Abstract
Organizations are required to adhere to the Occupational Safety and Health Administration’s (OSHA) Respiratory Protection Standard (29 CFR 1910.134) if they have workers that wear a respirator on the job. They must also have an employee “suitably trained” to administer their program. The National Institute for Occupational Safety and Health and its National Personal Protective Technology Laboratory have worked to champion the occupational health nurse in this role by collaborating with the American Association of Occupational Health Nurses to develop free, online respiratory protection training and resources (RPP Webkit). This article describes the development, content, and success of this training. To date, 724 participants have completed the training, 32.6% of whom lead their organization’s respiratory protection program, 15.3% who indicated they will lead a program in the near future, and 52% who did not lead a program, but indicated that the training was relevant to their work. The majority “strongly agreed” the training was applicable to their work and it enhanced their professional expertise.
Keywords
It is estimated that more than 5 million U.S. workers in more than 1.3 million workplaces are required to wear respiratory protection to control inhalation exposures while performing their jobs (OSHA, 2016). When worn correctly, respirators can protect workers from exposure to harmful respirable gases, particles, vapors, dust, and fumes. However, studies have repeatedly indicated that workers’ respirator compliance has been poor across various industries and occupational settings (Beckman et al., 2013; Peterson, Novak, Stradtman, Wilson, & Couzens, 2015). Emerging pathogens, such as influenza A (H1N1) in 2009 and Ebola in 2015, have brought the importance of respiratory protection to the forefront after workers became sick, with some attributing their illness to poor training and preparedness by their employer (Nolan & Rosenberg, 2014).
Organizations are required to follow the Occupational Safety and Health Administration’s (OSHA, 2011) Respiratory Protection Standard (29 CFR 1910.134) if their workers wear respirators to perform their jobs. The Standard indicates that organizations must have a comprehensive written respiratory protection program documenting policies and procedures for nine required program elements (e.g., hazard assessment, medical evaluation, respirator fit testing, employee training, and program evaluation). In the REACH II study conducted in 98 acute care hospitals in six U.S. states (Peterson et al., 2015), researchers observed high compliance in the study hospitals with some program elements, including initial medical evaluation, fit testing, and training. Despite this, workers in these hospitals demonstrated low compliance with the Centers for Disease Control and Prevention’s (CDC) airborne precautions guidelines, which recommend use of a respirator when caring for patients with known or suspected aerosol transmissible diseases or when conducting aerosol generating procedures. These findings most likely reflect that these hospitals also had low compliance with program evaluation processes, medical re-evaluation, and respirator maintenance, which are also required elements of the OSHA Standard. These findings highlight the need for organizations to meet all required standard elements to ensure workers are adequately protected.
The many required elements of the respiratory protection program necessitate leadership and oversight, which OSHA emphasizes in its Standard by mandating organizations designate a “suitably trained” person to lead their programs. This role is key to the success of the program, which the occupational health nurse should be well prepared to lead. In an effort to promote and prepare occupational health nurses for this leadership role, the National Institute for Occupational Safety and Health’s (NIOSH) National Personal Protective Technology Laboratory (NPPTL) began a multi-phase process (see Figure 1).
