Abstract
Background:
Farmers with chronic obstructive pulmonary disease (COPD) often face both respiratory issues and psychological distress, which can exacerbate their condition. However, no prior research has examined how the frequency of respiratory symptoms is associated to psychological distress in these individuals. Therefore, this study aimed to explore this relationship among U.S. farmers living with COPD.
Methods:
A cross-sectional study involved 101 participants, a mix of on-site and online recruits, assessing respiratory symptoms and psychological distress in farmers with COPD. The study employed standard self-reported measures and utilized both simple and multiple linear regression to analyze the association between respiratory symptoms and psychological distress.
Findings:
Participants reported notably higher levels of respiratory symptoms (61.6 [SD = 13.3]) compared to the reference score of 12, along with elevated psychological distress (25.9 [SD = 10.6]). Factors like COPD duration, income, smoking, and emergency department (ED) visits correlated with respiratory symptoms, while age, COPD duration, income, smoking, pesticide exposure, and farm type were associated to psychological distress. Notably, even after accounting for age, smoking, and pesticide exposure, a significant association remained between respiratory symptoms and psychological distress (β = 0.46, p < .001).
Conclusion:
Respiratory symptoms were significantly associated to psychological distress, even when considering other factors. While this aligns with existing research, a future longitudinal study is crucial to establish the cause-effect relationship between these variables. Understanding this relationship could inform the development of targeted interventions to alleviate psychological distress in individuals with respiratory symptoms.
Implications for Occupational Health Nursing Practice:
The correlation between COPD symptoms and psychological distress in farmers emphasizes the need for integrated nursing care. Occupational health nurses should prioritize combined respiratory and mental health assessments.
Background
Farmers account for only 1.3 % of the U.S. population. However, they produce food materials used to manufacture clothing and many other products, making major contributions to the U.S. economy (Lepley, 2019). Farmers are surrounded by hazardous substances that can cause chronic obstructive pulmonary disease (COPD) (Fontana et al., 2017) and exacerbate respiratory symptoms in those who already have COPD (Global Initiative for Chronic Obstructive Lung Disease [GOLD], 2020). Farmers with COPD experience persistent restricted airflow and difficulty breathing which cannot be fully recovered (GOLD, 2020), and they may suffer periods of acute worsening of respiratory symptoms that are Acute Exacerbations of Chronic Obstructive Pulmonary Disease (AECOPD) (Whittaker et al., 2022).
Exacerbation of COPD is a life-threatening event related to lung function decline leading to serious consequences including decreased physical activity, poorer quality of life, and increased mortality (Ritchie & Wedzicha, 2020). Farmers with COPD face greater challenges in avoiding risk factors for acute exacerbations compared to the general population with COPD. Despite being highly exposed to harmful substances, the usage rates of respiratory protective devices among farmers are low (Damalas & Abdollahzadeh, 2016). If they continue to work on the farm, farmers deal with vapors, dust, gases, or fumes and run the risk of developing AECOPD (Fontana et al., 2017).
Farmers are also at a greater risk than non-farmers of developing psychological distress due to the uncertainty of finances, productivity, and market prices (Daghagh Yazd et al., 2019). It was reported that a considerable proportion (16%) of individuals with COPD perceive psychological distress to be a trigger for AECOPD (Werchan et al., 2019). It was also revealed that worsening COPD symptoms were significantly associated with psychological distress among people with COPD in general (Mathew et al., 2019).
The impact of psychological distress on COPD is still unclear. However, it has been shown that psychological distress can trigger COPD symptoms by increasing basal cholinergic tone and/or vagal variations, which can lead to airway constriction (Liccardi et al., 2018). Another factor is that psychological distress can impact the immune systems of people with COPD, consequently predisposing them to infections that trigger AECOPD (Pumar et al., 2014).
The potential role of psychological distress in worsening COPD symptoms has been reported among individuals with COPD in general, but no studies have examined this relationship among farmers with COPD. Given that farming activities may increase a farmer’s risk of developing AECOPD, it is crucial to comprehend any additional AECOPD risks that may exist among this vulnerable population. By preventing or minimizing AECOPD, farmers with COPD will have the opportunity to lead healthier lives and preserve their ability to work on the farm. Since psychological distress may be a trigger for AECOPD, it is important to understand the role of psychological distress in aggravating COPD symptoms. Therefore, this proposed study aims to explore (1) the frequency of respiratory symptoms and the level of psychological distress, (2) the factors related to increased respiratory symptoms and psychological distress, and (3) the association between respiratory symptoms and psychological distress among farmers living with COPD in the United States.
Methods
This study was a cross-sectional correlational study. The target population of this study was farmers with COPD in the U.S. Farmers, as defined in this study, were people engaged in agriculture, raising living organisms for food or raw materials. They might own the farmed land or work as laborers on land owned by others. Both male and female farmers who were 18 years and older were eligible to participate in this study. G-power was used to calculate the sample size with at least 95 participants required for this study. This study was approved by the University of Alabama at Birmingham Institution Review Board (IRB-300009183). All respondents received informed consent before conducting the survey.
