Abstract
Study Design
Retrospective cohort study.
Objectives
To evaluate the complications of anterior lumbar interbody fusion (ALIF) in patients with primary hypercoagulable disorders and to compare outcomes between anterior and posterior spine fusions in this patient population.
Methods
The PearlDiver national patient database was queried for patients with primary hypercoagulable disorders who underwent ALIF. Primary endpoints included the prevalence of hypercoagulable disorders in patients who underwent ALIF, incidence of perioperative anticoagulation utilization, as well as the 30-day risks of postoperative complications, readmissions, and revision surgeries. Multivariate regression analysis was conducted to compare outcomes between hypercoagulable patients and non-hypercoagulable patients undergoing ALIF and between hypercoagulable patients undergoing anterior vs posterior lumbar fusion.
Results
Of the 211,390 patients who underwent ALIF, 3380 (1.60%) had a hypercoagulable disorder, with only 6.72% receiving perioperative anticoagulation. Within 30 days of ALIF, hypercoagulable disorders were identified as independent risk factors for hospital readmissions and both medical and surgical complications. Compared to posterior spine fusions, the anterior approach poses a greater risk for complications in this patient population.
Conclusions
Patients with hypercoagulable disorders undergoing ALIF are at increased risk for readmissions and postoperative complications compared to those with normal coagulation profiles. While the posterior approach may be a safer option in this patient population, further research is needed to clarify the safest surgical approach for this high-risk population.
Keywords
Introduction
Anterior lumbar interbody fusion (ALIF) is one of the most common spine procedures, indicated for a variety of conditions including lumbar radiculopathy, malignancy, trauma, and deformity. 1 By providing direct visualization of the anterior spinal column, ALIF allows for optimal endplate preparation for arthrodesis and avoids paraspinal muscle trauma. 1 As a result, the utilization of ALIF has increased over the past decade, with rates rising from 7.9% to 10.5% between 2010 and 2019, and this trend is expected to continue with the aging population.1,2
Despite its advantages, ALIF carries a significant complication profile. Common complications include venous injury, retroperitoneal bleeding, retrograde ejaculation, thrombosis, incisional hernia, and ileus. 3 This heightened risk is largely due to the anterior retroperitoneal access, which entails greater exposure to vasculature, visceral organs, and the genitourinary system. Patient risk factors for complications and poor clinical outcomes include obesity, diabetes mellitus, hypertension, smoking, previous retroperitoneal surgery, and preoperative anemia. 4
Given the risks of vascular injury, hemorrhage, and thrombosis during ALIF, understanding the impact of a preoperative primary hypercoagulable disorder is crucial. These disorders, including Factor V Leiden Deficiency, Prothrombin gene mutation, Hereditary Protein C&S Deficiency, lupus anticoagulant, and antiphospholipid syndrome are relatively common, with an estimated prevalence of 1%–5% in the general population. 5 It has been well established that the presence of these disorders increases the risk of venous thromboembolism (VTE) following surgery, with studies reporting its presence in up to 20% of patients with VTE.6,7 Furthermore, recent research has demonstrated that hypercoagulable disorders significantly elevate the risk of complications, including surgical site infections, pulmonary embolism, and myocardial infarctions, following various spine surgeries, including posterior lumbar fusion, anterior cervical discectomy and fusion, and posterior cervical laminectomy and fusion.8-11 However, there is a gap in the literature regarding the effects of these disorders on the outcomes of ALIF.
The objective of this retrospective study is to examine the effects of primary hypercoagulable disorders on complication rates following ALIF. Additionally, we aim to compare the complications of ALIF in hypercoagulable patients with those who undergo posterior lumbar fusion to assess the relationship between complication risk and fusion approach. We hypothesize that patients with hypercoagulable conditions will be at an increased risk of postoperative complications compared to those with normal coagulation profiles, and that this risk will be greater for patients undergoing ALIF than posterior fusion.
Methods
Data Source and Study Population
The PearlDiver Mariner Database (PearlDiver Technologies, Fort Wayne, IN, USA) was queried for patients who underwent anterior lumbar interbody fusion (ALIF) between 2010 and 2022. PearlDiver is a comprehensive nationwide dataset containing approximately 157 million deidentified patient records that includes demographics, diagnostic, and procedural data from all payer types and inpatient and outpatient settings. Due to the use of anonymized PearlDiver data and this study’s retrospective nature, informed consent was waived and Institutional Board Review approval was not required.
