouraging the maintenance of a home routine (ie, bathing, brushing teeth) as well as timed coordination of nightly interruptions (eg, bloodwork, vitals, wound checks) could lead to drastic improvement in patient sleep quality, thus improving multiple aspects of hospitalization. This study also provides patient-derived data on important areas of hospitalization that could be used to develop a more patient-centric instrument to measure patient satisfaction. It also suggests that future instruments may need to include methods to address patient tolerance in order to gain a deeper and more comprehensive assessment of patient satisfaction. Whether through targeted quality improvement initiatives or larger policy changes, this study will serve as a framework to produce meaningful change for patients and improved quality for all.
Supplemental Material
Supplemental Material, Interview_Guide - The Hospital Experience Through the Patients’ Eyes
Supplemental Material, Interview_Guide for The Hospital Experience Through the Patients’ Eyes by Haverly J Snyder and Kathlyn E Fletcher in Journal of Patient Experience
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Ms. Snyder received a Young Scholar in Hospital Medicine award from the Society of Hospital Medicine to fund her summer work on this project.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