Recruitment Strategies
Both on-site and online recruitment methods were used in this study. Flyers inviting farmers with COPD were distributed at the University of Alabama at Birmingham (UAB) COPD clinic. Online recruitment was conducted through Facebook. Organizations related to farmers and COPD were asked to post the study link on their Facebook pages. Also, paid Facebook ads were used to distribute the survey link to people who were farmers living with COPD. The target audience for Facebook ads were people associated with farming in the United States. All recruitment channels were launched at the same time, on November 2, 2022. The participants received a $25 electronic VISA gift card as an incentive after they completed the questionnaire.
To ensure data integrity, duplicate and inconsistent responses were excluded. “Fraudulent data” in this context refer to responses that may have been fabricated or submitted multiple times by the same individual, which can skew the study results. Measures were taken to identify and remove such responses, ensuring that the data collected accurately represented the target population of farmers with COPD. Overall, 579 responses were received: 575 from paid Facebook ads, three from free Facebook ads, and one from the UAB COPD clinic. However, only 414 respondents met the inclusion criteria and completed most of the survey. Potential fraudulent surveys were identified, and 246 duplicates were removed by comparing internet protocol (IP) addresses. Next, 145 inconsistent responses were excluded by checking for consistency between two sets of similar questions, leaving 101 responses for analysis.
Measures
Demographic Data
The respondents were asked to complete the survey following information: gender, age, years of experiencing COPD, emergency department (ED) visit history, race, income, smoking, pesticide exposure, work hours, off-farm job, and type of farm.
Level of Psychological Distress
The 10-item Kessler Psychological Distress Scale (K10) was used to assess the level of psychological distress among the respondents (Kessler et al., 2002). This instrument is in the public domain, valid (area under the curve [AUC] for content validity = 0.876), and reliable (Cronbach’s alpha = 0.92). The K10 is a self-report measure with a five-level response scale based on symptom frequency, yielding scores from 10 to 50, where higher scores indicate greater distress. The scale consists of 10 questions that ask about the frequency of various symptoms of distress over the past 30 days such as tired, nervous, hopeless, and depressed. Scores range from 10 (all answers “none of the time”) to 50 (all answers “all of the time”). Certain questions are linked; for instance, answering “none of the time” for questions 2 and 5 automatically scores 1 for questions 3 and 6. Scores of 10 to 15 indicate low distress, 16 to 21 moderate distress, 22 to 29 high distress, and 30 to 50 very high distress (Kessler et al., 2002).
Frequency of Respiratory Symptoms Data
The frequency of respiratory symptoms was assessed using part one of the St George’s Respiratory COPD-specific questionnaire (SGRQ-C), which includes seven questions (1–7). These questions inquire about the individual’s respiratory symptoms over the past three months such as coughing, sputum production, and breathlessness. Each question has a specific weight. Scores were generated by summing the weights for questions 1 to 7, dividing by the maximum possible weight for this section, and presenting the results as a percentage. Scores range from 0 to 100 with higher scores indicating more frequent respiratory symptoms.
The SGRQ-C part 1 does not offer specific interpretations for each score range. It generally signifies that a score of 0 represents no impairment, while a score of 100 represents maximum impairment (Jones, 2012). However, it has been found that SGRQ-C scores correlate with COPD severity levels. According to Rehman et al. (2020), an SGRQ-C score of around 40 approximately corresponds to a mild level of COPD symptoms. In addition, Horner et al. (2020) indicated that the average difference in SGRQ-C scores between each severity level is around 10 units. Therefore, for easier interpretation, SGRQ-C scores of 40, 50, 60, and 70 or more can be taken to suggest mild, moderate, severe, and very severe COPD respiratory symptoms, respectively. For example, if a respondent has an SGRQ-C score of 55, it implies that their level of respiratory symptoms is between moderate and severe. This instrument is also in the public domain and is regarded as reliable (person separation index [PSI] = 0.90) (Meguro et al., 2007) and valid (the correlations with existing standard respiratory symptom measures were tested [r = 0.64 – 0.79]) (Rehman et al., 2020).
Data Collection
The data for this study were collected online. All participants completed the screening questions and completed the consent form online through Qualtrics. To prevent missing data, all key items were designated as mandatory questions. Respondents recruited from the UAB COPD clinic accessed the survey by scanning the QR-code or typing in the URL address provided in the flyers. Those recruited through Facebook accessed the survey by clicking on the link attached with the Facebook ads.
Data Analysis
Data from the questionnaires were reviewed and transformed to ensure suitability for statistical analysis. This included converting data from ratio level to interval level, or binary as necessary to meet the requirements of the analytical methods employed. Means, standard deviation (SD), frequency, and proportion were used to summarize the demographic characteristics of the respondents. Two sample t-test or analysis of variance (ANOVA) was employed to compare the mean scores of the frequency of respiratory symptoms and the level of psychological distress. Simple linear regression was used to explore the correlations between the frequency of respiratory symptoms and each of the potential associated factors (such as age, smoking, and pesticide exposure), as well as the correlation between the level of psychological distress and each of the potential associated factors.
