Abstract
Background:
This study seeks to determine what handwashing facilities are available to workers, predominantly in the manufacturing and service industries, to find out if their workplace has the appropriate resources to conduct proper handwashing and how that affects handwashing satisfaction.
Methods:
This cross-sectional study surveyed U.S. adult workers (N = 241) on their workplace handwashing equipment and facilities. The associations between demographic characteristics, consistent handwashing, and handwashing satisfaction were evaluated using Fisher’s exact test.
Findings:
Eighty-eight percent of respondents reported consistent handwashing. Pulling a handle to exit the restroom was negatively associated with handwashing satisfaction (p = .004) and having difficulty with an automatic faucet or dispenser was negatively marginally significant in its association with handwashing consistency (p = .10).
Conclusion/Applications to Practice:
Greater understanding of the available equipment in workplace restroom facilities and how to improve selection and use of that equipment may improve workers’ handwashing experiences.
Background
Handwashing is one primary prevention method for halting the spread of pathogens. Although knowledge of handwashing importance is high, handwashing consistency rates can be low. One factor that influences proper handwashing is adequate equipment in restroom facilities because well-stocked facilities are shown to encourage handwashing (Centers for Disease Control and Prevention [CDC], 2021).
Consensus criteria for handwashing equipment and facilities are cleanliness, accessibility, and include a hands-free tap and soap dispenser, adequate water, and a disposable hand drying method (United Nations Children’s Fund [UNICEF] & World Health Organization [WHO], 2021). Barriers to effective handwashing include hand sanitizer becoming the primary source of hand hygiene, lack of no-touch technologies or ineffective operation of no-touch technologies (e.g., inadequate soap, inadequate water run time), rendering the handwashing process less effective (CDC, 2021).
While education and training can instill positive handwashing behaviors, environmental factors also influence handwashing. Access to proper equipment in restroom facilities to perform adequate handwashing is especially critical to workers. Workplace pathogens can proliferate, contaminate the environment, or spread to the community if workers are not engaging in proper handwashing. Studies on the social and environmental barriers to effective handwashing have largely focused on schools (Chittleborough et al., 2013; Grover et al., 2018; Reeves et al., 2012), healthcare settings (Houghton et al., 2020; Naikoba & Hayward, 2001), and food handling (Pragle et al., 2007; Todd et al., 2007; Verrill et al., 2021); however, few studies explore handwashing outside of these occupational settings. The purpose of this pilot descriptive, cross-sectional study was not only to build on the literature by determining what handwashing equipment is available in restroom facilities in a sample of workers—predominantly in manufacturing and service—but also to determine if workers find the restroom equipment in their work setting satisfactory to perform proper handwashing.
Methods
Survey data were collected from November 2020 to February 2021 via Qualtrics (Provo, Utah ©2020) from U.S. workers primarily from the manufacturing and service industries. Nonprobability and chain-referral sampling techniques were used. Participants (N = 312) aged 18 years and above completed the survey; telecommuting workers and workers predominantly working from home (n = 71) were excluded. A total of N = 241 were included in the final analysis.
The survey had eight demographic questions and 13 questions on workplace restroom handwashing facilities. Pictures accompanied answer selections to reduce ambiguity. Descriptive analysis of the main demographic and work characteristics of respondents, as well as facility characteristics, was determined. Fisher’s exact test was used to evaluate the association between these characteristics, consistent handwashing, and workers’ satisfaction with their ability to properly wash hands at their workplace. A value of p < .05 was considered statistically significant, while p
This study was approved by the University of Michigan institutional review board (Protocol ID HUM00189839).
