Abstract
Work provides satisfaction and stability to young adult cancer survivors. However, progressive health changes because of cancer may compromise safety and diminish functional ability. The purpose of this study was to describe long-term young adult cancer survivors’ work experiences and describe their interactions with occupational and environmental health professionals (OEHPs) within the workplace. Cancer survivors were recruited from the Los Angeles County Cancer Surveillance Program. Professional organizations provided access to OEHPs. Constructivist grounded theory guided individual semi-structured interviews during data collection and analysis. Processes of interaction between cancer survivors and OEHPs found to influence work included revealing the survivor-self, sustaining work ability, gatekeeping (employment opportunities, return to work), and accessing support. OEHPs appeared to facilitate survivors’ work ability in the long term if services were available, services were known to survivors, and survivors revealed needs. Educating workers about OEHP services throughout cancer experiences and survivorship could ultimately improve interactivity and provide supportive work environments.
Keywords
Background
Adolescents and young adults (ages 15-39) diagnosed with cancer are often referred to as “AYAs” in the oncology community (National Cancer Institute [NCI], 2018). Approximately 70,000 young people are diagnosed with cancer annually in the United States (NCI, 2018). Many young people are surviving, living long past the treatment phase (Bleyer, 2011; Houghton, 2017), and are considered cancer survivors, which is a defined time frame initiated at diagnosis through the remainder of life (NCI, 2014).
The 2008-2011 Medical Expenditure Panel Surveys revealed AYA cancer survivors (n = 1,464; 20.8%) experienced loss in work productivity as measured by missed work days in comparison with participants who did not have cancer (n = 86,865) (Guy et al., 2014). Similarly, common cancers without metastasis in survivors less than 65 years of age (25%) often resume full-time employment, but full work ability may not occur due to cancer-specific sequelae and treatment-related health problems several years after diagnosis (Katz, 2015; Parsons et al., 2012; Tevaarwerk et al, 2013; Von Ah et al., 2016; Williams, 2013; Yi & Syrjala, 2017). These results reveal the need for successful work transitions and sustained employment for cancer survivors given that paid employment provides income, health insurance, self-identity, self-esteem, and socialization (Moskowitz, Todd, Chen, & Feuerstein, 2014; Wells et al., 2013).
To date, many studies focus on return-to-work as an outcome, which may not consider job-related performance challenges during work entry or re-entry for AYA cancer survivors. For example, a survey conducted by the LiveStrong Foundation found cancer survivors (n = 1,542), with a mean age of 49 years (SD = 10.8) experienced discrimination, being passed-over for promotions, and employers being unwilling to reasonably accommodate workers with functional impairment (Moskowitz et al., 2014; Wells et al., 2013). Functional ability is the capacity of an individual to perform normally expected activities (Kirch, 2008). Full work ability means being occupationally competent within a vocation, while meeting health requirements within an organizational environment (Tengland, 2013). The findings that functional impairment is a strong predictor of work ability drives the importance of thorough assessment of employed cancer survivors’ functional abilities in relationship to work demands.
In contrast, the Conceptual Framework for Occupational Health Programs and Services (Rogers, 2003) relates individual well-being within a system where occupational health nurses aim to improve, protect, maintain, and restore health of the worker/workforce. Position statements published by The American Association of Occupational Health Nurses (AAOHN) support the framework by addressing worker health on a continuum from wellness to disability, with specific mention of cancer (AAOHN, 2013; Schill, 2017). NCI (2014) provides helpful guidance on their webpage for all working adult cancer survivors.
Essentially, the work life of AYA cancer survivors during a career is multi-dimensional and not well understood (Wells et al., 2013). Hence, the overarching goal of this research was to construct an explanatory framework grounded in data from participants that illustrated processes of interaction between AYA cancer survivors and occupational and environmental health professionals (OEHPs) within the context of the workplace. More specifically, we sought to explain the interactions between long-term AYA cancer survivors and OEHPs, how interactions influence survivors’ ability to work over time, and the contextual factors that affect interaction and processes between AYA cancer survivors and OEHPs.
Method
Research Design
A qualitative study using constructivist grounded theory methodology explored, in depth, the experiences of AYA cancer survivors in the workplace. Grounded theory methods consist of systematic guidelines for collecting and analyzing qualitative data to construct theories from the data themselves (Charmaz, 2014). Pragmatism-informed symbolic interactionism, a theoretical perspective that assumes society, reality, and self are constructed through interaction, provided a foundation for this study. Social symbolic interaction occurs in the workplace as a process involving intentional communication, interpretation, role taking, definition, self-direction, and continual adjustments that are made as people relate to each other (Charon, 2010). Through these symbols, participants share what they consider important, as well as how they understand information (Schwandt, 2015). Grounded theory methods provide in-depth descriptions of relevant interactions with a precise accounting of the meaning attributed directly to the experiences of the participants. The assumption that employment situations involve multiple important interactions among AYA cancer survivors and OEHPs influenced by complex work factors underlies this research study.
Eligibility and Recruitment
AYA cancer survivor participants were recruited from the Los Angeles County Cancer Surveillance Program (CSP). CSP is the population-based cancer registry for collecting, storing, and studying data on persons with cancer in Los Angeles County. The CSP is a member of the statewide population-based cancer surveillance system, the California Cancer Registry (CCR), also part of the NCI–funded Surveillance, Epidemiology, and End Results (SEER) program. California Health and Safety Code, Section 103885, mandates physicians, hospitals, and other facilities that diagnose and treat cancer patients to report every cancer diagnosed within the state to the California Department of Public Health, manager of the CCR (CCR Department of Public Health, n.d.). The CCR will only release information to qualified researchers under tightly controlled circumstances where the research has first been approved by the California Committee for the Protection of Human Subjects (12-06-0472). The CSP were queried for an AYA cancer survivor sample diagnosed between 2002 and 2007. This study was also approved by the University of California, Los Angeles Office of the Human Research Protection Program (11-001999).
