Abstract
Background:
Farmers have an increased risk of developing chronic obstructive pulmonary disease (COPD) and psychological distress. The potential role of psychological distress in worsening COPD symptoms has been reported among the general population, but no studies have examined this relationship among farmers with COPD, which is the purpose of this study.
Methods:
This study used the data from the 2017 Behavioral Risk Factor Surveillance System (BRFSS). Farmers reporting both psychological distress and COPD symptoms were included in this study (n = 239). Both unadjusted and adjusted logistic regressions were used to explore the association among psychological distress, age, health status, smoking, and COPD symptoms, with crude and adjusted odds ratio (OR) and 95% CIs reported.
Findings:
The unadjusted analysis suggested that COPD symptoms were significantly associated with psychological distress among farmers (OR = 2.05 [1.18, 3.58]). While adjusted models showed the significant association between COPD symptoms and psychological distress among farmers after controlling for smoking, age, and health status (adjusted OR = 2.08 [1.10, 4.01]).
Conclusion/Implications for Practice:
These results suggest that psychological distress is associated with an increased risk of COPD symptoms in farmers, which is consistent with observations from studies in non-farmers. Occupational health professionals need to provide screen for COPD among farmers as well as psychological distress screening and mental health promotion among farmers with COPD.
Keywords
Background
Chronic obstructive pulmonary disease (COPD) is a fatal disease affecting 200 million people worldwide (European Respiratory Society, 2017). This chronic condition causes progressive inflammation throughout the respiratory system and permanent destruction of distal respiratory tissue (Goldklang & Stockley, 2016). As a result, individuals living with this disease suffer from persistent difficult breathing and productive cough (Singh et al., 2019). Furthermore, they occasionally experience a sudden worsening symptom called acute exacerbation of COPD (Global Initiative for Chronic Obstructive Lung Disease [GOLD], 2020).
Although the most common risk factor of COPD is smoking (GOLD, 2020), some people develop COPD as a result of exposure to environmental components unique to farm environments (Cho et al., 2015). Farmers work in complex environments that expose them to multiple hazards, including organic dust, pesticides, and zoonotic pathogens (Nordgren & Charavaryamath, 2018), which have been associated with an increased risk of developing COPD (Maesano et al., 2019). Furthermore, studies have observed that farmers have a higher prevalence of COPD (5.1%) compared to the general population (2.9%), even though the prevalence of smoking among farmers is lower (Guillien et al., 2018). Farmers with COPD are more likely to have respiratory symptoms since farm tasks can produce hazardous aerosols which trigger respiratory inflammatory responses (Nordgren & Charavaryamath, 2018) and aggravate symptoms of COPD (GOLD, 2020).
Prior studies revealed that farmers tended to have higher prevalence of psychological distress than general populations (Austin et al., 2018; Fragar et al., 2010; Torske et al., 2016). Individuals with COPD also were reported as having an increased risk of psychological distress (Ivziku et al., 2019; Karadag et al., 2008; Kühl et al., 2008; Wagena et al., 2005). Multiple co-morbid conditions and smoking were reported as risk factors of developing psychological distress in people living with COPD (Verhaak et al., 2005) while age, profitability (Feng et al., 2015), drought (Hanigan et al., 2018), and exposure to pesticides (Harrison & Mackenzie Ross, 2016) also influenced psychological distress among farmers.
Psychological distress has been linked to worsening respiratory symptoms (Yohannes & Alexopoulos, 2014) and has the potential to trigger an acute exacerbation of COPD (Werchan et al., 2019). Understanding every possible risk factor for COPD exacerbation is important since this critical event is negatively related to the prognosis of the disease (Çolak et al., 2019), health-related quality of life (Gayan-Ramirez, 2018), and mortality rate (García-Sanz et al., 2017). In fact, increasing numbers and severity of acute COPD exacerbations are related with increased risk of death (Rothnie et al., 2018). Therefore, it is critical to understand the relationships of potential exacerbation triggers with exacerbation frequency and severity among people diagnosed with COPD.
