Abstract
Study Design
Retrospective database analysis study.
Objective
Coagulopathy, often defined as an International Normalized Ratio (INR) > 1.2, is associated with poor postoperative outcomes. We aimed to evaluate interactions between coagulopathy and non-elective surgery status regarding clinical outcomes among patients undergoing single-level lumbar decompression.
Methods
Data were obtained from the National Surgical Quality Improvement Program (2016-2021). Hierarchical regression models were used to evaluate associations between non-elective surgery and preoperative INR >1.2 with hospital length of stay (LOS) and home discharge. Effect modification of INR > 1.2 by non-elective surgery status and thrombocytopenia (platelet count < 150 k/mcL) was assessed. Random forest modeling simulated outcomes had coagulopathic patients presented with INR ≤ 1.2.
Results
Among 34 591 patients (median age, 60 years), 8.5% underwent non-elective surgery and 1.8% had INR > 1.2. Non-elective surgery was associated with longer LOS (β = 3.4; P < 0.001) and reduced home discharge (OR, 0.20; P < 0.001). INR > 1.2 was also associated with prolonged LOS (β = 0.97; P < 0.001) and reduced home discharge (OR, 0.65; P < 0.001). Interactions for LOS were observed between INR >1.2 and both non-elective surgery (P < 0.001) and thrombocytopenia (P = 0.001). Simulated normalization of INR among non-elective surgery patients was associated with a reduction in LOS by a median of 2.5 days (IQR, 1.4-5.4 days decrease) and increase in home discharge by 17%.
Conclusions
Non-elective surgery and preoperative INR > 1.2 were associated with prolonged LOS and lower odds of home discharge after single-level lumbar decompression. The effect of INR > 1.2 on LOS was more pronounced for non-elective cases and patients with thrombocytopenia.
Keywords
Introduction
Lumbar decompression is a common neurosurgical procedures, with the number of cases continuing to increase each year.1,2 The vast majority of patients receive these procedures on an elective basis to treat degenerative pathologies. Still, unplanned surgeries may be necessary for indications such as traumatic injury or neoplasm. 3 It is well-established that non-elective spinal surgery is associated with worse outcomes, including higher cost of care, longer hospital length of stay (LOS), and increased perioperative complications compared to elective surgery.3–5
Optimizing preoperative management for patients undergoing urgent surgery may mitigate these risks. With the use of anticoagulant medications becoming more prevalent in an aging population, obtaining appropriate hematologic control before surgery is an important aspect affecting outcomes. Achieving adequate hemostatic control is particularly important in spine surgery, where postoperative complications such as epidural hematomas can cause severe neurological deficits. 6 However, decision-making regarding the use of reversal or pro-hemostatic agents and the appropriate time to proceed to surgery is complex, as the risk of bleeding complications must be weighed against the risk of further neurological compromise caused by delaying decompression to optimize hematologic control.
Despite the clinical importance of this issue, there is limited high-quality evidence guiding the management of patients undergoing lumbar decompression while on chronic anticoagulation. This issue particularly affects non-elective surgery, where discontinuing antiplatelet or anticoagulation medications before surgery in accordance with guidelines may not always be possible. 7
This study aims to evaluate the impact of preoperative hematologic parameters on outcomes after lumbar decompression. Additionally, we examine how these factors interact with the distinction between elective and non-elective surgery status. We hypothesize that hematologic abnormalities would be associated with disproportionately worse outcomes in non-elective lumbar decompression procedures.
Methods
Study Design and Population
This was a retrospective database analysis study using the American College of Surgeons National Surgical Quality Improvement Program (NSQIP) database. We initially queried the database for all patients undergoing spinal surgery from 2016 to 2021, then narrowed the cohort to patients undergoing a primary procedure with a Current Procedural Terminology (CPT) code of 63030 or 63047. These CPT codes represent single-level laminectomy or laminotomy procedures in the lumbar spine region. We adopted the approach of filtering by CPT codes, based on a prior NSQIP study that investigated outcomes after lumbar spinal surgery. 8 Next, to reduce potential confounding from patients with severe diagnoses requiring prolonged LOS such as severe polytrauma, tumors, or infections, we also applied International Classification of Diseases 10th edition (ICD10) diagnosis codes. The included ICD10 codes were under the categories of M43 – other deforming dorsopathies (i.e., spondylolysis, spondylolisthesis), M47 – spondylosis, M48 – other spondylopathies, M51 – intervertebral disc disorders, and M54 – dorsalgia (i.e., radiculopathy, sciatica). We then excluded patients with missing data for preoperative International Normalized Ratio (INR), partial thromboplastin time (PTT), or platelet count (Plt), as well as those missing data for elective surgery status, age, discharge disposition, or American Society of Anesthesiologists Physical Status (ASA-PS) classification. The cohort selection process is outlined in the Supplemental Figure. Informed consent was not obtained due to the retrospective use of a national database.
Exposure
The primary exposure in this study was the classification of procedures as either elective or non-elective surgery. Non-elective surgery status was defined in NSQIP as a procedure not meeting either of the following criteria: the patient must be brought from their home or normal living environment on the day of surgery, and the surgery must be a non-emergent or non-urgent scheduled procedure. The secondary exposures in this study were preoperative hematologic abnormalities, defined as INR > 1.2, PTT > 35 s, or Plt < 150 k/mcL.9,10 These preoperative values were obtained from the laboratory tests drawn closest to the time of procedure initiation. Each exposure was considered simultaneously within the statistical models.
Of note, we selected INR > 1.2 as a sensitivity-oriented cutoff based on prior large surgical cohorts from NSQIP showing that postoperative adverse outcome risk is possible with INR values close to the normal laboratory value (i.e., 1.1) and on laboratory references that place 1.2 near the upper bound of normal.10,11 Cervical spine surgery literature has also identified higher complication rates with INR values between 1.25 and 1.5 in a NSQIP cohort, supporting our approach of using a lower cutoff. 12 However, as described below, we did perform sensitivity analyses to validate our primary finding at different INR cutoff values.
Outcomes
The primary outcome in this study was hospital LOS, defined as the number of days between hospital admission and discharge. The secondary outcome in this study was discharge disposition to home vs any non-home facility (i.e., skilled or unskilled nursing facilities, acute care, rehab, senior community, hospice, or inpatient mortality).
