Abstract
Study Design:
Retrospective observational study.
Objective:
To investigate the relationship between the extent of ligament ossification and the range of motion (ROM) of the lumbar spine and develop a new scoring system.
Methods:
Forty-three patients (30 men and 13 women) with lumbar spinal canal stenosis who underwent decompression from January to December 2018. Ligament ossification at L1/2 to L5/S was assessed on plain X-ray (Xp) and computed tomography (CT) using a modified Mata scoring system (0 point: no ossification, 1 point: ossification of less than half of the intervertebral disc height, 2 points: ossification of half or more of the intervertebral disc height, 3 points: complete bridging), and the intra-rater and inter-rater reliability of the scoring was assessed. The relationship of the scores with postoperative lumbar ROM was investigated.
Result:
Intra-rater reliability was high (Cronbach’s α was 0.74 for L5/S on Xp but 0.8 or above for other sections), as was inter-rater reliability (Cronbach’s α was 0.8 or above for all the segments). ROM significantly decreased as the score increased (scores 1 to 2, and 2 to 3). A significant moderate negative correlation was found between the sum of the scores at L1/2-L5/S and the ROM at L1-S (ρ = − 0.4493, P = 0.025).
Conclusion:
Our scoring system reflects lumbar mobility and is reproducible. It is effective for assessing DISH in fractures and spinal conditions, and monitoring effects on treatment outcomes and changes over time.
Introduction
Diffuse idiopathic skeletal hyperostosis (DISH) is characterized by progressive ossification of ligaments throughout the body. In the spine, ossification of the anterior longitudinal ligament causes ankylosis. The condition was first reported by Forestier et al 1 in 1950 and was subsequently defined as DISH by Resnick et al,2,3 who specified the criteria for diagnosing DISH as showing 1) a bony bridge spanning at least 4 contiguous vertebrae along the anterior or lateral aspect of the vertebral bodies, 2) relatively preserved intervertebral disc height, and 3) the absence of ankylosis in the sacroiliac joints. The prevalence of DISH in adults is 2.9% to 27.2%.4-8 DISH has been linked to old age, male sex, diabetes, hypertension, and obesity,4,8,9-12 and influences on ligament ossification include genetic(e.g., COL6A1) 13 metabolic (e.g., diabetes),11,12 and endocrine factors (e.g., growth hormones), 14 along with vitamin A, 15 and signal transduction. 16 However, the cause of DISH is unclear. Clinically, DISH causes back pain, restricted range of motion (ROM), reduced vital capacity, aspiration, and airway obstruction.17-20
A problem in patients with DISH is reduced spinal flexibility resulting from the formation of a bone bridge across vertebral bodies due to ligament ossification. In patients with reduced spinal flexibility, a vertebral fracture can occur with only minor trauma. If the fracture is the reverse Chance type, spinal fusion is required.21-23 When a fracture occurs in the vertebra just below the bridged vertebral bodies, the extended lever arm causes a high stress concentration, making it more difficult for the fracture site to fuse. 24 Similarly, progressive degeneration after lumbar decompression may necessitate reoperation, and spinal fusion is more likely to result in a nonunion.25,26 In thoracic vertebrae, there is a higher likelihood that thoracic spondylotic myelopathy develops between the vertebral bodies that are bridged together or in the adjacent vertebra. 27
These problems are associated with the extent of ligament ossification. Spinal flexibility decreases as the number of vertebral bodies involved in bridging increases, predisposing the patient to a fracture. The longer the lever arm, the greater the mechanical load that is applied to the adjacent vertebral bodies and spinal segments, which is more likely to lead to a fracture or progressive intervertebral degeneration. Grading and scoring are used as indicators to show the extent of progression. By assigning a numeric score to the extent of progression, the data can be used to make quantitative assessments of ligament ossification and evaluate the extent of progression, treatment outcomes, etc.
