Abstract
Study Design
Narrative Review.
Objectives
We aim to investigate the integration and impact of enabling technologies, such as augmented reality, virtual reality, mixed reality, navigation, robotics, and artificial intelligence within the domain of spinal surgery.
Methods
We made a literature review for articles that examined the progression of adoption from initial to subsequent adopters. We also analysed the key determinants that influence adopting these technologies into clinical settings. These include cost-effectiveness, ease of integration, patient acceptance, learning curves, and availability of training resources. Based on the available data a suggestion has been made on the adoption framework for clinical utility.
Results
These technological advancements have the potential to transform surgical practice, offering improved precision and efficiency. The journey toward widespread adoption presents challenges, which include the financial implications, the necessity for specialized training, and the complexities associated with integration. To navigate these hurdles, the study proposes recommendations aimed at improving cost efficiency, streamlining technology integration, investing in professional development, and nurturing a culture of innovation and research.
Conclusions
A framework has been established for the evaluation and integration of state-of-the-art technologies in spinal surgery, thereby maximizing their potential impact on surgical outcomes and patient welfare.
Keywords
Introduction
The integration of advanced technologies into spine surgery has heralded a transformative shift in medical practices, significantly enhancing surgical precision, safety, and patient outcomes. 1 This evolution marks a pivotal moment in the pursuit of minimally invasive and patient-centred surgical interventions, driven by rapid advancements in navigation, robotics, augmented reality (AR), virtual reality (VR), and mixed reality (MR) technologies. 2 As we are on the verge of this potential technological revolution, it becomes imperative to critically evaluate the impact of these innovations on spine surgery practices and patient care.
The advent of navigation, robotics, AR, VR, and MR technologies in spine surgery introduces a new paradigm of surgical precision and efficiency. 3 These technologies require surgical teams to re-evaluate their surgical workflow, from preoperative planning through intraoperative guidance to postoperative assessment. 4 AR technology, for example, has been instrumental in improving the accuracy of pedicle screw placement,5,6 while VR has created immersive training environments, enabling surgeons to refine their skills in a risk-free setting.7,8 MR combines virtual and real-world elements to provide a holistic surgical experience in which the surgeon can interact with the environment. 9 Despite these advancements, integrating such technologies into clinical practice is met with varied challenges and considerations, including cost, institutional readiness, and surgeon and patient acceptance.
While the literature highlights the benefits and learning curves associated with technological advancements, there remains a critical gap in understanding the comprehensive impact of these technologies in improving patient outcomes.2,10 The adoption cycle of these innovations, from the early to the late adopters, and the specific technological advancements that have marked this transition are areas that require further exploration. Rapid and wide adoption of these advancements is often stymied by high capital costs associated with spine-related technologies and knowledge gaps that still exist amongst multi-disciplinary healthcare professionals on their effective utilization.10,11 These challenges underscore the necessity for a comprehensive review. This paper aims to describe a framework in which various healthcare stakeholders can reproducibly evaluate various innovative technologies in spine surgery. Not only will this aid a more uniform approach to enabling technology evaluations, but it also addresses the knowledge gaps and lays the groundwork for future research in this rapidly evolving field.
Adoption Cycle
The adoption cycle of technology in spine surgery represents a pivotal framework for understanding the integration of new innovations into clinical practice. This iterative process is distinguished by various stages, each characterized by the distinct profiles, motivations, and behaviours of different groups of adopters, ranging from the initial embracement by early adopters to the widespread acceptance among later adopters, spanning the spectrum from the enthusiast to the cynic. These distinctions are crucial for navigating the pathway through which technological advancements transition from novel concepts to integral components of standard care in spine surgery. Both early and later adopters can make significant contributions to the establishment of emerging technologies.