Potential Confounders
Efforts were made to control for potential confounders in the relationship between elective surgery status, hematologic abnormalities, and the outcomes of interest. We first controlled for patient baseline factors, including age, sex or gender identity, race, and body mass index (BMI). We then accounted for clinical factors such as having an ASA-PS classification of III, IV, or V, since these have been associated with poorer postoperative outcomes and greater rates of complications. 13 ASA-PS was also used in our models to control for differences in patient comorbidity burden that may affect outcomes. Finally, the presence of a comorbid bleeding disorder and the need for a red blood cell (RBC) or whole blood transfusion within 72 h before surgery were also considered clinical factors acting as potential confounders. 14
Statistical Analysis
Univariable analyses were performed to compare groups of elective vs non-elective surgery patients. Then, we constructed a hierarchical linear and logistic regression for associations with hospital LOS and home discharge, respectively. These models were adjusted for the potential confounders above and included a random effects term to account for clustering by procedure type. To investigate whether an abnormal INR has different effects on outcomes for elective vs non-elective surgery patients, we tested for interaction between elective surgery status and an INR > 1.2 in each model. We also separately tested for interaction between abnormal INR and abnormal Plt for each outcome. When the interaction terms were significant, we performed stratification and evaluated effects at each factor level. These interaction tests were conducted to explore whether the impact of coagulopathy on outcomes varied across clinically distinct subgroups, which could inform more tailored perioperative management strategies. Where the interaction between INR > 1.2 and non-elective surgery status was significant, we performed sensitivity analyses by repeating the interaction test with coagulopathy defined as INR > 1.5, which is a common surgical cutoff,12,15 as well as INR as a continuous variable.
Then, we sought to understand the relative importance of INR, Plt, and other factors in influencing the outcomes of interest. For elective surgery patients, random forest models were specified to predict each outcome using the covariates from earlier models. Both models were trained on 80% of the data and tested on the remaining 20%, using 500 trees and sampling 3 predictors at each split. For LOS, model performance was assessed using R2, and for home discharge, it was assessed using the area under the receiver operating characteristic curve. Feature importance was evaluated using the percent increase in mean squared error for LOS and mean decrease in accuracy for home discharge. These values were plotted for visualization. Finally, to assess the importance of INR on outcomes, we identified a subgroup of patients with an INR > 1.2. We artificially specified these patients to present with an INR ≤ 1.2 and used the random forest models to simulate outcomes. These simulated outcomes were compared to the original outcomes. Finally, we repeated the model generation, feature importance, and outcome prediction process for patients undergoing non-elective surgery and characterized differences between elective and non-elective surgery results.
The Kruskal-Wallis test was used for univariable comparisons of continuous variables, and the Chi-squared test was used for comparisons of categorical variables. All P-values were deemed significant if less than 0.05, and all statistical analysis was performed in R (version 4.2.2).
Results
Study Population
Our study included 34 591 patients undergoing single-level lumbar decompression procedures. The median age was 60 years (IQR, 46-70 years), and the cohort was predominantly male (N = 19 583, 57%). Few patients presented with INR > 1.2 (N = 628, 1.8%), PTT > 35 s (N = 2,126, 6.1%), or Plt < 150 k/mcL (N = 1,648, 4.8%) on preoperative labs. The median hospital LOS was 1 day (IQR, 0-2 days), and most patients achieved home discharge (N = 31 810, 92%).
Characteristics of Patients Undergoing Lumbar Decompression Surgery, Stratified by Elective Versus Non-elective Surgery
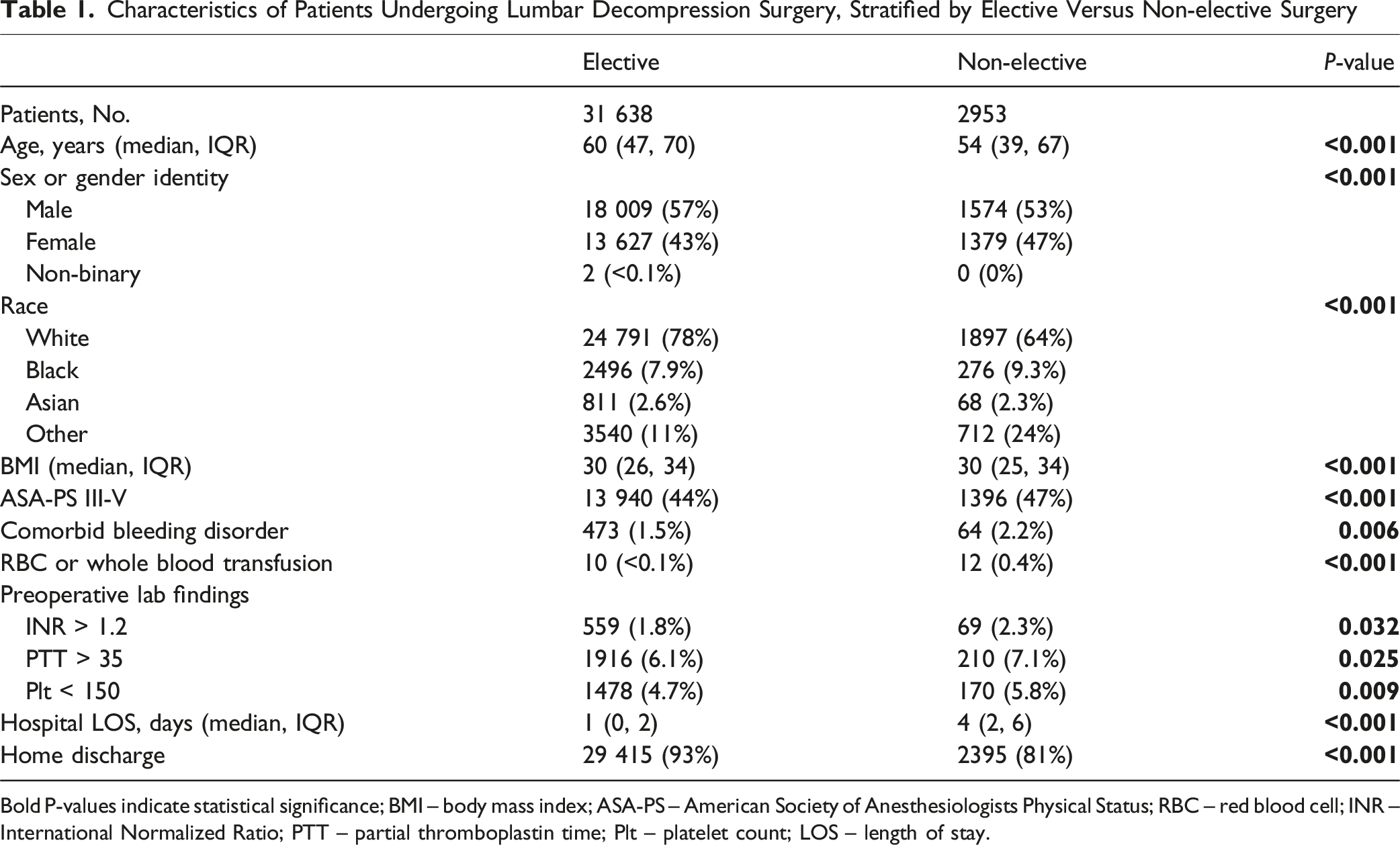
Bold P-values indicate statistical significance; BMI – body mass index; ASA-PS – American Society of Anesthesiologists Physical Status; RBC – red blood cell; INR – International Normalized Ratio; PTT – partial thromboplastin time; Plt – platelet count; LOS – length of stay.
