Abstract
Study Design
Prospective multicenter cohort study.
Objective
To evaluate the impact of surgeon experience on surgical safety, radiographic outcomes, and patient-reported outcomes (PROMs) following anterior cervical discectomy and fusion (ACDF) in patients with cervical degenerative disc disease (CDDD).
Methods
This prospective cohort study was conducted at five spine-specialized institutions in Japan. A total of 208 patients with CDDD who underwent ACDF between 2019 and 2022 were enrolled. Procedures were performed by either board-certified spine (BCS) surgeons (n = 150) or non-BCS (NBCS) surgeons (n = 58) under direct BCS supervision. Demographics, surgical variables, radiographic outcomes, and clinical results were compared. Evaluations included surgical duration, estimated blood loss (EBL), complications, cervical alignment and range of motion (ROM), Japanese Orthopaedic Association (JOA) scores, Visual Analog Scale (VAS), JOACMEQ, and SF-36 scores.
Results
Surgical duration was comparable between groups, but EBL was significantly greater in the NBCS group (20.2 ± 35.0 mL vs 12.2 ± 13.7 mL, P = .020). Complication rates were low and similar. No major adverse events occurred in either group. Cervical alignment was maintained, and ROM slightly decreased postoperatively without intergroup differences. Both groups showed significant neurological improvement. Gains in JOA scores, reductions in VAS scores, and improvements in JOACMEQ and SF-36 scores were comparable.
Conclusions
ACDF performed by NBCS surgeons under BCS supervision achieved clinical outcomes equivalent to those by BCS surgeons. These findings underscore the effectiveness of structured supervision in ensuring surgical safety and fostering competency in spine surgery.
Keywords
Introduction
Cervical degenerative disc disease (CDDD) is a leading cause of cervical radiculopathy and myelopathy, frequently resulting in neck pain, limb numbness, and impaired motor function. In patients unresponsive to conservative treatment, anterior cervical discectomy and fusion (ACDF) is a widely accepted surgical intervention aimed at decompressing neural structures and stabilizing the cervical spine.1,2 Compared to posterior approaches, the anterior route allows for direct access to ventral compressive pathology. Still, it requires meticulous dissection through a confined anatomical space surrounded by vital structures such as the esophagus, trachea, and carotid sheath. This complexity introduces technical challenges and increases the risk of intraoperative complications if exposure is inadequate or surrounding tissues are improperly handled.3-9
As such, performing an ACDF requires a precise understanding of regional anatomy and refined surgical skills. The surgeon’s level of experience may therefore have a significant impact on both procedural safety and clinical outcomes. In many clinical settings, particularly in academic and training hospitals, ACDF is performed not only by experienced surgeons but also by less-experienced surgeons under the supervision of senior staff.10,11 Although supervision is expected to minimize risks, the extent to which the operating surgeon’s experience influences factors such as operative time, blood loss, complication rates, and postoperative recovery remains unclear.12-16 To date, no prospective multicenter studies have evaluated the relationship between surgeon experience and clinical outcomes in ACDF. Therefore, a clearer understanding of this relationship is essential not only for ensuring patient safety but also for guiding the development of effective surgical training programs.
This large-scale, prospective, multicenter study aimed to investigate the impact of surgeon experience on both surgical and clinical outcomes following ACDF for CDDD, using a comprehensive, multidimensional approach that integrated traditional clinical and radiographic assessments with both physician- and patient-reported outcomes.
Materials and Methods
Study Design, Patient Demographics, and Characteristics
This prospective multicenter study enrolled 208 patients with CDDD, defined as symptomatic disc degeneration including cervical disc herniation (CDH), cervical spondylotic radiculopathy (CSR), and cervical spondylotic amyotrophy (CSA), who underwent ACDF at five medical institutions in Japan between January 2019 and December 2022. Patients were considered eligible if they met all of the following criteria: (1) presence of at least one clinical sign, such as cervical radiculopathy or muscle weakness with atrophy; (2) confirmation of anterior compression of the spinal cord or nerve roots on magnetic resonance imaging (MRI); (3) no previous cervical spine surgery; and (4) availability of postoperative follow-up data for at least two years. Patients were excluded if they were asymptomatic or presented with cervical kyphosis, active infection, rheumatoid arthritis, ankylosing spondylitis, spinal tumors, or coexisting lumbar spinal stenosis.
Preoperative evaluations were conducted in outpatient clinics by the assigned primary surgeon, regardless of whether the surgery was ultimately performed by a board-certified spine (BCS) or a non-BCS (NBCS) surgeon. Surgical indication and extent of fusion were determined through discussion among the institutional spine team. Demographic characteristics, medical history, presenting symptoms, imaging findings, surgical details, and clinical outcomes were prospectively recorded for all patients. The study protocol was approved by the Ethics and Institutional Review Board (approval number: 20180045), and written informed consent was obtained from all participants prior to surgery.