The associations between the frequency of respiratory symptoms and level of psychological distress were explored with both simple and multiple linear regression. For the multiple regression analysis, age, smoking status, and history of pesticide exposure were statistically controlled because they were identified factors related to increased respiratory symptoms among people with COPD (Kham-Ai et al., 2023; Pourhassan et al., 2019). The standardized coefficient (β), F-value, and the effect size of the model (Adjusted R2) were reported. All the tests were two-tailed under the significance level of 0.05. All statistical analyses were conducted using R version 4.0.2 (R core team, 2020).
Findings
Respondent Characteristics
As described in Table 1, among the total 101 respondents in this study, most of them (77%) were males. The average age of respondents was 40 years old and the average period of experiencing COPD was about 5 years. However, more than half of the respondents (58%) reported visiting the emergency department twice or more in the previous year due to shortness of breath. Most of the respondents (72%) chose not to disclose their race. However, of those who reported race, 72% were African American.
Characteristics of the Respondents
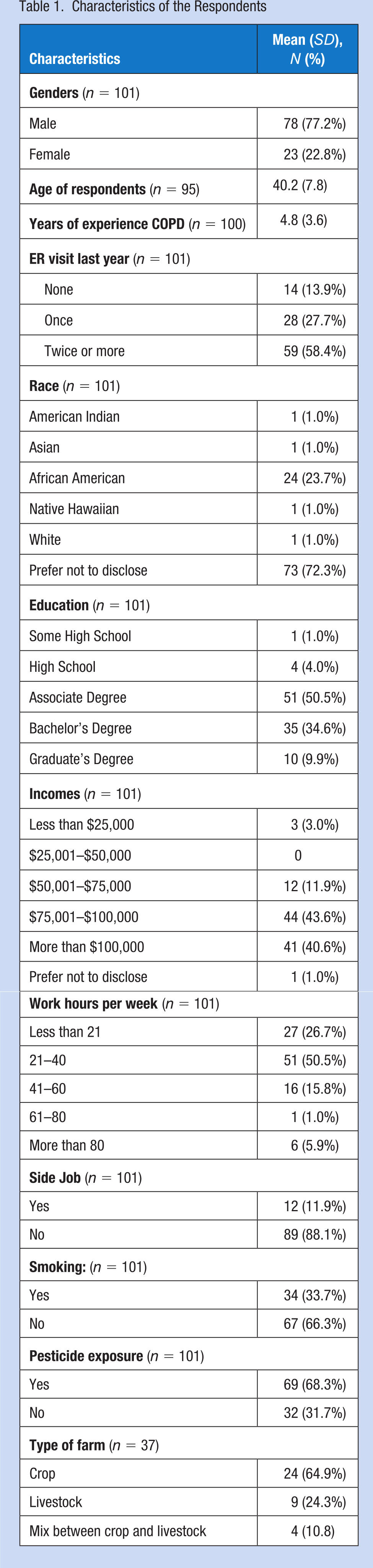
The majority of the respondents graduated from colleges with associate degree (50%) and bachelor’s degree (35%). Forty-three percent had annual incomes between $75,001 and $100,000, while another 40% made more than $100,000 a year. Half of the respondents worked on the farm for 21 to 40 hours per week, and most of them (88%) did not have any off-farm jobs. More than half of the respondents (68%) indicated that they were exposed to pesticides. Even though all of the respondents had been diagnosed with COPD, 34% of them were still smoking. Only 37 of 101 (31 %) respondents provided information for the type of farm employment and most of the responses (65%) indicated that they worked on a crop farm.
Frequency of Respiratory Symptoms and Level of Psychological Distress
Frequency of Respiratory Symptoms
The average score of the frequency of respiratory symptoms (SGRQ-C score) among the respondents was 61.6 (SD = 13.3), indicating that they had a severe level of respiratory symptoms. It was also found that mean scores were not significantly different according to age, gender, race, education, work hours, off-farm job, pesticide exposure, or type of farm. However, the average score of the frequency of respiratory symptoms among the respondents was significantly different based on income (p = .020), smoking status (p < .001), and history of ED visits in the previous year (p = .001) (Table 2).