Symptoms of COPD have been found to be bidirectionally associated with psychological distress (Atlantis et al., 2013), as psychological distress can exacerbate COPD symptoms (Liccardi et al., 2018; Mathew et al., 2019; Pembroke et al., 2006; Pumar et al., 2014), while COPD symptoms can, in turn, contribute to the development of psychological distress (Atlantis et al., 2013; Pumar et al., 2014). It was reported that factors related to COPD symptoms such as inflammation and hypoxia potentially impact the prevalence of depression in people with COPD, as well as the COPD outcomes such as severity of the disease, functional limitation, and quality of life (Pumar et al., 2014). Conversely, the COPD symptoms might be triggered by infections in the patients with immunization impaired by phycological distress (Pumar et al., 2014). Another potential link is that psychological distress may contribute to airway constrictions by increasing basal cholinergic tone and/or vagal fluctuations (Liccardi et al., 2018).
Farmers are exposed to specific risk factors of both psychological distress and symptoms of COPD. Furthermore, psychological distress is related to worsening respiratory symptoms in people with COPD. As a result, farmers with COPD may be in danger of worsening COPD symptoms and COPD exacerbation due to psychological distress, and COPD symptoms and exacerbations may lead to psychological distress. Prior studies have revealed potential influences of psychological distress on worsening respiratory symptom and inducing COPD exacerbation; however, no studies have examined this among farmers, which is the purpose of this study.
Methods
We conducted a secondary data analysis using data from publicly available components of the Behavioral Risk Factor Surveillance System (BRFSS) 2017 (Centers for Disease Control and Prevention [CDC], 2018). This is the nation’s premier system of health-related telephone surveys that collects data in all 50 states, the District of Columbia, and participating U.S. territories. This study used only publicly available components of the BRFSS, which was considered a University of Alabama at Birmingham IRB-approved public data set.
The respondents of BRFSS (CDC, 2018) were individuals aged 18 or older residing in the United States who were randomly selected using telephone numbers. The dataset did not include industry and occupational data, therefore, we used specific survey questions as a proxy to identify farmers. In 2017, the BRFSS included 450,016 respondents across the United States, in which 2,994 participants answered that they did farm or ranch work for the question “What type of physical activity or exercise did you spend the most time doing during the past month” and the question “What other type of physical activity gave you the next most exercise during the past month.” Among these 2,994 identified farmers, 318 answered questions in the section on respiratory health (COPD symptoms), and among those, 239 answered the questions about psychological distress, resulting in final sample of 239 participants.
Measures
The dependent variable was COPD symptoms, while the independent variable was psychological distress among farmers. Individuals were classified as having COPD symptoms if they answered “yes” to one of three questions indicating in the past 3 months if they had a cough on most days, coughed up phlegm or mucus on most days, and/or had shortness of breath either when hurrying on level ground or when walking up a slight hill or stairs.
Psychological distress of the respondents was evaluated using the question “within the last 30 days, how often have you felt this kind of stress.” This question prologue explains that “stress means a situation in which a person feels tense, restless, nervous, or anxious, or is unable to sleep at night because his or her mind is troubled all the time.” The respondents who answered, “None of the time” for this question were labeled as not having psychological distress, while those who answered “A little of the time” to “All of the time” were classified as having psychological distress.
Covariates study included age (imputed value), health status, and smoking. Health status was defined as general health evaluated by the question “would you say that in general, your health is,” which could be responded with a 5-rating scale answer ranging from poor to excellent. Smoking was described as tobacco use evaluated by the question “Have you smoked at least 100 cigarettes in your entire life,” which could be responded with “yes” or “no.”
