Abstract
Study Design
Multicenter, cross-sectional study of cross-cultural adaptation and psychometric validation of a patient-reported outcome measure.
Objective
To adapt and validate the Spanish version of the AO Spine Patient-Reported Outcome Spine Trauma (PROST) questionnaire for assessing functional outcomes in patients with traumatic spinal injuries.
Methods
The translation followed Beaton’s standardized cross-cultural adaptation process: forward translation, synthesis, back-translation, expert committee review, and final version development. Adult patients (≥18 years) with spinal trauma within the last 13 months were recruited from 4 Level 1 trauma centers across Latin America. Exclusion criteria included polytrauma (ISS >15), complete paralysis (ASIA A–B), and cognitive impairment. Participants completed the Spanish PROST and the SF-36. Concurrent validity was evaluated using Spearman’s correlation between PROST and SF-36 domains. Internal consistency was assessed via Cronbach’s alpha.
Results
A total of 108 patients were included (mean age 46 ± 15.8 years; 57% male). The Spanish PROST showed excellent internal consistency (α > 0.96). It showed a strong correlation with the SF-36 Physical Functioning domain (rs = 0.83;
Conclusion
The Spanish AO Spine PROST is a valid, reliable tool for assessing functional outcomes in spinal trauma patients. These findings support its use in both clinical practice and research settings within Spanish-speaking populations.
Introduction
Spinal trauma represents a significant global concern, primarily due to its well-documented clinical and socioeconomic consequences, which can encompass severe impairment, disability, and even mortality.1,2 Current estimates suggest that the global incidence of traumatic spinal injury is approximately 10.5 cases per 100,000 individuals, with significant geographical variations. 3 Despite spinal cord injury being the primary source of morbidity and mortality, the presence of concomitant non-vertebral injuries, in addition to the physiological impact of trauma, increases the severity and adds complexity to the clinical management of spinal trauma patients. 4
The available literature reflects a discrepancy between the burden of spinal trauma and research production. 5 While high-income countries primarily contribute to the data and research that inform spinal management, the proportion of traumatic spinal injury patients is significantly higher in low- and middle-income countries compared to high-income countries.3,5 To address this disparity, there is a necessity to implement a global strategy that will harmonize research methodologies and tools, with the aim of facilitating the assessment of complex variables, including spinal trauma outcomes.6,7
The majority of existing instruments designed to evaluate the outcomes of treatment for spinal diseases have been developed for chronic degenerative conditions and, therefore, offer only a limited degree of usefulness in the context of spinal trauma.6,7 We believe that this is a critical issue to resolve to promote global research and improve the accuracy of data on spinal trauma injuries.
The AO Spine Knowledge Forum (KF) Trauma developed a disease-specific outcome measure for patients suffering from spinal trauma: the PROST questionnaire. The original questionnaire was developed and validated in Dutch.8,9 Subsequently, cross-cultural adaptations of the PROST questionnaire were performed for English, Nepali, German and Slovak versions, with outstanding results.10-13 The present study aims to perform a cross-cultural validation of the AO Spine PROST questionnaire from English to Spanish in people who have suffered traumatic spinal fractures.
Materials and Methods
Ethics Approval and Informed Consent
The study was approved by the Institutional Review Board of each participating center. The approval codes were 8936, 2017-97, 15018, and CEC/17/2022. All participants provided written informed consent prior to enrollment, in accordance with the Declaration of Helsinki and local ethical regulations.
Translation and Cross-Cultural Adaptation
The AOSpine PROST was translated and culturally adapted from English to Spanish in accordance with established guidelines by Beaton et al 14 . This process consisted of 4 stages: forward translation, synthesis, back translation, and expert committee review.
Initially, two native Spanish speakers with a high level of proficiency in English independently translated the AOSpine PROST from English to Spanish. Both were teachers; one specialized in English language and the other in orthopedic biomechanics. A meeting with the two translators and a recording observer was held to discuss the translations and create a synthesized version. Subsequently, two independent, bilingual native Spanish speakers, who were also physiotherapists and orthopedic researchers, translated the synthesized text back into English. These back translators were blinded to the original AOSpine PROST to avoid introducing information bias.
In the next stage, an expert committee was convened to review all translations and written reports. The committee was comprised of spinal surgeons from a participating center, physical therapists, and experienced translators. The committee assessed the equivalence of the pre-final Spanish version to the original English AOSpine PROST in terms of semantics, idioms, and conceptual meaning. Following this discussion, the expert committee developed the final Spanish version of the questionnaire.
