Abstract
Background:
In Ethiopia, most family planning users rely on short-acting contraceptives, despite the greater effectiveness of long-acting and permanent methods (LAPCMs). Previous studies on users’ intention to adopt LAPCMs have reported inconsistent findings. This study aimed to determine the pooled prevalence of intention to use LAPCMs and identify associated factors among Ethiopian family planning users.
Methods:
A systematic search was conducted in PubMed, Scopus, the Cochrane Library, and Google Scholar. Data were extracted using Microsoft Excel and analyzed with STATA version 11. A random-effects model was applied to estimate pooled prevalence, while heterogeneity was assessed using the Cochrane Q test and I2 statistic.
Results:
Six studies involving 2773 participants were included. The pooled prevalence of intention to use LAPCMs was 50.98% (95% CI: 43.57–58.40). Significant factors associated with intention included good knowledge (POR = 4.81, 95% CI: 2.01–11.52), positive attitude (POR = 3.15, 95% CI: 2.21–4.50), higher educational attainment (POR = 6.23, 95% CI: 2.71–14.35), and the absence of myths and misconceptions (POR = 2.19, 95% CI: 1.10–4.38).
Conclusion:
Intention to use LAPCMs among Ethiopian family planning users is moderate, indicating suboptimal uptake. Knowledge, education, attitudes, and misconceptions strongly influence this intention. Interventions that improve awareness, dispel misconceptions, and foster supportive attitudes are critical for enhancing adoption. Policymakers and health organizations should prioritize targeted education and behavior change strategies to strengthen family planning outcomes.
Keywords
Background
Family planning (FP) enables couples to make informed decisions about whether, when, and how often to have children. This contributes to improved maternal and child health, greater educational and economic opportunities for women, and broader social and national development benefits. 1 Contraceptive methods are generally classified as short-acting, long-acting, or permanent. Long-acting contraceptive methods are reversible and provide effective pregnancy prevention for extended periods without frequent user action, while permanent methods are irreversible procedures intended for lifelong contraception.2–4 Together, long-acting and permanent contraceptive methods (LAPCs) offer highly effective, convenient, and cost-efficient pregnancy prevention.5,6
Despite these advantages, the global utilization of LAPCs remains limited. Research suggests that meeting the demand for modern contraception could prevent 1.6 million newborn deaths and 170,000 maternal deaths annually, yet more than 225 million women in developing countries who wish to avoid pregnancy still lack access to effective methods. 7 In Africa, unmet need for FP remains high, with 53% of married women reporting gaps—more than double the level observed in developed regions.8,9,10 Most FP users in low-income countries rely on short-acting methods, which are less effective than LAPCs. 11 Consequently, maternal and neonatal mortality rates remain disproportionately high in sub-Saharan Africa and South Asia, which account for about 80% of global deaths from preventable pregnancy-related cause. 12
In Ethiopia, similar challenges exist. According to the 2019 Ethiopian Demographic and Health Survey (EDHS), approximately 22% of married women have an unmet need for FP. Although contraceptive coverage has improved over the past decades, the majority of users still depend on short-acting methods, while LAPCs, the most effective options, remain underutilized. 13 This low uptake persists despite government efforts to expand access, revealing gaps in both service delivery and user acceptance.
The intention to use LAPCs is a critical step toward actual utilization. According to the Theory of Planned Behaviour (TPB), intention is shaped by attitudes, subjective norms, and perceived behavioral control, and it strongly predicts whether individuals translate preferences into practice.14,15 Similarly, the Ideational Behaviour Model (IBM) emphasizes how knowledge, attitudes, social norms, self-efficacy, and myths or misconceptions interact to influence contraceptive behaviors. 16 Previous studies from different regions of Ethiopia have shown that intention toward LAPCs use is influenced by a range of factors, including socio-demographic characteristics, reproductive health profiles, knowledge levels, personal attitudes, partner support, and cultural or religious perceptions.1,17–22 Misconceptions and negative ideational factors often drive preference for short-acting methods, despite the long-term benefits of LAPCs.
