Abstract
In this article, I describe a study exploring horizontal violence and nurses’ perceptions of the phenomenon within the context of two 28-bed inpatient hospital units. The purpose of the study was to develop a clearer understanding of horizontal violence, incorporating observation and inquiry to identify the language nurses use to describe their experiences and factors in the nursing work environment that may perpetuate the phenomenon. Observation, review and analysis of policies, and interviews with staff were completed between June and November 2012. Thematic analysis resulted in five themes: (a) behaviors are minimized and not recognized, (b) fear inhibits all reporting, (c) avoidance and isolation are coping strategies, (d) lack of respect and support, and (e) organizational chaos. The findings suggest future interventions must address a range of factors that perpetuate horizontal violence within the nursing work environment with consideration for the embeddedness and complexity of the phenomenon.
Horizontal violence in nursing is defined as any “hostile, aggressive, and harmful behavior by a nurse or a group of nurses toward a co-worker or group of nurses via attitudes, actions, words, and/or other behaviors” (Thobaben, 2007, p. 83). Behaviors associated with horizontal violence contribute to an unsafe work environment and poor patient outcomes (Joint Commission, 2008). Its presence adversely affects nurses’ morale, sense of worth, and physical and mental health (Dehue, Bolman, Vollink, & Pouwelse, 2012; Kivimaki, Elovainio, & Vahtera, 2000; Quine, 2001). Horizontal violence also affects nursing recruitment and retention (Simons, 2008; Wilson, Diedrich, Phelps, & Choi, 2011).
The phenomenon was first identified in the nursing literature over three decades ago and is described as a “persistent occupational hazard within the global nursing workforce” (Vessey, DeMarco, & DiFazio, 2010). Horizontal violence continues to be an issue within the profession despite an expanding body of research and the development of interventions to address related behaviors (Mitchell, Ahmed, & Szabo, 2014; Roberts, 2015). The term horizontal violence is used interchangeably with terms such as lateral violence (Roberts, 2015; Sheridan-Leos, 2008), bullying (Quine, 2001), incivility (Clark, 2008), hazing (Brown & Middaugh, 2009), mobbing (Yildirim & Yildirim, 2007), relational aggression (Dellasega, 2009), and disruptive behavior (Joint Commission, 2008; Walrath, Dang, & Nyberg, 2010). The absence of consistent agreed-on definitions of these terms contributes to difficulty determining prevalence. The lack of agreed-on definitions also contributes to the lack of recognition of the phenomenon (Crawshaw, 2009). Further complicating recognition, researchers suggest that horizontal violence may be so ingrained in the nursing culture that individual nurses do not recognize it when they witness or experience it. These researchers contend that until a phenomenon is named and recognized, it cannot be addressed (Sellers, Millenbach, Ward, & Scribani, 2012).
Despite this potential lack of recognition, studies of the horizontal violence often rely on self-report, using self-completion questionnaires, such as the Negative Acts Questionnaire, or interviews to investigate and measure prevalence (Roberts, 2015). Moreover, many workplace violence policies, including zero tolerance policies, rely on nurses to identify colleagues who exhibit the related behaviors as the first step in addressing horizontal violence in their workplace (Joint Commission, 2008). If it is true that nurses do not recognize horizontal violence when they experience or witness it and cannot name it, both the lack of recognition and inability to name it are barriers to accurate measurement and to effective intervention (Sellers et al., 2012). These barriers must be better understood and addressed if interventions are to be effective. The purpose of the study was to develop a clearer understanding of the phenomenon by incorporating observation and inquiry to identify the language nurses use in describing their experiences and factors in the nursing work environment that may perpetuate the phenomenon. The following questions were the basis for the study:
Is the phenomenon present and can it be observed? If so, what does it look like?
What are nurses’ perceptions of horizontal violence? How do they experience, understand, and explain the phenomenon?
What environmental factors contribute to the perpetuation of the phenomenon?
Method
Approach and Perspective
Qualitative inquiry is recognized as a valid approach to gaining an understanding of a multifaceted phenomenon within a context-bound setting (Patton, 2002). As the purpose of this study was to develop a clearer understanding of the complex phenomenon of horizontal violence in the context of two hospital units, a descriptive exploratory approach was used. Data collection methods included nonparticipant overt observation, document review, and nonstructured and semistructured interviews. Nonstructured interviews with staff were impromptu conversations about the events of the day and occurrences on the units. Semistructured interviews with nurse participants focused on their experience and sense making of horizontal violence.
