Abstract
Despite public perception that firefighters are a fit and healthy workforce, epidemiologic data suggest that firefighters suffer from a disproportionally high burden of cardiovascular disease, cancer, musculoskeletal injuries, and psychological distress (Daniels et al., 2014; Kales et al., 2007; Soteriades et al., 2011; Stanley et al., 2018). Studies have obeserved that cardiovascular disease has contributed to 45% of on duty fatalities, with firefighters experiencing an increased risk for a variety of cancers (Daniels et al., 2014; Lee et al., 2020). Workplace injuries have resulted in lost work time for 46% of firefighters with reported fire-related injuries, and overexertion/strain was the cause of 29% of reported fire-related firefighter injuries (Campbell, 2018; Orr et al., 2019). In addition to physical injuries, firefighters are at an increased risk for posttraumatic stress disorder (PTSD) and depression (Armstrong et al., 2016; Pinto et al., 2015).
Regular and frequent bouts of physical activity (PA) in the general population have been shown to prevent the onset of cardiovascular diseases and cancer, and decreased risk and severity of various disease states (National Cancer Institute, 2017; U.S. Department of Health and Human Services, 2018). In addition, routine PA can improve several mental health outcomes and musculoskeletal fitness, which are associated with an improvement in overall health status and a reduction in the risk of disability and chronic disease (U.S. Department of Health and Human Services, 2018). Nonetheless, firefighters may not be engaging in as much PA as needed to gain the potential benefits to reduce the risk of the chronic diseases they suffer from most. One study found that 25% of firefighters studied did not meet 12.0 metabolic equivalents (METs) of aerobic capacity, the minimum level of fitness necessary to safely perform required activities on the job (Korre et al., 2018). This finding may be due to the weight status (i.e., normal weight, overweight, or obese) of firefighters. In North America, it is estimated that 78% of career firefighters are categorized as overweight and obese of whom 40% are obese (Korre et al., 2018; Poston et al., 2011), and excess body fat was correlated with lower fitness and PA (Poston et al., 2011).
Knowing that firefighters may have excess body fat and therefore may not be engaging in appropriate levels of PA for on duty performance may indicate that firefighters are also not achieving PA levels to help reduce their risk for developing chronic diseases. Quantifying the amount of time firefighters spend in light, moderate, vigorous, and very vigorous levels of PA across different weight status categories may help occupational health and safety professionals determine whether low levels of PA are a risk factor for the onset of the chronic diseases that firefighters suffer from most. There are currently few, if any, studies that have objectively measured total, that is both on and off the job, levels of PA in urban firefighters as well as determined whether they are accurate in predicting their own levels of PA. To date, PA levels have been measured and collected by researchers through focus group discussions (Lovejoy et al., 2015) and self-reported measures (Durand et al., 2011; Hsiao et al., 2015; Leischik et al., 2015; Neto et al., 2019), with only one study objectively measuring levels of PA to assess the effects of exercise interventions on health and fitness of firefighters (Andrews et al., 2019). Other studies have reported objectively measured and self-reported PA levels during planned burned activities or wildfire suppression but these levels are not generalizable to firefighters working in large urban metropolitan areas (Chappel et al., 2016; Vincent et al., 2016).
This pilot study’s primary goal was to objectively describe the PA levels of healthy weight, overweight, and obese urban firefighters to better understand their engagement in sedentary, light, moderate, and vigorous levels of PA. A secondary goal of this study was to determine whether urban firefighters were accurate in predicting their total weekly levels of PA by comparing self-reported PA levels with their objectively measures levels.
Materials and Methods
Study Design and Participant Recruitment
A repeated measures study design was used to assess self-reported and objectively measured levels of PA from a non-probabilistic sample of firefighters (
Survey Instrument and Study Measures
Objectively measured levels of PA were collected using ActiGraph wGT3X-BT accelerometer devices over 7 consecutive days while firefighters were on and off work-shift. Actigraph software calculated the number of minutes participants spent in sedentary, light, moderate, vigorous, and very vigorous PA levels by counts per minute. Each minute was assigned a level of PA intensity according to definitions established by Freedson and colleagues: light (101–1,952 counts per minute), moderate (1,953–5,724 counts per minute), vigorous (5,725–9,498 counts per minute), and very vigorous (≥9,499 counts per minute). Because of a low number of minutes reported in very vigorous activity, our study combined number of minutes in vigorous and very vigorous and reported these combined results as vigorous.
