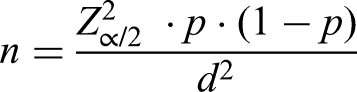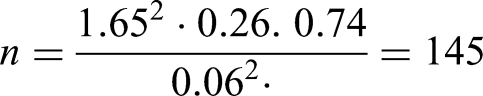Abstract
Objectives: To investigate sexual practices and HIV risk perception among MSM, identifying associated risk factors and determinants. Methods: A cross-sectional epidemiological study was conducted with 144 MSM in Teresina, Piauí, Brazil, using the snowball sampling technique. Participants were recruited via snowball sampling and underwent rapid HIV testing, in addition to completing questionnaires on sexual practices, risk perception, and illicit drug use. Results: The majority of participants showed an unsatisfactory perception of HIV risk. Factors associated with this perception include non-penetrative sex as an HIV preventive measure, which increased the chances of having an unsatisfactory risk perception by 1.45 times (P = .04), engaging with known HIV-positive individuals without knowledge of their viral load (ORa = 2.70; P = .043), and using illicit drugs before/during sex (ORa = 0.29; P = .048). Conclusions: The results indicate a high prevalence of risky sexual practices and an unsatisfactory HIV risk perception among the MSM studied.
Plain Language Summary
This study examines sexual practices and perceptions of HIV risk among men who have sex with men (MSM) in Teresina, Brazil. MSM are significantly more likely to contract HIV compared to the general population, with various factors influencing their risk. Despite this high vulnerability, many MSM do not perceive themselves to be at significant risk of HIV infection. Researchers surveyed 144 MSM to understand their sexual behaviors and how they perceive the risk of HIV. The study found that many MSM engage in risky sexual practices, such as not using condoms during oral sex, even though most use them during anal sex. Additionally, the study revealed that MSM often has a false sense of security when having sex with steady partners compared to casual partners. Key factors associated with a poor perception of HIV risk included low family income, engaging in non-penetrative sex as a preventive measure, having sexual relations with known HIV-positive individuals without knowing their viral load, and using illicit drugs during sexual activity. For instance, using illicit drugs, known as “chemsex,” significantly increases risky behaviors, leading to a higher chance of HIV transmission. The study emphasizes the need for targeted health education and interventions for MSM. It suggests promoting regular condom use, better understanding of HIV transmission risks, and discouraging the use of drugs that impair judgment during sexual activities. Effective public health initiatives should be culturally sensitive and accessible to MSM of all income levels. By addressing these issues, health programs can better support MSM, reduce HIV transmission rates, and improve overall well-being.
Introduction
When considering HIV infection, men who have sex with men (MSM) bear a disproportionately high burden compared to the general population and other vulnerable groups. 1 MSM are approximately 28 times more likely to contract HIV worldwide than the general population.2,3 Various biological, behavioral, and structural factors contribute to this elevated risk. The situation in Brazil is particularly concerning, as recent research indicates that the estimated prevalence in this population (18%) is significantly higher than the average for the general population of the country (0.6%).3‐5
According to the Joint United Nations Programme on HIV, Brazil presents a concentrated epidemic characterized by epidemiological contexts in which the infection disproportionately affects key populations.4‐6 Health authorities are concerned as global progress against HIV is slowing down, and although new HIV infections are declining, the reduction has not been very significant. Globally in 2021, the decrease was only 3.6% compared to 2020, representing the lowest annual reduction since 2016. 4 Meanwhile, in Latin America, between 2010 and 2019, new infections increased by 21%.4‐6
Brazil has the largest population of people living with HIV in Latin America, followed by Mexico and Colombia, with an average of 36.8 thousand new AIDS cases annually over the past five years. However, the AIDS detection rate has been declining since 2012, with the year 2020 observing the highest annual reduction in the rate, which dropped to 14.1 cases per 100 thousand inhabitants, partly due to underreporting caused by the overload of health services during the COVID-19 pandemic. 7
In the municipality of Teresina, Piauí, in the northeastern region of Brazil, from 2018 to 2022, 2264 HIV cases were reported, with approximately 25% among MSM. 8 These high rates among MSM are associated with the adoption of unprotected sexual practices, such as receptive anal intercourse without protection, acquisition of other risky behaviors, prejudice, and discrimination.9‐12
The vulnerability of the MSM group is due to behavioral, social, and cultural factors. Since the beginning of the HIV epidemic, lack of information, stigma associated with infected individuals, fear of discrimination resulting from sexual practices, and breach of confidentiality in health services are factors contributing to the lack of seeking care and knowledge of serological status, consequently resulting in increased HIV occurrence in MSM. 13
Despite the high vulnerability of MSM to HIV, a study conducted in Brazil in 2019 shows that only 5% of the surveyed MSM assess their risk of HIV infection as high, with over 30% engaging in unprotected sex. 14 This failure to use condoms during sexual relations among MSM is influenced by pre-judgment of partner appearance, consumption of sexually explicit media, drug use, having a steady partner, among other factors.11,14‐16
Considering the increasing spread of HIV among the MSM population in Brazil and particularly in Piauí, and the scarcity of studies on HIV risk perception among this group, it is relevant to investigate how MSM perceive the risk of HIV infection and what factors may influence this risk. Thus, given the shortage of studies from this analytical perspective, the conduct of this study is justified, aiming to analyze HIV risk perception among MSM in a northeastern capital of Brazil.
