Abstract
The following fictional case is intended as a learning tool within the Pathology Competencies for Medical Education (PCME), a set of national standards for teaching pathology. These are divided into three basic competencies: Disease Mechanisms and Processes, Organ System Pathology, and Diagnostic Medicine and Therapeutic Pathology. For additional information, and a full list of learning objectives for all three competencies, see http://journals.sagepub.com/doi/10.1177/2374289517715040.1
Keywords
Primary Objective
Objective: RS4.4: Asthma. Compare and contrast the clinicopathological features and causes of asthma and describe the morphologic changes and consequences that result in airflow obstruction.
Competency 2: Organ System Pathology; Topic: Respiratory System (RS); Learning Goal 4: Obstructive Diseases of the Lung.
Patient Presentation
A 13-year-old male presents to the emergency department with acute onset of breathlessness. He has had recurrent, episodic attacks of wheezing, cough, dyspnea, itchy red eyes, nasal discharge, stuffiness, and occasional chest tightness for past 2 years. Initially, his symptoms were relieved by short-acting β-blocker, albuterol. However, the frequency and the severity of the symptoms have increased for the past 1 month with the patient waking up with these symptoms. He has a history of eczema. His family history is significant for asthma in his mother.
Diagnostic Findings
Physical examination reveals respiratory rate of 22/min and diffuse wheezing all over the lung fields. Pulmonary function test (PFT) shows FEV1/FVC (forced expiratory volume at 1 second [FEV1]/forced ventilatory capacity [FVC]) of 0.65. Forced expiratory volume at 1 second is 60% of predictive and post-bronchodilator therapy the FEV1 increases to 74% of predictive. Chest X-ray is normal.
Question/Discussion Points
What Is the Diagnosis Based on Clinical Findings and Pulmonary Function Test?
Clinical presentation (recurrent, episodic attacks of wheezing, cough, dyspnea, itchy red eyes, nasal discharge, stuffiness, and chest tightness), and PFT findings (FEV1/FVC of 0.65, FEV1 is 60% of predictive and post-bronchodilator therapy the FEV1 increases to 74% of predictive) are consistent with the diagnosis of asthma. Diagnosis of asthma can be confirmed if the evidence of airway obstruction is seen on PFT, especially if it is reversible with a bronchodilator as seen in our case.
What Type of Lung Disease Is Asthma, and What Are Other Diseases in That Category?
Obstructive diseases of lung are characterized by an increased airflow resistance due to partial or complete obstruction of airway at any level from the trachea to the respiratory bronchioles. In contrast, restrictive diseases show reduced lung parenchymal expansion leading to decreased total lung capacity. Obstructive pulmonary diseases can be distinguished from restrictive diseases based on pulmonary function tests. Obstructive disorders show decreased maximal airflow rates during forced expiration, usually expressed as the FEV1 over the FVC. Obstructive pulmonary diseases generally show a FEV1/FVC ratio of less than 0.7 contrasting with restrictive diseases that are characterized by a proportionate reduction in both total lung capacity and FEV1, resulting in normal FEV1/FVC ratio.
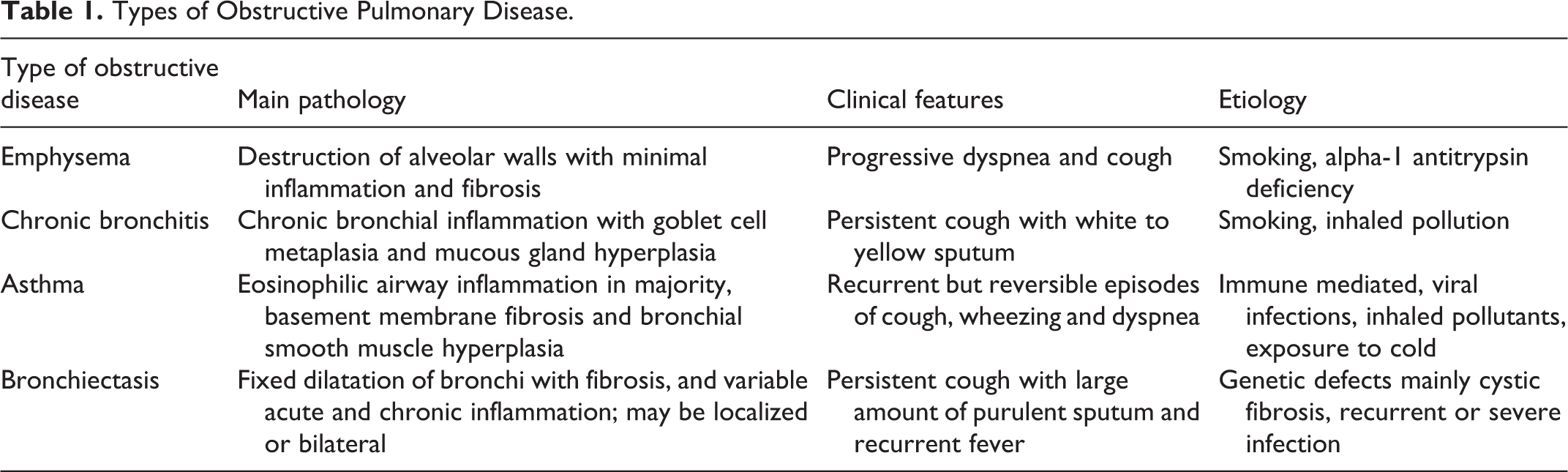