Data Analysis
Sample mean, standard deviation (SD), frequency, and proportion were used to summarize the demographic characteristics of the participants. The differences between participants with and without COPD symptoms were evaluated with two-sample t test and Chi-square test where appropriate. The associations between COPD symptoms occurrences and each of the potential risk factors were explored with both unadjusted and adjusted logistic regressions. Unadjusted odds ratio (OR), covariates adjusted ORs, and the 95% confidence interval (95% confidence interval [CI]) were reported. Potential interactions were evaluated and removed from the multiple logistic regression model if not significant. All the tests were two-tailed under the significance level of 0.05. The statistical analyses were conducted using R version 4.0.2 (R Core Team, 2020).
Results
The average age of participants was 60 years of age with the SD of 13.4 (Table 1). The majority were male (70.3%) and white (95.4%). About half (47.3%) reported household incomes of $50,000 or more per year. Approximately one-third (31.4%) reported at least one COPD symptom, and almost half (45.4%) reported psychological distress symptoms. Most of them reported a good or a very good health status (34.6% and 38.0%, respectively) versus excellent (15.6%), fair (10.1%), and poor (1.7%). Slightly more than half reported not-smoking, compared to those that did (43.9%). Among farmers with COPD, they were more likely to be older (age M = 63.2 vs 59.1, p =.0279). Farmers with COPD symptoms reported having poorer health (20.2% vs 5.4%, p =.0017), and were more likely to report having psychological distress (57.3% vs 39.6%, p = .0107)
Demographic Characteristics Among Farmers (N=239)
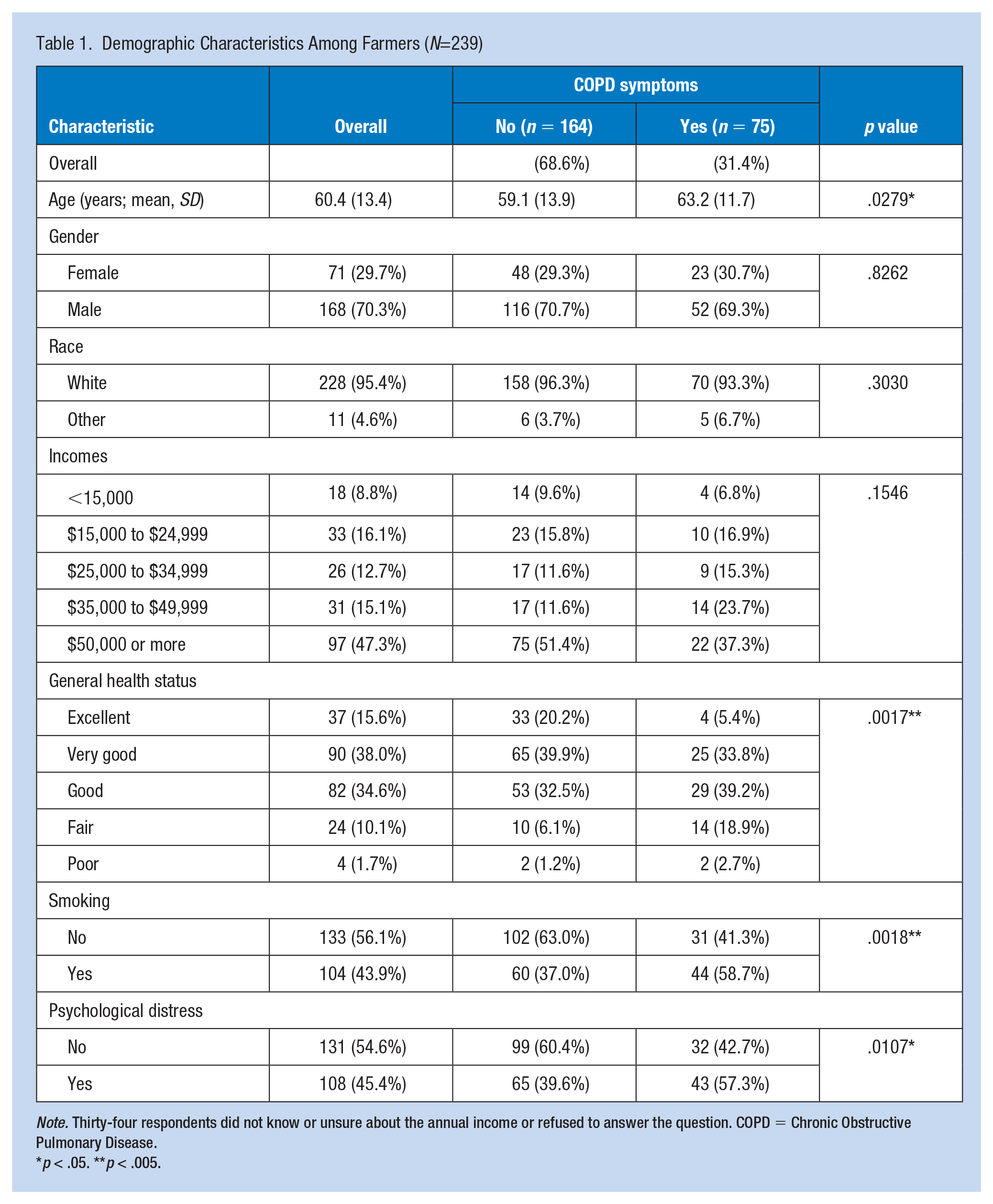
Note. Thirty-four respondents did not know or unsure about the annual income or refused to answer the question. COPD = Chronic Obstructive Pulmonary Disease.