Other scoring systems have been reported for assessing ligament ossification in DISH. Mata et al 28 used frontal and lateral plain X-ray (Xp) images to develop a 0 to 3 point scale based on morphology and evaluated the extent of ligament ossification in the spine and extremities. Yaniv et al 29 used thoracolumbar computed tomography (CT) images to develop a 0 to 6 point scale and evaluated the natural course of ligament ossification over a 10-year period. Kuperus et al 30 performed chest CT and used CT images of the thoracic spine to assess the progression of ligament ossification over 5 years according to a scoring system divided into bridge-score and flow-score components, each with a 0 to 3 point scale. However, these scoring systems assessed only the morphological features of ligament ossification on Xp and CT, without correlating scores with clinical findings. The scoring systems should consider both the morphology of the ossification and reduced spinal flexibility.
In this study, we examined the relationship between the morphology of ligament ossification and lumbar ROM and developed a simple scoring system.
Methods
The study cohort comprised 43 patients with lumbar spinal canal stenosis who underwent decompression from January to December 2018. Lumbar spine Xp was performed on all participants in a standing position to obtain frontal and lateral flexion/extension views. The Xp was performed within 6 months after surgery, and whole-spine CT scans were carried out 1 week after surgery.
Our new scoring system for ligament ossification was created by modifying the criteria of the Mata scoring system as follows: 0 point = no ossification; 1 point = ossification of less than half of the intervertebral disc height; 2 points = ossification of half or more of the intervertebral disc height; and 3 points = complete bridging (Figure 1). Using the modified Mata scoring system, the 5 spinal segments from L1/2 to L5/S were assessed using frontal and lateral Xp views in the neutral position, 3 times by a first observer, and then once by a second and a third observer. In the same manner, sagittal, coronal, and 3-dimensional CT images were used to assign scores to the 5 spinal segments. If scores on the frontal and lateral views were different, the higher score was adopted. The intra-rater reliability was determined using the 3 sets of scores by the first observer on Xp and CT images, and inter-rater reliability was evaluated based on the first set of scores by the first observer and the scores from observers 2 and 3. Then, the 3 observers collectively determined a valid score for each spinal segment using CT images, and examined the relationships of the scores with lumbar ROM. The 3 observers are spine surgeons who have been engaged in clinical practice and research for more than 10 years and have extensive experience in imaging diagnosis and measurement on X-ray and CT.
