Abstract
Study Design
Narrative Review.
Objectives
Endoscopic spine surgery is becoming an increasingly popular approach to treat spinal disease due to its minimally invasive nature. Although certain adverse events are well-reported within the literature, there is a scarcity of information for complications that are rare but still potentially serious. The purpose of this study is to describe these rare complications of endoscopic spine surgery and discuss management and prevention strategies.
Methods
A search was conducted in PubMed and Embase to review the literature for all adverse events following endoscopic spine surgery, with no restrictions on publication year. Cohort and case report studies describing infrequently reported complications were collected for analysis.
Results
A total of 38 studies were included which described rare complications in 93 patients following endoscopic spine surgery. These included neurological events (seizure, pseudomeningocele, pneumocephalus, upper limb palsy), vascular events (hemorrhage, hematoma, arteriovenous fistula), mechanical events (cage migration, guidewire breakage), and additional events (discal pseudocyst, pulmonary edema, arrhythmia, total spinal anesthesia).
Conclusions
Endoscopic spine surgery is rapidly evolving and emerging as a popular alternative to conventional approaches. Though regarded as a generally safe form of surgery, it is imperative that surgeons are aware of all complications which may occur, even those that may be infrequently reported in the literature.
Keywords
Introduction
Endoscopic spine surgery has evolved significantly since its inception, expanding from limited applications to a wide range of spinal degenerative diseases, including lumbar, cervical, and thoracic regions. 1 The minimally invasive nature of endoscopic spine surgery has led to its popularity due to its potential for improved patient outcomes, reduced recovery times, and decreased morbidity rates. 2
Numerous studies have demonstrated the efficacy and safety of endoscopic spine surgery, reporting significant reduction in pain and restoration of function postoperatively.3-6 However, complications in endoscopic spine surgery are not uncommon, with dural tears, perioperative hematoma, transient dysesthesia, nerve root injury, and recurrent disc herniation being reported in the literature. 2 Reassuringly, complication rates have decreased over time, likely due to improved techniques, enhanced training, and increased surgeon experience.1,7
As more surgeons are being trained in endoscopic spine surgery, the learning curve associated with this technique is becoming better understood. 8 Rare complications, such as subarachnoid hemorrhage 9 and pseudomeningocele, 10 have been reported in the literature, highlighting the need for awareness and vigilance among surgeons. With the growing number of surgeons performing endoscopic spine surgery, there is a potential risk of increased rare complications, particularly if proper training using established protocols is not ensured.
While systematic reviews have described the most common complications in endoscopic surgery, there is a dearth of literature aggregating and highlighting rare complications. This study aims to describe rare complications associated with endoscopic spine surgery, discuss prevention and management strategies, and emphasize the importance of proper training and adherence to established protocols to minimize these risks.
Methods
Literature Search
The following search was conducted in PubMed and Embase in October 2023: ((((spine OR spinal)) AND (endoscopic OR endoscopy OR thoracoscopic OR thoracoscopy OR microendoscopic OR microendoscopy)) AND (transforaminal OR foraminal OR interlaminar OR discectomy OR diskectomy OR microdiscectomy OR decompression OR fusion OR foraminotomy OR laminectomy OR biportal OR uniportal)) AND (complication OR adverse).
Screening Criteria
Studies were excluded from review if they were not in English, involved a subject population under 18 years of age, or did not discuss surgical complications. The focus was primarily on case series and case reports, but also included cohort studies. Articles were included for review if they focused on endoscopic surgeries of the spine and described infrequently reported complications. For the purposes of this study, data on frequently encountered complications was not collected. These more frequently encountered complications included hematoma, infection, dural tear, transient neurological deficits, and incomplete decompression. Six authors were involved in the screening process, and each paper was screened independently by two authors at each stage of screening. Any disagreements were resolved by a third author.
Data Collection
From each included study, the following information was collected: complication and number of patients who had experienced the reported complication, procedure type, indication for surgery, spinal region, and surgical approach.