Results
Consistent Handwashing
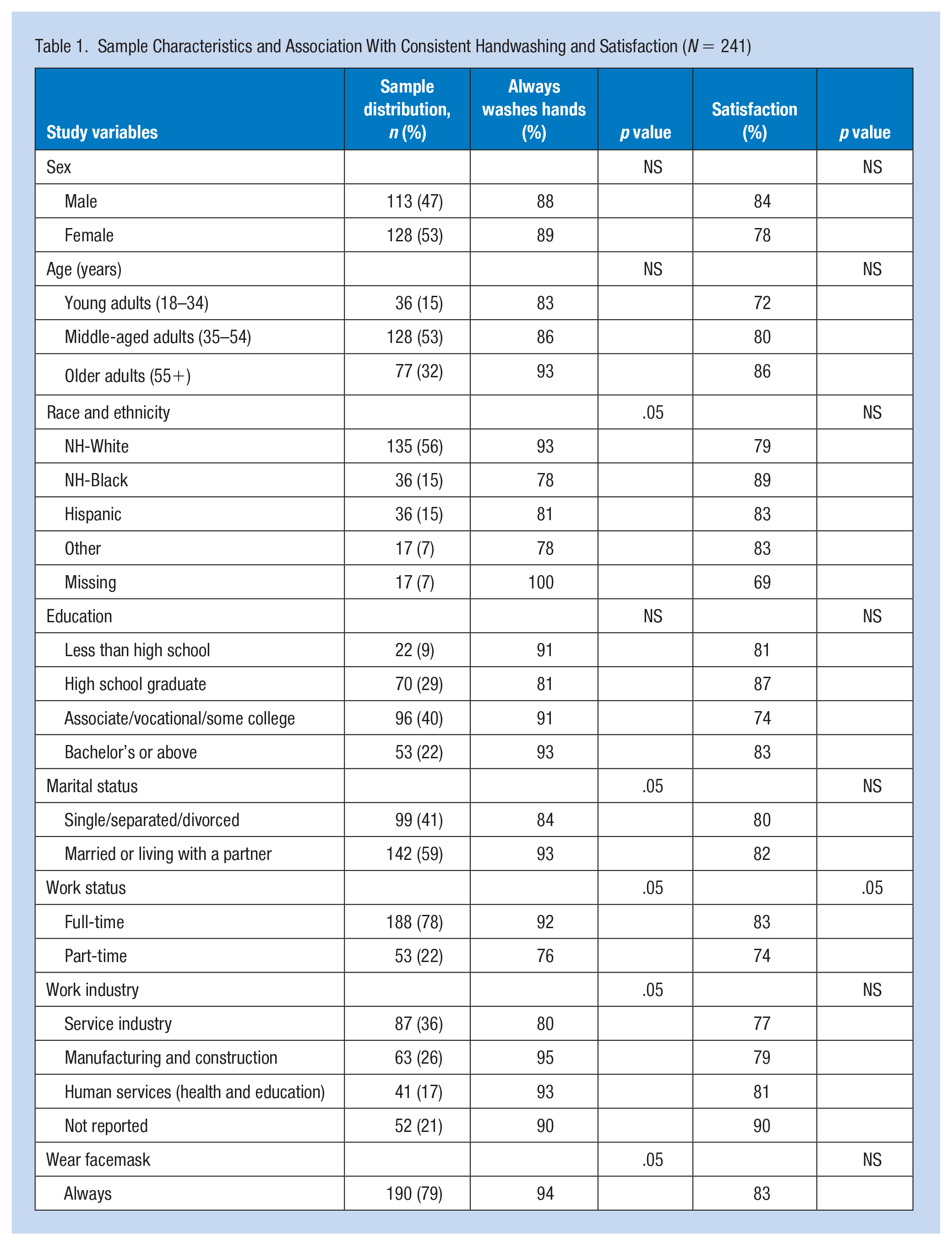
Eighty-eight percent (n = 212) of respondents reported always washing their hands after using the restroom, while the remaining 12% reported doing it very often or sometimes. Consistent handwashing was significantly associated with race and ethnicity (p = .002), with 93% of non-Hispanic Whites reporting consistent handwashing compared with 79% of respondents from other races and ethnicities. Consistent handwashing was also significantly associated with being married or cohabiting with a partner (p = .033), working full-time (p = .012), and working in the Manufacturing and Construction and Human Services sectors (p = .031) (Table 1). The only facility characteristic positively associated with consistent handwashing was a manual hand drying device compared with an automatic paper tower dispenser or hand dryer (93 vs. 83%). Pulling a handle to exit the restroom was negatively associated with consistent handwashing and having difficulty with an automatic faucet or dispenser was negatively marginally significant (Table 2).