p < .05. **p < .005.
The unadjusted logistic regression analysis suggested that the odds of COPD symptom occurrence for the farmers with psychological distress was 2.05 (95% CI = [1.18, 3.58]) times the odds for those without psychological distress (Table 2). It also showed that the risk of COPD symptom occurrence was significantly associated with age (OR = 1.02, 95% CI = [1.00, 1.05]), general health status (OR = 1.86, 95% CI = [1.36, 2.59]), and smoking (OR = 2.41, 95% CI = [1.39, 4.25]).
Multiple Logistic Regression of COPD Symptoms Associated With Psychological Distress Among Farmers (n = 239)
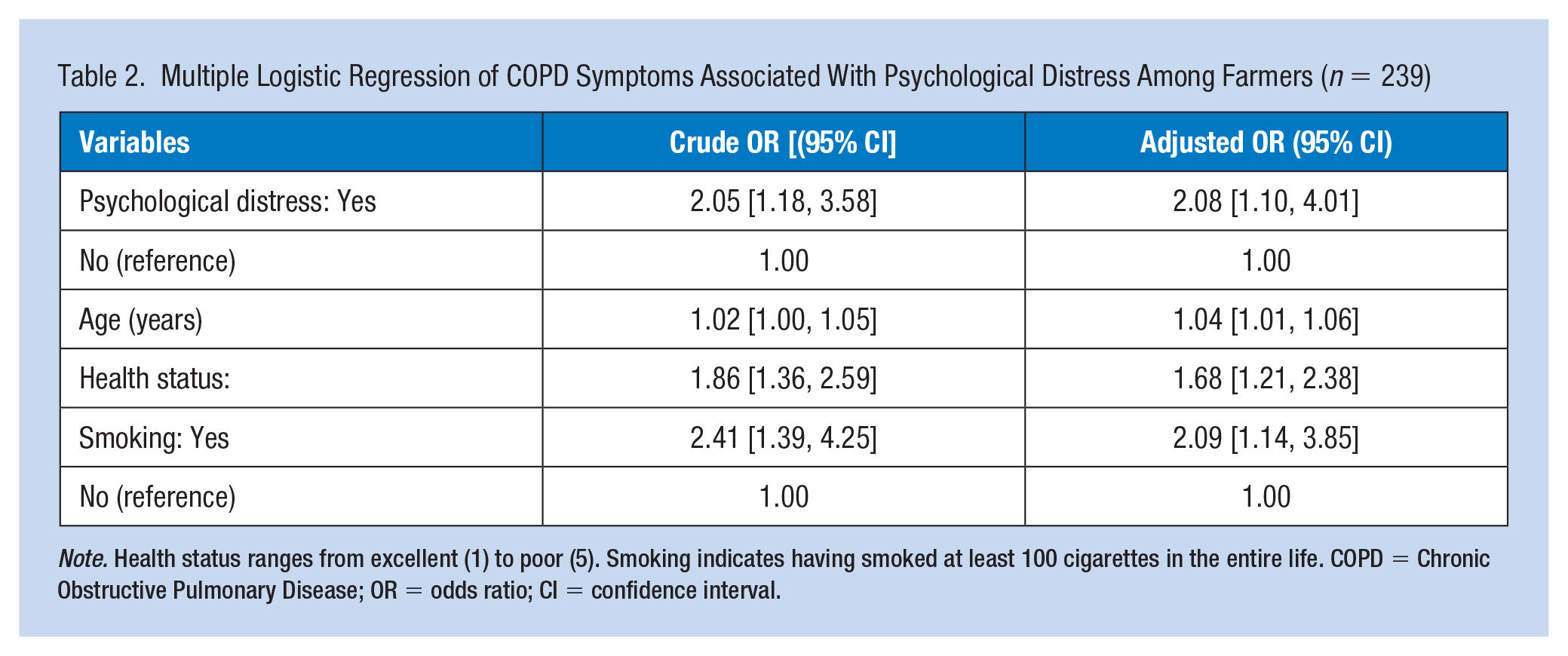
Note. Health status ranges from excellent (1) to poor (5). Smoking indicates having smoked at least 100 cigarettes in the entire life. COPD = Chronic Obstructive Pulmonary Disease; OR = odds ratio; CI = confidence interval.
The adjusted model yielded a significant model (p < .0001) with acceptable performance (C-statistic = .72). The odds of COPD symptom occurrence for the farmers with psychological distress was 2.08 (95% CI = [1.10, 4.01]) times greater relative to those without psychological distress after controlling for smoking, age, and health status. It was also revealed that smoking status (OR = 2.09, 95% CI = [1.14, 3.85]), age (OR = 1.04, 95% CI = [1.01, 1.06]), and general health status (OR = 1.68, 95% CI = [1.21, 2.38]) remained significantly associated with the occurrence of COPD symptom after controlling for each other.
Discussion
The results of this study showed that farmers with psychological distress might have increased risk of COPD symptom occurrence, which is consistent with prior studies conducted with the general population (Werchan et al., 2019; Yohannes & Alexopoulos, 2014). According to the prior studies, the association between COPD symptoms and psychological distress could be bidirectional (Atlantis et al., 2013). It was reported that psychological distress