Abstract
Aim:
The aim of this study was to evaluate the effect of calcium phosphate based desensitizing agent on shear bond strength of self-etch/adhesive resin cements to dentin.
Materials and Methods:
Eighty dentin specimens were prepared from freshly extracted human third molar teeth and were classified, randomly (
Results:
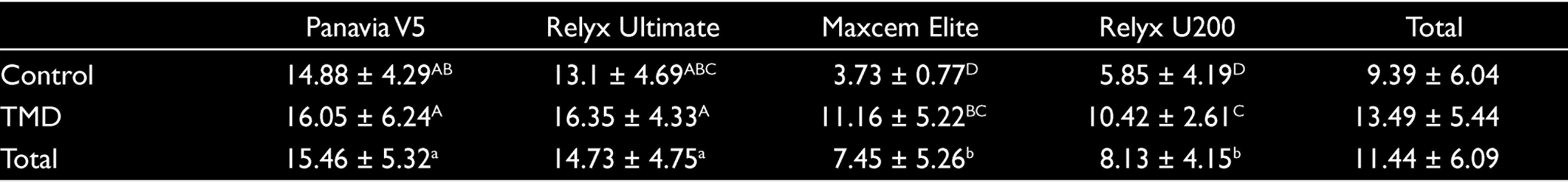
The higher shear bond values were observed in the groups with Teethmate Desensitizer applied and cemented with self-etch (16.05 ± 6.24 and 14.73 ± 4.75), whereas the lowest bonding values were observed in the groups with self-adhesive resin cement without Teethmate Desensitizer (3.73 ± 0.77 and 5.85 ± 4.19;
Conclusions:
Calcium phosphate desensitizer did not adversely effected shear bond strength of self-etch/adhesive resin cements to dentin. It even significantly increased the shear bond strength of self-adhesive resin cements.
Keywords
Introduction
Fixed crown and bridge dentures are metal-supported or fully ceramic restorations applied to restore lost teeth and surrounding tissues, function, phonation, and esthetics in dentistry today. 1 Nearly 1.5 to 2 mm teeth tissue needs to be removed from teeth during preparation for fabricating fixed crown and bridge dentures.2, 3 A great number of dentin tubules are uncovered to the oral environment after preparation and prepared teeth become more sensitive to external factors.4, 5
Dentin hypersensitivity is characterized by a short, sharp, and localized pain by stimulating the exposed dentin tubules with osmotic, chemical, and mechanical effects. Nowadays, dentin hypersensitivity is explained by “hydrodynamic theory.” According to this theory, chemical and physical stimulants can cause internal or external fluid movement within the dentin tubules, stimulate nerve fibers in the pulp/dentin interface, and induce painful discomfort.6, 7
Many desensitizing agents and methods could be used in the treatment of dentin hypersensitivity. Some of them occlude the dentin tubules, whereas others block neural transmission or precipitate proteins in the tubule. 7 When the dentin tubules are occluded, dentin hypersensitivity passes as the movement of dentin fluid decreases. 8 Some topical desensitizers in clinical usage have a temporary effect or maybe ineffective over time. 9 In recent years, calcium phosphate desensitizing agents have become popular because of their easy application, biocompatibility, tubule blocking ability, and noncoloration. 10
Calcium phosphate based Teethmate (TMD; Kuraray, Noritake, Tokyo, Japan) has a rapid treatment effect on exposed tubules and quickly and effectively occludes dentin tubules. TMD contains dicalcium phosphate anhydrous (DCPA; CaHPO4) and tetracalcium phosphate (TTCP; Ca4(PO4)2O) that naturally transforms to hydroxyapatite (HA; Ca10(PO4)6(OH)2) crystals with water on dentin surface and inside tubules.11, 12
Resin cements are often used for luting both metal-supported and full ceramic restorations due to their durable bonding to tooth structures and prosthetic restorations and their superior mechanical properties. Durable adhesion between dentin and resin cements is very important to prevent debonding, secondary decay, microleakage, and tooth or restoration breakage. 13 Some components inside desensitizing agents may inhibit the formation of a durable bond between the resin cements and the dentin, or may undergo structural changes in time and adversely affect the adhesion. However, some components in desensitizers affect the occluding and sealing features of resin cements by preventing durable adhesion between the hybrid layer and dentin.14, 15
The aim of this study was to investigate the effect of calcium phosphate desensitizing agent on shear bond strength of self-etch/adhesive resin cements to dentin. The null hypothesis was that calcium phosphate based TMD could not affect the bond strength of adhesive resin cements to dentin.