Associations with Length of Stay
Hierarchical Linear Regression for Associations With Hospital Length of Stay (in Days)
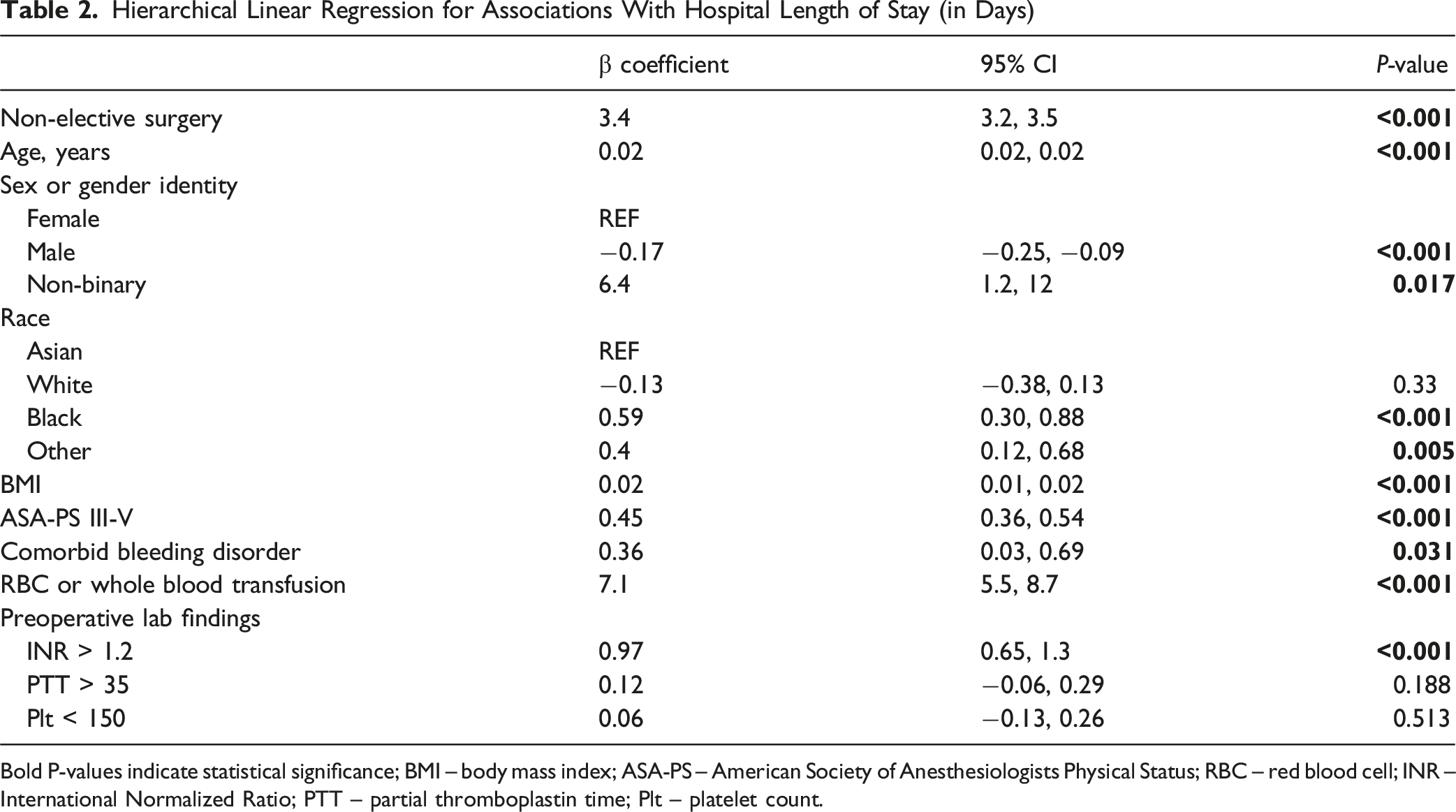
Bold P-values indicate statistical significance; BMI – body mass index; ASA-PS – American Society of Anesthesiologists Physical Status; RBC – red blood cell; INR – International Normalized Ratio; PTT – partial thromboplastin time; Plt – platelet count.