Identification of Study Cohorts
International Classification of Disease (ICD) ninth (ICD-9) and 10th (ICD-10) edition and Current Procedural Terminology (CPT) codes were used to identify patients (Supplemental Table 1). The query included patients who underwent 1 to two-level ALIF with or without posterior instrumentation. Patients were further stratified based on the diagnosis of at least 1 primary hypercoagulability disorder, including, Factor V Leiden deficiency, prothrombin gene mutation, hereditary Protein C&S deficiency, antiphospholipid syndrome, and lupus anticoagulant. Additionally, to assess anticoagulation utilization in hypercoagulable patients undergoing ALIF, data on anticoagulation use, type (Aspirin, Clopidogrel, low molecular weight heparin, unfractionated heparin, Warfarin, and Factor Xa inhibitors), and timing (from preoperative day 2 to postoperative day 2) were retrieved.
For the secondary analysis, we identified patients with hypercoagulable disorders who underwent a one-level ALIF with or without one-level posterior instrumentation, as well as those who underwent a one-level posterior lumbar interbody fusion (PLIF) or transforaminal lumbar interbody fusion (TLIF).
Exclusion criteria included age <18 years, rheumatoid arthritis, cauda equina syndrome, <90 days follow-up, and surgical indications for trauma, malignancy, or infection. Patient characteristics (ie, age, ECI, sex) and rates of comorbidities were collected and compared between ALIF patients with and without a hypercoagulable disorder.
Primary Endpoints
The primary endpoints were to characterize the prevalence of hypercoagulable disorders among ALIF patients, evaluate anticoagulation utilization rates (including type and timing), and assess the 30-day risks of postoperative complications, all-cause readmissions, and revision rates at two- and 5-year intervals in this patient population compared to those with a normal coagulation profile.
The secondary endpoints included comparisons of the 30-day risks of medical and surgical complications, readmissions, and revision rates between hypercoagulable patients undergoing one-level ALIF and those undergoing one-level posterior lumbar fusion.
Medical complications included deep vein thrombosis (DVT), pulmonary embolism (PE), arterial embolism/thrombosis, pneumonia, transfusion, blood loss anemia, myocardial infarction (MI), acute kidney injury (AKI), sepsis, stroke, and surgical site infection (SSI). Surgical complications include retroperitoneal hematoma, epidural hematoma, superficial hematoma, deep infection, durotomy, and debridement. An aggregate of all hematoma types was combined to form the “aggregate hematoma” complication group.
Statistical Analysis
The student’s t-test and Pearson chi-squared test of independence were used to compare continuous and categorical variables, including patient demographics, Elixhauser Comorbidity Index (ECI), and hospital length of stay (LOS). To compare outcomes between hypercoagulable- and non-hypercoagulable patients undergoing ALIF, multivariate logistic regression analysis was utilized with age, ECI, gender, multi-level ALIF, and number of posterior levels fused included as covariates. To compare hypercoagulable patients undergoing 1 level ALIF vs 1 level posterior fusion, multiple logistic regression with age, gender, and ECI was employed.
All statistical analyses were conducted using RStudio (Version 4.4.2) within the PearlDiver Mariner Database program. A p-value <0.05 indicates statistical significance.
