Abstract
The following fictional case is intended as a learning tool within the Pathology Competencies for Medical Education (PCME), a set of national standards for teaching pathology. These are divided into three basic competencies: Disease Mechanisms and Processes, Organ System Pathology, and Diagnostic Medicine and Therapeutic Pathology. For additional information, and a full list of learning objectives for all three competencies, see http://journals.sagepub.com/doi/10.1177/2374289517715040. 1
Keywords
Primary Objective
Objective CBV3.1: Drug-induced Vasculitis. Describe how a drug-induced vasculitis depends on a functioning immune system. 1
Competency 2: Organ System Pathology. Topic: Cardiovascular-Blood Vessels (CBV): Learning Goal 3: Vasculitis 1
Secondary Objective
Objective IMM1.4: Autoimmune Diseases. Discuss the clinical presentation and pathophysiologic bases of autoimmune diseases including the efficient use of laboratory tests to make a definitive diagnosis and manage the disease. 1
Competency 3: Diagnostic Medicine and Therapeutic Pathology. Topic: Immunology (IMM): Learning Goal 1: Pathogenesis, Diagnosis, and Treatment of Immunologic Disorders 1
Patient Presentation
A 42-year-old woman presents to urgent care with complaints of a red rash on her legs. Her past medical history is significant for new-onset hypertension, type 2 diabetes mellitus, and hyperlipidemia. Current medications include metformin and hydrochlorothiazide. The patient reports that she was recently started on hydrochlorothiazide by her primary care provider due to elevated blood pressures. She tolerated the medication well, but within a week began to notice a raised red rash on her lower extremities. She reports no associated symptoms such as itching, burning, or paresthesia. She has no pain. She has never had this happen before.
Diagnostic Findings, Part 1
Vital signs are within normal limits. Physical examination reveals nonblanchable palpable violaceous papules on the bilateral lower extremities distributed evenly across the anterior and posterior lower and upper leg and extending superiorly toward the gluteal region (Figure 1). Cardiac examination reveals a regular rate and rhythm with a normal S1 and S2. There is no friction rub or murmur. Respiratory examination reveals normal work of breathing with breath sounds clear to auscultation bilaterally. The abdominal examination demonstrates no pain to palpation, normal bowel sounds, and no hepatomegaly or splenomegaly. The musculoskeletal examination is negative for joint swelling, erythema, or arthritis. Muscle strength is 5/5 throughout with no paresthesia.
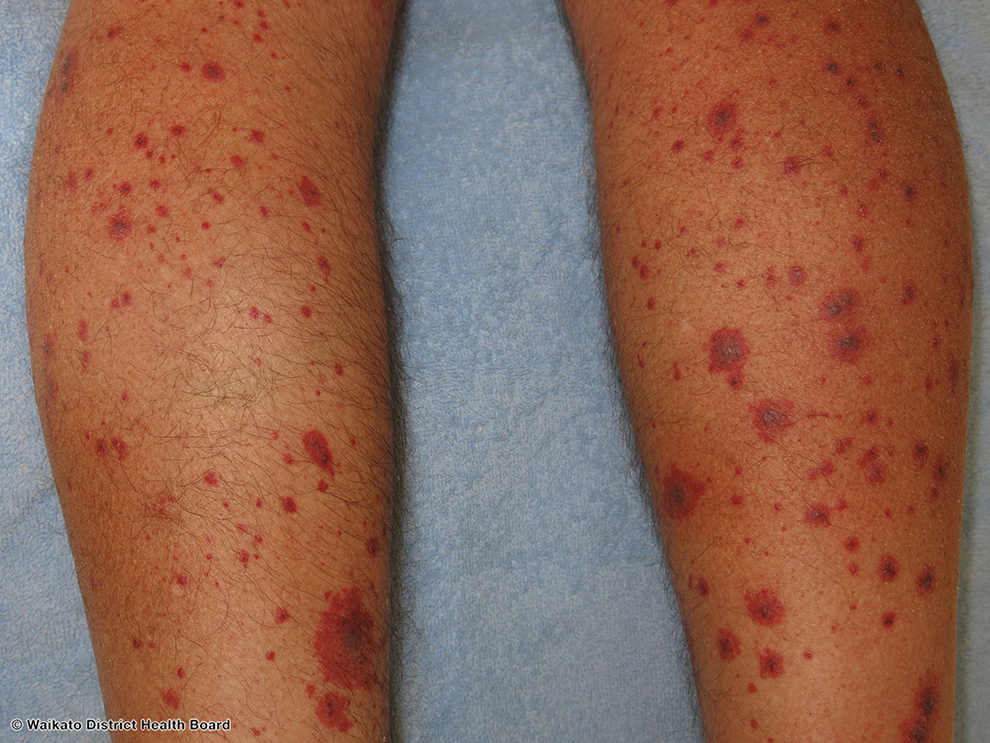
Violaceous palpable papules are present on the bilateral lower extremities. Note the varying sizes of the lesions as well as the apparent difference in age. This indicates an evolving rash. This figure was reproduced with permission from DermNetNZ. Republished under (CC BY-NC-ND 3.0 NZ). Oakley A. cutaneous small-vessel vasculitis. DermNetNZ. 2016. https://www.dermnetnz.org/topics/cutaneous-small-vessel-vasculitis/.