This study was conducted from a constructivist perspective, where meaning and sense making are studied because meaning and sense making shape action (Guba & Lincoln, 2008). I was interested in the nurses’ understanding of the phenomenon of horizontal violence and actions taken in response to their experiences. A constructivist perspective allows for multiple interpretations of realities and alternative interpretations of data (Fetterman, 1989). In using this approach, I did not seek to uncover a single truth but to develop an understanding of the multiple, situational realities experienced by individuals in their day-to-day work lives.
Site Selection and Access
Although horizontal violence is recognized as a problem within all health care professional groups, nurses are understood to be at the greatest risk for intraprofessional aggression (Vessey et al., 2010). Nurses in some settings are at greater risk than others (Hawkins & Kratsch, 2004). Based on the responses of 303 nurses to an Internet survey advertised in print and on the website for the publication Nursing Spectrum, horizontal violence in the form of bullying occurred most frequently in medical/surgical (23%), critical care (18%), emergency (12%), operating room/post anesthesia care unit (9%), and obstetrical (7%) areas of care (Vessey, DeMarco, Gaffney, & Budin, 2009). Although I did not have control over which units would volunteer to participate in the study, I hoped the participating units would be units where horizontal violence was suspected.
A number of potential research sites were identified through my professional network. When an associate chief nursing officer at the first facility approached expressed interest, I forwarded a letter of introduction and summary of the study to her. After a formal presentation to the nursing executive committee and representatives of the nurses’ union, participation by this 400+-bed not-for-profit urban health care facility in the Northeastern United States was approved. Three nurse managers who believed their staff morale was adversely affected by horizontal violence granted me permission to observe day-to-day activities on their units. Unfortunately, one of the three managers was laid off and the unit’s participation was withdrawn when its management was merged with that of another unit. The two units remaining were each 28-bed inpatient units: one general medical/surgical unit (Unit A) and one specialty surgical unit (Unit B).
Participants and Consent
A summary of the planned study and a copy of the consent form were posted in the break rooms on both units. The 120 hospital staff (80 nurses, 22 patient care assistants, 14 unit secretaries, two nurse educators, and two nurse managers) on the payrolls of the participating units and any hospital staff coming to the units to provide care were eligible to participate. I reviewed both documents with each staff member and explained how they could participate or opt out of participation. Although I was granted general permission to observe on both units staff members could opt out of further participation by declining opportunities to interact or speak with me. Only one nurse declined participation. Patients and their visitors were not included in the study, and observations did not take place in patient rooms to maintain privacy and confidentiality.
Protection of Human Participants
Initial approval for the study was obtained from my academic institution. The participating facility’s Institutional Review Board (IRB) determined that because I was not a member of staff or working with a researcher at the facility, my study would not require their review. Letters outlining this decision and verifying permission to conduct research in the hospital were submitted to my academic institution’s IRB and final approval was granted.
All study participants were verbally consented to assure confidentiality. Names and other identifiers were removed from field notes and pseudonyms were used in transcripts. I was aware that exploring and recounting experiences of the phenomenon of horizontal violence might be distressing for some participants. Resources for counseling were identified in advance of participation and provided during the consent process.
Data Collection
Data collection took place over the period of 5 months between June and November 2012.
Document review
Document review focused on policies related to behavioral expectations, specifically the facility’s workplace violence policy and codes of conduct. My intent in reviewing and analyzing these documents before spending time on the units was to understand the facility’s policies related to behavioral expectations and become familiar with the language used to describe reportable behaviors in these policies. I continued to review distributed educational materials, posters, assignment rosters, and hospital forms throughout the study to develop a better understanding of the workplace and unit culture. Analysis of these materials was outlined and documented using a worksheet adapted from worksheets for document analysis developed by the Education Staff at the National Archives and Records Administration in Washington, D.C. (National Archives, n.d.).
