Abstract
Aim:
The aim of this study was to evaluate the effect of desensitizer, temporary cements, dentin cleaning methods on shear bond strength (SBS) of self-etch and self-adhesive resin cements to dentin.
Materials and Methods:
Four hundred eighty buccal or lingual/palatine coronal portions of human molar teeth were mounted in the acrylic blocks. Teeth surfaces were prepared until the dentin was exposed. Specimens were divided into four groups. One group separated as control and three groups of teeth were treated with a desensitizing agent containing calcium-phosphate desensitizer (Teethmate Desensitizer, TMD), resin-based self-reinforcing monomer (Shield Force Plus, SFP) and 2-hydroxyethyl methacrylate and glutaraldehyde (Gluma Desensitizer). Two different temporary cement containing calcium hydroxide (Dycall) and zinc oxide based (Rely X Temp NE) temporary cement were applied to the dentin surfaces. Temporary cement was removed with one of three cleansing techniques: 2% chlorhexidine digluconate and glass particles containing agent (Consepsis Scrub), cleansing bur (OptiClean), and ıntra/extracoronal rotary brush (Starbrush). All groups were further divided into two cementation subgroups (Panavia V5 and Panavia SA). The SBS (MPa) was measured using a universal testing machine at 0.5 mm/min crosshead speed. The data were analyzed statistically with a four-way analysis of variance and Tukey’s Honest Significant Difference test (α = 0.05).
Results:
Although SFP showed higher SBS, there was no statistically significant difference between other groups (P > .05). There were no significant differences between temporary cements (P > .05). OptiClean rotary bur showed higher mean SBS values in all groups. The dual-polymerized Panavia V5 showed the highest SBS values in all groups (P <.05).
Conclusion:
Cleaning of dentin surface from temporary cement remnants with a silicon bur and dual-cure resin cement showed the highest bond strength values.
Introduction
Dentin hypersensitivity may occur after tooth preparation or cementation procedures because of exposed dentin tubules. Desensitizing agents are used to decrease or prevent dentin hypersensitivity. Mechanism of desensitizer is by the way of occluding or sealing of dentin tubules.1, 2 Several treatment methods such as tubular obturating and surface covering procedures, adhesives, anti-inflammatory agents, and lasers may be applied to the sensitive surface after tooth preparation. 3
A durable cementation is crucial for long-term restoration survival, marginal sealing, and strong adhesion. Today, resin cements are indispensable in the cementation of restorations for a strong adhesion.4–6 It was previously reported that adhesive cementation techniques improve the optical properties, fracture resistance, bond strength, and thereby improve clinical performance of metal-free restorations.7, 8 Improvements in the bonding characteristic of resin luting agents to dentin increases the success of restorations. 9 Resin cements are classified dual-cure, light-cure, and self-cure according to polymerization type; in addition also named total-etch, self-etch, and self-adhesive by their adhesive scheme. 6 Conventional resin cement application requires pretreatment of dentin surface, which is technique-sensitive and time-consuming. To reduce the sensitivity of cementation procedures, self-adhesive resin cements were recently developed, because they do not require pretreatment of dentin. Their adhesion mechanism is realized by the acidic monomers in its content infiltrated into the demineralized collagen network.6, 10 Adhesive resin cements exhibit low solubility and microleakage in the oral environment compared with traditional cements. 7 Resin cements adhesion to dentin might be adversely affected by the preparation design, preparation coarseness, contamination from blood and saliva, type of temporary cement, dentin surface cleaning techniques, desensitizing agents, and type of adhesive cements.11, 12
Provisional restorations are used to protect the pulp after the preparation and to meet the esthetic and functional needs of the patient, and these restorations are fixed onto teeth with temporary cement. 13 Eugenol-free zinc oxide and calcium hydroxide based temporary cements are most commonly used for provisional cementation. Temporary cement remnants of prepared teeth surface may have a negative effect on definitive adhesion.12–14 Rotary silicone bur, brushes, and chemical removal techniques have been used removing contaminated dentin surfaces to retrieve durable bond strength.13–15 Terata 16 indicated that mechanical removal of temporary cement remnants and debris with a dental probe was not completely effective. Chemical treatment after mechanical removal of cement significantly increased wettability and bonding values.11, 16
The aim of the present study was to investigate the effect of desensitizers, temporary cements, and cleaning methods on self-etch/adhesive resin cement shear bond strength (SBS) to dentin. The hypotheses of the study were planned to be such that SBS between dentin and resin cement would be affected by the type of temporary cement and dentin cleaning methods (H0) and would not be affected type of desensitizing agents (H1) and significant difference would be found between the resin cements in terms of SBS (H2).