Question/Discussion Points, Part 1
Discuss the Differential Diagnosis for the Presenting Lesion
Palpable purpura, raised, nonblanching violaceous lesions, presenting in an otherwise well woman are concerning for vasculitis. Consideration of the cause is key to identifying the correct diagnosis and treatment. There are several common causes of vasculitis including urticarial vasculitis, septic vasculitis, and autoimmune vasculitides such as hypersensitivity (leukocytoclastic) vasculitis, Henoch-Schönlein purpura (immunoglobulin A vasculitis), granulomatosis with polyangiitis (GPA), eosinophilic GPA (EGPA), and microscopic polyangiitis (MPA). 2,3 Systemic immune complex vasculitides such as systemic lupus erythematosus, rheumatoid arthritis, and Sjögren syndrome can also present with purpuric lesions. Additionally, it is important to consider thrombocytopenia and its respective causes; however, this will usually present with a nonblanchable petechial rash versus the palpable purpura seen here. 3 Primary infection of the skin such as cellulitis or erysipelas would be unlikely to present with palpable purpura; however, they are important to consider. Less common causes to consider include hematologic malignancies which could manifest in similar lesions (Sweet syndrome), and Kaposi sarcoma in the setting of severe immunodeficiency such as acquired immunodeficiency syndrome (AIDS). 4
Due to her age and lack of other findings including systemic symptoms, the greatest likelihood for the cause of her rash would be a hypersensitivity drug reaction to her recent use of hydrochlorothiazide.
What Is the Mechanism for Hypersensitivity Vasculitis?
Hypersensitivity vasculitis is an inflammatory autoimmune vasculitis. It requires a triggering molecule to complex with circulating immunoglobulins. The complexes deposit within small blood vessel walls leading to an inflammatory response within the blood vessels themselves. 2,5 The inciting molecule is often a drug or microbial molecule, each accounting for approximately 20% of cases of hypersensitivity vasculitis. 2 The complex deposits activate the complement system causing the recruitment of neutrophils from the bloodstream. 5 The neutrophils release their contents locally causing inflammation and cellular destruction. The presence of neutrophils and any remaining neutrophil debris (leukocytoclasis) in the vascular walls is known as “leukocytoclastic vasculitis.” The inflammation and cellular destruction subsequently leads to blood vessel leakage. 5 This leakage is responsible for the raised red lesions that are characteristic of hypersensitivity vasculitis. 5 The skin lesions are nonblanchable due to the extravasated red blood cells. Contrast this with rashes caused by blood vessel dilation, in which blanching the rash essentially clamps the blood vessel, causing the disappearance of the lesion. 2,3
What Further Testing Is Indicated?
