Abstract
Study Design
Randomized controlled trial.
Objectives
To compare the effect and safety of 2 anesthetic methods using in the operation of Transforaminal Endoscopic Lumbar Discectomy.
Methods
From the January of 2020 to the December of 2021, 230 consecutive patients that underwent TELD were applied with two methods of anesthesia. All the patients were divided into two groups. The Monitored Anesthesia Care (MAC) group used the local anesthesia (LA) with MAC that based on the combination of dexmedetomidine and butorphanol tartrate. The LA group used the local anesthesia only. Then the Visual Analogic Scale (VAS) through the operating period was compared between the two groups at the time points of before operation (T0), inserting of the puncture needle (T1), establishing of the working cannula (T2), excision of the fibrous rings (T3) and immediately postoperatively (T4). Also, the satisfaction degree of the patients for the course of the operations and the occurrence of the complications were compared between the two groups.
Results
There were no differences of the VAS around the operating area at the time point of T0. Then the MAC group expressed lower scores at all other points of T1, T2, T3 and T4. Then the satisfaction degree of the MAC group was superior than the LA group. No difference was observed for the occurrence of the complications.
Conclusions
MAC based on the combination of dexmedetomidine and butorphanol tartrate is an ideal method of anesthesia for TELD with enough effect and safety.
Keywords
Introduction
In the past two decades, 1 Transforaminal Endoscopic Lumbar Discectomy (TELD) has been proved to be an effective and safe method for the treatment of Lumbar Disc Herniation.2–4 Compared with the conventional operations, such as the usual discectomy and micro endoscopic discectomy, TELD has the advantages of less invasion, shorter stays in the hospital, quicker returning to work, less complications and less costs.
Even with the advantages above, there were still some questions which were still waiting for improvement about TELD. Especially, the most suitable analgesic method for TELD was still with controversial. Several researches have tried different methods and compared the effects and safety. In the current article, we introduced Monitored Anesthesia Care (MAC) mode into the curse of TELD, the mode was based on the combination of dexmedetomidine and butorphanol tartrate to strength the effect of local anesthesia (LA). According to our experience, this method could satisfy enough to TELD and ensure the patients remain comfortable without severe complications.
Materials and Methods
Patient Selection
The prospective comparison was conducted in the consecutive patients who underwent TELD between January 2020 to December 2021. The method of anesthesia used for every patient was applied randomly. This study was performed in line with the principles of the Declaration of Helsinki and the approval was granted by the Ethics Committee of General Hospital of Northern Theater Command (2019.12.5/(2019) 798). All the patients signed informed consent forms. The treatment group was named MAC group as the abbreviation of Monitored Anesthesia Care, the operations of this group were undergone using the anesthesia of LA with MAC, whichbased on the combination of dexmedetomidine and butorphanol tartrate. The control group was named as LA group as the abbreviation of Local Anesthesia, which used the local anesthesia only. All the operations were carried out in the same hospital by the same surgeon.
The inclusion criteria were: (1) with the symptoms of radiating pain in line with the Magnetic Resonance Imaging (MRI) and Computerized Tomography (CT) related to only one segment LDH, (2) had experienced conservative treatment at least 1 month but without obvious effect, (3) with complete clinical and radiological data both pre- and post-operative. The exclusion criteria were: (1) with the history of previous operation in the lumbar spine, (2) the patients that could not ensure the operation of TELD and had to change the operating method.
Operative Techniques and the Method of Anesthesia
All the operations were carried out with the standard prone position. The C-arm fluoroscope was applied to confirm the target intervertebral space and marked. After local anesthesia of the skin and the trajectory with 1% lidocaine, the puncture needle was inserted to the superior articular process. The position of the needle was adjusted with the help of the C-arm fluoroscope. In our experience, the C-arm fluoroscope was enough to confirm the position of the needle for most patients. Rarely, when there was difficultness for induce the needle, the dynamic view was considered. After that, the following operations were carried out as the standard percutaneous transforaminal endoscopic spine system. 5 As the standard percutaneous transforaminal endoscopic system introducing, the foraminoplasty was performed if necessary. Then, after cutting appropriate area of the annulus fibrosus, the nucleus pulposus was removed gradually.