Materials and Methods
Twenty hundred forty caries-free, extracted human molars were used in this study. Teeth were disinfected with 0.2% sodium azide for up to seven days, and stored subsequently in distilled water at 4°C until use. The roots of the teeth were cut away and the crowns were divided into two parts mesiodistally at the central groove under water cooling. Each part of the crown was embedded in a mold with the buccal or lingual surface facing upward using self-cure acrylic resin (Villacryl SP, Zhermack, Badia Polesine, Italy). Specimen surfaces were ground with a standard-grit diamond rotary cutting instrument (105–125 µm, Diatech) until dentin was exposed, then to obtain a standard smear layer, the surfaces were polished with 600 grit silicon carbide abrasive paper and were washed with ethylenediamine tetraacetic acid for 2 min to simulate sensitive dentin tubules.
The specimens were divided into four groups each containing 120 specimens. One group served as a control (C) and had no desensitizing agent. Calcium-phosphate based (Teethmate Desensitizer, T), self-reinforcing monomer (Shield Force Plus, S) and 2-hydroxyethyl methacrylate (HEMA), and glutaraldehyde (Gluma Desensitizer, G) desensitizers were applied to exposed dentin surfaces according to manufacturer instruction (Figure 1). All groups were divided further into two subgroups in which a calcium hydroxide (Dycall) or a zinc oxide (Rely X Temp NE) based temporary cement was applied to the dentin surfaces. To simulate temporary restoration, acrylic resin plates, 5×7×1 mm in dimension, were made with temporary restoration material (Imident, Imicryl, Konya, Turkey). Then, the acrylic resin plates were cemented to the dentin surfaces according to manufacturer’s instructions under 2.5-kg static load for 5 min. All specimens stored in distilled water at 37˚C ± 2˚C for 24 s. Acrylic resin plates were removed mechanically by using a carving instrument and rinsed with water until the dentin surface was macroscopically clean, then temporary cemented specimens were divided into three subgroups. Temporary cement residues were removed with one of three cleaning methods: 2% chlorhexidine gluconate and glass particles containing agent (Consepsis Scrub, C), cleaning bur (OptiClean, O), and intracoronal rotary brush (Starbrush, S). Consepsis Scrub was applied by using a rotary instrument with a rubber cup at 5000 rotations per minute (r/min) under water cooling. A-silicone coated cleaning bur and intracoronal rotary brush were used with a hand piece at 5000 r/min with water cooling for 15 s.