Frequency of Respiratory Symptoms and Level of psychological distress of the Respondents
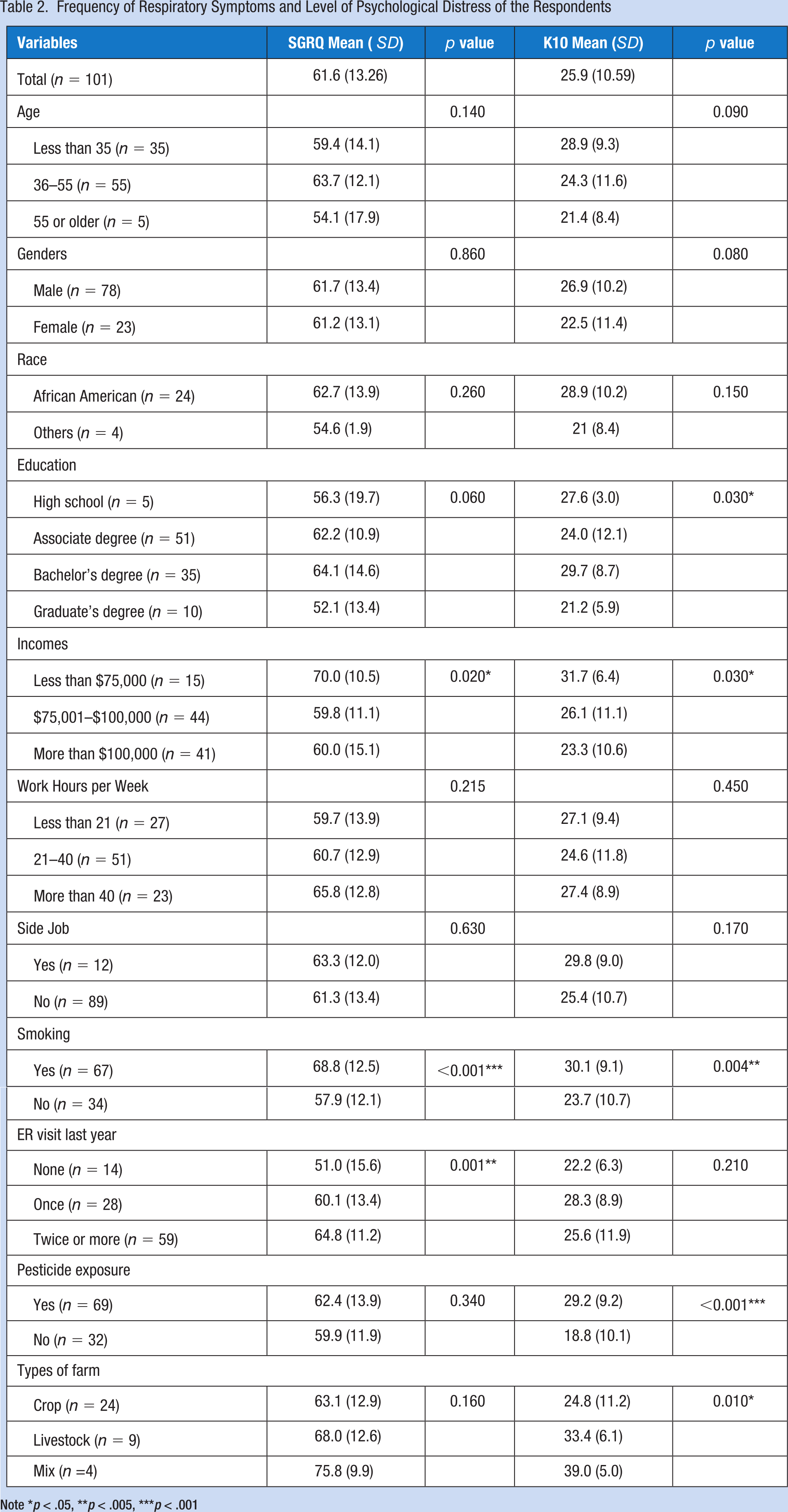
Note *p < .05, **p < .005, ***p < .001
Level of Psychological Distress
The average score of the level of psychological distress was 25.9 (SD = 10.6), indicating that they experienced a high level of psychological distress. There were no significant differences in this score among the respondents based on age, gender, race, work hours, off-farm job, or history of ED visits in the previous year. However, the average score of the level of psychological distress among the respondents was significantly different based on education (p = .030), income (p = .030), smoking status (p < .004), pesticide exposure (p < .001), and type of farm (p = .010) (Table 2).
Factors Related to Increased Respiratory Symptoms and Psychological Distress
Factors Related to Increased Respiratory Symptoms
The statistical analysis showed that the number of years post-COPD diagnosis, income, smoking, and history of ED visits in the previous year were factors associated with the frequency of respiratory symptoms. Number of years post-COPD diagnosis was significantly associated with an increased frequency of respiratory symptoms (β = 1.09, p = .002).
Income was negatively associated with the frequency of respiratory symptoms. Respondents who made $75,001 to $100,000 a year (β = −10.21, p = .009) and those earning more than $100,000 a year (β = −10.06, p = .011) had significantly lower scores for the frequency of respiratory symptoms compared to those with an annual income of less than $75,000. Respondents who smoked tended to have higher scores for the frequency of respiratory symptoms compared to those who did not smoke (β = 10.85, p < .001). Similarly, respondents who visited the ED once (β = 9.26, p = .027) or at least twice (β = 13.85, p < .001) in the previous year due to shortness of breath tended to have higher scores than those who never visited the ED (Table 3).