BCS and NBCS Surgeons
In Japan, the qualification of BCS surgeon is granted upon fulfillment of several requirements: (1) certification as a Spine Specialist by the Japanese Orthopaedic Association (JOA), (2) active membership in the Japanese Society for Spine Surgery and Related Research (JSSR), (3) a surgical record of more than 300 spine and spinal cord procedures, including at least 200 performed as the primary surgeon—of which at least 20 must involve the cervical spine and 60 the lumbar spine, (4) attendance at a minimum of two JSSR annual meetings within the past 5 years, and (5) authorship of at least five clinical publications related to spine or spinal cord disorders.
In this study, 23 BCS surgeons and 12 NBCS surgeons were included. Unlike the North American training system, Japan lacks a formal residency or fellowship structure in spine surgery. Instead, spine surgeons are classified simply as either BCS or NBCS, based on their qualifications and experience.
Radiographic Images and MRI Findings
In the present study, radiological assessments of the cervical spine were determined by measuring the C2-7 angles on lateral radiographs taken in the neutral, flexion, and extension positions at two-time points: before surgery and at the 2-year postoperative follow-up. The C2-7 angle was measured using the Cobb method, which calculates the angle between the lower endplates of the C2 and C7 vertebrae. Cervical range of motion (ROM) was determined by subtracting the flexion C2-7 angle from the extension C2-7 angle. In addition, preoperative MRI was used to evaluate the level of spinal compression and to detect any intramedullary high-signal intensity areas on T2-weighted images.
Clinical Outcomes
Clinical outcomes were evaluated both preoperatively and at two years after surgery. The Japanese Orthopaedic Association (JOA) score, with a maximum of 17 points, was used to assess neurological status. The JOA recovery rate (%) was calculated using the following formula: (JOA score at 2 years postoperatively – preoperative JOA score)/(17 – preoperative JOA score) × 100, representing the percentage improvement from baseline. 17 Pain and stiffness in the neck or shoulders, chest tightness, and pain or numbness in the arms, hands, or lower body (from the chest to the toes) were assessed using the Visual Analog Scale (VAS), ranging from 0 to 100 mm, with lower scores indicating less pain and greater comfort. PROMs were evaluated using the JOA Cervical Myelopathy Evaluation Questionnaire (JOACMEQ) and the 36-Item Short Form Health Survey (SF-36).18,19 The JOACMEQ assesses quality of life and functional status across several domains, including the cervical spine, upper and lower extremities, and bladder function. The SF-36 comprises eight subscales—physical functioning (PF), role-physical (RP), bodily pain (BP), general health (GH), vitality (VT), social functioning (SF), role-emotional (RE), and mental health (MH)—as well as two summary scores: the physical component summary (PCS) and the mental component summary (MCS).
Any surgery-related event occurring within 30 days postoperatively was classified as a perioperative complication. Perioperative complications were predefined as major adverse events, including C5 palsy, neurological deterioration, surgical site infection (SSI), hematoma, dural tear, cerebrospinal fluid (CSF) leakage, implant failure, airway obstruction, or screw misplacement. Dysphagia was not systematically recorded because it was not included in the prespecified list of major complications and is primarily a patient-reported symptom without a standardized objective assessment method, making uniform evaluation difficult.
Statistical Analysis
Continuous variables are reported as means ± standard deviations, and categorical variables are presented as percentages. To compare baseline demographics, surgical characteristics, radiographic findings, and clinical outcomes between the BCS and NBCS groups, unpaired t-tests were used for continuous variables, and chi-square tests were applied to categorical variables. Multiple regression analysis was conducted to adjust for potential confounding factors in the comparisons of JOA scores, VAS, JOACMEQ, and SF-36 outcomes. The minimum clinically important difference (MCID) for the JOA score was defined as 2.5 points. 20
In the JOACMEQ, treatment was considered effective if (1) the post-treatment score increased by at least 20 points compared to the pre-treatment score, or (2) the pre-treatment score was below 90 and the post-treatment score reached 90 or higher. Patients whose scores were 90 or above both before and after treatment were included in the dataset but excluded from the effectiveness analysis. The effective rate for each group was calculated using the following formula: (Number of patients classified as “effective”)/[(Total number of patients in the group) – (Number of patients with both pre- and post-treatment scores ≥90)]. 18 Group comparisons of effective rates were performed using the chi-square test.
Statistical significance was determined at P-values of <.05 and <.001. All statistical analyses were performed using SPSS version 29.0 (IBM Corp., Armonk, NY, USA).