Schematic Diagram Showing the Method for Specimen Preparation
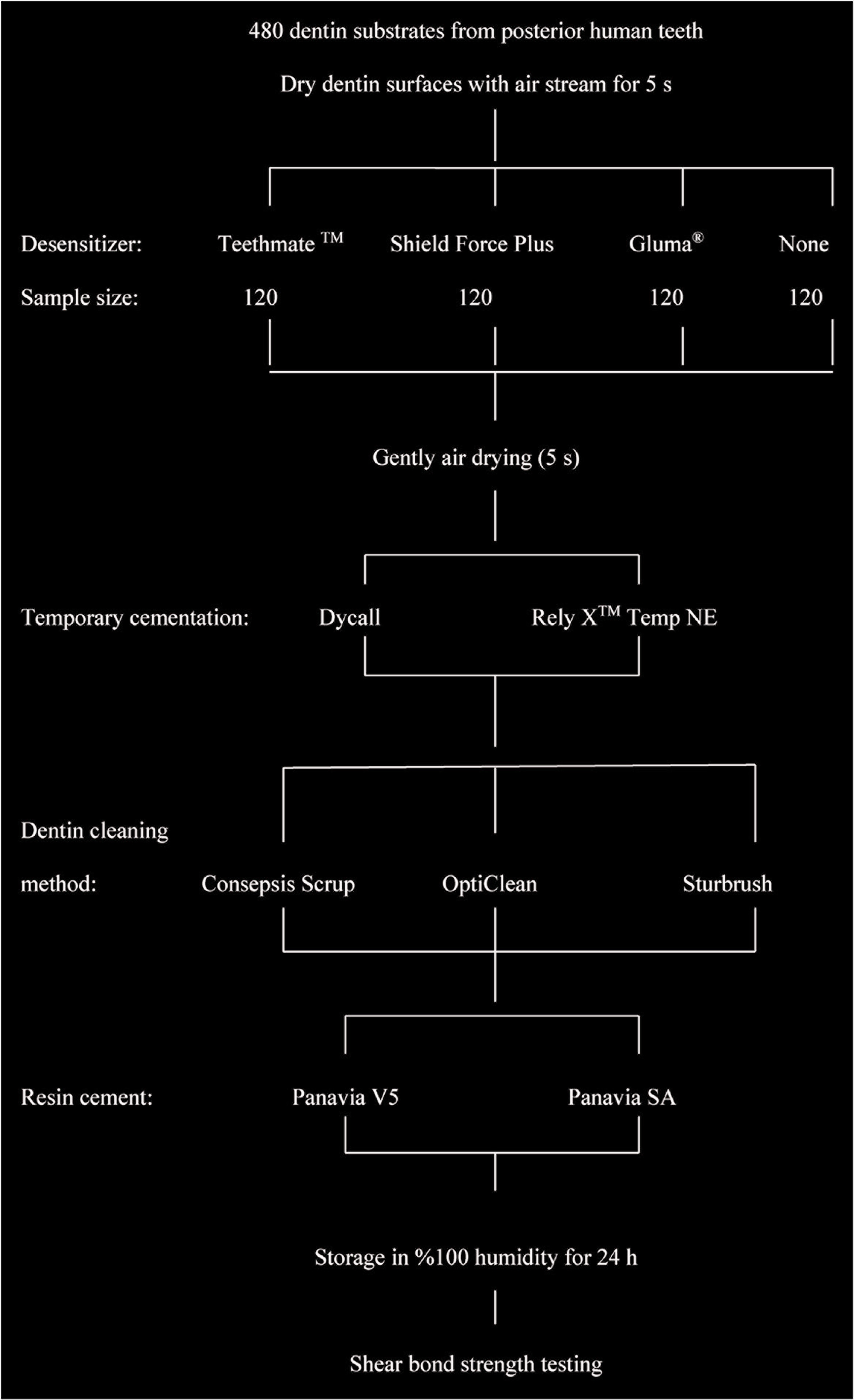
After applying the dentin cleaning methods, all groups were further divided into two subgroups (n = 10), in which a dual-cure resin cement (Panavia V5) or a self-adhesive resin cement (Panavia SA) was used. A transparent plastic mold with a hole (3-mm diameter and 2-mm height) was used to apply the resin cement to dentin surfaces. Materials used in this study are presented in Table 1. The specimens were stored in distilled water at 37°C for 24 h. After storage, SBS were tested in a universal machine (Instron Corp, Canton, MA, USA) at a crosshead speed of 0.5 mm/min. Fracture surfaces were examined with a stereomicroscope (Olympus SZ-4045 ESD, Tokyo, Japan) at a 30× magnification and the type of the failure was noted as adhesive, cohesive, or mixed (a combination of adhesive and cohesive failures). Kolmogorov–Smirnov test used to determine normal distribution and data were normal distribution (P > .05). Data were analyzed by four-way analysis of variance (SPSS version 21.0, SPSS Inc., Chicago IL, USA). Means and standard deviation of SBS were calculated, and mean values were compared by the Tukey’s Honest Significant Difference test (α = .05).
