Abstract
Study Design
Multicenter cohort.
Objectives
A report from the International Spine Study Group (ISSG) noted that surgeons failed to achieve alignment goals in nearly two-thirds of 266 complex adult deformity surgery (CADS) cases. We assess whether personalized interbody spacers are associated with improved rates of achieving goal alignment following adult spinal deformity (ASD) surgery.
Methods
ASD patients were included if their surgery utilized 3D-printed personalized interbody spacer(s) and they met ISSG CADS inclusion criteria. Planned alignment was personalized by the surgeon during interbody planning. Planned vs achieved alignment was assessed and compared with the ISSG CADS series that used stock interbodies.
Results
For 65 patients with personalized interbodies, 62% were women, mean age was 70.3 years (SD = 8.3), mean instrumented levels was 9.9 (SD = 4.1), and the mean number of personalized interbodies per patient was 2.2 (SD = .8). Segmental alignment was achieved close to plan for levels with personalized interbodies, with mean difference between goal and achieved as follows: intervertebral lordosis = .9° (SD = 5.2°), intervertebral coronal angle = .1° (SD = 4.7°), and posterior disc height = −0.1 mm (SD = 2.3 mm). Achieved pelvic incidence-to-lumbar lordosis mismatch (PI-LL) correlated significantly with goal PI-LL (r = .668, P < .001). Compared with the ISSG CADS cohort, utilization of personalized interbodies resulted in significant improvement in achieving PI-LL <5° of plan (P = .046) and showed a significant reduction in cases with PI-LL >15° of plan (P = .012).
Conclusions
This study supports use of personalized interbodies as a means of better achieving goal segmental sagittal and coronal alignment and significantly improving achievement of goal PI-LL compared with stock devices.
Keywords
Introduction
As the population in most developed countries continues to shift toward an older demographic, the health problems that afflict the elderly will become increasingly more prevalent and in need of care. The prevalence of adult spinal deformity (ASD) has been estimated to be as high as 60% among the older population. 1 ASD can profoundly impact the health of those affected, including through back and leg pain, weakness, myelopathy, disability, and mobility issues.2–7 Many individuals with symptomatic ASD may be temporized with nonoperative treatments, but when these therapies fail to provide adequate relief, patients may seek operative care. 8 Although a growing number of reports support the potential for operative treatment to provide significant benefit for symptomatic ASD,6,7,9-18 these procedures are often complex and continue to be associated with high rates of complications.17,19-24 Mechanical complications, including proximal junctional kyphosis/failure (PJK/PJF) and rod fracture, are by far the most common complications, especially with longer-term follow-up.12,25
The goals of surgical treatment for ASD broadly include decompression of neural elements, correction of malalignment, and typically creation of a construct with durable mechanical stability that will promote solid bony arthrodesis. Although the first objective may be relatively clear and straightforward, the other 2 objectives are intertwined and their optimal achievement remains a matter of research and debate. Multiple studies have shown that correction of malalignment promotes better patient outcome and reduces risk of mechanical complications. However, there remains considerable controversy regarding what constitutes optimal goals for spinal alignment in ASD surgery. Nevertheless, regardless of the chosen strategy, the surgeon has an increasing array of sophisticated software tools to meticulously plan the desired goals for spinal realignment prior to entering the operating room.
Despite being armed with a detailed surgical plan for realignment, recent reports suggests that even among experienced deformity surgeons, it remains challenging to achieve the preoperative goal alignment in ASD surgery.26,27 Smith and colleagues, 27 through the International Spine Study Group (ISSG), assessed whether the surgeon’s preoperative goals for sagittal alignment following ASD surgery were achieved in 266 complex adult deformity surgery (CADS) cases. Surgeons were required to document and submit to a central location the planned goals for thoracic kyphosis, sagittal vertical axis, and pelvic incidence to lumbar lordosis (PI-LL) mismatch prior to surgery. The authors found that surgeons failed to achieve goal alignment of each sagittal parameter in ∼25%–30% of ASD patients, and that goal alignment for all 3 parameters was only achieved in 37.2% of patients. Notably, those at greatest risk for not achieving goal alignment were those with more severe deformities. The authors concluded that further advancements are needed to enable surgeons to more consistently translate their patient-specific preoperative alignment goals to the operating room. 27
Personalized medicine has markedly impacted many aspects of health care, including spine surgery. 28 For example, patient-specific precontoured rods designed based on preoperative alignment planning can aid in achieving alignment and may have the added benefit of reducing rod breakage.29-32 Although patient-specific rods may help to lock in desired alignment, deformity correction primarily occurs through osteotomies and through release and realignment of the disc spaces. Personalized 3D-printed interbody spacers have recently become available, with applications for anterior lumbar interbody fusion (ALIF), lateral lumbar interbody fusion (LLIF), and transforaminal lumbar interbody fusion (TLIF). It remains to be determined whether this ability to more predictably control the disc space translates into improved ability for the surgeon to achieve goal alignment. Our objective in this study was to assess the effectiveness of 3D-printed personalized interbody spacers in achieving goal alignment following ASD surgery based on a multicenter patient cohort. In addition we provide comparisons of rates of achieving goal alignment with the previously published ISSG CADS study 27 that relied on use of stock (not personalized) interbody implants.
Methods
Study Design and Patient Populations
This multicenter, retrospective cohort study was conducted to assess radiographic outcomes of consecutive complex ASD patients
This study utilized secondary research consisting of de-identified data for which consent is not required and no direct patient involvement occurred and was exempt from institutional review board review.
