Abstract
The development of metastatic cutaneous squamous cell carcinoma in an otherwise healthy and young individual should prompt physicians to investigate for an underlying cause of immunosuppression. The following case presents an individual who underwent Mohs surgery of a poorly differentiated squamous cell carcinoma. Four months following Mohs surgery, the patient presented with lymphadenopathy and new skin nodules. Metastatic disease or infection were included in the differential diagnosis. An immunosuppression work-up was completed and the patient was diagnosed with human immunodeficiency virus (HIV). Treatment with antiretroviral therapy was initiated 1 month prior to treatment of the metastatic disease with an immunomodulator, cemimplimab-rwlc. This contribution highlights the importance of determining the immunological status of a patient who presents with metastatic disease following a complete tumor clearance.
Keywords
A 56-year-old man with a history of cutaneous squamous cell carcinoma, presented to the clinic with a 0.9 × 0.5 × 0.2 cm lesion on his right superomedial forehead (see Figure 1). Histologic sections demonstrated nests of atypical squamous cells extending into the dermis. A diagnosis of moderately to well-differentiated, invasive squamous cell carcinoma was made. Mohs surgery was performed and histologic subtype was found to be poorly differentiated squamous cell carcinoma. Five stages were required for tumor clearance (see Figure 2). At the time of Mohs surgery, there was no palpable lymphadenopathy. After second intent healing for several weeks to achieve granulation, a full thickness skin graft was used to repair the defect. The postoperative course was complicated by prolonged wound healing and hypergranulation. He was treated with fractionated Er: Yag laser and standard wound care measures every 2 weeks until the lesion was nearly healed.

Poorly differentiated cutaneous squamous cell carcinoma.

Five stages of Mohs surgery were required for tumor clearance.
Four months following Mohs surgery, the patient presented with new nodules lateral to the skin graft and associated right preauricular lymphadenopathy (see Figure 3). Differential diagnosis included metastasis versus bacterial infection. Cultures and biopsy were obtained. Biopsy of the 0.5 × 0.5 × 0.5 cm lesion showed irregular lobules of atypical squamous epithelium within the dermis, and an epidermal connection was not identified, which was concerning for metastasis. Subsequent imaging and a right preauricular lymph node fine needle aspiration were consistent with metastatic squamous cell carcinoma. A positron emission tomography scan and computed tomography scan were performed. Imaging was significant for increased uptake in the submandibular, tubular gastric, and posterior cervical regions bilaterally, and the lymph nodes adjacent to the subclavian vessels in the upper chest. These findings were consistent with extensive metastatic squamous cell carcinoma in the head, neck, and upper chest.
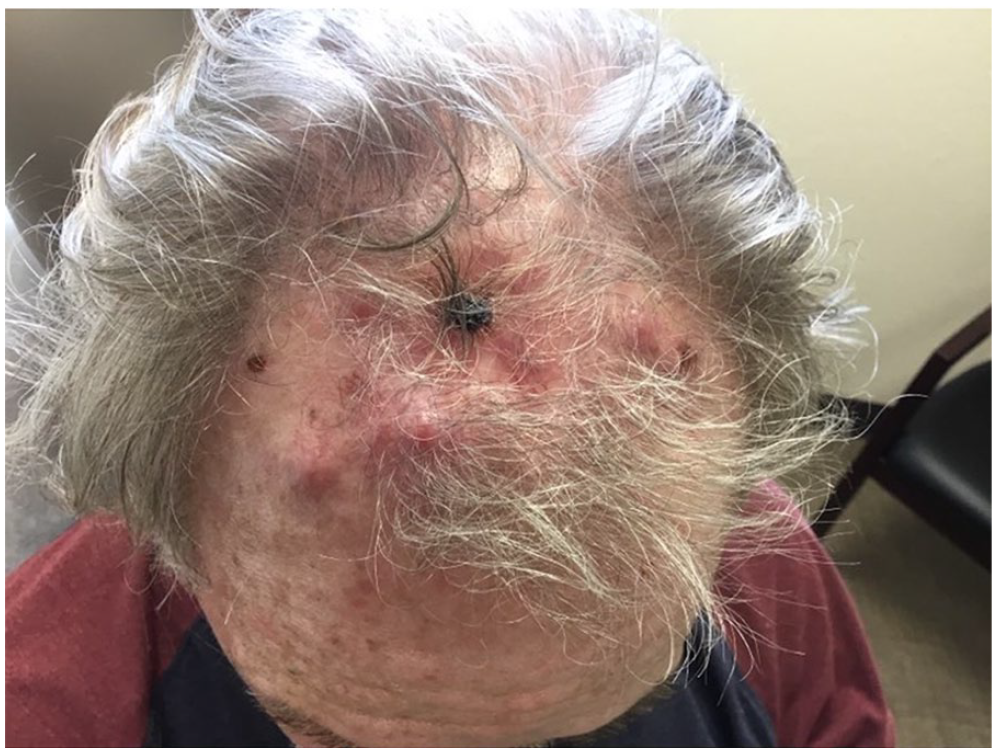
Metastatic cutaneous squamous cell carcinoma.