Results
Demographics
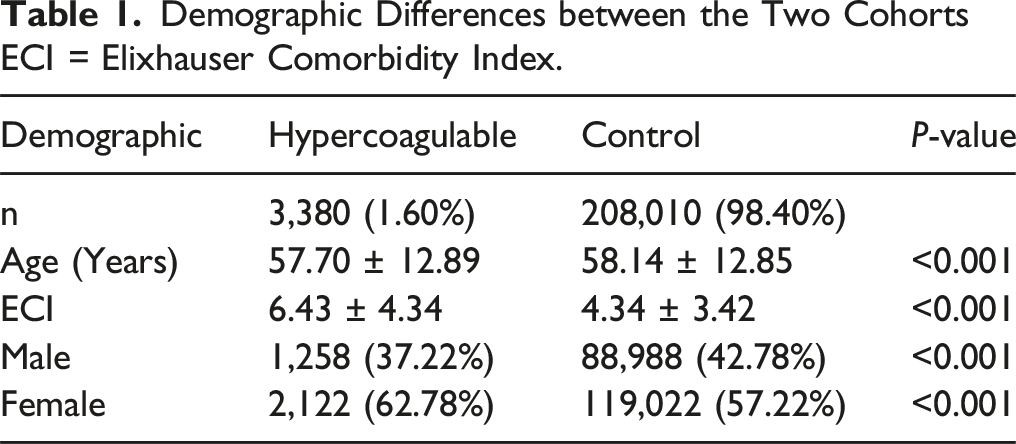
Demographic Differences between the Two Cohorts ECI = Elixhauser Comorbidity Index.
Anticoagulation Utilization among Hypercoagulable Patients
Utilization of VTE Prophylaxis Separated By Time of Administration and Anticoagulation Type.
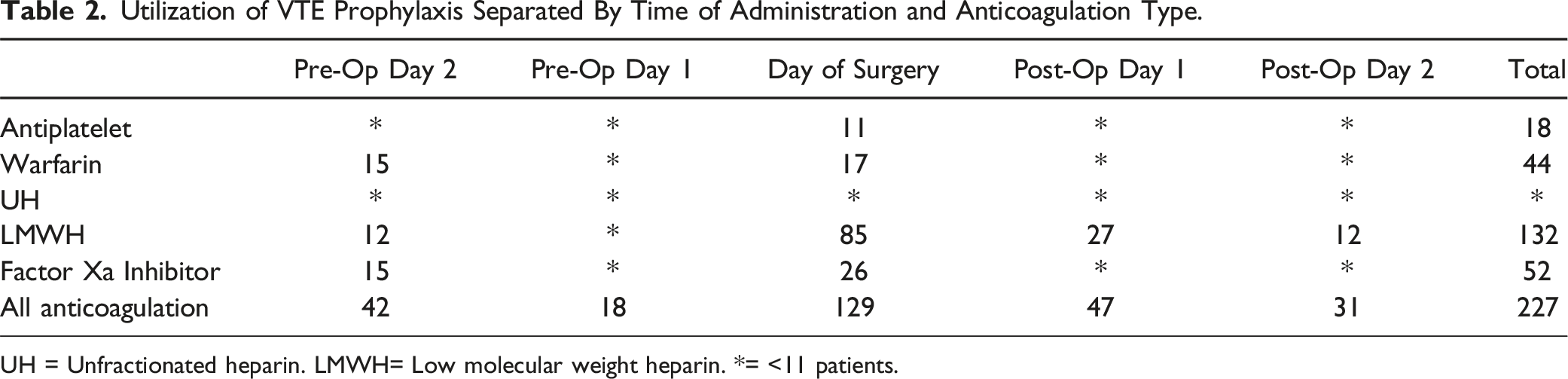
UH = Unfractionated heparin. LMWH= Low molecular weight heparin. *= <11 patients.
Complications following ALIF in Hypercoagulable Patients
Multiple Logistic Regression Analysis Outcomes between Hypercoagulable and Control Patients Following ALIF.