Methods
Epidemiological study, cross-sectional conducted following the recommendations of the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE).
The study occurred in the municipality of Teresina, the capital of Piauí, Brazil, 16 at the Testing and Counseling Center (CTA) of the State Health Department of Piauí. The choice of the CTA was made to ease access for the target population of the study, as it is centrally located, well-known to the MSM population, and provides exclusively reserved physical space for this purpose.
The source population consisted of MSM residing in the city of Teresina, Piauí, totaling 16,040 (IBGE, 2023). For the sample size calculation, the following formula was used, based on the population proportion estimate for an infinite population:
The first instrument was validated by Almeida et al 17 and was applied in this study to collect information on the personal characteristics of the sample and sexual practices, comprising a total of 35 questions.
The second instrument is an HIV risk perception scale, consisting of eight questions, previously validated in European Portuguese by Napper et al 18 and adapted cross-culturally by Torres et al 19 Each of the eight questions allows responses with scores ranging from 1 to 6. Some questions have a negative connotation, inversely affecting the response classification. The maximum score on the scale is 40 points, corresponding to 100%. Thus, risk perception was classified as follows: 1% to 79% – unsatisfactory; 80% to 100% – satisfactory.
Considering that the instruments were being applied at a different time, by other researchers, and in a different context, a pilot study was conducted with 14 MSM (10% of the sample) prior to data collection. The objective was to definitively test the instruments regarding their feasibility and the field researchers. It should be noted that the results obtained were not included in the final estimates and hypothesis tests. However, the pilot study was important as a rehearsal for data collection, allowing for necessary adjustments.
Data collection was conducted by undergraduate, master's, and doctoral students in Nursing, previously trained by the study advisor, and took place from October to December 2023, carried out in two consecutive stages. In the first stage, rapid HIV testing and counseling were performed on those MSM who agreed to do so, following the recommendations of Ministry of Health Ordinance No. 77 of January 12, 2012. In the second stage, the two research instruments were applied to MSM whose rapid test results were non-reactive, after signing the Informed Consent Form. Those with reactive results were referred to the HIV reference center in Teresina. It is noteworthy that partnership was sought with the LGBT movement, represented in this study by the LGBT Citizenship Promotion Reference Center (CRLGBT), aiming to refer participants.
The sampling execution was built using the “snowball” technique, which is indicated for rare or unknown populations, or with special characteristics, or when there is no list of its members, making access and approach difficult. Initially, key informants were utilized, sourced from the CRLGBT, who constituted the first seeds of the study (zero wave), in order to locate other MSM participants for the research. Then, these seeds were asked to indicate new contacts with the desired characteristics from their own personal network, and so on, new waves were established until the sample frame reached its planned size. It is emphasized that with the collaboration/information from CRLGBT, four socializing venues of the study's target population (bars, squares) were visited, located in different geographic areas of the municipality, where new seeds were found.