However, the available evidence is fragmented, with studies conducted in different local contexts reporting varying prevalence rates and determinants of intention. To date, no comprehensive synthesis has been undertaken to provide pooled estimates of intention to use LAPCs and the associated factors in Ethiopia. This knowledge gap limits policymakers and program planners from designing context-specific and evidence-driven strategies to expand LAPC uptake.
Therefore, this systematic review and meta-analysis aimed to determine the pooled prevalence of intention to use long-acting and permanent contraceptive methods among family planning users in Ethiopia and to identify key factors influencing this intention. The findings are expected to guide targeted interventions, inform policy decisions, and strengthen family planning programs to improve maternal and child health outcomes in Ethiopia.
Materials and methods
This systematic review and meta-analysis was conducted in accordance with the PRISMA guidelines to promote clear and transparent reporting 23 (Supporting Information File 1). Adhering to these standards enhances the rigor, credibility, and reproducibility of the findings. Additionally, the review protocol was registered in the International Prospective Register of Systematic Reviews (PROSPERO) with the registration number CRD42024584447.
Searching strategy of articles
To ensure a thorough review of relevant studies, several databases were searched, including PubMed, Scopus, the Cochrane Library, and Google Scholar. The study specifically aimed to assess the prevalence of intention to use long-acting and permanent contraceptive methods among women accessing family planning services in Ethiopia, enabling a detailed and focused analysis. A customized search strategy was created for each database using Medical Subject Headings (MeSH) terms. The search terms included: “Intention to use” OR “intention to utilize” AND “Long-acting” OR “lengthy acting” AND “Permanent” OR “lasting” AND “Associated factors” OR “Predictors” OR “Determinants” AND “Family planning users” OR “Contraceptive users” AND “Ethiopia” (Supporting Information File 2).
Inclusion criteria
We included all English-language studies conducted in Ethiopia that reported on the prevalence of intention to use long-acting and permanent contraceptives and/or its associated factors among women of family planning users up to August 25, 2024.
Exclusion criteria
Studies focusing on specific demographic characteristics, case reports, case series, letters to the editor, or those that did not provide prevalence data on intention to use long-acting and permanent contraceptives were excluded.
Outcome of review
The primary outcome of this review is the prevalence of intention to use long-acting and permanent contraceptives and the factors associated with it among women of family planning users.
Study selection
All articles retrieved from the different databases were imported into EndNote X7 for reference management. Duplicate records were removed, and two reviewers (YAF and WCT) independently screened the titles, abstracts, and full texts of the studies to evaluate their eligibility for inclusion. The level of agreement between the two reviewers was assessed, and inter-rater reliability was calculated using Cohen’s kappa statistic to ensure transparency in the selection process.
Data extraction
Following the review of titles, abstracts, and full texts of the selected articles, data extraction was conducted using a standardized approach adapted from the Joanna Briggs Institute (JBI). This task was undertaken independently by two reviewers (YAF and AMZ), who thoroughly evaluated each included article. Any discrepancies or uncertainties were resolved through discussions among the reviewers until a consensus was reached. Key details from each study, including the first author’s name, geographic location and setting, publication year, study design, participant demographics, and sample size, were thoroughly extracted. In addition, key risk factors and the prevalence of intention to use long-acting and permanent contraceptive methods, along with their corresponding 95% confidence intervals, were documented to provide a comprehensive summary of the existing evidence on this topic.