Participants completed a baseline questionnaire assessing self-reported PA (using the International Physical Activity Questionnaire [IPAQ]) and demographic characteristics. Self-reported levels of PA questions asked firefighters to report various levels of PA over the previous 7 days. At the end of the 7-day observation, the actigraphs were collected and a follow-up questionnaire assessed the same measures as those at baseline. Body mass index (BMI) was assessed using self-reported height and weight defined according to the CDC guidelines as normal weight (BMI = 18.5–24.9 kg/m2), overweight (BMI = 25–29 kg/m2), or obese (BMI > 30 kg/m2; Centers for Disease Control and Prevention, 2017).
Data Analysis
We used descriptive statistics for continuous variables expressed as means and for categorical variables as frequencies. An analysis of variance test was used to examine the relationship between time spent in each level of PA across weight class. The significance level was set at 5%. All statistical analyses were done on SPSS v25 (IBM Corp., Armonk, NY).
Results
Among all firefighter participants, the majority were male (94.4%), White Hispanic race/ethnicity (94.4%), between 31 and 50 years of age (82.4%), and overweight (38.9%; Table 1).
Demographic Characteristics of a Sample (
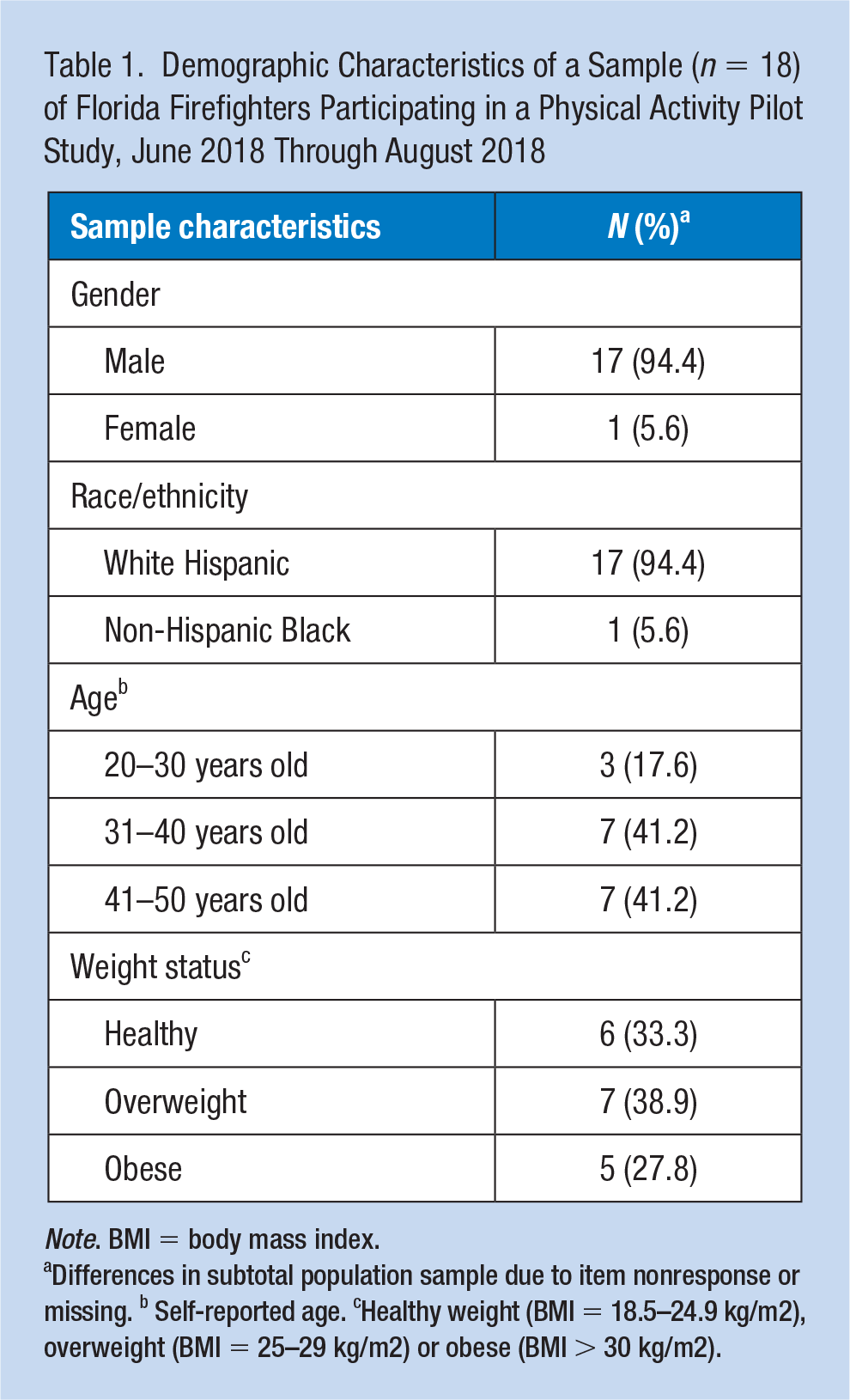
Differences in subtotal population sample due to item nonresponse or missing. b Self-reported age. cHealthy weight (BMI = 18.5–24.9 kg/m2), overweight (BMI = 25–29 kg/m2) or obese (BMI > 30 kg/m2).