could trigger COPD symptoms by contributing to airway constriction (Liccardi et al., 2018; Mathew et al., 2019). Liccardi et al. (2018) explained this potential causal effect of psychological distress that psychological distress could lead to the increased basal cholinergic tone and/or vagal fluctuations and causes airway constrictions. Another potential effect of psychological distress is that psychological distress could impair the immune system leading to respiratory infections, which can induce COPD symptoms (Pumar et al., 2014). Conversely, COPD symptoms can stimulate psychological distress in individuals with COPD. Previous studies showed that inflammation and hypoxia, which were common symptoms of individuals with COPD had a potential impact on the prevalence of depression and quality of life in people with COPD (Pumar et al., 2014).
The average age of study participants was 60 years which is consistent with the data from the 2017 Census of Agriculture which indicated that most farmers in the United States were 55 to 64 years old. We also found that more than one-third of the participants had at least one COPD symptom, implying that the possible prevalence of COPD symptoms among the participants were relatively high compared with the estimated prevalence of COPD in general population (7%–19%) (Mosenifar, 2020). This may be due to differences in definitions between Mosenifar’s study and ours. In this study, we used symptoms of COPD screened by a set of questions, whereas they estimated the prevalence of COPD based on a more specific screening method using both questionnaires and spirometry tests. It may also be possible that the prevalence of this disease in the general population is underestimated among farmers. The prevalence of farmers having psychological distress found in this study was 45%, which is higher than previous studies (31%–38%) (Feng et al., 2015; Fragar et al., 2010; Hoang et al., 2020).