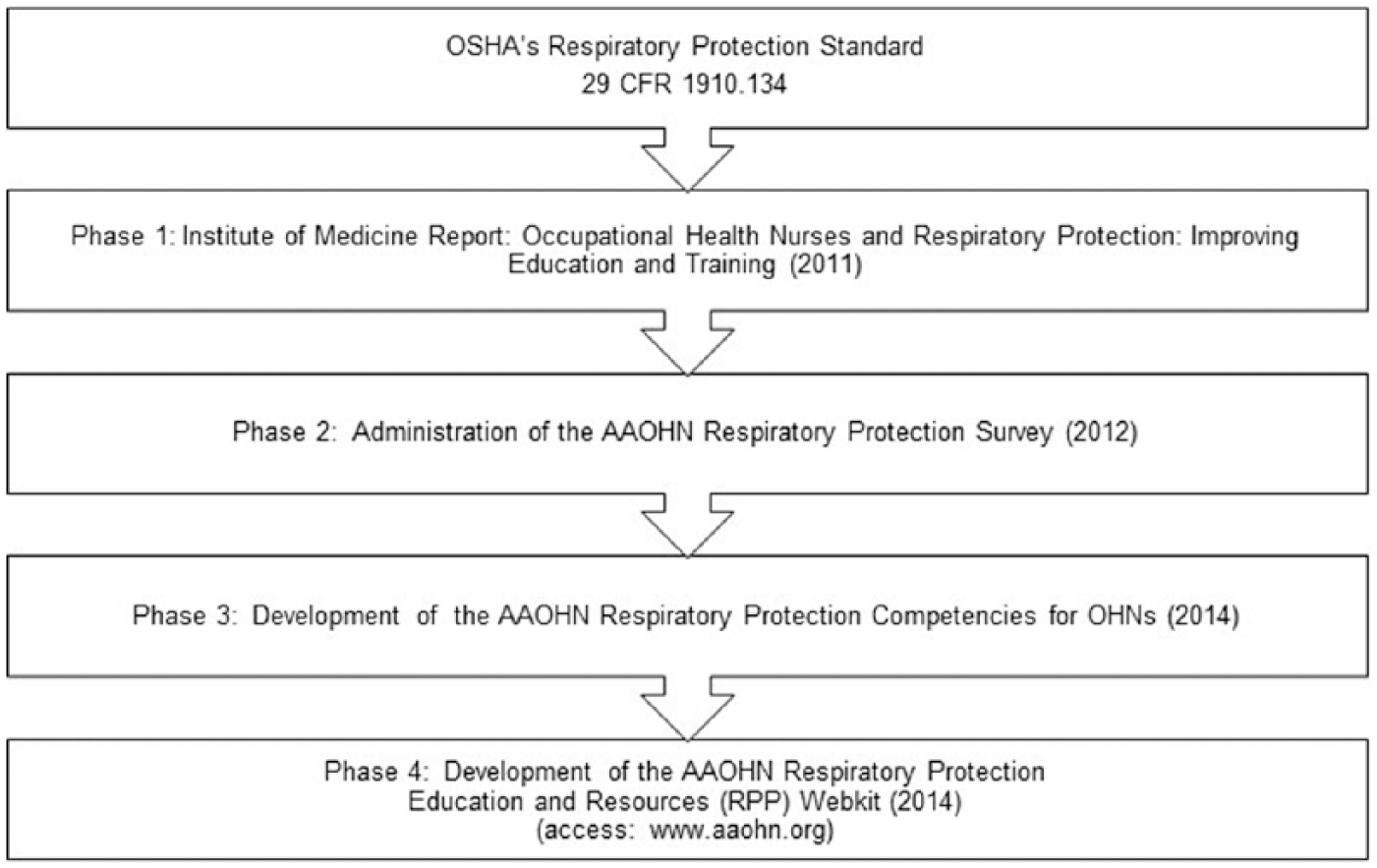

Initiatives aimed at advancing respiratory protection competency in occupational health nurses.
Phase 1: Institute of Medicine (IOM) Recommendations
The first phase of this initiative included a request on the part of NIOSH/NPPTL to the IOM to evaluate existing respiratory protection curricula and training approaches used by NIOSH Education and Research Centers (ERCs) and other occupational health programs. In addition, the IOM was asked to develop recommendations to improve occupational health nurses’ education and training in the selection, use, care, and maintenance of respirators. An ad hoc committee was formed and ultimately provided seven recommendations for improvements in respiratory protection curricula for occupational health nursing programs (IOM, 2011).
To address the IOM recommendations, the American Association of Occupational Health Nurses (AAOHN) formed a Respiratory Protection Advisory Group in December 2011, which included stakeholders from CDC/NIOSH/NPPTL, AAOHN, the American Board for Occupational Health Nurses, Inc. (ABOHN), the Association of Occupational Health Professionals in Healthcare (AOHP), and the American Nurses’ Association (ANA). The Advisory Group addressed two of the seven IOM recommendations in subsequent phases (i.e., Phase 2: the implementation of a national survey of occupational health nurses to assess their current roles and responsibilities and their education and training needs regarding respiratory protection and Phase 3: the NPPTL to explore the development of respiratory protection core competencies). This article provides an overview of how Phases 2 and 3 were implemented to address a third IOM recommendation for the NPPTL to expand online resources relevant to educating and training occupational health nurses about respiratory protection. More specifically, this article provides a description of how the fourth phase of the NIOSH/NPPTL initiative was implemented including the development, pilot testing, and implementation of the AAOHN Respiratory Protection Education Program and Resources (RPP) Webkit. The RPP Webkit includes online and face-to-face training as well as online respiratory protection resources to prepare occupational health nurses and other occupational safety and health professionals to serve as their organizations’ respiratory protection program administrator.
Phase 2: AAOHN Respiratory Protection Survey
The Respiratory Protection Advisory Group collaborated with researchers at the University of California, San Francisco, to conduct a survey that examined the roles and responsibilities of occupational health nurses related to respiratory protection, including the types of respiratory protection education and training these nurses received. The survey development, pilot testing, administration, and findings have been described elsewhere (Burgel et al., 2013; Burgel et al., 2014; Taormina & Burgel, 2013). In brief, participants were asked to rate their perceived level of competence (novice, beginner, competent, proficient, or expert; Benner, 1984) and their comfort with required respiratory protection program elements on a 5-point Likert scale (1 = not at all comfortable to 5 = extremely comfortable). Participants were also asked to provide professional and workplace demographic data (i.e., education, years working as an occupational health nurse, presence of a respiratory protection program at their worksites, and, if present, whether they were primarily responsible for the programs.)