Out of the total 10,080 minutes in a week, the objective accelerometer data documented that our sample of firefighters spent an average of 6,804 minutes in sedentary activity, 2,620 in light activity, 902 in moderate activity, and 18 minutes in vigorous. The remaining minutes unaccounted for (264 minutes) are considered non-wear time of the actigraph. Obese firefighters spent the most time in sedentary activity (8,033 ± 2,543 minutes/week), followed by overweight firefighters (6,533 ± 1,587 minutes/week) and then healthy weight firefighter (5,846 ± 1,160 minutes/week, Table 2). Healthy weight firefighters had the largest number of recorded minutes spent in light and moderate PA levels throughout a typical work week (3,243 ± 890 minutes/week and 1,299 ± 556 minutes/week, respectively), followed by overweight firefighters (2,689 ± 823 minutes/week, 669 ± 521 minutes/week, respectively) and then by obese firefighters (1,927 ± 1,425 and 668 ± 738 minutes/week, respectively).
Self-Reported and Objectively Measured Levels of Urban South Florida Firefighters (
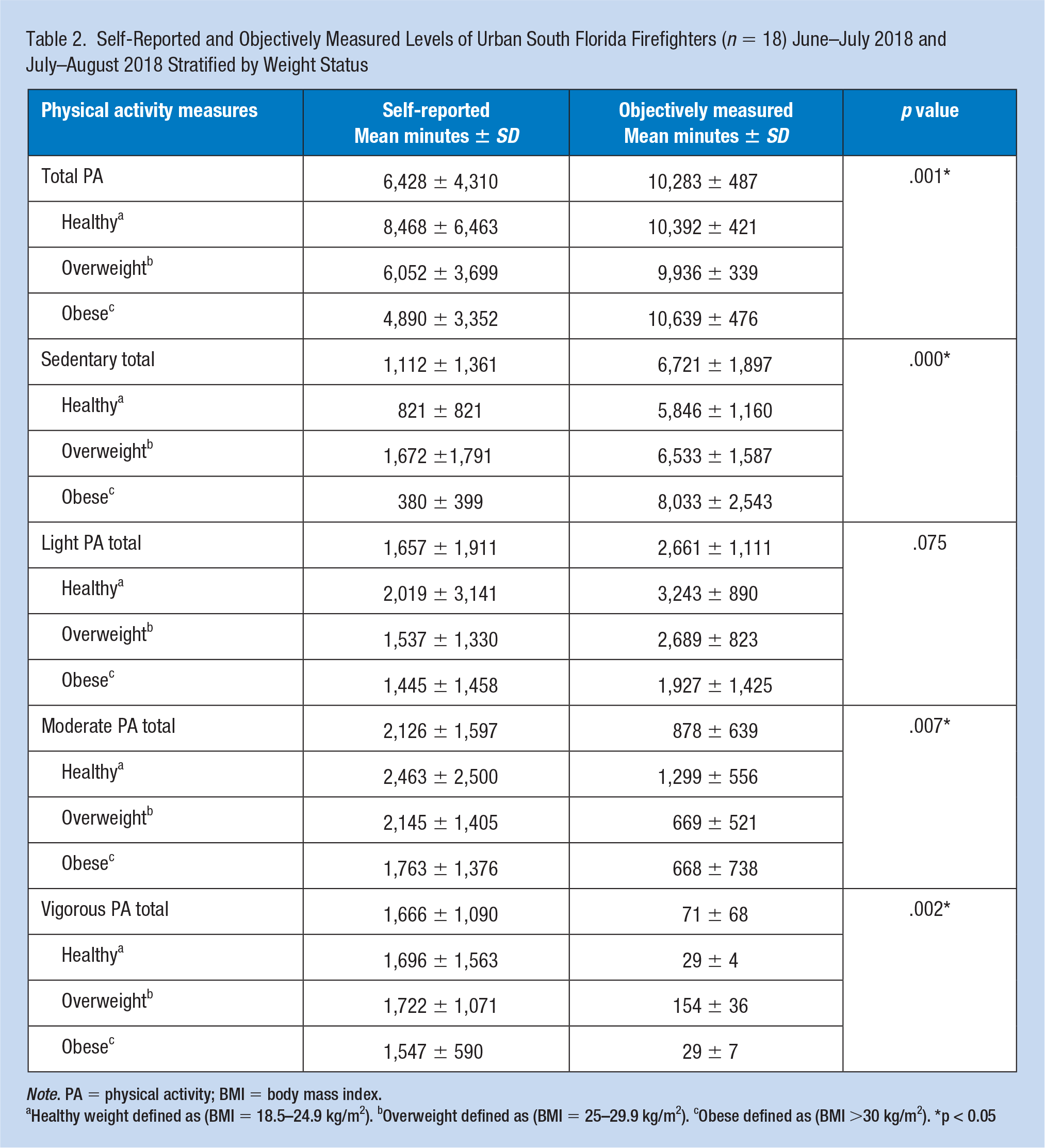
Healthy weight defined as (BMI = 18.5–24.9 kg/m2). bOverweight defined as (BMI = 25–29.9 kg/m2). cObese defined as (BMI >30 kg/m2). *p < 0.05
Comparing self-reported versus objectively measured sedentary PA levels, firefighters significantly underestimated the total number of minutes in sedentary PA across all weight status categories (1,112 ± 1,361 minutes/week vs. 6,721 ± 1,897 minutes/week,
Discussion
Pilot study findings suggest that paid professional firefighters engage in varying levels of PA during a typical work week and these levels vary based on weight status categories. We found healthy weight firefighters spend more time engaged in light and moderate PA than overweight and obese firefighters, whereas overweight and obese firefighters spend more time in vigorous PA than healthy weight firefighters.