Materials Used in This Study
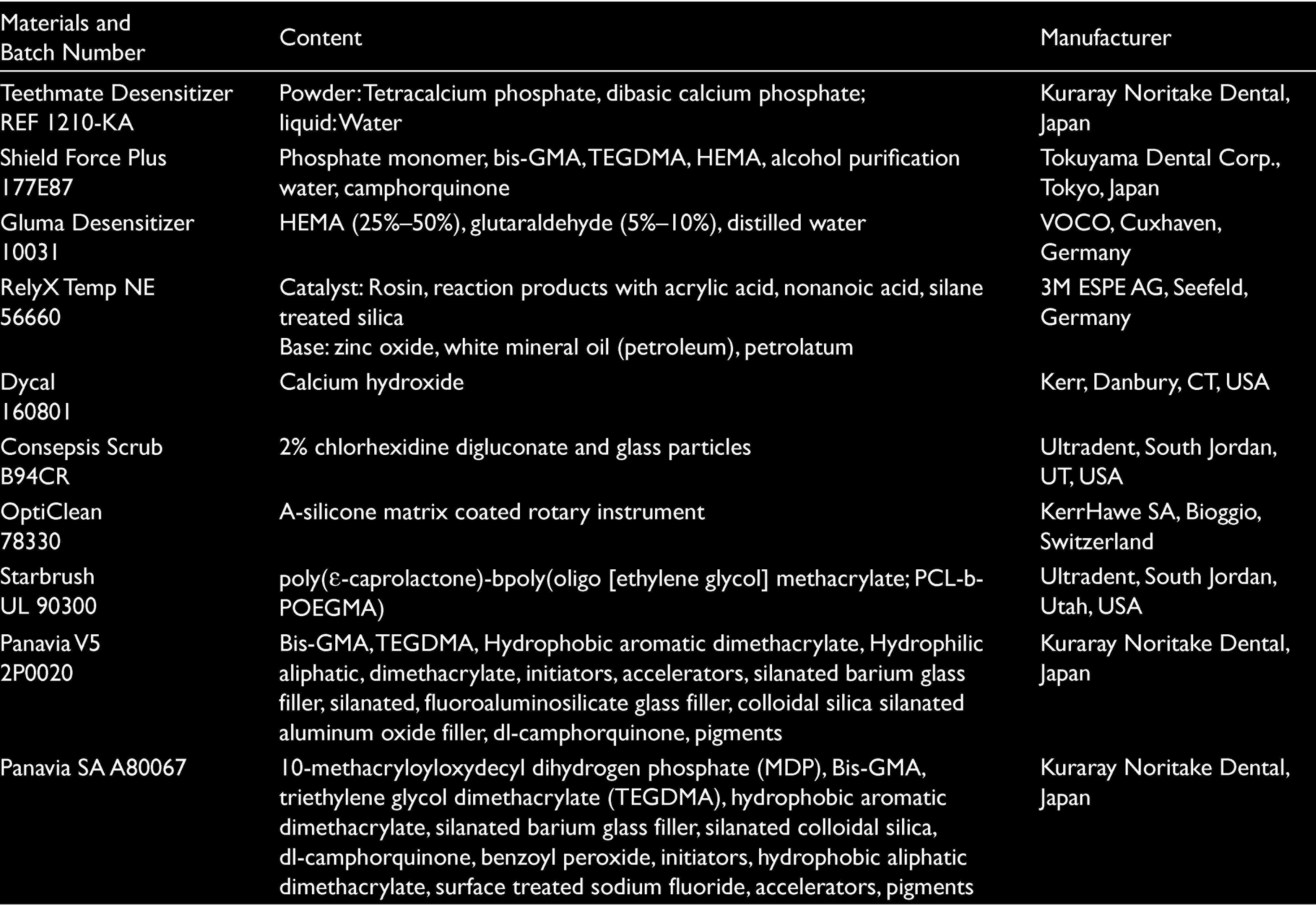
Results
The results of analysis of variance used to test the SBS values are shown in Table 2 and Figure 2, and mean SBS values and the differences among groups are shown in Table 3.
The desensitizer, cleaning methods, and the type of resin cements significantly affected the SBS to dentin (P < .05) except type of temporary cement (P > .05). There was interaction between desensitizer, temporary cement, cleaning agent, and resin cements (P <.05). However, no interaction found between the cleaning methods–resin cements and temporary cement–cleaning methods–resin cements (P > .05; Table 2).