Results
A total of 38 case reports were included, describing 93 patients who had experienced rare complications following endoscopic spinal surgery (Figure 1). Complications were categorized into three broad categories (neurologic, vascular, mechanical) or a fourth category (other complications) if they did not adequately fit into the former three. Flow diagram of included studies.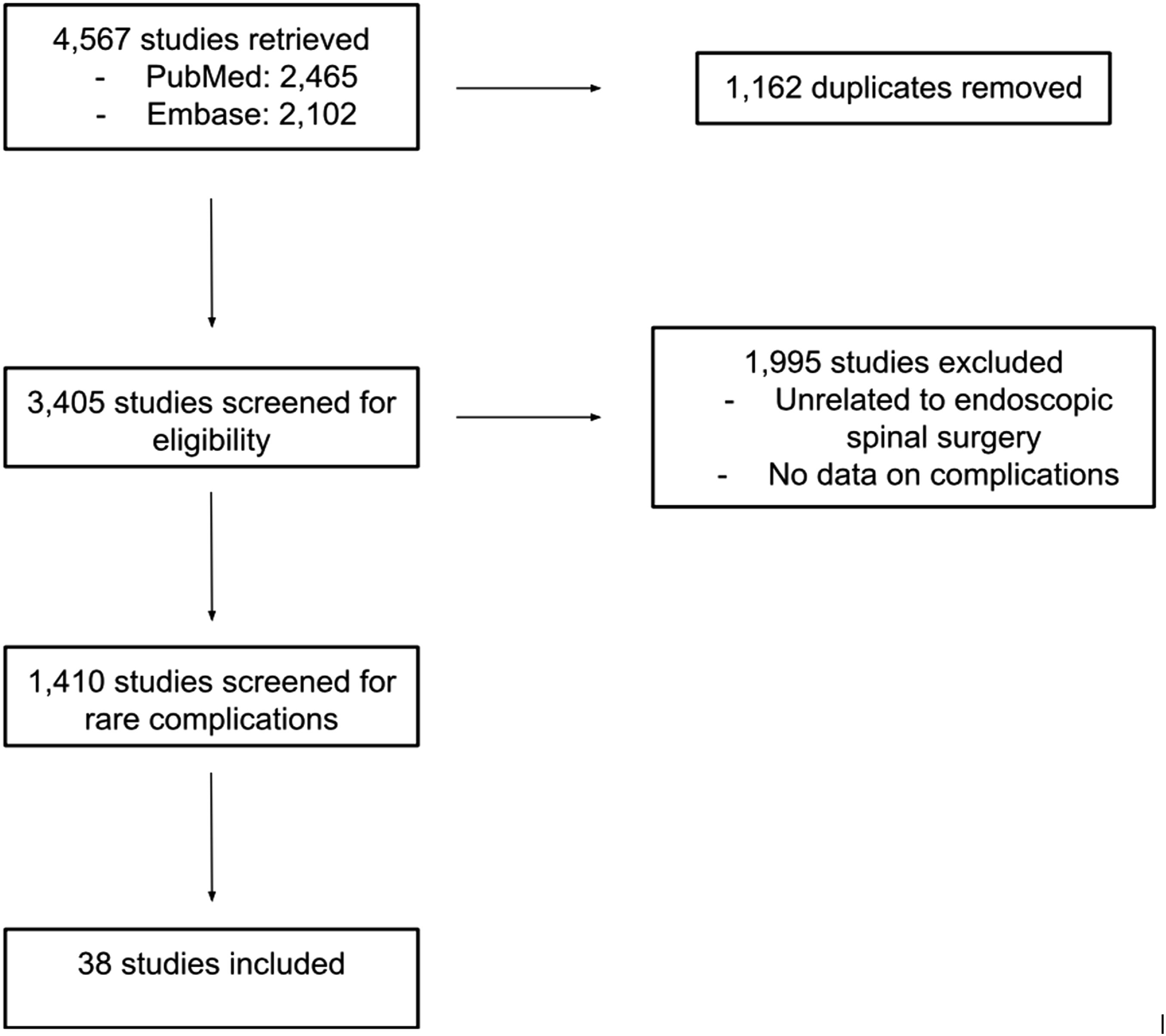
Rarely Reported Neurological Complications of Endoscopic Spinal Surgery. PELD = Percutaneous Endoscopic Lumbar Discectomy; TLIF = Transforaminal Lumbar Interbody Fusion; BESS = Biportal Endoscopic Spinal Surgery; FELD = Full Endoscopic Lumbar Discectomy; PPCED = Posterior Percutaneous Endoscopic Cervical Foraminotomy and Discectomy.
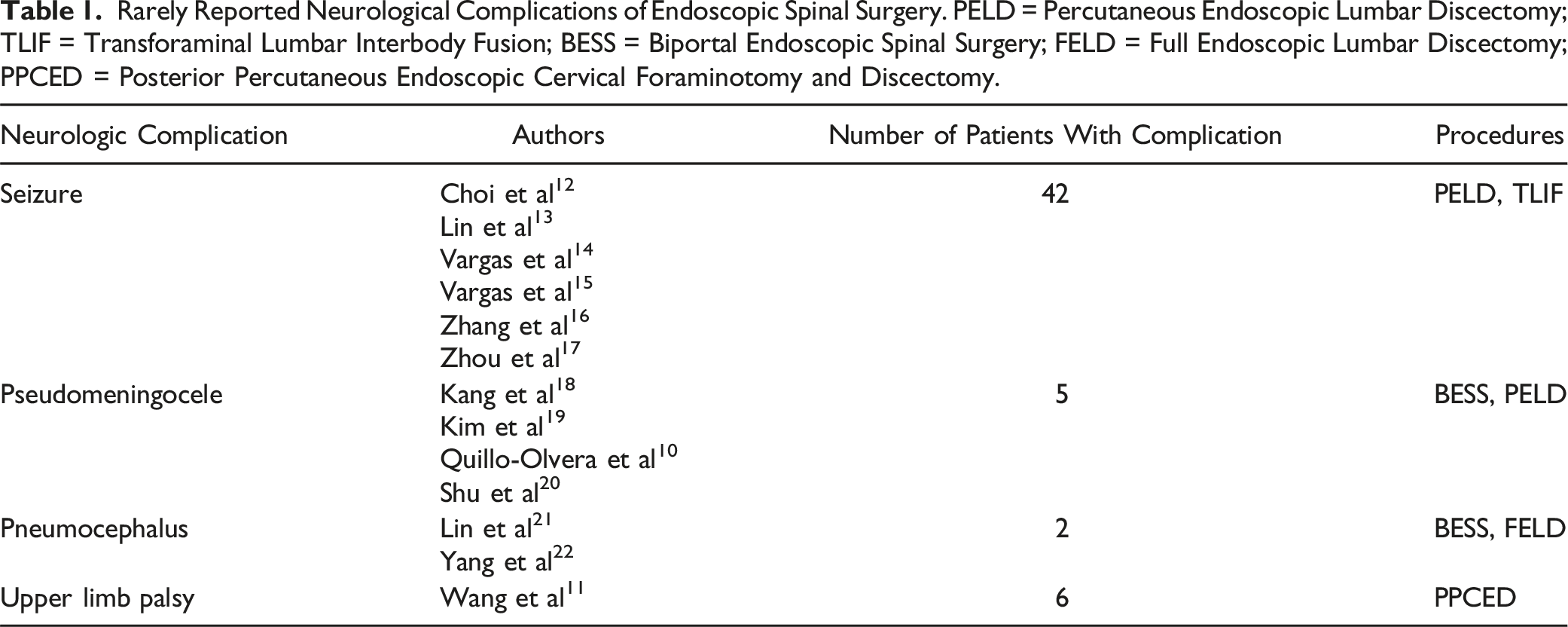
A second notable rare postoperative complication was seizure in patients without a known history of seizures. For example, four out of nearly 17,000 patients who underwent PELD developed postoperative seizure in a large retrospective analysis in Korea. 12 Strikingly, all four patients reported neck pain prior to seizure onset and had longer mean operative time. Another study on 816 patients who underwent percutaneous endoscopic spine surgery found 3 out of 816 patients experienced seizure, who all had a unique prodromal symptom of uncontrolled hypertension with decreasing pulse rate prior to seizure onset. 13 The authors found infusion of cefazolin, the infusion rate, prolonged operative time, dural tear, and sevoflurane anesthesia may be associated with seizure. At a third institution where seizure incidence after percutaneous endoscopic spine surgery was 0.52%, 52% of patients who experienced seizure (15/24) had definitive dural tears. 16 Agitation, myotonia, increased respiratory rate, tachycardia, hypertension, hypocapnia, metabolic acidosis, and hyperlactatemia were observed. The estimated duration of seizure was 3 hours and there were no significant adverse effects of seizures on clinical outcomes at 6 months postoperatively. Two other case reports were notable for rare findings of pneumocephalus on CT, spinal headaches and diplopia, intraventricular hemorrhage, or hydrocephalus.14,15 In these case reports on seizure following endoscopic spine surgery, postoperative seizures were managed with sedatives (e.g., IV midazolam) and analgesics with no reported long-term seizure-related complications.12-16
Two other case reports in this review also demonstrate pneumocephalus as the primary complication with and without seizure.21,22 Following pure oxygen and hyperbaric oxygen therapy, the man with generalized tonic-clonic seizures, tachypnea, and pneumocephalus regained consciousness 8 hours after the operation and had full recovery in mental status. 21 The 79-year-old female who developed pneumocephalus without seizure was treated with a vacuum drain which drained approximately 150 mL of CSF and she subsequently recovered with hydration and bed rest. 22