This study is based on secondary data from the BRFSS, which was not designed particularly to explore the association between COPD symptoms and psychological distress among farmers. We had to apply answers to a question about psychological distress and three questions about COPD symptoms in the survey to assess for participants’ psychological distress and COPD symptoms. We also assumed that people who indicated that they spend the most time doing agricultural or ranch work in the previous month were farmers. Furthermore, BRFSS is a national survey of the population conducted across the United States, and not specifically among farmers. Furthermore, this was a secondary data analysis of cross-sectional data, and the causal effect of psychological distress on COPD symptoms among farmers cannot be inferred.
An important limitation of the study is the representativeness of the dataset to the U.S. population. The Respiratory Health (COPD symptoms) module was optional in the 2017 BRFSS, and only nine states asked questions about it. Furthermore, the questions in this module only questioned if the respondents had any breathing problems, which could not be used to classify whether the respondents had COPD. As a result, the variables analyzed in this study may not be as reliable as those assessed using specific standard measures, and the study’s findings cannot be inferred to the U.S. population. However, as a proof of concept effort to justify a study, analysis of this dataset suggests that the future study of relationships between psychological distress and COPD exacerbations among farmers is reasonable.
Another concern is that the majority of the participants in this study are white. Therefore, the findings of this study may not apply to people of other races or ethnic groups. However, the proportion of white farmers in this study was similar to that in the 2017 Census of Agriculture (United States Department of Agriculture, 2019). The findings of this study are limited as well since we cannot identify the causal effect of psychological distress on COPD symptoms since the association between these two variables can be bidirectional.
Despite the noted limitations of the study, it serves an important purpose. As a proof of concept effort to justify a study, analysis of this dataset suggests that the future study of relationships between psychological distress and COPD exacerbations among farmers is reasonable and would make an important contribution to our understanding of COPD exacerbation in this at—risk population.
Implications for Occupational Health Practice
This study revealed the potential influence of psychological distress on increasing COPD symptoms among farmers. Although further research is necessary, the results of this study suggest some implications for occupational health professionals, especially for occupational health nurses, occupational medicine physicians, and occupational health psychologists. It is critical for occupational health nurses responsible for promoting farmers’ health to assess their clients’ psychological distress. The campaigns for screening psychological distress among farmers, especially in those with COPD need to be launched. The occupational health nurses may also go a step further by developing programs or campaigns that can promote mental health and reduce psychological for farmers and individuals living with COPD. Occupational medicine physicians and advanced practice nurses who treat farmers with increased COPD symptoms or COPD exacerbation should be aware of the role of psychological distress in worsening COPD symptoms so that they may formulate with the patient a comprehensive treatment plan. Finally, it is necessary that occupational health psychologists and occupational health nurses work together to enhance mental health and minimize psychological distress among farmers, particularly those with COPD.
Applying Research to Occupational Health Practice
This study involved secondary data analysis using the 2017 BRFSS to evaluate the association between COPD symptoms and psychological distress among farmers. The results of this study showed that increased COPD symptom is significantly associated with psychological distress among farmers. It suggests that psychological distress may influence exacerbating symptoms of COPD among farmers living with COPD. It may be critical for occupational health professionals to be concerned about the initial impact of psychological distress on respiratory symptoms among farmers living with COPD. To promote their well-being, it is necessary to screen and prevent psychological distress among farmers with COPD, especially in those experiencing COPD exacerbation.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Exemption
This study used only publicly available components of the BRFSS, which was considered a UAB IRB-approved public data set. Furthermore, this study did not involve merging any of the data sets in such a way that individuals might be identified. As a result, this study was not considered human subject research.
