Abstract
Aim:
To evaluate the shear bond strength (SBS) of resin cements, flowable composites, and a preheated composite in luting glass-ceramic to dentin.
Materials and Methods:
In total, 108 noncaries human third molar teeth embedded in acrylic blocks, grinded from the occlusal surfaces until dentin was exposed, and divided into 9 randomized groups (n = 12). In total, 108 ceramic samples prepared in disc shape (3mm × 3mm) from IPS e. max CAD (Ivoclar Vivadent) blocks. Four adhesive resin cements: Variolink Esthetic DC (Ivoclar Vivadent), G-CEM LinkForce (GC), Panavia V5 (Kuraray Noritake), Maxcem Elite Chroma (Kerr), and three flowable composites: G-ænial Universal Flo (GC), Herculite XRV Ultra Flow (Kerr), Vertise Flow (Kerr), and one preheated composite: Enamel Plus HRI (Micerium) luted to the prepared occlusal surfaces of the teeth with total-etch, self-etch, and self-adhesive protocols. Then samples were thermocyled (5,000 cycles, 5–55°C, dwell time 20 s). SBS test was performed in a universal testing machine (at 0.5 mm/min). Failure modes were examined under a stereomicroscope at ×25 magnification. Data were analyzed using Kruskal–Wallis and Dunn–Bonferroni tests (α = 0.05).
Results:
There were statistically significant differences among material types (P < .05). Highest SBS values found in G-ænial Universal Flo (15.43 ± 5.67), and the lowest values obtained in Maxcem Elite Choroma (SA) (1.25 ± 1.47). There were no significant differences between self-etch (Panavia V5, Maxcem Elite Choroma [SE]) and self-adhesive (Maxcem Elite Choroma [SA], Vertise Flow) protocols (P > .05).
Conclusion:
Flowable composites can be alternatives to resin cements when bonded with total-etch procedures. Bond strength of self-etch and self-adhesive applications is still to be developed.
Abbreviations
CAD/CAM: Computer-aided design and computer-aided manufacturing
GDM: Glycerol 1,3-dimethacrylate
HEMA: Hydroxyethyl methacrylate
MPa: Megapascal
N: Newton
SA: Self-adhesive
SE: Self-etch
SBS: Shear bond strength
Introduction
In addition to the improvements in the ceramic and adhesive systems in dentistry, new techniques, such as computer-aided design and computer-aided manufacturing (CAD/CAM), have helped clinicians produce esthetic and durable restorations with superior mechanical properties in a single visit to the office. 1 For ultimate success, durable and lasting restorations can be achieved by the adhesive cementation of all-ceramic restorations to tooth structures. 2
Luting agents can be bonded to tooth surfaces with adhesive systems classified as total-etch, self-etch (SE), and self-adhesives (SA).3–5 For the ideal application of total-etch and self-etch systems, one or more steps are needed, whereas self-adhesive systems require no prior steps. 6 Postoperative sensitivity is not detected with self-etch systems as is the case for total etch systems. Adhesives that utilize a total-etch strategy have a superior clinical performance in terms of load bearing and durability; however, many clinicians are more likely to prefer more straightforward and less technique-sensitive materials or approaches. 7
“Universal” or “multimode” adhesives are the most contemporary products in the market. A durable and lasting bond to tooth structure can be achieved most effectively using self-etch or universal adhesives with a selective etching technique because the effectiveness of acid etching on dentin still remains controversial.8,9
Flowable composites can be used to cement porcelain (all-ceramics) in addition to their many other functions. The most remarkable features of flowable composites comprise the effective penetration of surface irregularities with a high surface wetting ability, the radiopaque nature, the ability to form a thin layer on the surface, and the variety of color choices. 10 In recent studies, the bond strength of flowable composites has been shown to be similar to resin cements. A similar mechanical performance was observed with different resin-based luting agents (flowable resin composites and resin cements). Flowable composites can be used as alternatives to cementing all-ceramics. 11
Preheated resin composites are also suggested as a viable option to cement indirect restorations. In some studies, the long-term benefits of using preheated composites for the cementation of all-ceramic restorations have been shown.12,13 Using preheating composites, the viscosity of a material is reduced, decreasing the ultimate film thickness, which provides clinicians with better control of the material. An improved adaptation to the preparation walls as well as a better depth and degree of polymerization can also be achieved.14,15
The aim of this in vitro study was to evaluate the shear bond strength (SBS) of resin cements, flowable composites, and a preheated composite with different adhesive protocols for luting lithium disilicate glass-ceramics to dentin with a universal adhesive. The null hypothesis was that material types used for adhesive cementation would not affect the SBS values of a glass-ceramic to dentin.