Four-Way Analysis of Variance Results
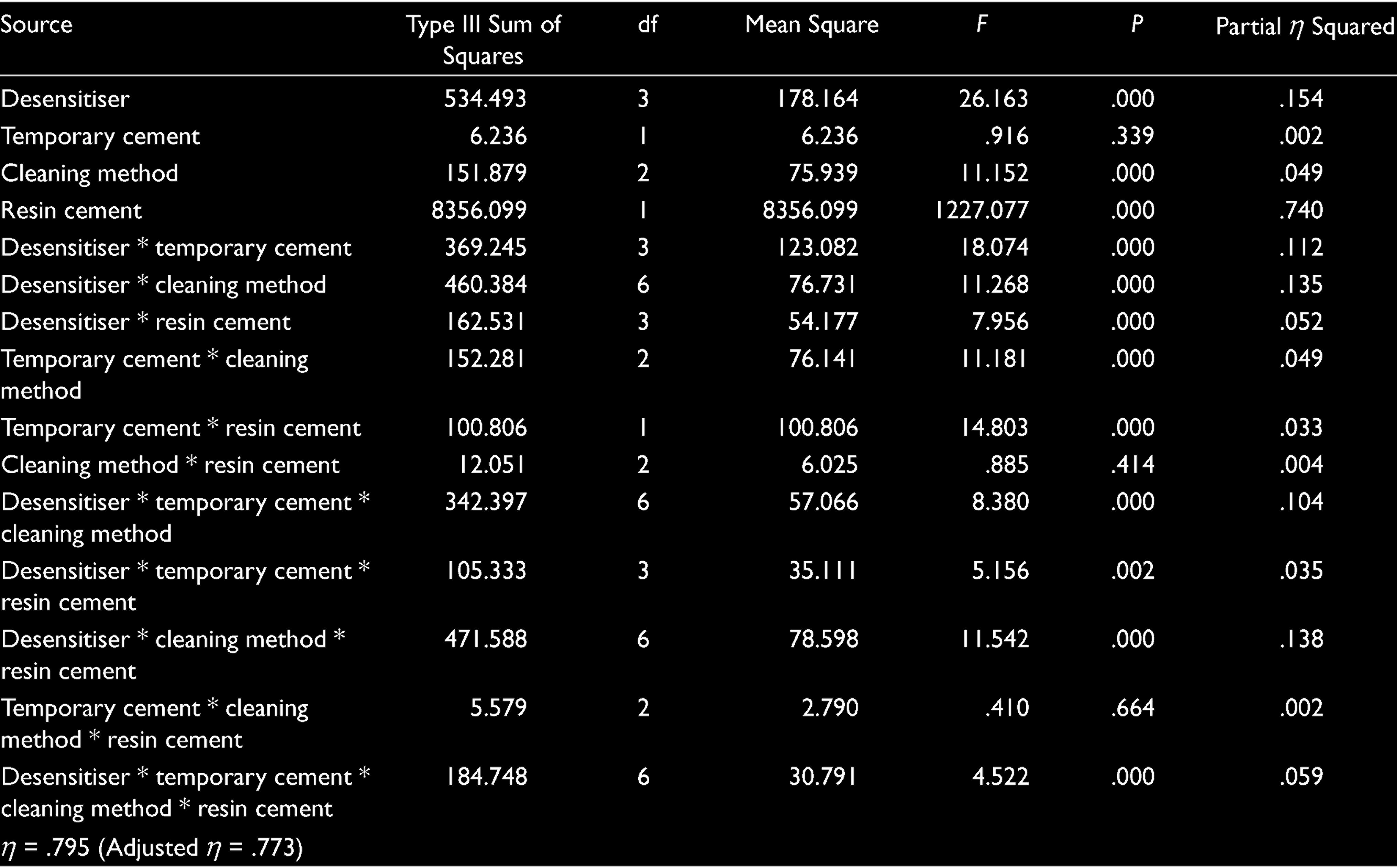
The lowest SBS values were obtained with no desensitizing control groups (P <.05) and highest SBS values were obtained with Shield Force Plus (SFP) groups and no significant differences were found between other desensitizer groups (P > .05). There were no significant differences between mean SBS values of temporary cements (P > .05). When cleansing methods were compared, highest SBS values were obtained with OptiClean groups (P <.05). The highest SBS values were obtained with dual-polymerized resin cement and significant differences were found in all groups (P <.05). The highest SBS value was obtained with Teethmate-RelyX TempNE-OptiClean-Panavia V5 (TROD; 19.51 ± 4.65) and no significant difference was found with Shield Force Plus-RelyX TempNE-OptiClean-Panavia V5 (SROD; P > .05). The lowest SBS value was obtained with Teehtmate-Dycall-OptiClean-Panavia SA (TDOS; 1.94 ± 0.40) and no significant differences were found with Control-Dycall-OptiClean-Panavia SA (CDOS) and Shield Force Plus-Dycall-OptiClean-Panavia SA (SDOS; P > .05; Table 3).