Finally, three case reports and one retrospective review describe postoperative pseudomeningocele as a possible complication of endoscopic spine surgery.10,18-20 For example, a 52-year-old male who underwent PELD was readmitted 6 weeks postoperatively with progressive right leg pain; revision surgery demonstrated a pseudomeningocele-containing nerve root herniating through a small dural defect. 20 During the dissection process, the pseudomeningocele was broken and the nerve root was consequently entrapped. A microsurgical technique was adopted to relocate the nerve root into the thecal sac and to repair the dural tear. A second case report of a 61-year-old female who underwent PELD/foraminotomy had postoperative fever with severe low back pain radiating down right leg; MRI demonstrated pseudomeningocele and nerve root herniated through dural sac. 10 Subsequent cultures demonstrated pseudomeningocele was infected. After antibiotics and direct microscopic dura repair, the patient improved significantly. A final pseudomeningocele case report utilized a patch to seal small dural tear in a 45-year old male who underwent biportal endoscopic discectomy. 18 Lastly, a retrospective review of 25 biportal endoscopy cases with known dural tear reported two postoperative pseudomeningocele; both were treated with patch technique and fibrin glue with one requiring delayed conversion to open repair due to patch failure. 19
Rarely Reported Vascular Complications of Endoscopic Spinal Surgery. FELD = Full Endoscopic Lumbar Decompression; TLIF = Transforaminal Lumbar Interbody Fusion; PELD = Percutaneous Endoscopic Lumbar Discectomy; PECD = Percutaneous Endoscopic Cervical Discectomy; FETD = Full endoscopic Transforaminal Lumbar Discectomy.

In 2021, Bae et al described the first case of a spinal subdural hematoma (SSDH) in a 68 year old female after a full-endoscopic interlaminar lumbar decompression for disc protrusion at L4-L5. 25 This patient began noticing complications a few days post-op and MRI indicated hematoma formation at L5-S1, which required an emergent open surgical decompression with hematoma evacuation before resolution. In another large-scale study looking at 412 patients treated with transforaminal percutaneous endoscopic lumbar discectomy (PELD) for disc herniations, 4 patients (0.97%) developed inguinal pain from retroperitoneal hematomas (RPH) within 4 hours postoperatively. 24 The mean age was 42.5 years, with the youngest being 31 and the oldest being 64. Two of these patients with severe diffuse-type RPH required open hematoma evacuations while the other two had localized RPH that was treated conservatively with monitoring.