Materials and Methods
Setting and Design
This study was designed as an in vitro research and was performed in the laboratory of Ege University Dentistry Faculty. This study was conducted from January 2018 to March 2019. The adhesive systems used in this study and their compositions are shown in Table 1. A total of 108 unrestored, caries-free, human molar teeth extracted in the last six months for periodontal reasons were used in the study. Soft- and hard-tissue residues on the external surfaces of the teeth were cleaned using periodontal curettes and were grinded with sandpaper. They were then disinfected with 5% sodium hypochlorite diluted 1:10 for 30 min, rinsed under running water for 15 min, and stored in distilled water at +4°C until used. To expose the occlusal dentin surfaces, the teeth were grinded with a coarse grit diamond rotary cutting instrument under water. In total, 100, 400, and 600 silicon carbide sheets (Abramin; Struers) were used to standardize the dentin surfaces under water for 20 s. The teeth were then mounted in a plastic holder filled with autopolymerizing acrylic resin with the exposed occlusal surfaces upward and parallel to the ground. The teeth were randomly divided into nine groups (n = 12).
Materials Used in the Study
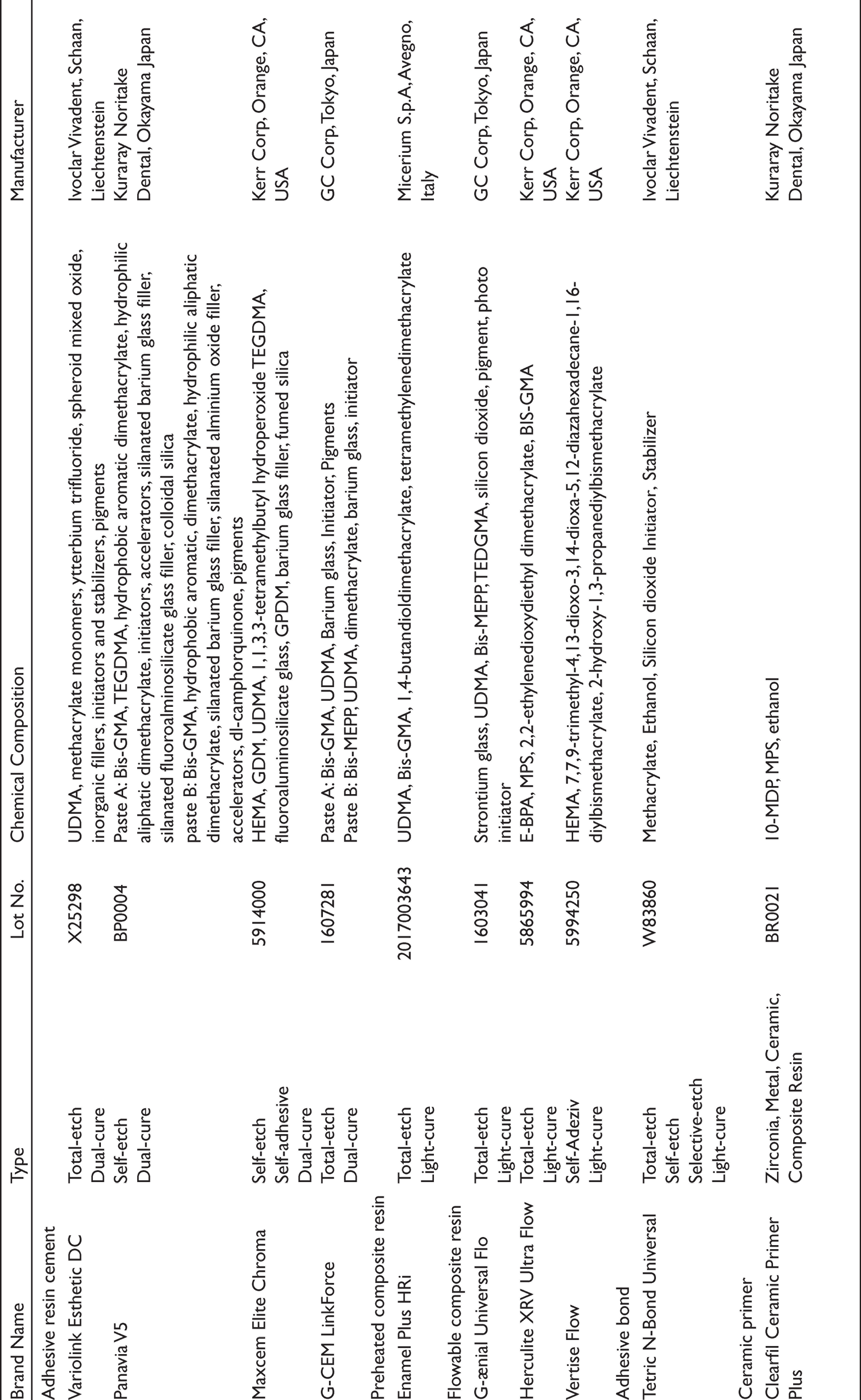
Sample Preparation
A total of 108 disc-shaped samples (3 mm diameter, 3 mm height) were obtained from lithium disilicate glass-ceramic CAD/CAM blocs (IPS e. max CAD; Ivoclar Vivadent, Schaan, Liechtenstein) using a low-speed diamond saw (Mecatome T180; Presi, Grenoble, France) (Isomet 1000; Buehler). The prepared surfaces of the samples were examined under a light microscope to verify that they were free of any defects, fractures, or cracks. They were then crystallized in a furnace (Programat® P710; Ivoclar Vivadent, Schaan, Liechtenstein) according to the manufacturer’s protocol. The bonding surfaces of the samples were polished with P600, P1200, and P2000 silicon carbide sheets (Abramin; Struers), respectively. The IPS e. max CAD ceramic samples were randomly divided into nine test groups (n = 12).
Prior to the cementation procedures, the ceramic samples were cleaned using an ultrasonic cleaner for 5 min. Uncontaminated adhesive surfaces were etched using 5% hydrofluoric acid (IPS Ceramic Etching Gel, Ivoclar Vivadent, Schaan, Liechtenstein) for 20 s, rinsed under a water spray, and dried with mild air pressure. Silane (Clearfil Ceramic Primer, Kuraray, Okayama, Japan) was