AYA cancer survivors were eligible for this study if they were diagnosed with cancer between the ages of 15 and 39, off cancer treatment for a minimum of 5 years, and employed during the data collection period. The AYA cancer survivors were required to speak and understand English well enough to converse with the principal investigator (PI) during individual, semi-structured interviews. A total of 343 AYA cancer survivors met the eligibility criteria among the Los Angeles County CSP. In Los Angeles County, approximately 2,600 AYAs are diagnosed with cancer each year (Liu et al., 2017). The program provided researchers with a random sample of potential participants.
Recruitment
The study PI contacted all AYA cancer survivors (N = 343) by standard mail sent to their home address. Potential participants were sent a letter of invitation describing the study, the interview guide, and the PI’s contact information. Sixty letters were returned due to lack of a forwarding address; 15 AYA cancer survivors responded and 12 were interviewed. The interested individuals who contacted the PI about the study were rescreened for eligibility including employment status. At the end of the study, purposive sampling (Charmaz, 2014) within the CSP data set was utilized to recruit male participants within the AYA cancer survivor sample as initial respondents were exclusively female, and male perspectives of employment situations as AYA cancer survivors were needed to nuance the data.
Twelve OEHPs were recruited from southern California chapters of national organizations for individual semi-structured interviews. OEHPs included nurses, physicians, industrial hygienists, and safety and human resource professionals. The AYA cancer survivor interviewees identified interactions with three OEHP groups and based on the frequency of interactions mentioned, the following were selected for recruitment: occupational health nurses (n = 6), human resource personnel (n = 3), and occupational safety professionals (n = 3). Nurses were oversampled as they were the most frequently identified profession by AYA cancer survivors as interacting with them within the workplace. Participation in this study was voluntary; thus, women and minorities were included as eligible. The PI obtained written consent from all participants prior to interviews.
Data Collection
A semi-structured interview guide was developed that featured open-ended questions to elicit experiences of interactions between AYA cancer survivors and OEHPs within the workplace. The interview guides were developed from a review of the literature, with evaluation and feedback from content experts. The domains for the AYA cancer interviews included experiences at work following cancer treatments and during long-term survivorship, experiences interacting with OEHPs in the workplace, and services or changes needed to promote work ability and sustainability. The OEHP interview guide included the following key probes: how OEHPs meet and engage with workers, identification of AYA cancer survivors in the workplace, and educational needs to enhance understanding of AYA cancer survivors’ needs at work over time. Interviews were conducted in person by the PI at each participant’s preferred venue on a date/time convenient for them. All participants were invited to send electronic messages or call with additional comments following interviews. Two participants provided additional insights via email following their interviews.
Data were collected and analyzed concurrently by the PI using procedures informed by constructivist grounded theory. All interviews were digitally audio-recorded and transcribed verbatim by transcriptionists familiar with qualitative research methods. The PI cleaned all transcripts of identifiers immediately upon receipt from the transcriptionist. Transcripts were organized and stored using Atlas.ti8 (Muhr, 2018). Pseudonyms were assigned to each participant to preserve confidentiality following consent. Recordings of interviews were erased following transcription. In appreciation for participation, a US$25.00 gift card was given to each participant.
Analysis
A systematic, iterative, line-by-line coding procedure started with attaching labels to depict the meaning of data segments within the Atlas.ti8 software program. Analytic techniques included initial, focused, axial, and theoretical coding procedures as described by Charmaz (2014). Constant comparison between codes was conducted often, during each stage of analysis, and codes were frequently revisited utilizing an iterative process which generated code categories. Situational analysis and mapping provided additional perspective on the human and nonhuman contextual factors (Clarke, 2009) within the workplace. Trustworthiness of analysis is a credibility criterion used in qualitative investigations involving generation of reflexive, analytical notes and detailed memos (Munhall, 2012). Memo-writing expanded categories, specified their properties, defined relationships between categories, and identified gaps for further data collection using theoretical sampling (Charmaz, 2014). AYA cancer survivors and OEHPs codes compared perceptions of interactive experiences within each group. Peer debriefing with expert qualitative researchers provided consensual validation of codes and analysis.