Factors Associated With Increased Respiratory Symptoms
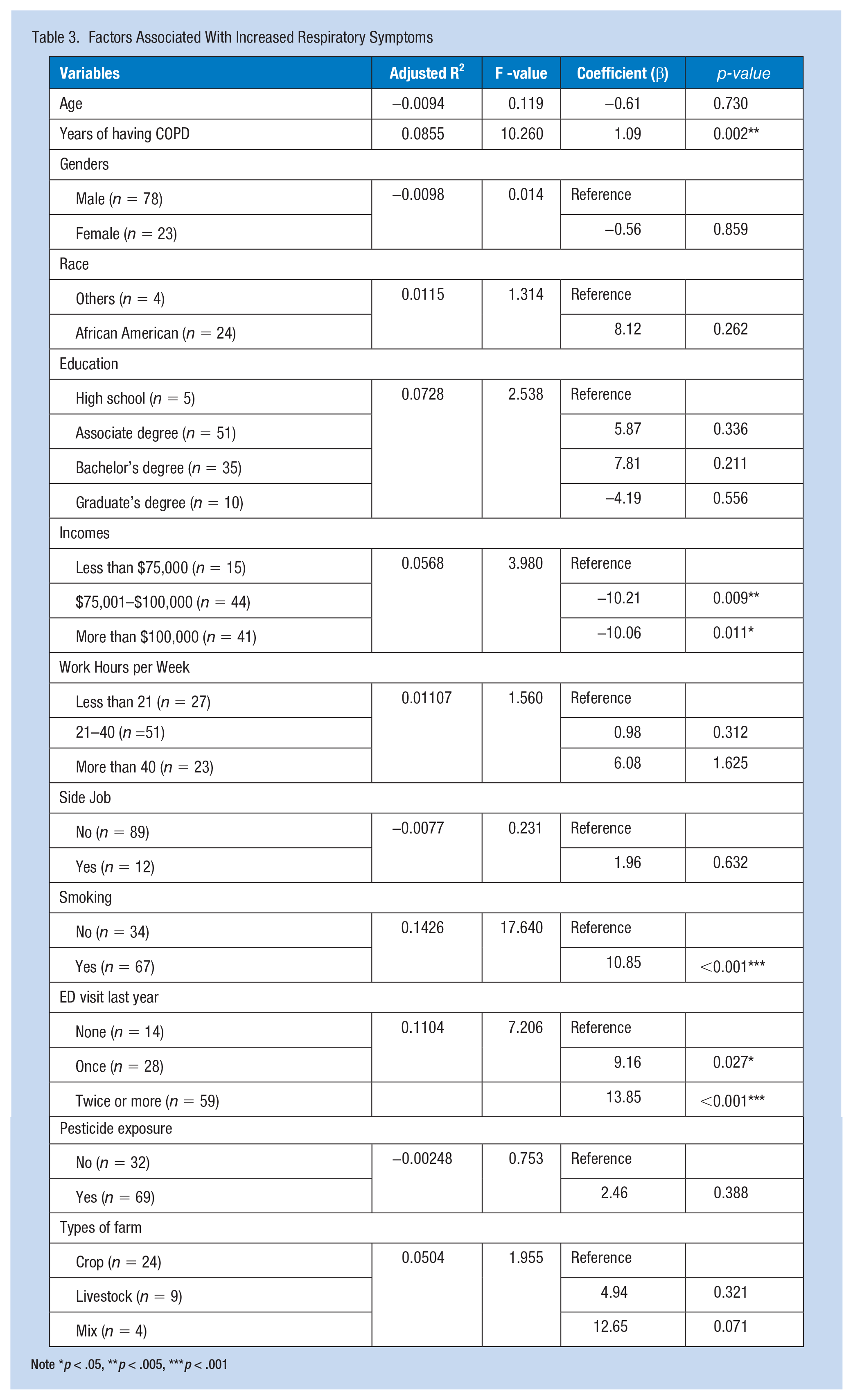
Note *p < .05, **p < .005, ***p < .001
Factors Related to Psychological Distress
Simple linear regression analysis showed that age, years with COPD, income, smoking status, pesticide exposure, and type of farm were significantly associated with the level of psychological distress. It was found that older age was significantly associated with a decrease in the level of psychological distress (β = −0.47, p < .001). However, the number of years experiencing COPD was significantly associated with a higher level of psychological distress (β = 0.69, p = .019). Respondents with an annual income of more than $100,000 had significantly lower levels of psychological distress compared to those earning less than $75,000 a year (β = −8.39, p = .008).
Another factor related to the level of psychological distress was smoking. Respondents who smoked had significantly higher levels of psychological distress compared to those who did not smoke (β = 10.85, p < .001). The results also indicated that respondents exposed to pesticides had significantly higher levels of psychological distress compared to those without pesticide exposure (β = 10.33, p < .001). Respondents who worked on livestock farms had significantly higher levels of psychological distress than those who worked on crop farms (β = 8.65, p = .030), and those who worked on both crop and livestock farms also had significantly higher levels of psychological distress than those who worked solely on crop farms (β = 14.21, p = .011) (Table 4).