Due to the wide array of causes of vasculitis, it is important to rule out systemic disease in this patient. It would be prudent to check a complete blood count (CBC) with differential, complete metabolic panel (CMP), antinuclear antibodies, anti-cyclic citrullinated protein antibodies, rheumatoid factor, and the antineutrophil cytoplasmic antibodies (ANCA). 6 These will effectively measure for systemic involvement, such as in systemic lupus erythematosus, rheumatoid arthritis, Sjögren syndrome, and the ANCA vasculitides (GPA, EGPA, and MPA) as her age and gender place her at high risk for systemic autoimmune disease. 2,7 Additionally, these will also help rule out hematologic malignancy, immunodeficiency, and infection. Measuring complement levels could also be considered; however, these will be nonspecific as they are often lowered due to immune complex deposition, but they may add to the overall diagnostic picture. 5 If the clinical history is consistent with a risk for hepatitis, then the respective hepatitis panels should also be performed. 7 It is also important to rule out visceral organ damage due to systemic vasculitides, which can be measured with the above tests and urinalysis and followed up with more targeted testing or imaging if abnormal results return. 2,7 And of course, erythrocyte sedimentation rate (ESR) should be performed to evaluate for inflammation. Electrolyte imbalances should be checked within the CMP.
Biopsy of the presenting lesion would be indicated in this patient as it would be both demonstrative of the underlying pathological process and required for a final diagnosis of hypersensitivity vasculitis. 7 This can be done at the same time that the other labs are drawn if the clinical suspicion of vasculitis is high.
Diagnostic Findings, Part 2
Due to the high suspicion for hypersensitivity vasculitis, hydrochlorothiazide is stopped immediately. Laboratory results include a normal CBC with differential, CMP, and urinalysis. Erythrocyte sedimentation rate is mildly elevated at 26 mm/h (reference range for females, 0-20 mm/h). Antinuclear antibodies, rheumatoid factor, and ANCA are all negative.
Question/Discussion Points, Part 2
What Is the Significance of the Lab Results?
The lab results above demonstrate a lack of systemic involvement from her vasculitis. This makes a systemic autoimmune disease highly unlikely. Also, there is no evidence of infection making microbial antigens doubtful as a triggering factor. Her ESR was mildly elevated which is very likely due to the localized inflammation within the small blood vessels. In cases of hypersensitivity vasculitis, the ESR is often one of the only abnormal lab values, although it is not elevated in all cases. 7
What Findings Would Make You Concerned That This Was Not a Hypersensitivity Vasculitis and Further Causes Should Be Investigated?
Any signs of systemic illness in this patient should make you question a diagnosis of hypersensitivity vasculitis. Hypersensitivity vasculitis is localized to the blood vessels and visceral involvement is rare. 2 An elevated white blood cell count should give cause to investigate infectious and other autoimmune causes. A positive test result on any autoimmune antibody or any abnormal urinalysis results should prompt you to identify the source, as hypersensitivity vasculitis is unlikely to cause abnormalities in these labs.
How Would Your Differential Diagnosis Change If This Were An Immunocompromised Patient?
A vasculitis, as described in the pathophysiology above, is inherently dependent upon a functional immune system to produce the relevant pathology. 2,5,7 An immunocompromised patient would be very unlikely to exhibit this type of hypersensitivity reaction and consideration must be made for infectious and malignant causes as these patients are at greater risk. Primary skin infections should be quickly ruled out, as delays in treatment could result in systemic spread and death. Consideration should be made for Kaposi sarcoma which can cause violaceous lesions in immunocompromised individuals and is classically associated with AIDS. 8 Hematologic malignancies are associated with several blood abnormalities. These can cause discoloration and/or bruising of the skin that may be mistaken for purpuric lesions such as in Sweet syndrome. 4
Diagnostic Findings, Part 3
A biopsy of a lesion is performed to confirm the diagnosis. To ensure diagnostic accuracy, an early papule is identified and confirmed with the patient that it had been present for less than 48 hours. Direct immunofluorescence (DIF) is also performed (not shown).
Question/Discussion Points, Part 3
Describe the Biopsy Findings. Do the Biopsy Findings Support or Refute a Diagnosis of Hypersensitivity Vasculitis?
The biopsy demonstrates neutrophilic perivascular inflammation. Also present are signs of fibrinoid necrosis and erythrocytes outside of the blood vessel wall (Figure 2).