Asthma, emphysema, chronic bronchitis, and bronchiectasis are common obstructive lung diseases. Each has distinct clinical and pathologic characteristics (Table 1). 2 Emphysema and chronic bronchitis are frequently grouped as chronic obstructive pulmonary disease (COPD), as the majority of patients share features of both. Also, both entities are triggered by cigarette smoking. Asthma can be distinguished from COPD by the presence of reversible bronchospasm.
Types of Obstructive Pulmonary Disease.
What Are the Differential Diagnoses Based on Clinical Findings?
Cystic fibrosis and noncystic fibrosis bronchiectasis
Both cystic fibrosis (CF) and diffuse non-CF bronchiectasis present with chronic cough and abundant sputum production that is atypical for an asthmatic child. Furthermore, recurrent chest infections are seen in CF patients from a very young age. Patients with non-CF bronchiectasis frequently report productive cough with sputum expectoration, respiratory distress, growth retardation, and night sweats.
Primary ciliary dyskinesia
Primary ciliary dyskinesia (PCD) commonly involves lower airways. It may present as chronic asthma which is usually unresponsive to maintenance therapy. Patients with unexplained respiratory distress at birth and recurrent upper and lower respiratory infections should be screened for PCD.
Protracted bacterial bronchitis
It presents as chronic cough (lasting ≥ 4 weeks) not responding to asthma treatment and require a prolonged (minimum of 2 weeks) course of antibiotic treatment.
Airway foreign body
The sudden onset of respiratory symptoms is more suggestive of an accidental foreign body aspiration than a sudden onset of asthma. It is more common in young children. The patient may present with choking, persistent cough, unilateral and monophonic wheeze, and respiratory distress.
Vocal cord dysfunction
It is characterized by inappropriate adduction of the vocal cords during inspiration induced by exercise, psychological stress, or local irritation like reflux. It frequently coexists with asthma but is unresponsive to bronchodilator therapy. Patients present with breathlessness, intermittent aphonia or dysphonia, choking sensation, chest tightness or pain, difficulty swallowing, and throat clearing. Direct visualization of the vocal cords by endoscopy is the gold standard for the diagnosis. Abnormal shape of the inspiratory loop is seen on spirometry consistent with a variable extrathoracic obstruction.
Bronchiolitis obliterans
Bronchiolitis obliterans occurs secondary to viral and mycoplasma pneumonia infections. It frequently presents as persistent wheezing, rather than paroxysmal symptoms. Computed tomography scan shows a characteristic mosaic pattern and air trapping.
What Is Asthma?
Asthma is a chronic, episodic, inflammatory disorder of the airways associated with bronchoconstriction and airflow limitation that is at least partly reversible, either spontaneously or with treatment. The hallmarks of the disease are as follows
2
: ○ Increased airway responsiveness resulting in episodic bronchoconstriction ○ Inflammation of the bronchial walls ○ Increased mucus secretion
How Does It Present Clinically?
Patients with asthma present with dyspnea, cough, and wheezing due to sudden episodes of bronchospasm.
2
According to the latest National Asthma Education and Prevention Program guidelines, correctly diagnosing asthma is important by establishing the following
3
: ○ Episodic symptoms of airflow obstruction or airway hyperresponsiveness ○ Airflow obstruction or symptoms are at least partially reversible ○ Exclusion of alternative diagnoses.
