Abstract
Blastomycosis is a rare endemic fungal infection caused by the dimorphic fungus Blastomyces dermatitidis. It is more likely to occur in persons living in areas of the United States and Canada, which border the Ohio and Mississippi River Valleys and the Great Lakes region. Most infections are localized to the lungs, often presenting as acute or chronic pneumonia. Occasionally, patients progress to develop disseminated disease and extrapulmonary infections. Blastomycosis tends to be misdiagnosed initially at clinical evaluation as it is rare and may resemble other common conditions. We present a case of a 78-year-old immunosuppressed renal transplant patient who was suspected of having gout but eventually was diagnosed with an unusual presentation of septic arthritis of the ankle secondary to blastomycosis.
Keywords
Introduction
Blastomyces dermatitidis, a dimorphic fungus, is the causative agent of blastomycosis, an uncommon disease that affects both immunocompetent and immunosuppressed hosts. The infection is prevalent in endemic regions of B dermatitidis, which border the Ohio and Mississippi River Valleys and the Great Lakes Region, including the midwestern, south-central, and southeastern United States and 4 Canadian provinces spanning Saskatchewan to Quebec.1,2 Within these endemic regions, B dermatitidis grows in specific environments, including soils and decaying organic matter located near water sources. Infection is frequently established in persons exposed to these environments through occupational or recreational activities, particularly following events that disrupt the soil and allow for aerosolization and inhalation of spores, although skin inoculation secondary to trauma may occur less frequently. 2 Of those infected, approximately 50% will develop manifestations of the disease, whereas others will have subclinical or asymptomatic infections. 1
Of those who develop symptomatic infections, the majority will be localized to the lungs and present acutely with constitutional symptoms and pneumonia, or less commonly as acute respiratory distress syndrome. If left untreated, the infection may progress to chronic pneumonia accompanied by weight loss, night sweats, and hemoptysis.2,3 Severe pulmonary infection is more likely to occur in immunosuppressed patients; however, it has been noted in the immunocompetent hosts and likely results from exposure to large infectious doses. In 25% to 30% of cases, even following resolution of a pulmonary infection, B dermatitidis will disseminate to other organs and manifest as extrapulmonary disease, particularly in the immunosuppressed. Cutaneous manifestations are common and occur in 40% to 80% of disseminated cases, presenting as multiple papulopustular, ulcerated, or verrucous lesions on exposed areas and less frequently in the oral, nasal, and pharyngeal mucosa. Osseous involvement manifests as osteomyelitis in 5% to 25% of cases and tends to involve the long bones, vertebra, skull, and ribs in order of frequency. 4 Septic arthritis may occur through direct extension of B dermatitidis into the joint space or via hematogenous spread. 2 Genitourinary involvement manifesting as prostatitis and epididymitis occurs in 10% of male cases, while tubo-ovarian abscesses, endometritis, and salpingitis have been reported in female cases. Central nervous system involvement occurs in less than 5% to 10% of cases and manifests as meningitis or intracranial abscesses. 4
As blastomycosis is a relatively rare infection with numerous manifestations, it tends to be misdiagnosed initially upon clinical evaluation. Clinicians, particularly those practicing in the endemic areas of B dermatitidis, should be cognizant of the clinical manifestations of the disease. We present a case of a 78-year-old immunosuppressed renal transplant patient with an atypical extrapulmonary infection of B dermatitidis. He was initially suspected of having gout; however, when pain medications, oral corticosteroids, and a xanthine oxidase inhibitor failed to improve his symptoms, he was reevaluated and diagnosed with septic arthritis of the ankle secondary to blastomycosis.