Early Adopters
Early adopters in spine surgery are typically distinguished by their enthusiasm for innovation, readiness to engage with new technologies, and ability to foresee the potential benefits of these advancements for patient outcomes and surgical efficiencies. These individuals or entities are often at the forefront of adopting pioneering technologies such as AR, robotics, and artificial intelligence (AI) within surgical practices.2,10 Their adoption is motivated by a strong belief in the transformative potential of technology, a dedication to pushing the boundaries of spine surgery, and enabled by a permissive financial healthcare ecosystem.
The significance of early adopters extends beyond the initial usage of new technologies. They play a crucial role in the ongoing refinement, validation, and optimization of these innovations and applications in real-world scenarios.5,12,13 Through comprehensive testing, constructive feedback, and dedicated clinical application, early adopters aid in the evolutionary development of technological solutions, enhancing their adaptability, effectiveness, and safety for broader application. Despite facing numerous challenges such as increased costs, the necessity for specialized training, and the complexities of navigating regulatory environments, the contributions of early adopters are indispensable. They lay the groundwork for subsequent phases of adoption, gradually identifying barriers and improving on the early versions for subsequent wider adoption.
Later Adopters
Later adopters join the technology adoption cycle armed with insights and evidence accumulated from the pioneering experiences of early adopters. This group typically exhibits a more conservative approach, prioritizing solid evidence of clinical efficacy, cost-benefit analyses, and the practicality of technology integration into existing workflows before committing to new technologies. Móga et al, 14 and Marwaha et al, 15 illustrate the transition phase, wherein later adopters progressively embrace technology, encouraged by its demonstrated advantages and overcoming initial reservations.
For later adopters, factors including empirical evidence of improved patient outcomes, endorsements from peers, and the availability of comprehensive training programs are pivotal in influencing their adoption decisions. This group plays a fundamental role in the standardization of new technologies in spine surgery, facilitating the accessibility and adoption of innovations across a wider spectrum of the medical community. The evolution from early to later stages of adoption is crucial for reaching a critical mass, ultimately establishing the technology as a new standard of care in the field.
Challenges and Considerations for Adoption
Both early and later adopters encounter distinct challenges throughout the technology adoption cycle. Early adopters must navigate the uncertainties and risks associated with introducing untested technologies, while later adopters face the intricacies of assimilating these innovations into established practices and systems. Scholarly discussions address these challenges, underscoring the necessity for a conducive ecosystem that supports the adoption journey. 11 This ecosystem should provide clear regulatory guidelines, comprehensive training, education opportunities, and financial incentives, all of which are critical to allow for a wider adoption and transition of these new technologies from experimental use to mainstream clinical practice.
The adoption cycle of technology in spine surgery is a dynamic, ongoing process that mirrors the continual evolution of technology and its integration into the medical field. As the cycle advances, the collective experiences and insights of both early and later adopters enrich the pool of knowledge, fostering further innovation, refinement, and adoption. This cyclical process ensures the sustained advancement of spine surgery, leveraging cutting-edge technological innovations to enhance patient care, improve surgical outcomes, and redefine the standards of medical practice in the field.7,9
Digitalization of Surgery
The digitization of surgical procedures, particularly within spine surgery, heralds a significant move towards a healthcare system that is more efficient, precise, and patient-centric. The introduction of digital technologies and AI into the operating room marks the beginning of an era characterized by transformation. 15 There is a potential impact that machine learning models have on the processes of clinical prediction and decision-making, emphasizing the accuracy and potential these technologies possess in enhancing patient outcomes. The incorporation of digital instruments into surgical practices not only simplifies the workflow of procedures but also amplifies the surgeon’s capability in planning, performing, and evaluating surgical interventions with an unprecedented level of detail and understanding. 15 Moreover, the role of digitalization extends past the procedural elements of surgery to encompass aspects of patient engagement and care following the operation. 16 Digital platforms serve as a bridge, improving the line of communication between patients and healthcare providers, which facilitates both superior pre-operative preparations and post-operative care. This comprehensive approach to patient care, bolstered by digital advancements, plays a crucial role in elevating patient satisfaction levels and achieving superior clinical outcomes. 15
