Abstract
Dupuytren’s disorder is considered a genetic disorder and therefore not covered under workers’ compensation. Personal risk factors include workers of Northern European descent and workers that are older than 50 years. However, new evidence has shown that certain occupational activities may increase the risk of developing this disorder. This article is a review of the literature with a case study. Work-related and personal risk factors are explored, as well as interventions and return to work recommendations.
Keywords
Case Study
TT is a 60-year-old female who works as a computer analyst for a department store chain. Several years ago, TT noticed several hard painless nodules on the palm of her right hand. The nodules were located between the fourth and fifth fingers. However, 6 months ago, TT started to develop contractures in the fourth and fifth fingers. TT reports that she is right handed and that her work as a computer analyst entails using a computer and mouse for 6 to 8 hours a day. She denies any use of alcohol or tobacco products. Health history includes hyperlipidemia for which she is taking a low-dose statin. Surgical history includes a total abdominal hysterectomy due to uterine cancer 10 years ago. TT reports a 20-year use of oral contraception. In addition to a low-dose statin, TT takes an 81-mg aspirin every day for cardiovascular prophylaxis. Family history is positive for cardiovascular disease and breast cancer on the maternal side and positive for cardiovascular disease on the paternal side. She reports an allergy to Septra, which manifested itself as an abdominal rash. Due to the contractures, she is unable to use her mouse. TT sought treatment at an occupational health clinic and was diagnosed with Dupuytren’s contracture.
Dupuytren’s Contracture
Dupuytren’s contracture is a connective tissue disorder involving collagen deposition and is characterized by progressive fibrosis and thickening of the palmar fascia. Collagen is a protein that can be found in skin, blood vessels, muscles, bone, cartilage, and tendons. Collagen comes in 28 types and two forms, fibrillar and non-fibrillar. The most common types are fibrillar, including Type 1 that is found in skin, tendons, vascular ligature, and bone. Type 2 is found in cartilage. Type 3 is considered a main component of reticular fibers. Reticular fibers are synthesized by fibroblasts and, for example, form the stoma that supports lymphoid organs. Normally, Type 1 collagen is found in the tissues of the hand; however, in Dupuytren’s contracture, Type 1 collagen is replaced by Type 3 (Hindocha, John, Stanley, Watson, & Bayat, 2006).
Genetic markers may include genes that encode for proteins in the Wnt-signaling pathway. The Wnt-signaling pathway regulates fibroblast proliferation (Dolmans et al., 2011). In Dupuytren’s contracture, this pathway becomes overstimulated leading to fibrosis that invades the dermis resulting in contractures (Evert-Jan, van Beuge, Bank, & Werker, 2016). It is speculated that this process may be T-cell mediated involving the presence of CD3 lymphocytes (Evert-Jan et al., 2016). It is unclear as to whether one single gene is responsible for the development of Dupuytren’s contracture or whether the etiology of the disease may be from environmental and/or occupational exposures, especially vibratory exposure, as well (Larsen et al., 2015). The pathology of vibratory exposure and Dupuytren’s contractures may be due to chronic ischemia and an inflammatory response due to possible repetitive micro-damage to the hand (Rehman, Goodacre, Day, Bayat, & Westerhoff, 2011). The micro-damage generates superoxide free radicals and hydrogen peroxide that damage the perivascular connective tissue. To repair the connective tissue, fibroblasts invade the area. When fibroblasts are stimulated, an increase in the production of collagen Type 3 results (Rehman et al., 2011).
Dupuytren’s disease is considered a benign but debilitating disease due to a decrease in range of motion and grip strength. It begins with the development of painless nodules in the palm of the hands. There is also a triangular “puckering” in the palm between two joints. These nodules are the result fascia thickening. As the disease progresses, these nodules form longitudinal bands and contract. The most common joints involved are the metacarpophalangeal and proximal interphalangeal (Rehman et al., 2011).
Epidemiology
Dupuytren’s contracture is considered a genetic disorder; however, environmental risk factors may be involved (Table 1). Most affected are those of Northern European descent, affecting males more than females (Hindocha et al., 2006). Individuals begin to develop signs and symptoms in their 50s. Occupation-related risk factors may be heavy manual work and vibration exposures.