Other rare vascular complications during endoscopic spine surgeries include injuries to the arterial vasculature,26,28 pseudoaneurysms, 27 and the formation of AV fistulas,29,30 which all occurred in endoscopic discectomies. In a study evaluating the efficacy of anterior percutaneous endoscopic cervical discectomy (APECD) for cervical intervertebral disc herniation, one patient (1 of 121 discs, 0.8%) developed a carotid artery injury that required treatment with angiographic stenting. 26 A right-sided approach was taken to address the herniation at C5-C6, and the surgeon had difficulty setting the cannula into the disc, so a trephine saw was used to enlarge the opening in the anterior longitudinal ligament and anterior annulus fibrosus.
Additionally, pseudoaneurysm is a rare but possible vascular complication of endoscopic spinal surgery. A 39-year-old man underwent full endoscopic transforaminal lumbar discectomy (FETD) at L4-L5 with use of guidewire and cannulated dilator to access the foraminal space. The surgery was uneventful, but three hours post-op the patient developed left flank pain and was found to have a pseudoaneurysm of the left lumbar segmental artery, which was subsequently embolized via endovascular coiling. 27
Lastly, cases of AV fistula have been rarely reported. During a PELD for L4-L5 herniation in a 38 year-old male, surgeons encountered increased blood extravasation from the disc space and a drop in blood pressure. 29 The bleed was resolved with hemostasis and the rest of the procedure was uneventful until 12 hours post-op, when the patient developed hypotension and tachycardia. CT imaging revealed an AV fistula between the right common iliac vein and artery, which was successfully treated with endovascular stenting.
Rarely Reported Mechanical Complications of Endoscopic Spinal Surgery. TLIF = Transforaminal Lumbar Interbody Fusion; PELD = Percutaneous Endoscopic Lumbar discectomy; ALIF = Anterior Lumbar Interbody Fusion.
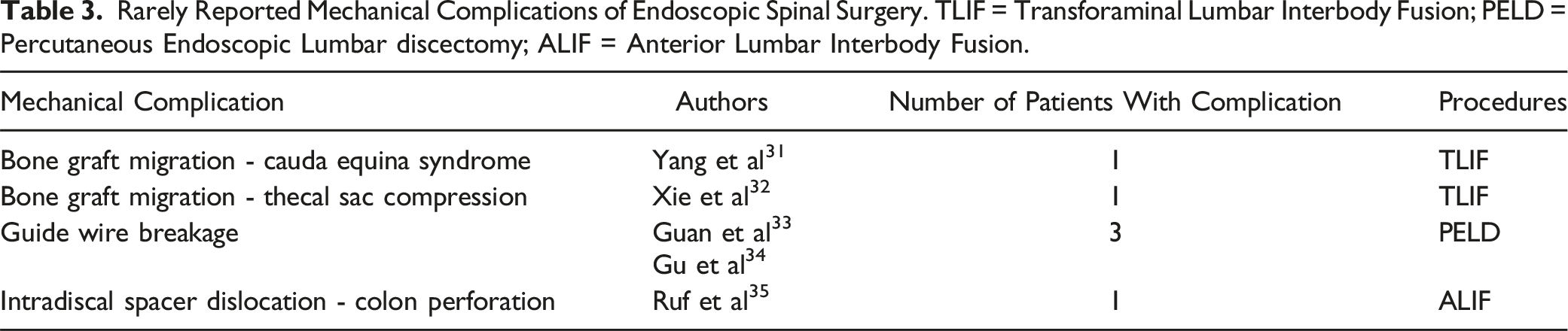

Complications during PELD procedures are also noteworthy, with one study reporting guidewire breakage in two patients (aged 28 and 33) who experienced guidewire breakage. 34 Both cases involved difficulties in positioning the guidewire, leading to breakage and entrapment in disc fragments. The broken guidewires were retrieved using straight grasping forceps under endoscopy, leading to immediate recovery and stable postoperative courses. Furthermore, another study reported a 28-year-old man with guidewire breakage during a PELD for an L4-L5 herniated disc. 33 The guidewire was successfully retrieved under endoscopy, and the patient remained symptom-free for 6 months.
Ruf et al reports a 39-year-old man with L5/S1 spondylolisthesis who underwent posterior instrumentation and endoscopic anterior insertion of two cages. 35 Four years post-operation, he noticed an interbody cage in the toilet after experiencing abdominal pain and diarrhea. Radiographic examination revealed perforation of the sigmoid colon and anterior dislocation of the remaining cage. The surgical intervention included partial resection of the colon, removal of the second cage, and packing of the defect with autologous cancellous bone and antibiotics. The patient recovered without infection, achieving solid bony fusion within 6 months.
Rarely Reported Additional Complications of Endoscopic Spinal Surgery. PELD = Percutaneous Endoscopic Lumbar Discectomy; PEID = Percutaneous Endoscopic Interlaminar Lumbar Discectomy; PECD = Percutaneous Endoscopic Cervical Discectomy.