For the anesthesia, two different methods were applied. In the LA group, only the local anesthesia with 1% lidocaine was inserted throughout the trajectory and around the operating area. For the MAC group, a combined method of anesthesia was implemented on the basis of LA. The protocol of the method was concluded as Figure 1. Approximately, the whole process of the operation was divided into 3 phases as preparation, pre-operation and operation. In the phase of preparation, the dexmedetomidine was injected intravenously as the dosage of 1 μg/kg and maintained for 15 min. Then, the phase of pre-operation was followed. In this phase, the position of the patient should be placed properly and the channel of the endoscope should be established precisely according to the need of the operation. 1-2 mg of butorphanol tartrate was used intravenously at the beginning of this phase, then the 1% lidocaine was used as the same method of the LA group. After the establishment of the channel, the endoscope was introduced to the operation area and the phase of the operation began to excise the discectomy. In this process, the dexmedetomidine was maintaining intravenously as the dosage of 1 μg/kg and stopped as the requirement of the surgeon. The methods of anesthesia using in the two groups.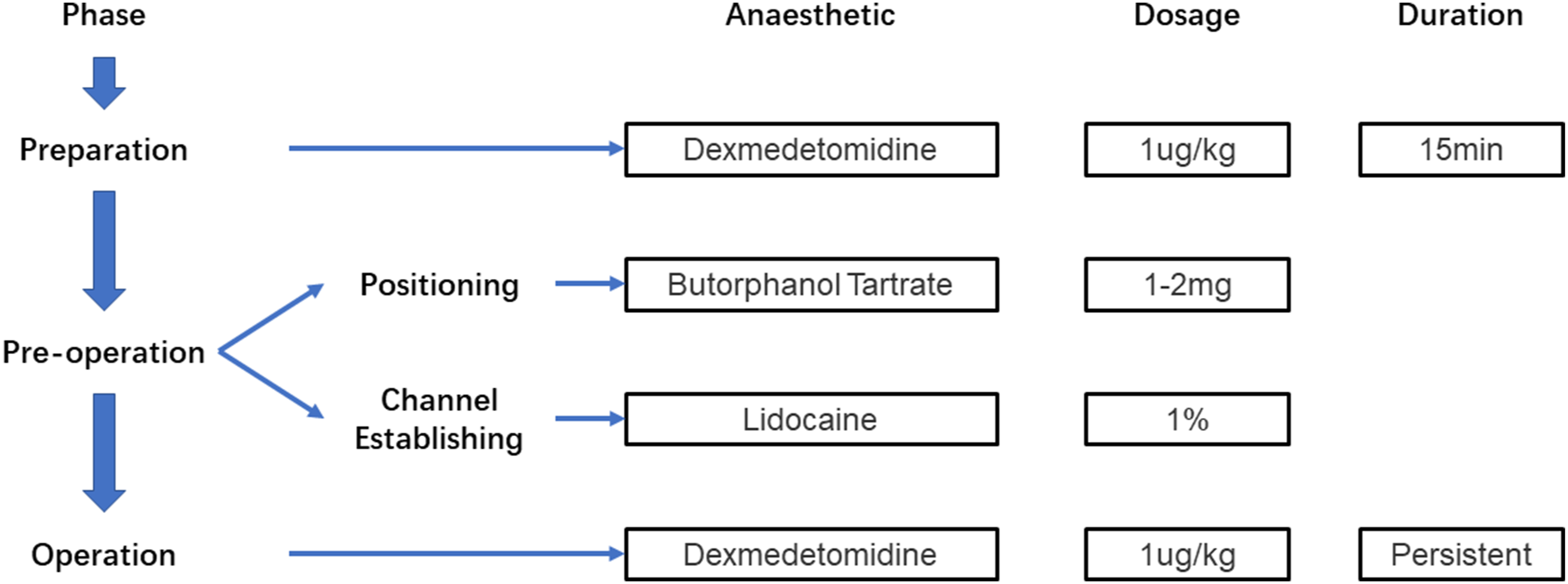
Post-Operative Management
The treatments post-operatively were the same for all the patients as function exercises, using of analgetic, dressing change every 3-4 days.