Personal Risk Factors
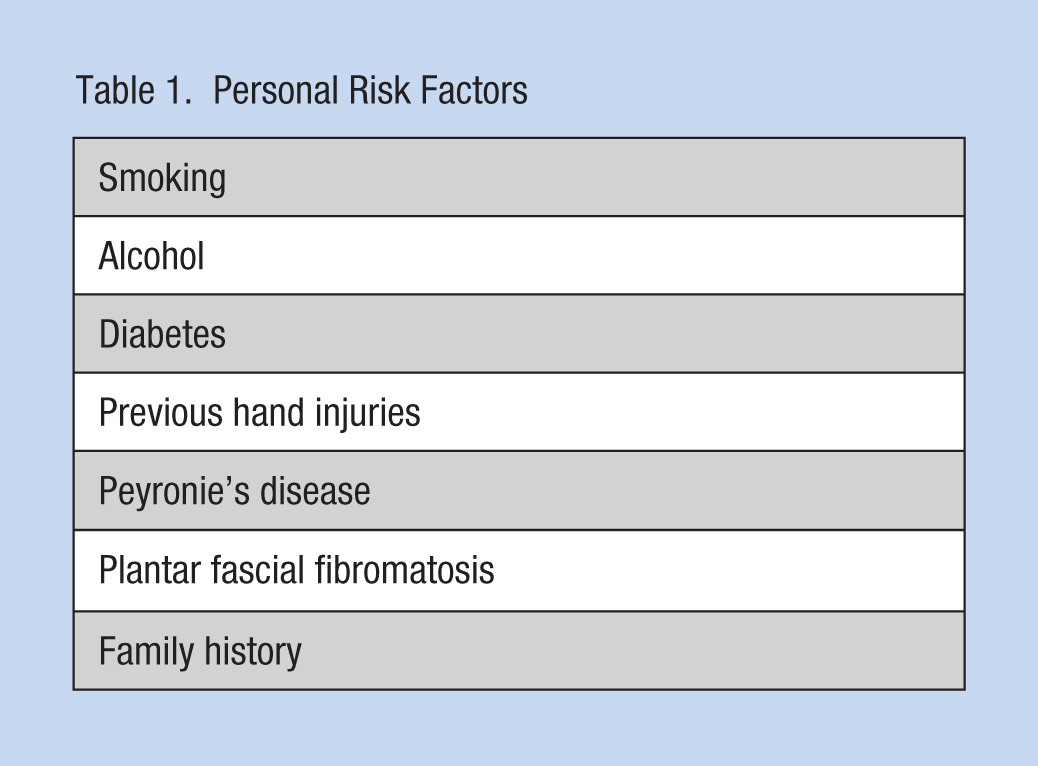
Diagnosis
The diagnosis of Dupuytren’s contracture is made by visual inspection of the hand and clinical presentation. The severity of the disorder is graded from 1 to 3. The presence of hard nodules with an aponeurosis and puckering is considered to be Grade 1. Grade 2 has the peritendinous band which causes a mild contracture of the fingers. Grade 3 is a severe presentation that presents with a full flexion contracture. Workers may be asked to flatten their hands on the table to determine whether the fingers have full range of motion (Hart & Hooper, 2005).
Both hands may be involved; however, one hand may have a more severe presentation. For example, a non-dominant hand may have a more severe presentation than a dominant hand (Hart & Hooper, 2005). Diagnostics such as magnetic resonance imaging (MRI) or computed tomography (CT) scan is rarely indicated except if tumors are suspected.
Review of the Literature
Dupuytren’s contracture is considered a genetic disorder, but environmental and occupational risk factors may exist. In 2008, a cross-sectional survey was conducted to investigate personal risk factors and occupational exposures (Lucas, Brichet, Roquelaure, Leclerc, & Descatha, 2008). Of a survey of 2,406 male workers, 212 men were diagnosed with Dupuytren’s contracture. Each individual diagnosed with Dupuytren’s contracture was asked to provide a health history, leisure manual exposures, and occupational biomechanical exposures to vibrations and manual work. Work tasks were divided into using a tool with a handle, using a vibratory tool, manual handling, and repairing mechanical equipment. Life time exposure was calculated. These occupational exposures were also investigated when assessing leisure activities. Personal risk factors were assessed including family history, diabetes, smoking, and alcohol use. The conclusion of the study revealed that after adjusting for personal risk factors, manual work, especially those tasks that involve manual handling and vibratory tools, was associated with the development of Dupuytren’s contracture. However, further studies were needed to confirm the results and investigate causation.