In addition, firefighters poorly predicted their true PA levels. Specifically, they underestimated the number of minutes they spent in sedentary and light PA and overestimated the number of minutes spent in vigorous PA, suggesting that our sample of firefighters thought they were more active than they truly were. Overall, obese firefighters were the worst at predicting their total number of minutes in PA, followed by overweight and then healthy firefighters.
Limitations of this pilot study include the small sample size and the representation of only one fire department in Florida. It is possible that the participating fire department requires its firefighters to meet and maintain certain physical fitness goals, which may vary from other departments that have different health and fitness policies in place. In addition, the stations we recruited from may have different cultures about exercise and, therefore, have different weight status and ideas about PA. The measure of weight status category was calculated from self reported firefighter survey data. Objective measures of body mass index or a height to waist ratio may strengthen the accuracy of individual weight status category. Some categories of self-reported PA had high standard deviations, potentially due to the smaller sample size. Future research should include the recruitment of a larger sample of firefighters to better understand the within- and between-group variation in PA. A strength of this study is the sampling of urban firefighters in Florida. Though a small sample size, the firefighters recruited appear to work in heavily populated areas of a major metropolitan city and typically do not engage in wildland fire suppression activities that may generate different typical PA levels. To our knowledge, this is the first time objectively measured levels of PA have been recorded for urban working firefighters. A recent study objectively measured levels of PA and cardiorespiratory fitness of Midwest structural firefighters (100% of sample was overweight/obese) and found similar findings of 61% of their waking hours being spent in sedentary activity, 35.4% in light, and 3.6% in moderate PA (Barry et al., 2019). However, this sample of firefighters may not be generalizable to the broader culture and fast pace of firefighting work found in urban Miami.