Materials and Methods
Eighty caries-free and unrestored recently extracted human third molar teeth were used in this in vitro study. Teeth were cleaned from soft tissue, disinfected with sodium azide, and stored in distilled water at 4°C till used. Specimen teeth were sectioned from cementoenamel junction and crowns were embedded in 25-mm diameter and height cylindrical molds buccal surface upward (Figure 1). A 600 grit silicon carbide abrasive paper was gently applied to the dentin surface for polishing and standardizing surfaces after buccal enamel was removed. Then, all dentin specimens were rinsed and cleaned with water to remove debris consisted during preparation.
The View of the Prepared Dentin Specimens

All dentin specimens were classified into four groups, randomly (
Materials Used in this Study
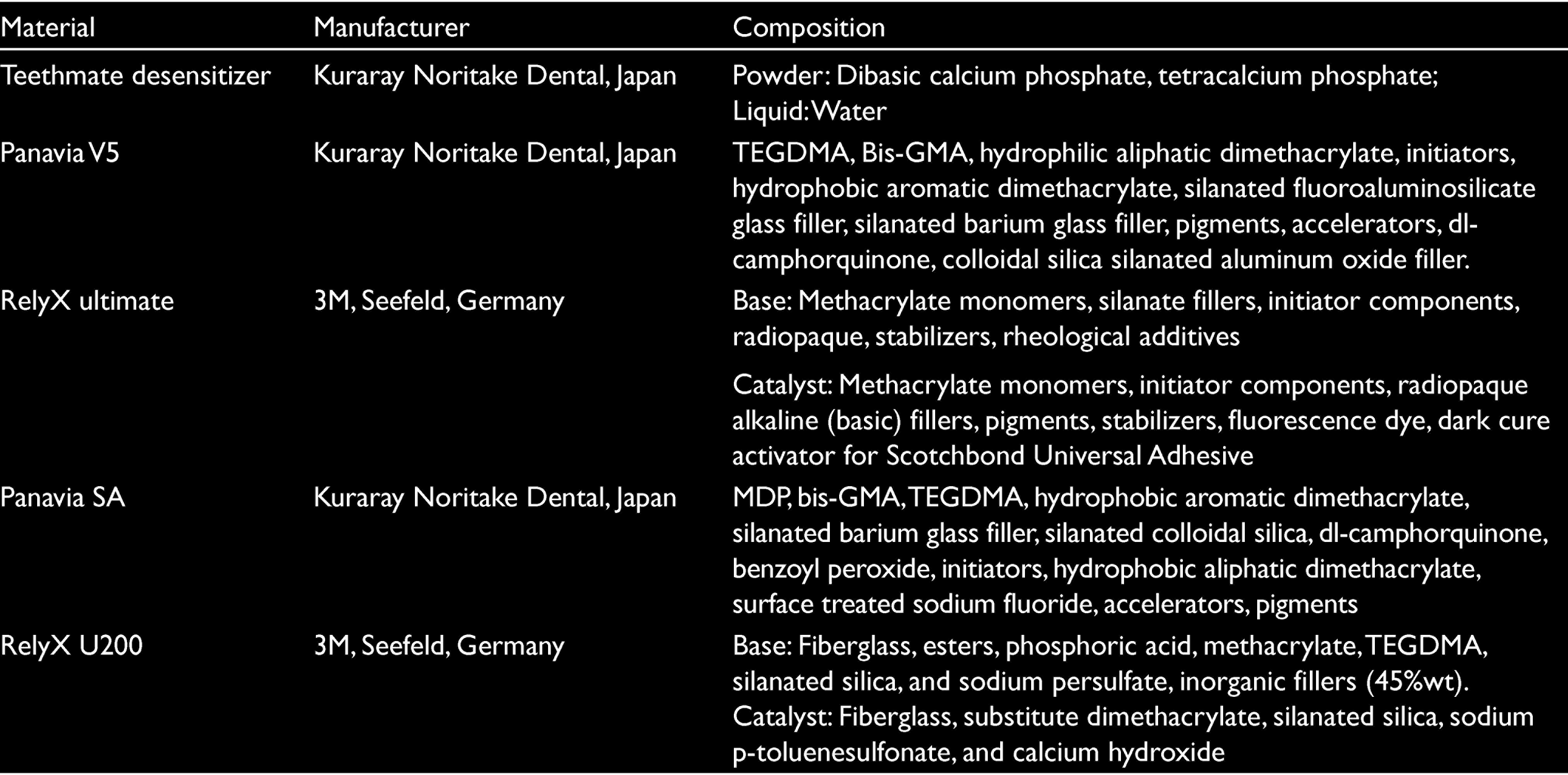

All specimens were first kept in the incubator at 37°C for 24 h and then thermal cycled at 5–55°C temperature changes in the bath for 30 s, transfer time 2 s to 6000 r/min. A universal testing machine at a crosshead speed of 0.5 mm/min was used for shear bond strength. Dentin surfaces were examined to determine failure type after the shear test with a stereo microscope (Olympus SZ-4045 ESD, Tokyo, Japan) at x30 magnification. Dentin surfaces were also examined with a SEM (Evo LS10, Zeiss, Germany) at x5000 and x10000 magnifications after applying desensitizer.