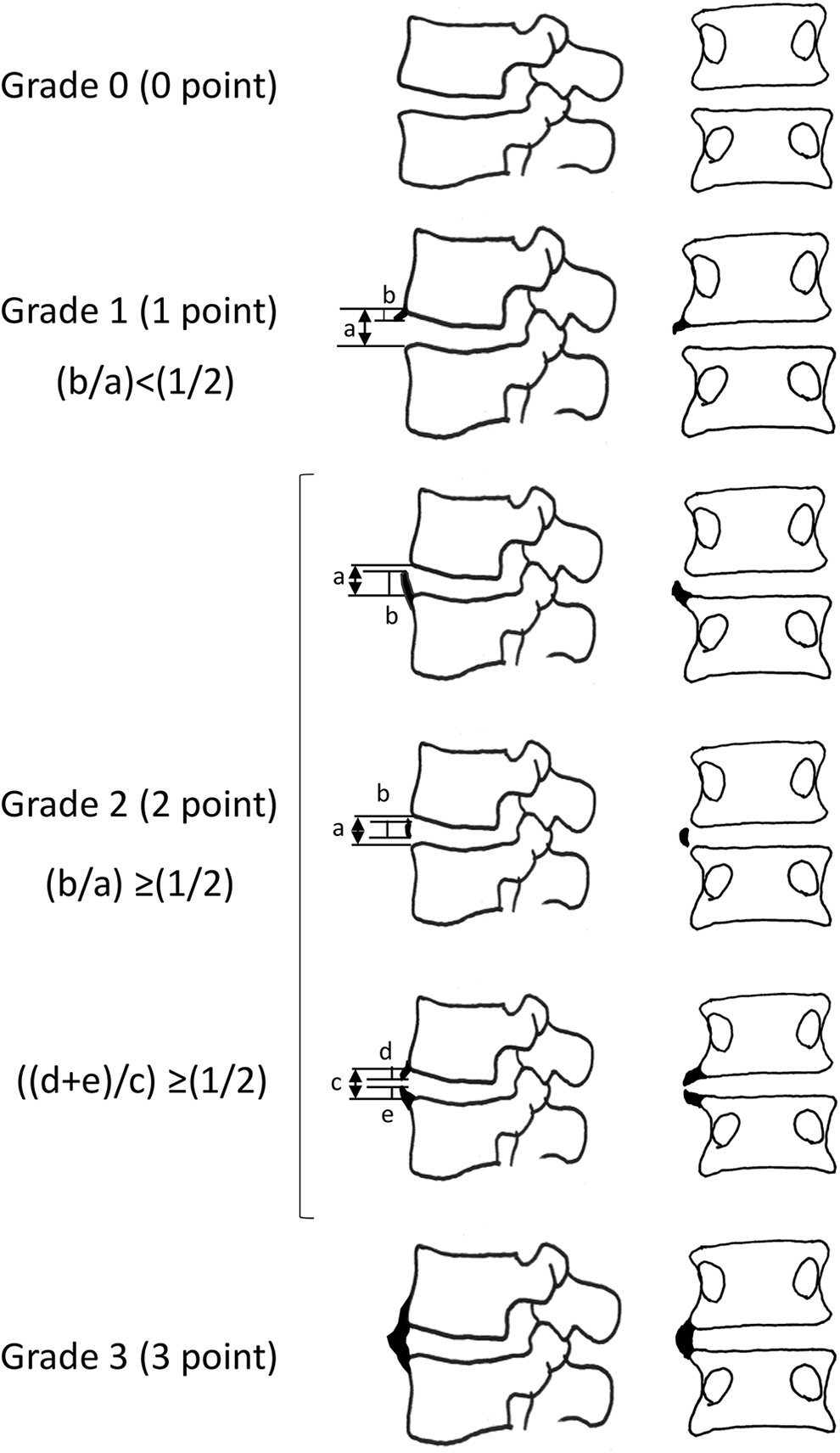
Modified Mata score. Grade 0 (0 point): no ligament ossification. Grade 1 (1 point): with ligament ossification of less than half of the intervertebral disc height. Grade 2 (2 points): with ligament ossification of half or more of the intervertebral disc height. Grade 3 (3 points): complete bridging.
Using the positions of maximum flexion and maximum extension on postoperative lateral Xp views, the angle of each spinal segment from L1/2 to L5/S was measured. A lordosis was defined as a positive angle. The value obtained by subtracting the flexion angle from the extension angle was defined as the ROM at each spinal segment. The ROM at L1-S was measured in the same manner. Next, the relationship between the ROM and observer scores at each segment was analyzed, as was the relationship between the ROM and the sum of scores at L1-S.
For statistical analysis, intra-class correlation coefficients (Cronbach’s α) were calculated for intra-rater and inter-rater reliability. Analysis of variance was used for the differences in ROM among spinal segments. To examine the relationship between modified Mata scores and the measured angles, Spearman’s rank correlation coefficients were calculated. Dunn’s test was used to compare the ROM among modified Mata scores. A P value of < 0.05 was considered to be statistically significant. The software used was SPSS for Macintosh version 24.
Because this study was retrospective, the patient’s informed consent was obtained by opting out. We announced on the website of the Clinical Research Support Center and the Department of Orthopedic Surgery of our university hospital, or on the hospital bulletin board that we would be conducting this study, and provided an opportunity to reject the use of the data. This study was approved by the institutional review board at our University Hospital (IRB approval no., 20 181 005 001). The authors declared no potential conflicts of interest with respect to the research, authorship, and publication of this article.
Results
The cohort of 43 patients comprised 30 men and 13 women with a mean age of 70.4 ± 9.7 years. The Cronbach’s α for intra-rater reliability was 0.74 for L5/S by Xp but 0.8 or higher for the other segments, which demonstrated high intra-rater reproducibility (Table 1). For inter-rater reliability, Cronbach’s α was 0.8 or higher for all segments on both Xp and CT, which showed high inter-rater reliability (Table 2).
Intra-rater Reliability of the 3 Sets of Modified Mata Scores Given by Observer 1 on Plain X-ray and CT Images.