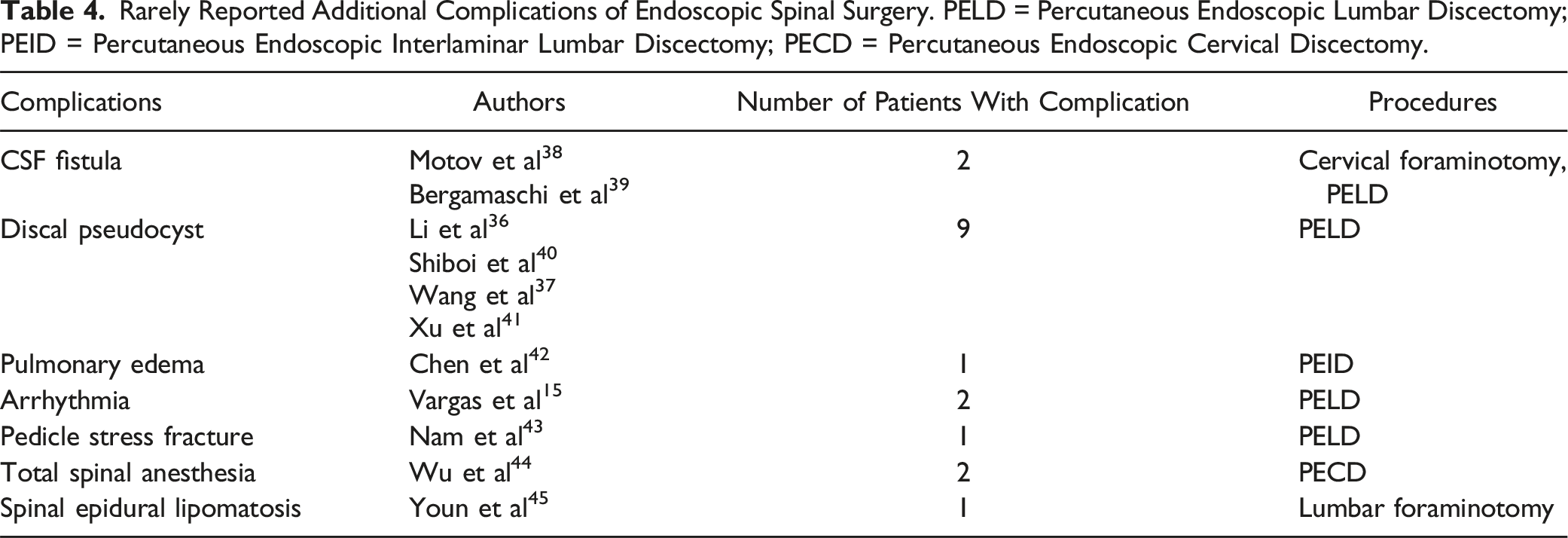
Additionally, a case of negative pressure pulmonary edema (NPPE) was described in a 22 year-old amateur male basketball player undergoing percutaneous endoscopic interlaminar lumbar discectomy (PEID) for L5-S1 herniation. 42 The patient developed NPPE during extubation and was subsequently treated with positive pressure ventilation and administration of dexamethasone, antibiotics, and furosemide.
Discussion
To our knowledge, this is the most comprehensive description of less commonly reported complications within the field of endoscopic spinal surgery. While there is growing evidence characterizing the more frequently encountered complications, the literature remains scarce regarding those that are rarely reported, though potentially dangerous to patients undergoing endoscopic spinal surgery. The following discussion highlights the important takeaways regarding this aggregation of cases.
Rare Neurological Complications
In addition to rare perioperative nerve injury after cervical foraminotomy, 11 we identified several rare neurological complications associated with endoscopic spine surgery, notably seizures and pneumocephalus.12-17,21,22 The reported rate of seizure following an endoscopic spine surgery case series generally ranged from 0.02% to 0.52%, though one case series reported three out of fifteen (20%) of patients with postoperative seizure with recognized incidental durotomy. The only reliable prodromal symptom was neck pain following an endoscopic lumbar spine procedure.12,17 Notably, Choi et al. found patients with neck pain following PELD had a mean maximal cervical epidural pressure of about 72 mmHg, vs 44 mmHg in patients without postoperative neck pain. 12 The studies associated the saline infusion rate, intrathecal leakage of cefazolin (a known GABA receptor antagonist) or air (resulting in pneumocephalus) in the setting of incidental durotomy, use of the anesthetic sevoflurane, and extended operative time with a higher risk of postoperative seizure.12-17,46,47 For example, Choi et al. hypothesized continuous infusion of saline may increase intracanalicular pressure, compressing the thecal sac and thus creating a cerebrospinal (CSF) fluid pressure wave in the cephalad direction. 12 This in turn may lead to increased intracranial pressure (ICP) and thus lead to seizure development. This may even occur due the transiently high starting pressure of gravity-assisted irrigation. 15 Prior studies have suggested ideal irrigation pressures should be at or below 30 mmHg, up to a maximum of 50 mmHg, to optimize safety.2,48-52 As such, spine surgeons should be mindful of keeping saline infusion pressure around a maximum 30 mmHg and only transiently increase to 50 mmHg if further bleeding control is necessary, with either gravity or low-pressure pump. It is also important to keep a patent outflow cannula through one of the portals via a fascia incision perpendicular to the skin incision for working portal, which allows fluid to continually extravasate from the surgical site and prevents increasing pressure.2,53 Additionally, avoidance of cefazolin in saline infusion, caution with induction using sevoflurane, and taking additional measures prevent, recognize, and effectively treat incidental durotomies, may assist in seizure prevention in the endoscopic spine surgery setting.10,18-20
Another rare postoperative complication was dural pseudomeningocele.10,18,20 Pseudomeningocele, a part of a continuum that includes CSF fistulas, is caused by a breach in the dural-arachnoid layer. Although pseudomeningocele is generally asymptomatic and self-resolving with bedrest and watertight skin closure, symptomatic pseudomeningocele in the spine surgery setting commonly presents as postural headaches, recalcitrant back pain, a fluctuant mass that increases with Valsalva, and radiculopathy especially in cases of an entrapped nerve root.54,55 MRI demonstrates CSF extravasation into the paraspinal musculature as well as possible fistula formation and/or nerve root herniation through the durotomy.18,20 Management of this complication is controversial, but in cases of symptomatic pseudomeningoceles, surgery is often recommended. 54 Surgery entails exploration of the pseudomeningocele, reduction of nerve roots, excision of fistula tracts, and dural repair if possible. In cases where dural repair is not possible, a patch should be used; a drain should not be inserted such that a hematoma can compress over the patch and close the area. 18
Overall, several preventative measurements should be implemented to prevent unlikely but potentially serious complications following endoscopic spine surgery. For example, minimization of cervical nerve root traction can help prevent ULP and measures to prevent, recognize, and treat incidental durotomy are paramount to the avoidance of seizure, pneumocephalus, or pseudomeningocele. Furthermore, the choice of anesthetic agent, irrigation pressure, and operative time must be optimized to minimize morbidity. With respect to detection of rare complications when they do occur, unexpected neck pain should alert the endoscopic spine surgeon to the possibility of impending seizure and symptoms such as postural headache and fluctuant mass with Valsalva maneuver should invoke MRI imaging for possible pseudomeningocele.