Results
Patient Demographics and Characteristics
Demographics of 208 Patients With CDDD Who Underwent ACDF by BCS or NBCS Surgeons
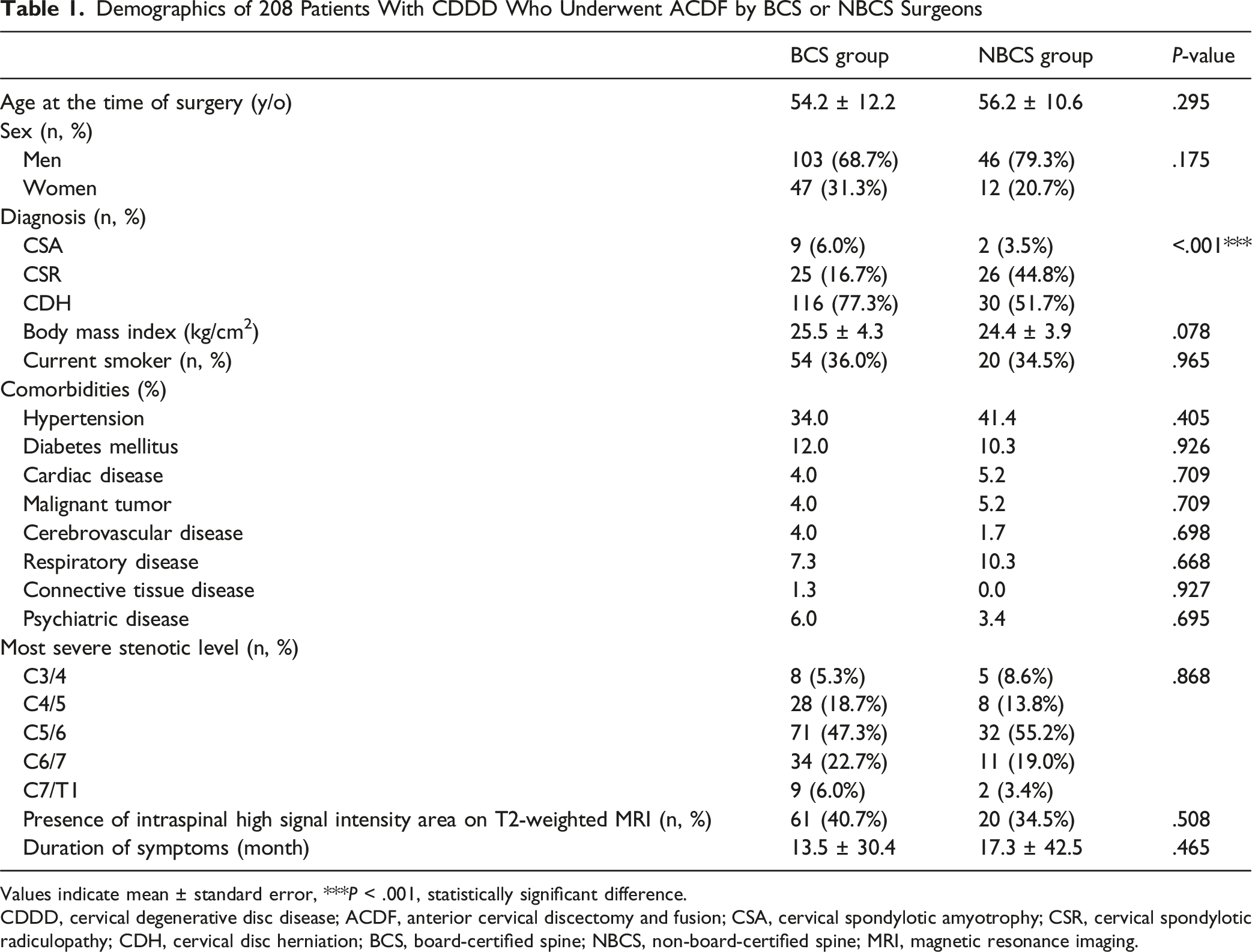
Values indicate mean ± standard error, ***P < .001, statistically significant difference.
CDDD, cervical degenerative disc disease; ACDF, anterior cervical discectomy and fusion; CSA, cervical spondylotic amyotrophy; CSR, cervical spondylotic radiculopathy; CDH, cervical disc herniation; BCS, board-certified spine; NBCS, non-board-certified spine; MRI, magnetic resonance imaging.