applied to the ceramic surfaces for 60 s and dried with mild air pressure. For the total-etch cemented groups, the dentin surfaces were etched for 15 s with 37% phosphoric acid (Total Etch, Ivoclar Vivadent), washed for 15 s, and dried with air flow. A universal bond (Tetric N-Bond Universal, Ivoclar Vivadent) was applied to the dentin surfaces by gently rubbing them with an applicator for 20 s. For the total-etch adhesive system groups, adhesive resin cements (Variolink Esthetic DC, G-CEM LinkForce), flowable composite resins (G-ænial Universal Flo, Herculite XRV Ultra Flow), or a preheated composite resin (Enamel Plus HRI Dentin) was applied to the ceramic surfaces and luted to dentin. The preheated composite resin material (Enamel Plus HRI Dentin) was heated to 55°C in a heating unit (ENA Heat; Micerium S.p.A) before application. Cemented ceramic samples were fixed in a fixator for 10 min with an applied pressure of 500 g, and the excess cement was removed using an applicator. In total, 20 s light curing was directed from two different surfaces for polymerization (LY-B200 Dental LED Curing Light, Shanghai S&D Dental International Co. Shanghai, China) (1500 mW/cm2, 420–480 nm). For the self-etch adhesive system groups, without acid application, the teeth were bonded with a universal bond (Tetric N-Bond Universal, Ivoclar Vivadent) by rubbing the dentine surface for 20 s and were slightly dried with a light air flow. Self-etch resin cements (Panavia V5, Maxcem Elite Chroma) were applied to the ceramic surfaces, and cementation was accomplished with a standardized pressure as previously described. For the self-adhesive system groups, adhesive resin cement (Maxcem Elite Chroma) and flowable composite resin (Vertise Flow) were applied to the ceramic surfaces and luted to dentin as previously described. All specimens were stored in distilled water at room temperature for 24 h. Samples were then thermocycled in deionized water between 5°C and 55°C for 5,000 cycles with dwell times of 20 s and transfer times of 10 s in each bath.
Observational Parameters
The SBS test was performed using a universal testing machine (AGS-J, SHIMADZU, Kyoto, Japan) at a crosshead speed of 0.5 mm/min until a fracture occurred, and the maximum force was recorded in newton (N). The results were expressed in megapascal (MPa) values. The S = L/A formula was used to calculate the shear bond strength (S) values (MPa), where L is the load at failure (N) and A is the measured adhesive area (mm2).