Survey respondents included 2,072 occupational health nurses who were members of AAOHN, AOHP, and/or ANA, and/or certified by ABOHN. Findings indicated that occupational health nurses responsible for their organizations’ respiratory protection programs were more likely to indicate greater perceived competence and comfort with respiratory protection program elements compared with occupational health nurses who worked for organizations with a respiratory protection program but for which they were not responsible or organizations that did not have a program. In addition, those with higher levels of education, more years of occupational health nursing experience, membership in a professional nursing organization, and those employed in the health care sector were associated with higher perceived respiratory protection competence. However, 17% (n = 360) of respondents perceived their level of competence to be “beginner” or “novice” in regard to respiratory protection program elements. Further, 28% reported “none” or “slight” comfort in their ability to explain the difference between a N95 respirator and a surgical mask, with a large portion of these respondents perceiving themselves to be at the novice or beginner level of competence. Also, program elements including respiratory protection policy development and evaluation, as well as respiratory maintenance (e.g., inspecting, cleaning repairing), ranked low in comfort among participants. Although some of these findings were not unexpected, they highlighted the need for training to increase the knowledge of and comfort level across RPP elements among occupational health nurses, as well as across self-reported competence levels.
Recommended Training Methods
This survey also assessed how occupational health nurses achieved and maintained respiratory protection competence and their preferred method(s) of learning (Burgel et al., 2014). The majority indicated they had acquired their knowledge of respiratory protection through on the job training (68%), a NIOSH spirometry course (55%), or professional conferences (40%). The higher perceived competence and greater comfort in respiratory protection was associated with online continuing education, continuing education offered by manufacturers or vendors of respiratory protection equipment, networking, or train-the-trainer programs. With respect to preferred methods of training, a large portion (83%) of nurse respondents indicated face-to-face conferences and workshops, followed by self-paced educational training modules (41%), live webinars (49%), recorded online education and training modules (41%), and case studies (23%). These preferences varied by level of perceived competence and years of work experience as an occupational health nurse. For example, case studies and simulations were the preferred method for occupational health nurses with less than 10 years of experience compared with those with more than 23 years, who preferred attending face-to-face conferences. These findings highlight the need for offering varied training options to foster occupational health nurses achieving and maintaining competence. Based on the survey findings, the Advisory Board mapped a plan to first offer respiratory protection training through both online and face-to-face strategies followed by other modalities such as case studies.
Phase 3: Development of Occupational Health Nurses’ Respiratory Protection Competencies
Findings from the occupational health nurse respirator protection survey were used by the Advisory Group to develop the Occupational Health Nurse Respiratory Protection Competencies (Burns et al., 2014). From these, a matrix was created consisting of the eight AAOHN’s Occupational Health Nursing Competencies (AAOHN, 2007) on one axis (e.g., Clinical Practice; Health Promotion and Disease Prevention) and Occupational Health Nursing Competency Levels for Respiratory Protection (i.e., competent, proficient, and expert) on the second axis. Within this matrix, the Advisory Group mapped aspects of a respiratory protection program (e.g., medical evaluation, fit testing, training). The competency structure was designed to ensure that occupational health nurses competent in respiratory protection would be, at a minimum, knowledgeable about the basics of the OSHA Standard and how it is applied to workers in their work setting. Having this foundation would enable nurses to achieve proficient and expert competency in respiratory protection by taking a leadership role in evaluating the success or gaps in their organization’s program (proficient), and then developing plans to improve their program (expert). These competencies were used to inform the development of the AAOHN RPP Webkit.
Phase 4: Development and Implementation of the AAOHN RPP Webkit
The existing Advisory Group was expanded to include occupational health specialists with expertise in respiratory protection from healthcare/hospitals, academia, government agencies, and private corporations. Several of these members were part of the previous work groups described above. This group was charged with reviewing training materials developed by occupational safety and health faculty and staff at the University of Texas Health Science Center at Houston (UTHealth) School of Public Health. The UTHealth team was charged with developing a training presentation that could be delivered online and face-to-face, together with a comprehensive package of online respiratory protection resources and materials relevant to the required OSHA Standard’s program elements.
RPP Webkit Development
To ensure that the basics of the OSHA Standard were adequately covered in this training, the RPP Advisory Group initially mapped OSHA Standard components pertaining to all required program elements. The elements were then mapped to the Respiratory Protection Competencies, focusing specifically on the “competent” level, while ensuring a foundation was provided for later training at the “proficient” and “expert” level. This process resulted in 10 self-paced, training modules listed in Table 1. The outline of this training was then used to gather respiratory protection resources that occupational health nurses could use to build knowledge and expertise. As expected, numerous resources were found in existing NIOSH, NPPTL, and OSHA materials. Several valuable resources from state health department websites in California (California Department of Public Health [CDPH] Occupational Health Branch, 2015) and Washington (Washington State Department of Labor & Industries [DOL & I], 2016) were also used. These resources were used, in part, to develop the training script. Resources, and accompanying URLs, relevant to a particular training module were described at the end of each module. These resources were compiled and posted as part of the RPP Webkit as outlined in Table 2.