Case Presentation
We present a case of 78-year-old man who is a renal transplant recipient maintained on immunosuppressive therapy of mycophenolate and tacrolimus. He has a history of gout; basal cell carcinoma, for which he received extensive Mohs surgery; and end-stage kidney disease due to polycystic kidney disease, for which he received a living-related donor renal transplant 25 years ago. The patient initially presented to his physician with complaints of left ankle pain and swelling for more than 6 months. He was thought to have left Achilles tendinitis. He was referred to podiatry and physical therapy. However, due to no improvement in his symptoms, crystal-induced arthropathy was considered. He was managed with pain medications, a xanthine oxidase inhibitor, and oral steroids, but again his symptoms did not improve. He underwent a left lower extremity magnetic resonance imaging (MRI) (Figure 1), which revealed some enhancement but no fluid collection. He ultimately underwent incision and debridement of his left ankle. Only 1 of the 4 tissue sample cultures grew Staphylococccus epidermidis in broth media, which was deemed to be a contaminant. Histopathology eventually revealed the presence of broad-based budding yeast consistent with B dermatitidis (Figure 2). Antimicrobials were switched to itraconazole, as the patient was reluctant to take amphotericin B due to its potential for nephrotoxicity. Swelling improved but he continued to have joint pain affecting his quality of life. He eventually underwent below-the-knee amputation after 3 months of therapy with documented therapeutic levels of itraconazole, which failed to resolve his symptoms. His B dermatitidis urine and serum antigens remain positive and he continues to be on itraconazole 18 months since his diagnosis.
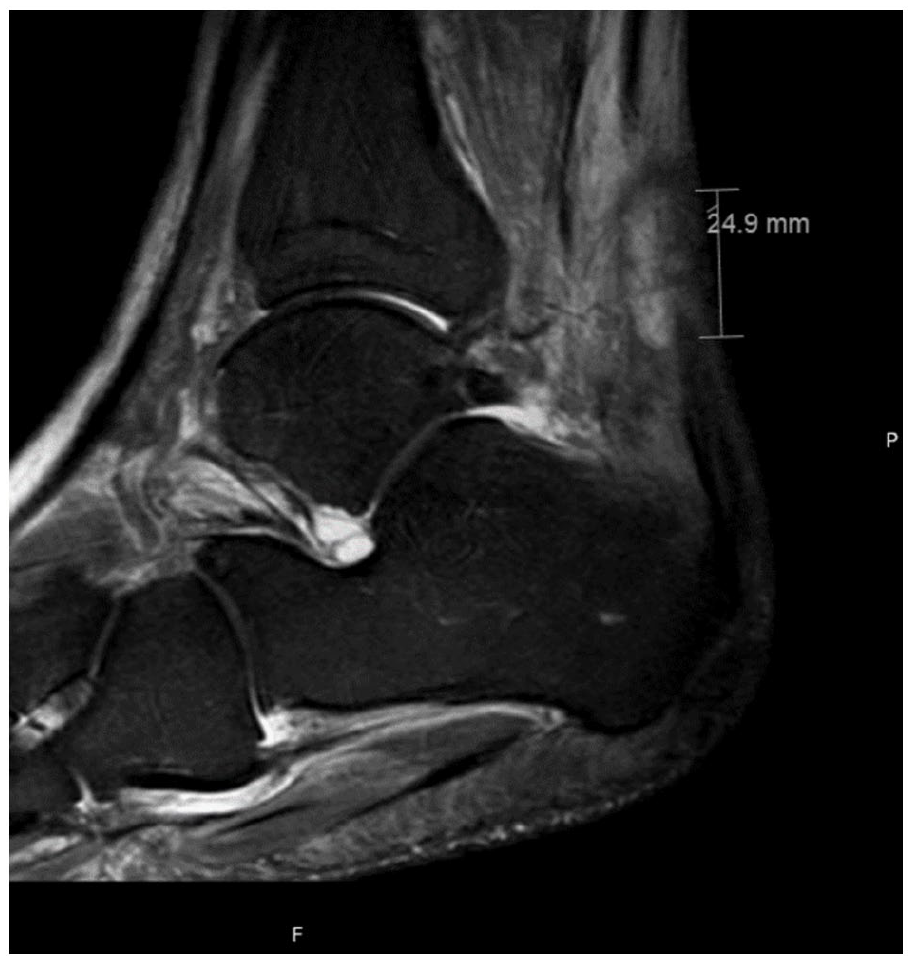
Magnetic resonance imaging of the left ankle showing fluid collection in the peritendinous location, along the anterior and lateral aspect of the Achilles tendon.

Grocott-Gomori’s methenamine silver stain of numerous monomorphic yeast demonstrating broad-based budding, morphologically consistent with Blastomyces sp.