Statistical Data Analysis
The data were analyzed using the Statistical Package for the Social Sciences (SPSS) software, version 26.0. It is emphasized that some variables were recategorized to enable the basic assumptions of the statistical tests. Descriptive analysis used frequency distribution, measures of position, and dispersion. The Shapiro-Wilk test was applied to verify the assumption of normal distribution of continuous quantitative variables.
To explain the joint effect of predictor variables on the response variable, Multiple Logistic Regression (MLR) was used with odds ratios and respective confidence intervals. The criterion for including variables in the logistic model was the association at the 20% level (P < .200) in the univariate analysis. The permanence of variables in the model, in turn, was association at the 5% level (P < .05). The final MLR model was adjusted by the Enter method, which forces the entry of all variables into the model. Multicollinearity of explanatory variables was checked by the VIF (Variance Inflation Factor) test, adopting a cutoff point of VIF above four. 20
Ethical Approval and Informed Consent
Participants were invited to voluntarily participate in the research after reading and signing the Informed Consent Form (ICF) and receiving a copy of the ICF. The research was conducted in accordance with Resolution 466/12 of the National Health Council, which defines the ethical aspects of research involving human subjects. It was approved by the Ethics and Research Committee of the Federal University of Piauí, Brazil, under protocol number 6.415.820.
Results
A total of 199 MSM were approached, with eight excluded for being on PrEP, seven testing positive for HIV, and 40 refusing testing, resulting in a final sample of 144 MSM, as planned.
The sample of MSM had an average age of 26.4 years (SD = 6.0), with the vast majority identifying as male (99.3%), cisgender male (91.7%), homosexual (72.2%), with an average family income of R$ 4878.00; an average of 18.2 years of education, and living with parents or relatives (67.4%) (Table 1).
Description of Personal Characteristics in the Sample. Teresina/PI – 2023 (n = 144).
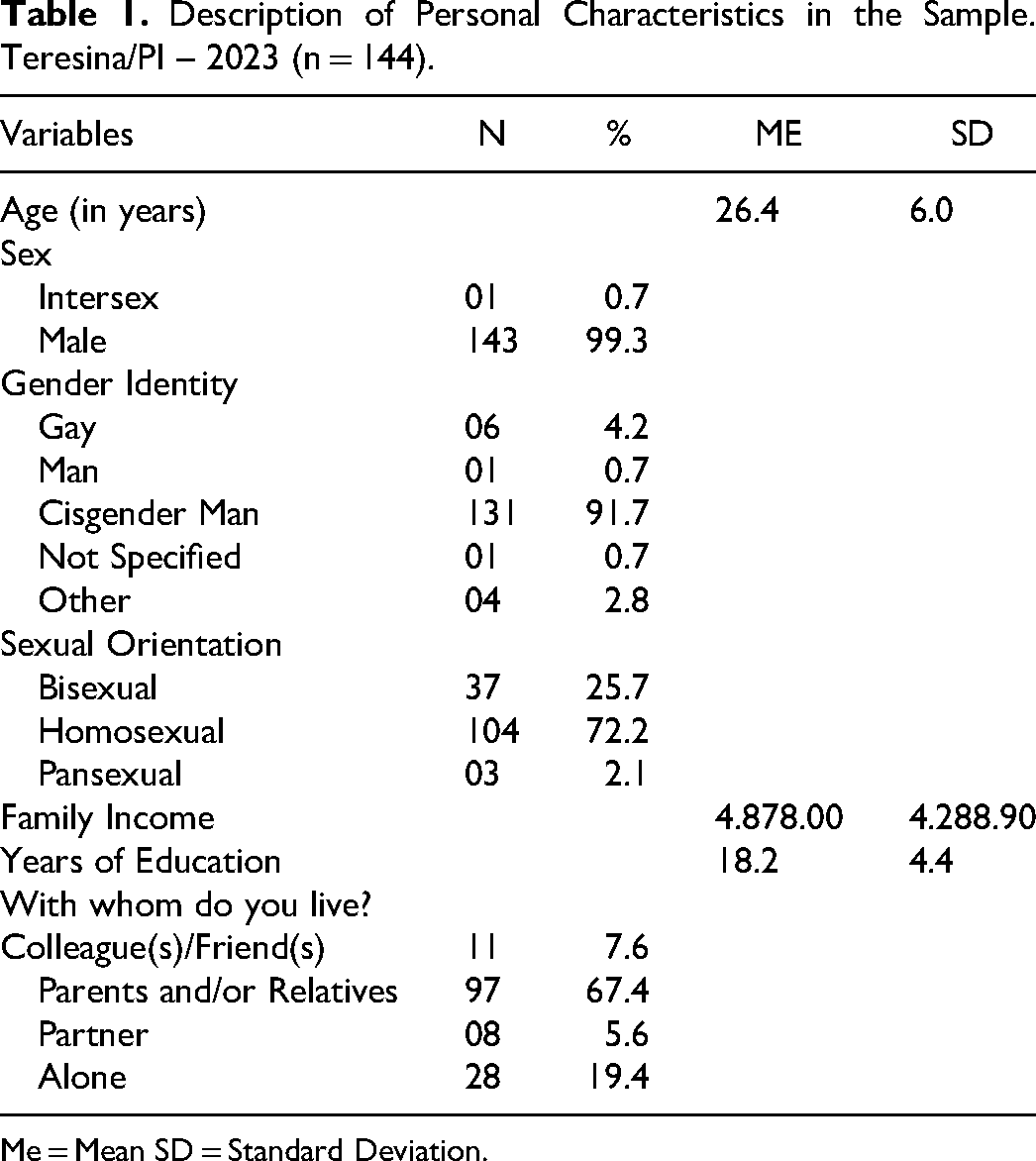
Me = Mean SD = Standard Deviation.