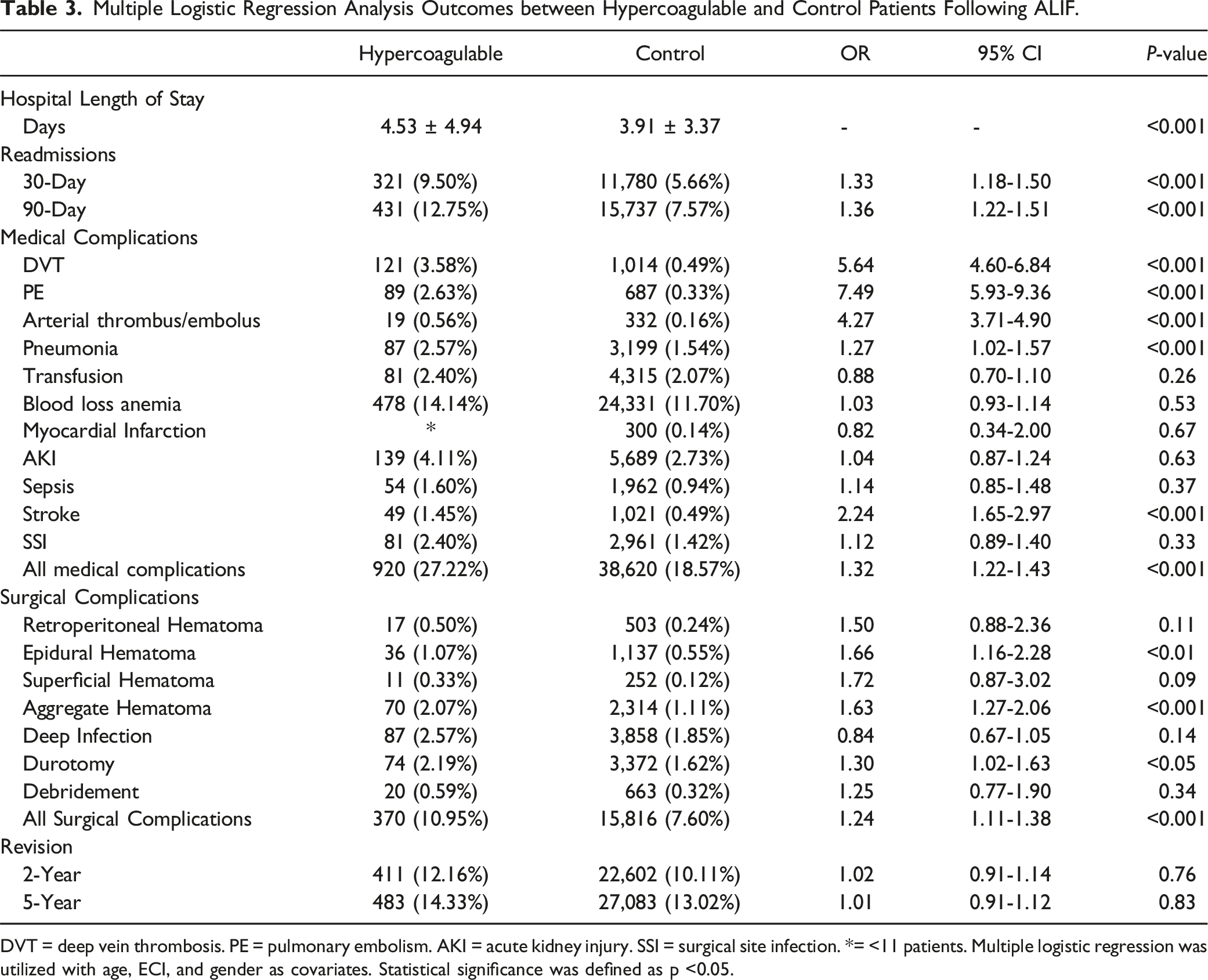
DVT = deep vein thrombosis. PE = pulmonary embolism. AKI = acute kidney injury. SSI = surgical site infection. *= <11 patients. Multiple logistic regression was utilized with age, ECI, and gender as covariates. Statistical significance was defined as p <0.05.
For 30-day medical complications, hypercoagulable patients had increased risks for DVT (OR: 5.64, [4.60-6.84], P < 0.001), PE (OR:7.49, [5.93-9.36], P < 0.001), arterial embolism/thrombosis (OR: 4.27, [3.71-4.90], P < 0.001), pneumonia (OR: 1.27, [1.02-1.57], P < 0.05), stroke (OR: 2.24, [1.65-2.97], P < 0.001), and overall medical complications (OR: 1.32, [1.22-1.43], P < 0.001) (Table 3).
Among surgical complications, risks were also higher for epidural hematoma (OR: 1.66, [1.16-2.28], P < 0.01), aggregate hematoma (OR: 1.63 [1.27-2.06])], durotomy (OR: 1.30, [1.02-1.63], P < 0.05), and overall 30-day surgical complications (OR: 1.24, [1.11-1.38], P < 0.001).
No significant differences were found in revision rates at two- and 5-years.