The practical benefits of integrating advanced technological solutions into clinical settings demonstrate the concrete advantages of employing state-of-the-art technologies in clinical practices.4,10 For example, the introduction of novel surgical technologies offers enhanced precision in complex procedures like deformity correction, where the meticulous placement of surgical implants is paramount for the patient’s recovery and the overall success of the surgery. 17 The positive changes in patient outcomes and procedural efficiencies that accompany the advent of digital innovations surgery is fraught with challenges and spine surgery is no exception to it.4,10 Issues such as the increased costs associated utilizing cutting-edge technologies and the lack of comprehensive knowledge among healthcare professionals are significant obstacles to the universal adoption of these innovations. These concerns highlight the need for a deep understanding and strategic planning to ensure the widespread accessibility and utilization of the benefits offered by digitalization in the surgical domain.11,15
The literature review by Marwaha et al, 15 explores the promising future of spine surgery through the lens of digital technology and AI, offering insights into a future where surgical procedures are enhanced by predictive analytics, virtual reality simulations, and robotic assistance. This forward-looking perspective not only foresees a surgical landscape characterized by heightened precision and safety for patients but also opens the door to innovative treatment options and recovery methodologies, heralding a new era of surgical excellence and patient care. 15
Technological Advancements in Spine Surgery
The technological landscape of spine surgery has undergone a remarkable transformation, driven by the advent and integration of numerous technological advancements. These innovations, encompassing a diverse range of applications from enhanced imaging and precise navigation systems to the incorporation of robotics and AI, have collectively reshaped the paradigms of spinal treatment. The assimilation of these cutting-edge technologies into the realm of clinical practice signifies a monumental stride towards improving surgical accuracy, elevating patient safety, avoiding complications, and optimizing outcomes in the treatment of spinal disorders.
Imaging and Navigation Systems
Given the intricate three-dimensional anatomy of the spine and the delicate neurovascular structures involved, these innovations have enhanced both safety and efficiency during spine surgeries. A notable advancement has been the widespread adoption of Computer Assisted Navigation (CAN), commonly referred to as navigation, aimed at maximizing efficiency and minimizing complications related to surgical trauma. The evolution of imaging and navigation systems has been considered a significant milestone in the field of spine surgery, offering tools that have substantially improved preoperative planning and intraoperative guidance. Ranging from technologies such as Image-Guided Navigation (IGN) systems with 2-D/3D navigation capabilities to Augmented Reality Head-Mounted Displays (AR-HMDs), new standards are being set towards surgical precision. 14
Novel Intraoperative 3D imaging tools directly connected to the navigation systems have gained improved imaging quality and portability thus improving the overall workflow of the surgery and accuracy during navigation. 18 These systems enable improved placement of pedicle screws and other spinal implants with greater accuracy, thereby reducing the likelihood of complications and re-operations.19,20 By facilitating real-time visualization of anatomical structures during procedures, these technologies have played a pivotal role in improving surgical procedures, reducing the incidence of revision surgeries, and shortening hospital stays as visualization can be achieved through smaller working windows.21,22
Robotic-Assisted Surgery
Robotic-assisted surgery represents another milestone of innovation in spine surgery. 10 This technology provides surgeons with heightened precision and control, aiding in the accurate placement of spinal implants using rigid navigation arms. The use of robotics in spine surgery can overcome some human physiological limitations and allow surgery to be performed in a less invasive approach, thereby contributing to a reduction in blood loss, post-operative pain, post-operative infections, and patients’ recovery period.23,24 Integrating robotic systems into spinal procedures may allow for more consistent and predictable surgical outcomes from an instrumentation perspective. 25
Artificial Intelligence and Machine Learning
The incorporation of AI and ML into spine surgery is revolutionizing the landscape of clinical decision-making and patient management. 15 AI and ML models are capable of analysing extensive datasets to forecast clinical outcomes, refine surgical planning, and pre-emptively identify potential complications. Such AI models aid in the data-driven patient clustering based on their risk factors to predict the outcomes with surgical management. 26 These advanced technologies augment the surgeon’s decision-making process, enabling a more personalized surgical approach and enhancing the efficiency and effectiveness of surgical procedures.27,28 The AR and VR technologies provide surgeons with immersive visualizations of patient anatomy, allowing for enhanced preoperative planning and intraoperative navigation. These technologies improve surgical precision and may also aid in medical education and training. 29
Summary of Enabling Technologies in Spine Surgery.