When asked about sexual practices, 37.9% reported using condoms in sexual relations with a steady partner, and 69.4% with casual partners, but the majority of them primarily had steady partnerships (40.3%). The use of dating apps was prevalent at 56.3%, through which they met their sexual partners. The main measure adopted to prevent STIs was condom use (90.3%), followed by testing (32.6%). They reported an average of six sexual partners in the last 12 months, with whom they engaged in penetrative sex, with 41.7% unaware of the partner's serological status. However, 33.3% stated they would engage in a relationship with a known HIV-positive person. Also in the last 12 months, 84% engaged in oral sex and anal sex (79.2%) as the insertive partner with a person of the same sex, and 12.5% visited gay saunas, adult theaters, gay bars, or other cruising spots. Group sex was also part of the sample's sexual practices (47.2%). Condom use is predominant in anal relations (93.8%); however, in oral and vaginal sexual relations, only 6.9% and 15.3% use condoms, respectively. Alcohol use before sexual relations was reported by a significant portion of the sample (57.7%), and illicit drugs by 18.7%, with marijuana being the most commonly reported (18.8%) (Table 2).
Description of Sexual Practices in the Study Sample of MSM. Teresina/PI – 2023 (n = 144).

Me = Mean SD = Standard Deviation.
In the reduced model, the variables that remained statistically associated with unsatisfactory perception of HIV risk were family income, non-penetrative sex, engaging with known HIV-positive individuals, and using illicit drugs before/while having sex. Family income revealed a negative association, meaning that for every thousand reais increase, the chances of an unsatisfactory perception of HIV risk decreased by 86% (P = .046). Conversely, non-penetrative sex as an HIV preventive measure increased the chances of having an unsatisfactory risk perception by 1.45 times (P = .04), engaging with known HIV-positive however, without knowledge of their viral load individuals increased it by 2.7 times (ORa = 2.70; P = .043), and using illicit drugs before/during sex increased the chances by 29% (ORa = 0.29; P = .048) (Table 3).
Logistic Models for Unsatisfactory Perception of HIV Risk in the Study Sample. Teresina/PI – 2023 (n = 144).