AAOHN’s RPP Webkit Training Modules
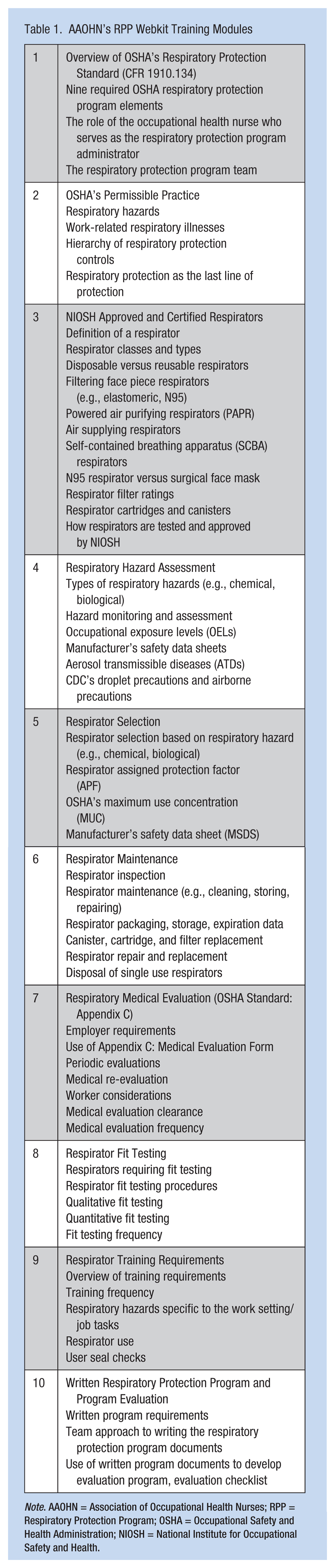
Note. AAOHN = Association of Occupational Health Nurses; RPP = Respiratory Protection Program; OSHA = Occupational Safety and Health Administration; NIOSH = National Institute for Occupational Safety and Health.
Topics of the RPP Webkit’s Online Resources
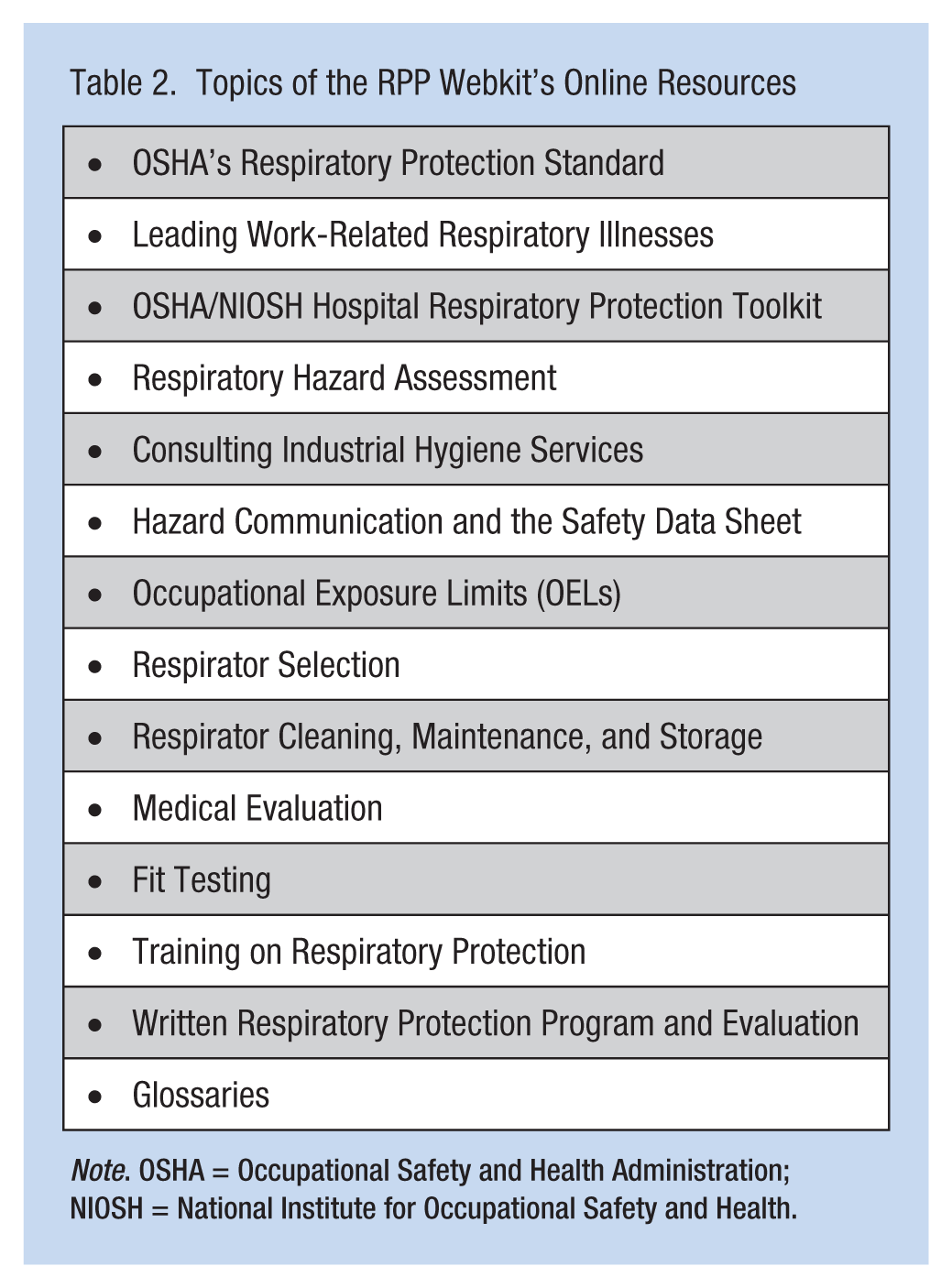

Note. OSHA = Occupational Safety and Health Administration; NIOSH = National Institute for Occupational Safety and Health.