For validation, the final version of the questionnaire was administered to the 108 participants who were subjects of the study.
Patients and Study Procedures
Adult patients (≥18 years of age) with traumatic spinal column injuries sustained within 13 months before the study were included. Eligibility required the ability to comprehend and accurately complete the questionnaires, thus excluding individuals with cognitive impairment. Patients with complete paralysis (ASIA impairment grade A or B at hospital discharge) and polytrauma (ISS >15) were excluded. Recruitment occurred at 4 level 1 trauma centers in Latin America. Patients who attended follow-up appointments at outpatient clinics within 13 months post-trauma were evaluated for eligibility. After obtaining informed consent, the participants were asked to complete the questionnaire.
Instruments
The questionnaire was administered in paper format, and a member of the research team subsequently collected the responses and entered the data into the electronic form hosted on the REDCap platform. REDCap (Research Electronic Data Capture) is a secure, web-based software platform designed to support data capture for research studies, developed by Vanderbilt University. The first section of the questionnaire was the AOSpine PROST, which included 19 questions addressing various aspects of functioning. Each item utilized a 0-100 numeric rating scale, where 0 represented no function and 100 denoted pre-injury functional level. The scale was supplemented with smiley faces at the end of the ruler. For concurrent validity, the AOSpine PROST was compared with a validated outcome instrument for patients with traumatic spinal column injuries. However, in the absence of such an instrument, the AOSpine PROST was followed by the Medical Outcomes Study 36-item Short-Form Health Survey (SF-36) as a reference standard. The SF-36 is the most commonly used generic instrument for measuring outcomes in studies involving patients with spinal trauma. It comprises 36 questions assessing eight health subscales, from which the physical component summary (PCS) and mental component summary (MCS) were derived. Scores range from 0 to 100, with higher scores indicating better outcomes. Additionally, patients were asked to respond to questions regarding any difficulties encountered while completing the AOSpine PROST, any questions deemed inapplicable, any relevant questions that were missing, and their self-reported degree of recovery. The research team also gathered background information on the participants, including demographic information and trauma-related factors, and evaluated their recovery using both clinical and radiological findings.
Statistical Analysis
Descriptive statistics and frequency analyses were performed to summarize patient characteristics. Concurrent validity was assessed by calculating the Spearman correlation coefficient (rs) between the AOSpine PROST and the SF-36. The rs ranges from +1 to −1, where +1 represents a perfect positive correlation, 0 indicates no correlation, and −1 reflects a perfect negative correlation. A correlation coefficient of 0.70 or greater was considered evidence of acceptable concurrent validity.
Results
Demographic Data
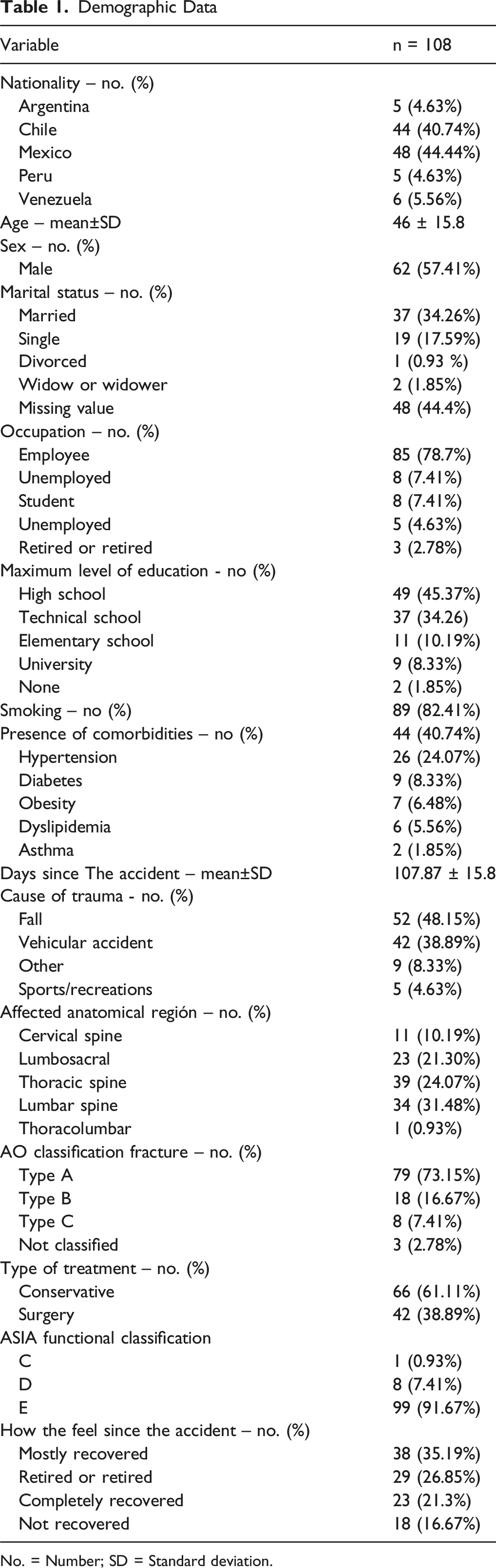
No. = Number; SD = Standard deviation.