Clinical Data
All the patients were evaluated with the Visual Analogic Scale (VAS) for pain of the low back around the operating area. The evaluating timepoints were set as following, beginning of the operations (T0), inserting of the puncture needle (T1), establishing of the working cannula (T2), excision of the fibrous rings (T3) and immediately postoperatively (T4). Meanwhile, the satisfaction during the operation was judged by the patients using a points-scoring system from 1-10. The point of 10 corresponds to most satisfactory and the point of 1 corresponds to most dissatisfactory. The complications were recorded and compared between the two groups including the injury of the nerve root, leakage of cerebrospinal fluid, infection and minor complications such as paralysis of the limbs.
Statistical Analysis
GraphPad Prism 8.0.2 (GraphPad Software Inc., San Diego, CA, USA) was used for statistical analyses. The data were compared between the two groups as the repeated measurements. Chi-square test was used to compare the counting parameters. P < .05 was set as the statistical significance.
Results
Baseline Demographics
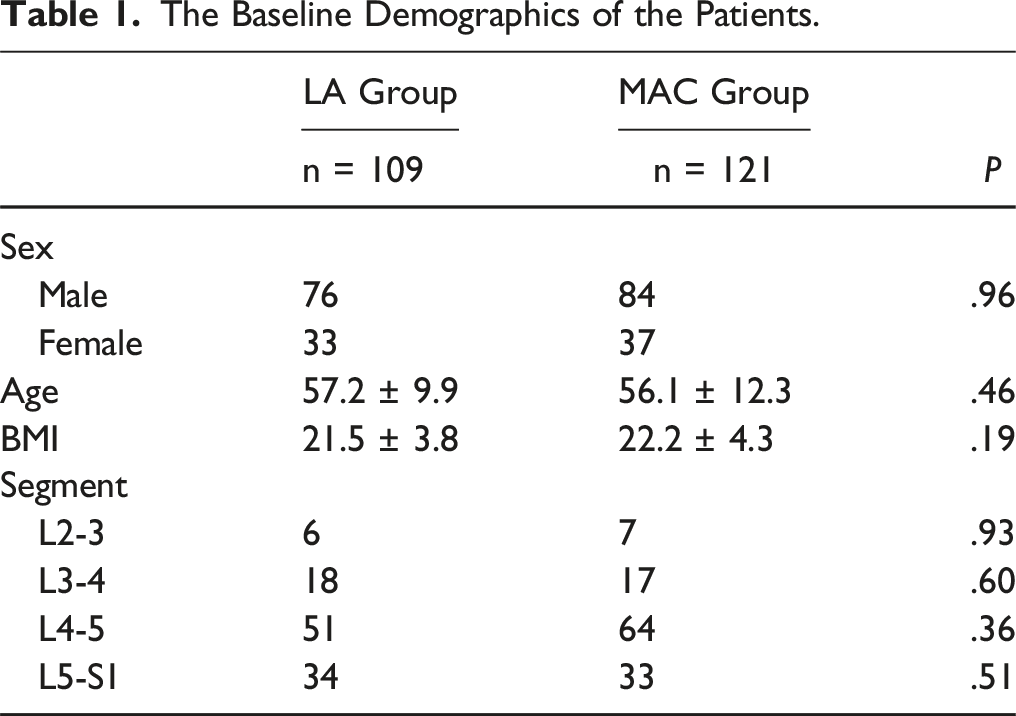
The Baseline Demographics of the Patients.