Factors Associated With the Level of Psychological Distress
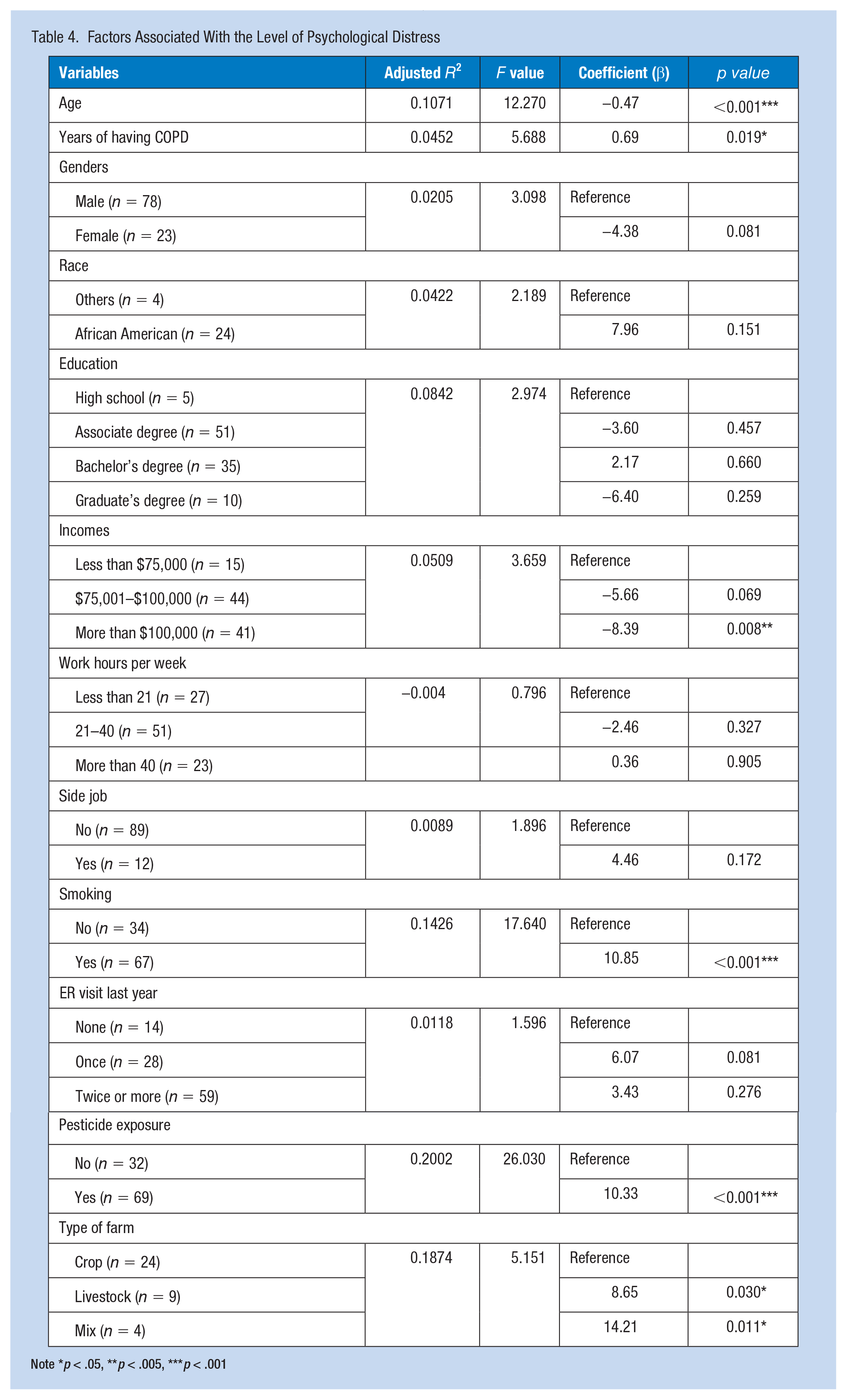
Note *p < .05, **p < .005, ***p < .001
Association Between the Frequency of Respiratory Symptoms and the Level of Psychological Distress
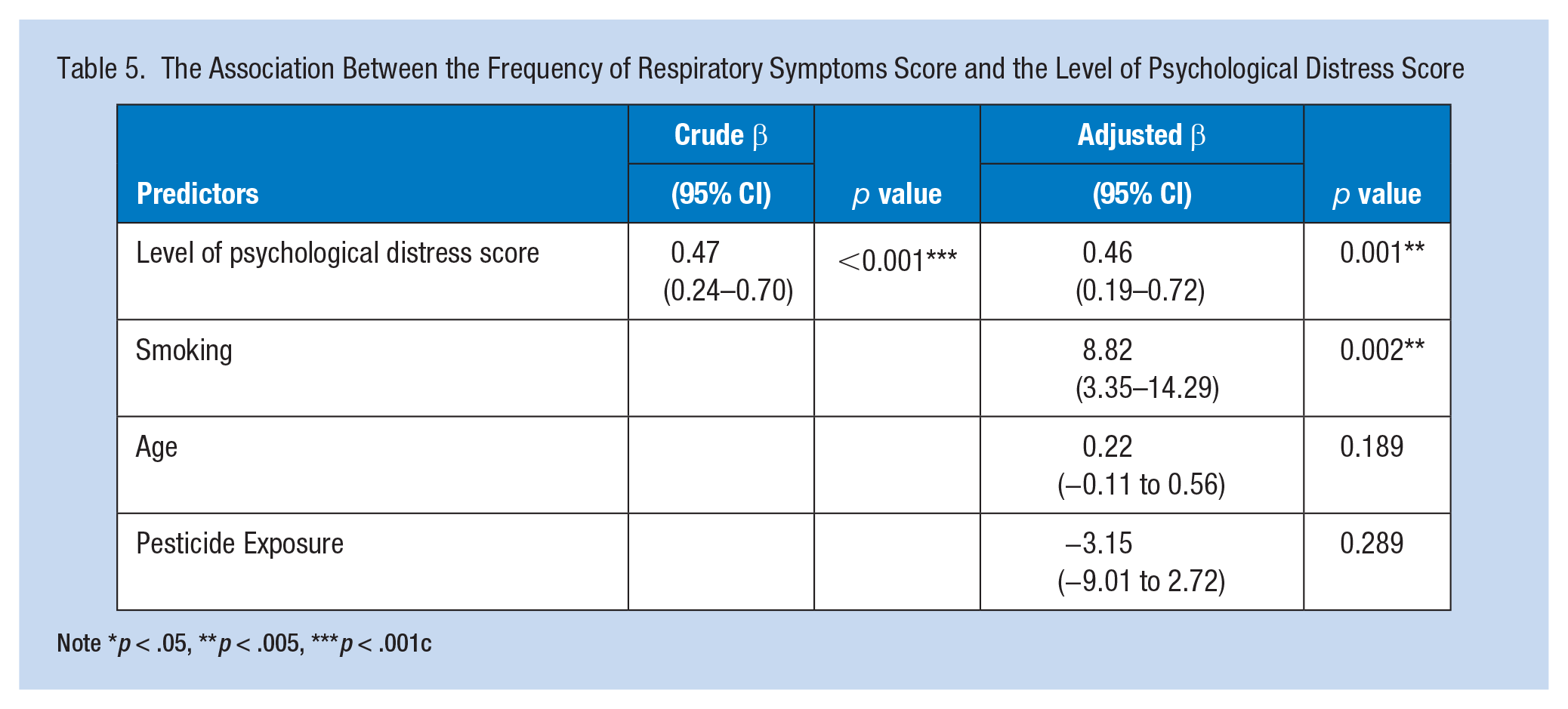
As presented in Table 5, simple linear regression showed that the frequency of respiratory symptoms was significantly associated with the level of psychological distress (β = 0.47, p < .001). In the multiple linear regression test, the frequency of respiratory symptoms was still significantly associated with the level of psychological distress (β = 0.46, p < .001) after controlling for the variables age, smoking status, and history of pesticide exposure.
The Association Between the Frequency of Respiratory Symptoms Score and the Level of Psychological Distress Score
Note *p < .05, **p < .005, ***p < .001c
Discussion
This study found that the average age of the participants was 40 years old, which is lower than the average age of farmers in the United States (57 years old) (United States Department of Agriculture, 2017). Furthermore, the average age of the participants was relatively low when considering that they were diagnosed with COPD, which is more common in older adults (GOLD, 2020).
The lower average age observed in our study might be influenced by several factors that warrant further exploration. First, it is important to consider whether participants had comorbidities that could impact their COPD diagnosis and age distribution. Second, investigating participants’ smoking history and exposure to other inhalants such as pesticides or industrial fumes, could provide insights into potential risk factors contributing to COPD at a younger age. In addition, the demographic