Surgical Information and Perioperative Complications
Comparison of Surgical Information and Perioperative Complications Between BCS and NBCS Group
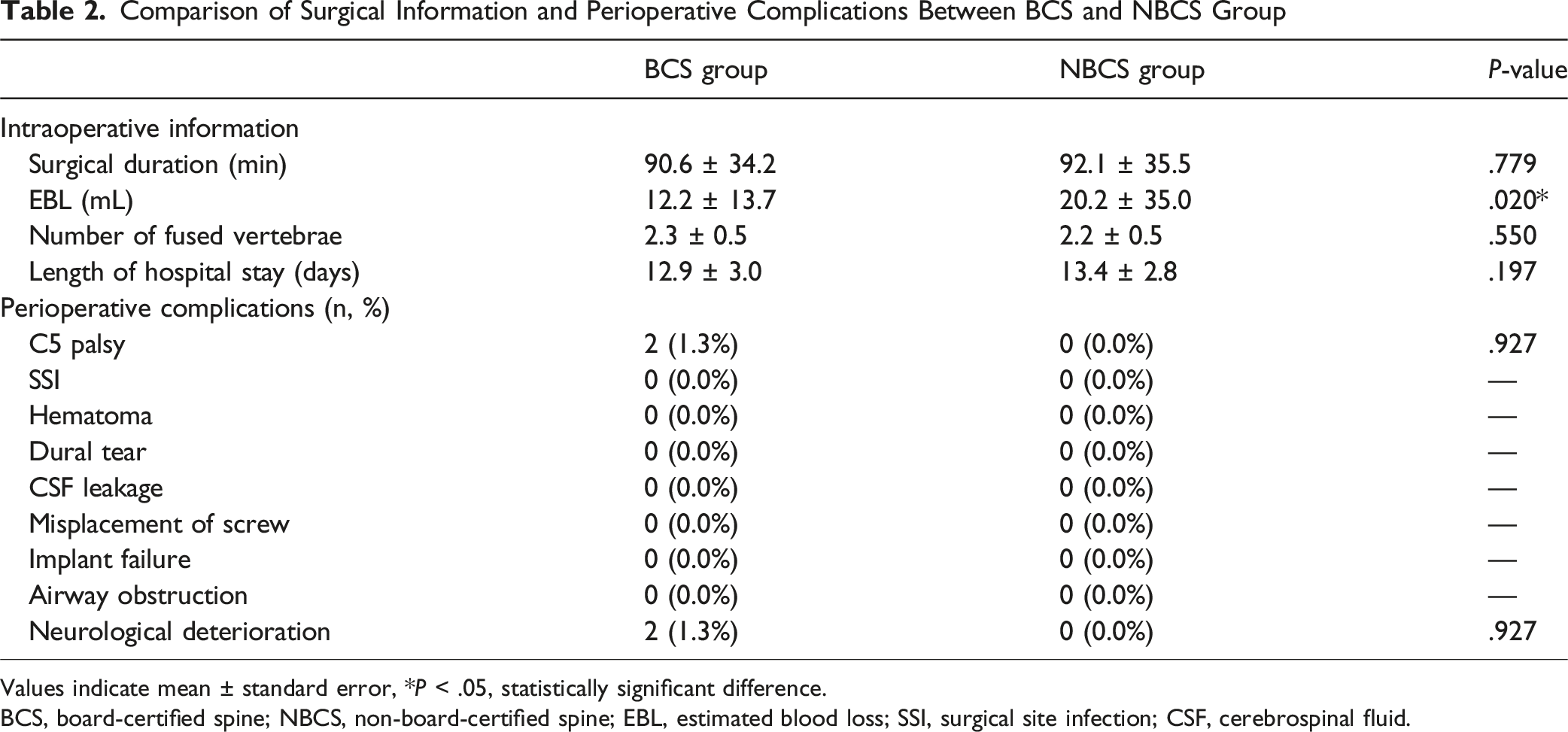

Values indicate mean ± standard error, *P < .05, statistically significant difference.
BCS, board-certified spine; NBCS, non-board-certified spine; EBL, estimated blood loss; SSI, surgical site infection; CSF, cerebrospinal fluid.