ALIF vs Posterior Lumbar Fusion in Hypercoagulable Patients
Multiple Logistic Regression Analysis for Outcomes Between Hypercoagulable Patients Following ALIF vs Posterior Fusion.
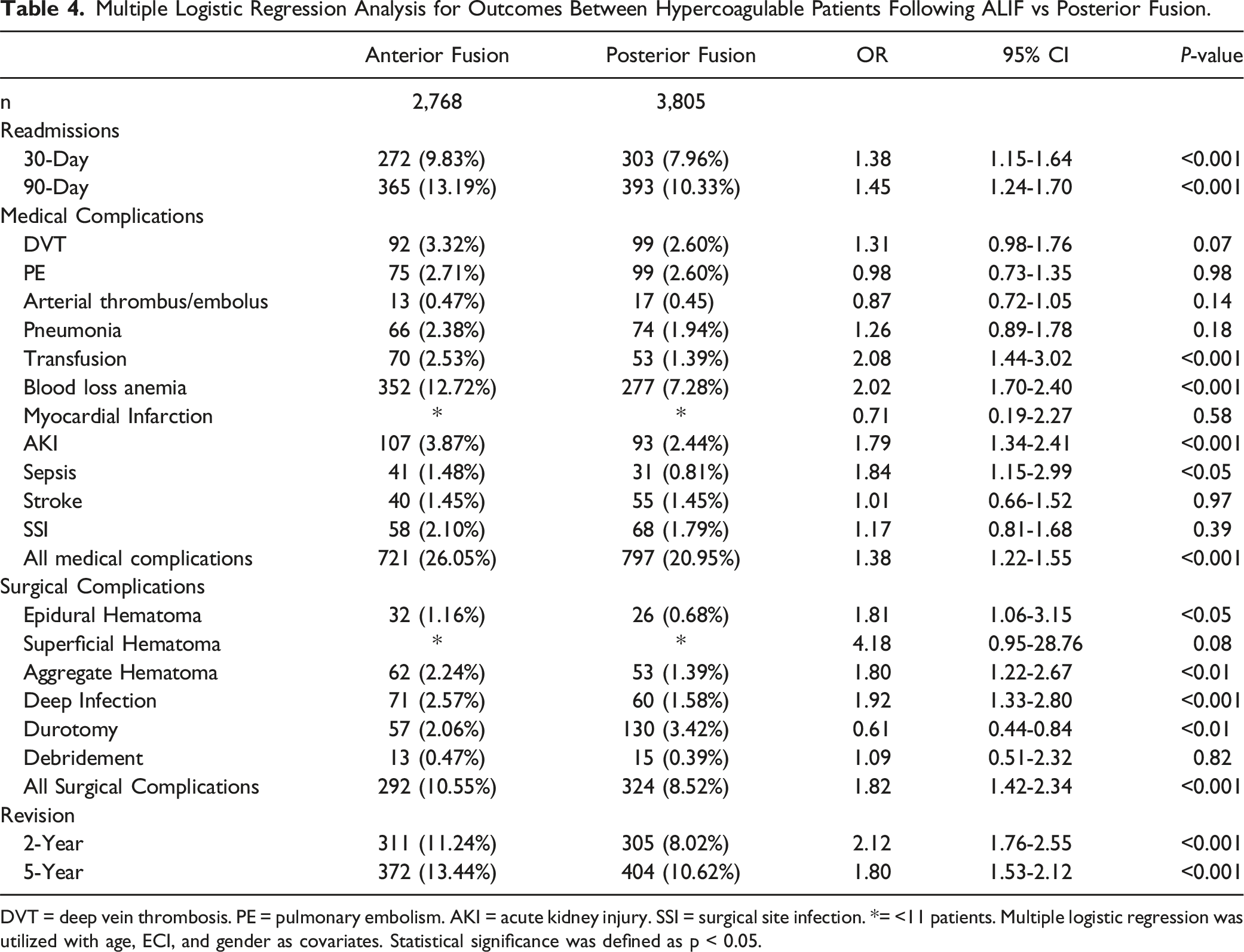
DVT = deep vein thrombosis. PE = pulmonary embolism. AKI = acute kidney injury. SSI = surgical site infection. *= <11 patients. Multiple logistic regression was utilized with age, ECI, and gender as covariates. Statistical significance was defined as p < 0.05.