Rare Vascular Complications
Despite the advancement and high success rates of endoscopic spine surgery, rare vascular complications are still reported among patients undergoing such procedures. These vascular complications generally consist of hemorrhages, hematomas, arterial injuries, and AV fistulas.
Intracranial hemorrhage is a rare but potentially fatal complication of endoscopic spinal surgery. In the case of the 54 year-old male who underwent L5-S1 endoscopic laminectomy and discectomy found to have intracranial hemorrhage, the possible intradural migration of irrigation fluid may have contributed to the fatal outcome. 23 Other contributing factors, as noted by the authors, included the inappropriate manipulation by the initial inexperienced surgeon, who had less than 10 cases in spinal endoscopic surgery, and an extended surgery time to rectify the intra-operative dural tear that resulted in CSF fluid leakage. The presence of dural tears is associated with an increased rate of other perioperative complications which often worsens prognosis and recovery in patients. 56 This was evident in the case of another patient who developed Fisher Grade IV subarachnoid hemorrhage. 14 In these instances, longer operative times and continuous irrigation can increase intracranial pressure and further exacerbate intracranial hemorrhage formation. 2 These unfortunate cases demonstrate the possible cause of incidental unrecognized durotomy with intradural migration of irrigation fluid, and warn against use of continuous irrigation. The case of spinal subdural hemorrhage on the other hand is unique because the authors confirm that the dura remained intact during the procedure. While the exact cause is unknown, they believe the most likely explanation was damage to the bridging vessels between the inner and outer layers of the dura mater secondary to dural manipulation via irrigation pressure. In each of these cases, best practices for minimizing poor outcomes include maintaining caution when performing endoscopic surgery, especially in the setting of potentially challenging anatomy (such as calcified herniated disc), reducing the use of continuous irrigation when possible (not recommended to elevate the irrigation saline beyond 200 mL/min23), and closely monitoring patients with longer surgery times or unexplained neurological deterioration postoperatively.
As for retroperitoneal hematoma, Ahn et al. found 4 cases in their cohort of 412 patients (0.97%). 24 In the two patients who had severe hematomas requiring evacuation, one had associated liver cirrhosis and the other had a recurrent herniation that prompted a repeat PELD. In the other two patients with localized RPH managed conservatively, no associated prior risk factors were noted and no active bleeding was noted intraoperatively. Therefore, proper risk assessment prior to surgery is important for guiding management when complications may arise, with conditions like cirrhosis and prior surgery heightening risk of severe bleeding. While most hematomas present asymptomatically, rarely they can cause devastating neurological deterioration. Preventative measures such as modifying surgical techniques, taking caution to avoid major vascular structures, and using various hemostasis measures can help reduce unwanted hematoma formation. 57
In the case of carotid artery injury, the authors determined that the artery was cut by the teeth of the trephine saw used to enlarge the cannula opening. 26 To avoid this complication, the authors recommended against use of a trephine saw to divide the anterior pathway and instead gradually advance the cannula with serial dilation sleeves under fluoroscopic imaging. They also attributed this injury to the patient’s relatively narrow anterior disc height (4.0 mm); the same complication reported by Gastambide et al attributed the injury to the patient’s thick, short neck and inability to detect carotid pulse. 58
Other types of vascular damage include pseudoaneurysms, as seen in the case of FETD at L4-L5. 27 The authors postulate that the technical step involving the surgeon is puncturing with the guide needle without a clear line of vision in a trial-and-error manner to access the foraminal region predisposes to multiple attempts and greater risk of damage to adjacent structures. This mechanism of injury was also suggested by Ahn et al. in their study investigating postoperative retroperitoneal hematomas. 24 These injuries can be prevented through adequate technical skill training among surgeons to reduce the likelihood for inaccurate needle penetration.