Following the SBS test, the failure modes of the specimens were examined under a stereomicroscope (Leica S8 APO, Heerbrugg, Switzerland) at ×25 magnification and recorded as an adhesive failure if the fracture occurred at the adhesive interface, a cohesive failure if the fracture occurred either in the tooth tissues or in the adhesive itself, or a mix failure if the fracture occurred both in the tooth tissue and in the adhesive. Mix failures were further classified according to the amount of adhesive left on the dentin tissues as 25%–50%, 50%–75%, and 75%–100%.
Statistical Analysis
The statistical analyses were performed using SPSS statistical software (22.0, SPSS Inc., Chicago, IL, USA). The normality of the data distribution was tested using the Kolmogorov–Smirnov test. Because the data were not normally distributed, they were further analyzed using the nonparametric Kruskal–Wallis test for multiple comparisons. The descriptive statistics for the permanent data not showing a normal distribution were set as (Median [Min – Max]). Dunn–Bonferroni tests were used for pairwise comparisons between the groups. The statistical significance was set at α = 0.05.
Results
The SBS test results (Median [Min – Max]) and differences among the materials are presented in Table 2. According to the Kruskal–Wallis analysis, there were statistically significant differences among the adhesive resin cements, flowable composites, and the preheated composite material (P < .05). The samples that failed before the shear bond test were not included in the statistical evaluation. One sample of the Enamel Plus HRI material, two samples of the Panavia V5 material, and four samples of each Maxcem Elite Chroma (SA) and Vertise Flow were debonded before the SBS test.
Comparison of SBST Values (MPa) Among the Materials
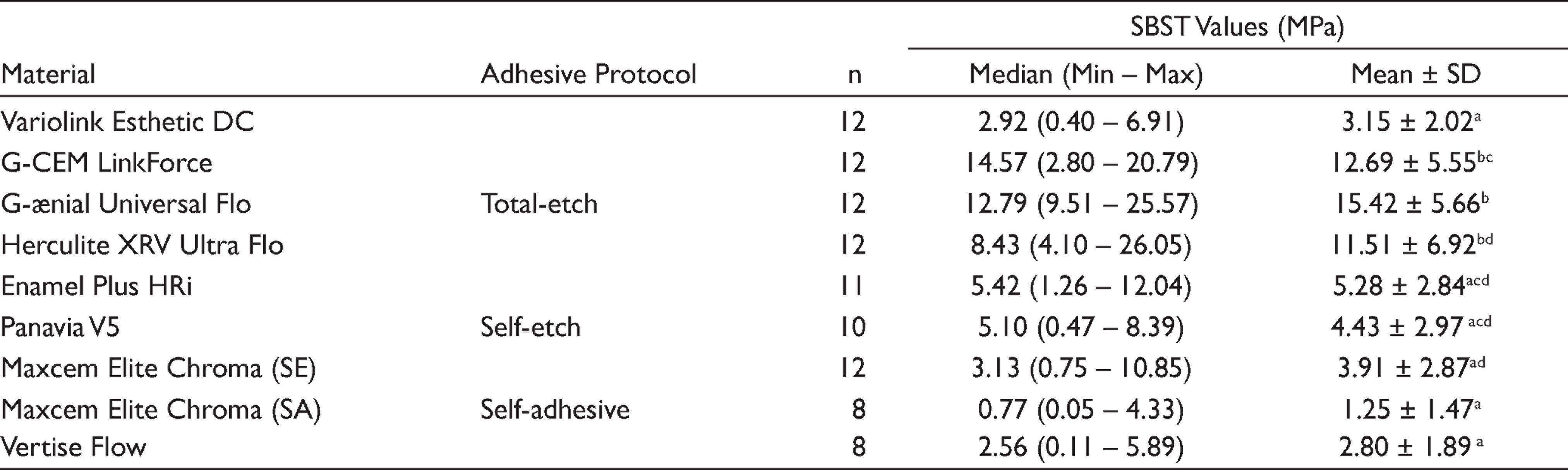
Significantly different at P < .05.
The SBS values of the G-ænial Universal Flo were significantly different from Variolink Esthetic DC (P < .001), Enamel Plus HRi (P = .045), Panavia V5 (P = .018), Maxcem Elite Chroma (SE) (P = .001), Maxcem Elite Chroma (SA) (P < .001), and Vertise Flow (P = .001) materials. The highest SBS values were found for the G-ænial Universal Flo (15.43 ± 5.67) material. However, there were no statistically significant differences among the G-ænial Universal Flo, G-CEM LinkForce, and Herculite XRV Ultra Flow materials (P > .05).