Postoperative Radiological Outcomes
Comparison of Preoperative and 2 Years Following Surgery Each Cervical Sagittal Parameter Between BCS and NBCS Group
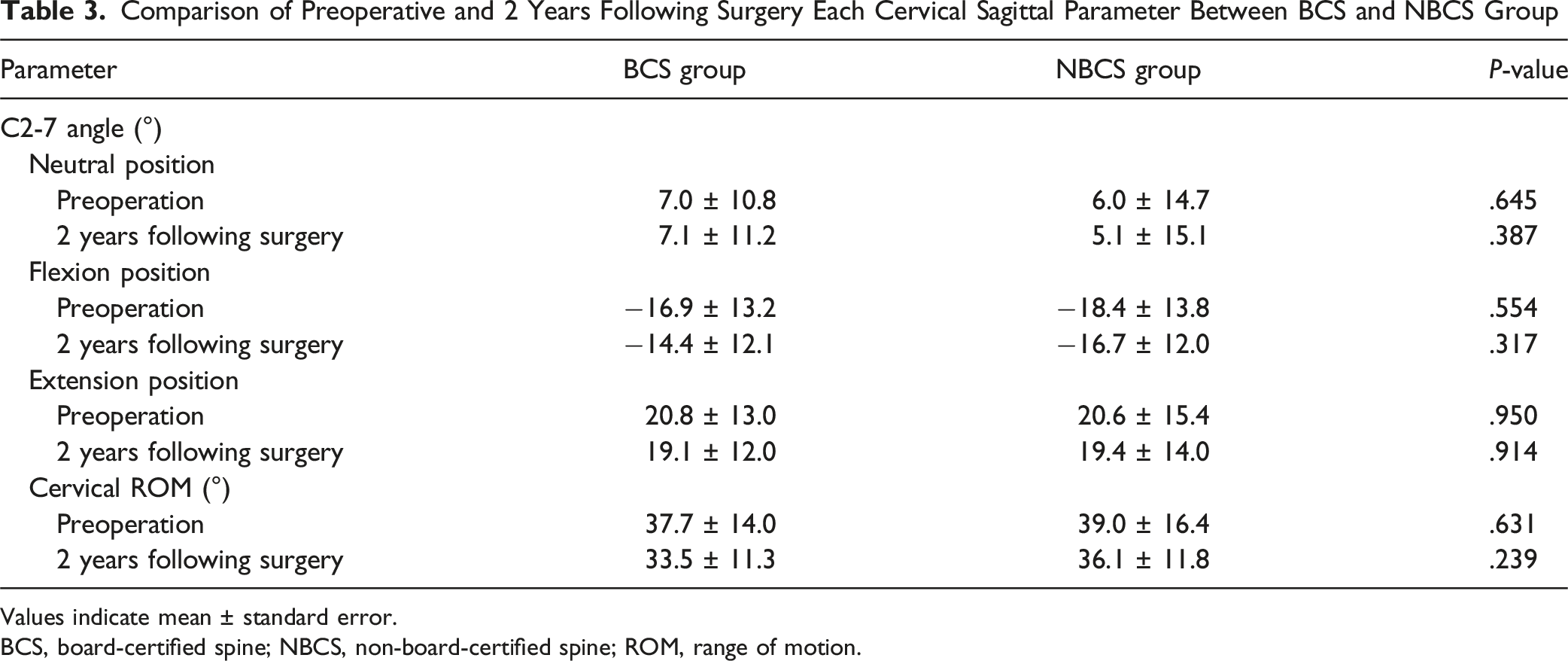
Values indicate mean ± standard error.
BCS, board-certified spine; NBCS, non-board-certified spine; ROM, range of motion.
Clinical Outcomes After ACDF
Clinical outcomes between the BCS and NBCS groups were evaluated and compared using multiple regression analysis, adjusting for potential confounders that differed significantly between groups (diagnosis and amount of EBL). No additional complexity-related variables showed intergroup differences at baseline; therefore, only these factors were included in the models. The JOA score was improved significantly after surgery in both groups. The preoperative JOA score was 13.5 [95% CI: 12.8 to 13.9] in the BCS group and 13.4 [13.0 to 14.0] in the NBCS group (P = .725), and the postoperative score was 16.2 [15.8 to 16.6] and 16.0 [15.5 to 16.4], respectively (P = .605). The change in JOA score was similar between the two groups (ΔJOA: 2.7 [2.0 to 3.1] vs 2.6 [1.8 to 2.7], P = .807), and so was the JOA score recovery rate (56.6% [45.3 to 68.0] vs 67.4% [47.9 to 86.9], P = .354).
VAS scores for neck and shoulder pain decreased from 49.1 [44.2 to 54.0] mm to 34.0 [29.0 to 39.1] mm in the BCS group and from 57.0 [48.6 to 65.3] mm to 33.3 [24.6 to 42.0] mm in the NBCS group. Although both groups showed reductions in pain levels, the change from baseline, expressed as ΔVAS, did not significantly differ between the groups (−15.1 [−21.2 to −8.9] mm vs −23.8 [−34.4 to −13.2] mm, P = .169). Similarly, changes in VAS scores for chest tightness and extremity numbness were comparable between the groups. In particular, pain or numbness in the arms or hands, the ΔVAS was −26.1 [−32.0 to −20.2] mm in the BCS group and −31.8 [−42.0 to −21.6] mm in the NBCS group (P = .201).