Mean and SD Values for Shear Bond Strength (MPa) and Significance
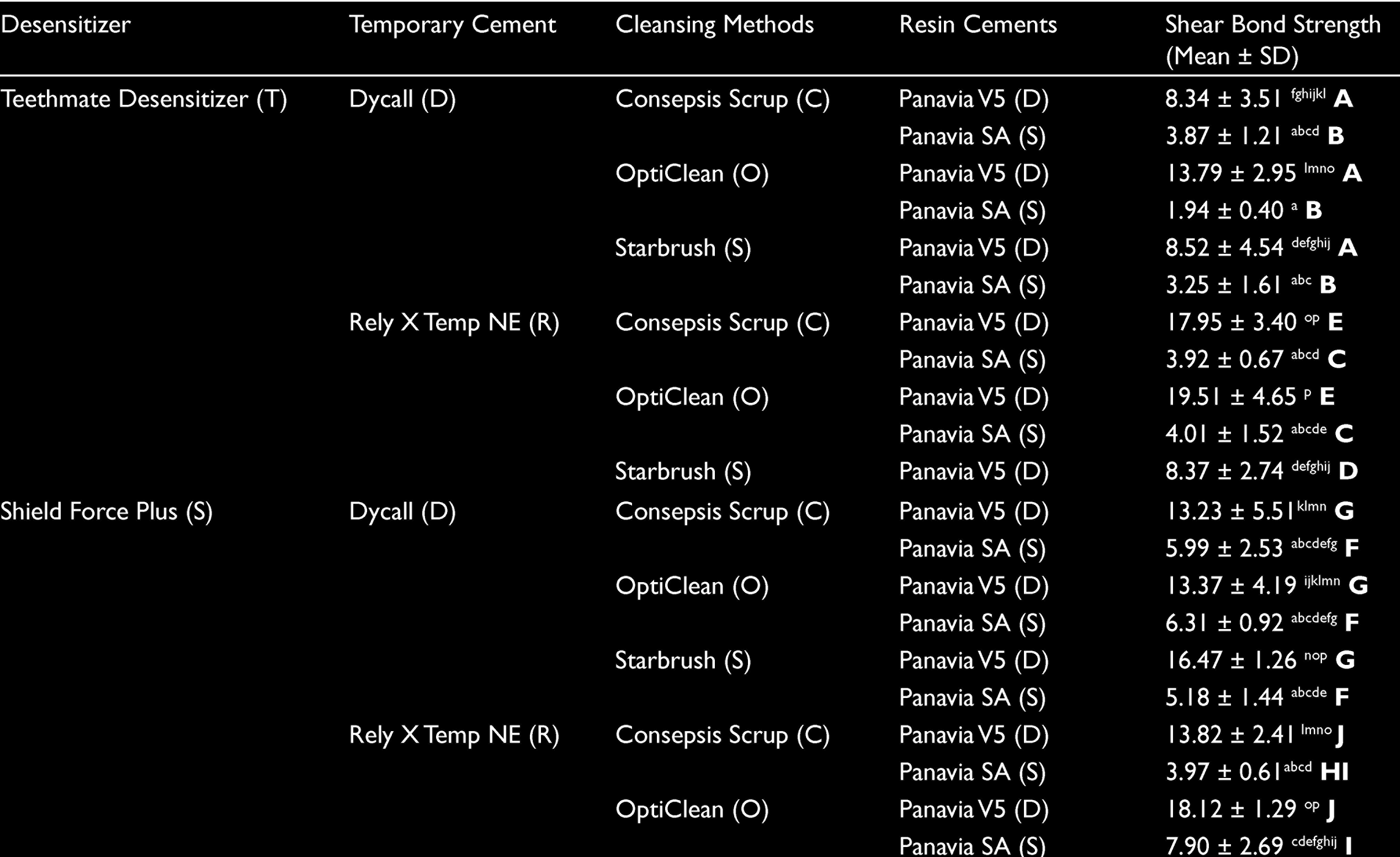


Adhesive fractures were the most common failure type in the PSA-cemented groups and for all groups. The mixed and cohesive failure types were mostly obtained in OptiClean and PV5 cemented groups.