skew toward younger participants could partly be attributed to the nature of online surveys, which tend to attract younger respondents more readily than older demographics (Dillman et al., 2014). Furthermore, generational differences in health care trust, access, and overall utilization could explain this phenomenon. Younger individuals might have different attitudes toward participating in health-related studies, better access to online resources, and a greater tendency to seek medical attention earlier, leading to earlier diagnosis of COPD. The average age of individuals with COPD also varies depending on the stage of COPD, as it is lower among people with the initial stages and higher among those with the more severe stages (Martinez et al., 2016).
The average score (SGRQ-C) of the frequency of respiratory symptoms of the participants was 61.6 (SD = 13.3) implying that they had a severe level of respiratory symptoms. This finding is consistent with previous studies, which found that farmers with COPD tended to have more respiratory symptoms, compared to non-farmers with COPD (Clark et al., 2014; Woldeamanuel et al., 2020). Also, the average score of the level of psychological distress in the current study was 25.9 (SD = 10.6) indicating that participants had a high level of psychological distress. This is consistent with the results from Wang et al. (2023) indicating that psychological distress is common among individuals with COPD (80% of the participants experienced psychological distress). The results of this study are also consistent with the study by Rudolphi et al. (2020) that investigated psychological distress among young farmers and found that more than half of the participants met the criteria of having a psychological distress issue.