The SBS results of the Maxcem Elite Choroma (SA) material were significantly different from the G-CEM LinkForce (P < .001), G-ænial Universal Flo (P < .001), and Herculite XRV Ultra Flow (P < .001) materials. The samples cemented with Maxcem Elite Choroma (SA) showed the lowest SBS values. However, the differences between the SBS values of the Maxcem Elite Choroma (SA) and Variolink Esthetic DC, Enamel Plus HRi, Panavia V5, Maxcem Elite Choroma (SE), and Vertise Flow groups were statistically insignificant (P > .05).
While there were statistically significant differences between the adhesive resin cement materials G-CEM LinkForce and Variolink Estheitc DC (P = .004), Maxcem Elite Chroma (SE) (P = .021), Maxcem Elite Chroma (SA) (P < .001), no statistically significant difference was observed for the Panavia V5 material (P > .05). The G-CEM LinkForce material showed the highest SBS value among all the adhesive resin cements.
While there was statistically no difference between G-ænial Universal Flo and Herculite XRV Ultra Flow flowable composite materials (P > .05), the SBS value of Vertise Flow was found to be considerably lower than that of the G-ænial Universal Flo (P = .001) and Herculite XRV Ultra Flow (P = .034) materials.
The differences between the materials that were cemented with self-etch (Panavia V5, Maxcem Elite Choroma [SE]) and self-adhesive protocols (Maxcem Elite Choroma [SA], Vertise Flow) were statistically insignificant; however, the difference among the materials cemented with the total-etch protocol was statistically significant.
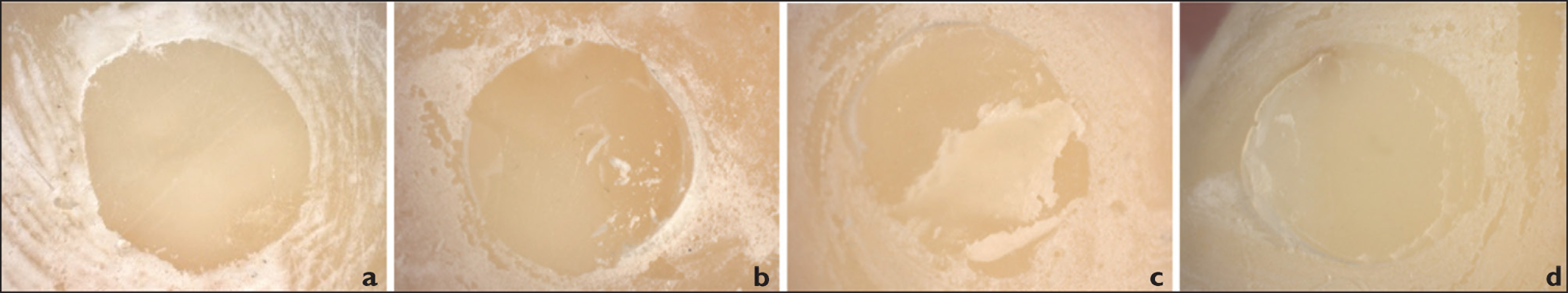
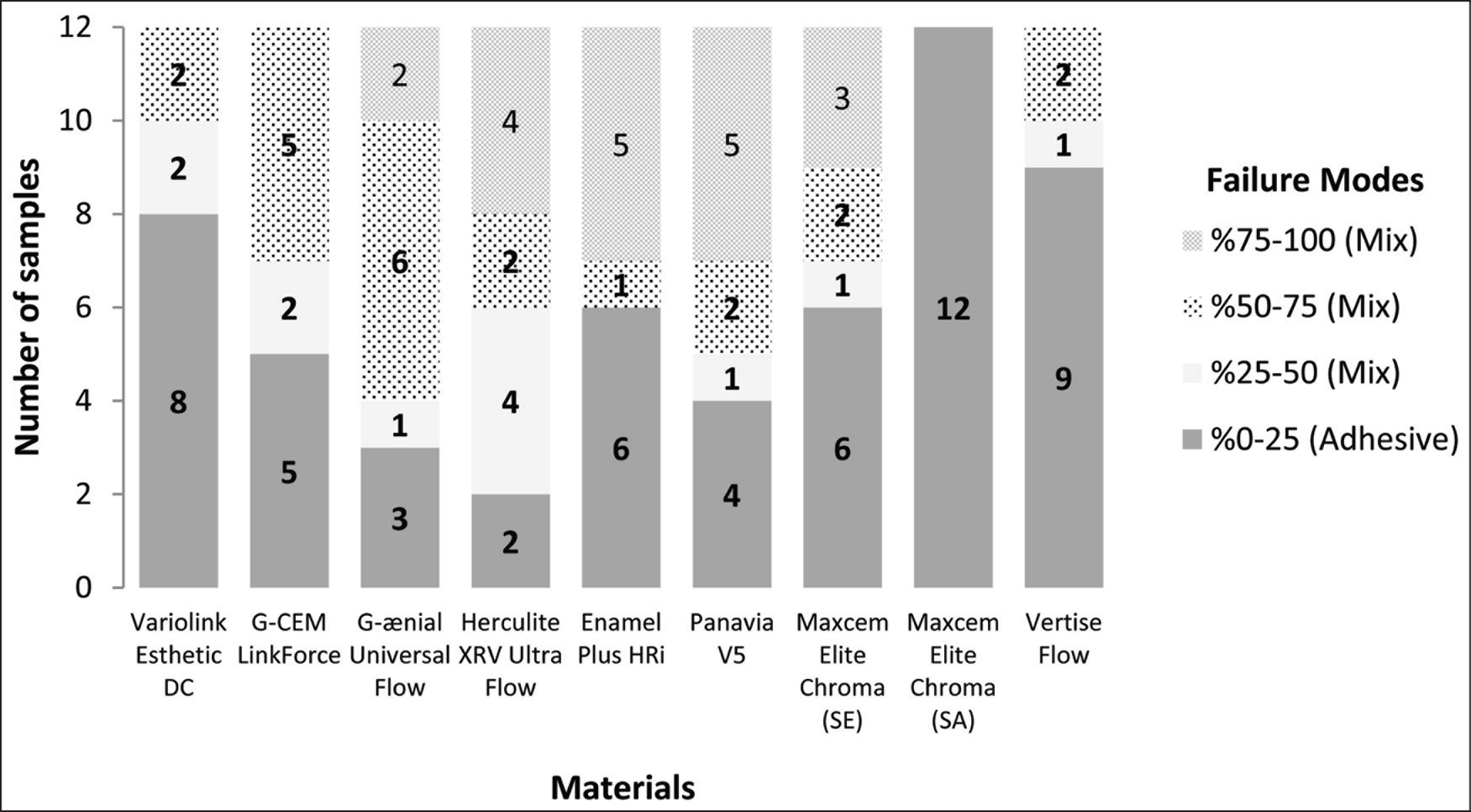