Data Collection
Full-length standing anteroposterior and lateral radiographs were obtained for all patients at the time of enrollment and at follow-up visits. Planned PI-LL mismatch, intervertebral lordosis angle (IVL), intervertebral coronal angle (IVCA), and intervertebral posterior disc height (IVPH) were prescribed in a personalized manner for each patient by the surgeon during the planning process for the personalized interbody implants. Radiographs from the first follow-up visit were analyzed at a central site using validated software (Spineview, ENSAM Laboratory of Biomechanics, Paris, France). 33 Achieved PI-LL mismatch, IVL, IVCA, and IVPH were determined.
Data Assessment and Statistical Analysis
Statistical analysis was performed using Python 3.11. Descriptive statistics were reported as mean and standard deviation (SD) for continuous variables and frequencies with percentages for categorical variables. Pearson chi-square test was used to compare categorical variables. Continuous data were assessed for normality using the Shapiro-Wilk test. Relationships between continuous variables with a normal distribution were assessed using Pearson correlation. Relationships between continuous variables with a nonnormal distribution were assessed using Spearman Rank correlation. Comparison with CADS proportions were performed with a two-proportion z-test. All tests were two-tailed, with a significance level of α = .05.
As determined by the operating surgeon prior to surgery, goal alignment parameters were compared with achieved alignment based on standing radiographs obtained at the first follow-up after surgery (typically 6 weeks). Goals were compared with achieved alignment, and the overall mean and SD for all patients were calculated for each radiographic parameter’s offset (achieved minus goal). In addition, comparison of rates of achieving goal PI-LL mismatch were compared with published data from the ISSG CADS study. 27
Results
Patient Population
Baseline Demographic, Radiographic, and Operative Parameters for 65 Adults With Spinal Deformity Treated With Surgery Including Personalized Interbody Spacers. a
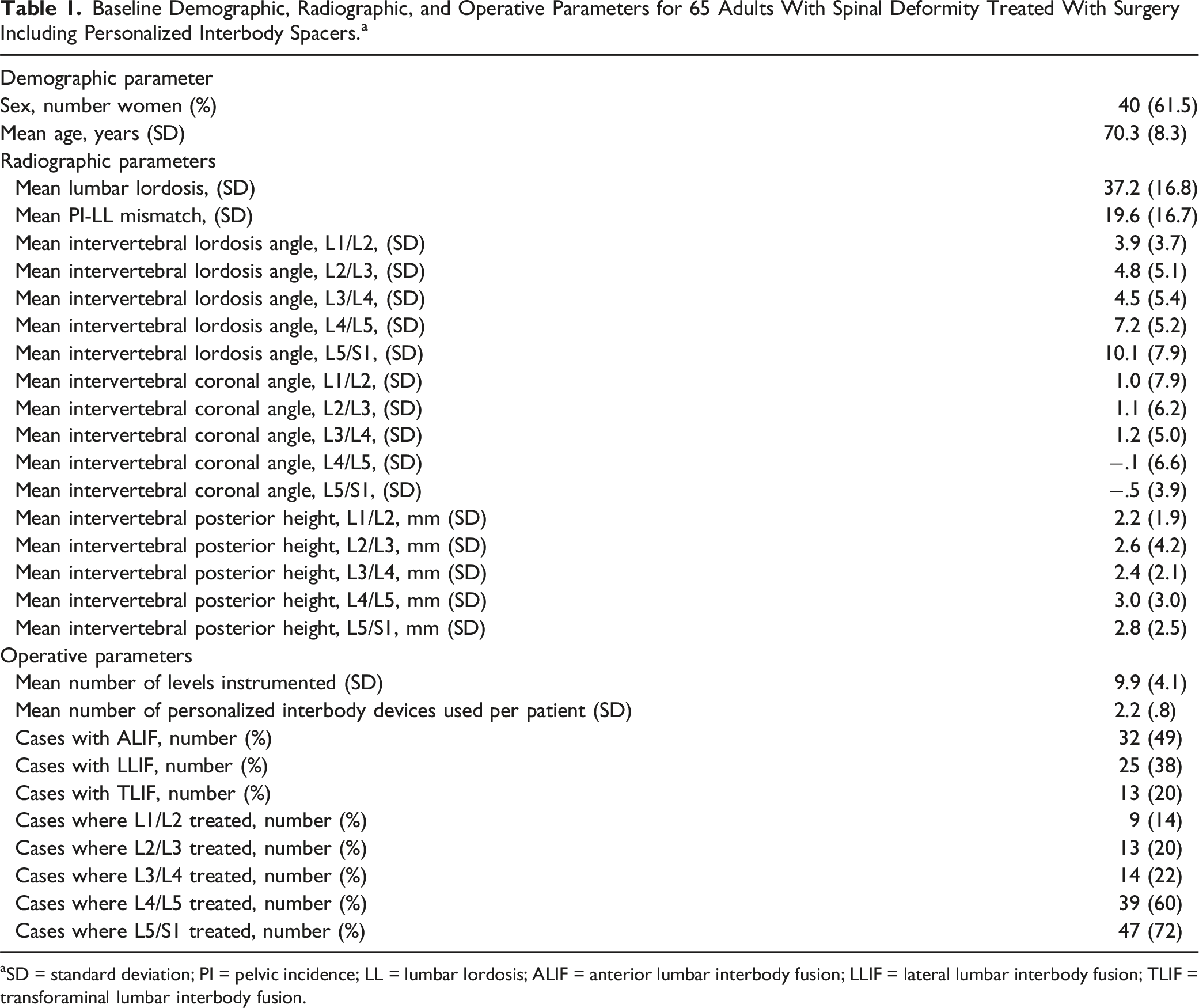
aSD = standard deviation; PI = pelvic incidence; LL = lumbar lordosis; ALIF = anterior lumbar interbody fusion; LLIF = lateral lumbar interbody fusion; TLIF = transforaminal lumbar interbody fusion.
