Abstract
Occupational health nurses are familiar with environmental exposures workers encounter in their workplaces. However, employees are only “on-the-job” about one third of each workday, with a multitude of potential exposures in other environments that can affect their health. This article addresses some of the major exposures employees encounter outside the workplace—air, water, and soil pollution, and hazardous wastes—including a discussion of several well-known national and international environmental incidents. The major sources of these pollutants and how they contaminate the environment were investigated. Finally, risk assessment and communication along with effective strategies for educating employees and the community are presented.
Keywords
Most occupational health nurses are familiar with environmental contaminants encountered in the workplace, but they may not be familiar with environmental contaminants that can affect employees where they live and play, and how these additional exposures can affect the health of employees and their family members. This article addresses possible localized and global exposures employees may encounter in their daily lives. Some exposures (e.g., hobbies, additional occupations, and avocations) may be within the control of employees and their family members, but others (e.g., smog, generalized pollution of the air and soil) are not. Occupational health nurses are tasked with ensuring workplace health and safety, but may not focus on exposures employees encounter at home and in their neighborhoods and communities.
National and international environmental incidents could highlight the impact of non-work-related exposures. Workers may be unaware of the sources of environmental pollutants and how they move through the environment. Understanding how toxins and particles travel from their source to produce symptoms can inform occupational health nurses when they treat and educate workers and their family members. Finally, the article examines the principles of risk assessment and risk communication, skills that occupational health nurses can use to address employee and community concerns, while educating them to live healthier lives.
The Non-Work Environment
Individuals are products of the environments in which they were born and raised. Health is affected not only by what they consumed but also by the environments in which the consumables are produced, by hobbies and daily activities, and by the acquisition of learned and personal preferences. Documenting these environmental influences can be accomplished by a complete environmental assessment. Occupational health nurses can use the “I PREPARE” mnemonic (Paranzino, Butterfield, Nastoff, & Ranger, 2005; Figure 1), a tool that focuses attention on lifetime exposures. Knowing worker and family backgrounds (i.e., location of homes, past working and living exposures, personal environmental concerns, and current and past recreational activities) can direct occupational health nurses to areas