What Is Acute Severe Asthma (Formerly Known as Status Asthmaticus)?
It is defined as a state of unrelieved attacks of asthma, formerly known as status asthmaticus. It is rare and may prove to be fatal. Usually, it is seen in patients with a long history of severe asthma. Patients may be asymptomatic between episodes. 2
What Are the Risk Factors of Asthma?
Certain factors contribute to the development of airway hyper-reactivity, leading to asthma. These are given as follows
2
: ○ Environmental allergens ○ Exercise, hyperventilation ○ Viral respiratory infections ○ Exposure to cold ○ Aspirin or nonsteroidal anti-inflammatory drug (NSAID) hypersensitivity ○ Inhaled air pollutants such as smoking, sulfur dioxide, ozone, and nitrogen dioxide. Occupational exposure including fumes (epoxy resins, plastics), organic and chemical dusts (wood, cotton, platinum), gases (toluene), or other chemicals (formaldehyde, penicillin products)
What Are the Different Types of Asthma?
Asthma is classified as atopic or non-atopic based on presence or absence of an evidence of allergen sensitization. It may also be categorized according to the triggers that lead to bronchoconstriction. Table 2 shows various types of asthma. 2
Types of Asthma.
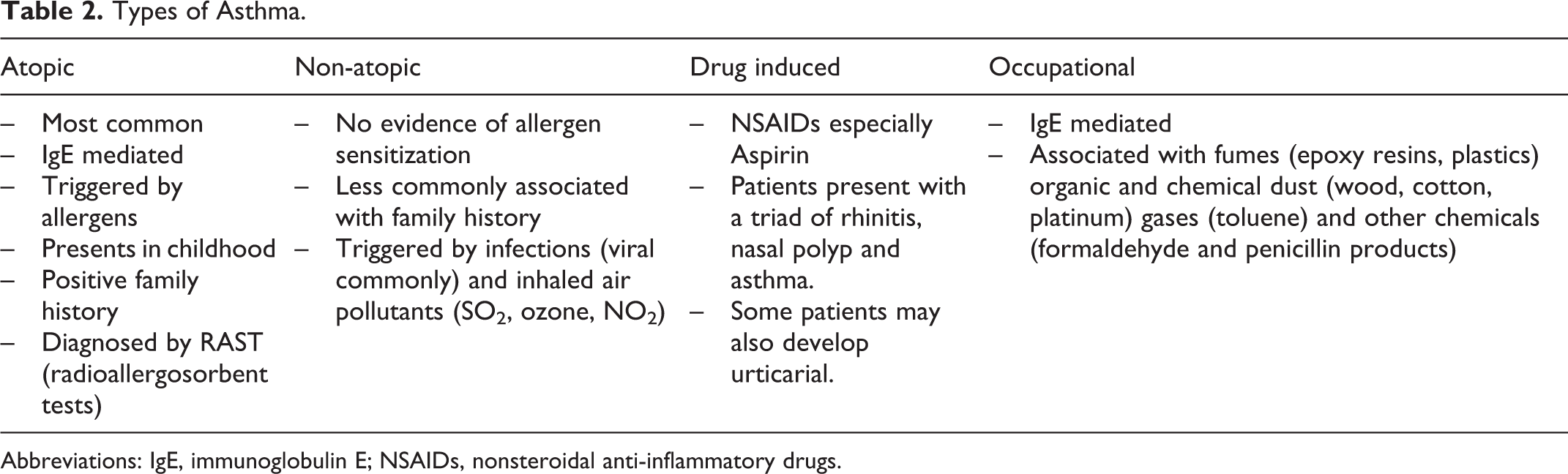
Abbreviations: IgE, immunoglobulin E; NSAIDs, nonsteroidal anti-inflammatory drugs.
What Is the Pathogenesis of Asthma?
Asthma results from an interplay between genetic factors, environmental factors, and immune response. Airway inflammation forms the core pathophysiologic mechanism. The pathogenesis of asthma is depicted in Figure 1. Atopic asthma is characterized by a TH2 and immunoglobulin E (IgE) response to allergens in genetically predisposed individuals. The asthma related genetic polymorphisms possibly influence immune process. Some of the genetic associations are described below
2
: ○ Chromosome 5q has a susceptibility locus for asthma close to the gene cluster encoding the cytokines IL-3, IL-4, IL-5, IL-9, and IL-13 and IL-4 receptor among which IL13 gene polymorphisms have the strongest and most consistent association. ○ Alleles of class II HLA are associated with production of IgE antibodies against some antigens, like ragweed pollen. ○ ADAM33 (a metalloproteinase) gene polymorphisms may be related to increased proliferation of bronchial smooth muscle cells and fibroblasts. ○ β2-adrenergic receptor gene variants are linked to differential in vivo airway hyper-responsiveness and in vitro response to β-agonist stimulation. ○ IL-4 receptor gene variants are linked to elevated total serum IgE, atopy, and asthma.