Radiographic Analysis of Patients Treated with Personalized Interbodies
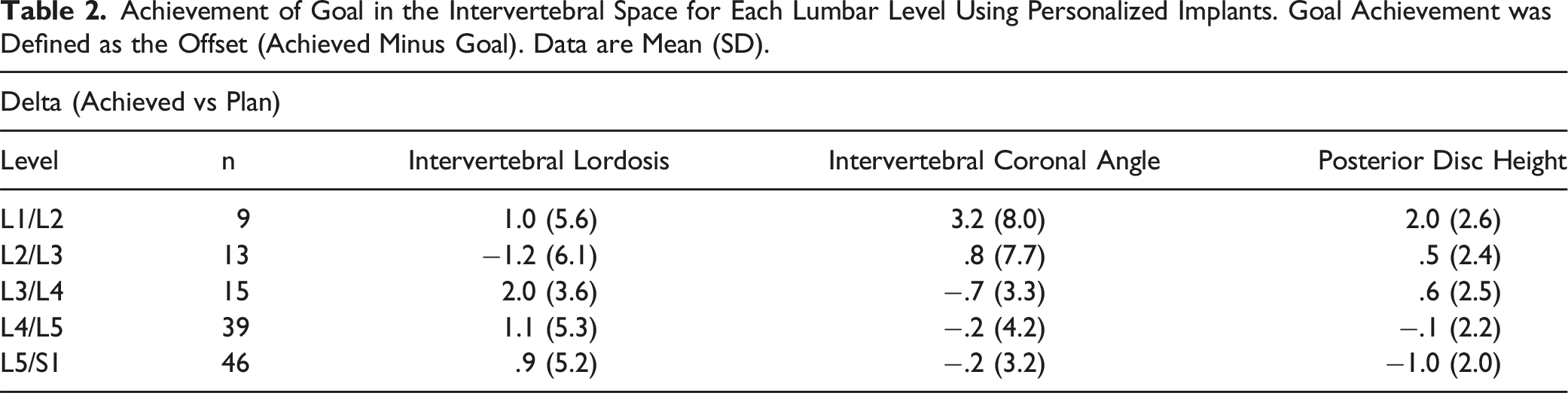
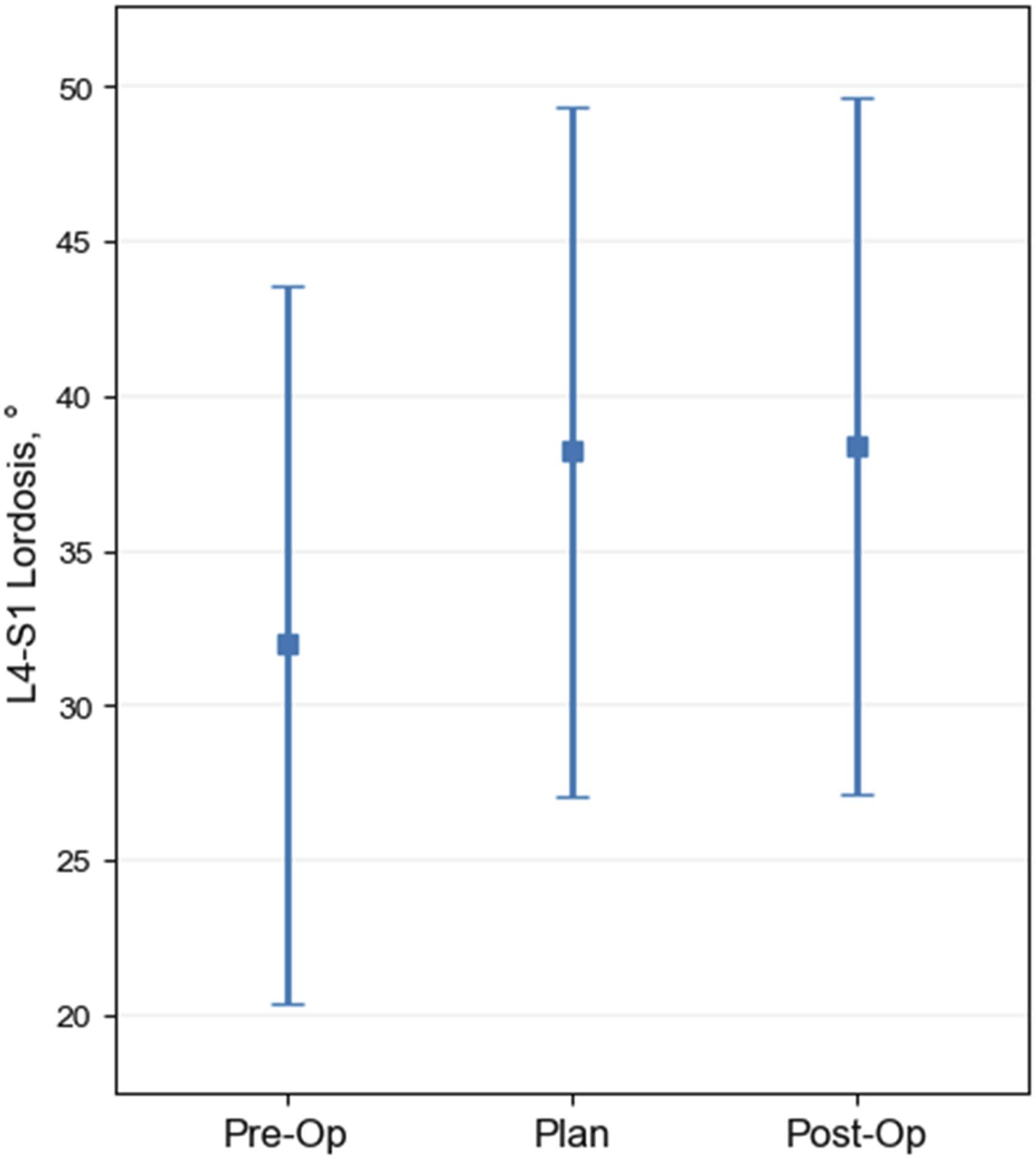
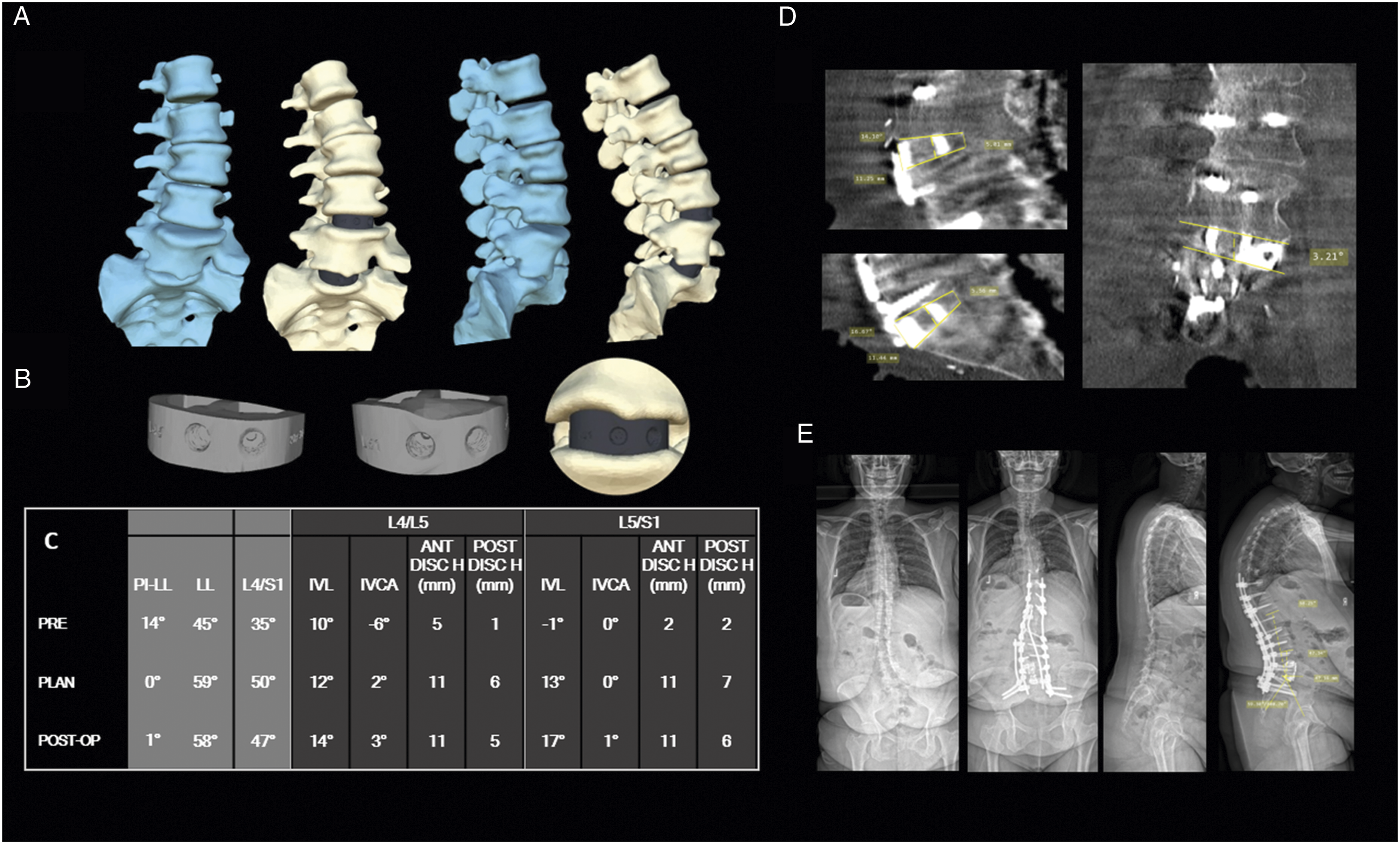
The segmental alignment offset between achieved and goal for all levels treated with personalized interbody implants is graphically depicted in Figure 1. On average, the IVL was achieved with an offset of .9° (SD = 5.2°), IVCA was achieved with an offset of .1° (4.7°), and IVPH was achieved with an offset of −.1 mm (SD = 2.3 mm). The offset between achieved and goal segmental alignment is stratified by vertebral level in Table 2. The baseline, goal, and achieved L4-S1 lordosis are shown in Figure 2. At baseline the mean L4-S1 lordosis was 32° (SD = 11.6°), and the mean achieved L4-S1 lordosis of 38.4° (SD = 11.3°) was within .2° of the mean plan (38.2°, SD = 11.1°). An example patient illustrating the achieved vs planned alignment is shown in Figure 3. Segmental alignment offset between achieved and goal for all levels treated with personalized interbody implants for 65 adults surgically treated for spinal deformity. Mean offsets (SD) are .9° (5.2°) for intervertebral lordosis (IVL), .1° (4.7°) for intervertebral coronal