Articulate Storyline (Articulate Global Inc., 2001-2013) was used to develop 10 online training modules, incorporating a variety of interactive educational modalities including voice-over presentation, videos, animated photographs, interactive quizzes, and resources with URL links that were embedded throughout and at the end of each training module. Respiratory protection videos previously developed by OSHA (2009-2012) and NIOSH (available on the OSHA website: https://www.osha.gov/SLTC/respiratoryprotection/training_videos.html and YouTube: https://www.youtube.com/results?search_query=osha+respirator+training+) were instrumental in providing instruction pertaining to (a) classes of respirators (e.g., air purifying, atmosphere supplying respirators, (b) types of respirators (e.g., N95 filtering face piece, elastomeric, powered air purifying respirator, self-contained breathing apparatus [SCBA]), (c) how to don and doff the respirator, (d) purpose of the respirator user seal checks, (e) how to conduct negative pressure and positive pressure seal checks, (f) signs that a respirator seal is inadequate, and (g) types of respirator fit testing used by organizations. In the absence of video, photographs combined with animation features were used to illustrate details (e.g., the difference between the N95 respirator and surgical mask).
Respiratory protection materials are an integral part of the respiratory protection program (e.g., respirator manufacturer’s insert) meriting detailed review of their content and use. To ensure these details were not overlooked within the online training format, these documents were presented in a scanned interactive video format, and verbal instruction was concurrently provided on the specifics of the form. The user can manually move through the form and review its contents. For example, the respirator manufacturer’s insert is a document that RPP administrators must develop familiarity and workers must be trained to use. The manufacturer insert is presented so the participant can review its format, organization, and typical information including details on intended use, donning, doffing, and user seal checks. This same instructional approach was used to illustrate details of the Medical Evaluation form (OSHA Standard; Appendix C), as well as the respirator details typically outlined in a manufacturer’s safety data sheet (SDS).
RPP Webkit Pilot Testing
Convenience sampling was used to select occupational health nurses for pilot testing the training before it was launched on the AAOHN website or delivered face-to-face. Through email invitations, the authors solicited feedback on the online training from occupational health nurse graduate students and practicing occupational health nurses in North Carolina (n = 14). Those nurses who participated were paid $25 for their time. The authors also solicited feedback for the face-to-face training from members of the Houston, Texas AAOHN Chapter (n = 31); five $25 gift cards were raffled at the end of the training. All pilot test participants also received 1 hour of continuing education.
For purposes of testing the content, occupational health nurses were asked to complete a pre- and post-test before and after the training. Among those nurses who took the training online, their mean pre-test score was 80% and their mean post-test score was 91%. The face-to-face training mean pre-test score was 64% and mean post-test score was 80%. For the face-to-face training, participants did not improve on questions pertaining to hazard assessment and respirator type specific to biological hazards; the online participants did improve in these areas. These differences may be attributed to the 1-hour time limit for the face-to-face training, whereas those nurses who took the online training could participate in the training at their own pace, including reviewing slides and resource content repeatedly as needed without a time limit.
Participants were also asked to provide feedback about the quality of the training, how it could be improved, and any technical aspects about respiratory protection and the OSHA Respiratory Protection Standard that needed modification or improvement. Online participants indicated that they liked the URL links to external resources; however, some nurses asked to have the resources provided at the end of each module. The revised training modules include these resources. The authors also incorporated quiz questions throughout the training modules per nurses’ suggestions. Several participants indicated that the training was well organized and concise, and the training videos were extremely helpful. Given the large amount of content covered in the training, the majority of participants indicated that they spent 60 to 90 minutes completing the modules. With respect to the training length, half (7/14) indicated “it was the right length of time,” whereas the rest indicated “it was a little too long, but worth it.” The face-to-face training was well received, with participants indicating that the training should be delivered over 90 minutes rather than 60 minutes. The face-to-face offering was provided again in a 90-minute session in which participants indicated that a half-day workshop would be best. This feedback emphasizes the value of the RPP Webkit being online and available at all times for participants to review material at their own pace and as often as they desire.