in need of further investigation. For example, hobbies, secondary jobs, and family interests may increase exposure to dusts, chemicals (e.g., auto-body work, farming, and carpentry), fumes, and vapors (e.g., welding and work with leaded glass), symptoms that increase or improve when workers or family members are at home or work. Also, past experience in the military (i.e., loud noises, traumatic stress) or working in specific industries and on farms in the area may be informative. Using a tool such as I PREPARE and having a complete environmental history of workers and their families will better prepare occupational health nurses to provide prevention or mitigation strategies.
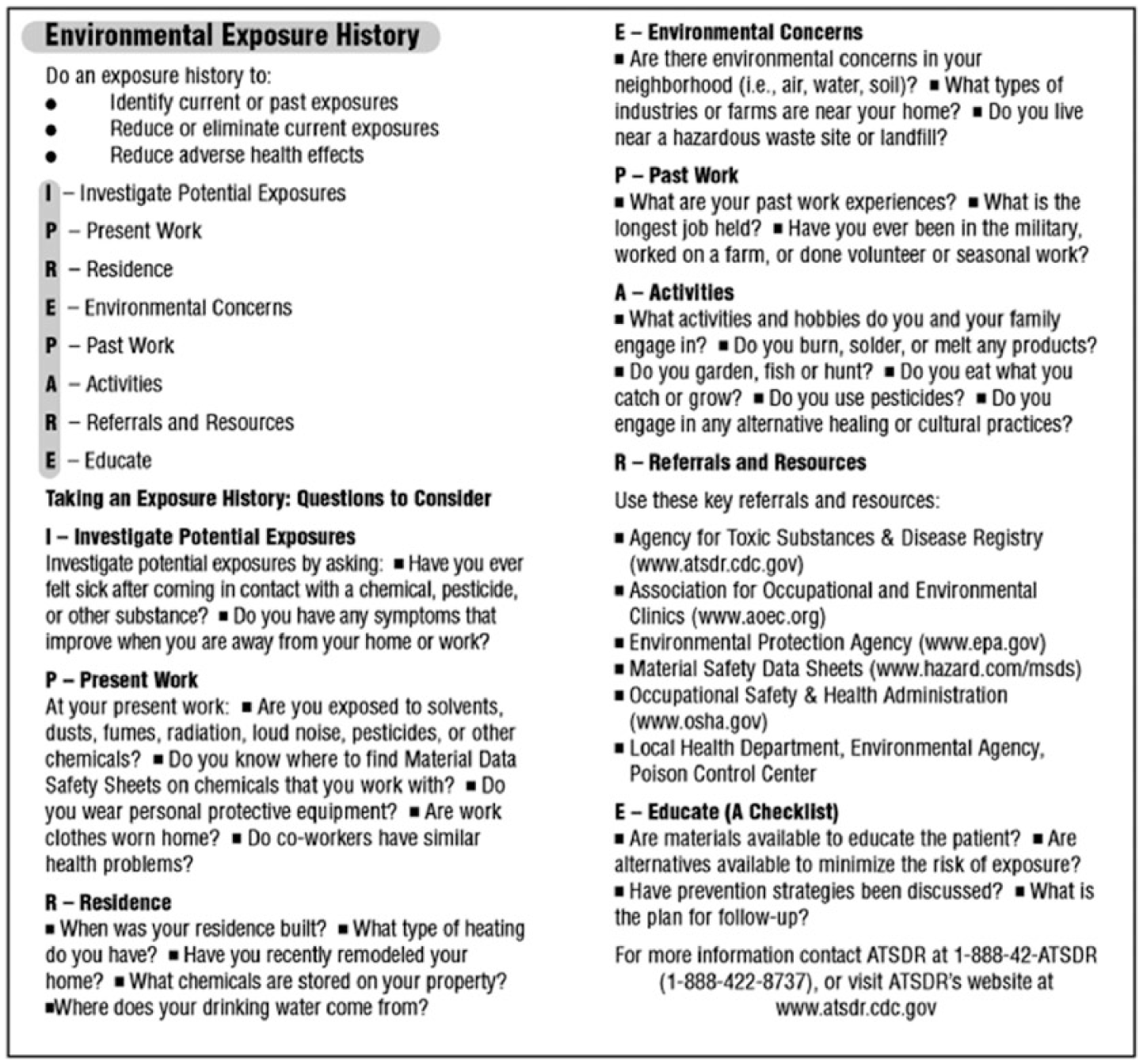
I PREPARE—An environmental exposure history assessment tool.
History of Environmental Incidents
During the second half of the 20th century, interest in the effects of dust, chemical, and other toxic material emissions on humans, animals, vegetation, air, soil, and water increased. These national and international incidents raised citizen awareness and motivated them to take action to preserve the health of themselves and the world around them as well as highlighting the evolution of the environmental movement and potential areas of concern to employees and their family members.
Air Pollution
From October 27 to 31, 1948, an air inversion in Donora, Pennsylvania, sickened 7,000 and killed 20 residents. It started with a heavy fog, and as the days passed, the fog became a thick, acrid smog. On October 31, the Donora Zinc Works shut down its furnaces only hours before the fog was finally dispersed by rain. According to the U.S. Environmental Protection Agency (EPA; 2014a), Donora had had frequent pollution problems prior to this incident. The numerous steel and zinc smelters in the area had long caused incidents of dirty air, but this episode offered no escape for residents who breathed toxic pollutants in lethal doses. A photograph of Donora street taken at noon on October 29, 1948, is shown in Figure 2.

Photo from Donora, Pennsylvania, taken at noon on October 29, 1948.
Water Pollution
In January 1988, a 4-million-gallon oil storage tank split apart and collapsed in Floreffe, Pennsylvania. The tank, owned by the Ashland Oil Company, was being filled to capacity after being moved and rebuilt at a new location south of Pittsburgh, Pennsylvania (EPA, 2015b). The spill escaped containment dikes, flowed into the Monongahela River, washed over two dam locks, and eventually contaminated the drinking water for an estimated 1 million residents of Pennsylvania, Ohio, and West Virginia (EPA, 2015b). This major cleanup took many months and was hindered by cold temperatures and the rocky/steep terrain of the area. Contractors used booms, vacuum trucks, and other equipment to recover approximately 20% of the spilled oil (EPA, 2015b). A photograph of the destroyed oil storage tank at Floreffe, Pennsylvania, is shown in Figure 3.

A destroyed tank at the Ashland oil facility.