angle (IVCA), and −0.1 mm (2.3 mm) for intervertebral posterior disc height (IVPH). Achievement of Goal in the Intervertebral Space for Each Lumbar Level Using Personalized Implants. Goal Achievement was Defined as the Offset (Achieved Minus Goal). Data are Mean (SD). L4-S1 lordosis in 65 adult spinal deformity patients treated surgically with personalized implants. Baseline (Pre-Op) mean = 32° ± 11.6°, goal (Plan) 38.2° ± 11.1°, and achieved (Post-Op) 38.4° ± 11.3°. Patient example illustrating achieved vs planned alignment. Patient is a 53-year-old woman with global sagittal malalignment (adult spinal deformity with fractional curve at lumbosacral junction). Shown are antero-posterior (AP) and lateral 3D reconstruction views (A) of preoperative (blue) and planned (beige) alignment and geometry of personalized implants for L4/5 and L5/S1 which was derived from mapping the intervertebral space of the corrected alignment with superior and inferior implant surfaces matching vertebral endplate topography (B). Table of preoperative, planned, and postoperative alignment for pelvic incidence to lumbar lordosis mismatch (PI-LL), lumbar lordosis (LL), L4-S1, and intervertebral space planning for L4-L5 and L5-S1 (C). One-year postoperative CT showing fusion, implant contact, and alignment in lateral and coronal views (D) and preoperative and postoperative standing x-rays with AP and lateral views (E). IVL = intervertebral lordosis angle; IVCA = intervertebral coronal angle; ANT DISC H = anterior disc space height; POST DISC H = posterior disc space height.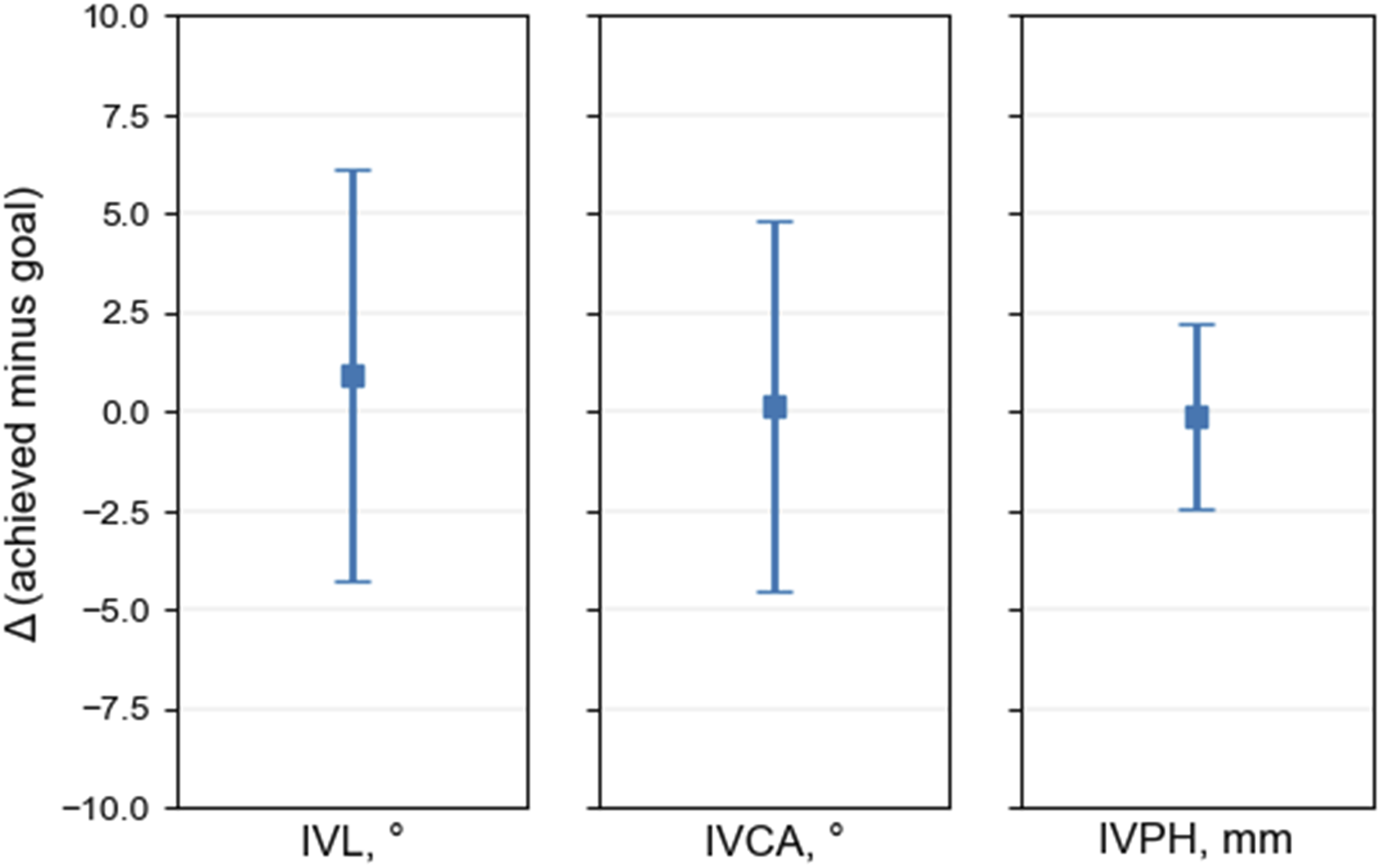
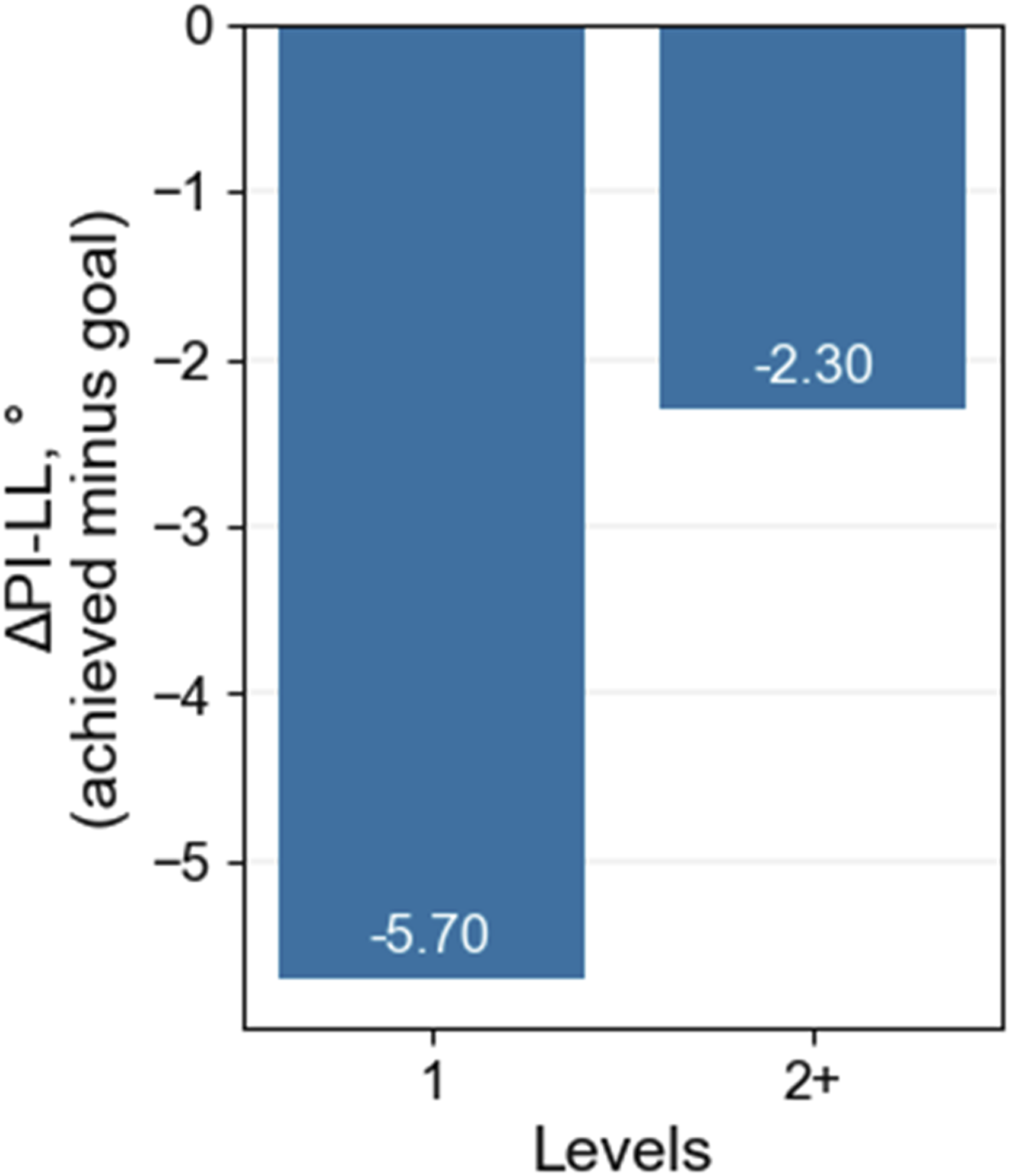
The achieved PI-LL mismatch correlated significantly with the goal PI-LL (r = .668, P < .001; Figure 4). Overall, the mean difference in postoperative PI-LL, in comparison with the plan, was −3.4° (SD = 12.3°). For patients treated at 1 level with a personalized interbody spacer, the mean offset of PI-LL mismatch (achieved minus goal) was −5.70°. There was a trend toward closer planned vs achieved alignment when 2 or more personalized interbody devices were used vs a single level treated with personalized devices, although this difference did not reach statistical significance (P = .37; Figure 5). Scatter plots of achieved vs goal sagittal alignment and baseline sagittal alignment vs difference between goal and achieved alignment for 65 adult spinal deformity patients treated surgically