Sample Characteristics and Association With Consistent Handwashing and Satisfaction (N = 241)
Restroom Facility Characteristics and Association With Consistent Handwashing and Satisfaction (N = 241)
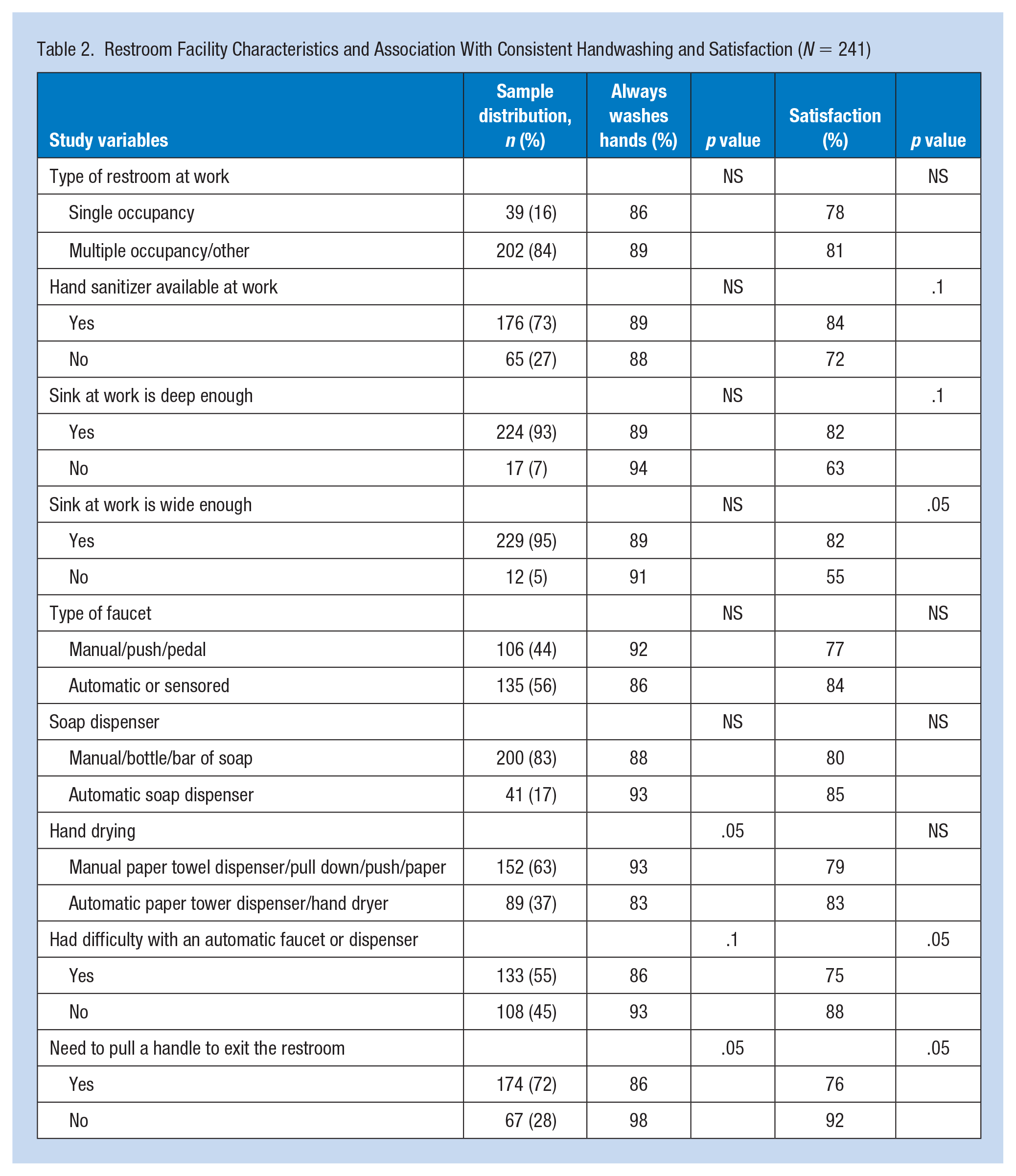
Handwashing Satisfaction
Eighty-one percent (n = 195) of respondents reported feeling satisfied with their ability to properly wash their hands at work. Characteristics positively associated with proper handwashing satisfaction included working full-time (p = .023) and having a sink large enough to perform hand hygiene without touching the sink basin (p = .042). Having a sink deep enough (p = .094) and having access to hand sanitizer (p = .063) were positively marginally associated with higher satisfaction (Tables 1 and 2). One third of respondents thought their workplace restroom facilities’ technology impeded handwashing quality due to short water run times. Pulling a handle to exit the restroom (p = .005) and having difficulty with an automatic dispenser (p = .013) were negatively associated with satisfaction in the ability to properly wash their hands (Table 2). No demographic characteristics were significantly associated with handwashing satisfaction.
Discussion
Workplace restroom facilities having adequate equipment to perform handwashing is critical to public health. In this study, surveying workers predominantly in the manufacturing and service industries, revealed that certain demographic characteristics (e.g., non-Hispanic White, married, or cohabitating) were significantly associated with handwashing satisfaction. An assessment of handwashing in more than 50 countries analyzed demographic and health information as indicators of handwashing behavior; the study found disparities in access and promotion to handwashing within countries (Kumar et al., 2017). Potential disparities in handwashing knowledge, access, and promotion among the U.S. diverse workforce need to be further explored.