Risk of bias (quality) assessment
Quality assessment was performed using the Joanna Briggs Institute (JBI) critical appraisal checklist for analytical cross-sectional studies, which comprises nine evaluation criteria. 24 These criteria assess: (1) the suitability of the sampling frame for the target population, (2) the appropriateness of the sampling method, (3) whether the sample size was sufficient, (4) the clarity in describing study subjects and settings, (5) whether data analysis adequately covered the identified sample, (6) the validity of the methods used to identify the condition, (7) the consistency and reliability of how the condition was measured across participants, (8) the suitability of the statistical analysis used, and (9) whether the response rate was acceptable. Each item was scored as 1 for “yes” or 0 for “no”/“not reported,” resulting in a total score between 0 and 9. Based on these scores, studies were classified as low quality (0–4), medium quality (5–7), or high quality (8–9).
Outcome measurement
The dependent variable in the review was the intention to use long-acting and permanent contraceptive methods. In the original research, this variable was measured by identifying women who were not currently using LAPCs at the time of the survey but expressed a desire to use these methods. Responses were categorized as “yes” for those who intended to use these methods and “no” for those who did not.18,25
Data synthesis and analysis
Data extraction was carried out using a Microsoft Excel spreadsheet, and the data were subsequently imported into STATA version 11 for further analysis. Descriptive summaries of the included studies and their key findings were presented using tables, charts, and forest plots. Due to the presence of heterogeneity among the studies, a random-effects model was employed to calculate the pooled prevalence estimate. Heterogeneity was evaluated with Cochrane’s Q test and the I2 statistic, with I2 values interpreted as follows: none (0%), low (<25%), moderate (25%–75%), and high (≥75%). 26 To assess factors influencing the intention to use long-acting and permanent contraceptive methods, odds ratios with 95% confidence intervals (CI) were calculated. Subgroup analyses were conducted to reduce random variations in the point estimates of the individual studies, while sensitivity analyses explored possible sources of heterogeneity. Publication bias was assessed using funnel plots and Egger’s test. 27 The pooled odds ratios (POR) with corresponding 95% CIs were computed to identify factors associated with the intention to use these contraceptive methods.
Results
Study selection
A comprehensive search across multiple databases identified 19,100 articles related to the intention to use long-acting and permanent contraceptives among family planning users. This included 17,990 articles from Google Scholar, 385 from PubMed, 428 from Scopus, and 297 from the Cochrane Library. After removing 16,211 duplicate studies, 2791 articles were excluded based on title and abstract screening. Of the remaining 98 full-text articles assessed for eligibility, 92 were excluded due to differences in study populations or unreported outcomes of interest. Consequently, six studies were selected for inclusion in the final meta-analysis (Figure 1).

Study selection flow diagram for the systematic review and meta-analysis on the intention to use long-acting and permanent contraceptives and related factors among family planning users in Ethiopia, 2024.
Characteristics of the included studies
All the studies included utilized a cross-sectional design to evaluate the intention to use long-acting and permanent contraceptive methods. Published between 2014 and 2022, these studies collectively involved 2773 participants out of a possible 2828, with sample sizes ranging from 388 25 to 594. 5 The reported prevalence of intention to use long-acting and permanent contraceptives varied between 38% 18 and 60%. 28 Two studies were conducted in the Tigray Region1,5, one in the Oromia Region, 25 one in the Amhara Region, 22 one in the Southern Region, 18 and one in Addis Ababa 28 (Supplemental Table 1).
Meta-analysis
Intention to use long-acting and permanent contraceptives
The overall pooled prevalence of the intention to use long-acting and permanent contraceptives in the included studies from Ethiopia was 50.98% (95% CI: 43.57, 58.40; Figure 2). The random effects model revealed moderate heterogeneity across the studies (I2 = 58.9%, p = 0.032). To address this, sensitivity and subgroup analyses were conducted.