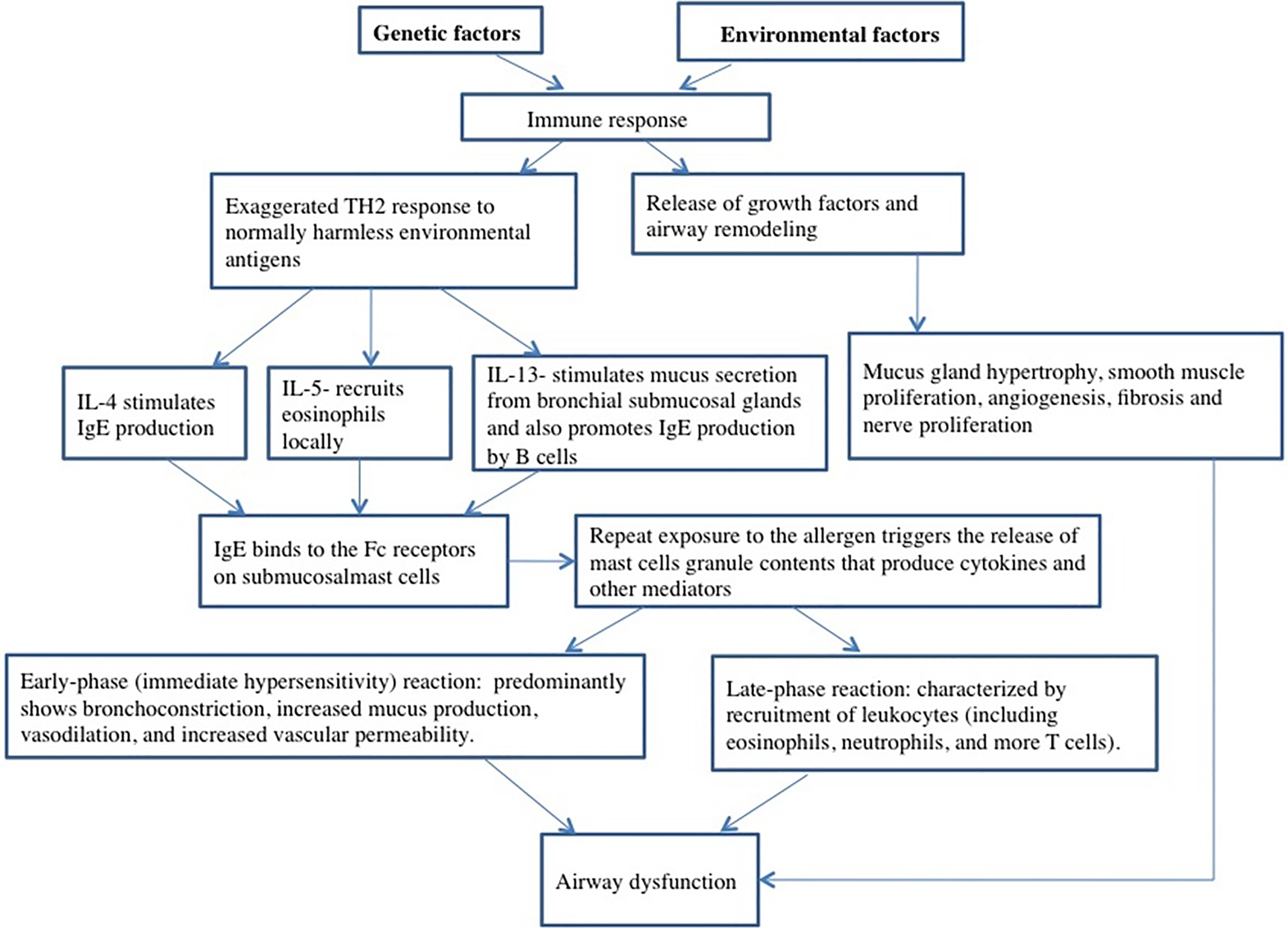
Pathogenesis of asthma.