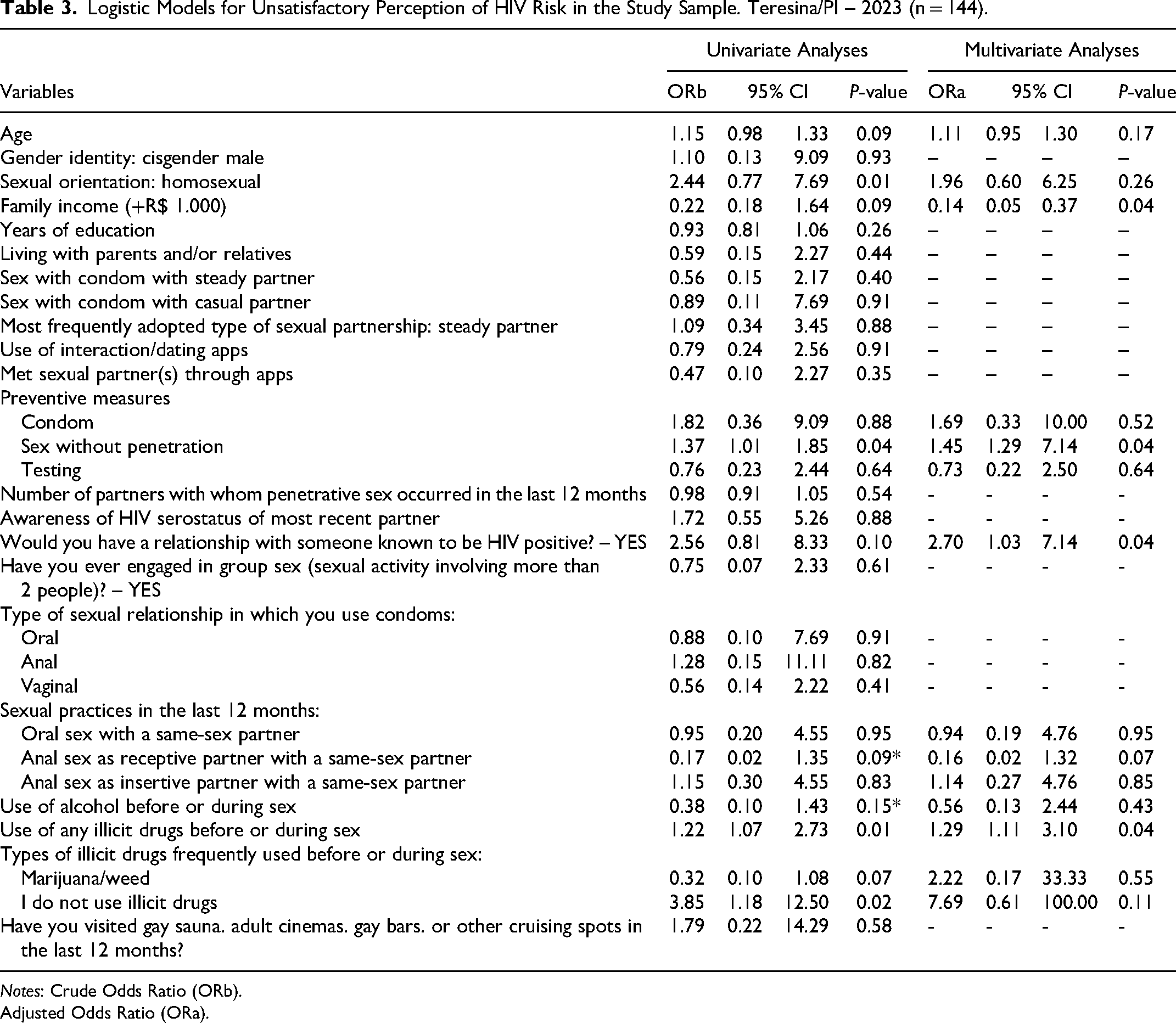
Notes: Crude Odds Ratio (ORb).
Adjusted Odds Ratio (ORa).
Discussion
This study presents significant findings regarding the sexual practices of the studied MSM and the factors influencing their unsatisfactory perception of HIV risk. In general, factors such as family income, engaging in non-penetrative sex as an HIV preventive measure, interacting with known HIV-positive individuals, and using illicit drugs during sex were linked to a higher likelihood of having an unsatisfactory perception of HIV risk.
The descriptive analysis of the sexual practices of MSM indicated that although most MSM reported using condoms during anal sex (93.8%), this usage is much lower for other practices, such as oral sex (6.9%). This points to a selective behavior that may contribute to a misguided perception of the protection offered by condoms, depending on the type of sexual practice.21‐24 The selectivity in condom use also varied according to the type of partner, with significantly higher usage among casual partners compared to steady partners, suggesting a false perception of security associated with steady relationships.23,25
Only 9% of the sample has a satisfactory perception of HIV risk, highlighting the need for targeted actions for this population. This finding is concerning and can be explained by a series of behavioral, social, and structural factors, 26 and is consistent with a cross-sectional study conducted with MSM in three Brazilian municipalities, which revealed that less than 5% of participants consider themselves at high risk for HIV infection. 27 Therefore, it is essential and urgent to implement health education interventions targeting this population to raise awareness about HIV infection. 28
The multivariate analysis revealed several factors that influence the unsatisfactory perception of HIV risk in this population, which will be discussed below.