A preference for manual hand drying (e.g., push-paddle or push bar paper towel dispenser) and dissatisfaction with restroom equipment technology (n = 80) indicates that technology may impede consistent handwashing—from start to finish—and satisfaction if there are sensor barriers/errors. While well-designed restroom equipment technology can facilitate handwashing, there are existing challenges (e.g., sensor detection and sensitivity) that can still be improved (Ram, 2013). Furthermore, it is critical for handwashing equipment to be regularly maintained to ensure its proper functioning to promote hand hygiene (e.g., sufficient water run times, water temperature, paper towels dispense without clogging).
Implications for Occupational Health Practice
Consistent handwashing was negatively associated with pulling a handle to exit the workplace restroom. Bathroom door handles can be rife with pathogens (CDC, 2021) and approximately three quarters of respondents had to touch an additional surface to exit, potentially rendering the handwashing process ineffective. Nearly two thirds of respondents did indicate using a paper towel to exit and nearly 75% had access to hand sanitizer immediately outside of the restroom to reperform hand hygiene. Handwashing satisfaction was positively associated with having a sink of sufficient width and depth, where the hands do not touch the basin. Additional research is needed not only on which sink designs but also which soap dispenser and hand drying mechanisms are optimal for proper handwashing. For example, some hand drying methods may spread more droplets (e.g., hand dryers) or require touching additional surfaces, and small, shallow sink designs with taps directly over the water drain lead to poor handwashing use in healthcare settings (Kotsanas et al., 2013; Marcenac et al., 2021). Handwashing barriers can be engineered-out in design.