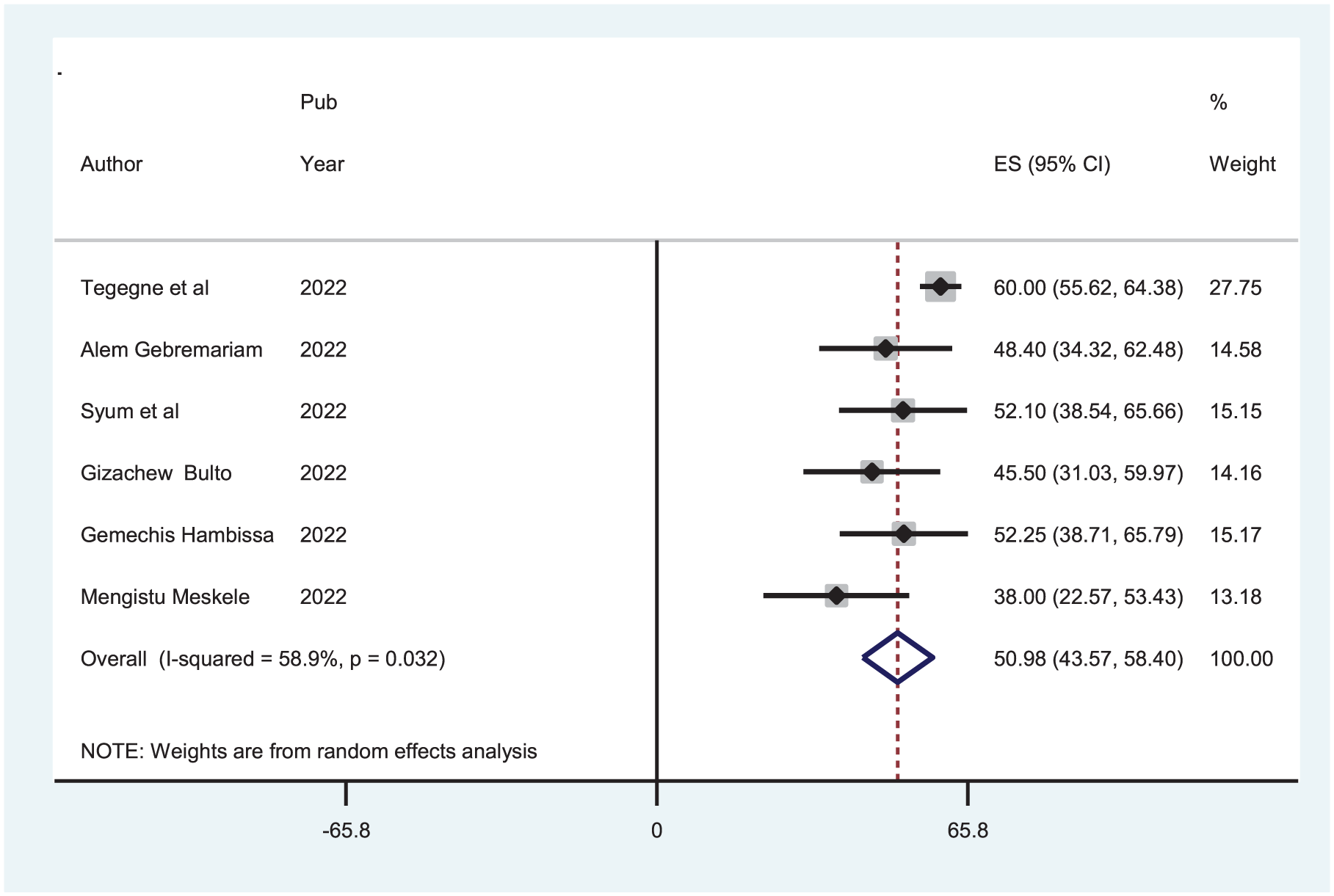
Forest plot illustrating the pooled prevalence of intention to use long-acting and permanent contraceptives among family planning users in Ethiopia, 2024.
Subgroup analysis
A subgroup analysis based on the sampling technique of the primary studies showed a higher prevalence of intention to use long-acting and permanent contraceptives in studies using systematic random sampling at 53.93% (95% CI: 47.62, 60.24). In contrast, studies using purposive sampling reported the lowest prevalence at 38% (95% CI: 22.57, 53.43; Figure 3).