with personalized implants. Shown is a plot for PI-LL mismatch. PI = pelvic incidence, LL = lumbar lordosis. Offset of PI-LL (achieved minus goal) for 65 adults surgically treated for spinal deformity, stratified by number of levels treated with a personalized interbody spacer (1 (1) level or more than 1 (2+) level).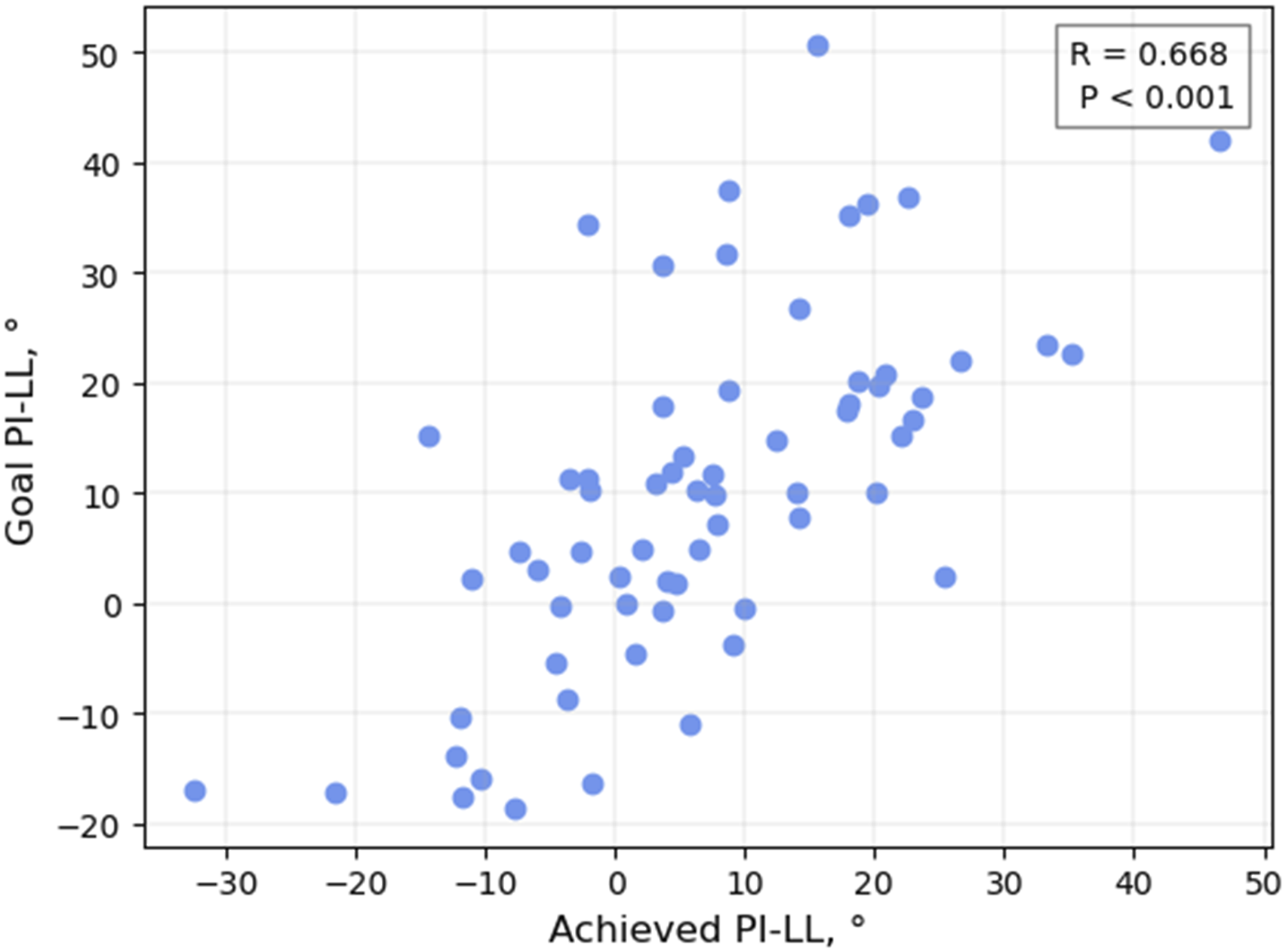
Comparison of Alignment Between Personalized and Stock Devices (International Spine Study Group Complex Adult Deformity Surgery)
Compared with the ISSG CADS cohort that utilized stock interbodies, utilization of personalized interbodies resulted in significant improvement in achieving PI-LL mismatch within 5° of the preoperative plan (31.5% vs 44.6%, P = .046, Figure 6). Furthermore, compared to ISSG cases, utilization of personalized interbodies led to a significant reduction in cases in which the PI-LL mismatch exceeded 15° (15.3% vs 30.8%, P = .012, Figure 6). Percentage distribution of the magnitude of offsets of the PI-LL achieved compared to the plan for 65 subjects with adult spinal deformity treated with personalized implants based on a 3D preoperative plan compared to 266 patients treated with stock implants through the international spine study group (ISSG) complex adult deformity surgery (CADS) analysis.