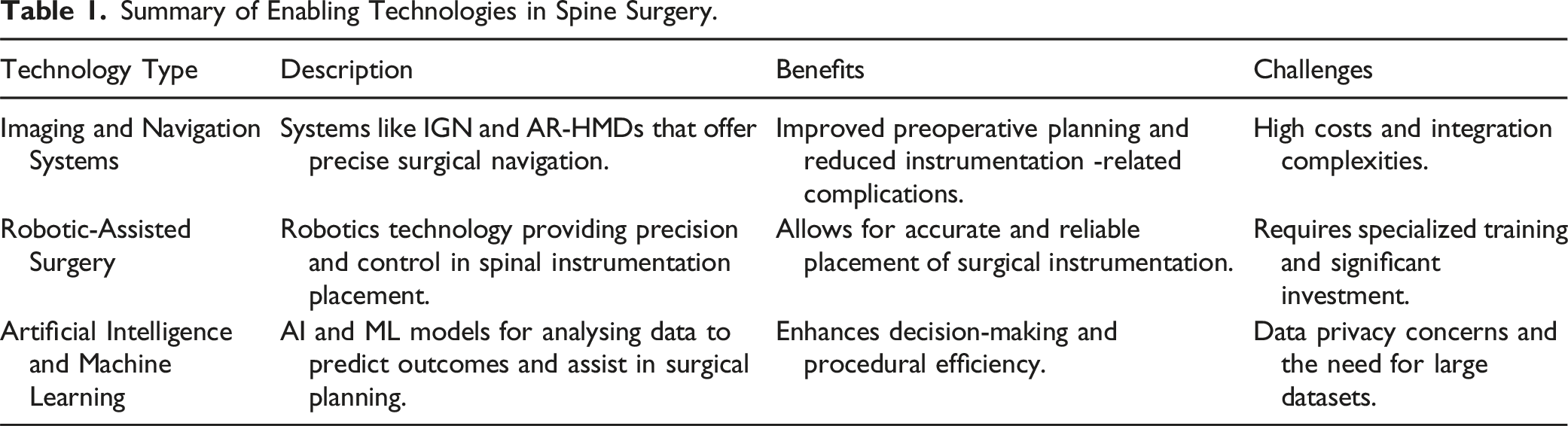
Factors Determining the Adoption
The successful integration of technological advancements into the practice of spine surgery is multifactorial. While the benefits of these technological advancements are well documented, their adoption is accompanied by a set of challenges. The financial implications of deploying state-of-the-art technologies, the necessity for specialized training for healthcare professionals, and the hurdles of integrating these innovations into existing healthcare infrastructures are significant barriers. 11 Moreover, ensuring equitable access to these technologies necessitates a careful evaluation of cost-benefit considerations and the formulation of fair healthcare policies. These determinants not only influence the speed at which new technologies are adopted but also sculpt the evolving landscape of spinal care.
Cost-Benefit Ratio
A foremost factor in the adoption of novel technologies in spine surgery is the evaluation of the cost-benefit ratio. The financial burden associated with acquiring and maintaining advanced surgical technologies, alongside the necessity for specialized training presents a significant consideration; and another potential challenge on the already burdened healthcare system. Decision-makers meticulously balance the capital cost of the technology against expected enhancements in patient outcomes, surgical efficiency, and the potential for decreasing long-term healthcare expenditures. 10 This careful assessment ensures that the advantages of new technological implementations substantiate the investments made. Zausinger et al 33 found that avoiding a revision procedure saved an average of $27,813.18 with the use of navigation in spine surgery. Meanwhile, a cost-effectiveness analysis by Al-Khouja et al 34 indicated that intra-operative imaging costs between $8820.51 and $9188.87. In contrast, the cost of revision surgery falls between $17,650 and $39,643. This analysis underscores the economic benefit of preventing revision surgery, despite the higher initial expense of navigation systems. As navigation systems become more cost-effective, its usage is expected to rise. It is noted that the operative time for pedicle screw placement is shorter when using navigation compared to fluoroscopy, although the surgeon’s familiarity with navigation may influence these results. 34 The expansion of applications for this technology will drive the growth and adoption of navigation-based systems.