Observation
I was a nonparticipant observer on both units, dressed in solid-colored trousers and a plain shirt with a hospital id badge. Observation occurred across all shifts with approximately half of the hours occurring on day shifts and half of the remaining hours split between evening and night shifts. The majority of my observations took place at the unit secretaries’ desk, a public space at the center of each unit. Additional observations occurred in the hallways, break rooms, and in the shared medication room. Observation was overt and participants were aware of the study aims and its focus on “any noncaring, nonsupportive behavior between nurse colleagues.” Although I took note of helping behaviors on both units, my focus was on the nonhelping behaviors outlined and described in the first three columns in Table 1.
Manifestations of Horizontal Violence Observed and/or Reported.
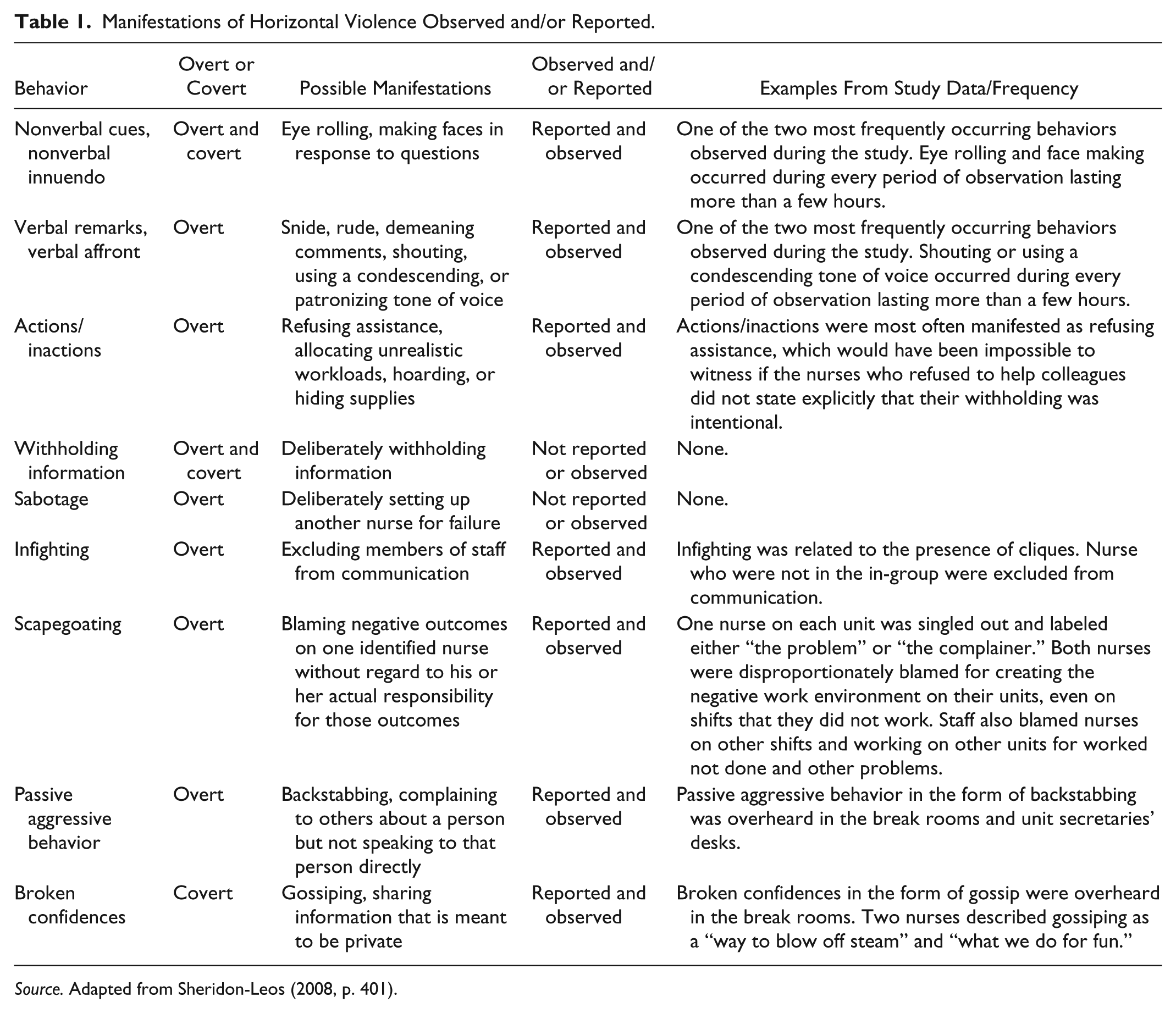
Source. Adapted from Sheridon-Leos (2008, p. 401).