Discussion
This case highlights an atypical presentation of extrapulmonary B dermatitidis infection in an immunosuppressed patient. This patient developed septic arthritis secondary to disseminated blastomycosis, which was confirmed by histopathological evidence of broad-based budding yeast and serological evidence of B dermatitis infection.
Blastomycosis typically begins with constitutional symptoms, such as malaise, fever, and chills. 3 As infection is most frequently established in the respiratory tract, patients may experience pneumonia or more frequently remain asymptomatic, as seen in our patient. Once B dermatitidis is within the alveolar macrophages, the infection may be controlled or disseminate depending on the efficiency of the host immune response. 2 Given our patient’s immunosuppressed status, dissemination is not unexpected. Both mycophenolate and tacrolimus can lead to infections including fungal infection. The latter has a boxed warning for increased risk of developing serious infections and malignancies that may lead to hospitalization or death. Once dissemination of infection occurs, the most frequent manifestations include cutaneous lesions and osteomyelitis, which did not occur in our patient. Instead, he experienced septic arthritis, which is uncommon and rarely has been reported as an isolated manifestation of disseminated disease in the literature. Of the reported cases, septic arthritis due to B dermatitidis is commonly monoarticular, frequently involving the knee, hip, ankle, or elbow, and presents acutely with severe pain, swelling, redness, warmth, and a restricted range of motion of the involved joint, often accompanied by a fever.5-9 Septic arthritis may progress to joint destruction and decreased function without treatment. 9 Although our patient presented with joint pain and swelling, it occurred over a period of 6 months and he lacked the typical signs of septic arthritis and disseminated B dermatitidis infection, such as a fever and cutaneous manifestations. These findings could be attributed to lower levels of inflammation caused by his immunosuppressed status and steroid use. This atypical presentation in the setting of immunosuppression is consistent with the diagnosis of osteoarticular blastomycosis.
In our case, there was a delay in the diagnosis of septic arthritis. Clinically, if blastomycosis is in the differential for septic arthritis, arthrocentesis with synovial fluid analysis should be performed. 9 Culturing the specimen may provide a definite diagnosis; however, since the organism is slow growing, cultures need to be incubated for up to 6 weeks. Histopathology from a tissue biopsy or cytology from synovial aspirate can provide a presumptive diagnosis based on the characteristic features of broad-based budding yeasts with a double-contoured cell wall morphology. 1 In addition, urine and serological assays may be used; however, they may be falsely negative in localized infections and are relatively nonspecific as cross-reaction with the Histoplasma capsulatum antigen occurs.1,4
Once infection is confirmed, treatment options for blastomycosis include antifungal chemotherapy. In those who are immunosuppressed or have disseminated or life-threatening infections, amphotericin B is the treatment of choice for 2 weeks or until clinical improvement. Thereafter and in cases with mild to moderate disease without dissemination, itraconazole is typically used for 6 to 12 months or for the remaining course of the infection. 1 Surgical irrigation and debridement are required if loculations are present, and amputation may be required in severe cases. 4 In our patient, prior to the diagnosis of B dermatitidis, the initial approach was focused on controlling his pain and swelling. However, after the diagnosis was made, itraconazole was used due to the potential nephrotoxic effects associated with amphotericin B and the patient’s preference for avoiding the need for renal replacement therapy in the form of hemodialysis.
Conclusion
Septic arthritis due to blastomycosis is rare and should be considered in any patient presenting with culture-negative monoarticular arthritis who lives within or recently traveled to an endemic area. Although septic arthritis in blastomycosis tends to present acutely with constitutional symptoms, respiratory involvement, and characteristic cutaneous lesions, it may follow an atypical presentation. Our case depicted an unusual presentation of osteoarticular blastomycosis in an immunosuppressed patient, manifesting solely as chronic joint pain and swelling. These atypical cases of osteoarticular blastomycosis may be difficult for clinicians to diagnose and are prone to common cognitive errors, such as anchoring bias. Recognizing the varied clinical presentations of blastomycosis provided with a high degree of suspicion in the right clinical context may lead to early diagnosis and treatment, which is essential to limit morbidity and mortality in the affected patients.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Prior Presentation of Abstract Statement
Abstract was presented at 2022 Midwest Clinical and Translational Research Meeting (sponsored by Midwest AFMR and CSCTR), March 3-4, 2022, Chicago, Illinois.
Ethics Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