Implications for Occupational Health Nursing Practice
Regularly engaging in PA is commonly recommended as a way to prevent the onset of chronic diseases. Firefighters as a workforce suffer from higher rates of various chronic diseases compared with the average population; therefore, it is important for firefighters to understand what it means to be engaged in various levels of PA to achieve their PA goals. Firefighters may not be engaging in as many minutes of light, moderate, and vigorous PA as they believe. This may result in firefighters not achieving the PA levels they desire and skew their understanding of what it takes to achieve health and safety on the job. Further research on the contribution that these levels of PA have on each weight class’ disease rate may help better explain the incidence of chronic diseases among both healthy and overweight/obese firefighters. Future researchers should consider collecting PA levels in larger cohorts of firefighters. Nonetheless, weight status may be attributable to levels of PA (i.e., those who moved more, weigh less), and being at a healthy weight is important in preventing the onset of many chronic diseases. Occupational health nurses should aim to support firefighters in achieving PA levels to assist firefighters to not only achieve a healthy weight but also understand what it means to be engaged in each level of PA to help decrease chronic disease risk.
Applying Research to Occupational Health Practice
This pilot study of career urban firefighters suggests that those firefighters who are obese spend a greater proportion of their time in sedentary levels of PA, whereas firefighters who have a healthy weight as per their BMI values spend less time in sedentary activity. The difference in mean total self-reported minutes and objectively measured minutes was significantly least for healthy weight firefighters and greatest for obese firefighters, suggesting that firefighters are not able to accurately predict their true objective PA levels. Employers should encourage their firefighters to move and/or exercise more often through clinical care visits or worksite wellness programs which will decrease their risk for chronic disease and injury. In addition, educating firefighters on what qualifies as light, moderate, and vigorous PA and how much is suggested daily may help this workforce achieve these various levels.
Footnotes
Acknowledgements
The authors thank all the Florida firefighters who took the time to participate in the research study.
Authors’ Note
This study’s research protocol was reviewed and approved by the university’s institutional review board (No. 20180602).
Authors’ Contributions
HK, KS, LB, NSS, and AJCM conceived the study, participated in its design and coordination, performed statistical analyses, and co-drafted the manuscript. HK and AJCM collected field data, entered study data, assisted in data analysis, and interpreted study results. HK, KS, LB, NSS, and AJCM performed statistical analysis, interpreted study results, and helped with the manuscript draft. All authors read, revised, and approved the final manuscript.
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by a start-up faculty package to the senior author and principal investigator of this pilot study.
Author Biographies
Hannah Kling, MPH, is a doctoral prevention science and community health student in the department of Public Health Sciences at the University of Miami, Miller School of Medicine. Hannah’s primary research interests are in occupational health and safety and the prevention of chronic diseases. She in interested in finding ways in which physical activity in the workplace (or lack thereof) influence the onset and treatment of chronic diseases within worker groups.
Katerina M. Santiago, MPH, is a research support specialist for the Public Health Sciences Department at the University of Miami, Miller School of Medicine. Her research interests include cancer epidemiology and prevention, health equity in vulnerable populations, and occupational safety and health. Katerina works primarily on the Florida state-funded Firefighter Cancer Initiative and the FEMA-funded national Fire Fighter Cancer Cohort Study (FFCCS) aimed at identifying work-related risk factors such as occupational chemical exposures and reducing cancer burden in the fire service.
Leonor Benitez, RN, BSN, COHN-S, currently serves as the Occupational Health Nurse and Infection Control Officer for the City of Miami Fire Rescue. Since receiving her Bachelor of Science in Nursing, she has over 20 years of specialized experience related to the Occupational Health field, including but not limited to, achieving the designation of Certified Occupational Health Nurse - Specialist (COHN-S), as well as, the creation/implementation of an occupational health and wellness program at two Fortune 500 companies. Leonor continues to work on various projects in connection with the Florida state-funded Firefighter Cancer Initiative and the University of Miami.
Natasha Schaefer Solle, PhD, RN, is a Research Assistant Professor in the Department of Medicine at University of Miami Miller School of Medicine and Sylvester Comprehensive Cancer Center (SCCC). Dr. Schaefer Solle’s research interests focus on occupational cancer risks and improving cancer screening in underserved communities. She is currently funded through a NIOSH K01 to study cervical cancer risk and screening among female firefighters.
Alberto J. Caban-Martinez, DO, PhD, MPH, is an Associate Professor (tenure-track) at the University of Miami, Miller School of Medicine. He oversees a lab that conducts robust occupational and environmental health surveillance activities and provides rigorous scientific evidence about effective ways to improve the well-being of worker populations. He is currently the co-principal investigator of the Florida state-funded Firefighter Cancer Initiative and the principal investigator of the FEMA-funded national Fire Fighter Cancer Cohort Study (FFCCS).