Results
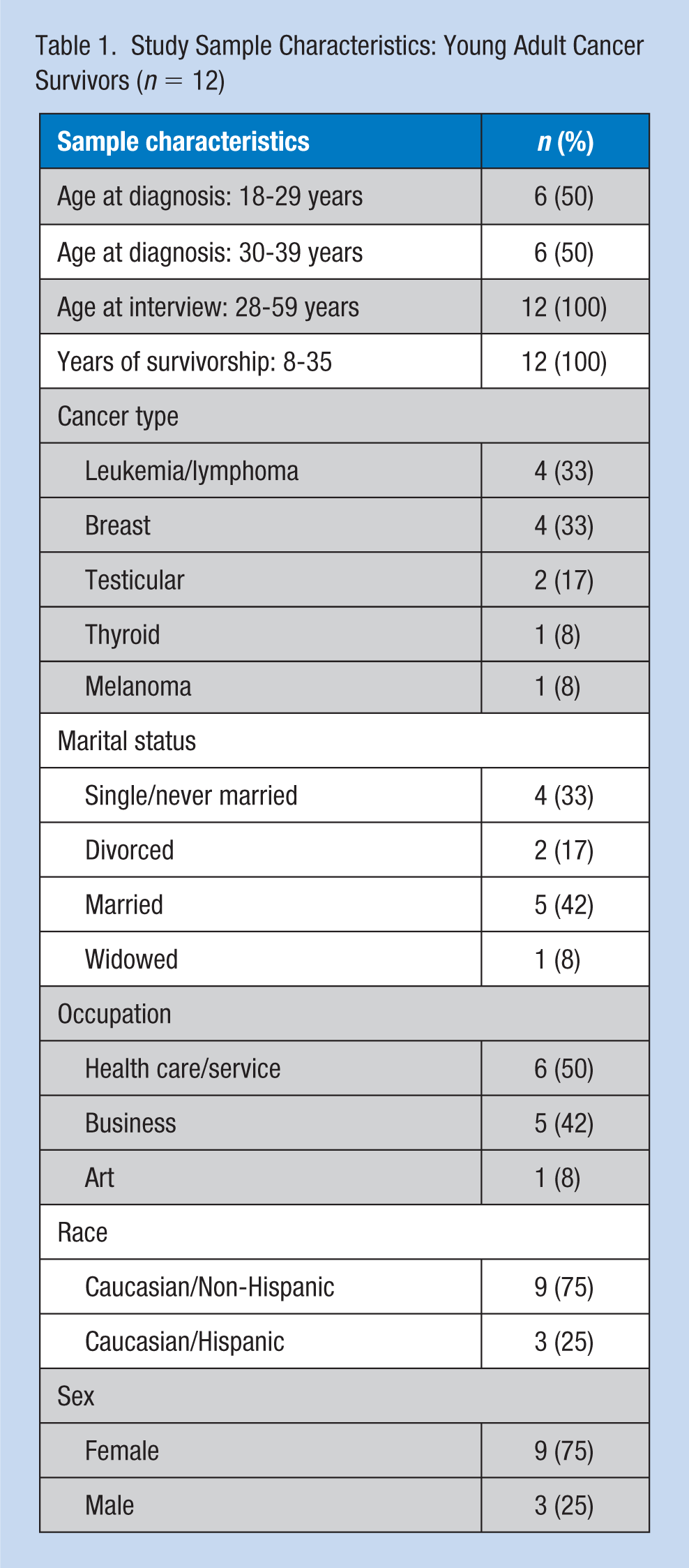
Twelve AYA cancer survivors participated in individual interviews with an average age of 29 years at diagnosis. As AYA cancer survivors were recruited at least 5 years after diagnosis and treatment, the mean age at time of interview was 43.9 years with the length of survivorship averaging 14.8 years (Table 1). One-third (n = 4) of the AYA cancer survivors were diagnosed with breast cancer, another third (n = 4) had experienced leukemia or lymphoma, and the remaining one-third (n = 4) had a history of melanoma, testicular, or thyroid cancer. Nine (75%) of the participants were female, and three (12%) were male. Five survivors were married (42%), four (33%) were single, two were divorced (17%), and one was widowed. All participants were of Caucasian race with three of Hispanic ethnicity. Occupations of the AYA survivors represented a variety of industries: four (33%) worked in health care, three (25%) were small business owners, and two (17%) were engaged in sales. The remaining three participants were employed in education, art, or the beauty industry.
Study Sample Characteristics: Young Adult Cancer Survivors (n = 12)
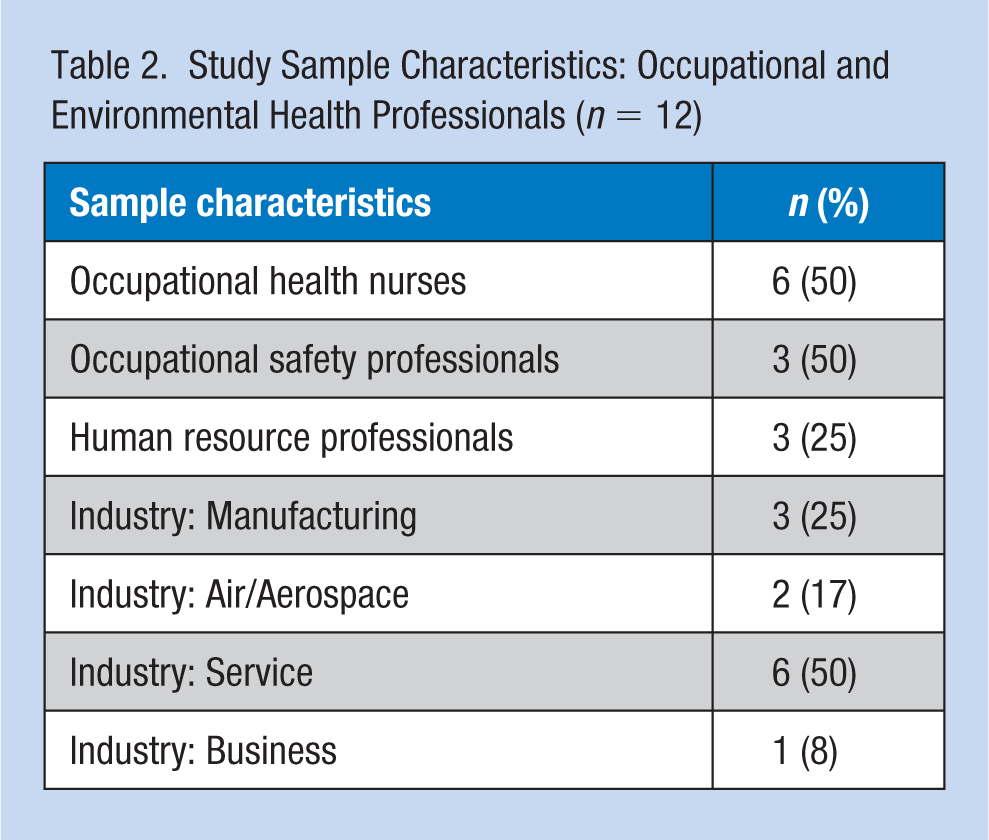
Twelve OEHPs included representation from occupational health nursing (n = 6; 50%), 25% (n = 3) were from occupational safety professionals, and 25% (n = 3) were from human resources as determined by the AYA cancer survivors’ interviews that reported interactions with specific OEHPs within the workplace (Table 2).