Regarding medical complications, ALIF was associated with higher risks for transfusions (OR: 2.08, [1.44-3.02]), blood loss anemia (OR: 2.02 [1.70-2.40]), AKI (OR: 1.79, [1.34-2.41]), sepsis (OR: 1.84, [1.15-2.99]), and overall 30-day medical complications (OR:1.38, [1.22-1.55]) (P < 0.001) (Table 4).
Regarding surgical complications, ALIF patients had greater risks for epidural hematoma (OR: 1.81, [1.06-3.15]), deep tissue infection (OR: 1.92, [1.33-2.80]), and overall 30-day surgical complications (OR: 1.82, [1.42-2.34]) (P < 0.001) (Table 4). However, ALIF patients had lower risk for durotomy (OR: 0.61, [0.44-0.84], P < 0.01).
Hypercoagulable patients who underwent ALIF were at higher risk for revision surgery 2-years (OR: 2.12, [1.76-2.55]) and 5-years (OR: 1.80, [1.53-2.12]) (P < 0.001) after the index procedure.
Discussion
The outcomes of ALIF in patients with hypercoagulable disorders have not been well characterized. In this study, we identified 3380 (1.60%) patients with hypercoagulable disorders who underwent ALIF, with only 6.72% receiving anticoagulation therapy. As hypothesized, these patients experienced longer hospital stays and increased risks of hospital readmissions, DVT, PE, pneumonia, neurologic complications, durotomy, and epidural hematoma compared to those with normal coagulation profiles. Furthermore, compared to hypercoagulable patients undergoing posterior fusion, the anterior approach was also associated with elevated risks of readmissions and complications, including transfusions, blood loss anemia, AKI, sepsis, epidural hematoma, and deep infections. This study is the first to demonstrate that the anterior approach to interbody fusion places hypercoagulable patients at increased risk for poor outcomes.
These findings are consistent with existing literature documenting elevated complication risks in hypercoagulable patients undergoing spine surgery. For instance, Puvanesarajah et al 11 reported higher rates of VTE, medical complications, infections, same-day transfusions, and 2-year reoperation rates following posterior lumbar fusion. Bronheim et al 10 documented increased transfusion rates, septic shock, and cerebrovascular accident following cervical laminectomy and fusion. However, this study specifically highlights ALIF outcomes in this high-risk population, filling a critical gap in the literature.
Our results confirm that hypercoagulable disorders are independent risk factors for PE and DVT following ALIF. Hematologic studies have linked conditions such as Factor V Leiden to elevated risks of VTE, which are further exacerbated by postoperative immobility. 12 Despite these risks, we found that only a small proportion of this patient population received perioperative anticoagulation therapy, highlighting potential gaps in care. This emphasizes the lack of specific and standardized guidelines for VTE prophylaxis in high-risk patients undergoing ALIF, as current recommendations remain vague and largely rely on surgeon discretion. 13 More specifically, the North American Spine Society (NASS) suggests that chemoprophylaxis may be considered only for long and complex surgeries, such as anterior or combined anterior-posterior approaches, and in patients with known thromboembolic risk factors. 14 Similarly, the American College of Chest Physicians (ACCP) advises a combination of mechanical and chemical prophylaxis for high-risk patients. 15 However, these guidelines do not provide clear recommendations on specific regimens, which likely contributes to the inconsistent use of anticoagulation observed in our study.
Furthermore, the timing of VTE prophylaxis is also poorly defined by NASS and ACCP guidelines. While 1 study recommends initiating thromboprophylaxis 6 to 9 hours after elective spine surgery, this suggestion is based on data that includes other orthopaedic procedures. 16 Our findings indicate that when surgeons use VTE prophylaxis, their practice aligns with this recommendation, as anticoagulation therapy was most commonly initiated on the day of surgery.