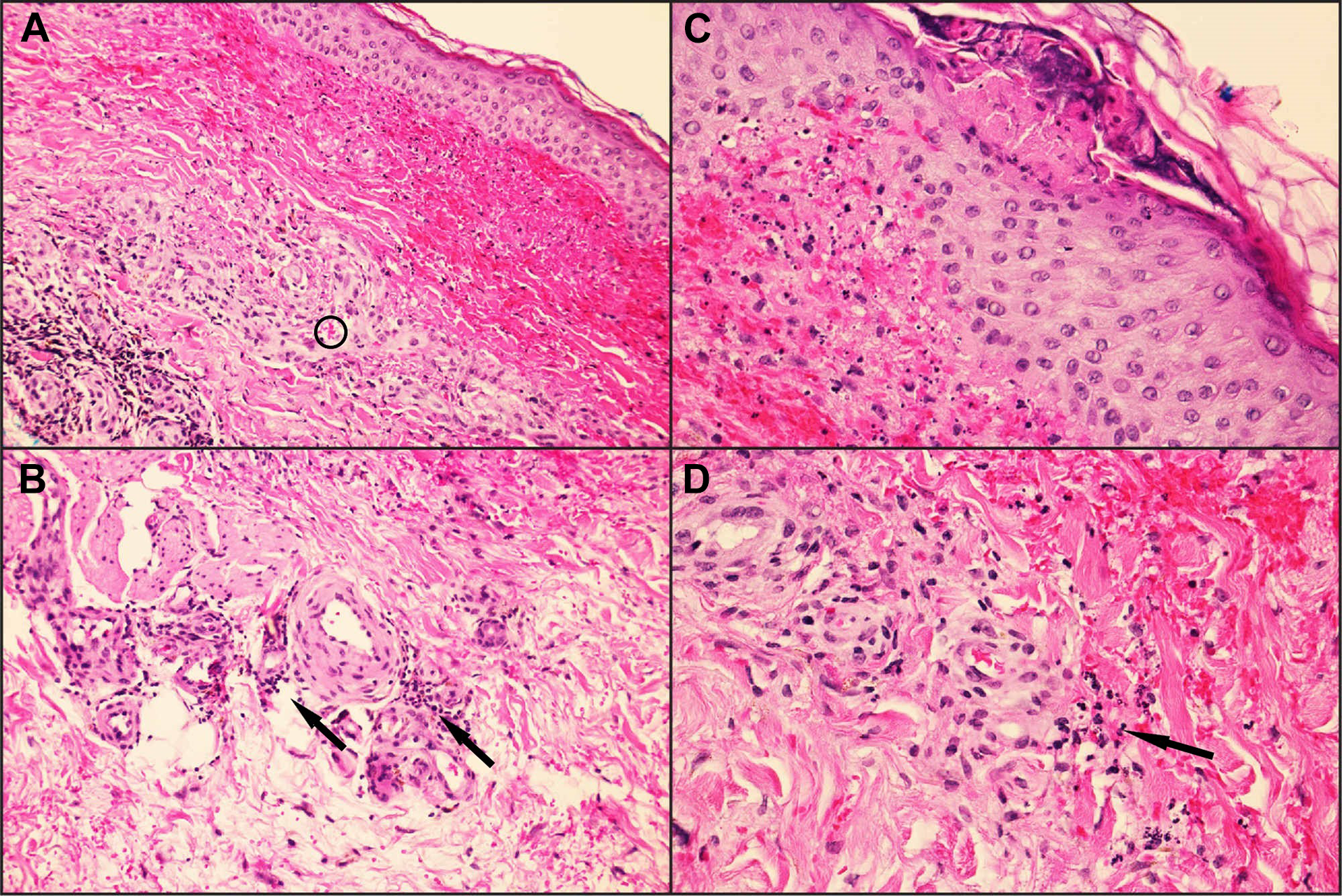
(A and B) A biopsy demonstrating perivascular neutrophilic infiltrate (arrows) with extravasated red blood cells (circle), indicative of leukocytoclastic vasculitis. (C) A biopsy of the surface lesion demonstrates disruption of the epidermis with underlying protein debris and hemorrhage. (D) An inflammatory infiltrate (arrow) invading the postcapillary venules of the papillary dermis (hematoxylin-eosin stain). Magnification (A ×200, B ×400, C ×400, and D ×400). This figure was reproduced with permission from cureus. Republished under (CC-BY 3.0). Bourji K, Marchitto M, Kuppalli S, Dang J, Dogra B. Case report: drug-induced leukocytoclastic vasculitis in a patient with classic Ehlers-Danlos syndrome. Cureus. published online October 15, 2019. doi:10.7759/cureus.5915.