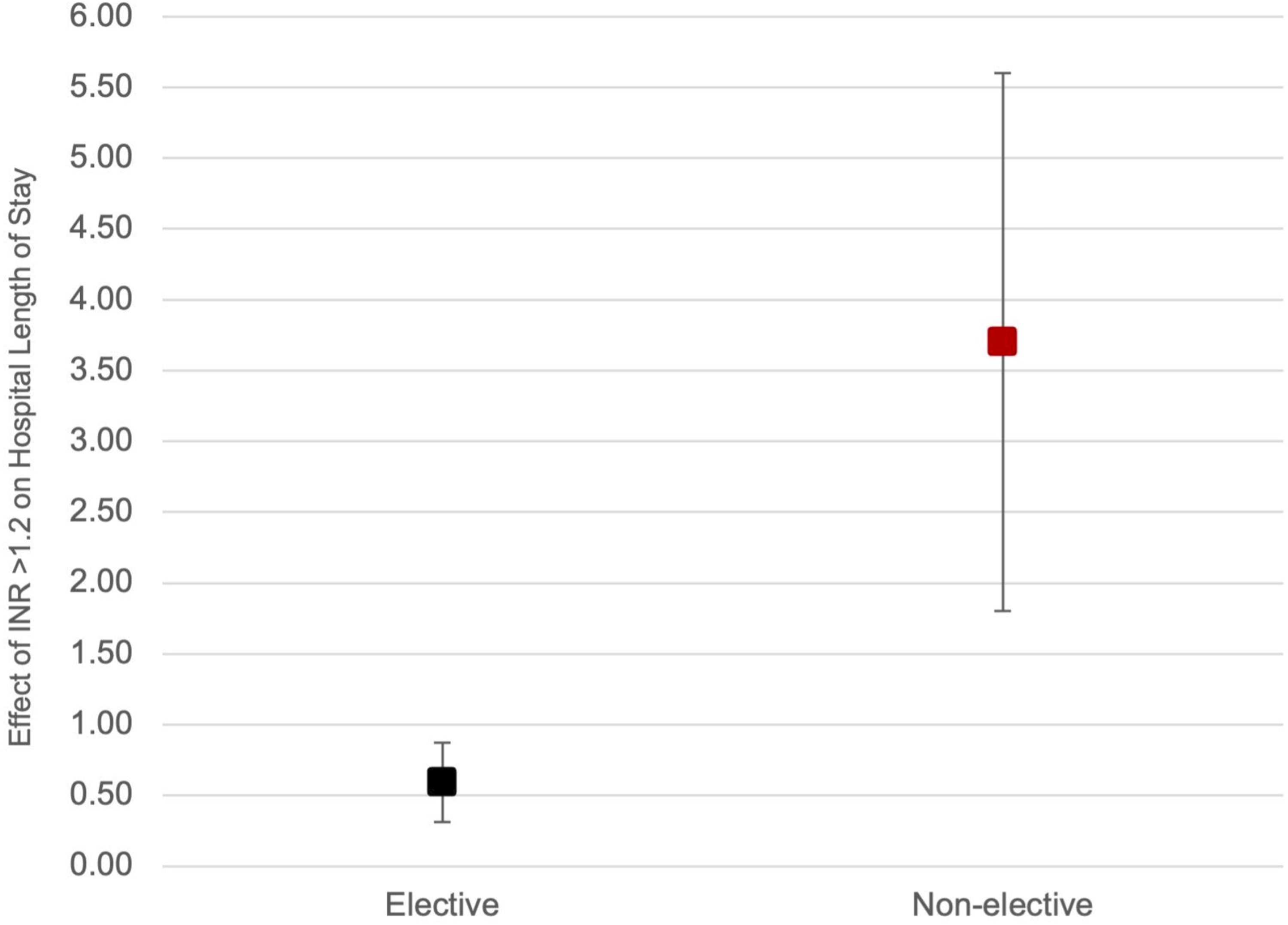
Effect of International Normalized Ratio on Hospital Length of Stay, Stratified by Elective Surgery Status. INR – International Normalized Ratio
As the interaction between INR >1.2 and non-elective surgery status was significant, we repeated this interaction test in the same model after redefining coagulopathy as INR >1.5, and again with INR as a continuous variable. Both interaction terms were significant (both P < 0.001).
Associations with Home Discharge
Hierarchical Logistic Regression for Associations With Home Discharge
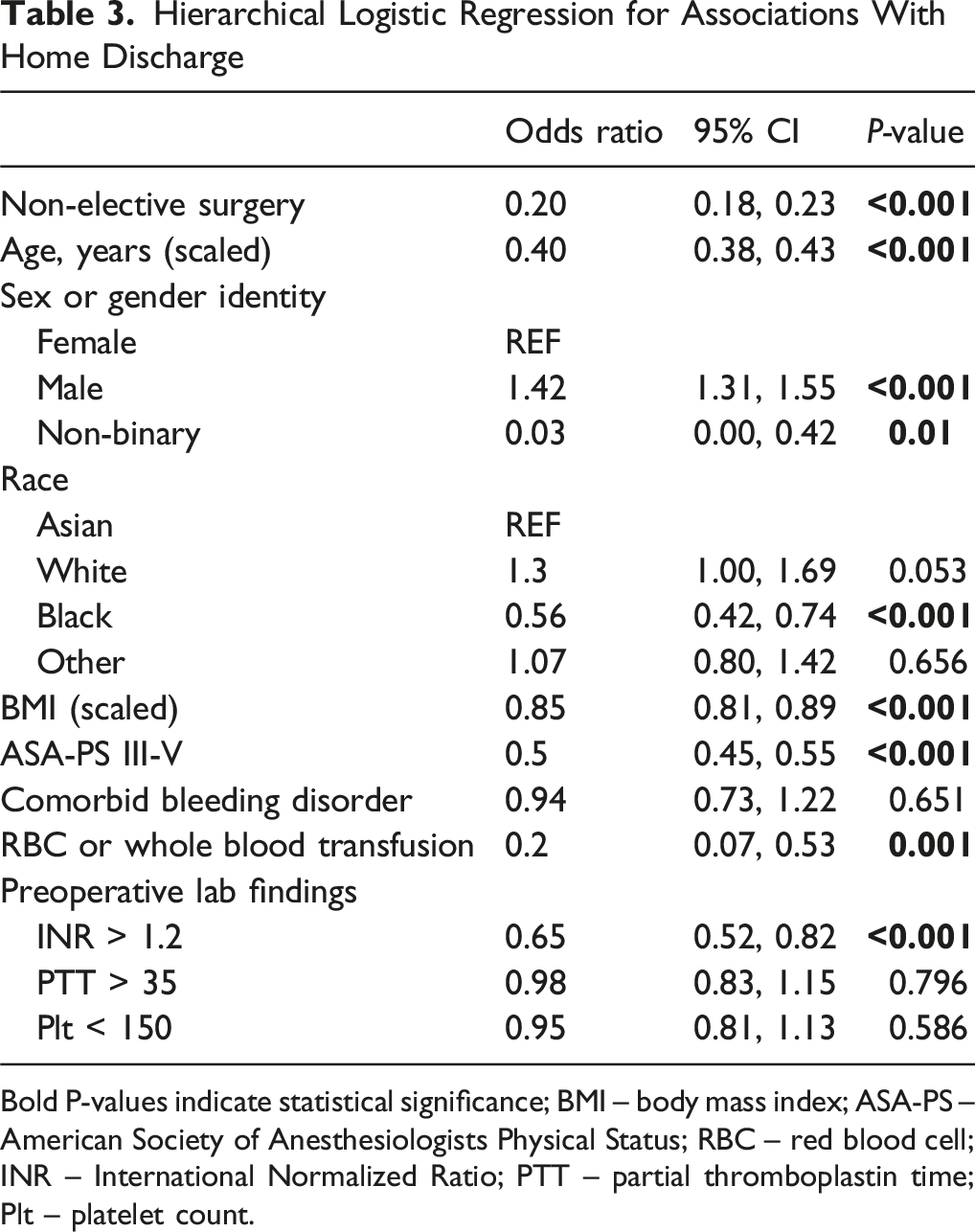
Bold P-values indicate statistical significance; BMI – body mass index; ASA-PS – American Society of Anesthesiologists Physical Status; RBC – red blood cell; INR – International Normalized Ratio; PTT – partial thromboplastin time; Plt – platelet count.