Discussion
The hypotheses were claimed that the SBS between dentin and resin cement would be affected by the type of temporary cement and dentin cleaning methods (H0) and type of desensitizers (H1) and type of resin cements (H2). The SBS between dentin and resin cement affected by the type of cleaning methods and resin cement but not affected by the type of temporary cement and desensitizers. The hypotheses were partially confirmed.
To reduce or stop fluid movement in dentin tubules, which cause hypersensitivity, different types of desensitizers could be used before temporary crown cementation with temporary cement contains zinc oxide or calcium hydroxide. Resin-based SFP, Gluma, and calcium-phosphate-based TMD were used in the present study. SFP includes HEMA, Bis-GMA and triethylene glycol dimethacrylate (TEGDMA), and three-dimensional self-reinforcing (3D-SR) monomers, which interact with the calcium ions to seal dentinal tubules. Gluma contains HEMA primers and could reduce the sensitivity by precipitating plasma proteins in exposed tubules.17, 18
In this study, resin-based SFP, Gluma, and calcium-phosphate-containing TMD increased the SBS compared to the nontreatment group. Garcia et al. 18 applied TMD and Gluma to dentin and tested the SBS of dual-polymerized resin cement (Panavia F 2.0; Kuraray, Tokyo, Japan) to dentin. They stated that TMD and Gluma showed higher SBS compared to the control group, but Gluma were not significant, statistically. Atay et al. 19 also tested the SBS of self-adhesive Panavia SA and self-etch (Multilink N; Ivoclar, Schaan, Liechtenstein) resin cements to dentin using Gluma and TMD, but stated that there was no significant difference between TMD and Gluma, statistically. Ugur and Altıntas 17 applied TMD and SFP to dentin and measured the SBS of dual-cure Panavia V5 to dentin. Both desensitizers increased the SBS compared to the control group, but only resin-based SFP was statistically significant.
TMD containing dicalcium phosphate anhydrous (DCPA) and tetracalcium phosphate (TTCP) turns into hydroxyapatite (HA) crystals during dentin application and blocks the dentin tubules successfully. Although dentin tubules and surfaces are covered with TMD, Ca in HA crystals acts as a receptor for pulling 10-methacryloyloxydecyl dihydrogen phosphate (MDP) in a hybrid layer. This interaction between HA and MDP might explain the increased bond strength PSA and PV5 to dentin after TMD application.
The highest SBS values were tested in resin-based self-reinforcing monomer SFP in this study.Arita et al. 20 applied three resin-based barrier coat, Hybrid Coat II and SFP, and two glass ionomer-based (Clinpro XT Varnish and Fuji VII) tooth coating materials on dentin surface and tested the SBS of resin composite to dentin and they stated that the highest bonding strength values were found in SFP.
Thanks to HEMA, resin-based desensitizing agents penetrate the dentin tubules better and the dentin surface becomes even more wet for a durable adhesion. However, 3D-SR monomer matrix in SFP diffuses into more inner parts of dentin tubules and forms versatile cross-links with HA crystals that may be the cause for higher bonding strength in this study. When the studies in the literature were evaluated, it was seen that resin-based desensitizers generally increase the SBS of resin cements to dentin.17–20
Type of temporary cements, dentin cleaning methods, and dentin surface pretreatments with acids or adhesives are most important factors that must be done before permanent cementation.10, 12 In this study, we choose eugenol-free zinc-oxide-based and calcium-hydroxide-based temporary cement and the results showed that there was no significant difference between temporary cements.