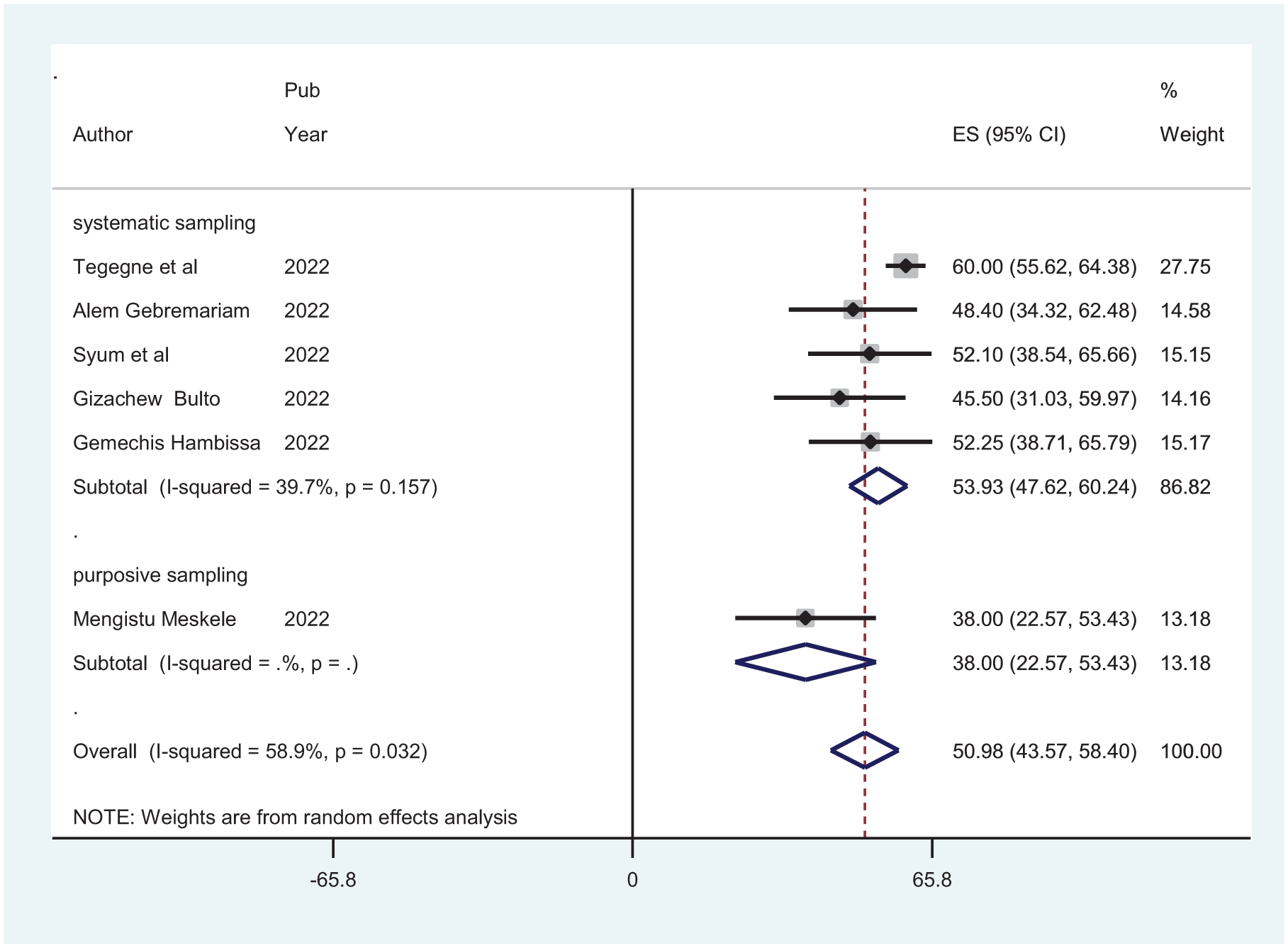
Subgroup analysis of the intention to use long-acting and permanent contraceptives among family planning users in Ethiopia, 2024.