Representative failures of stereomicroscope images are shown in Figure 1. Figure 2 shows the frequency of the failure modes of the adhesive material groups. The statistical analyses revealed that according to the chi-square test, there was a significant interaction between the distribution of failure modes and adhesive materials (P = .001). The failure modes of the debonded samples before the shear bond test were considered adhesive failures. Higher bond strength values were obtained for the G-ænial Universal Flo, G-CEM Link Force, and Herculite XRV Ultra Flow materials, respectively, which showed fewer adhesive failures than the other groups. The mode of failures was mostly a mix type for these materials. Lower bond strength values and a higher number of debonded samples were observed for the self-adhesive groups of Maxcem Elite Chroma (SA) and Vertise Flow, which showed higher adhesive failures. Moreover, all the samples of Maxcem Elite Choroma (SA) showed adhesive failures. Eight adhesive and four mix types of failures were observed for Variolink DC. For the Panavia V5 group, the mix type of failure was mostly observed. Half of the Maxcem Elite Choroma (SE) and Enamel Plus HRI groups showed adhesive failures, while the other half showed mix failures.
Stereomicroscope images of failure types at ×25 magnification: (a) adhesive (0%–25%), (b) mixed (25%–50%), (c) mixed (25%–50%), and (d) mixed (75%–100%).
Failure Mode Distribution for the Evaluated Groups Paired by SBS Test
Discussion
In the current study, the SBS of four different adhesive resin cements, three different flowable composites, and one preheated composite to IPS e. max CAD and dentin were tested. According to the results, there were significant differences among the materials (adhesive resin cements, flowable, and preheated composites) used. Based on the results, the null hypothesis that different materials used for adhesive cementation would not affect the SBS values was rejected.