Study Sample Characteristics: Occupational and Environmental Health Professionals (n = 12)
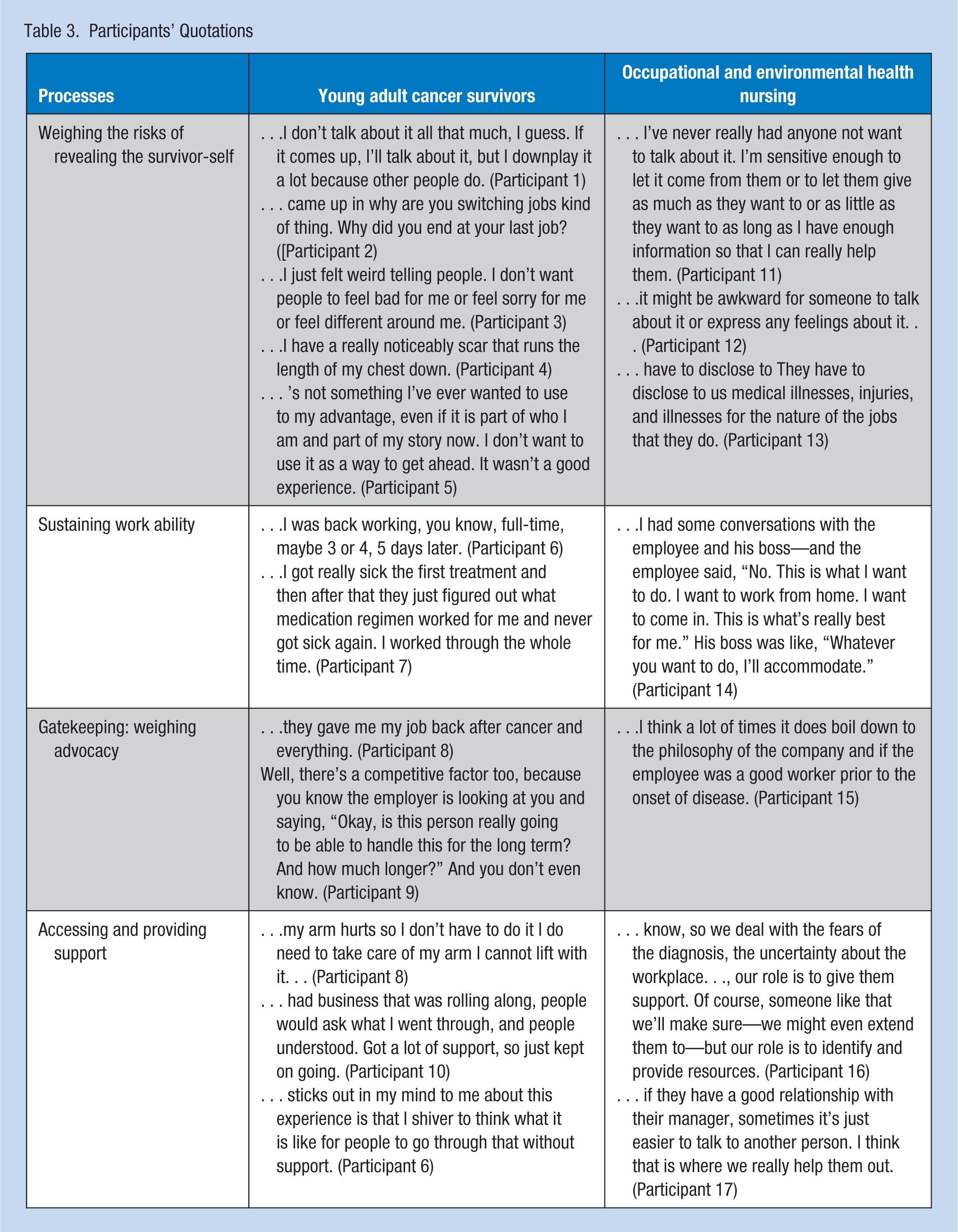
Twenty-four interviews were sufficient to achieve thematic and theoretical saturation. Six processes emerged, each describing interaction among AYA cancer survivors and OEHPs within the context of the workplace. Themes from the AYA cancer survivor perspective included the processes of revealing the survivor-self, the process of sustaining work ability, and the process of accessing support. Occupational health nurses’, occupational safety professionals’, and human resource professionals’ themes were the process of sustaining survivors’ work ability, the process of gatekeeping, and the process of accessing support for survivors (Table 3).