This biopsy confirms that the lesions are leukocytoclastic vasculitis. There are no bacterial organisms present indicating the absence of infection. There is also no sign of malignancy. To investigate further, the biopsy should be sent for DIF staining to identify the deposition of immune complexes. Direct immunofluorescence would demonstrate immune complexes and complement C3 within small vessel walls. 3,5,7 A negative result would not rule out hypersensitivity vasculitis, but a positive result can be confirmatory, especially in an individual with new-onset disease. 6
What Other Drugs Are Known to Commonly Trigger Hypersensitivity Vasculitis? Which Microbial Infections Are Commonly Implicated?
Although there is no definitive list of which drugs can trigger hypersensitivity vasculitis, broad categories have been implicated as common triggers. Even so, it is paramount that recent changes in drug regimens should always be considered when encountering a new-onset vasculitis. Common triggering drug classes include antibiotics, nonsteroidal anti-inflammatory drugs (NSAIDs), and thiazide diuretics as was the case here. 5 In the case of suspected vasculitis due to antibiotics, the diagnosis becomes more complicated due to the possibility of the infection itself as an inciting factor.
Microbial causes of hypersensitivity vasculitis can be bacterial or viral. However, the most commonly implicated pathogens are Streptococcal and Staphylococcal infections. 5 When attempting to differentiate an antibiotic eruption as opposed to a microbial eruption, it is essential to remember that the timeline of the microbial eruption would likely be in the post-infectious stage, as this is the point at which the body has developed the necessary antibodies to form the circulating immune complexes. 2,5,7
Briefly Describe the Treatment Approach for This Patient
The cornerstone of treatment in hypersensitivity vasculitis is the removal of any offending agents and an appropriate adjustment of therapy. 2,6 Any underlying infections must be addressed. Further therapy is guided by the patient’s condition and presentation. Mild disease may be managed conservatively with leg compression and elevation. 6 For more severe disease or in cases that do not resolve with conservative treatment, steroid tapers may be considered. 2,6 For disease recalcitrant to steroid therapy, consider specialist referral. Rarely, disease-modifying antirheumatic drugs can be used in severe cases of hypersensitivity vasculitis. 6
The prognosis of hypersensitivity vasculitis is excellent. Spontaneous resolution of these lesions occurs in 90% of patients within a few weeks to months. 6 The mortality rate is approximately 2%; however, this is due to cases with visceral involvement, damaging vital organs. 6
In all cases of hypersensitivity vasculitis, close follow-up is recommended within 2 to 4 weeks and subsequently as needed on a case-by-case basis. It is important to confirm the appropriate resolution of the lesions, as lesions that do not resolve may be due to another, the more dangerous underlying cause that was not caught on the initial labs. 6 Lesions that do not resolve warrant further investigation and/or a repeat of the initial labs. Ensure that patients are aware that they should call or return to the clinic if they experience a worsening of symptoms, presentation of new symptoms, or if they are having any difficulties with the treatment plan. In these cases, treatment may need to be altered or alternative diagnoses considered.
Teaching Points
Hypersensitivity vasculitis is a leukocytoclastic vasculitis resulting from the circulation of an inciting antigen.
The differential diagnosis for hypersensitivity vasculitis is broad including medication changes, infectious agents, autoimmune vasculitides, malignancy, and immunodeficiency.
The inciting antigen may be a microbial fragment or a drug. Commonly implicated drug classes are antibiotics, NSAIDs, and thiazide diuretics.
Circulating immunoglobulins complex with these antigens to form circulating immune complexes which deposit within small venules near the skin, particularly in the lower extremities.
Activation of the immune response, particularly the complement system results in local inflammation, destruction of the vasculature, and extravasation of blood and blood products.
Hypersensitivity vasculitis, as shown by its pathophysiological mechanism, is dependent upon a functional immune system.
The diagnosis of hypersensitivity vasculitis is driven by the patient’s history and presentation. Biopsies are performed to confirm the diagnosis.
The treatment of hypersensitivity vasculitis is generally conservative but driven by the patient’s presentation. Any offending agents should be removed. Underlying infections, if present, should be treated. Steroids may be considered for severe cases.
All patients should have close follow-up within 2 to 4 weeks to confirm the improvement of the lesions.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