The long-term durability of the bond between the resin cement and the tooth is still controversial, and there is a general consensus that the adhesive bond obtained with current dentine adhesives deteriorates over time.16,17 The bond strength depends on the ceramic material’s composition, the mechanical and/or chemical interaction between the ceramic and adhesive material, exposed dentin substrate’s properties and hydrophilicity after preparation, and the physicochemical properties.18,19 Hence, choosing the most appropriate cementation method for the specific ceramic material improves the durability of the bond strength.
In addition to resin cements, flowable composites and preheated composites can also be used for the cementation of all-ceramic restorations. The mechanical properties of flowable composites were reduced to 60%–70% because their filler content was decreased by 50% compared to the conventional composites. The most important advantage of flowable composites is their ability to create a minimum thickness layer by penetrating the surface irregularities due to their increased wetting capacity. 10 In the present study, two of the flowable composites, G-ænial Universal Flo and Herculite XRV Ultra Flow, cemented with a total-etch protocol and one of the adhesive resin cements, G-CEM LinkForce, cemented with a total-etch protocol showed the highest SBS values. Featuring a high filler rate of 62 vol %, G-CEM LinkForce has been designed for a strong adhesion. 20 The other flowable composite used, Vertise Flow, which was cemented with a self-adhesive protocol, showed lower SBS values than the other flowable composites. Moreover, prior to testing, four samples failed of 12 in the mentioned group. Spazzin et al. concluded that the mechanical performance of flowable composites and resin cements displayed a similar performance, where they adhered to porcelain samples with two flowable composites (Filtek Z350 Flow ve Tetric-N Flow) and three different resin cements (Variolink Veneer, Variolink II Ligth-cured, Variolink II dual-cured). 11 Barceleiro et al. investigated the SBS of feldspathic porcelain laminate veneers to bovine enamel with dual-cure resin cement and a light-cure flowable composite and found comparable results. 21 They proposed that flowable composites can be used as an alternative to resin cements in the cementation of porcelain laminate veneer restorations not exceeding a 2-mm thickness.
Many studies have demonstrated the benefits of the long-term use of preheated composites with a high filler content in the cementation of all-ceramic restorations.12,13 Tomaselli et al. concluded that flowable composites and preheated conventional composites showed a similar microshear bond strength on luting ceramic veneers. 22 In the present study, the preheated composite material Enemal Plus HRI was heated to 55°C in a heating unit before application. The SBS values of Enamel Plus HRI were found to be 5.28 ± 2.84 MPa, which was lower than G-ænial Universal Flo, while there were no significant differences among the other materials tested. Similar to the present study, Demirbuga et al. found that there were significant differences between the bond strengths of preheated and nonheated composites to dentin surfaces. 23 Goulart et al. evaluated the microtensile bond strength and adhesive interfaces of indirect restorations luted with preheated composite resin. 12 One resin cement (RelyX ARC) and two composite resins (Venus and Z250 XT) were used in their study, and the materials were preheated to 64°C. They found that the composite resin showed similar or higher microtensile bond strength results compared to resin cement. They revealed that thinner luting interfaces were obtained by preheating the composite resin with closer contact between the luting agent and the adhesive layer. Resin cements with a high configuration factor and a low viscosity may generate relatively high contraction stress. This stress may cause microleakage in a restoration due to the debonding of the luting material. 24
In the present study, among the adhesive resin cements, total-etch resin cement G-CEM LinkForce showed higher SBS values than total-etch resin cement Variolink Esthetic DC, self-etching Maxcem Elite Chroma (SE), and self-adhesive resin cement Maxcem Elite Chroma (SA). Sokolowski et al. found that Variolink Esthetic DC showed a high solubility value. 25 Resin materials immersed in water might result in some components (unreacted monomers or fillers) dissolving and leaching out of the material. Withal stated that self-adhesive cemented Maxcem Elite Chroma demonstrated the highest water sorption. 26 This material contains HEMA (hydroxyethyl methacrylate) and GDM (glycerol 1,3-dimethacrylate), which is one of the highest hydrophilic materials among dental resins. The polymer matrix expands due to the water sorption induced by HEMA. 27 This may explain the adhesive failure of 4 of the 12 samples for Maxcem Elite Chroma (SA) and the lower SBS values of Variolink Esthetic DC and Maxcem Elite Chroma (SA) in this study. In contrast, Petropoulou et al. stated that there were no interactions between the resin cement types (conventional, self-etching, or self-adhesive) with water. 28