VAS of the Back Pain
The VAS scores around the operating area were compared between the two groups at the time points. The results showed that there were no differences at the time point of T0. Then the MAC group expressed lower scores at other points as T1, T2, T3 and T4. (Figure 2). The compare of the VAS scores around the operating area at different time points. Every time point corresponded to the beginning of the operations (T0), inserting of the puncture needle (T1), establishing of the working cannula (T2), excision of the fibrous rings (T3) and immediately postoperatively (T4). *means there was difference between the two groups with the P < .05.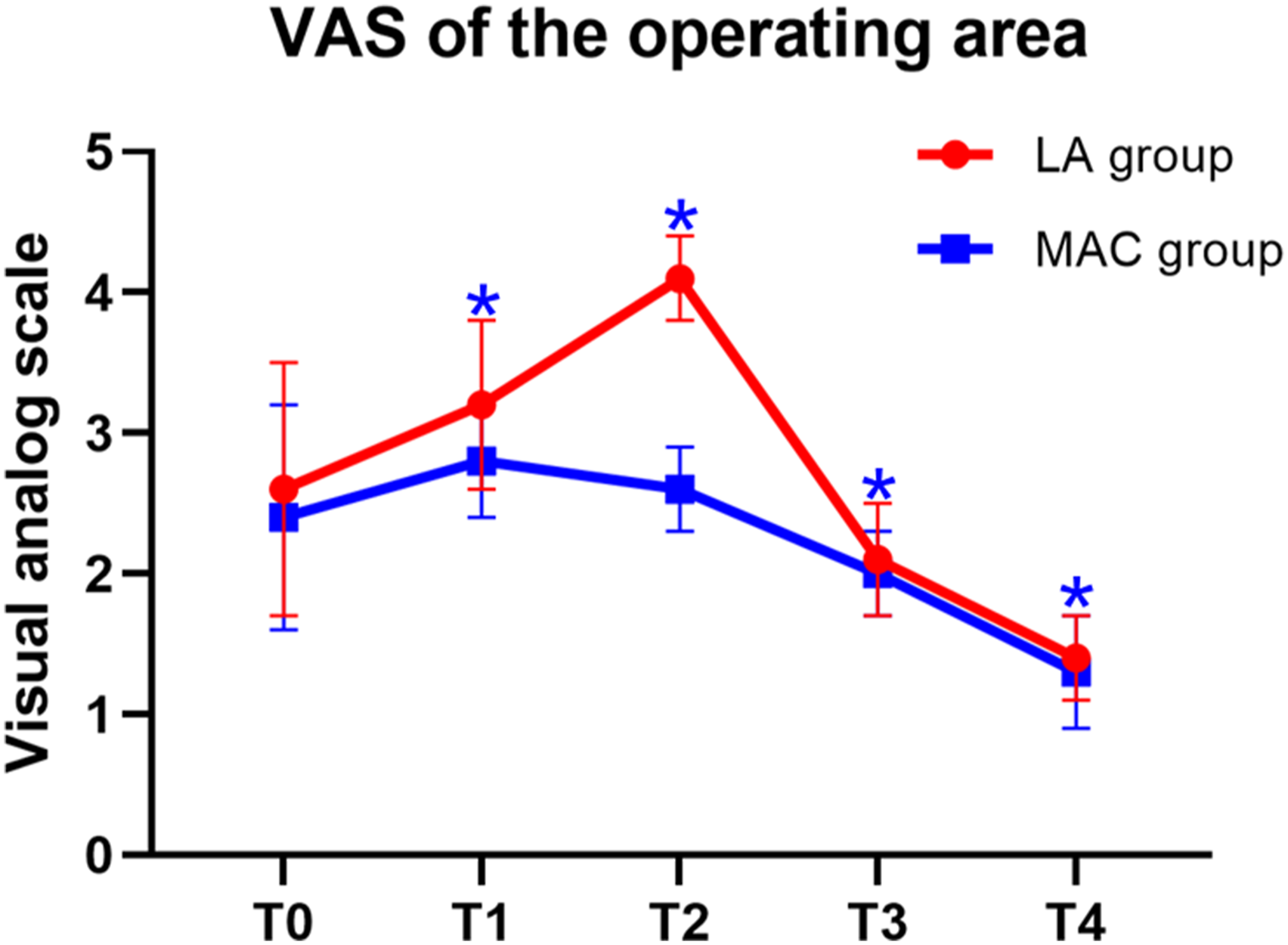
Degree of Satisfaction
The satisfactory degree of the MAC group (9.4 ± 1.8) was obviously superior than the LA group (8.9 ± 1.7) (P < .05).
The Occurrence Rates of Complications
No serious complications were recorded in both groups. Only 2 case of transient paralysis in the limbs was observed in the LA group and 1 cases in the MAC group, without difference.