Study limitations include self-reported data creating the possibility of social desirability bias (e.g., overreporting handwashing). Data were cross-sectional and subject to changes over time, given the survey was administered during the COVID-19 pandemic. In addition, the small sample size did not allow multivariate analyses and the study sample may not be representative of other industries. Limitations notwithstanding, this study underscores aspects of restroom facilities that may be associated with consistent handwashing. Future studies should include assessments of hand contamination before and after facility changes (e.g., sink types, soap dispensers, hand drying mechanisms) and assess if modified restroom items (e.g., toe pulls instead of handles) can increase consistent handwashing and satisfaction, as well as decrease hand contamination.
Handwashing is a cornerstone of disease prevention and has vast public health implications. Greater understanding of the available equipment in workplace restroom facilities and how to improve selection and use of that equipment may improve workers’ handwashing experiences. Enhancing handwashing consistency and satisfaction will bolster handwashing’s critical role in preventing the spread of infectious diseases between workers and within their communities.
Applications to Professional Practice
Handwashing is critical in disease prevention. In the workplace, it is often unclear whether people can conduct proper handwashing. It is imperative for workers to prevent the spread of pathogens not only among themselves but also the community. Certain restroom equipment and features reduce workers’ consistent handwashing and self-reported handwashing satisfaction. If no-touch technologies are present in the workplace restroom, it is important to verify the sensor and detection technology ensure things such as adequate water run time (e.g., 20 seconds nonstop), paper towels dispense immediately upon motion detection, and restroom equipment is maintained. Handwashing satisfaction decreased when workers had to pull the door handle to exit—touching a potentially contaminated surface—rendering the handwashing process less effective. Occupational health professionals should consider workplace restroom facility design and note aspects that can be altered (e.g., toe pulls vs. door handles) to enhance workers’ handwashing experiences.
Footnotes
Acknowledgements
We would like to thank the various site supervisors and local chapters at United Auto Workers, Stephanie Kellam at UnitedHealthcare, Thelma Green at Brighter Bites, Lou Weeks at UNITE HERE Local 1, Matthew A. Hughes at the University of Utah, Scott Patlovich at The University of Texas Health Science Center at Houston, and Krista Patlovich at The University of Texas School of Public Health at Houston for helping us distribute the survey.
Authors’ Note
To view the full survey instrument, please contact the corresponding author.
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Human Subjects Review Details
The Institutional Review Board at the University of Michigan approved this exempt research, HUM00189839, on October 20, 2020.
Author Biographies
Aurora Le, PhD, MPH, CSP, CPH, is the John G. Searle Assistant Professor of Environmental Health Sciences at the University of Michigan School of Public Health. Her research interests center around occupational health and safety, particularly occupational health disparities, psychosocial factors of work, and industrial hygiene. Her contribution includes conceptualization, data curation, investigation, project administration, supervision, validation, writing the original draft, reviewing, and editing.
Maria Perez-Patron, PhD, MHS, is an adjunct faculty member and statistician at Texas A&M University School of Public Health. Her research interests center around population and health, and demography. Her contribution includes conceptualization, data curation, formal analysis, validation, writing the original draft, reviewing, and editing.
Lauren M. Ward, MPHTM, is a graduate student in the Department of Environmental Health Sciences at the University of Michigan School of Public Health. Her interests include infectious diseases and community health. Her contribution includes writing the original draft, reviewing, and editing.
Andrew Comai, MS, is the industrial hygienist at the International Union of the United Auto Workers. His contribution includes data curation, reviewing, and editing.
Elizabeth L. Beam, PhD, RN, is an Assistant Professor at the University of Nebraska Medical Center College of Nursing. Her research focuses on educational technology and human behavior in infection control training. Her contribution includes conceptualization, reviewing, and editing.
Shawn G. Gibbs, PhD, MBA, CIH, is Dean of the Texas A&M University School of Public Health and Professor of Environmental and Occupational Health. His expertise is in the disruption of highly infectious diseases, industrial hygiene, exposure assessment, and environmental microbiology. His contribution includes conceptualization, reviewing, and editing.