What Are the Morphologic Changes Seen in Asthma?
Gross Appearance
In patients with severe asthma, the lungs appear overinflated showing atelectatic areas. The most prominent gross finding includes airways (bronchi and bronchioles) occluded by thick, tenacious mucus plugs. 2
Microscopic Appearance
A characteristic microscopic finding is Curschmann Spiral (Figure 2) seen in sputum or bronchoalveolar lavage samples of asthma patients. It is the result of mucus plugs extruding from subepithelial mucous gland or bronchioles. Numerous eosinophils with Charcot-Leyden crystals
○ Airway wall thickening
○ Subbasement membrane fibrosis (due to type I and III collagen deposition)
○ Increase in vascularity and squamous metaplasia
○ An increase in the size of the submucosal glands and number of airway goblet cells
○ Hypertrophy and/or hyperplasia of the bronchial wall muscle
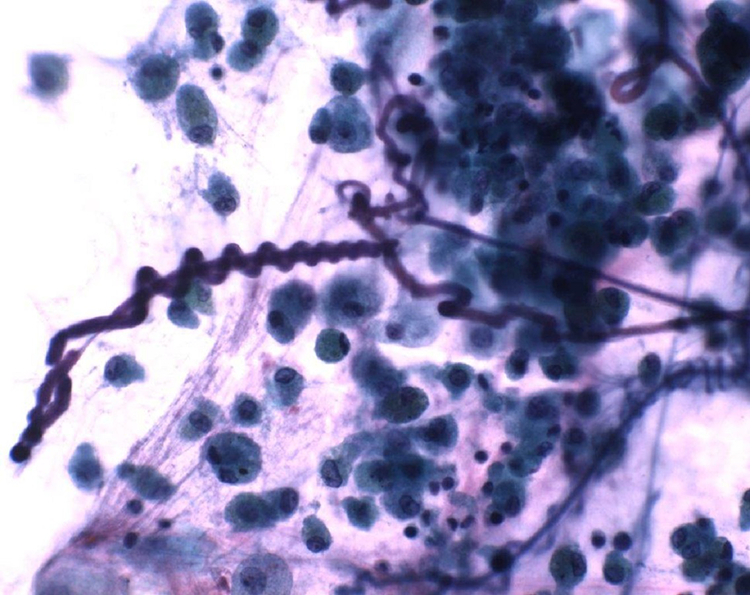
Curschmann spiral (1000×).
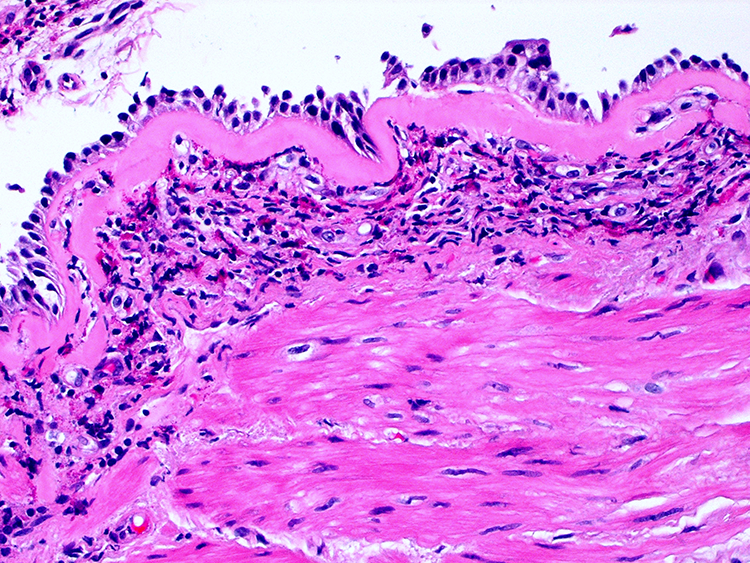
Sub-basement membrane fibrosis and submucosal eosinophilic infiltration (×200 magnification).