AAOHN Academy’s Implementation and Evaluation of the RPP Webkit
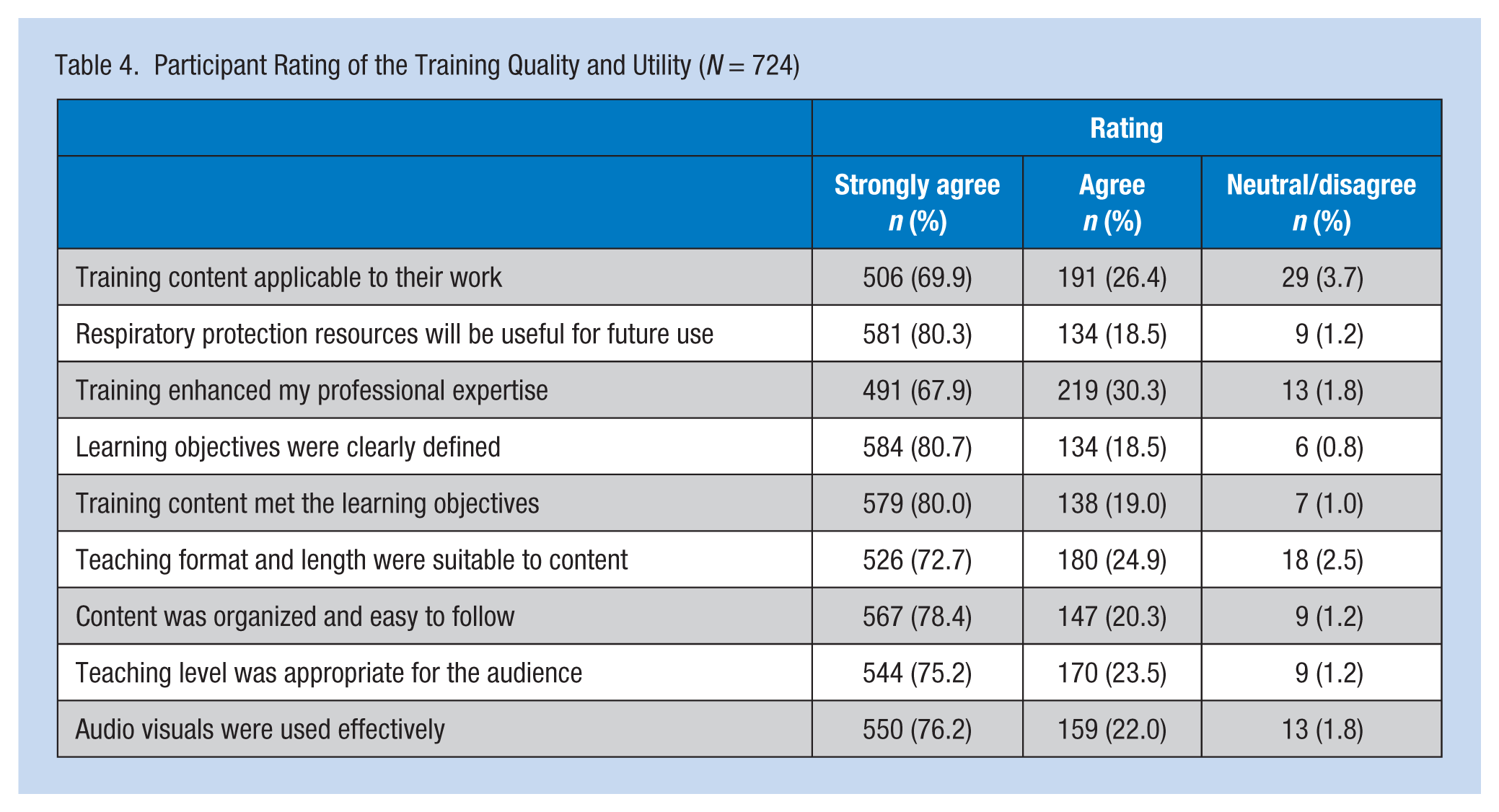
The RPP Webkit, including the online training and resources, went live on the AAOHN website in June 2014. As of January 2016, 747 participants had completed the online training, with 724 (97.0%) completing a post-training survey (Table 3). The majority of participants were registered nurses and had earned a bachelor of science in nursing (64.0%) or higher degree (22.3%), and worked in health care (36.2%), manufacturing (23.8%), or off-site/stand-alone occupational health clinic (13.9%). One third (32.6%) indicated they were responsible for their organization’s respiratory protection program; a smaller, but not an insignificant number (n = 111, 15.3%) indicated they would be responsible for their respiratory protection program in the near future. Half (n = 311, 52%) of the participants indicated they were not responsible for leading the program; however, 94% indicated that this training was relevant to their work and 98% indicated that the RPP resources would be useful in the future. The majority (69%) of all participants indicated that the training provided them with more knowledge on which to base decisions in their clinical practice and the training would assist them to do a better job (data not shown). Almost all (99.7%) indicated that they would recommend this course to others. Overall, the training was positively evaluated (Table 4), with the majority indicating that they “strongly agreed” or “agreed” program content was applicable to their work, the RPP Webkit resources would be useful in the future, and the training enhanced their professional expertise.