To remove temporary cement remnants, mechanical and chemical techniques or their combinations could use. In previous studies, removing remnants mechanically is found to be ineffective methods.21, 22 Zortuk et al. 21 removed the temporary cement remnants on dentin by using a dental explorer, a pumice, OptiClean bur, and Er: YAG laser and tested the bond strength by using self-adhesive resin cement. They stated that dentin cleaning methods do not affect the bond strength statistically.
Altintas et al. 13 evaluated the effect of three provisional cements (calcium hydroxide, eugenol-free, and light-cured provisional cements) and two cleaning techniques (dental explorer and air–water spray) on the SBS of porcelain laminate veneers and stated that no significant differences were found. Song et al. 14 evaluated the effect of dentin cleaning methods (orange solvent, ultrasonic cleaning, and air abrasion) on the retention of cemented crowns using resin-modified glass ionomer and zinc phosphate cement. The study showed that temporary cement did not have a significant effect on retention.
Sarac et al. 11 investigated the effect of dentin cleaning techniques (Sikko Tim, Cavity Cleanser, OptiClean) on the SBS of a dual-polymerizing resin cement and dentin wetting. The results showed that all methods showed stronger SBS values than control specimens. Also in another study, Saraç et al. 23 evaluated dentin cleaning agents (Cavity Cleanser, Consepsis Scrub, and Sikko Tim) and etching systems (total etch and self-etch) on bond strength of resin cement to dentin and stated that Consepsis Scrub and Sikko Tim showed higher SBS. They stated that Consepsis Scrub has higher SBS values as an abrasive as it is applied with a rotary tool. The use of a rubber cup and a rotary instrument bur (Consepsis Scrub and OptiClean) can clean the dentin surface more effectively because of abrasive effect and could increase SBS.
Dual-polymerized resin cement achieves the highest SBS values in all groups. A study evaluated the effects of desensitizing resin (Gluma Desensitizer), resin sealing (Clearfil SE Bond, Syntac), and provisional cement (Freegenol) on SBS of dentin luted with conventional resin cements (Variolink II, Panavia 21) and self-adhesive (RelyX Unicem). The result of this study showed that Gluma and resin sealing have a beneficial effect on the SBS of self-adhesive resin cement. Sailer et al. 10 stated that contamination of dentin with temporary cement has no influence on the SBS of dual polymerizing or self-adhesive resin cement but conventional resin cements have shown highest SBS values.
Conclusions
With the limitation of this study, the following could be concluded.
Resin-based desensitizers have a beneficial effect on SBS of dual-cure and self-adhesive resin cements to dentin.
Types of the temporary cements (provided that they do not contain eugenol) have not a significant effect on bond strength.
Dentin cleaning methods especially silicone bur increased the bond strength.
Finally, dual-polymerized resin cement achieved higher SBS values according to self-adhesive.
Footnotes
Acknowledgements
The authors thank Yuzuncu Yil University Central Laboratory.
Author Contribution
Study methodology was designed by all authors. Conceptualization, data curation, formal analysis, investigation, and validation were made by Ugur and Kavut. Funding acquisition, resources, visualization, writing original draft, and software management were handled by Ugur and Akdeniz. Project administration, supervision, writing review, and editing were done by Kulunk and Tanrikut. The final article was approved by all the authors.
Clinical Significance
Resin-based desensitizers and cleaning of temporary cement debris with silicone-coated rotary instruments may improve the bonding quality of dual-cure resin cement to dentin.
Conflict of Interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Policy and Institutional Review Board Statement
Local independent ethics committee of Yuzuncu Yil University Medicine Faculty approved the study (statement B.30.2.YYU. 0.01.00.00/08).
Funding
This research was supported by Yüzüncü Yıl University Scientific
Research Projects under Project TSA-2017-6035.