Demographic Characteristics
Participants were recruited from 4 healthcare centers. In terms of nationality, 44.44% of participants were Mexican (n = 48), 40.74% were Chilean (n = 44), 5.56% were Venezuelan (n = 6), and Argentinean and Peruvian nationalities each accounted for 4.63% (n = 5). The mean age of the sample was 46 years (SD = 15.8). Regarding sex distribution, 57.41% of the participants were male (n = 62) and 42.59% were female (n = 46).
Marital status showed a variety of responses, with the most common being married (34.26%, n = 37) and single (17.59%, n = 19). A small proportion of participants reported being divorced (0.93%, n = 1), separated (0.93%, n = 1), or widowed (1.85%, n = 2). Marital status was unavailable for 44.44% of participants (n = 48).
Most participants were employed (68.52%, n = 74). Other occupations included students (7.41%, n = 8), homemakers (7.41%, n = 8), unemployed individuals (4.63%, n = 5), self-employed workers (3.71%, n = 4), and retirees (2.78%, n = 3). Job seekers accounted for 0.93% (n = 1), while 4.63% (n = 5) were categorized as “Other.”
Clinical Characteristics
The thoracic spine was the most frequently affected region, reported in 39 participants (36.11%), followed by the lumbar spine with 34 participants (31.48%). Other affected areas included the lumbosacral junction (23 participants, 21.30%), cervical spine (11 participants, 10.19%), and lastly, a single case involved the thoracolumbar junction (0.93%, n = 1).
Functional classification of neurological status, based on the AOSpine classification, revealed that most participants were classified as Grade E (n = 99,91.67%), followed by Grade D (n = 8,7.41%) and Grade C (n = 1,0.93%).
Concurrent Validity
Spearman Correlation Between AOSpine PROST and SF-36 Subscales
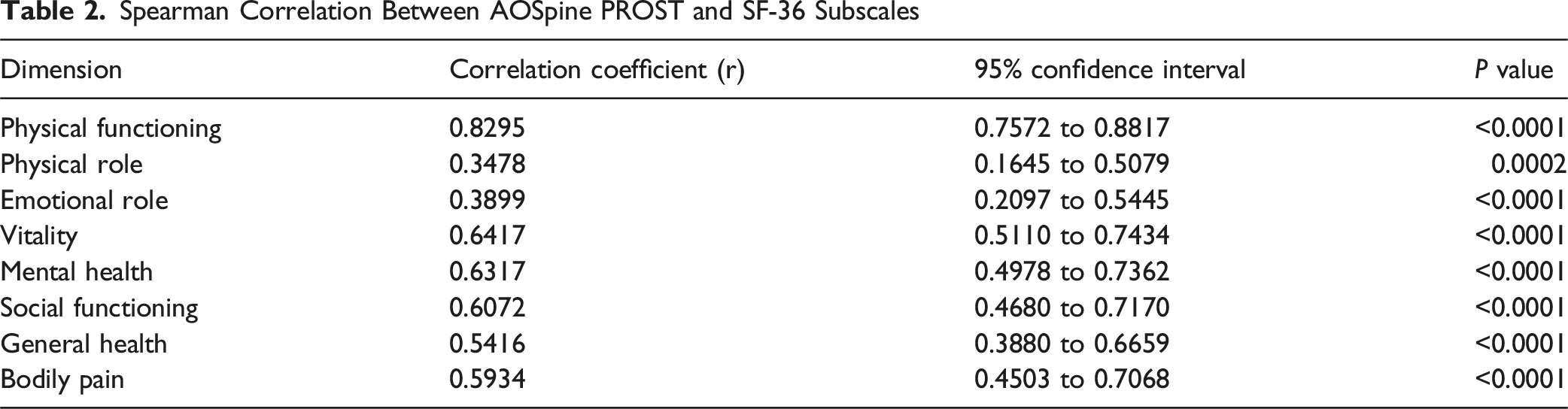
The strongest correlation was observed with the Physical Functioning dimension (r = 0.8295; 95% CI: 0.7572 to 0.8817;
Moderate correlations were identified with Role Physical (r = 0.3478; 95% CI: 0.1645 to 0.5079;
Finally, moderate to strong correlations were found with General Health (r = 0.5416; 95% CI: 0.3880 to 0.6659;
Internal Consistency
To assess the reliability of the AOSpine PROST, we calculated the internal consistency using Cronbach’s alpha. The scale demonstrated excellent internal consistency with an overall Cronbach’s alpha coefficient of 0.96. This finding confirms that the items within the AOSpine PROST are highly reliable and consistently measure the same construct.