27
PI = pelvic incidence; LL = lumbar lordosis.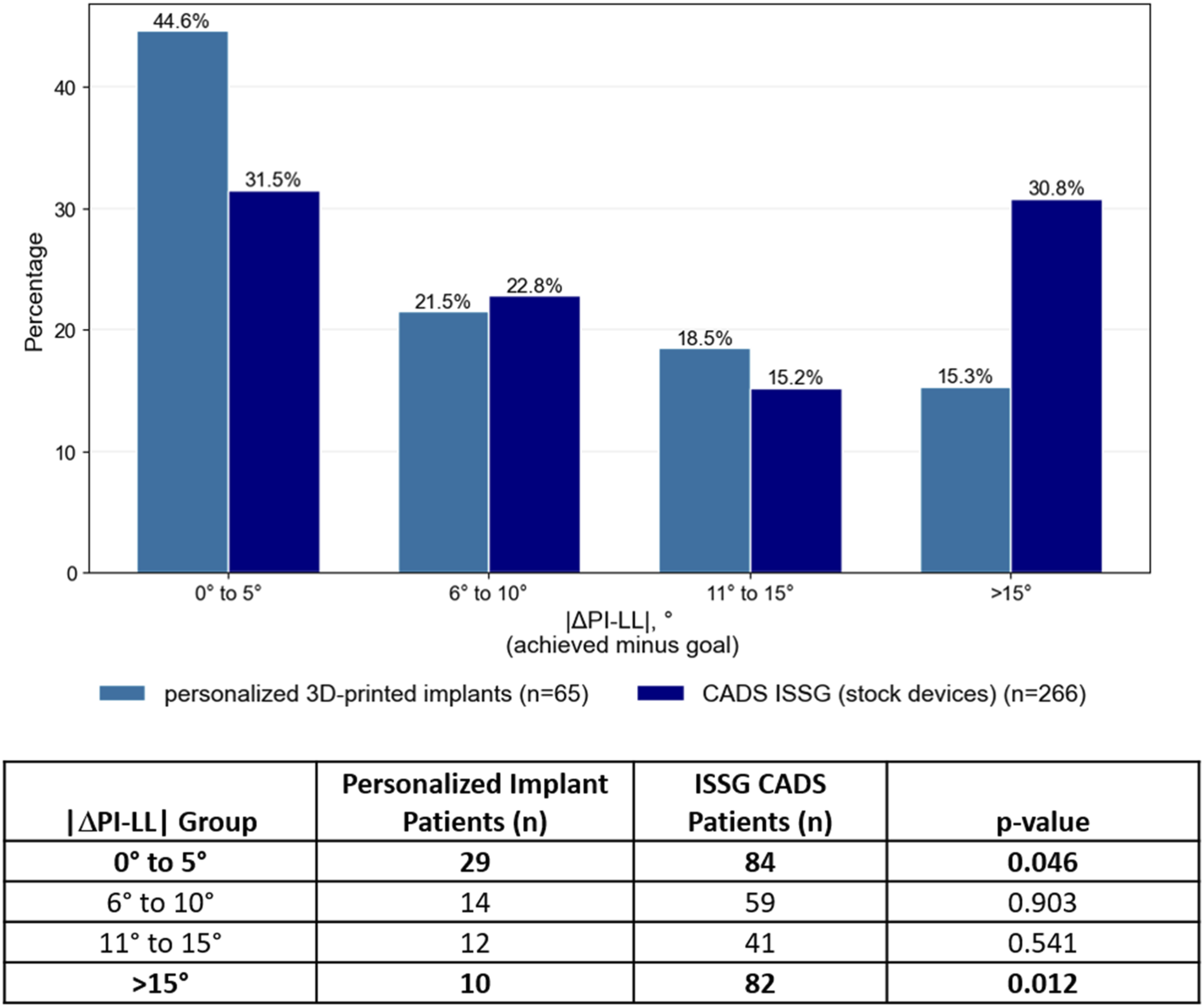
Discussion
A critical goal of spinal deformity correction surgery is to achieve appropriate alignment that will support favorable clinical outcomes and minimize the risk of mechanical complications. Although significant progress has been made in defining optimal spinal alignment for ASD surgery, there remain many areas of debate and further research is needed. There are increasingly sophisticated software tools to enable surgeons to meticulously plan each spinal deformity correction prior to entering the operating room. However, the ability to translate these plans in to the operating room and achieve the desired goal spinal alignment remains imperfect. Smith et al recently demonstrated, that even among an experienced group of ASD surgeons, the preoperative goal alignment for 3 key sagittal alignment parameters was only achieved in approximately one-third of patients. 27 The present study assesses whether the ability to control the intervertebral disc space alignment through personalized interbody spacers can aid in achieving the surgeon’s goal alignment targets.