Training Participants’ Demographic and Occupational Characteristics (N = 724)
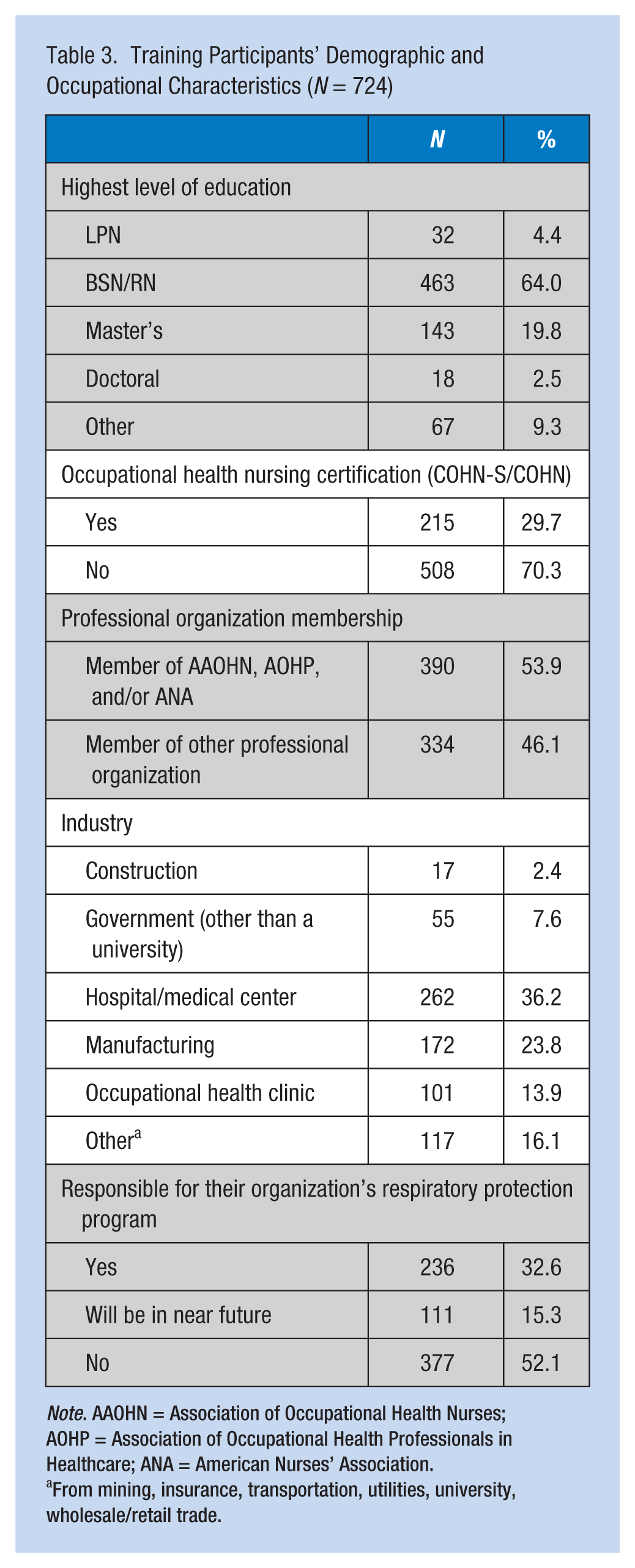
Note. AAOHN = Association of Occupational Health Nurses; AOHP = Association of Occupational Health Professionals in Healthcare; ANA = American Nurses’ Association.
From mining, insurance, transportation, utilities, university, wholesale/retail trade.
Participant Rating of the Training Quality and Utility (N = 724)
Accessing the AAOHN RPP Webkit
The online respiratory protection training and resources are offered free to AAOHN members and non-members through the AAOHN Academy (www.aaohn.org). Members can simply log into the AAOHN website’s Education page. Non-members of AAOHN must first create a guest AAOHN account. This training also offers free continuing education credit.
Next Steps
So far, the development and implementation of the AAOHN RPP Webkit has been successful and well received by occupational health nurses. The number of participants who have completed this training in the first 18 months suggests the training is relevant to occupational health nursing roles and responsibilities, and several of the long-term goals of the IOM (2011) Report are being met. Next steps for building on the RPP Webkit include developing case studies specific to respiratory protection, based on IOM recommendations and feedback from the Respiratory Protection Survey of occupational health nurses, described above (Burgel et al., 2014). An online AAOHN webinar of respiratory protection case studies was offered to members in February 2015 (Pompeii & Delclos, 2015), which will be incorporated as an interactive case study module into the existing RPP Webkit. In addition, AAOHN will offer respiratory protection competencies training relevant to “proficient” and “expert” occupational health nurses, including training on how to develop written respiratory protection program documents, and how to use these documents to effectively evaluate a respiratory protection program, including measuring adherence with respirator use and appropriate respirator use practices (e.g., respirator donning, doffing, and user seal checks) by frontline workers.