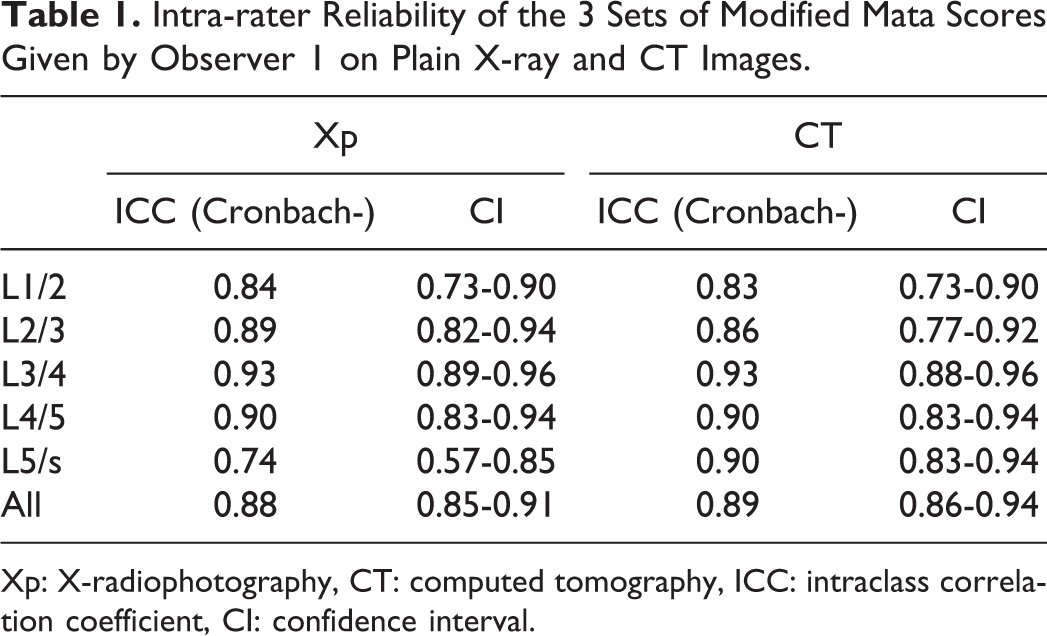
Xp: X-radiophotography, CT: computed tomography, ICC: intraclass correlation coefficient, CI: confidence interval.
Inter-rater Reliability of Modified Mata Scores Given by Observers 1, 2, and 3 on Plain X-ray and CT Images.
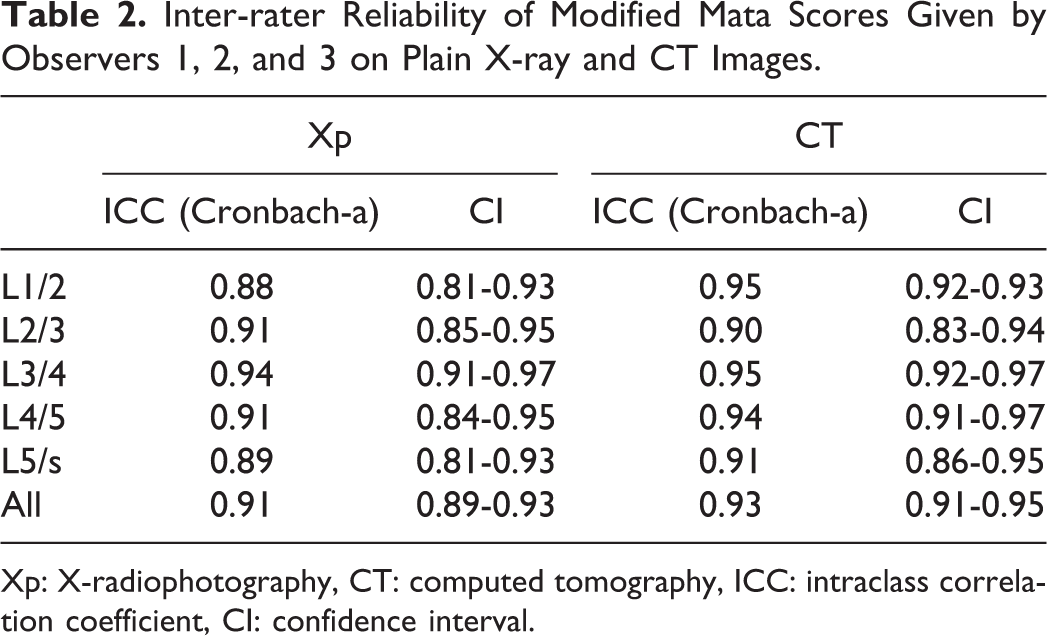
Xp: X-radiophotography, CT: computed tomography, ICC: intraclass correlation coefficient, CI: confidence interval.