Initially, there is a notable negative correlation between family income and an unsatisfactory perception of HIV risk, indicating that the chances of an unsatisfactory risk perception decreased by 86% (P = .046) for each additional thousand reais in family income. Although this finding is peculiar, it suggests that MSM with higher family income may have better access to health information, preventive resources, and health services such as PrEP and PEP, which improves their understanding and perception of the risks associated with HIV.24,29,30 These findings are reinforced by the most recent Brazilian epidemiological bulletins, which point to a concentration of the main prevention strategies among higher-income MSM. 31
On the other hand, the practice of non-penetrative sex as a preventive measure was associated with a 1.45-fold increase in the chances of having an unsatisfactory perception of HIV risk (P = .04). This finding is concerning as it indicates that a significant portion of MSM may mistakenly consider non-penetrative sex as a sufficient preventive measure against HIV infection. Although the risk of HIV transmission through non-penetrative sex is lower, it is not nonexistent and should be considered.32,33 Additionally, non-penetrative sex refers only to penile penetration, while a variety of other challenging practices can increase the risk of injury, diminish the perception of safety, and expose MSM to HIV and other STIs.25,27
Another interesting finding of this study was a 2.7-fold increase in the likelihood of having an unsatisfactory perception of HIV risk for those who reported engaging with a known HIV-positive person without knowledge of their viral load. This result can be explained by the lack of understanding of the concept “undetectable = untransmittable” (U = U), which has proven fundamental for HIV prevention, 34 improving the quality of life for people living with HIV/AIDS, and reducing stigma in this population.
Our main hypothesis for this finding is that the absence of broader discussions on the topic may lead some MSM to be unaware or not fully understand that a person with HIV who maintains an undetectable viral load through antiretroviral treatment does not transmit the virus to sexual partners.34,35 Thus, the lack of knowledge about U = U can lead to unfounded and misguided fears and an unsatisfactory perception of risk, even when engaging in relationships with HIV-positive partners who are on effective treatment. Implementing educational strategies that promote knowledge about U = U and encourage regular testing and effective treatment can be crucial in improving the perception of HIV risk.33‐35
An additional significant component identified was the use of illicit drugs before or during sexual activity, also known as “chemsex.” 36 This practice increased the likelihood of having an inadequate perception of HIV risk by 29% (ORa = 0.29; P = .048). A low perception of HIV risk can result in the use of illicit substances, with 18.8% of participants reporting drug use. This can also impair judgment and lead to unsafe sexual behaviors, such as not using condoms. Drug use tends to prolong sexual experiences, thereby increasing the number of partners per session and the prevalence of high-risk sexual behaviors.36,37
Research suggests that drug use in conjunction with sexual activity is common among MSM in Brazil, 38 which may, among other issues, affect the negotiation of condom use during sexual activity. An online study conducted in Amsterdam involving 290 middle-aged MSM found a chemsex prevalence rate of 11.4%. Chemsex involves using drugs to engage in sexual activity with multiple people over an extended period, ranging from several hours to several days. Three primary types of drugs are associated with chemsex: methamphetamines, mephedrone, and GHB/GBL (gamma-hydroxybutyric acid/gamma-butyrolactone), with GHB being the most commonly used drug. 39
The consumption of illicit drugs during sexual relations has often been associated with casual sex practices, shaping lifestyles with higher risk and modes of social and affective interaction between partners who aim to become more uninhibited and free from sexual taboos. This type of behavior exploded in Europe over a decade ago, and currently, experts have been observing growth in Brazil as well, especially after the COVID-19 pandemic, which becomes a major concern for health authorities as it can pose a significant risk to the progress of HIV prevention achieved over the years.36‐39
Our findings highlight the need for more targeted and comprehensive public health initiatives that not only encourage the regular use of condoms but also educate people about the modes of HIV transmission and discourage the use of drugs that impair judgment during sexual activity.40‐42 Prevention campaigns should be specifically designed to demystify the safety of relationships with HIV-positive partners and non-penetrative sex. To ensure that accurate information and preventive resources reach all parts of the MSM community, it is imperative that these interventions be accessible to all income levels and culturally sensitive.41,42
Limitations
The main limitation of this study was the sample's resistance to HIV testing, which was a criterion for inclusion/exclusion in the study. However, this was successfully addressed without detriment to the study after providing intensive information. The sampling approach using the snowball technique imposes limitations on the generalization of results to the broader MSM population in the capital. However, it is important to note that strategies were implemented to mitigate this potential issue, such as seeking seeds in various parts of the city, which facilitated capturing diverse profiles.