Implications for Occupational Health Nursing Practice
Occupational health nurses deliver health and safety programs and services to workers, worker populations, and community groups. Their practice focuses on promotion and restoration of health, prevention of illness and injury, and protection of workers from work-related and environmental hazards. Occupational health nurses, employed in organizations where workers are required to wear respiratory protection, should be practicing, at a minimum, at the competent level outlined in the Respiratory Protection Competencies (Burns et al., 2014). Having a fundamental knowledge of work-related hazards that can result in respiratory illness and how to protect from these hazards using personal protective equipment is essential. In addition, occupational health nurses in these settings should have practical knowledge about the required RPP elements mandated by OSHA. It is noteworthy that some studies have reported that although hospitals may have some required RPP elements in place, workers closest to the bedside who are at greatest risk of respiratory illness were the least compliant in using respiratory protection (Peterson et al., 2015). Hospitals had written respiratory protection program documents and workers could recall being fit-tested; however, ongoing training was lacking and frontline workers were unclear about when and how to wear respiratory protection or which types of respiratory protection to choose. The training and resources provided in the RPP Webkit can prepare occupational health nurses to effectively coach workers and managers, through training (and other program elements), on the importance of respiratory protection, correct respirator type, and when and how respirators should be worn. More specifically, this training provides a comprehensive overview of OSHA’s Respiratory Protection Standard’s nine required program elements that organizations are mandated to have in place if their workers are required to wear respirators to perform their jobs. This training is essential content for occupational health nurses responsible for leading their organizations’ respiratory protection programs, as well as those working in organizations with respiratory protection programs.
In Summary
The National Institute for Occupational Safety and Health’s National Personal Protective Technology Laboratory have supported a four-phase process, including the development of the RPP Webkit, for championing occupational health nurses serving as their organizations’ respiratory protection program administrators.
The RPP Webkit includes a 60 to 90 minute self-paced online training program as well as online resources. This training provides an overview of OSHA’s Respiratory Protection Standard’s nine required program elements and details how to implement these elements as the program’s administrator.
The RPP Webkit is available free to AAOHN members and non-members on the AAOHN website. The RPP Webkit is always available for use. Free CNE credits available.
Footnotes
Acknowledgements
The authors gratefully acknowledge the consultation, participation, and contributions of Debra Novak, PhD, RN, NIOSH Project Officer, Senior Service Fellow CDC/NIOSH/NPPTL. The authors appreciate the assistance of the respiratory protection working group including Candace Burns, PhD, ARNP, Professor and Director, Occupational Health Nursing Program and Deputy Director, Sunshine Education and Research Center (ERC), University of South Florida; Paxson Barker, PhD, Associate Professor, Department of Nursing, Washington Adventists University; Annette Byrd, MPH, RN, IC®, Education Consultant to AAOHN; Kim Gordon, MSN, MA, RN, COHN-S, FAAOHN, Deputy Director and Director of Continuing Education, Heartland Center for Occupational Safety and Health and WORKSAFE IOWA, University of Iowa; Mary Ann Gruden, MSN, CRNP, NP-C, COHN-S/CM, Manager, Employee Health Services, Allegheny General Hospital; Ann Lachat, RN, BSN, FAAOHN, COHN-S/CM, former Chief Executive Officer, American Board of Occupational Health Nurses, Inc. (ABOHN); Mary Gene Ryan, MPH, BSN, COHN-S/SM, FAAOHN, Executive Director MGRyan & Co., Inc.; Deborah Taormina, MS, RN, ANP-BC, COHN-S, Occupational Health Nurse Practitioner, Occupational Health Center, Stanford University. The authors also acknowledge contributors to the development of the RPP Webkit, So Young Kwon, PhD, Educational Developer; Michelle Karpman, PhD, Research Associate; Janelle Rios, PhD, Continuing Education and Outreach Specialist; Joy De Los Reyes, MPH, Project Manager at the University of Texas Health Science Center at Houston, School of Public Health and the Southwest Center for Occupational and Environmental Health.
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded by the National Institute for Occupational Safety and Health and the National Personal Protective Technology Laboratory (Contract #:254-2012-M-52637).
Author Biographies
Lisa Pompeii, PhD, COHN-S, FAAOHN, associate professor, Environmental and Occupational Health Sciences, School of Public Health, University of Texas Health Science Center at Houston.
Annette Byrd, MPH, RN, IC®, educational director for the American Association for Occupational Health Nurses (AAOHN).
George L. Delclos, MD, PhD, MPH, professor, Environmental and Occupational Health Sciences, School of Public Health, University of Texas Health Science Center at Houston.
Sadie H. Conway, PhD, assistant professor, Environmental and Occupational Health Sciences, School of Public Health, University of Texas Health Science Center at Houston.