Adoptability and Ease of Integration into Current Standard of Care
The ease with which these new technologies can be assimilated into surgical practices and workflows critically affects their adoption rate. Innovations that effortlessly merge with the current standards of care, necessitating minimal modifications to existing protocols are easily adopted. Further, technologies that are cost-efficient, ease to use providing obvious reproducible benefits to the patients finds their way into earlier adoption. Móga et al. highlight the importance of factors such as the learning curve for surgeons and staff, adaptability to various surgical contexts, and integration capabilities with other digital health systems to be pivotal in determining a technology’s adoption viability. 14 For example: adoption of these technologies has been shown to increase the operative time (35.6% longer with navigation), reliability on the datasets that were used to train the system and vulnerability to the software malfunctions. 35
Patient Acceptance
Patient receptiveness also plays a role in the adoption of technological advancements in spine surgery. Innovations promising to improve patient outcomes, diminish recovery durations, and enhance overall patient experiences are more likely to be welcomed by both patients and healthcare practitioners. As outlined by Marwaha et al, technologies that manifest tangible benefits in terms of patient safety, comfort, and satisfaction garner greater acceptance. 15 The willingness of patients to undergo procedures employing novel technologies might have an influence on the surgeons’ adoption decisions. However, there is evidence gap to prove improved clinical benefits with the adoption of these technologies in routine clinical care.
Learning Curve
The learning curve associated with new technologies emerges as a major decisive factor in their adoption. Technologies that demand extensive training or cause substantial disruptions to established surgical workflows will typically encounter significant resistance for adoption by surgeons. The presence of thorough training initiatives and support from technology manufacturers can alleviate these obstacles, promoting smoother adoption processes. Nevertheless, a technology that is truly associated with ease of use, a manageable learning curve, and associated with obvious surgical efficiency and clinical benefits will generally be quickly adopted by surgeons.5,36 Additionally, literature stresses the critical nature of education and training in surmounting the initial challenges posed by complex new technologies.2,10 20–30 cases have been considered as the necessary threshold to adapt to these technologies such as navigation and robotics in spine surgery and be efficient with their workflows.5,37