Participants’ Quotations
The Experiences of AYA Cancer Survivors
The process of revealing the survivor-self
The process of revealing the cancer survivor-self is complex within the context of work environments resulting in a variety of contrasting experiences from AYA cancer survivors. One survivor participant found disclosure of a cancer history normalizing, reflecting that when information is shared with colleagues in the workplace, it is news that is no longer shocking or stigmatizing but relatable as cancer has become a common diagnosis. Two other AYA cancer survivors reported that revealing experiences about their personal cancer journeys helped others who may be going through similar circumstances themselves, with coworkers, or with family/close friends. In contrast, one survivor thought she was sharing her medical history confidentially with a supervisor and was astonished to discover the supervisor informed coworkers and others in the workplace. Trust within their working relationship was jeopardized by the sequential chain of communication and interactions that disclosed private health information without permission from the AYA cancer survivor.
Half (n = 6) of the AYA cancer survivors maintained employment in the same workplace before cancer and after treatment. All participants in this situation shared their diagnoses, and the seriousness of it were known to others from the beginning and throughout treatment and recovery. All participants, male and female alike, felt “safe” and expressed sentiments about supervisors and colleagues like “He always had my back.” Early revelations of personal health news often generated support about a known and respected member of the working team who was grappling with a life-changing experience. One AYA cancer survivor shared how frequently she had taken leaves of absence for various reasons and was always welcomed back to work.
Searching for a new job post-cancer treatment was a quandary for a few AYA cancer survivors. Explaining a gap in employment to potential future employers seemed daunting. For example, questions from human resource professionals surprised one AYA cancer survivor who was asked to explain reasons for job interruptions and changes. She said she typically downplayed the cancer part of her life, if it came up, and preferred not to talk about it.
A few AYA cancer survivors found paid employment post-treatment working for agencies or organizations that serve cancer survivors. These AYA cancer survivors reported the open and honest work environment was comfortable and supportive. However, becoming emotionally close to others in the workplace who experienced cancer recurrence created fear and ultimately resulted in resignation from such emotionally immersive positions. As shown, AYA cancer survivors in this study might opt to reveal a cancer history or choose to keep personal health information private in the workplace. Most AYA cancer survivors not only reported being “careful” about what to reveal and to whom in the work environment, but also reflected after several years post-treatment, they had learned how to discuss cancer experiences without making people feel uncomfortable.
AYA cancer survivors’ perceptions of attitudes about cancer survivors in the workplace affected their process of disclosing their diagnosis and workplace accommodation needs. In several interviews, the AYA cancer survivors pondered if cancer is a common diagnosis, or if stigma still exists within the workplace. One survivor wondered if a cancer history generated sympathy or if it created fear in employers about potentially high insurance expenditures for someone with a serious preexisting disease. Another cancer survivor shared it is best to avoid including cancer in a cover letter as it may eliminate an opportunity to be interviewed, or to prove fitness for duty and general overall good health. Some survivors were unaware of the legal boundaries of interview questions in employment situations.
Some AYA cancer survivors experienced job insecurity following a cancer diagnosis and treatment, fearing closer scrutiny of work performance and potential for termination. To avoid revealing the survivor-self to others in administrative positions within the workplace, AYA cancer survivors reported they self-accommodated by informally limiting activities, sometimes aided by trusted peers. Avoiding seeking formal assistance for accommodations protected the identity of the AYA cancer survivor–self.
The process of sustaining work ability
Some survivors experienced uncertainty about health during long-term survivorship that could have impact on work performance. One survivor reported persistent fatigue despite a lengthy interval since diagnosis and treatment. She mused that the fatigue could be related to aging, although she was in her early 30s at the time of interview. Despite the fatigue, she maintained a rigorous work schedule. Panic attacks several years following cancer treatments plagued one AYA cancer survivor, who resolved this issue with counseling and medications. During that time, he did not reveal his continuing fear for cancer recurrence and consequential panic-attacks to coworkers and subordinates; he simply kept working at building his business while maintaining treatment.
Following breast cancer surgery and reconstruction, a survivor utilized the lift team at the health care facility where she was employed as it was readily available to all staff. However, the job required occasional sweeping and cleaning which caused arm pain, so a colleague offered to complete these tasks for her. An AYA cancer survivor who worked at an elementary school avoided playground activity during peak sunlight; trusted peers unofficially accommodated her job responsibilities when outdoor activities were required. None of the AYA cancer survivors were given formal work limitations by their health care providers, resulting in AYA cancer survivors navigating the workplace to self-accommodate and sustain long-term ability to work.
Sustaining work ability was driven by determined AYA cancer survivors who had a strong desire to thrive in a workplace where revealing the survivor-self was not comfortable or when job or health insecurity existed. As formal limitations were not given by health care providers, it is possible symptoms were accepted as a natural consequence of cancer or its treatments. AYA cancer survivors could also fear symptoms indicating potential cancer recurrence and denied their existence. Alternately, if OEHPs were present, sustaining work was enhanced by expertise and support services.
The process of accessing support
Most commonly, AYA cancer survivors sought support from trusted colleagues and superiors within their immediate work environment if their employment continued from before cancer well into long-term survivorship. Social support was more difficult to obtain in new employment situations post-treatment. Work environments that center on services for cancer survivors provided essential support, such as individual and group counseling, in alignment with the mission of their business.
A few AYA cancer survivors proactively recognized their need for occupational interventions in the workplace without formal recommendations from health care professionals and independently accessed support. One young woman sought advice from a safety professional specialized in ergonomics to adjust her workstation following surgery and treatment for cancer. The self-advocated accommodation allowed the AYA cancer survivor to work comfortably and without occurrence of lymphedema in her affected arm. Other AYA survivors needed support from trusted subordinates or family members to manage small business operations. Due to the autonomous nature of small business ownership, these survivors were also able to modify work schedules to enhance energy and efficiency in the presence of work demands.