Statistical Analysis
Mean bonding values and standard deviations were calculated using a statistical program (SPSS version 20.0, IBM, Chicago, IL, USA). Mean bonding values were contrasted by two-way ANOVA and a multiple comparison test was performed with a Tukey’s honestly significant difference test (
Results
The two-way ANOVA result is given in Table 2. The main effect of treatment was found to be significant on shear bond strength (
Two-Way ANOVA Results
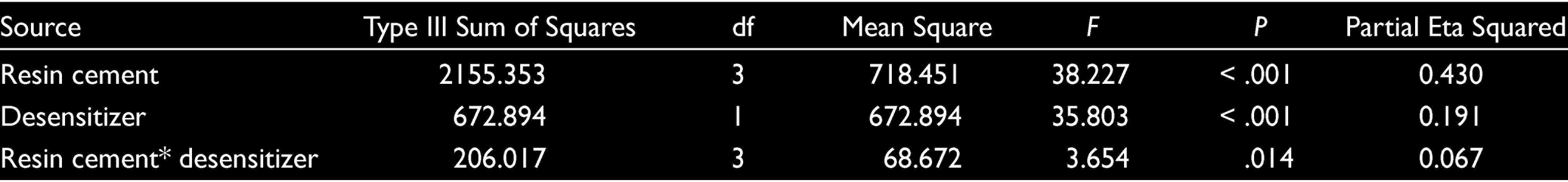

*Adjusted
The mean value, standard deviation, and multiple comparisons of the groups are shown in Table 3. The highest values were observed in the Panavia V5 and RelyX Ultimate groups treated with TMD, whereas the lowest values were observed in the untreated Maxcem Elite and Rely X U200 groups. Graph of shear bond strength according to the treatment method and resin cement is shown in Figure 2.
Mean and Standard Deviation Values for Shear Bond Strength (MPa)
Graph of Shear Bond Strength Values
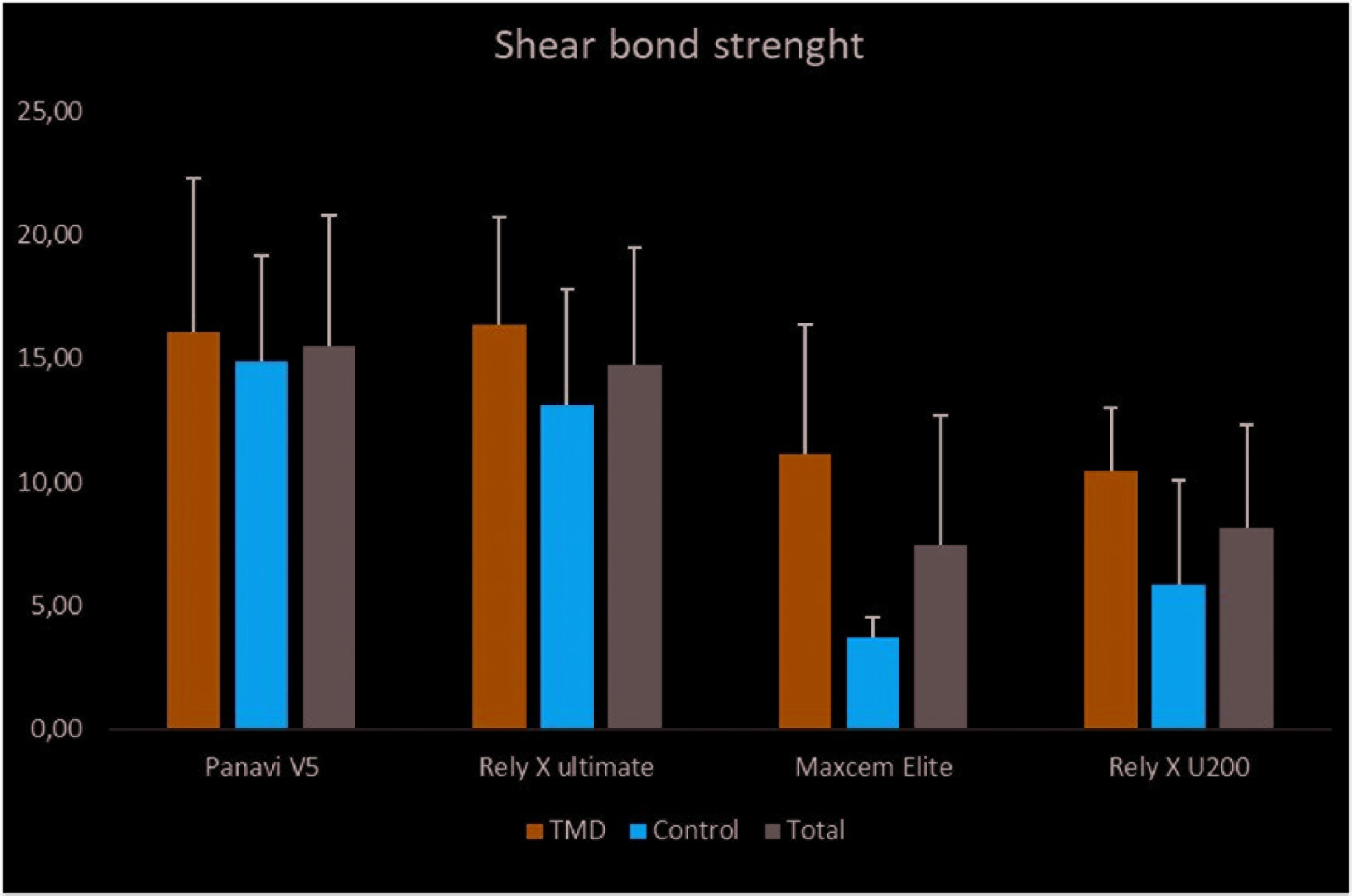
The most common adhesive failure was adhesive type. Mix-type adhesive failures were also seen in PV5-TMD and RUN-TMD specimens. Adhesive-type failures were observed in all PSA and RXU specimens. Dentin surfaces examined with a SEM are shown in Figures 3a and b. Dentin surfaces were found to be covered with calcium phosphate TMD in all treated groups.
Dentin Surfaces Examined with a SEM at x5000 Magnification

Dentin Surfaces Examined with a SEM at x10000 Magnification

Discussion
In this study, it was predicted that the shear bond strength values would not affect the groups with calcium phosphate containing desensitizer. However, the results of this study showed that bonding strength values increased in PSA and RXU groups significantly but were not significantly different in PV5 and RUN groups. The null hypothesis was partially confirmed.