Accessibility for Training and Support
The availability of training and support resources is imperative for the successful adoption of innovative technologies in spine surgery. Proper training equips surgeons with the competence to utilize new technologies effectively, while ongoing support from manufacturers addresses emerging technical challenges. As noted by Berwick, accessible training programs and reliable technical support play a significant role in adoption decisions, ensuring healthcare providers exploit the full potential of these advancements. 11
Directions of Use
In consideration of the comprehensive examination of technological advancements in spine surgery and the multifaceted factors influencing their adoption, it is essential to propose actionable recommendations to safely and responsibly integrate these innovations into clinical settings. These recommendations aim to navigate the barriers hindering adoption while capitalizing on opportunities to elevate patient care through the adoption of cutting-edge technologies as shown in Figure 1. Factors determining the adoption of technology in spine surgery and recommended strategies on managing them.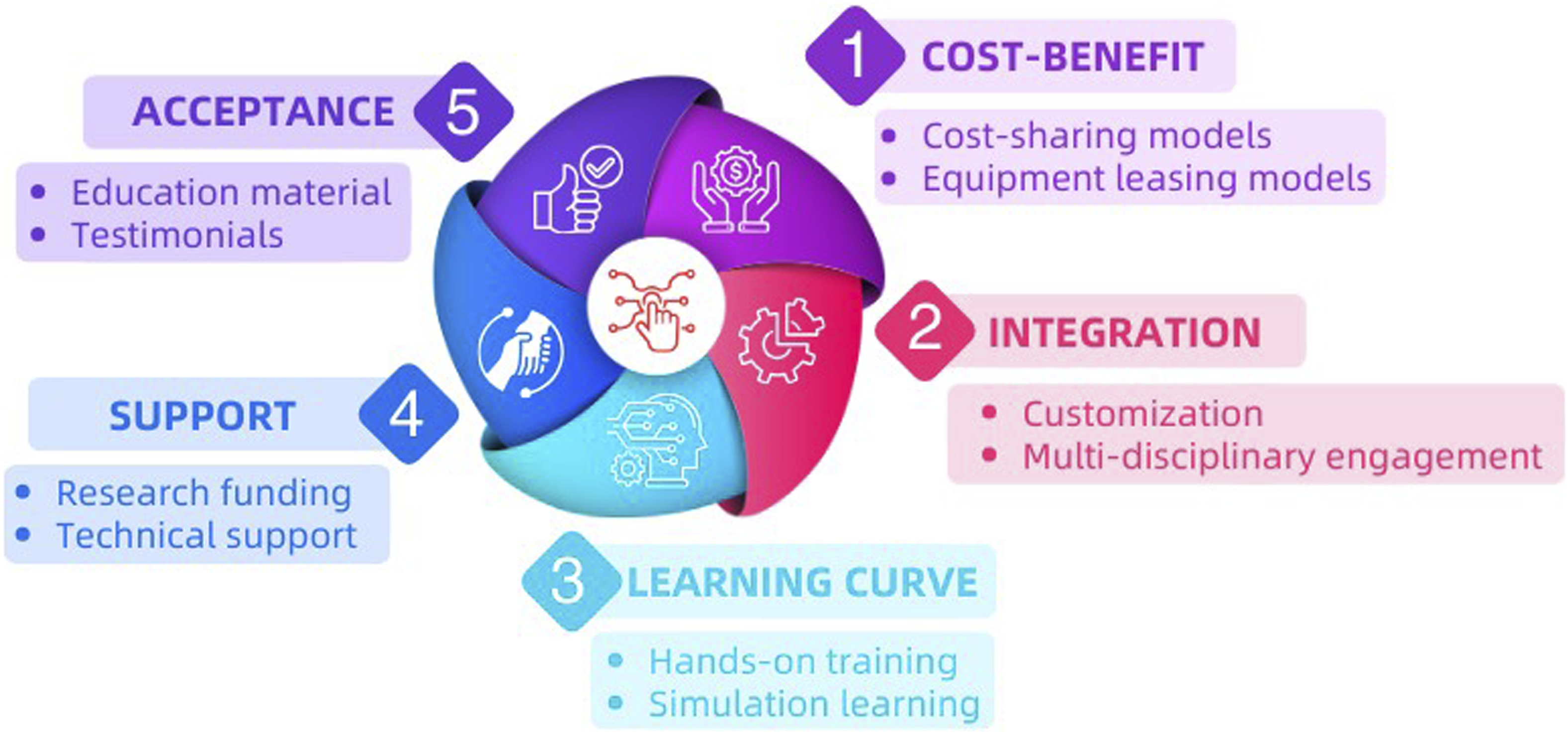
Enhancing Cost-Effectiveness
It is crucial for healthcare providers and decision-makers to prioritize evaluating the cost-effectiveness of new technological adoptions. Strategies to improve cost-effectiveness include negotiating favourable purchasing agreements, exploring leasing options for high-cost equipment, implant-use-based options, and adopting cost-sharing models to alleviate financial burdens. Conducting in-depth cost-benefit analyses and considering the long-term benefits for patient outcomes and the potential for healthcare savings is vital. There are also challenges in determining the most accurate method of cost determination. Traditional cost-accounting has gaps in the evaluation of time and personnel. Time-driven activity based costing has grown into a reliable method to incorporate specific personnel, activities, and time of activities into the cost equation. The results of such analyses should be broadly communicated to stakeholders, crafting a persuasive narrative for the investment in innovative technologies.