Discussion
Operations should be applied to the patients if the conservative managements fail to relieve the symptoms. With the development of the minimally invasive spine surgery, 6 TELD has been proved to be the appropriate method to treat the LDH with ideal effectiveness and safety.
Suitable method of anesthesia is important to TELD. As a minimally invasive operation, the TELD needs an ideal anesthesia which should consider the requirements of the surgeons and the patients, which include enough effect of reducing the pain throughout the whole operation, also the reservation of the consciousness for the patients to alert the abnormity of the lower limbs during the operation. Normally, the local anesthesia could ensure enough effect during the course of the operation. But occasionally, the irregular irritating might bring terrible feeling to the patients. Even more seriously, some sensitive or nervous patients might move the lower limb or the body uncontrollabl. These movements could bring dangerous to the patients and disturbed the surgeons who were operating attentively in the narrow fields. Many researchers have made effort to improve the method of the anesthesia using for TELD. Also, when the patients felt pain in the operation, more LA had to be applied. That could complicate the operations and bring uncomfortableness to both the surgeons and the patients. Under some conditions, some patients had to convert to general anesthesia.
More than one papers of meta-analysis have concluded initially that Epidural Anesthesia (EA) may be a safe and effective method for TELD with better clinical results. Meanwhile, the authors suggested that more high-quality researches should be implemented.7,8 Also with this anesthesia, some complications associated with EA still worried the surgeons such as the injury of the dural sac and the nerve root, retention of urine. Also, the course of EA may prolong the operation and increase the risk of infection since the puncture area is around the operation field. In order to simplify the operation course, some surgeons tried the method of conducting EA via the intervertebral foramen 9 or injecting the anaesthetic into the intervertebral disc. 10 All these methods could get enough effect for TELD, but could not avoid the complications. More important, the anesthesia based on EA could not ensure the immediate reaction of the limbs needed by the surgeons. Though more surgeons have gained enough confidence to perform PELD under general anesthesia, most surgeons still feel comfortable with the patients keep awake or sedated. Also, in order to reveal the advantages of TELD as a kind of minimally invasive surgery, the general anesthesia should be avoided. Meanwhile, some aged patients and the patients with medical diseases which could not tolerant general anesthesia could benefit from our method.
Other researches have tried the method of adding anesthesia effect using intravenous medication. Gadjradj et al 11 used dexmedetomidine as sedative during the operation of Percutaneous Transforaminal Endoscopic Discectomy (PTED) on the base of LA. The results showed that LA added with conscious sedation could provide ideal effect and yield high satisfactionfrom both the surgeons and the patients. Also, some researches referred to other usages of anesthetics such as preemptive analgesia (PA), 12 or even general anesthesia. 13 As motioned above, these methods often are related to adverse events caused by the anesthesia itself. So, it seemed some improvements should be applied to change the methods of anesthesia in the operation of TELD. Some retrospective comparative researches have approved that the combination of different kinds of anesthetic might ensure the effect of anesthesia and avoid the adverse effect meanwhile.
In the current research, we tried the combination of dexmedetomidine and butorphanol tartrate as the anesthetics to TELD. The results showed that this combination could ensure the effect and safety of the operation. Also, the mode of MAC gives the surgeons a chance to invite the anesthetists into the operation. The anesthetists could control of the pain effectively, adjust the using of anesthetics timely and keep the vital signs constantly during the operation. The help of the anesthetists is important for the surgeons performing the operation successfully and safely.
Above all, we concluded that the mode of MAC based on the combination of dexmedetomidine and butorphanol tartrate is an ideal method of anesthesia for TELD.
Footnotes
Acknowledgements
We should appreciate all the participants of the current research and wish them good recovery.
Author Contributions
All authors contributed to the study conception and design, especially Yu Chen and Hai-long Yu. Material preparation, data collection was performed by Shuang Wang and Hong Wang, then the data were analyzed by Shuang Wang, Liang Zheng, Xiao Yang and Jun-xiong Ma. Also, the three first authors wrote the first draft of the manuscript. Liang-bi Xiang revised the manuscript and corrected it. Then the Correspondence author Yu Chen and Hai-long Yu determined the final version. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The current research was supported by a grant from the Applied Basic Research Programs of Liaoning Province (2022020777-JH2/1015, SW).