One AYA cancer survivor desperately needed psychological help to grapple with the magnitude of her cancer experience, but such resources were not readily available to those who are contracted or self-employed. Eventually, she was referred to a counseling service by her health care provider. Similarly, services and resources of OEHPs were noted to be a luxury by an AYA survivor working for a small company. Requirements for OEHP services are related to industry type and company size according to the Occupational Safety and Health Administration (OSHA). Hence, small businesses and entrepreneurial pursuits required AYA cancer survivors to self-accommodate and advocate for self in the workplace. There were also some instances when the AYA cancer survivors were unaware of occupational services even in workplaces where they existed.
The Experiences of OEHPs
The process of sustaining survivors’ work ability
When AYAs disclosed their cancer survivor-selves to OEHPs, psychological and physical comfort, as well as safety, were the overarching goals identified by Nursing, Human Resources and Safety Professionals. Creating safe, private places for conversation about needs and for assessment was essential to ensure confidential implementation of engineering and/or organizational changes. Occupational and Environmental Health Nurses perceived themselves as trustworthy and expressed that private health information was commonly shared with them. One nurse reported a company requirement for employees to disclose illnesses and injuries due to potential risk for injury post-job offer, or with return-to-work from a medical leave of absence. Nurses also heard about workers’ cancer diagnoses from others within the workplace. A network of supervisors or coworkers reported cancer news to the company nurse to be helpful in case of emergent health events, or perhaps because they feared cancer cluster situations from exposures within the workplace. AYA cancer survivor employees who had an exemplary work history were often returned to work without question.
Safety professionals shared innovative strategies to accommodate AYA cancer survivors in the workplace when AYA cancer survivors’ needs were revealed. Adaptive equipment for shoulder problems and voice recognition with prolonged computer use were examples given of customized accommodations for survivors’ specific needs. Administrative controls were implemented to accommodate issues with fatigue. A flexible work schedule, closer parking or access to building entryways, and working from home to reduce commute time were found to be helpful to AYA cancer survivors. Inter-disciplinary collaboration with other OEHPs facilitated referrals for specialized accommodations in large companies.
The process of gatekeeping: Weighing advocacy
The nurse is typically the OEHP to greet AYA cancer survivors when they return-to-work or are offered employment for the first time within a company. It is the nurse, together with the occupational and environmental health team, who determines risk associated with job responsibilities and what health conditions are contraindicated to protect health and prevent disease in workers. A nurse revealed if workers are actively receiving treatment for cancer, they are not placed in jobs that expose them to certain chemicals. However, upon return-to-work, cancer survivors typically resume former work responsibilities, even if that meant returning to the same exposures. One nurse reported that excellent health was a job requirement for all workers in her industry as positions required a high level of physical rigor. If a medical condition was diagnosed, risk for unemployment was a real possibility. Worker characteristics were also found to influence gatekeeping work processes.
Unfortunately, the process of gatekeeping can also mean closing the gate to employment if AYA cancer survivors were unable to perform essential job functions and accommodation efforts were ineffective or not feasible. One nurse reported that if an employee is unable to return to their previous position, the survivors wondered and worried about their future career prospects considering financial resources and health insurance. Listening, coaching, and providing support with exploration of new realities was often a service provided by OEHPs in the workplace during these difficult situations. Advocacy on behalf of AYA cancer survivors, or the employer, is a common ethical dilemma for OEHPs when return-to-work situations lack clarity or information about health issues and need for accommodations in the workplace.
The process of accessing support for survivors
Nurses most commonly served as sources of information and evaluated usefulness of services available in the workplace or community at large. Employee Assistance Professionals (EAPs) were recognized as being extremely valuable when change of employment status occurred. Interprofessional collaboration was acknowledged by OEHPs to benefit AYA cancer survivors during work transitions.
Some AYA cancer survivors relied on the nurses’ expertise to detect changes in health because of exposures while working. One nurse reported routinely evaluating outdoor workers for skin cancer. The same nurse transferred to another department within the company and reflected on how she still heard from former patients, which seems to indicate that positive relationships and trust had developed. All nursing professionals in occupational and environmental health services reported long-term, trusting relationships with workers when interactions were frequent, meaningful, and genuinely caring.
Discussion
The focus of this study was to explain interactions of long-term AYA cancer survivors with OEHPs in the workplace. The grounded theory techniques used in this research revealed complex processes of interaction and contextual influences within the workplace while understanding of employment issues grounded by the experiences of AYA cancer survivors and OEHP participants was generated. The primary finding in this study demonstrates that AYA cancer survivors and OEHPs are reaching toward similar goals including support and sustainability of survivors’ ability to work. The results indicated that both survivors and OEHPs must navigate challenges to reach goals. AYA survivors need to weigh the risks of revealing their cancer history, while the OEHPs in rather precarious positions between employer and AYA cancer survivors struggled with advocacy issues (Figure 1).