Comparison of Clinical Outcomes Between BCS and NBCS Group
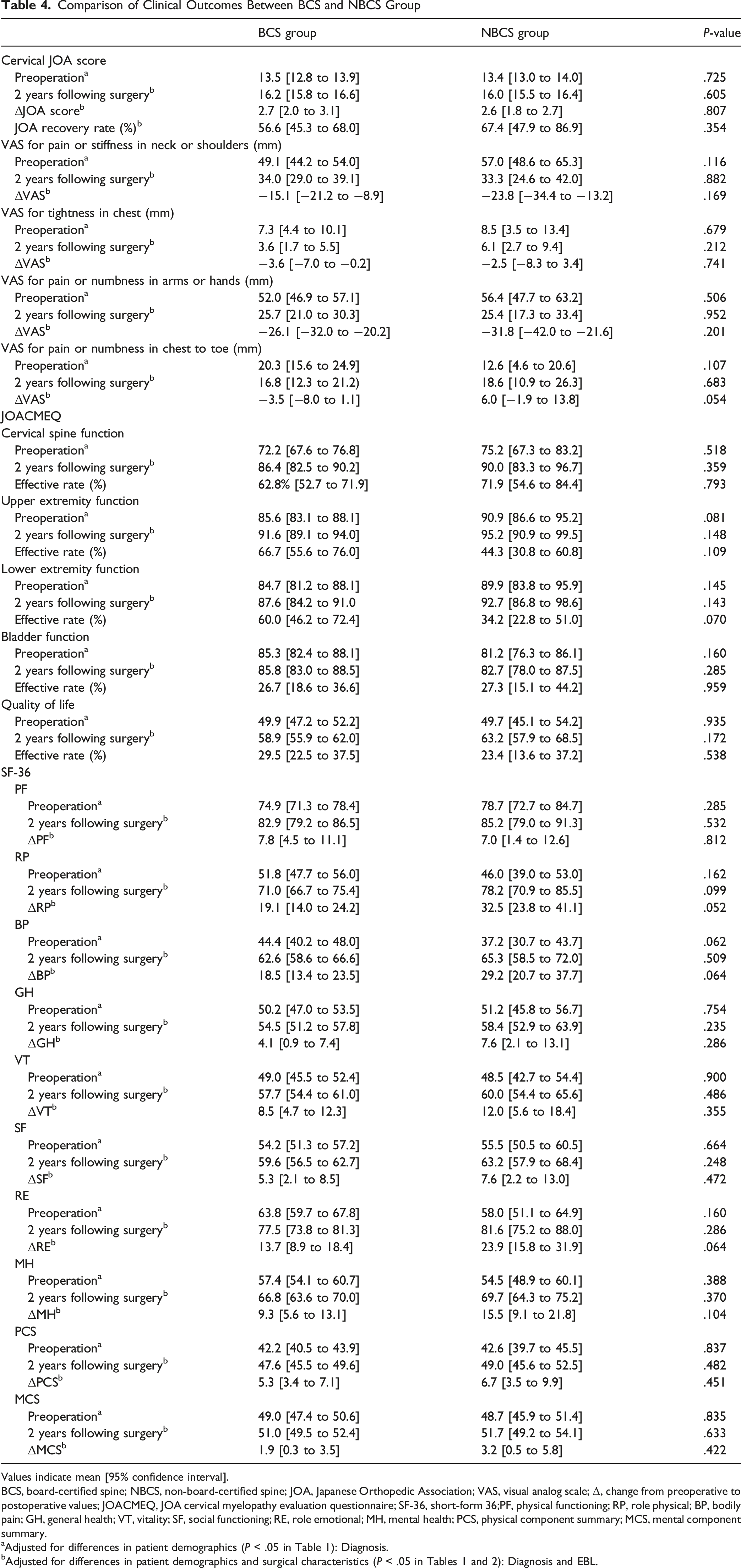
Values indicate mean [95% confidence interval].
BCS, board-certified spine; NBCS, non-board-certified spine; JOA, Japanese Orthopedic Association; VAS, visual analog scale; Δ, change from preoperative to postoperative values; JOACMEQ, JOA cervical myelopathy evaluation questionnaire; SF-36, short-form 36;PF, physical functioning; RP, role physical; BP, bodily pain; GH, general health; VT, vitality; SF, social functioning; RE, role emotional; MH, mental health; PCS, physical component summary; MCS, mental component summary.
aAdjusted for differences in patient demographics (P < .05 in Table 1): Diagnosis.
Subgroup Analyses
In subgroup analyses limited to patients with CDH, baseline demographics and comorbidities were comparable between groups (Supplemental Table 1). Although the NBCS group had a greater EBL (21.8 ± 35.9 mL vs 12.3 ± 13.7 mL, P = .026), there were no significant differences in operative time, perioperative complications, radiographic alignment, or clinical outcomes. Both groups achieved comparable improvements in JOA scores, VAS, JOACMEQ, and SF-36 (Supplemental Tables 2-4).