Quality of the included studies
Among the included studies, five (83.33%) were rated as high quality, receiving scores between 8 and 9, while one study (16.66%) was classified as medium quality. The assessment was based on the nine criteria outlined in the Joanna Briggs Institute (JBI) critical appraisal checklist (Supporting Information File 3).
Publication bias
Both visual inspection of funnel plot asymmetry and Egger’s regression test were conducted to assess publication bias. The results indicated evidence of publication bias, as Egger’s test showed a statistically significant result (p = 0.000). In addition, the funnel plot displayed an asymmetrical distribution of studies, suggesting that smaller studies with non-significant or unfavorable results may be underrepresented. This pattern indicates the potential influence of selective publication, where studies with significant findings are more likely to be published. The observed asymmetry should therefore be considered when interpreting the pooled estimates, as it may have led to an overestimation of the true effect size (Figure 4).

Graphic representation of publication bias using funnel plots of all included studies in Ethiopia, 2024.
Sensitivity analysis
Due to the presence of publication bias indicated by Egger’s test (p = 0.000), a sensitivity analysis was performed; revealing that no individual study had a substantial impact on the overall findings (Figure 5).

Analysis of the sensitivity of the studies included in the meta-analysis.
Associated factors
The study analyzed various factors associated with intention to use long-acting and permanent contraceptives. However, some were excluded due to inconsistencies in how the independent variables were classified or grouped. Three studies found a significant association between knowledge of long-acting permanent methods and intention to use long-acting and permanent methods. Pooled odds ratio of women with a good understanding of long-acting permanent methods were 4.81 times more likely to use them than those with poor knowledge of long-acting and permanent methods (POR = 4.81, 95% CI: 2.01, 11.52). Three studies identified a significant association between positive attitude and intention to use long-acting and permanent contraceptives. Those women who had positive attitudes toward long-acting and permanent contraceptives were 3.15 times more likely to use them than those who had negative attitudes (POR = 3.15, 95% CI: 2.21, 4.50). Two studies identified a significant association between respondent’s higher educational level and intention to use long-acting and permanent contraceptives. Those women with higher educational levels were 6.23 times more likely to use than those with illiterate (POR = 6.23, 95% CI: 2.71, 14.35). Lastly, two studies found that women who had no myths and misconceptions were 2.19 times more likely to use long-acting and permanent contraceptives than those who had myths and misconceptions (POR = 2.19, 95% CI: 1.10, 4.38). Given the heterogeneity in these studies (I2 = 75.3%, p = 0.000), a random-effects model was used for the analysis (Figure 6).

The forest plot of the association between factors and intention to use long-acting and permanent contraceptives among family planning users in Ethiopia, 2024.
Discussion
Understanding women’s intentions to use long-acting and permanent contraceptives (LAPCs) is crucial for assessing the impact and reach of family planning programs. 5 In Ethiopia, LAPCs are essential for managing reproductive health and achieving long-term family planning objectives. However, there is a lack of comprehensive data on the prevalence of these intentions among women utilizing family planning services. This systematic review aims to fill this gap by gathering and analyzing available evidence to provide a clearer insight into these intentions. In Ethiopia, the pooled prevalence of intention to use long acting and permanent contraceptive among family planning users was 50.98% (95% CI: 43.57, 58.40).
This finding is lower than a similar study conducted in Malawi (69.29%) 29 and Nigeria 69%. 30 The lower prevalence of intentions to use long-acting and permanent contraceptive methods (LAPCs) in Ethiopia compared to Malawi and Nigeria could be due to several factors. These might include differences in the effectiveness and reach of health education campaigns, with Malawi and Nigeria possibly having more robust programs that promote LAPCs. Cultural and religious beliefs in Ethiopia may also be more conservative, leading to lower acceptance and intention to use these methods. 31 Additionally, disparities in access to family planning services, socioeconomic conditions, and government support for reproductive health programs could further contribute to the lower intention rates observed in Ethiopia.