The mean ROM at L1-S was 26.8 ± 11.3°. The mean ROM at each spinal segment was 5.2 ± 3.2° at L1/2, 4.9 ± 3.7° at L2/3, 4.9 ± 4.2° at L3/4, 5.1 ± 3.9° at L4/5 and 6.5 ± 5.3° at L5/S (Table 3). The percentage of the ROM at each segment in the total ROM at L1-S was 20.1 ± 11.1% for L1/2, 18.8 ± 10.8% for L2/3, 17.9 ± 12.8% for L3/4, 19.3 ± 11.0% for L4/5 and 24.2 ± 17.9% for L5/S. Although the ROM tended to be greater at L5/S, the differences were not significant (Table 3).
ROM at Each Spinal Segment and Its Percentage in the Total Lumber ROM.
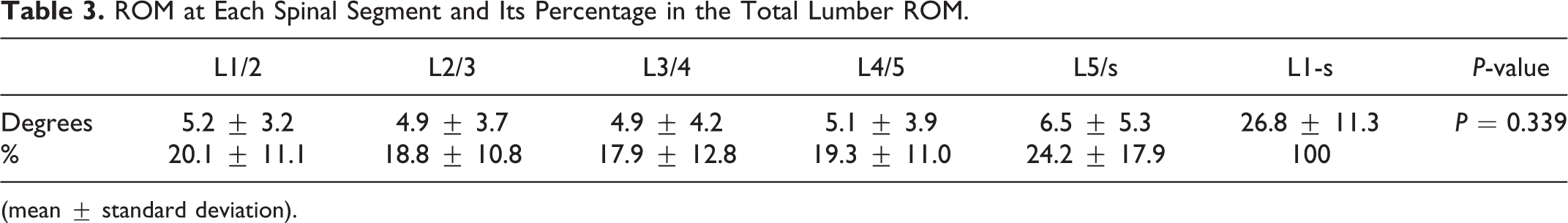

(mean ± standard deviation).
Analysis of modified Mata scores in all patients at all spinal segments (n = 215) showed 88 segments with score 0, 53 segments with score 1, 65segments with score 2, and 9 segments with score 3. The mean ROM was 7.1 ± 0.4° for score 0, 5.7 ± 0.5° for score 1, 3.5 ± 0.5° for score 2, and 0° for score 3, and a significant weak negative correlation was found between the scores and ROM (ρ = −0.4471, P < 0.0001). Comparisons of the ROM between each scores found significant differences in all cases except between scores 0 and 1. For the spinal segments that were scored 1 or higher, the ROM decreased as the score increased (Figure 2).