Discussion
This prospective study is the largest and most comprehensive to date evaluating whether surgical outcomes of ACDF differ between procedures performed by BCS surgeons and those by NBCS surgeons under direct supervision from BCS surgeons. Our results demonstrated that, although surgeries performed by NBCS surgeons were associated with a greater amount of EBL, there were no significant differences in surgical duration, perioperative complication rates, changes in cervical alignment, neurological improvement, or physician- and patient-reported outcomes. These findings suggest that ACDF for CDDD can be safely and effectively performed by less-experienced surgeons when supported by appropriate supervision and a structured institutional educational system.
Previous studies have indicated that surgical outcomes may be influenced by surgeon experience, particularly during the early stages of training.12-14 For example, Zekaj et al 15 reported that while novice surgeons had longer operative times, complication rates remained similar under expert supervision, underscoring the importance of guidance in maintaining procedural safety. Our study found that although amount of EBL was significantly higher in surgeries performed by NBCS surgeons, other key metrics, including surgical duration and length of hospital stays, were comparable between the two groups. These findings indicated that, with direct supervision from BCS surgeons, NBCS surgeons were capable of achieving clinical outcomes comparable to those of BCS surgeons. A key strength of this study was its prospective design and relatively large cohort, which minimized selection and recall bias, allowing for a more accurate evaluation of the impact of surgeon experience on clinical outcomes after ACDF.
Perioperative complications following ACDF have been variably reported in the literature, with risk factors including advanced age, prolonged surgical time, anemia, and diabetes.3-8,21 Gruskay et al, 5 utilizing an extensive national database, linked these factors to higher complication rates and extended hospital stays. Conversely, long-term prospective studies by Buttermann et al and Hirvonen et al demonstrated low complication rates and sustained clinical benefits, emphasizing the procedure’s safety and durability.1,22 In our study, no major complications—such as SSI, dural tears, CSF leakage, hematoma, or implant failure—were observed in either group. Postoperative C5 palsy or neurological deterioration was infrequent and occurred only in the BCS group, without statistical significance. These results demonstrated that ACDF can be safely performed by NBCS surgeons, with perioperative outcomes comparable to those of BCS surgeons.
Cervical alignments, such as lordosis and sagittal balance, are essential for preserving spinal biomechanics and preventing adjacent segment degeneration. Their maintenance largely depends on surgical technique, including precise disc space preparation and appropriate graft placement.9,23-26 In this study, radiographic analyses showed that cervical sagittal alignment and ROM were well maintained regardless of surgeon experience. Both groups demonstrated stable C2-7 angles in neutral, flexion, and extension positions, with only minor reductions in ROM at the 2-year follow-up, findings consistent with postoperative changes after ACDF. These results showed that all cases were performed with a consistent surgical technique, indicating that, under direct supervision, surgeon experience did not have a significant impact on the biomechanical outcomes of ACDF. A clear system of intraoperative guidance provided by experienced attending surgeons, therefore, appears to play a crucial role in maintaining surgical quality.
In addition to physician-assessed measures such as the JOA score, PROMs provide important information about postoperative neurological improvement by capturing patients’ perspectives on function and QOL.27-29 In our study, PROMs, including the JOACMEQ and SF-36, revealed no significant differences in pain relief, functional improvement, or health-related QOL between the BCS and NBCS groups. These findings suggest that, from the patient’s perspective, the level of surgeon experience did not substantially affect postoperative satisfaction or improvement, provided the surgery was appropriately supervised. However, the JOACMEQ effective rates for upper and lower extremity function were numerically lower in the NBCS group; although not statistically significant, these secondary, dichotomized endpoints were not powered a priori and should be interpreted with caution. In particular, although the differences in JOACMEQ effective rates for extremity function approached statistical significance, the study was not adequately powered for this secondary outcome, and a type II error cannot be excluded. Post-hoc analyses indicated that statistical power was sufficient for the primary outcome of JOA score improvement, but limited for dichotomized secondary endpoints such as JOACMEQ effective rates. As PROMs capture dimensions of care from the patient’s perspective, their inclusion in future studies is important for achieving more comprehensive and balanced outcome evaluations.
Additional subgroup analyses focusing only on patients with CDH yielded results consistent with those of the overall cohort. Although the NBCS group had higher EBL, perioperative safety, radiographic findings, and PROMs were otherwise similar between groups. These results support the reliability of our conclusions and indicate that diagnostic differences were unlikely to have influenced the main findings. These subgroup findings suggest that the main results were not explained by diagnostic imbalance. Nevertheless, differences in diagnostic composition between groups remain a potential source of confounding, and this heterogeneity should be considered when interpreting our conclusions.