Another study investigated an association between Dupuytren’s contracture and vibratory exposure (Palmer et al., 2014). The study consisted of a final sample of 4,969 employed or self-employed men. A total of 2,287 men reported an occupational exposure to vibratory tools. However, Dupuytren’s contracture was reported only by 72 participants. Non-occupational risk factors, such as genetic disposition, smoking, alcohol use, and diabetes, were considered; however, only age and smoking were adjusted because data for other personal risk factors were not collected. One limitation to the study was that it did not include early signs and symptoms of Dupuytren’s contracture. It was determined that long and elevated levels of vibratory exposures contributed to the development of the disorder.
Few studies included the development of Dupuytren’s contracture among women. Men are more at risk for development of the disorder (Hindocha et al., 2006). Degreef, Steeno, and De Smet (2008) investigated risk factors among women in the Scandinavian population. This study evaluated the risk of developing Dupuytren’s contracture in 130 women. Nineteen percent of the women reported a family history; one woman reported alcohol abuse. Twenty-two percent reported a positive smoking history, and 32% reported an occupation that involved manual work.
Descatha et al. (2014) continued to study the relationship between occupation, alcohol, and smoking with the development of Dupuytren’s disease. The participants reported carrying loads, the use of vibratory tools, alcohol use, smoking, and diabetes. The participants were 836 men and 160 women; the mean age for men was 68 years and for women 65 years. Men in the study reported alcohol abuse, diabetes, and greater than 15-year exposure to vibratory tools. Due to the small number of women, results of occupational exposure were inconclusive. Specific occupational exposures included hand-vibration tools and heavy manual handling.
Treatment Options
No permanent cures for Dupuytren’s contracture exist, and recurrence is possible with any intervention (Chen, Srinivasan, Shauver, & Chung, 2011). The goal of each procedure is to increase range of motion and grip strength. Treatment options should consider the surgeon’s level of comfort with each procedure and the worker’s goal. Open fasciotomy is a common but invasive surgical procedure that involves cutting the cords in the hand and removal of the diseased fascia. A partial fasciotomy entails removing the diseased tissue and leaving the normal fascia. Because this procedure is open and invasive, recovery time may be longer than less invasive procedures.
Needle aponeurotomy is a non-invasive procedure in which a needle is inserted into the cord and the fibers cut to release the contractures. As with open fasciotomy, needle aponeurotomy is performed under a local anesthetic.
Another non-invasive procedure is collagenase injection that uses an enzyme to breakdown the collagen. It is injected into the diseased cord, and the surgeon applies pressure to contract the fingers to facilitate the rupture of the cord.
Limited studies as to the effectiveness of each procedure exist (Ball, Pratt, & Nanchahal, 2013). Occupational therapy may include thermoplastic night splints and regular physiotherapy exercises for stretching and strengthening (Bayat & McGrouther, 2006).
Implication for Occupational Health Nursing
During the preplacement examination and, if indicated, annual occupational examinations, it is important to assess the palmer aspect of the hand, especially for at risk employees. The occupational health nurse may teach the importance of smoking cessation and limiting alcohol consumption if necessary. If nodules are present, the occupational health nurse may recommend that the employee visit a primary care provider for a referral to a hand specialist, as well as teach hand stretching exercises for early stages of the disorder. Occupational therapy may assist in teaching additional hand exercises that maintain range of motion in the hand in early and advance stages. An ergonomic consult may be obtained to decrease the amount of vibratory exposure and risks associated with manual handling. Once the contracture is repaired, it is important that the worker is cleared by the hand surgery prior to returning to work.
Because limited studies about whether Dupuytren’s contracture is work related, it may not be considered a disorder covered by workers’ compensation, especially if the worker was not exposed to vibratory sensations but has personal risk factors. It is the responsibility of the occupational health nurse to determine whether the employee is qualified for the position and whether the job is worsening the disorder.
Conclusion
Genetics and personal risk factors appear to contribute to the development of Dupuytren’s contracture; however, occupational exposure to vibratory tools may also increase the risk of developing this disorder. Few studies are available that support an association between occupational exposures and the disorder. Further studies should include women and those workers involved with computer work. In addition, further studies could investigate non-steroidal medications and heat therapy to decrease the inflammatory response and slow the progressive of disease. Early interventions such as stretching and massage to prevent contractures could be utilized.
TT was referred to her personal health care provider, and she elected to have collagenase injection therapy due to a shorter recovery time. In addition to her injection therapy, she was referred to occupational therapy for stretching and strengthening exercises. TT returned to full duty with no restrictions. However, TT was counseled about the risk of recurrence and encouraged to continue the home exercise program provided by the occupational therapist.
Footnotes
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Biography
Ann R. Lurati is a nursing lecturer at California State University, Monterey Bay.