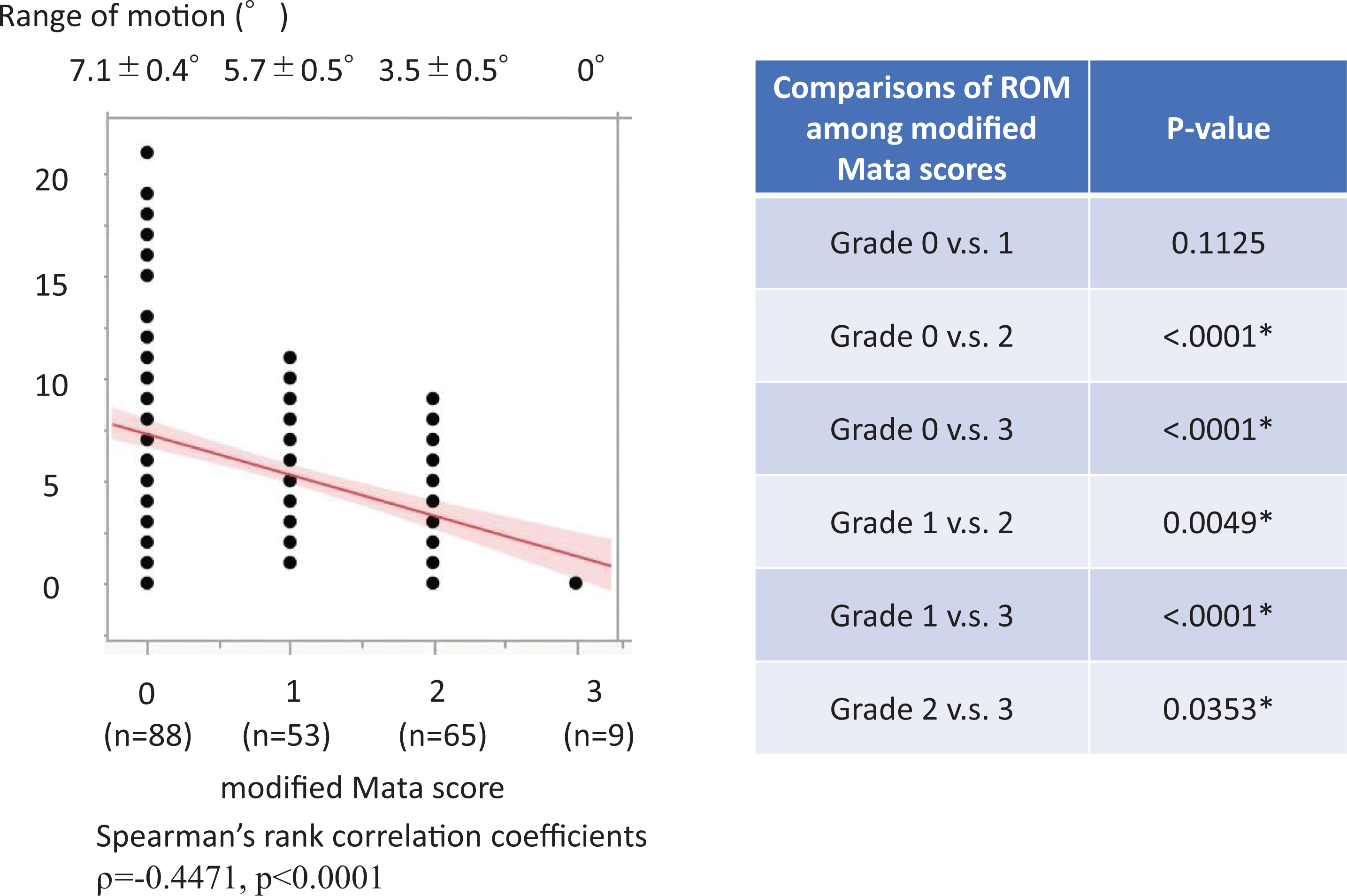
Comparisons of ROM among modified Mata scores. A significant weak negative correlation was found between modified Mata scores and ROM (ρ = −0.4471, p < 0.0001). Significant differences were also found in ROM except between Grades 0 and 1 (Dunn’s test; * = denotes a significant difference).
The relationship between the ROM at L1-S and the sum of the modified Mata scores at all the segments from L1/2 to L5/S (5 segments) in all patients was analyzed, which showed a significant moderate negative correlation (ρ = −0.4493, P = 0.0025). This indicates that the lumbar spinal mobility decreases as the sum of the scores increases (Figure 3).