Soil Pollution
Hydraulic fracturing (fracking), the injection of fluid under pressure to “fracture” rock and facilitate the capture of oil and natural gases, began in 1949 (Montgomery & Smith, 2010). Since the introduction of fracking in 1949 by Stanolind Oil, close to 2.5 million fracture treatments have been completed, including approximately 60% of all the wells drilled today (Montgomery & Smith, 2010). Of the slurry fluid injected into the ground, only 20% to 40% comes back to the surface, with the rest remaining underground (EEC Environmental, 2010). As fracking has increased, so has concern about its environmental effects (e.g., high usage of water, generation of significant wastewater, injection of non-recoverable chemicals into the ground, and the impact of these chemicals on surrounding soil, drinking water, and surface water) in the media and community (EEC Environmental, 2010). Although little existing information is available to document the variety and magnitude of chemical and dust exposures, questions about risks to oil and gas workers and exposure risks to the community remain. To address this concern, the National Institute for Occupational Safety and Health (NIOSH), an agency of the Centers for Disease Control and Prevention (CDC; 2010), is developing partnerships with the oil and gas industry to identify, characterize, and control (if necessary) workplace chemical exposures. Research is ongoing to determine community exposure risks where fracking is occurring to include noise pollution, air pollution, and light pollution resulting from 24-hour operations.
Global Pollution Incidents
The United States is not the only nation to experience pollution incidents. Many readers may remember the Great Smog of 1952 in London (MetOffice, 2015). After extended cold and heavy snow in November and December, residents of London were burning large amounts of coal with smoke pouring from their homes. According to Johnson (2002), anticyclones form when high pressure air subsides and falls, gradually warming as it descends, and creating an inversion, trapping smoke spilling from London chimneys. This inversion not only trapped chimney pollution but also particles and gases from factories and pollution coming from the continent to the east. The incident started on Friday December 5 and lasted until Tuesday, December 9. Health impacts of the fog included approximately 4,000 known deaths with many more probable (MetOffice, 2015). Other documented effects included breathing problems, reports of cattle asphyxiation, and the fog caused travel problems for days (MetOffice, 2015).
Another incident occurred in Bhopal, India, when a release of methylisocyanate occurred on December 3, 1984 (Union Carbide Corporation, n.d.-a). The investigation showed that a large volume of water was introduced into a storage tank, starting a chemical reaction resulting in a pressure release valve opening, allowing the gas to leak into the atmosphere (Union Carbide Corporation, n.d.-b). Ultimately, the investigation attributed the water leak to sabotage, followed by years of litigation in India and the United States. Official casualties provided by Union Carbide included approximately 5,200 deaths and several thousand individuals with permanent or partial disabilities. Investigators were not able to identify any employee responsible for the water leak and determined no valves were faulty.
A final example is the grounding of the Exxon Valdez on March 23, 1989. The 987 foot ship was loaded with 1,264,155 barrels of crude oil bound for Long Beach, California, transiting the Valdez Narrows, and grounded at Bligh Reef, rupturing eight of 11 cargo tanks and spilling 10.8 million gallons of oil in Prince William Sound (Exxon Valdez Oil Spill Trustee Council, 1990). Although no human lives were lost as a direct result of the spill, four deaths occurred during the cleanup. The Trustee Fund reported that losses to fisheries, subsistence livelihoods, tourism, and wildlife were immense. The report mentioned that the most significant loss was “the aesthetic sense that something sacred in the relatively unspoiled land and water of Alaska had been defiled” (para. 4).
More pollution incidents involving air, water, or soil can readily be found in the literature. A point to remember is that all of these incidents involved adding compounds that can adversely affect the life and health of human and other creatures in the environment, which reinforces the need for occupational health nurses to complete environmental assessments in local communities and identify potential lifelong exposures that may affect employees and their families.
Pollution Pathways
A concern about environmental incidents is that pollution events in one area can easily spread throughout the biosphere. For example, chemicals emitted into the air from a power plant will eventually settle on the sea, fresh water, or land, wherever prevailing winds take the chemicals. Eventually, these chemicals are eaten or absorbed by microorganisms, and then eaten by larger and larger organisms and animals. These chemicals, after bio-accumulation in fish or other animals, are then ingested by humans. A map of small particulate air pollution is shown in Figure 4.