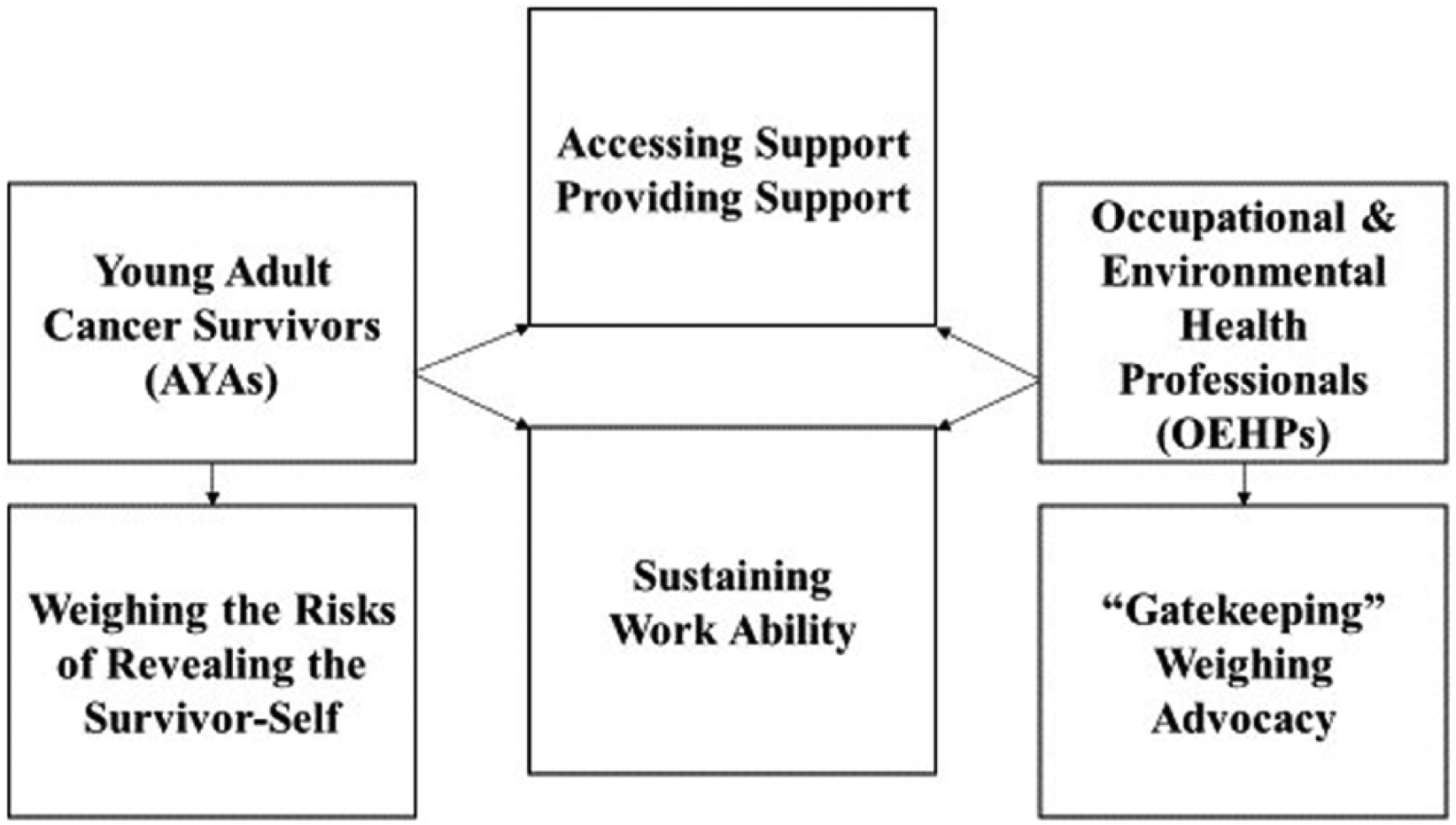
Interactions during employment and workplace processes between AYA cancer survivors and occupational and environmental health professionals.
Several major themes added previously undescribed findings within the AYA cancer survivor literature. The interactions between AYA cancer survivors and OEHPs were strongly dependent on AYA cancer survivors’ willingness to reveal their survivor-selves within the work environment. The United States Equal Employment Opportunity Commission (n.d.) protects all job applicants, regardless of age, against discrimination by disallowing questions about a candidate’s health before offering employment. However, once an AYA cancer survivor accepts a position, they may choose to reveal their cancer history to others within the workplace, or not. Anticipating questions and reactions from interviewers created fear and potential discovery and prevented early access to OEHPs if available in the setting. Part of the reluctance to reveal the survivor-self may be due to the disruption by cancer during a time when young adults are meeting developmental milestones related to dependence-independence and goal achievement (Zebrack, Bleyer, Albritton, Medearis, & Tang, 2006). Some AYA cancer survivors could have been striving to catch-up with these important markers during times of entry into the workplace.
The “gatekeepers” to returning to work were OEHPs who engaged in clearance processes to allow AYA cancer survivors to resume employment following extended absences. In return-to-work situations, revelations of the survivor-self were driven by a desire to re-enter the workplace. Work productivity has been reported to be a predictor for successful return-to-work regardless of diagnosis (Cancelliere et al., 2016) and seemed to influence who could return-to-work. Sustaining work ability involved complex processes of accommodation with or without OEHPs. Some AYA cancer survivors self-accommodated workplace needs through their own strategies or accessed supportive peers in their work environment. In some situations, AYA cancer survivors had no choice but to create their own safe and healthy workplace, as OEHPs were not present in small businesses. When OEHPs were invited into the process of accommodation, their expertise generated work controls that were customized to AYA cancer survivors’ needs.