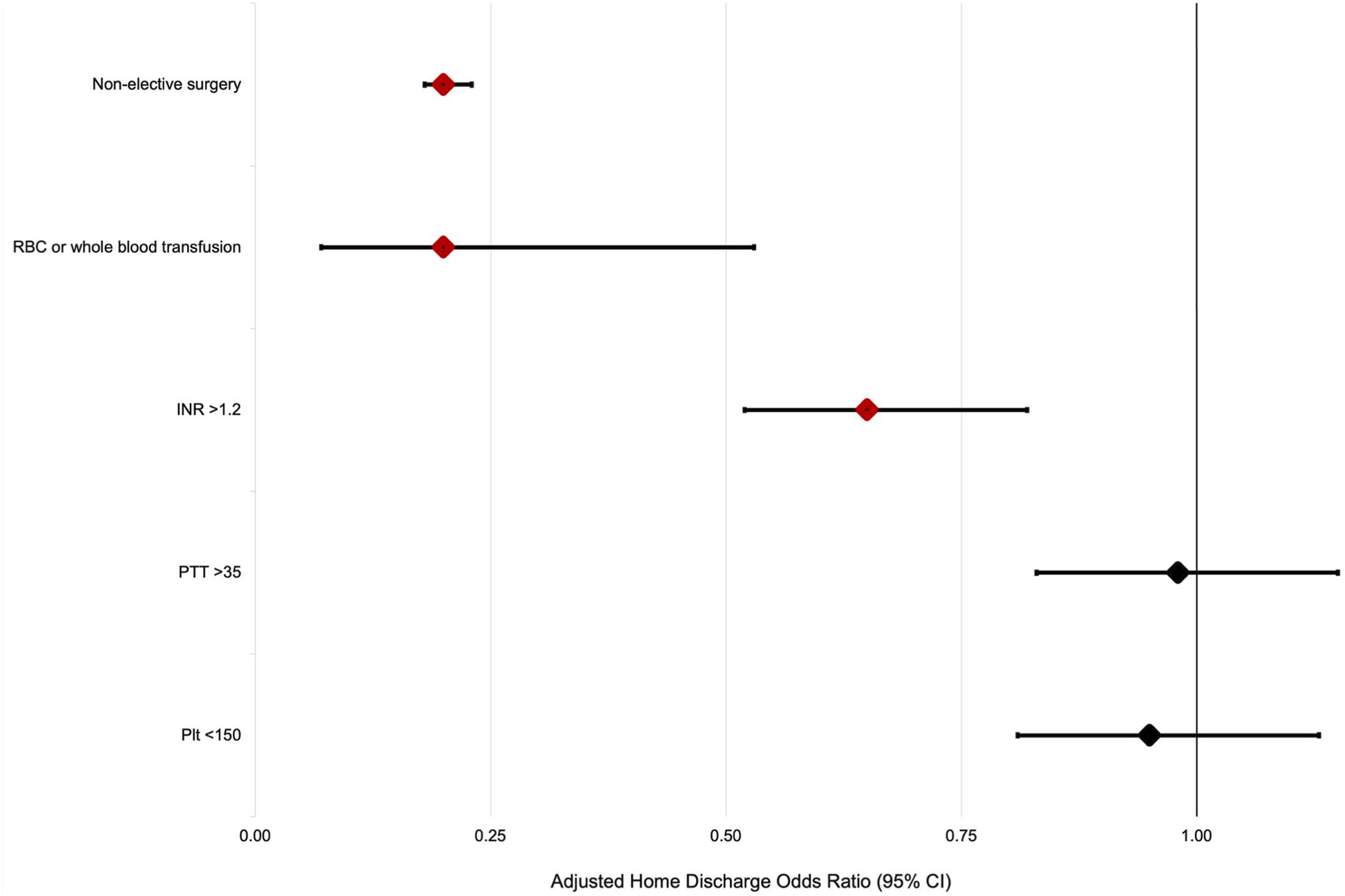
Selected Odds Ratios From Hierarchical Logistic Regression for Associations With Home Discharge. RBC – Red Blood Cell; INR – International Normalized Ratio; PTT – Partial Thromboplastin Time; Plt – Platelet Count
Feature Importance
Supplemental Tables 1-2 contain important metrics for both hospital LOS and home discharge. For hospital LOS among patients undergoing non-elective surgery, the most important predictive factors in order were age, race, comorbid bleeding disorder, and INR > 1.2 (Figure 3). This is in contrast to patients undergoing elective surgery, as the strongest predictors in this group were age, ASA-PS of III-V, RBC or whole blood transfusion, and race. INR >1.2 had a comparatively low impact in this group. Feature Importance for Random Forest Model Predicting Hospital Length of Stay, Stratified by Elective Surgery Status. INR – International Normalized Ratio; BMI – Body Mass Index; PTT – Partial Thromboplastin Time; ASA-PS – American Society of Anesthesiologists Physical Status; RBC – Red Blood Cell; Plt – Platelet Count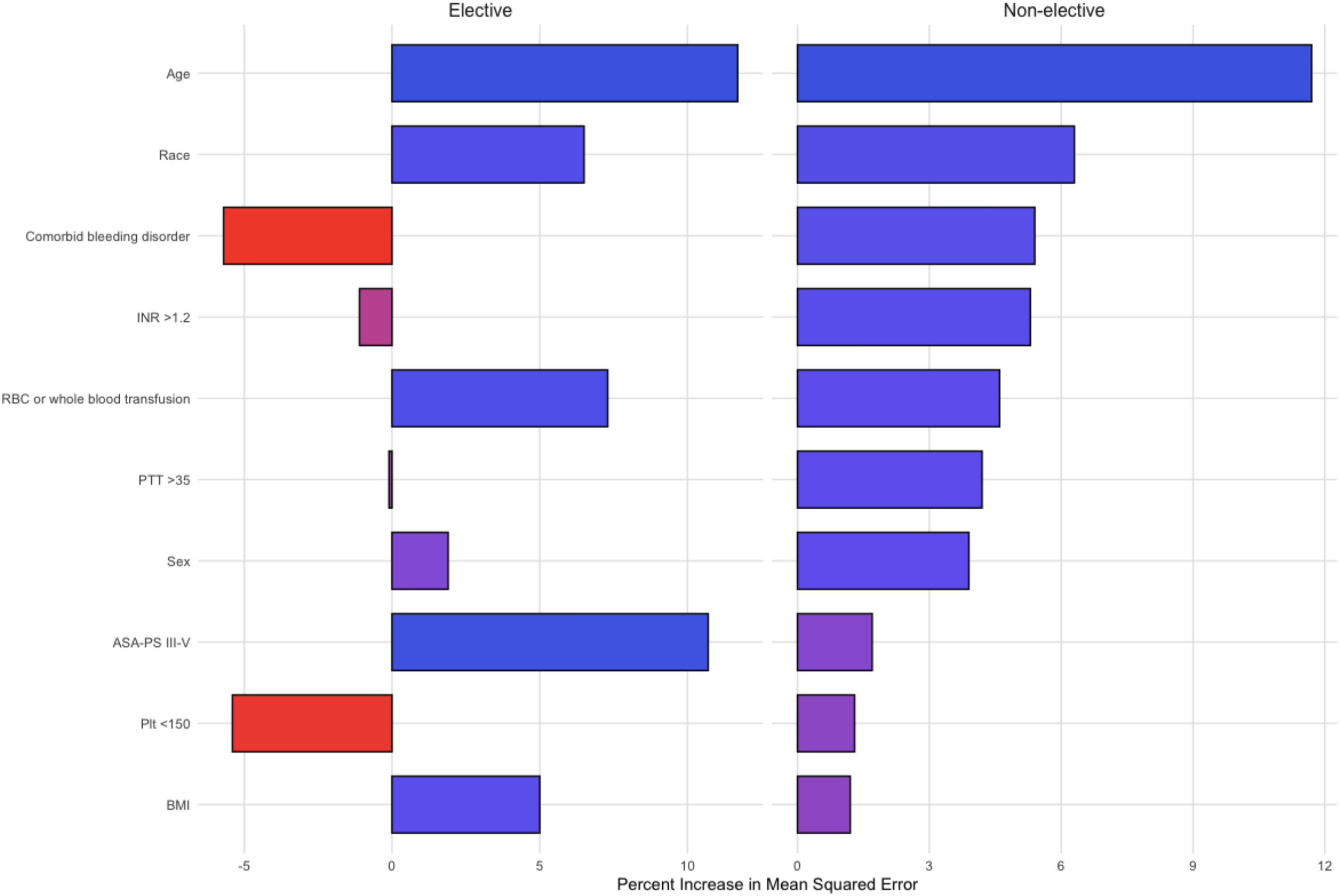