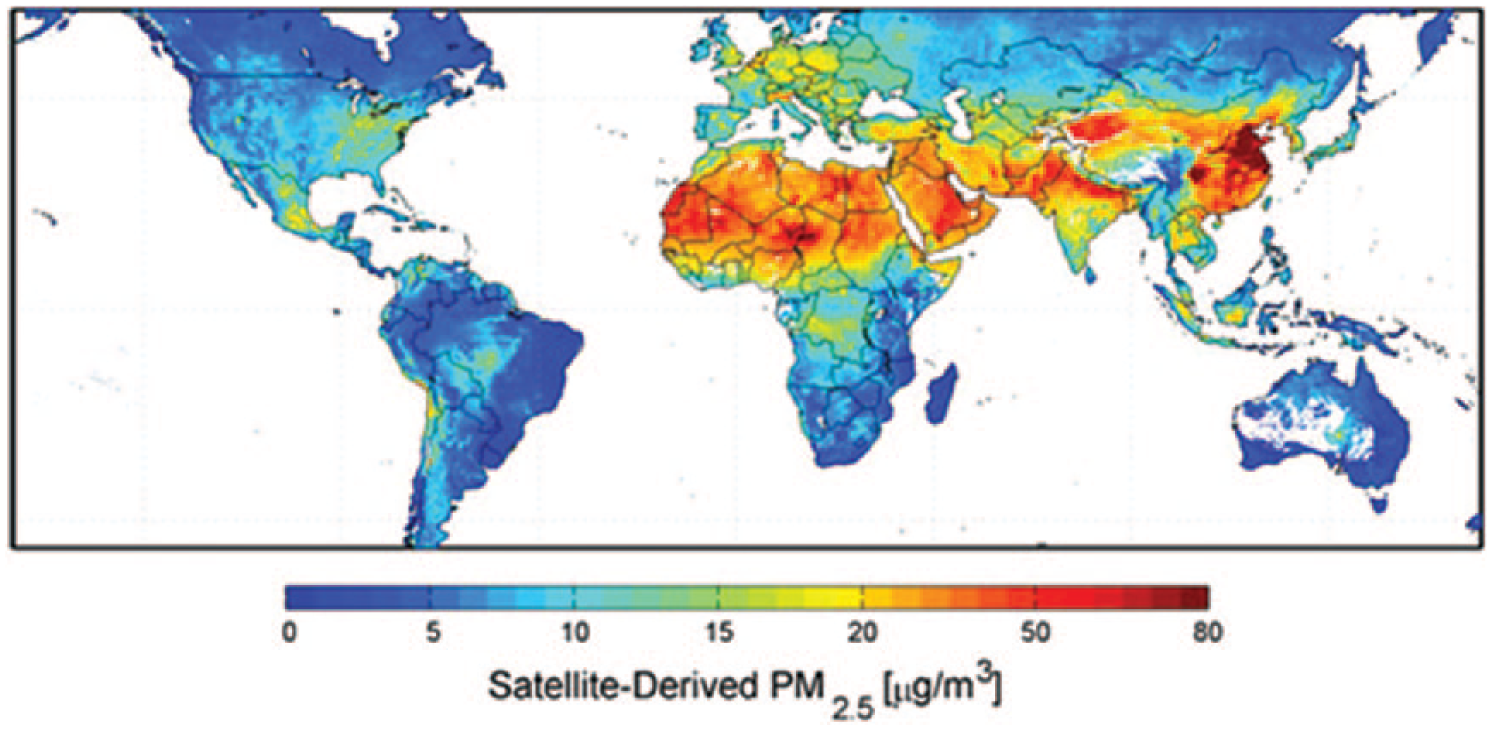
Global satellite-derived map of PM2.5 averaged over 2001-2006.
Once a pollutant is introduced into the environment, it spreads along prevailing wind, water, or weather patterns. Dispersal of pollutants can be predicted (see Figures 4 and 5). The key to whether a pollutant is toxic and the extent of toxicity depends on exposure dose, how and where the pollutant is metabolized by the body, where the chemical by-products are stored in the body, the length of exposure time, and workers’ current health at the time of the exposure. The relationship between dose and effect of the physical pollutant will determine the damage caused to living organisms. Or, as Paracelsus postulated many years ago, “The dose makes the poison” (Quote HD, n.d.).