However, this finding is higher than the study conducted in Comoros, which reported an 18.28% prevalence. 32 The greater intention to use long-acting and permanent contraceptive methods (LAPCs) in Ethiopia compared to Comoros may be due to several factors. Ethiopia likely has more robust and efficient family planning programs, leading to greater awareness and acceptance of long-acting and permanent contraceptives (LAPCs) among women. Additionally, differences in healthcare infrastructure and access to family planning services may make contraceptive options more accessible in Ethiopia compared to Comoros.
The findings of this study provide important insights into the factors linked to the intention to use contraceptives. In particular, having good knowledge, a positive attitude, higher levels of education, and the absence of myths and misconceptions were independently associated with a greater likelihood of intending to use long-acting and permanent contraceptive methods.
The present study found that women with a post-secondary education were 6.23 times more likely to intend to use long-acting and permanent contraceptive methods (LAPCs) compared to women without formal education. This finding is consistent with studies conducted in Pakistan 33 and Malawi. 34 It suggests that education significantly influences women’s intention to use LAPCs by providing them with the knowledge and positive attitudes needed to support their intention and eventual use of these contraceptive methods.
This study identified a significant association between knowledge of long-acting and permanent contraceptive methods and the intention to use them. Women with a solid understanding of LAPCs were 4.81 times more likely to intend to use these methods than those with limited knowledge. This finding is supported with study conducted in china. 35 The possible reason may be Women who have a solid understanding of LAPMs are more aware of their benefits, effectiveness, and long-term advantages, which increases their willingness to adopt them. 36 Additionally, Knowledgeable women may be better able to discuss LAPCs with their partners and healthcare providers, leading to greater acceptance and support for their use.
Women who hold a positive attitude toward long-acting and permanent contraceptive methods are 3.15 times more likely to intend to use them. This finding is consistent with studies conducted in China 35 and Scotland 37 This is likely due to their recognition of LAPCs’ benefits, reduced fears and misconceptions, and increased confidence in their safety and effectiveness. Furthermore, supportive social norms and a positive personal perspective also enhance their intention to adopt these methods. 38
This study revealed a significant association between being free from myths and misconceptions and intention to use long-acting and permanent contraceptive methods. Women who were not affected by myths and misconceptions about LAPCs were 2.19 times more likely to express an intention to use these methods. This finding aligns with research from Pakistan 33 and Kenya, 39 which also found that a lack of myths and misconceptions was associated with a greater intention to use LAPCs. The finding that women without myths or misconceptions about long-acting and permanent contraceptive methods are more likely to intend to use them highlights the importance of accurate information. Clear understanding reduces fear and anxiety, leading to more informed decisions. This fosters positive attitudes and reflects a supportive environment that promotes the intention to use LAPCs.
Strength and limitations of the study
This systematic review and meta-analysis represent the first attempt to evaluate the intention to use long-acting and permanent contraceptive methods among family planning users in Ethiopia. However, several limitations should be noted. First, the review was limited to English-language articles with accessible full texts, potentially excluding relevant studies published in other languages. Second, inconsistencies in variable categorization across the included studies hindered a comprehensive analysis of pooled odds ratios for all factors associated with LAPCs. All of the studies included were facility-based cross-sectional designs, which may limit the generalizability of the findings to the wider population. Additionally, the review incorporated studies from only five regions of Ethiopia, which could affect the accuracy of the overall prevalence estimate for the intention to use LAPCs among family planning users.