An immunosuppression work-up was completed following poor wound healing and metastasis. A complete blood count, which was within normal limits, was completed to rule out lymphoma. Although the patient denied human immunodeficiency virus (HIV) risk factors, due to employment as a surgical scrub technician, HIV testing was initiated. The patient tested positive for HIV-1, and his CD4+ T-cell count was 190 cells/mm3. Infectious disease and oncology were consulted. He began antiretroviral therapy with bictegravir, emtricitabine and tenofovir alafenamide 1 month prior to starting treatment for the metastatic disease with cemiplimab-rwlc, an immunomodulator. The patient has completed his course of immunotherapy. His HIV remains well-controlled, and there have been no signs or symptoms of metastatic disease. He continues regular follow-up with oncology, dermatology, and infectious disease.
Discussion
The patient’s delayed wound healing and skin findings after the initial excision of the cutaneous squamous cell carcinoma were concerning for immunosuppression. Patients diagnosed with HIV have been shown to have a 5.4-fold increased risk of developing cutaneous squamous cell carcinoma when compared to the general population. 1 Our patient’s diagnosis of HIV-1 explained the aggressive nature of his squamous cell carcinoma and lymphadenopathy.
A diagnosis of HIV limits the treatment for metastatic cancer. A similar patient with HIV was diagnosed with a well-differentiated squamous cell carcinoma located on his scalp. Six months later, the disease had invaded the parietal bone. Chemotherapy was no longer an option for the patient due to his weakened immune system. 2 Treating disease early in immunosuppressed individuals is necessary to maintain control of the metastatic disease. Treating our patient’s metastatic disease posed great risks due to the HIV infection. Antiretroviral therapy was initiated to increase the CD4+ T-cell count prior to starting the patient on cemiplimab-rwlc. Cemiplimab-rwlc, a monoclonal antibody, acts by binding to PD-1 receptors found on CD4+ T-cells to prevent the inactivation of T-cells. 3
A concern following the initiation of HIV treatment was the development of immune reconstitution inflammatory syndrome (IRIS). Starting immunotherapy while on antiretroviral therapy increased his risk of developing a massive immune response. IRIS occurs in patients with HIV and involves the worsening of preexisting infectious processes after the onset of antiretroviral therapy. Patients may present with new or worsening symptoms following treatment initiation. 4 In this patient, IRIS would have likely targeted the tumor antigens. His risk of developing IRIS prompted a delay in starting immunotherapy, which proved to be beneficial.
This patient’s acquired immunodeficiency syndrome (AIDS)-defining illness was metastatic squamous cell carcinoma. This case is an example of how HIV may not present with general symptoms, such as fever and malaise. Metastatic disease should prompt physicians to investigate a potential underlying cause, such as immunosuppression. Considerations also need to be made in the initiation of immunomodulators in the setting of underlying HIV.
Footnotes
Acknowledgements
The authors would like to acknowledge assistance from the Skin Cancer and Dermatology Institute and the University of Nevada, Reno School of Medicine.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
Verbal informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