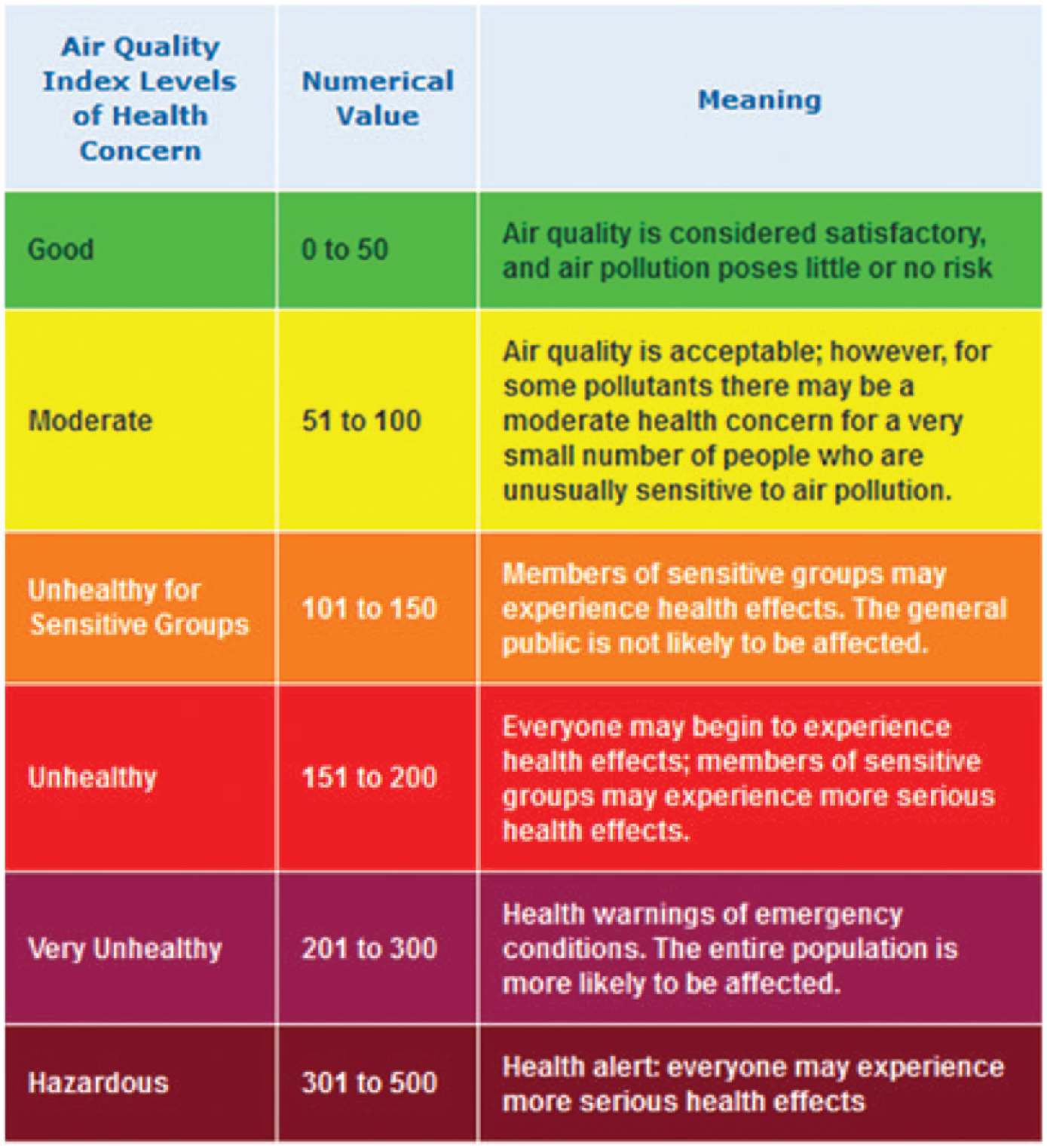
The Air Quality Index.
Environmental Exposures in the Community
Although a variety of environmental exposures are common in communities, this article concentrates on three areas of interest to most citizens: air pollution, water pollution, and hazardous substances, and how these exposures affect employees and their families. Occupational health nurses should be familiar with community environmental contaminants because employees and their families may need information about potential exposures.
Air Pollution
The Clean Air Act requires the EPA to set National Ambient Air Quality Standards (NAAQS) for six common air pollutants (i.e., criteria pollutants): ground-level ozone, particulate matter, carbon monoxide, nitrogen oxides, sulfur dioxide, and lead. Primary standards are based on human health, and secondary standards are designed to prevent environmental and property damage (EPA, 2016b).