Documentation included field notes detailing observed events and interactions, and records of informal conversations with staff. Initial periods of observation were scheduled during times when staff was likely to interact; handover, rounds, medication administration times, and during scheduled meetings and learning opportunities. There were 75 periods of observation lasting from 1 hour to 9 hours, with the average period of observation lasting 5 hours. Three hundred seventy hours of observation of the day-to-day activities and staff interaction on both units were completed over a period of 5 months.
Interviews
Members of staff participated in nonstructured and semistructured interviews. Nonstructured interviews, essentially informal conversations, with nurses, managers, doctors, unit secretaries, patient care assistants, transporters, housekeepers, and others, took place during every period of observation. In these conversations, participants recounted events of the day, informed me of occurrences I had missed, shared details about their lives outside of work, and asked questions about the study. Thirty-one staff members participated in semistructured interviews; 22 nurses (21 women/one man), two nurse managers (both women), two nurse educators (both women), and five administrators from Human Resources, Quality and Safety, Patient Experience, and Risk Management (all women).
Interviews with managers, educators, and administrators focused on their understanding of current policies and procedures to address the phenomenon, as well as their role in managing behavior within their unit or within the hospital facility. Some also shared their experiences of horizontal violence. Semistructured interviews with nurse participants focused on their experiences and sense making of the phenomenon. Although the term horizontal violence was listed in the title of the study in the study summary and consent forms, the phenomenon was otherwise not named to allow participants to use their own language to describe their perceptions and experiences but was broadly defined as “any physical or emotional, noncaring or nonsupportive behavior between nurse colleagues.”
The nurses participating in semistructured interviews were self-selecting. There was no incentive offered for participation. Twelve Unit A nurses were interviewed, and 10 Unit B nurses were interviewed. The majority of these nurses were women (n = 21) and White (n = 21), ranging in age from mid-20s to mid-50s. The majority held associate degrees in nursing (n = 16). Six nurses held bachelor’s degrees. One nurse interviewed was a new grad. The remaining nurses had from 2 to 14 years of experience on the units. This sample reflected the nurse demographics of the two units.
The semistructured interview questions with nurses included the following:
Why did you become a nurse?
Is nursing different than you thought it would be before you went to nursing school or before you started working as a nurse? How?
Tell me about a good day at work
Tell me about a bad day at work.
In sharing stories about a bad day at work when nurse participants recounted behaviors identified as related to horizontal violence in the literature, they were asked to elaborate.
The majority of the interviews were digitally recorded with consent and transcribed verbatim. I took notes (with consent) during these interviews to capture participants’ reaction to questions and summarize responses in case of recording failure. I also took notes (with consent) during interviews in cases where the participant did not wish to be digitally recorded. I created transcripts summarizing those interviews from these notes. Interviews ranged in length from 15 minutes to 2 hours.
Data Analysis
The document analysis worksheets, field notes, and interview transcripts were converted into Microsoft Word documents. I coded and analyzed the data thematically using applied thematic analysis as outlined by Guest, MacQueen, and Namey (2012). The majority of coding was completed by reading and rereading materials, systematically examining the data to identify common elements, highlighting these elements in printed copies of the data, and creating index cards of potential themes. These themes were further reduced and merged into five overarching themes.
Rigor
As the sole researcher, I attempted to maintain rigor and minimize bias in a number of ways. Throughout the study, I shared findings with another researcher experienced in qualitative methods. We met every 2 weeks during initial data collection and reviewed the development of the codebook and finalization of themes. I kept a reflective journal throughout the research process to assist in maintaining objectivity. I felt that my extended time in the field allowed me to establish a rapport and develop trust with the participants. Over time, the staff appeared willing to share experiences and perceptions openly, contributing to a more accurate picture of the unit culture. The use of multiple data collection methods also contributed to a more accurate depiction of the unit, staff, and their experiences. I reviewed interview transcripts or summaries with individual participants whenever possible. Moreover, a 14-page booklet summarizing the study findings was shared with all staff on both units via email and copies of the summary document were also left in the break room for their review. The seven nurse participants who provided feedback described that the findings resonated with their experiences and were an accurate picture of life on their units.