Predictors of hospital discharge to home among non-elective surgery patients were age, ASA-PS III-V, and INR > 1.2 (Figure 4). Age was also the strongest predictor for elective surgery patients, but race and BMI were more significant than an INR > 1.2. Feature Importance for Random Forest Model Predicting Home Discharge, Stratified by Elective Surgery Status. Plt – Platelet Count; ASA-PS – American Society of Anesthesiologists Physical Status; PTT – Partial Thromboplastin Time; INR – International Normalized Ratio; BMI – Body Mass Index; RBC – Red Blood Cell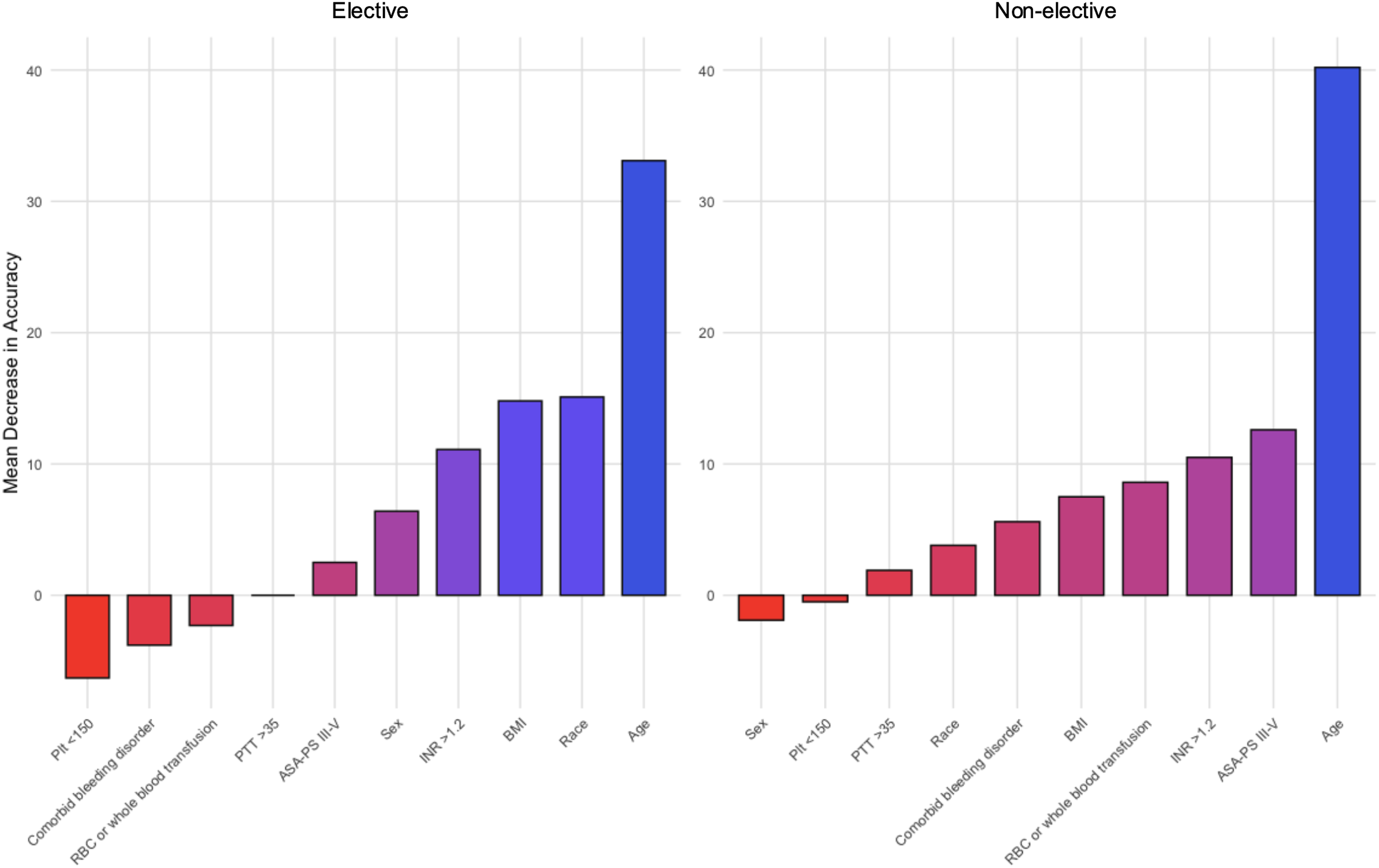
Simulated Outcomes
Changes in Hospital Length of Stay and Home Discharge Disposition After Modeling a Change in INR From >1.2 to ≤1.2 for All Patients With Preoperative INR >1.2
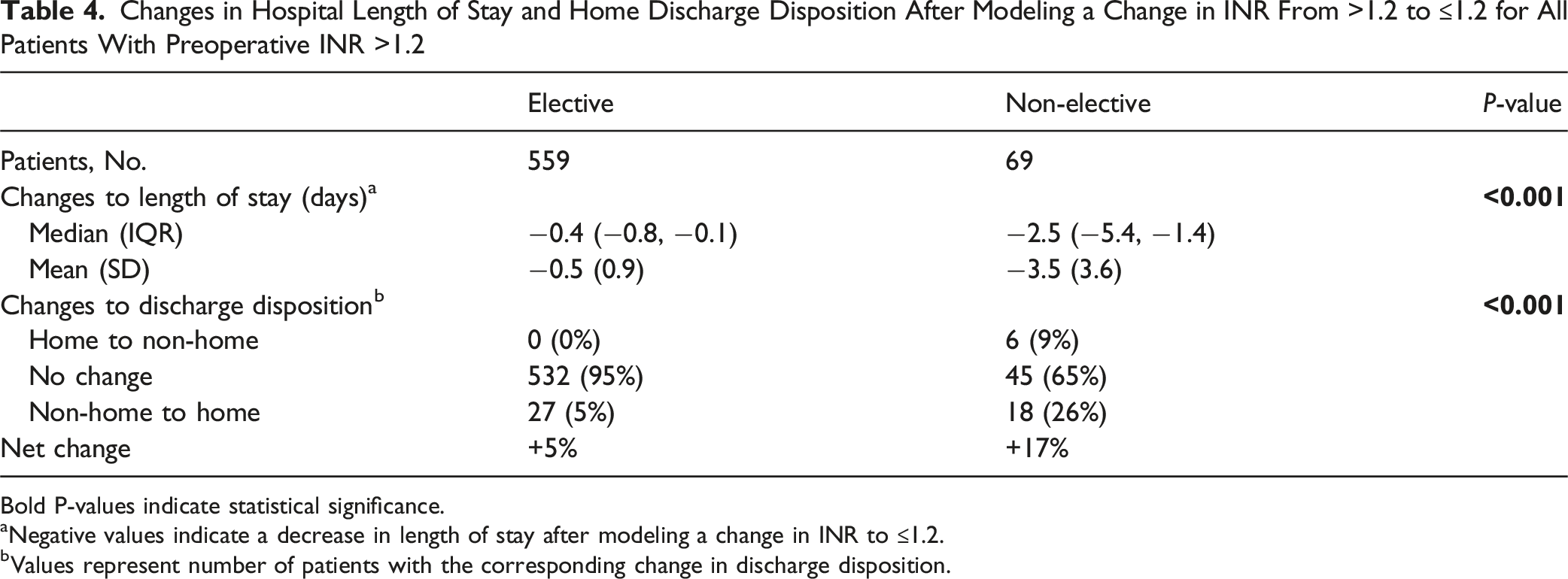
Bold P-values indicate statistical significance.
aNegative values indicate a decrease in length of stay after modeling a change in INR to ≤1.2.
bValues represent number of patients with the corresponding change in discharge disposition.
Discharge outcomes were also simulated after a change in INR to ≤ 1.2. Among non-elective surgery patients, 9% experienced an adverse transition from home discharge to non-home discharge. In comparison, 26% experienced a beneficial transition from non-home to home discharge, and the remaining 65% experienced no change. Among patients undergoing elective spinal surgery, 5% experienced a beneficial change in discharge disposition while the remaining 95% experienced no change.
Discussion
Optimizing perioperative coagulation status in patients who undergo single-level lumbar spine decompression may help in supporting postoperative recovery and avoiding adverse events. However, management of coagulation status in these patients remains inconsistent, in part due to the lack of standardized guidelines and high-quality evidence to define target values for coagulation tests and platelet counts. 15 Moreover, there has been limited study of how preoperative coagulation status may differentially impact postoperative outcomes in elective vs non-elective spine surgery. In our investigation, we found that elevated INR is associated with increased length of hospital stay among patients undergoing single-level lumbar spine decompression, with a greater effect among non-elective cases.