Ground-level ozone is created by chemical reactions between nitrogen oxides (NOx) and volatile organic compounds (VOCs) in the presence of sunlight (EPA, 2015c). Major sources of NOx and VOCs include industrial emissions, electric utilities, motor vehicle exhaust, gasoline vapors, and chemical solvents. Health effects of ozone include respiratory system irritation, impaired lung function, aggravation of asthma symptoms, and other chronic lung conditions, resulting in inflammation and damage of the lung lining (AirNow, 2009). AirNow (2009) also reported that populations most at risk of ozone exposure include children, adults who are active outdoors, older adults, individuals with existing respiratory impairments, and individuals with unusual sensitivity to ozone.
Particulate matter includes acids (i.e., nitrates and sulfates), organic chemicals, metals, soil and dust particles, soot and smoke (EPA, 2015d). According to the EPA, the size of the particles is directly related to their effect on health. Particles 10 micrometers in size or smaller (PM10) will typically pass into the lungs, potentially affecting the heart and lungs (EPA, 2015d). These inhalable course particles, larger than 2.5 micrometers (PM2.5) and smaller than 10 micrometers, are a mixture of smoke, soot, dust, salt, acids, and metals. Finer particles, less than 2.5 microns (PM2.5), are more dangerous with the potential to penetrate deeper into the lungs, and may be transported in the blood stream (CDC, 2014). Health effects of particulate pollution include coughing; eye, nose, and throat irritation; wheezing; reduced lung function; asthma attacks; heart attack; stroke; and early death (CDC, 2014; EPA, 2015d). Those individuals most at risk of particulate pollution include individuals with heart or lung diseases, older adults, babies, and children (CDC, 2014). The CDC (2014) identified potential sources of particulate matter (e.g., wood burning stoves, forest fires, power plants, agriculture, coal fires, factories, cars and trucks, dust on open lands and construction sites).
Occupational health nurses might be more familiar with industrial sources of particulate matter (e.g., spray painting, plowing and farming, stone crushing, conveyor belts, mining, asbestos fibers, and various manufacturing processes such as cutting, sanding, grinding, drilling, and scraping). Occupational health nurses must recognize that particulate matter and other sources of air pollution remain with workers after they leave work, often affecting family members who also live with these daily ambient exposures. For instance, workers may bring home dusts on their work clothes, exposing adults and children to these dusts, especially when laundering clothing.
Carbon monoxide (CO) is a colorless, odorless gas produced during combustion with the majority of emissions coming from mobile sources such as automobiles, motorcycles, and other power equipment (EPA, 2015a). Harmful health effects include reduced oxygen (O2) delivery to body cells and tissues which can cause death at extremely high levels (EPA, 2015a).
Although lead (Pb) is found naturally in the environment, environmental exposures were reduced by eliminating lead in gasoline. Unless lead is used in the industrial environment, its most common source today is in homes built before 1978 when lead-based paint was used on doors, walls, and windows. Lead-based paint that is peeling, chipped, chalking, cracked, damaged, or damp is a hazard, especially to children, and should be remediated (EPA, 2016a).
Water Pollution
Water is necessary for life, and pollution control measures are needed to improve and maintain water quality while reducing the need for costly wastewater and drinking water treatment (EPA, 2015f). The Clean Water Act authorizes the National Pollutant Discharge Elimination System (NPDES) permitting program (EPA, 2016e), regulating the discharge of water from pipes, man-made ditches, and other sources of water pollutants. Since the introduction of NPDES in 1972, the permit program has resulted in significant water quality improvement.
Because water pollutants come from both point and non-point sources, a variety of measures are needed to prevent and control pollution. Water is polluted by wastewater, storm water, and water runoff (non-point source pollution) caused by rainfall and snowmelt, vessel sewage discharge, and sediments (EPA, 2015f). Microorganisms living in water can feed on biodegradable substances producing waste products and depleting oxygen levels. Other microorganisms found in water, such as salmonella, campylobacter, giardia, and hepatitis A, can cause illness with typical symptoms of nausea, vomiting, and diarrhea. Ground water is found in soil or under rock structures called aquifers. Polluted ground water can contaminate drinking water for significant populations. Chemicals found in wastewater and fertilizers can also contaminate water quality, supporting weed and algae growth. Suspended matter does not dissolve in water and eventually settles to form a thick silt at the bottom. Toxic suspended chemicals can be harmful to aquatic life. Finally, use of chemicals by industry and agriculture (e.g., metals, solvents, pesticides, and petroleum) can also enter the water supply (Water Pollution Guide, 2015).