Findings
The facility’s Workplace Violence Policy defined workplace violence as “any physical assault, threatening behavior or verbally abusive remark that is made in the workplace and/or affects the workplace behavior of an employee.” The policy listed a range of reportable behaviors from “verbal threats, intimidation, or coercion” to “any unauthorized use or possession of firearms” and emphasized the importance of reporting behaviors that posed imminent threats to safety. The Code of Conduct outlined a wider range of behavioral expectations.
Intimidating and disruptive behaviors are unprofessional and not tolerated. Behaviors that are considered intimidating and disruptive can be verbal or physical. They include verbal outbursts and foul language; sexual harassment in any form; physical roughness; threats; refusing to perform assigned tasks; quietly exhibiting uncooperative attitudes during routine activities; reluctance or refusal to answer questions, return phone calls or pages; condescending language or voice intonation; and impatience with questions.
Most members of staff, other than the managers and nurse educators, were not familiar with the Workplace Violence Policy or the Code of Conduct. They did not have a clear sense of what behaviors were expected or reportable. Two nurses who were aware of the Code of Conduct suggested that everyone should have to abide by some behavioral code as a condition of employment, sign an agreement, and have it be binding. There was no such requirement. The human resource representative interviewed disclosed that very few reports related to employee behavior made it to her office. She added that the hospital had little success in pursuing behavioral complaints unless they were actionable under Equal Employment Opportunity law, involving allegations of discrimination based on race, color, sex, national origin, religion, age, disability, sexual orientation, or related to reprisal.
Overt observation helped answer the questions: Is the phenomenon present and can it be observed? And if so, what does it look like? The phenomenon of horizontal violence was visible in public and private areas on both units. With the exception of Withholding Information and Sabotage, I witnessed of each of the behaviors outlined in Table 1. Nonverbal cues/nonverbal innuendo and verbal remarks/verbal affront occurred most frequently, at least once during every period of observation lasting more than a few hours, most often in the form of eye rolling and face making, and shouting or using a condescending tone of voice. Actions/inactions were most often manifested as refusing assistance, which would have been impossible to witness if some of the nurses who refused to help colleagues had not shared with me that this withholding was intentional. Over time, I became aware of patterns of refusal. Infighting appeared to be related to the presence of cliques, which I felt were most visible on the night shift. This observation was supported by one of the managers who shared that cliques were an ongoing issue for the night nurses on her unit.
Scapegoating was less frequent, but over the course of 5 months, I identified one nurse on each unit who was singled out and labeled either “the problem” or “the complainer.” Both nurses were disproportionately blamed for creating the negative work environment, even on shifts that they did not work. Scapegoating occurred across shifts and across units as well, as groups of nurses blamed the shift before them or other units transferring patients for work not completed. Passive Aggressive Behavior in the form of backstabbing and Broken Confidences in the form of gossip were occasionally overheard in the break rooms. During lunch one afternoon, a nurse explained to me that gossiping was how nurses “let off steam.” Another explained, “It’s what we do for fun.” The majority of behaviors observed would not meet criteria for workplace violence as defined under existing policies but were prohibited and reportable under the Code of Conduct, which was not enforced.
Nurses shared their experiences and perceptions and of horizontal violence, confirming its presence on both units. Nurses who witnessed the phenomenon or were targeted by a coworker did not have a name for what they had experienced. Only one nurse used the term bully, defining a bully as “someone who makes you do their work for them.” More often, nurses described the behavior and attributed it to the perpetrator’s personality or work ethic, to something going on in that person’s life, or stress on the unit.
In recounting stories experiences of aggression, participants often asked me whether what they had experienced was reportable. Did I think they had been bullied? When directed to the Workplace Violence Policy and Code of Conduct, some nurses recognized the abuse they suffered met criteria for a reportable event. Only one nurse interviewed had ever formally reported a coworker.
Observations together with interview data helped to identify factors contributing to the perpetuation of horizontal violence on both units. These are summarized in five themes.