D’Arcangelo et al. investigated the effect of different luting systems on the microtensile bond strength of resin-based composite and ceramic restorations to dentin. 29 They found that the highest mean bond strength of indirect glass-ceramic restorations were the ones luted with a self-adhesive system. On the contrary, according to the results of this study, materials cemented with self-adhesive protocol Maxcem Elite Chroma (SA) and Vertise Flow showed lower SBS values. Because these cements cannot completely remove the smear layer, which may cause a weak hybrid layer between the resin cement and dentin, a lower SBS of the self-adhesive resin cements would be inevitable. A hybrid layer cannot be created with self-adhesive resin cements because they interact superficially with mineralized tissues and are not able to demineralize the smear layer completely. 30 Ferreira-Filho et al. stated that there were no significant differences between simplified adhesive systems and three-step etch-and-rinse or two-step self-etch adhesives. 31 On the contrary, in the present study, there were significant differences between materials cemented with total-etch among self-etch and self-adhesive protocols, but there was no significant difference between materials cemented with self-etch (Panavia V5, Maxcem Elite Chroma [SE]) or self-adhesive (Maxcem Elite Chroma [SA], Vertise Flow) protocols. Self-etch adhesives facilitate the passage of fluids from the oral environment to dentin, and vice versa, by behaving as permeable membranes, which leads to degradation. Moreover, after the application of a one-step self-etch adhesive, relatively fewer hydrophobic monomers would be available on the tooth surface, resulting in a decrease of the mechanical strength of the adhesive and impaired bond strength. 32
The analyses of the failure mode revealed that all samples of Maxcem Elite Chroma (SA) failed adhesively at the luting agent dentin interface, which is similar to the results of Lührs et al 33 . They stated that a 100% adhesive failure in their experimental group could be rationalized by the weak layer of collagen, which is short of hydroxyapatite between Maxcem Elite Chroma (SA) and the unaffected dentin. 33 Scanning electron microscopy studies with self-adhesive materials showed very little and shallow interactions between resin and dentin without a hybrid layer formation.34,35 In total, 4 of 12 samples of each Maxcem Elite Chroma (SA) and Vertise Flow were debonded before the SBS test and were regarded as adhesive failures. Vertise Flow and Variolink Esthetic DC predominantly failed adhesively at the luting agent dentin interface. This higher adhesive failure rate at the luting cement–dentin interface registered for these materials is a consequence of the lower bond strength of the luting cement to dentin. Herculite XRV Ultra Flow and G-ænial Universal Flo showed fewer adhesive failures at the luting agent dentin interface given that they bonded more effectively to dentin.
This study has several limitations. First, the samples were not stored in saliva or under an occlusal load and oral temperatures, which better mimic the actual oral environment. Rather than on smooth surfaces, testing assembly should be performed on naturally formed and shaped surfaces for the C factor to be taken into consideration. Clinical trials on the efficacy of adhesive systems should be evaluated by means of retainability, and marginal adaptation and microleakage should follow the laboratory tests to accumulate further evidence.
Conclusion
Within the limitations of this study, the following conclusions can be drawn:
G-ænial Universal, the flowable composite used with a total-etch procedure, showed a higher SBS than other luting materials, while Vertise Flow, the other flowable composite luted with a self-adhesive protocol, showed a lower SBS than the other luting materials. Flowable composites can be alternatives to resin cements for luting lithium disilicate glass-ceramics when bonded by total-etch procedures. No statistically significant difference was found between the self-etch or self-adhesive procedures of the adhesive resin cement Maxcem Elite Chroma. Preheated composite Enamel Plus HRi showed comparable results with all the materials tested except the flowable composite G-ænial Universal Flo. During clinical practice in bonding of glass-ceramic restorations to tooth structures, composite resins or flowable composites may safely be used.
Footnotes
Acknowledgements
This research was presented at the ICP & EPA Joint Meeting, Amsterdam, The Netherlands, on September 4–7, 2019.
Author Contributions
Alev Mutlu: Study and experimental design, data conception, sample preparation, performed the experiment analysis and interpretation of the results, manuscript writing.
Ayse Atay: Data collection, data acquisition and analysis, interpretation of the results and manuscript writing.
Ebru Çal: Study and experimental design, data collection, data acquisition and analysis, data interpretation, analysis and interpretation of the results, manuscript proofreading.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Policy and Institutional Review Board Statement
The study protocol was approved by the Ethical Committee of Ege University, Turkey (Number: 17-8.1/10). All the procedures have been performed as per the ethical guidelines lay down by Declaration of Helsinki.
Data Availability Statement
Data will be available on valid request by contacting corresponding author mail.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Ege University, Scientific Research Project Coordination Unit (Project Number: 18-DİŞ-005).