Within our total study population of patients who underwent either elective or non-elective single-level lumbar spine decompression, preoperative INR > 1.2 was independently associated with increased LOS and lower odds of home discharge. This finding supports previous research indicating that the use of anticoagulant (AC) or antiplatelet (AP) therapies is linked to prolonged hospitalization in patients undergoing single-level lumbar spine surgery. 16 For elective spine surgery patients, a recent Delphi study achieved consensus recommendations for stopping AC/AP medications at specific preoperative time points (2 days before surgery for direct oral anticoagulants, 5 days for warfarin, and 7 days for other AC/AP medications). 17 Notably, prior NSQIP studies have found that patients who underwent elective anterior cervical spine surgery with a preoperative INR > 1.25 were at higher risk of adverse postoperative outcomes, including postoperative hematoma or 30-day readmission or reoperation. However, this was not observed among patients who underwent elective cervical spine surgery via a posterior approach. 18 Therefore, target perioperative INR may vary depending on the specific spine level and surgical approach.
Importantly, patients may present with multiple types of coagulopathies, including abnormalities in the clotting cascade, factor abnormalities, and thrombocytopenia. For neurosurgical patients, a preoperative platelet count of at least 100 k/mcL is commonly targeted, as platelet counts below this threshold have been associated with adverse outcomes, such as hemorrhagic complications.19,20 We elected to use a higher platelet count cutoff at 150 k/mcL to reduce the number of false negative cases of thrombocytopenia included in our analyses. Our study found a significant interaction between INR > 1.2 and thrombocytopenia, which suggests that patients with both types of coagulation abnormalities are more susceptible to longer hospital stays. The etiology of how coagulation abnormalities prolong hospitalization is not fully understood. However, it is possible that these patients have underlying comorbid conditions, such as kidney or liver dysfunction, which complicate postoperative recovery. For patients who present with multiple types of coagulopathies, stricter adherence to target INR values and platelet counts, as well as administration of necessary reversal agents, may be associated with improved outcomes.
The urgency of spine surgery may influence the association between preoperative coagulopathy and postoperative recovery. For patients requiring urgent spinal cord decompression, achieving a safe coagulation status before surgery may necessitate rapid administration of anticoagulation reversal agents or platelet transfusions. Our study found that elevated INR was associated with longer hospital LOS for non-elective surgery patients compared to elective surgery patients. This finding remained significant regardless of defining elevated INR as >1.2 or >1.5, as well as when it was considered as a continuous variable. Moreover, in the subgroup of non-elective patients, elevated INR was a strong predictive feature of hospital LOS, while it had far less of an impact on LOS among patients undergoing elective surgery. These findings indicate that among patients requiring urgent spine surgery, those with a suboptimal preoperative coagulation status represent a particularly vulnerable subgroup who require careful monitoring of hemodynamic status during the perioperative period and may require prolonged postoperative recovery.
Delineating the relationship between preoperative coagulopathy and postoperative outcomes in lumbar spine surgery is challenging, given the limited ability to perform prospective studies due to the need for clinical equipoise. To further interrogate the results from our multivariate regression models, our investigation used random forest models to simulate outcomes based on an INR threshold of 1.2. The results demonstrated that patients with simulated INR ≤ 1.2 were estimated to experience significantly shorter hospital stay and higher likelihood of home discharge. Therefore, future research should investigate whether administering reversal agents to achieve an INR ≤ 1.2 before surgery may support postoperative recovery. Early reversal of anticoagulation therapy has been previously recommended for patients with acute spinal pathology who require emergency surgery.21,22 Our investigation findings corroborate prior studies, which emphasize the importance of anticoagulation reversal in non-elective spine surgery.
Limitations
The retrospective study design limits our ability to determine a causal relationship between exposures and observed outcomes. Our study is also limited by available data within the NSQIP, which does not include information on when reversal agents or platelet transfusions were administered, nor long-term recovery of neurologic function. Future studies are needed to understand if delaying surgery to optimize coagulopathy benefits patients without significantly impacting neurologic outcomes. Moreover, as we only have access to preoperative INR values, we are not able to account for potential decreases in INR with the administration of reversal agents or with natural normalization. To that point, we were unable to determine exactly when lab values were obtained prior to the procedure and did not have data on whether patients were taking antithrombotic medications. We also could not ascertain the presence or severity of chronic liver disease or cirrhosis, which can elevate INR independent of anticoagulation and thus may confound associations between observed coagulopathy and outcomes. Additionally, data submission to NSQIP is at the discretion of participating trauma centers, so there exists the potential for selection bias. Selection bias may also exist in our choice to include only patients undergoing single-level lumbar spine procedures, which were chosen due to data availability. Our findings may therefore not be generalizable to other spine surgery types, and further studies are warranted to investigate potential differences. Finally, our random forest simulations assumed normalization of INR in isolation and did not account for correlated comorbidities such as diabetes, hypertension, or anticoagulant use. These exploratory analyses should therefore be interpreted cautiously as hypothesis-generating rather than causal proof. Despite these limitations, our study provides valuable insights into the associations between preoperative coagulopathy and postoperative outcomes, which may guide future investigations in this area.
Conclusion
Coagulopathy, defined as a preoperative INR > 1.2, is associated with prolonged LOS and reduced odds of home discharge for patients undergoing single-level lumbar decompression surgery. The detrimental effect of coagulopathy on LOS is amplified for patients undergoing non-elective surgery and for those who were thrombocytopenic. This evidence suggests that achieving a preoperative target INR ≤ 1.2 may be beneficial for reducing adverse outcomes after lumbar decompression surgery, especially in the case of non-elective operations.
Supplemental Material
Supplemental Material - Interaction of Preoperative Coagulopathy and Non-Elective Status in Association With Length of Stay for Patients Undergoing Lumbar Spinal Decompression Surgery
Supplemental Material for Interaction of Preoperative Coagulopathy and Non-Elective Status in Association With Length of Stay for Patients Undergoing Lumbar Spinal Decompression Surgery by Vikas N. Vattipally, BS, Kathleen R. Ran, AB, Kelly Jiang, MS, Patrick Kramer, BS, Carly Weber-Levine, MD, MS, Jacob Jo, MD, Liam P. Hughes, MD, Jawad M. Khalifeh, MD, Daniel Lubelski, MD, Ali Bydon, MD, Timothy F. Witham, MD1, Tej D. Azad, MD, MS, Nicholas Theodore, MD, MS in Global Spine Journal
Footnotes
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Disclosures
Nicholas Theodore receives royalties, holds stock ownership, has consulted for, and has served on the scientific advisory board/other office for Globus Medical.
IRB Approval
This study was approved by the Johns Hopkins University Institutional Review Board (IRB00265490).
Supplemental Material
Supplemental material for this article is available online.