Themes
Behaviors are minimized and not recognized
The lack of clearly defined behavioral expectations and lack of knowledge of and enforcement of the Code of Conduct contributed to a lack of recognition of behaviors as problematic and reportable. Even the nurse managers and educators, the unit staff most familiar with policies, were not sure about the policies or reportable behaviors. One nurse educator shared, “I am not sure if there is a policy that covers bullying here. There is no clear-cut definition of bullying to work with. It’s so unclear.” When asked about expected behaviors, a manager reported, “I don’t think we have defined it. We are revising our policies. The Code of Conduct might have a better understanding of what is expected in behaviors, what is acceptable.”
As the behaviors associated with horizontal violence were tolerated, nurses and other staff members appeared to accept them as part of the job and minimized the long-term impact on communication, teamwork, and safety. Addressing conflicts with colleagues was not a priority for the nurses with some even stating that they did not care about getting along with their coworkers. These nurses described that taking care of their assigned patients was the priority above all else:
At the end of the day, it doesn’t matter how my peers treat me, I am here for my patients and I can go to sleep at night. I am here to make sure that the patient got the assistance they needed.
Nurses described a focus on their own patient assignment and having little time or concern for conflict resolution.
Fear inhibits all reporting
Horizontally violent behaviors, when recognized, were generally not reported. Approximately half of the nurses interviewed identified barriers to reporting; among those fears was the fear of reprisal. “If I complain, no one will help me.” “If you say anything, then it is going to be worse.” Nurses also described a fear of being labeled. “If I report, then I’ll be a snitch.” “If I file an incident report, I’ll be labeled a complainer.”
This fear of reporting extended beyond horizontal violence into reporting of medication errors on one unit and unsafe staffing on the other. Two or three nurses on each unit believed they would be labeled incompetent if they made a mistake or couldn’t manage their patient load on their own. Even concerns about missing medications and supplies were suppressed, as these nurses knew their colleagues and managers often labeled nurses who verbalized frustrations as complainers. A few nurses shared their belief that reporting did not result in change. They described that nothing happened when reports were made and reporting was not worthwhile.
Avoidance and isolation are coping strategies
Twenty-one of the 22 nurses interviewed described themselves as conflict avoidant. A few shared that they knew what kind of day they would have as soon as they looked at the schedule. If they were on shift with staff they were in conflict with or felt they could not rely on, they described working alone and not asking for help because they believed they would not receive it.
It hasn’t been a unit well known for teamwork. People work singularly. “I just want to work by myself. If you need me call me, but I’m not reaching out to you.” Staff see themselves as team players but if you look closer they may not necessarily be. (Manager) I don’t ask unless I really need help. And that’s why, because no one will help me. You know, some of our nurses don’t even go to a code. They just keep going on with their day. So you know what, don’t expect me to help you. That’s how I feel. (Nurse)
Two nurses (one from each unit) independently shared purposefully positioning themselves at far ends of the unit hallways to avoid interaction and being asked to help nurses who would not help them.
Another finding, perhaps rooted in conflict avoidance, was a lack of bystander intervention. When a member of staff was subject to verbal abuse by a colleague, bystanders did not intervene, potentially further isolating the target and in their silence condoning the behavior. During the 370 hours of observation, I never witnessed any bystander intervention.
Lack of respect and support
The nurses described a lack of respect for their role and feeling unsupported, having no control over workflow or resources. Despite posters hanging on the walls of both units promoting teamwork, many members of staff did not feel included as part of the patient care team. Patient care assistants described not being included in the plan of care by the nurses. Nurses described having to track down physicians who had described the plan to the patient and not included them in the conversation.
Nurses and other staff described a disconnect with administration. They felt the hospital administration had no idea about what was happening on the units. One nurse shared, “I’ve never seen admin come to the floor, do rounds, talk to nurses, or make their face known. Makes you think admin doesn’t have an idea about what the front line does.”
Another nurse described lack of recognition of the role of the nurse: “Top down, the people don’t recognize the people at the bedside enough. I don’t think they do. It’s disappointing, and the nurses know that and feel that.”
Despite one senior administrator insisting that staff had to know how much workers’ hard work was appreciated, staff told me they did not feel valued. A few of the nurses felt that even their patients didn’t recognize or respect their role. “I feel like we’re Dunkin Donuts here . . . You’re customer service. We’re a hospital. I am not your waitress. I am not your bed companion. I’m not any of that.” In addition, when patients and families were verbally abusive and threatening, nurses felt they had no recourse. Nurses from both units shared that when a patient or family member was abusive, even their nurse managers failed to support them.