Lastly, AV fistula is a rarely reported but serious adverse event. In the case of fistula between the right common iliac vein and artery in a patient undergoing PELD at L4-L5, the authors believe the injury was caused by anterior perforation of the pituitary rongeur through both vessels. 29 To prevent this, the rongeur should not be inserted more than 3 cm into the disc space. This is supported by other studies finding ventral rongeur perforation to be the most common cause of anterior vascular injury, followed by curette and rongeur use together, and then curette use alone. 59 Risk factors that also increase likelihood of anterior perforation include degeneration of the anterior longitudinal ligament or annulus fibrosus, as well as their adhesion to prevertebral structures as caused by prior abdominal operations. The authors recommend use of a curette to first loosen disc fragments and to limit use of the rongeur to only pick these loose fragments from the space. They also advise to maintain a high degree of suspicion for vascular injury even in cases when abnormal bleeding becomes controlled, as the prone perioperative position can contribute to vascular tamponade which may mask a tear that must be repaired.
Prognosis varied among these rare vascular complications though most patients generally recovered following treatment. For arterial injuries, two patients underwent endovascular coiling achieved full recovery within 4-8 days, and one treated conservatively (NSAIDs and bed rest) recovered within one week.26-28 Two other patients with subarachnoid hemorrhage recovered with conservative measures by three months.9,14 Unfortunately, the patient with a postoperative intracranial hemorrhage (PIH) died on post-operative day two despite emergent thrombectomy and neurosurgical interventions. 23 As such, long term prognosis for patients suffering vascular complications after endoscopic spine surgery can vary widely depending on the severity and time of intervention.
Rare Mechanical Complications
Postoperative bone graft migration (PBGM) into the spinal canal is a rare but severe mechanical complication following endoscopic transforaminal lumbar interbody fusion (TLIF). The studies identified risk factors for PBGM including excessive graft volume, posterior placement of the graft, and endplate damage. Under continuous water irrigation, the insecure placement of bone graft materials, coupled with acutely increased intervertebral pressure, likely caused the migration of the bone graft into the spinal canal causing severe nerve compression and symptoms.60-62 Effective management emphasizes early recognition and prompt surgical intervention to remove the migrated grafts and alleviate symptoms. Preventive measures include using an appropriate graft volume, ensuring anterior placement, and securing the graft during surgery. The long-term outcomes and prognosis of patients with PBGM depend on the timely recognition and management of the complication. Early surgical intervention appears to be crucial in mitigating adverse outcomes, but further studies are needed to better understand the long-term prognosis of these patients.
Additionally, guidewire breakage during percutaneous endoscopic lumbar discectomy (PELD) is another rare but significant mechanical complication. Guidewires may be used in endoscopic spine surgery during dilation to facilitate the accurate and safe placement of dilation instruments and other surgical tools. The studies cited technical difficulties in positioning the guiding rod, inadequate handling, anatomical challenges like high iliac crests at L5-S1, and surgeon experience as risk factors for guidewire breakage. The pathophysiology involves repeated manipulation and redirection, leading to metal fatigue and fracture, with the guidewire becoming entrapped in disc fragments or spinal structures. Management focuses on immediate retrieval using endoscopic techniques and fluoroscopic guidance to address this. In both studies, prompt retrieval with straight grasping forceps under endoscopy was successful. For less experienced surgeons, converting to open surgery may be advisable to ensure safe removal as broken guidewire can become entrapped within disc fragments and pose a risk of further complications. With regard to prevention, the authors also recommend forgoing the use of a guidewire, as this is currently not a common practice during endoscopic discectomy.
Lastly, late dislocation of an interbody cage resulting in perforation of the sigmoid colon was found as a rare mechanical complication following endoscopic anterior lumbar interbody fusion. While late cage migration may not be unique to the endoscopic approach of interbody fusion, it remains a significant complication that surgeons must be aware of, even years postoperatively. The interbody cage dislocation involved incomplete or absent bony fusion, allowing repetitive micromotion to displace the cage. Additionally, bone quality and the extent of spondylolisthesis reduction play a role. In this case, anterior dislocation led to mechanical irritation and sigmoid colon perforation, causing transanal passage of the spacer. Managing such cases includes immediate surgical intervention to resect the perforated colon, remove the dislocated spacer, and pack the defect with autologous cancellous bone and antibiotics. Postoperative care involves monitoring for infection and routine radiographic follow-up to ensure solid bony fusion.