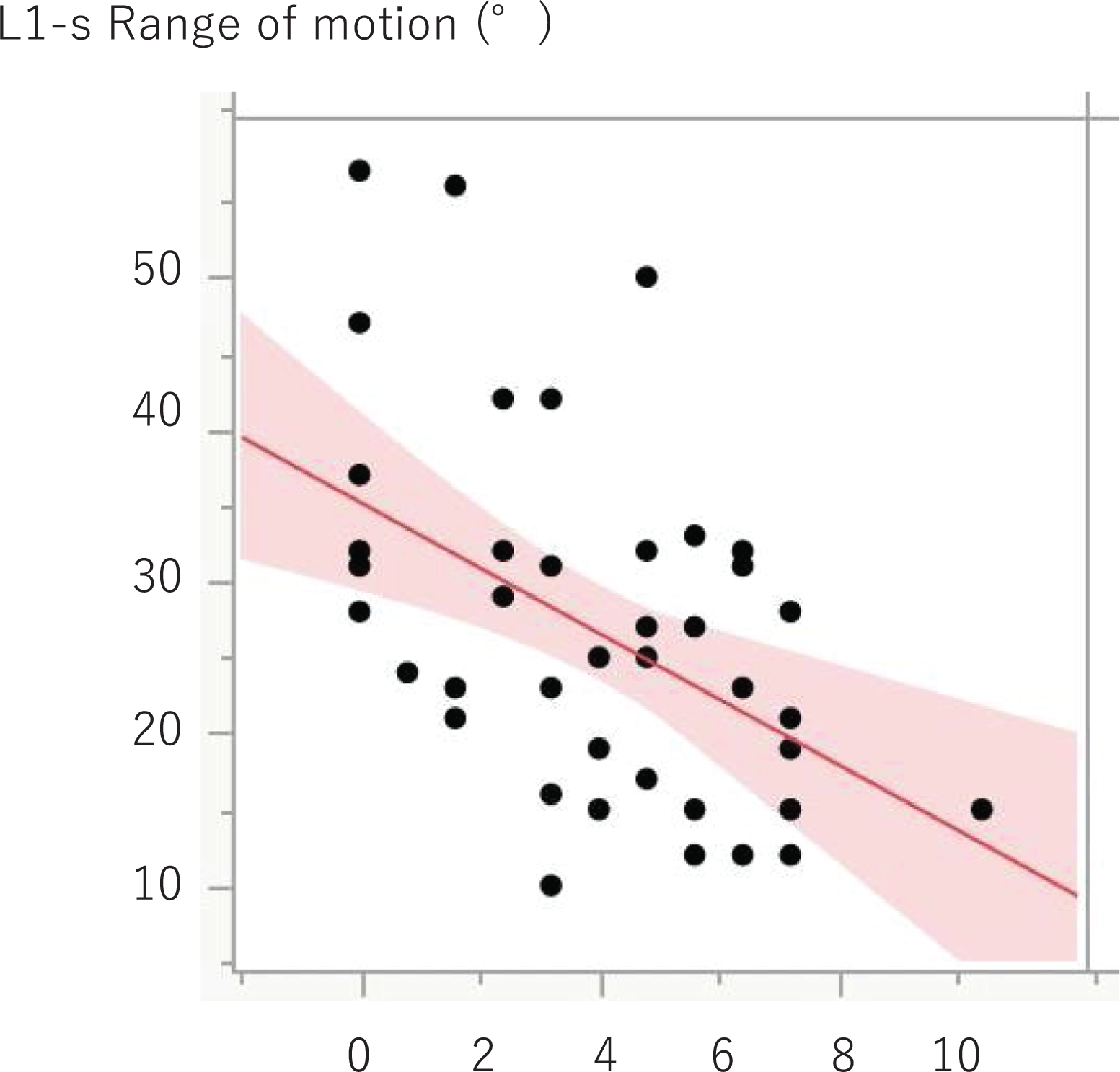
Total points for modified Mata scores (L1/2-L5/s). Spearman’s rank correlation coefficients ρ = −0.4493, P = 0.0025.
Discussion
In this study, we propose a new 0 to 3 point scoring system created by modifying the existing Mata scoring system. The system was developed using postoperative standing Xp and lumbar spinal CT images in patients who had undergone surgery for lumbar spinal canal stenosis. As most patients who receive Xp and CT examinations during a short period of time are those undergoing surgery, we decided to select surgical cases for the study cohort as it would allow us to obtain necessary data. The subjects comprised patients who met the diagnostic criteria for DISH and those who did not. Since it has been reported that patients who do not meet the diagnostic criteria may still be prone to ossification of the anterior longitudinal ligament, or a so-called pre-DISH condition,30,31 this study purely focused on the degree of ossification of the anterior longitudinal ligament and ROM at each lumbar segment. Scores were given to rate frontal and lateral Xp images, and sagittal and coronal CT images of the lumbar spine. Examination of these scores showed good reliability and reproducibility between observers using the scoring method. The ROM decreased as the observed score increased for the spinal segments scored Grade 1 or higher. A correlation was also found between the sum of scores and the lumbar ROM. These findings suggest that this approach is a simple scoring system consistent with intervertebral ROM in DISH.