Several limitations of this study should be noted. First, while the study was not randomized, there was no intentional triage of more complex cases to BCS surgeons. The observed differences in diagnostic distribution likely arose by chance; however, residual confounding cannot be entirely excluded, and case complexity may still have influenced outcomes. Second, all procedures performed by NBCS surgeons were conducted under direct supervision. The supervising BCS was present as the first assistant throughout the procedure, providing continuous guidance without taking over the surgical maneuvers, and the takeover rate was 0%. This structured supervision likely contributed to the comparable outcomes observed. Thus, our findings reflect the effectiveness of supervised training rather than the independent performance of NBCS surgeons. Future studies should investigate the performance of NBCS surgeons in unsupervised settings to more accurately assess their independent competency and surgical safety. Third, the study was conducted in Japan, where the structure of spine surgery training differs from that in other countries. In Japan, spine surgeons are classified as either BCS or NBCS based on surgical experience and academic activity, rather than through standardized residency or fellowship tracks. By contrast, in many North American and European countries, structured residency and fellowship programs offer standardized exposure to spine surgery before independent practice. These differences in training frameworks may limit the generalizability of our findings, and validation in countries with different systems is necessary. Fourth, although the difference in EBL between groups reached statistical significance (12.2 ± 13.7 mL vs 20.2 ± 35.0 mL), the absolute values were minimal and unlikely to represent a clinically meaningful difference. This difference was not associated with an increase in perioperative complications or neurological recovery. It should be interpreted as reflecting statistical sensitivity rather than an actual difference in surgical invasiveness. Fifth, MCIDs have not been established in Japanese populations for outcome measures other than the JOA score. While the observed improvements and 95% CIs for JOA generally exceeded the established threshold of 2.5 points, the absence of validated MCIDs for VAS, SF-36 subscales, and JOACMEQ domains limits the extent to which the clinical relevance of these changes can be interpreted. Sixth, fusion status and reoperations for pseudarthrosis were not systematically assessed in this study. Although sagittal alignment and cervical ROM were evaluated, the lack of information on bony fusion limits the ability to consider long-term biomechanical outcomes beyond the 2-year follow-up fully. Seventh, although dysphagia was not systematically recorded in this study, future prospective work should include standardized assessment instruments across sites to minimize underestimation and allow for a more reliable comparison of this complication. Lastly, long-term follow-up is necessary to determine whether the comparable outcomes observed between BCS and NBCS surgeons are sustained over time.
Conclusion
This prospective multicenter study evaluated the influence of surgeon experience on surgical and clinical outcomes in patients with CDDD following ACDF. While surgeries performed by NBCS surgeons were associated with a greater amount of EBL, surgical duration, perioperative complication rates, cervical alignment and mobility on radiographic assessment, and postoperative physician- and patient-reported outcomes were comparable between the two groups. These findings indicate that ACDF for CDDD is a safe and effective surgical procedure, even when performed by NBCS surgeons under direct supervision from experienced spine surgeons, thereby contributing to the advancement of surgical education and patient care.
Supplemental Material
Supplemental Material - Does Surgeon Experience Influence Surgical Safety and Patient Satisfaction After Anterior Cervical Discectomy and Fusion? A Prospective Multicenter Comparison Study Between Non-Board-Certified and Board-Certified Spine Surgeons
Supplemental Material for Does Surgeon Experience Influence Surgical Safety and Patient Satisfaction After Anterior Cervical Discectomy and Fusion? A Prospective Multicenter Comparison Study Between Non-Board-Certified and Board-Certified Spine Surgeons by Toshiki Okubo, Narihito Nagoshi, Junichi Yamane, Norihiro Isogai, Reo Shibata, Takahiro Kitagawa, Kentaro Ago, Takeshi Fujii, Yosuke Horiuchi, Takahito Iga, Kazuki Takeda, Masahiro Ozaki, Satoshi Suzuki, Morio Matsumoto, Masaya Nakamura, Kota Watanabe in Global Spine Journal
Footnotes
Acknowledgments
We extend our sincere appreciation to all participating institutions for their collaboration and support. During the preparation of this manuscript, ChatGPT (OpenAI) and Grammarly (Grammarly Inc.) were used to refine grammar and correct typographical errors. These tools were employed solely to enhance clarity and readability, without altering the scientific content or interpretation of the results.
ORCID iDs
Ethical Considerations
The study protocol was approved by the Institutional Review Board (approval number: 20180045).
Consent to Participate
Written informed consent was obtained from all participants prior to their inclusion in the study.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The datasets generated and/or analyzed in this study are available from the corresponding author on request.
Supplemental Material
Supplemental material for this article is available online.