Preventing cage migration in lumbar interbody fusion involves several strategies. Osteoporosis management is crucial, as low bone mineral density (BMD) significantly increases the risk of cage migration. Preoperative optimization of BMD through pharmacological agents such as bisphosphonates or denosumab can be considered. Endplate protection is another key factor; meticulous surgical technique to avoid endplate injury during cage insertion is essential, as endplate damage is strongly associated with cage migration.63,64 Proper cage positioning is also vital for stability. Anterior placement of the cage has been shown to reduce the risk of migration and subsidence by distributing the load more evenly across the endplate. Cage selection also plays a role; using bilateral cages rather than a unilateral single cage can provide better stability and reduce migration risk.65,66 Instrumentation is another critical aspect. Bilateral pedicle screw fixation is recommended over unilateral fixation to enhance stability and reduce the risk of cage migration. Finally, selecting an appropriately sized cage that fits well within the disc space is crucial. Undersized cages are more prone to migration, and using cages designed to maximize endplate contact can help reduce this risk. 67
Additional Rare Complications
Pseudocysts are cystic lesions that can arise in the spinal disc of the operative site and compress nerve roots leading to a recurrence of preoperative symptoms. The exact pathogenesis of pseudocysts remains unclear, though it may be in part due to fluid accumulation during and after surgery which causes a preformed cyst to enlarge. 37 They appear to be more common in young men and often present with unilateral radiculopathy and low back pain. Potential management options include surgical cystectomy and conservative treatment. 40 Prognosis is favorable, and lesions will often spontaneously regress within 6 months when treated with a combination of bed rest, NSAIDs, and physical therapy. 41
The case of negative pulmonary pressure edema is intriguing as it is the first of its kind in patients undergoing endoscopic spinal surgery. 42 The cause is thought to be laryngospasm during extubation leading to marked increases in inspiratory force and negative intrathoracic pressure leading to greater entering blood volume which overwhelms the alveolar vessels. Though this event is not directly related to the endoscopy surgery itself and more so attributable to anesthesia protocols, it is important for spinal surgeons to be aware of all adverse events which may occur during a case. Furthermore, the authors hypothesize that this patient’s younger age and athletic build may have predisposed him to this adverse event. Therefore, as endoscopic spinal surgery becomes increasingly popular in the younger demographic, surgeons must be aware that younger athletic males may be at greater risk for NPPE due to their ability to generate greater inspiratory pressures in response to laryngospasm.
Clinical Implications
Early recognition and prompt management of complications such as respiratory compromise due to CSF leak are essential for optimizing patient outcomes. Clinical vigilance for symptoms like progressive dyspnea, positional headaches, or neck swelling should prompt immediate diagnostic evaluation and, if confirmed, appropriate interventions such as imaging, surgical repair, or CSF drainage. 68 Once these complications are addressed acutely, long-term management requires a structured follow-up plan to ensure patient safety and prevent recurrence. Spine surgeons should monitor patients closely during postoperative visits for any residual or delayed symptoms, such as persistent headaches, neck pain, or changes in breathing patterns, which may indicate incomplete resolution of complications. Routine imaging may be considered in cases with atypical recovery trajectories, and patients should be informed to report new or worsening symptoms promptly. While there is no consensus on follow-up duration, a period of at least 6-12 months may be warranted, with a focus on ensuring stable resolution of symptoms and identifying any late-onset complications on an individual patient basis. 69 By integrating vigilance in both the acute and long-term phases of care, surgeons can improve outcomes for patients experiencing these uncommon but serious complications.
Limitations of Included Studies
The studies included in this review were predominantly retrospective cohort studies and case reports, both of which are subject to inherent limitations. Retrospective designs rely on past medical records, making them susceptible to recall bias as well as potentially incomplete data, which may limit a thorough portrayal of events surrounding individual cases. Case reports are subject to reporting and publication biases, as authors may choose to focus on atypical presentations and omit cases which follow a more predictable course. Furthermore, the lack of standardized data collection and reliance on clinical observations can perpetuate inconsistencies across studies. For instance, patient follow-up periods often varied, preventing comprehensive comparisons between cases. Lastly, the small sample sizes characteristic of case reports limit the generalizability of findings, which is to be expected of an analysis of rare complications Despite these limitations, this synthesis of less commonly reported complications provides valuable insights for clinicians, particularly in recognizing, managing, and preventing these rare events.
Conclusion
Endoscopic spine surgery is rapidly evolving and emerging as a popular alternative to conventional approaches. Though regarded as a safe generally safe form of surgery, it is imperative that surgeons are aware of all complications which may occur, even those that may be infrequently reported in the literature.
Footnotes
Declaration of Conflicting Interest
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Samuel K. Cho, MD, FAAOS, AAOS (Board or committee member), American Orthopaedic Association (Board or committee member), AOSpine North America (Board or committee member), Cervical Spine Research Society (Board or committee member), Globus Medical (IP royalties and Fellowship support), North American Spine Society (Board or committee member), Scoliosis Research Society (Board or committee member), Stryker (Paid consultant), Cerapedics (Fellowship support). The following individuals have no conflicts of interest: Ryan D. Stadler, BS, Nancy Shrestha, BA, Gabriel Dara, BA, Alexander Yu, BS, Mark Kurapatti, BS, Suhas Etigunta, BS, Daniel Berman, MD, Joshua Lee, MD, Brian Cho, MD.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