Topical agents are often used in the clinic to quickly relieve dentin sensitivity. Recently, TMD containing calcium phosphate, which quickly turns into HA crystals by clogging sensitive dentin tubules and does not cause tooth discoloration and toxic effect, has been introduced to the market.10–12 It is stated in the studies that the bond strength of the topical agents applied to the dentin surface is clogged and the dentin surface is coated with the agent and the resin cement will be affected due to organic contents between the dentin.16, 17
Covering dentin tubules and dentin surface with a topical desensitizing agent can directly affect the interaction of self-etch/adhesive resin cements with dentin. A durable adhesion between dentin and resin cements affects the clinical survey of both teeth and prosthetic restoration. 18 If a permanent adhesion cannot be achieved between dentin and resin cements, microleakage may occur, resulting in dentin hypersensitivity and secondary caries.18, 19 It is also important that topical agents applied to the dentin surface do not dissolve due to saliva and oral fluids. If these agents dissolve in the early period, hypersensitivity may continue and clinical problems may begin to appear again.20, 21 The etching process applied during the cementation can reopen the tubules and dentin hypersensitivity could occur again. For this reason, self-etch/adhesive resin cements that do not require etching are frequently preferred by clinicians.20, 22 In this study, we preferred self-etch/adhesive resin cements.