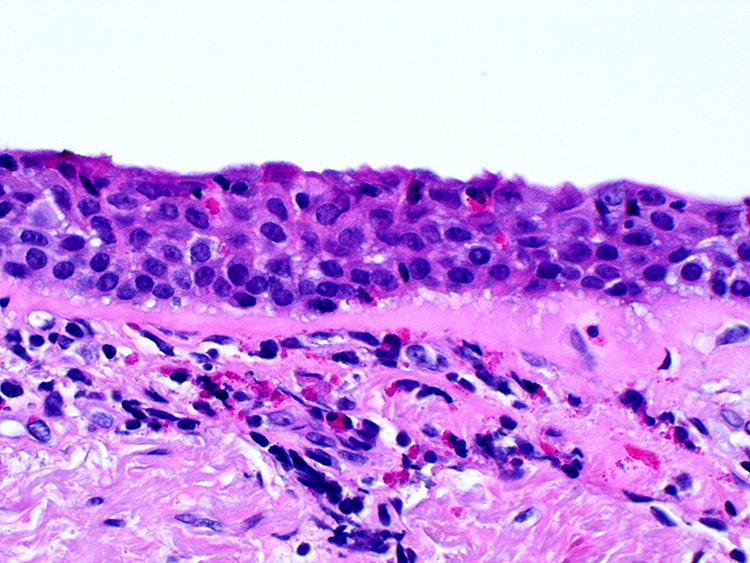
Squamous metaplasia, sub-basement membrane fibrosis and intraepithelial and submucosal eosinophilic infiltration (×400 magnification).
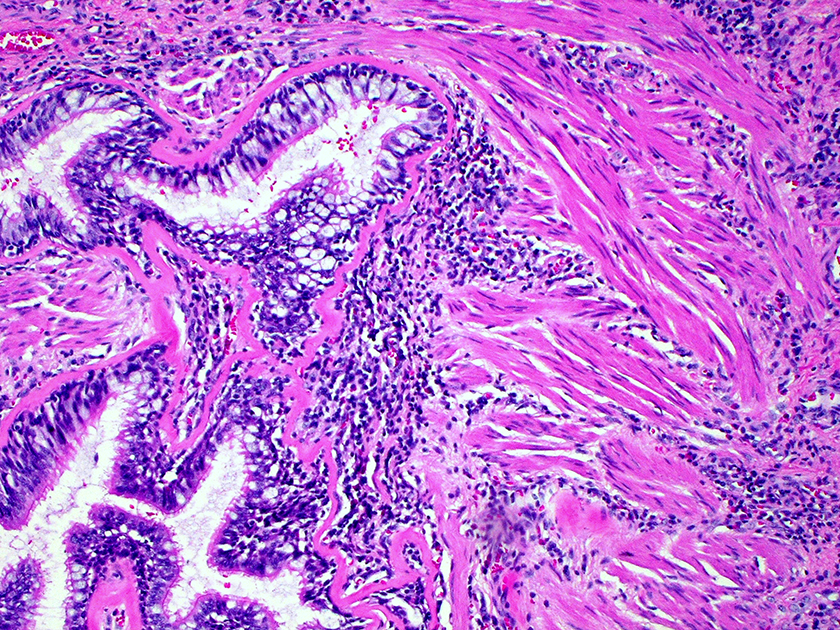
Goblet cell hyperplasia and smooth muscle hypertrophy (×100 magnification).
What Causes Airflow Obstruction in Asthma?
Airflow obstruction is a result of the following changes in asthma 4 :
Acute bronchoconstriction due to IgE dependent release of mediators (early asthmatic response) Airway edema associated with allergen challenge that occurs 6 to 24 hours later (late asthmatic response) Exudation of serum proteins and cellular debris resulting in chronic mucus plug formation Airway remodeling resulting from structural changes due to chronic inflammation that impacts the extent of airway obstruction reversibility
Airway obstruction leads to increased airflow resistance and expiratory flow rate reduction. These changes result in reduced air expulsion and may lead to hyperinflation of the lung. This overdistention helps preserve airway patency, thus improving expiratory flow. However, it also increases the work of breathing by altering pulmonary mechanics.
Teaching Points
Asthma results in reversible bronchoconstriction due to hyper-responsiveness of the airway to various stimuli. Atopic asthma is the result of an immunologic reaction to environmental allergens and is characterized by acute-phase (immediate) and late-phase reactions. Nonatopic asthma has less clear triggers but some viral infections and inhaled air pollutants are known to cause it. Almost all subtypes of asthma show eosinophils as key inflammatory cells but other inflammatory cells, for example, mast cells, neutrophils, and T lymphocytes can also be found. The irreversible component is the result of extensive airway remodeling (sub-basement membrane fibrosis, bronchial glands hypertrophy, and hyperplasia of smooth muscle).
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