All individuals are at risk of exposure to drinking water pollution. Occupational health nurses should encourage employees to regularly wash their hands, keep their hands away from their mouth after washing, and discourage employees from eating or drinking on the job site to prevent contamination. These recommendations also apply to family members at home, at play, and while traveling.
Hazardous Wastes in Soil and Water
The Agency for Toxic Substances and Disease Registry (ATSDR; 2014) lists many examples of potentially harmful or toxic compounds (e.g., acetone, arsenic, asbestos, benzene, carbon tetrachloride, ethylene oxide, and formaldehyde) that can pollute soil and water. Typical characteristics of these hazardous wastes include ignitability, corrosivity, reactivity, and toxicity (EPA, 2013). Hazardous wastes can affect every body system (cardiovascular, dermal, endocrine, gastrointestinal, hematological, hepatic, immunological, musculoskeletal, neurological, ocular, renal, reproductive, and respiratory), with many wastes being carcinogenic (ATSDR, 2011).
Although emergency responders, exposed workers, laboratory workers, and health care providers (including nurses) are most at risk of exposure to hazardous wastes, those working, living, or recreating near facilities where hazardous products are used and produced are also at risk, including the families of workers and their neighbors, many of whom are never assessed for occupational exposures.
Risk Assessment
Whenever occupational health nurses identify problems at workplaces or in communities, their first step is to evaluate how employees and the community may develop negative health effects from the environmental exposure. The four-step process, as detailed by Savage, Kub, and Groves (2016) and the EPA (2015e, 2016c), includes the following:
Hazard identification, including not only the agents that are present but also how the agents can affect human health;
Dose–response assessment, including the harmful effects that can occur through increased agent exposure;
Exposure assessment, including the route, amount, and duration of exposure as well as how the contaminant is absorbed, distributed, metabolized, and excreted by the body;
Risk characterization, including the exposure risk to exposed workers and the community.
Although occupational health nurses can use several sources to educate themselves on the process for conducting a risk assessment and the subsequent risk communication process, an excellent starting point is the EPA website, http://www.epa.gov/risk
After occupational health nurses have assessed the risks of interest in the community, they must learn about particular risks, so that they can discuss the risks with the community, answer questions, and direct workers and families to resources for more information.
Educating Workers About Environmental Health
Many resources can provide background knowledge necessary for the occupational health nurse to inform workers and their families. For interest in air pollution, a first step could be reviewing the Air Quality Index (AQI) on AirNow (2015), a website used to report the AQI to the general public. The AQI is a numerical presentation of pollution levels in the air ranging from 0 to 500 (see Figure 5). The higher the index, the greater the health concern to the local population. According to AirNow (2015), AQI values below 100 are “generally thought of as satisfactory” with values above 100 considered to be unhealthy; lower ranges are for those individuals more sensitive to certain pollutants, and higher values indicate that all individuals in the population could be affected. Occupational health nurses can check the AirNow (n.d.) Local Air Quality Conditions website on a daily basis by either selecting the local ZIP code or the state of interest (http://cfpub.epa.gov/airnow/index.cfm?action=airnow.local_state). Because occupational health nurses can immediately receive the day’s AQI Forecast for the area selected, they could send information to all employees via normal intercompany communication channels, including closed-circuit communication networks. The occupational health nurse could also show employees how to access the AQI via Facebook, Twitter, EnviroFlash email alerts, or the AirNow App for iPhones and Android. The AirNow site even has information about using the customizable AirNow Widget, which can be inserted on the company’s web page to automatically show current air quality and the next day’s forecast. The AQI Forecast along with its displayed color codes can readily inform employees and their families, so that they can plan or modify daily activities to protect their health. More information on using social media and other technologies can be found at http://cfpub.epa.gov/airnow/index.cfm?action=topics.about_airnow.
Because everyone drinks water, the occupational health nurse can educate workers and their families about needed precautions to minimize the risk of ingesting water-borne organisms and contaminants. The EPA provides information about National Primary Drinking Water Regulations, including a listing of contaminants and their maximum contaminant levels (MCLs; EPA, 2016d). This government site provides permissible limits of microorganisms, chemicals, and other compounds. Occupational health nurses, employees, and family members can easily find local annual drinking water quality reports by consulting EPA’s Consumer Confidence Report site (EPA, n.d.). Although some local drinking water reports are listed online, many are not. As an alternative, the occupational health nurse could search the website of its local water department for the most recent report of contaminants. Some local water companies mail reports annually to their customers. Another role of occupational health nurses is assisting employees in understanding these reports, so that they are aware of water-borne risks to their families and the community.