It is however essential to acknowledge that VTE prophylaxis carries inherent risks, as suggested by our findings of increased epidural hematoma rates in hypercoagulable patients. Cunningham et al found a higher incidence of epidural hematoma in patients receiving preoperative DVT prophylaxis, which, although rare, can lead to rapid neurologic deterioration.17,18 This underscores the challenge spine surgeons face in balancing the risk of neurological injury from epidural hematomas with the morbidity and mortality associated with VTE. Spine surgeons should strongly consider postoperative prophylaxis in this patient population, as suggested by our findings, the almost 8-fold risk of PE likely outweighs the risk of epidural hematoma. This is particularly true in ALIF cases that also involve direct posterior decompression, as circumferential lumbar fusions, and multi-level decompression are risk factors for VTE following degenerative spine surgery. 19
It is important to note that we did not find a difference in revision rates between the hypercoagulable and control cohorts, suggesting that although these patients face risk for poor short-term outcomes, long-term outcomes are not affected. Puvanesarajah et al 11 similarly found no difference in revision rates between patients with bleeding disorders and control patients who underwent posterior lumbar fusion.
Interestingly, when compared to the posterior approach, hypercoagulable patients undergoing ALIF demonstrated a higher risk of complications, despite a lower risk of durotomy. By directly comparing surgical approaches, we have shown that the elevated complication profile is associated with the anterior approach itself and not merely a consequence of undergoing surgery. Notably, posterior fusions are often used for multi-level procedures, whereas ALIF is typically reserved for one- to two- level surgery. By limiting our analysis to single-level procedures, we effectively controlled for this potential confounder. The higher risk of epidural hematoma with ALIF may, in part, be attributed to earlier initiation of VTE prophylaxis, as surgeons may have less concern for epidural bleeding in the anterior approach compared to the posterior procedures. 20 Furthermore, the significantly elevated revision rates observed at 2- and 5- years following ALIF highlight the long-term consequences of this approach in hypercoagulable patients. While prior studies have shown increased complication risks with posterior fusions in this cohort, our findings indicate that posterior fusion remains the safer option for hypercoagulable patients when compared to ALIF.9,11
This study is not without limitations. As it relies on the PearlDiver national database, the accuracy of patient identification depends on correct coding. As a result, the actual number of patients with a hypercoagulable disorder who underwent ALIF may be underreported. Additionally, we were unable to control for the type of graft material used in the fusion, which could impact outcomes. The use of de-identified databases does not account for surgeon preference or variability in surgical skill, both of which could influence complication and readmission rates. Furthermore, the small sample size limits our ability to perform a sub-analysis to evaluate the specific effects of individual hypercoagulable disorders, even though these conditions likely carry varying risks for clot formation. Similarly, the low number of patients who received VTE prophylaxis prevented us from evaluating its impact on this population. Lastly, since this database reports real world data, we were unable to control for surgeons who implemented ERAS protocols for DVT prophylaxis.
Conclusion
This study emphasizes the significant risks of medical and surgical complications faced by hypercoagulable patients undergoing ALIF. Despite the recognition of these risks, the low utilization of perioperative anticoagulation therapy suggests gaps in current clinical practice and highlights the need for more precise guidelines. The findings also suggest that posterior lumbar fusion may offer a safer alternative for this high-risk group. Future research should establish comprehensive evidence-based protocols for VTE prophylaxis to ensure consistent and effective care for hypercoagulable patients undergoing spine surgery.
Supplemental Material
Supplemental Material - Complications and Clinical Outcomes of Anterior Lumbar Interbody Fusion in Patients With Primary Hypercoagulable Disorders
Supplemental Material for Complications and Clinical Outcomes of Anterior Lumbar Interbody Fusion in Patients With Primary Hypercoagulable Disorders by Henry Avetisian, Will Karakash, Maya Abu-Zahra, Chimere Ezuma, Mirbahador Athari, Dil Patel, Jeffrey C. Wang, Raymond J. Hah, and Ram K. Alluri in Global Spine Journal
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Henry Avetisian, Will Karakash, Maya Abu-Zhara, Chimere Ezuma, Mirbahador Athari, and Dil Patel have nothing to disclose. Jeffrey C. Wang has received intellectual property royalties from Zimmer Biomet, NovApproach, SeaSpine, and DePuy Synthes. Raymond J. Hah has received grant funding from SI bone, consulting fees from NuVasive, and support from the North American Spine Society to attend meetings. Ram K. Alluri has received grant funding from NIH, consulting fees from HIA Technologies, and payment from Eccential Robotics for lectures and presentations.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Statement
ORCID iDs
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