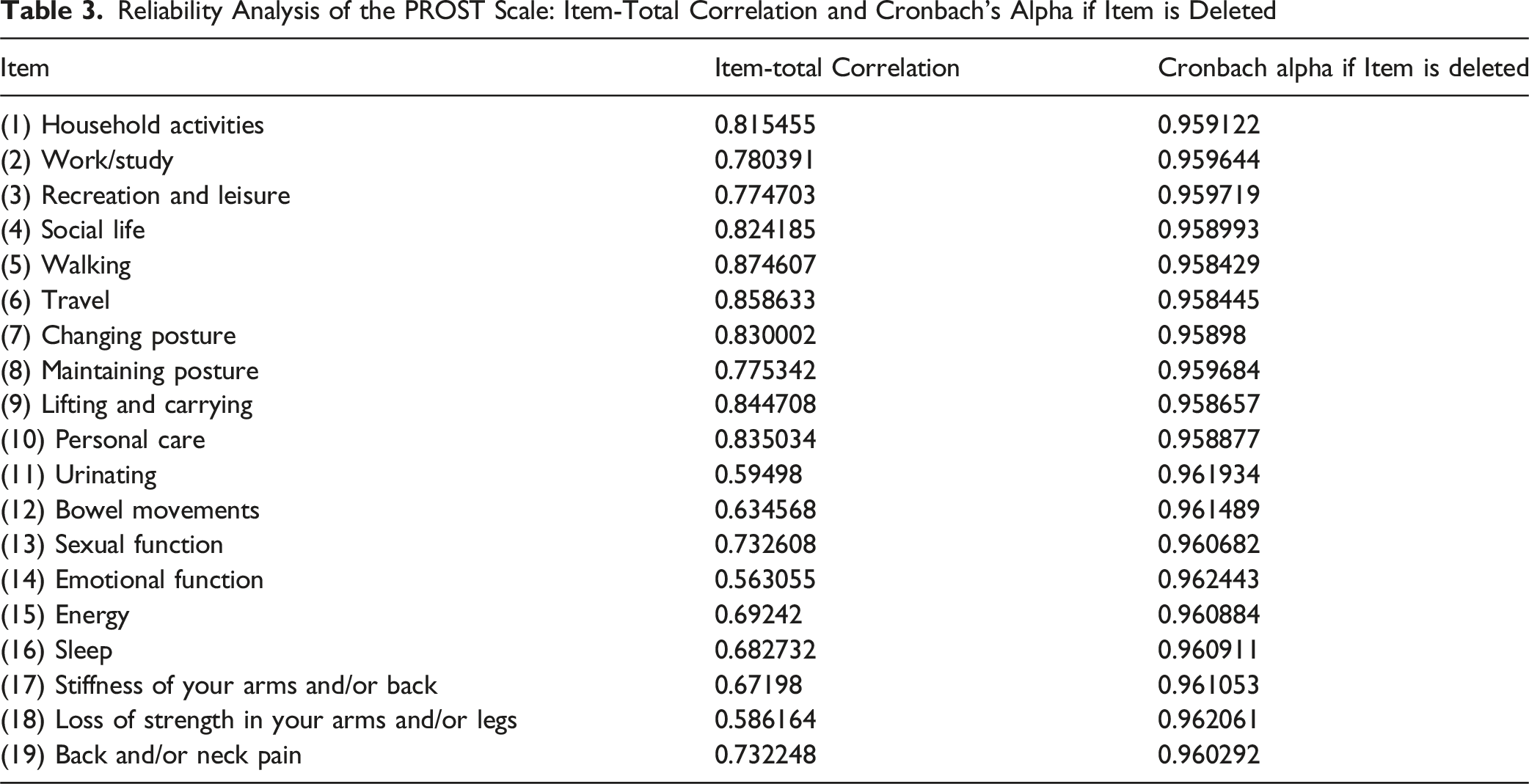
Further analysis of the item-total correlations revealed a strong degree of homogeneity among the scale’s components, with most items showing strong correlations with the total score. For instance, items such as “Walking” (0.87), “Travel” (0.86), and “Lifting and carrying” (0.84) demonstrated particularly high item-total correlations, indicating their strong contribution to the overall scale. In contrast, items related to “Emotional function” (0.56), “Loss of strength in your arms and/or legs” (0.59), and “Urinating” (0.59) showed the lowest item-total correlations. Despite these variations, the analysis showed that the deletion of any single item did not result in an increase in the Cronbach’s alpha value, reinforcing that all items are essential and contribute meaningfully to the scale’s overall reliability. This strong internal consistency provides robust evidence that the AOSpine PROST is a reliable tool for measuring spinal functional status in this population.