For hazardous wastes, facilities throughout the nation have been identified, including military installations, where waste sites are being remediated. The Resource Conservation and Recovery Act (RCRA) was enacted in 1976 and governs the disposal of solid wastes (EPA, 2014b). Occupational health nurses, employees, and their families can identify facilities in need of reclamation in their communities by searching the EPA Facility Information website at http://www.epa.gov/epawaste/hazard/correctiveaction/facility/index.htm and selecting the state of interest (EPA, 2014b). Search results will include data on the facility name, location, environmental indicator, and reclamation status. The site provides a Google interactive map of facilities in the area to assist the occupational health nurse and employees in identifying risks present in the community. If the occupational health nurse is unable to assist workers and their families in finding answers to their questions, they can be referred to the EPA and state environmental personnel who can provide additional assistance.
Communicating Risks to Employees and Families
Communicating environmental risks to employees is not always easy. Employees may express apathy about everyday risks, such as driving too fast, job-related respiratory exposures, or smoking, and it can be difficult for employees to change their behavior. However, once employees and the community are concerned about a risk (e.g., fracking), it may be equally difficult to minimize the identified risk and reassure the community.
Sandman (1994) discussed that in many cases, communication is a “one-way” street “with an identifiable audience to be warned or reassured and a source to do the warning or reassuring” (para. 3). Unfortunately, one-way risk communication is only effective when the audience accepts three assumptions. First, the source must be more knowledgeable than the audience. Second, the communicator must speak in the interest of the audience. Third, recommendations must be based on factual information regardless of personal values or preferences (Sandman, 1994). These assumptions are not always present as anyone who has ever attended a community meeting to discuss environmental problems in the community can attest.
It is preferable that risk communication be multidirectional and that the communicator design the message based on the audience’s thoughts and feelings about the issue. Sandman (1994) provided risk communication guidelines to use when addressing employees and the community about public disasters, but these principles can be applicable to all cases of environmental exposures and investigations. The occupational health nurse must remember that Risk = Hazard + Outrage (Sandman, 1994). If the community feels that they are being forced to accept a new facility when they are afraid of potential cancer, radiation exposure, or environmental waste, or the community suspects responsible parties are “hiding something” or when uncertainty about exposures and a lack of trust among the parties exists, community factions may have difficulty working together to resolve the issue.
Sandman (1994) recommended the following risk communication guidelines when working with workers, families, and the community:
These recommendations may be difficult to follow but will often result in better outcomes for your employees and the community. For more information to help self-educate about risk communication, the article found here by Covello and Sandman (2001) may be helpful: http://www.psandman.com/articles/covello.htm
Sources of Risk Communication Strategies
Many sources of risk communication strategies are available to the occupational health nurse.
The CDC website has “Gateway to Health Communication & Social Marketing Practice.” This site can inform the occupational health nurse when developing ongoing strategies for employee and family education programs: http://www.cdc.gov/HealthCommunication/HealthBasics/WhatIsHC.html
Unite for Sight (n.d.), an international organization based in New Haven, Connecticut, has an extensive offering (Module 1) detailing their presentation of Effective Health Communication Strategies: http://www.uniteforsight.org/health-communication-course/module1
Unite for Sight has other modules in their offerings that address Culture and its Influence on Health Communication; Interpersonal Communication; Mobilizing the Community; The Role of the Media in Health Promotion; Health Information: The Role of Information and Communication Technologies; and Risk Communication.
The occupational health nurse can use these and other websites to identify techniques and strategies, supported by facility management, to identify environmental risks in the community and develop effective facility-wide educational programs. Support from management encourages employees to “buy-in” to these educational programs, and adopt new health promotion and healthy living approaches for themselves and their families. The occupational health nurse will need to customize educational and outreach programs to meet the needs and interests of management and employees in the community. By adapting strategies to meet local needs, the occupational health nurse will increase the odds of success. Working within a well-planned and managed environmental education program should result in a healthier and more productive workforce while teaching employees and their families how to live healthier lives.
Footnotes
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