Streamlining Integration Processes
To ensure the seamless integration of new technologies into existing clinical workflows, it is recommended to engage multidisciplinary teams in the planning and execution stages. This approach ensures that the technologies meet the diverse needs and capabilities of all end-users. Offering customization options in some cases can also help adjust the technology to various clinical and surgical scenarios and patient requirements, thus facilitating smoother integration. Compatibility with existing healthcare informatics system is critical, as it promotes cross platform utilization, efficient data exchange, and care coordination.
Promoting Research and Innovation
Fostering research and innovation within the realm of spine surgery is imperative for the ongoing development of technological advancements. Healthcare institutions and funding organizations should support research efforts aimed at assessing the clinical and economic impacts of new technologies. Establishing partnerships among academic entities, industry representatives, and clinical practices can create an ecosystem that nurtures innovation and facilitates the swift application of research findings in clinical settings.
Fostering Patient Engagement and Education
Improving patient acceptance of new technologies necessitates proactive patient engagement and education by healthcare providers. Transparent discussions about the advantages and potential risks associated with new technologies can empower patients to make informed decisions regarding their treatment options. Providing educational materials, patient testimonials, and case studies demonstrating successful outcomes can significantly boost patient trust and confidence in new surgical technologies. Ultimately, robust peer-reviewed data is important to demonstrate the evidence-based nature of the decisions that surgeons make regarding patient care and new technology.
Investing in Training and Professional Development
A substantial investment in training programs for surgeons and their surgical team is essential to mitigate the learning curve associated with novel technologies. These programs should encompass hands-on training, simulation-based learning, and continuous professional development opportunities. Collaborating with technology manufacturers to offer specialized training and certification programs can ensure that healthcare professionals are well-equipped to leverage new technologies to their full potential.
Apart from the drive towards technological advancement and patient benefits, an overview of recommendations about the possible technologies that could be adopted based on the hospital set-up and patient load were outlined by Rossi et al. as given in Figure 2.