Other scoring systems showing the extent of ossification of the anterior longitudinal ligament in DISH have been published. The system from Mata et al 28 evaluated the morphology of ligament ossification in the spine and extremities using Xp images based on the following criteria: score 0 = no ossification; score 1 = ossification without bridging; score 2 = ossification with incomplete bridging; and score 3 = complete bridging. This scoring system has high intra-rater and inter-rater reliability and reproducibility, but distinguishing between scores 1 and 2 is difficult. Therefore, in this study, we attempted to improve the sensitivity by further dividing score 2 into ossification of less than half of the intervertebral disc height and ossification of half or more of the intervertebral disc height. As a result, better intra-rater and inter-rater reliability is achieved. As the Mata, Yaniv, and Jonneke systems all had scores based only on images without being related to clinical findings, our study has an advantage by relating scores to ROM.
The scoring system in this study had high reproducibility for both Xp and CT, although the reproducibility was lower for L5/S on Xp. This was potentially due to the difficulty of identifying the segment on frontal Xp views due to lumbar lordosis, as well as reduced visibility of ossification on lateral Xp views due to the overlapping ilium. However, L5/S is clearly visible by CT so highly reproducible scoring is possible at all spinal segments and, therefore, CT is recommended.
The problem with progressive bridging of vertebral bodies in DISH is the reduced flexibility of the entire spine, which predisposes the patient to a vertebral fracture after minor trauma and contributes to low rates of bone fusion after fractures. 24 Reduced spinal flexibility leads to chronic mechanical stress, which may cause thoracic spondylotic myelopathy, 27 and could become a risk factor for poor postoperative outcomes and reoperation in lumbar canal stenosis. 25 Low rates of bone union after spinal fusion surgery may also be due to reduced spinal flexibility. 26 Therefore, we considered it desirable to develop the scoring system linked to spinal mobility. Although our scoring system showed no significant difference in intervertebral ROM between scores 0 and 1, we judged that they should be separated based on the presence or absence of a tendency for ligament ossification. This study also demonstrated that the ROM decreases as the score increases from 1 to 2 and from 2 to 3, showing our scoring system to be consistent with clinical findings.
One limitation of this scoring system is that it does not take intervertebral degeneration into consideration. In addition to ossification of the anterior longitudinal ligament, other causes of decreased intervertebral mobility include reduced intervertebral space height and osteophyte formation, due to degeneration and degenerative facet joints. In this study, spinal segments in a patient without coexisting DISH were assigned a score of 0 despite having reduced mobility due to severe degeneration. To create a more clinically useful scoring system, horizontally extended osteophytes and intervertebral space height may also need to be included in the criteria, as in the scoring system by Kuperus et al. 30
Although the prevalence of DISH is reported to be higher among older adults, we found no correlation between the Modified Mata score and age (Pearson’s correlation coefficient: ρ = 0.1155, P = 0.4068). This was probably because the ages of the subjects in this study were high to begin with. Additionally, no correlation was found between the Modified Mata score and the number of decompressed intervertebral levels either (Spearman’s correlation coefficient ρ = 0.1317, P = 0.3998). This is probably because there are many other factors than just the degree of ligament ossification and changes in ROM that may cause extensive spinal canal stenosis that requires decompression, such as lumbar spinal alignment and occupation.
There are a few other limitations of this study. Firstly, ROM measurements were taken in patients with lumbar canal stenosis so data from the cohort may differ from healthy individuals. Secondly, because the study targeted the lumbar spine only, the scoring system may not be applicable to ligament ossification in the cervical or thoracic spine.
Conclusion
The new scoring system in this study based on the Mata scoring system reflects lumbar mobility, is simple to use, and is highly reproducible. It could be a useful tool for assessing fractures and spinal diseases, and monitoring effects on treatment outcomes and changes over time.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