Pei et al. 23 applied Biorepair and Dontodent, containing nanohydroxyapatite desensitizing toothpastes, to dentin and stated that both of them decreased the bond strength, although not statistically significant. Garcia et al. 24 examined the effects of Panavia F 2.0 resin cement and a composite resin (Estenia C&B, Kuraray Noritake Dental, Tokyo, Japan) on bonding strength to dentin using SuperSeal (Phoenix Dental, Fenton, MI, USA), Gluma (Heraeus Kulzer, Hanau, Germany), and TMD desensitizing agents, and observed that the bond strength increased significantly in all TMD applied specimens.
Gupta et al. 25 applied to dentin Sensodyne Repair and Protect, Teethmate Desensitizer, diode laser and evaluated the effect of bond strength of resin composite to dentin and stated that TMD increased the bonding values, if not statistically significant. Atay et al. 16 applied Gluma desensitizer, Nd: YAG laser, and TMD on dentin surface and evaluated the shear bond strength values by cementing self-etch (Clearfil Universal Bond, Kuraray, New York, NY, USA; Multilink N, Ivoclar, Schaan, Liechtenstein) and self-adhesive (Panavia SA) resin cements to dentin. As a result of this study, shear bond strength values were observed in TMD applied specimens, but were not found statistically significant. In addition, it was observed that bonding values of self-etch resin cements were significantly higher than those in self-adhesive cement. Uğur and Altıntaş 17 applied TMD on the dentin surface and tested shear bond strength values of Panavia V5 resin cement to dentin. They stated that TMD enhances bonding values even if it does not increase significantly.
Siso et al. 26 evaluated bonding strength effects of self-etch, etch and rinse procedures, self-etch + TMD and etch and rinse + TMD and stated that TMD decreased bonding values. Escalante-Otárola et al. 27 applied a toothpaste (Desensibilize Nano P) containing hydroxyapatite nanoparticles on dentin surface and luted resin composite with an etch-and-rinse adhesive system (Scotchbond Multi-Purpose; 3M ESPE, St. Paul, MN, USA). As a result of their work, they stated that using etch and rinse systems has increased the bond strength significantly. In our study, TMD enhanced bonding values of self-etch/adhesive resin cements to dentin and this rise was more evident in self-adhesive cements.
10-methacryloyloxydecyl phosphate (MDP) inside Panavia V5 tooth primer and Panavia SA interacts chemically with Ca ions of HA. Ca pulls chemical bonding agents, such as a receptor, to achieve a lockdown between the hybrid layer and HA. Thus, a micromechanical interlocking occurs between the dentin, HA, and the hybrid layer, and a durable bonding is observed even if the dentin tubules are blocked. 24 However, as it would continue to interact with the collagen fibers and functional monomers around HA for a long time, marginal microleakage would also be prevented. HA crystals attached to the collagen protect the collagen against hydrolysis, preventing their early degradation.16, 17, 24 This action mechanism of TMD may be the reason for the increase in bond strength values in our study.
There are temperature differences and pH changes in the real oral environment. As the tests in this study could not be performed in the oral environment, they could not adequately reflect the clinical conditions. Only one desensitizing agent was used in our study.
In addition, as only the shear test was applied, the inability to fully reflect the effect of chewing forces constitutes the limitations of this study. New studies can be made by considering these limitations.
Conclusion
Within the limitations, the following conclusions can be drawn from this study.
Calcium phosphate desensitizers can be recommended to be used by clinicians because they act quickly, eliminate sensitivity, have a practical use, are nontoxic, and do not stain the tooth.
At the same time, they contribute to the clinical survey of teeth and restoration because of their durable adhesion with self-etch/adhesive resin cements.
Footnotes
Acknowledgements
The authors would like to thank the central laboratory of Yüzüncü Yıl University.
Author Contribution
Study methodology was designed by all authors. Conceptualization, data curation, formal analysis, investigation, and validation were made by Kavut and Ugur. Funding acquisition, resources, visualization, writing original draft, and software management were handled by Kavut. Project administration, supervision, writing, reviewing, and editing were done by Kavut and Ugur. The final article was approved by all the authors.
Ethical Statement
Local independent ethics committee of Yuzuncu Yil University Medicine Faculty approved this study (statement B.30.2. YYU.0.01.00.00/95), and the patient informed consent was taken for specimen collection.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This research was supported by Yüzüncü Yıl University Scientific Research Projects under Project TSA-2017-6035.