Implication of the study
Despite its limitations, this systematic review and meta-analysis provides valuable insights for policymakers, health program planners, and stakeholders by identifying key factors influencing the intention to use long-acting and permanent contraceptives (LAPCs) among family planning users. The study highlights critical determinants such as education, knowledge, attitudes, and misconceptions, which can inform targeted interventions aimed at increasing LAPC uptake. However, the limitations—such as inclusion of only English-language studies, reliance on facility-based cross-sectional designs, and representation from only five regions—suggest that the findings may not fully reflect the intention of the broader population across Ethiopia. Stakeholders should interpret the results with caution, recognizing that the true prevalence and predictors might vary in unrepresented areas or community-based settings. By understanding these strengths and limitations, policymakers can design targeted education and awareness programs, address myths and misconceptions through culturally sensitive communication strategies, improve family planning services in regions with lower intention to use LAPCs, and guide future research to fill gaps in underrepresented regions and incorporate more diverse study designs. Overall, this study provides actionable evidence to strengthen family planning programs, increase LAPC adoption, and reduce barriers, while highlighting areas where additional research is needed to inform national strategies more comprehensively.
Conclusion
This systematic review and meta-analysis highlights that the intention to use long-acting and permanent contraceptives (LAPCs) among family planning users is moderate, suggesting that uptake of these methods remains suboptimal. Factors such as education, knowledge, attitudes, and misconceptions play a critical role in shaping this intention. Interventions aimed at improving awareness, correcting misconceptions, and promoting positive attitudes toward LAPCs are likely to increase their adoption. Policymakers and health organizations should prioritize targeted education and behavior change strategies to enhance family planning outcomes.
Supplemental Material
sj-docx-1-phj-10.1177_22799036251395262 – Supplemental material for Intention to use long-acting and permanent contraceptive methods and its predictors among family planning users in Ethiopia: Systematic review and meta-analysis
Supplemental material, sj-docx-1-phj-10.1177_22799036251395262 for Intention to use long-acting and permanent contraceptive methods and its predictors among family planning users in Ethiopia: Systematic review and meta-analysis by Yeshiwas Ayale Ferede, Agerie Mengistie Zeleke and Worku Chekol Tassew in Journal of Public Health Research
Supplemental Material
sj-docx-2-phj-10.1177_22799036251395262 – Supplemental material for Intention to use long-acting and permanent contraceptive methods and its predictors among family planning users in Ethiopia: Systematic review and meta-analysis
Supplemental material, sj-docx-2-phj-10.1177_22799036251395262 for Intention to use long-acting and permanent contraceptive methods and its predictors among family planning users in Ethiopia: Systematic review and meta-analysis by Yeshiwas Ayale Ferede, Agerie Mengistie Zeleke and Worku Chekol Tassew in Journal of Public Health Research
Supplemental Material
sj-docx-3-phj-10.1177_22799036251395262 – Supplemental material for Intention to use long-acting and permanent contraceptive methods and its predictors among family planning users in Ethiopia: Systematic review and meta-analysis
Supplemental material, sj-docx-3-phj-10.1177_22799036251395262 for Intention to use long-acting and permanent contraceptive methods and its predictors among family planning users in Ethiopia: Systematic review and meta-analysis by Yeshiwas Ayale Ferede, Agerie Mengistie Zeleke and Worku Chekol Tassew in Journal of Public Health Research
Supplemental Material
sj-docx-4-phj-10.1177_22799036251395262 – Supplemental material for Intention to use long-acting and permanent contraceptive methods and its predictors among family planning users in Ethiopia: Systematic review and meta-analysis
Supplemental material, sj-docx-4-phj-10.1177_22799036251395262 for Intention to use long-acting and permanent contraceptive methods and its predictors among family planning users in Ethiopia: Systematic review and meta-analysis by Yeshiwas Ayale Ferede, Agerie Mengistie Zeleke and Worku Chekol Tassew in Journal of Public Health Research
Footnotes
Ethical considerations
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
All relevant data are provided within the manuscript and it’s supporting information files.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