This study demonstrates a significant association between the frequency of respiratory symptoms and the level of psychological distress. This finding aligns with the research by Kham-Ai et al. (2023), which utilized secondary data from the 2017 Behavioral Risk Factor Surveillance System (BRFSS) to examine the relationship between COPD symptoms and psychological distress among farmers. Their analysis revealed that COPD symptoms were significantly associated with psychological distress among farmers even after adjusting for smoking, age, and health status (aOR = 2.08 [1.10, 4.01], p = .0261).
Other studies have investigated the association between COPD symptoms and psychological distress among people with COPD in general and found that COPD symptoms included breathlessness (Mathew et al., 2019), reduced lung function (Pembroke et al., 2006), and general negative COPD outcomes (Atlantis et al., 2013). Similar trends were found from longitudinal studies that explored the association between COPD acute exacerbation and found that increased COPD exacerbation was associated with psychological distress (Huang et al., 2021; Montserrat-Capdevila et al., 2018). Therefore, findings from this study are consistent with those in the existing literature.
Based on the findings of this study, screening for psychological distress among farmers with COPD should be considered to prevent its potential consequence of worsening respiratory symptoms in this population. Furthermore, clinicians should provide education and training on psychological distress management techniques as well as information about low cost available resources (such as websites, podcasts, or support groups) to farmers with COPD to make sure that they have access to psychological support when needed.
This study demonstrates a positive association between the frequency of respiratory symptom scores and levels of psychological distress scores among farmers living with COPD. This empirical evidence supports the hypothesis that psychological distress may worsen COPD respiratory symptoms in this population. However, further research is necessary to investigate this relationship within a broader and more diverse population. A longitudinal study design would be particularly valuable to explore the causal association between increased respiratory symptoms and psychological distress among farmers with COPD. In addition, future studies could benefit from incorporating objective measures of respiratory symptoms such as spirometry, to strengthen the study’s validity and reliability.
Limitations
As a cross-sectional correlational research, this study cannot define the causal relationship between the increased respiratory symptoms and psychological distress. Another major drawback of correlational studies is that the associations observed from the study may be influenced by unmeasured confounders. In addition, this study is the on-site recruitment of participants, which was conducted exclusively at a single COPD clinic at the University of Alabama at Birmingham. This may limit the generalizability of the findings as the sample may not fully represent the broader population of farmers with COPD. Future studies should consider recruiting from multiple clinical sites to enhance the diversity and representativeness of the sample.
The survey of this study was administered only in English which may have excluded farmers who are not proficient in English and resulted in a loss of potentially valuable participants. Also, this study used an online recruitment strategy and provided financial incentives; the risks of fraudulent activities such as multiple submissions by the same individual, were heightened, potentially compromising the study’s internal validity. Even though a fraud detecting software was used, there were significant number of potentially fraudulent responses. Therefore, future studies recruiting the participants online may need more restrictive strategies to detect fraudulent responses. An example of this strategy is tracking participants by using personal data.
Conclusion
The main finding of this study was that the frequency of respiratory symptoms is significantly associated with the level of psychological distress after controlling for other related factors. Even though this finding is consistent with existing literature, a longitudinal study is needed in future research to evaluate the causal association between the frequency of respiratory symptoms and the level of psychological distress.
Implications for Occupational Health Nursing Practice
The significant association identified between the frequency of COPD symptoms and psychological distress among farmers underscores the critical need for proactive and integrated occupational health nursing interventions. Acknowledging this relationship, nurses in occupational health settings should prioritize comprehensive assessments that consider both respiratory health and mental well-being among farming populations. Implementing tailored interventions such as regular health screenings, targeted education on symptom recognition, and access to mental health support can significantly contribute to early detection, management, and improved overall health outcomes.
Furthermore, advocating for and supporting longitudinal studies within this context will enhance the understanding of causality, enabling the development of more precise and impactful nursing strategies to promote the holistic health of farmers such as creating individualized care plans with respiratory therapy and mental health counseling. These approaches can be generalized to the broader U.S. farmer population ensuring effective occupational health nursing interventions nationwide. In addition, the farming industry should enhance respiratory protection, improve ventilation, and adopt safer pesticide practices. Combined with nursing strategies, these measures will comprehensively safeguard farmers’ respiratory and mental health.
Applications to Professional Practice
In this cross-sectional study among farmers, an investigation into the relationship between COPD symptoms and psychological distress revealed a significant correlation even after adjusting for relevant factors. This finding emphasizes the interconnectedness of respiratory health and mental well-being within farming communities. By recognizing this association, occupational health practitioners can implement targeted interventions encompassing comprehensive health assessments, education on symptom recognition, and accessible mental health support. These efforts aim to enhance early detection, holistic care, and improved overall well-being among farmers, underscoring the value of integrated health strategies in occupational settings
Footnotes
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Alabama Famer Federation (no grant numbers)
Human Subjects Review
This study was approved by the University of Alabama at Birmingham Institution Review Board (IRB-300009183).