Nurses identified another major stressor and potential patient safety risk: batched admissions and discharges. Physicians often told patients they would be discharged in the morning but would not return to the units to complete the required paperwork until the afternoon, when patients were discharged en masse. This created a chaotic environment where nurses managed multiple discharges as new admissions arrived. One manager identified discharges as a serious issue adversely affecting nurse/doctor relationships on her unit.
Discharge is a source for nurse/doctor frustration. It has elevated to violence. The doctor tells the patient they are going home in the morning. The nurse has to front the doctor as delays happen late in the day. Not a way to start the evening shift. It’s not fair to the evening nurses. They are blasted by the patient and by the family. (Manager)
Nurses had no power in controlling the flow of admissions to their own units. One evening when one nurse asked whether there could be a 15-minute delay in a transfer while she settled her first admission, the nurse on the transferring unit called bed management, who then called the receiving nurse telling her that her patient would be sent immediately. A nurse involved in the exchange shared, “Bed control is the bully now.”
Even nurse managers could not close beds or control patient flow. When one manager closed a bed on her unit because one patient in the shared room was extremely physically and verbally aggressive, the bed was unblocked from above and another patient was put into that shared room despite concerns for staff and patient safety. During the 5-month period of data collection, educational resources for nurses were cut and the majority of the associate chief nursing officer positions were eliminated. As part of one patient care initiative on one of the units, nurses had been given control over resources to improve their patients’ experience. That funding was also eliminated. In a conversation in the hall, a nurse who had been part of the committee to improve the patient experience described, “That [initiative] was about caring. Now that we don’t have it, we obviously don’t give a shit.”
Organizational chaos
All staff interviewed described system problems that adversely affected their ability to provide care. Nurses and Patient Care Assistants described not having access to equipment and tracking down medications and supplies that should have been readily available. Treatments were delayed when patients were not ready for transport when transport arrived and when transport did not arrive on time or was not available.
No equipment. Not restocked. No more flushes. No one answers your page in facilities. No one has taken the dirty linen and it’s overflowing. All of these factors are creating an environment that is more stressful than it has to be. It sets the tone. These increase the risk for violence. I’m not saying it’s directly related, but it does contribute to it happening. (Nurse Educator)
System failures also contributed to a sense that other people in the institution were not doing their jobs while the individual making that attribution felt they were hard working. Relationships between units and between shifts within units were also affected when the perception was that staff members on these other units and other shifts were intentionally passing on work they should have done. A nurse manager described ongoing conflict between her unit and the emergency department (ED).
There is a mutual lack of understanding and disrespect between the ED and the floors. The floors don’t understand the role of the ED and the ED doesn’t respect the floor nurses. Is the ED slammed or are they just dumping? That’s a huge risk factor for nurse-to-nurse violence. (Manager)
Every nurse interviewed believed a lack of accountability allowed people who had bad personalities or poor work ethics to stay on.
Despite the implementation of initiatives designed to improve patient flow at this facility, there was a lack of follow-up when transportation did not arrive, when medications were delayed, and when supplies ran short. There appeared to be no recourse other than to work around the problem or, as often happened, call and yell at someone in the department perceived to be behind the problem (often transport, pharmacy, or central supply).
Discussion and Implications
Results presented in this article focus primarily on the nonhelping behaviors between nurses on these two units. I feel it is important to acknowledge that more often than not, the nurses on both units answered call lights and alarms for one another, stepped in and offered help, started admission paperwork, or gave medications for a nurse who was busy with other patients. The staff provided excellent patient care. More than half the nurses interviewed identified their unit was a “good unit” and many chose to stay on their units rather than seek a promotion elsewhere. Float staff described the two units as two of the better units in the hospital. However, there was an undercurrent of aggression that ebbed and flowed, often around peak periods of activity. As a privileged observer, I was able to witness behaviors and patterns of behaviors that managers and other staff could only catch glimpses of. Watching nurses affected by the undercurrent was distressing. Instances often happened so quickly that even I wondered: Did I just see that? Nurses did not have time to stop in the moment and address the situation, if it had registered with them, and described being too tired at the end of the day to care.