Release and realignment of the intervertebral disc space is a primary tool in the correction of spinal deformity. Design of interbody spacers, as part of the overall realignment plan, enables surgeons to personalize the angular and height corrections that will best achieve the goal alignment, thereby facilitating transfer and execution of the preoperative plan into the operating room. The present study has tested this concept in clinical practice. Among 65 complex ASD patients, the achieved segmental lordosis at the level of the personalized spacer was, on average, with 1° of the planned segmental lordosis. The achieved segmental coronal alignment had a mean offset from goal of .1°, and the IVPH was achieved within a mean of −.1 mm of the preoperative goal. These findings suggest that personalized interbody spacers are effective in facilitating achievement of goal segmental alignment.
The PI-LL mismatch is a commonly used measure of lumbar sagittal alignment and has been correlated with clinical outcomes and mechanical complications, including proximal junctional failure.34–37 In the present study, the achieved PI-LL mismatch had an overall strong correlation with the planned PI-LL (r = .668, P < .001), and the mean offset between goal vs achieved PI-LL was −3.4°. Notably, compared with use of a personalized interbody spacer at 1 level, use of these spacers at 2 or more levels trended toward a closer achievement of goal PI-LL mismatch. Although this was not statistically significant, the present study may not have been sufficiently powered to detect this difference.
Achievement of goal PI-LL mismatch was significantly better among the patients with personalized interbodies compared with the published ISSG CADS series, in which stock devices were used. 27 This apparent benefit was most notable at the extremes of PI-LL mismatch. Patients with 1 or more personalized interbodies were significantly more likely to have an achieved PI-LL mismatch within 5° of plan compared with the ISSG stock interbody device cohort (44.6% vs 31.5%, P = .046). Perhaps more importantly, use of personalized interbodies was associated with a significant and marked reduction in the rate of achieving a PI-LL mismatch that was 15° or more from the goal (15.3% vs 30.8%, P = .012).
The present study demonstrates that use of a personalized interbody spacer has a high level of concurrence between the planned and achieved segmental alignment and PI-LL mismatch. However, it is important to note that even though interbody spacers can have substantial impact on segmental alignment and regional alignment to a lesser degree, they do not necessarily control the overall PI-LL mismatch. The majority of lumbar lordosis has been reported to occur in the lower segments of the lumbar spine (L4-5 and L5-S1), 38 suggesting that these levels may have the greatest potential for impact. Notably, the vertebral levels that were most commonly treated with personalized interbodies in the present study were L4-5 and L5-S1 which may help account for the improved achievement of goal PI-LL mismatch in the personalized interbody cohort.
Although the present study focused on complex ASD patients, the findings may have significant applications for short-segment spinal fusions performed for degenerative pathologies. Multiple prior studies have clearly demonstrated the importance of achieving sufficient segmental lordosis and overall PI-LL mismatch, even when performing short-segment fusions. In a series of 1-, 2-, or 3-level posterior lumbar fusions, Rothenfluh and colleagues 39 reported a 10-fold higher rate of revision surgery for adjacent segment disease if the PI-LL mismatch was not sufficiently maintained or restored. Multiple subsequent reports have provided similar findings.40-44 The demonstrated ability of personalized interbody spacers to provide a high level of achieving goal segmental alignment in the present study could facilitate improved alignment in short-segment fusions and warrants further study.
This study is not without limitations. The number of patients was relatively small and limited the granularity of statistical analyses that could be performed. In addition, preoperative alignment planning is not a completely standardized process, and the goals for alignment may have differed based on surgeon preferences.
Conclusion
Segmental alignment was achieved close to plan for levels with personalized interbodies, with mean difference between goal and achieved within 1°. Compared with the ISSG CADS cohort, utilization of personalized interbodies resulted in significant improvement in achieving PI-LL <5° of plan and showed a significant reduction in cases with PI-LL >15° of plan.
Collectively, this study supports use of personalized interbodies as a means of better achieving goal segmental sagittal and coronal alignment and significantly improving achievement of goal PI-LL compared with stock devices.
Footnotes
Author's Note
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by Carlsmed.