Discussion
The development of the AOSpine PROST has addressed a critical gap in the literature by providing a disease-specific outcome measure for patients with spinal trauma. 8 Previously, other non-specific patient reported outcomes have been used to analyse outcomes in spinal trauma care with an inevitable bias caused by the primary conflict that these tools were developed for other conditions different from trauma, such as degenerative diseases. 6 Very good results were obtained for the reliability and validity of the original version and the subsequent translation and cross-cultural adaptations of AOSpine PROST.8-13.Our study, which achieved excellent internal consistency (Cronbach’s α = 0.96), confirms that the Spanish version is a consistent and reliable tool. Notably, the lowest item–total correlations were found for “Urinating” (0.59) and “Emotional function” (0.56), consistent with prior evidence that the PROST primarily captures physical rather than mental or autonomic function. This nuance underscores the instrument’s strength in assessing domains most relevant to spinal trauma, while acknowledging more limited sensitivity to psychosocial aspects.
The SF-36 is the most commonly used generic instrument in studies of spinal trauma patients and was, for that reason, considered the standard against which to compare the AOSpine PROST in our research, as well as in previous AOSpine PROST validation studies.7 Our analysis revealed that the AOSpine Spanish PROST correlates strongly with the Physical Functioning domain of the SF-36, yielding results comparable to those of the original Dutch version and the subsequent English version. It can therefore be considered a reliable tool for assessing functional status in patients treated for spinal trauma.8-13
In the original tool validation and subsequent cross-cultural adaptations, other domains of PROST did not achieve as good results as functional status.8-13 We have described similar results with more moderate agreement among vitality, mental health, social functioning and pain. We agree with Sadiqi et al, 8 who found that AOSpine PROST total scores reflect the patient’s experienced physical rather than mental health. In a comparative analysis with previous AOSpine PROST validation studies, we found a weaker correlation with the emotional role than with the SF-36.
The importance of AOSpine PROST, as the first disease-specific outcome measure for spinal trauma patients, is that it provides a tool to harmonise clinical assessment of spinal trauma care and research.6-8 Our results define the AOSpine Spanish PROST as a valid and reliable tool that facilitates the comparison of different treatments or the analysis of long-term outcomes such as return to work and functional activity, as shown in previous literature.
Reliability Analysis of the PROST Scale: Item-Total Correlation and Cronbach’s Alpha if Item is Deleted
Conclusion
In conclusion, the Spanish version of the AOSpine PROST proved to be a valid and reliable instrument for assessing functional outcomes in patients with spinal trauma. It demonstrated particularly strong correlations with the Physical Functioning domain of the SF-36, and moderate to strong associations with other health dimensions such as Vitality, Mental Health, and Bodily Pain. These findings support its use in both clinical practice and research settings within Spanish-speaking populations.
Supplemental Material
Supplemental Material - Transcultural Adaptation and Validation into Spanish of the AO Spine PROST (Patient-Reported Outcome Spine Trauma) Questionnaire
Supplemental Material for Transcultural Adaptation and Validation into Spanish of the AO Spine PROST (Patient-Reported Outcome Spine Trauma) Questionnaire by Ignacio Cirillo, Pablo Carreño, Guillermo Ricciardi, Ratko Yurac, Gonzalo Kido, Victor Barrientos, Hugo Vilchis, Eduardo Laos in Global Spine Journal.
Footnotes
Acknowledgments
This study was supported by the AO Spine Foundation as part of its ongoing commitment to advancing spine research and education worldwide. The authors would like to thank AO Spine for their support and for fostering international collaboration in the field of spine care.
Ethical Approval
Approval Code CEC/17/2022, Ethics Committee of Hospital del Trabajador.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: this study was supported by a research grant from AO Spine.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