Contextual factors that affected interaction and processes between AYA cancer survivors and OEHPs in the workplace included the size of the company and the type of industry (OSHA, 1993). Federal mandates for the presence of OEHPs currently relate to number of employees exposed to hazardous situations. Laws also protect AYA cancer survivors in situations that create bias by controlling questions that can be asked by employers prior to job offers. These legal parameters are not age exclusive but apply to all applicants seeking employment. The knowledge of health care providers about AYA cancer survivor’s essential job functions and establishment of limitations were also found to influence interactions between AYA cancer survivors during the process of accommodation. Knowledge too was found to be important to AYA cancer survivors, who were often unaware of OEHP services within the workplace when available.
The strengths of this study include a unique perspective involving interactions between employed long-term AYA cancer survivors and OEHPs. The random sample of AYA cancer survivors encompassed Los Angeles County allowing for sampling of a diverse group of survivors. This study provides new knowledge about the phenomenon of work among AYA Cancer Survivors. Historically, young adults diagnosed with cancers have received relatively little research attention compared with children and older adults diagnosed with cancer (Houghton, 2017; NCI, 2018). In addition, young adult cancer survivors are not part of the Cancer Moonshot, a federal U.S. program aiming to accelerate cancer research (NCI, 2017). However, AYA cancer survivors are part of Workers With Higher Health Risks from a Total Worker Health Perspective (Schill & Chosewood, 2013).
AYA cancer survivors clearly strived to be successful and productive in society. OEHPs, if available and known, were shown to be supportive to AYA cancer survivors individually and as a team. However, small business situations and self-employment did not provide such services. Sustaining work and maintaining employment improved participants’ overall quality of life. This study also highlighted selected OEHP groups as identified by AYA cancer survivor participants based on interactions within varied workplaces. New knowledge of workplace and employment processes has been generated as a result.
Limitation of this qualitative investigation included a lower number of male participants in comparison with female AYA cancer survivor respondents. In addition, recruitment efforts were influenced by currency of contact information in the CSP data set. Also, due to the nature of semi-structured, in-person interviews, geographic span of sampling was limited to southern California.
Implications for Occupational Health Nursing Practice
Understanding interactions between AYA cancer survivors and OEHPs within the workplace were shown to promote awareness among OEHPs concerning challenges that confront AYA cancer survivors during work processes. Management requires education concerning the importance of confidentiality when personal health information is shared. Communication techniques also need to be taught to promote work environments that are supportive of AYA cancer survivors. Because health changes occurred during long-term cancer survivorship, routine safety assessments along with discussion about accommodation strategies could promote work sustainability. AYA cancer survivors also need education about OEHP services. Employers could provide a directory at hire, return-to-work, and online.
Lack of OEHP support in small businesses or industries that do not mandate these roles affected AYA cancer survivors’ ability to obtain supportive interaction and formal improvement of work processes to accommodate needs (OSHA, n.d.). Routine and periodic assessments and interventions aimed at decreasing symptoms associated with consequences of cancer need development to promote adaptation to the workplace. Ultimately, workplace strategies aimed to continue work ability among AYA cancer survivors will reduce the state and national fiscal burden of utilizing public funding to support those that are unable to work. The NCI can ultimately use this explanatory framework to develop evidence-based guidelines for occupational health nursing practice.
Applying Research to Practice
Understanding interactions between AYA cancer survivors and OEHPs within the context of the workplace promoted awareness among OEHPs concerning challenges that confronted AYA cancer survivors during work processes. Managers, supervisors, and department personnel require education highlighting the importance of confidentiality when personal health information is shared. Communication techniques need to be taught to promote supportive work environments. Because health changes occurred during long-term cancer survivorship, routine safety assessments along with discussion about accommodation strategies could promote work sustainability. AYA cancer survivors also need education about OEHP services periodically during employment.
Lack of OEHP support in small businesses that do not mandate these roles affected AYA cancer survivors’ ability to obtain supportive interactions and formal improvements of work processes to accommodate needs. Periodic assessments and interventions aimed at decreasing symptoms associated with consequences of cancer need development to promote adaptation to the workplace.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The first author was funded by the National Institute for Occupational Safety and Health training grant (Grant 5T420H008412-09) while acquiring a Doctor of Philosophy degree in Nursing at the University of California, Los Angeles.
Author Biographies
Dawn S. Stone, PhD, RN, ANP-BC, COHN-S is a recent graduate from the University of California Los Angeles School of Nursing. Her research interests include vulnerable populations in the workplace and total worker health.
Carol L. Pavlish, PhD, RN, FAAN is an Associate Professor at UCLA School of Nursing. She researches ethical dilemmas and moral distress in work settings and has developed proactive strategies to mitigate these in clinical practice.
Patricia A. Ganz, MD is a medical oncologist, and Distinguished Professor of Health Policy and Medicine at the UCLA Fielding School of Public Health and the David Geffen School of Medicine at UCLA. She has spent the past four decades conducting research on the long-term and late effects of cancer treatments, and is internationally and nationally known for her advocacy and policy work in cancer survivorship.
Elizabeth Anne Thomas, PhD, RN, teaches Nurse Practitioner students specializing in Occupational and Environmental Health at the University of California, Los Angeles. She uses her research to mentor undergraduate and graduate students in both quantitative and qualitative research methods.
Jacqueline N. Casillas, MD, MSHS, is a pediatric oncologist and a health services researcher at UCLA whose areas of interest are access to care, quality of life, and quality of care for long-term cancer survivors. She is also the Director of the Jonathan Jaques Cancer Institute at Miller Children’s and Women’s Hospital in Long Beach, California.
Wendie A. Robbins, RN, PhD, FAAN, FAAOHN is Director of the PhD Program at the UCLA School of Nursing and Director of the Occupational and Environmental Health Nursing Program, NIOSH Southern California Education and Research Center, Fielding School of Public Health.