Conclusions
We have observed a low perception of HIV risk among a sample of MSM, a growing use of illicit drugs during sex, and engagement in high-risk sexual behaviors such as unprotected anal sex. These findings underscore the urgent need for targeted interventions for this vulnerable population.
It is crucial to develop and implement health programs specifically tailored to MSM, addressing not only HIV prevention but also drug use, mental health, and overall well-being. These interventions should be adapted to the specific needs of this population and be accessible and culturally sensitive.
Supplemental Material
sj-docx-1-jia-10.1177_23259582241283196 - Supplemental material for Sexual Practices and HIV Risk Perception Among Men Who Have Sex with Men in Brazil
Supplemental material, sj-docx-1-jia-10.1177_23259582241283196 for Sexual Practices and HIV Risk Perception Among Men Who Have Sex with Men in Brazil by Telma Maria Evangelista de Araújo, Fernanda Raquel Costa Chaves, Mônica Graziela França Uchôa de Oliveira, André Felipe de Castro Pereira Chaves, Yndiara Kássia da Cunha Soares, Paulo de Tarso Moura Borges, Saulo Evangelista Moura Borges, Vitor Monte de Castro Alencar, Emerson Lucas Silva Camargo, Isabel Amélia Costa Mendes and Álvaro Francisco Lopes de Sousa in Journal of the International Association of Providers of AIDS Care (JIAPAC)
Supplemental Material
sj-docx-2-jia-10.1177_23259582241283196 - Supplemental material for Sexual Practices and HIV Risk Perception Among Men Who Have Sex with Men in Brazil
Supplemental material, sj-docx-2-jia-10.1177_23259582241283196 for Sexual Practices and HIV Risk Perception Among Men Who Have Sex with Men in Brazil by Telma Maria Evangelista de Araújo, Fernanda Raquel Costa Chaves, Mônica Graziela França Uchôa de Oliveira, André Felipe de Castro Pereira Chaves, Yndiara Kássia da Cunha Soares, Paulo de Tarso Moura Borges, Saulo Evangelista Moura Borges, Vitor Monte de Castro Alencar, Emerson Lucas Silva Camargo, Isabel Amélia Costa Mendes and Álvaro Francisco Lopes de Sousa in Journal of the International Association of Providers of AIDS Care (JIAPAC)
Footnotes
Acknowledgments
Does not apply.
Author Contributions
Conceptualization, study design, data acquisition, data analysis, interpretation of results, and drafted the manuscript: Araújo, Chaves, Oliveira, Chaves, Soares, Borges, Borges, Alencar, Camargo, Mendes, Sousa. Revised manuscript: Araújo, Chaves, Oliveira, Chaves, Soares, Borges, Borges, Alencar, Camargo, Sousa. All authors approved the final version and all authors agree to be accountable for all aspects of this work
Availability of Data and Material
Available upon request to the corresponding author.
Consent for Publication
Does not apply
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Coordination for the Improvement of Higher Education Personnel (CAPES), Grant/Award Number: 001-2023.
Ethics Approval and Consent to Participate
This study followed the ethical principles of research involving human beings established by Resolution 466/2012 of the National Health Council (CNS) and by the Declaration of Helsinki. The research was approved by the Ethics and Research Committee of the Federal University of Piauí, under opinion 6,415,820. The professionals who agreed to participate in the study signed the Informed Consent.
ORCID iDs
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.