38
Hence, due consideration should also be given towards the caseload and volume of surgeons in the healthcare facility before embarking on procurement of assistive technologies for spinal surgeries. With advancements in technology, new tools will continue to emerge, promising increased precision and surgical efficiency. Nevertheless, it is impractical to integrate all these innovations into the surgical workflow simultaneously. Surgeons must evaluate the benefits of individual systems and their applicability to their practice before considering integration. For instance, while both navigation and robotics hold potential for enhancing efficiency, prioritizing navigation systems for initial integration appears more advantageous. Navigation not only aids in pedicle screw trajectory guidance but also offers diverse applications such as screw planning, cage planning, and decompression adequacy estimation. In contrast, robotics primarily focuses on pedicle screw trajectory at present. Therefore, the strategic selection of technological advancements based on their broader utility can significantly optimize surgical outcomes and efficiency. Recommendation for technological upgrade based on institutional setup. 3D, three-dimensional; CT, computerized tomography.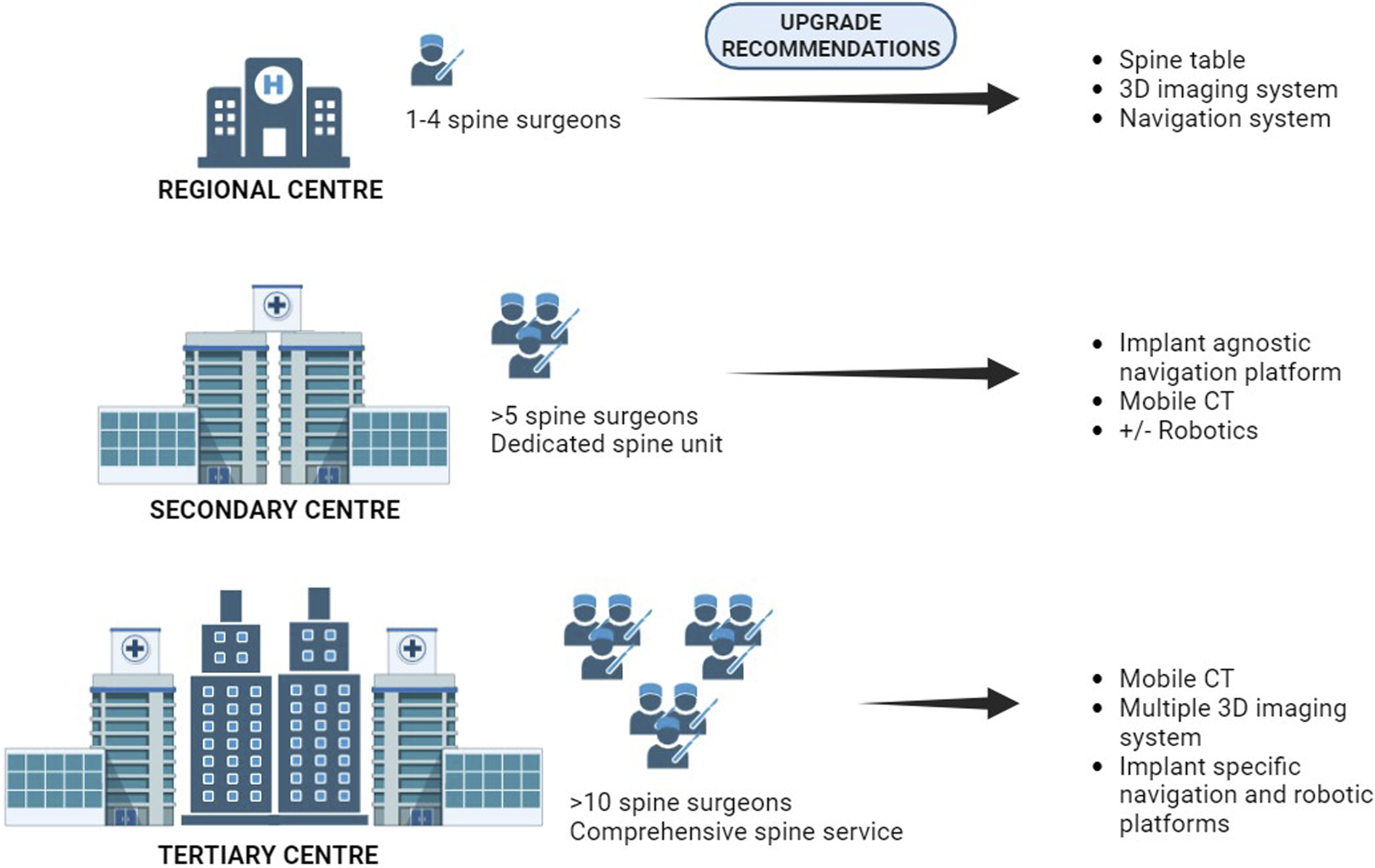
Conclusion
Recent technological advancements in spine surgery aim to improve the precision, efficiency, and safety of care delivered to patients presenting with spine pathology. As we navigate the complex landscape of integrating these technologies into clinical settings, it is evident that a multifaceted approach, considering cost-benefit analyses, integration, workflow, patient acceptance, learning curves, and the availability of training and support, is crucial for successful evaluation and adoption. As we create a reproducible method to responsibly adopt new technologies, we can build on these algorithms to further improve patient care in the future. One must not forget that these are only complementary and not competing technologies in assisting the surgeon at delivering the best possible care efficiently.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was organized and supported by AO Spine through the AO Spine Knowledge Forum Degenerative, a focused group of international experts. AO Spine is a clinical division of the AO Foundation, which is an independent medically-guided not-for-profit organization. Study support was provided directly through the AO Spine Research Department.