The study results support the findings of the study of New York State Nurses by Sellers et al. (2012) that suggests nurses do not recognize behaviors related to horizontal violence when they witness or experience them. The majority of nurses interviewed did not identify their experiences of aggression as horizontal violence or bullying or by any other term in the literature or workplace violence policies or codes of conduct. Instead, they described the behavior and attributed it to the individual’s personality, work ethic, life outside of work, or events on the unit. This finding supports findings from an early study by Farrell (1997), with nurses primarily attributing negative behaviors to individual personality.
Most nurses were unaware of the facilities’ workplace violence policies and codes of conduct. Even managers and nurse educators were unclear about policy language and the process for reporting. This finding supports other study findings that managers have insufficient resources and guidance to respond to workplace aggression (Johnson, Boutain, Tsai, & de Castro, 2015). Rayner and Lewis (2011) suggest that organizations support managers by providing them with clearly written policies that outline the actions they should take in response to bullying, as well as ongoing monitoring and review of these policies.
Nurses also need support to develop conflict management strategies and skills. The majority of nurses interviewed in this study described themselves as conflict avoidant, mirroring nursing’s conflict avoidant culture (Mahon & Nicotera, 2011). Although physicians at this facility were required to participate in a 2-day course focused on communication skills, these resources were not available to nurses. The management of conflict among nurses needs to be further addressed in research and practice (Brinkert, 2010).
Nurses working on both units identified a number of systems problems and stressors they believed contributed to behaviors associated with horizontal violence. Nurses’ lack of control over resources and workflow suggested that both units could be considered “toxic” work environments (Alspach, 2007; Rowell, 2005). Recent literature suggests competition for resources lays the foundation for bullying behaviors (Wheeler, Halbesleben, & Shanine, 2010). Given the responsibility nurses have for patients coupled with their focus on their individual patient assignments in environments of diminishing resources, competition for resources should be further investigated as a factor in horizontal violence between nurses.
Nurses on both units felt disrespected by administration that administrators had no idea what direct patient care involved or what it was like to be on the “front line.” Nurses felt they were being asked to do more with less. There was an environment of organizational chaos, described in the literature as “poor organization and coordination of the labour processes” (Roscigno, Hodson, & Lopez, 2009, p. 79). Analyses of other industries in the workplace literature reveals that all forms of incivility, including horizontal violence and excluding sexual harassment, are rooted in organizational chaos, as workers interfere with one another in a struggle to complete their own work (Roscigno et al., 2009). The role of organizational chaos in horizontal violence in health care is yet uninvestigated, but also worthy of future research.
Findings should be interpreted noting several limitations. This study took place in a single hospital facility in the northeastern United States. I was collecting data during a 5-month period between two layoffs when nurses at this facility were working without a contract. This study reflects a snapshot in time. The majority of the staff observed and interviewed were women and were White. Men were underrepresented. Of the 22 nurses participating in semistructures interviews, only one was a man. Less than 1% of nurse participants on either unit were non-White or a man. (This reflects the demographics of both units.) Staff members who participated in interviews were self-selecting. Although the data collected, resulting analysis, and development of codes and themes were reviewed with an additional researcher experienced in qualitative methods, I was the sole investigator.
Conclusion and Future Directions
This study has added overt observation of the phenomenon and inquiry into nurses’ perceptions of horizontal violence within the context of their current work environment to the discourse. Periods of observation provided me the opportunity to compare behavioral expectations outlined in policies and codes of conduct to behaviors enacted by participants. The gap between behavioral expectations and observed behaviors might indicate a lack of awareness of, or perhaps concern for, lower level behaviors associated with horizontal violence as problematic, especially as many of these behaviors took place in public areas of the unit, in full view of patients and visitors. This potential lack of awareness or concern merits future investigation.
In addition, findings suggest that interventions focused on a single cause may not be effective when more than one factor is likely contributing to the phenomenon, as was the case with these two units. Future interventions must address a range of factors that perpetuate horizontal violence within the nursing work environment with consideration for the embeddedness and complexity of the phenomenon.
Footnotes
Acknowledgements
I extend my sincerest gratitude to the participants in this study and thank Dr. Neenah Estrella-Luna and Dr. Susan Jo Roberts for their support.
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported in part by a research grant from the Gamma Epsilon Chapter of Sigma Theta Tau International.
