Abstract
Today’s employers are hiring a more age-diverse workforce. As Americans work longer, age-related changes often create activity limitations. Musculoskeletal disorders affect many older workers heightening their risk of workplace injury. Compounded by multiple comorbidities, older workers will need occupational health nurses with expert knowledge to maintain safe and productive workplaces. Older workers do not experience as many injuries as younger workers, but when they are injured, recovery is longer. The author developed and conducted a survey of New Jersey occupational health nurses. The results showed that overexertion injuries are the most frequently treated injuries in employee health offices. For occupational health nurses to keep employees safe, best practices must be delineated; this musculoskeletal safety guideline provides recommendations for evidence-based care of older workers.
Research indicates that over 20% of the U.S. population will be at least 55 years old by the year 2050 increasing the prevalence of chronic illness, musculoskeletal disorders, and occupational as well as non-occupational musculoskeletal injuries in older adult workers (Canning & Bloom, 2012). In addition, many older adults are choosing not to retire as early as previous generations. These trends suggest occupational health nurses and advanced practice nurses working in occupational health will be providing nursing care for a rapidly increasing elderly workforce employed in manufacturing and nonmanufacturing settings. These changes, leading to a new “multigenerational” workforce with multiple comorbidities, will require nurses with expert knowledge to evaluate and manage older employees with musculoskeletal injuries. Safety for the older worker must be a priority.
Besides changes in vision and hearing and decreased strength and flexibility, older adults experience musculoskeletal changes that can result in arthritis (Blagojevic, Jinks, Jeffrey & Jordan, 2010; Keller & Burns, 2010). To compound this physiological effect, the incidence of arthritis increases to one of every two individuals aged 65 years and older (Caban-Martinez et al., 2011). Research has documented how aging affects human body systems but evidence-based safety guidelines for older workers could provide the foundation for occupational health nurses to develop strategies and gain insight into the future nursing care needed by this population.
Needs Assessment
The increase in aging workers will bring challenges for nurses providing care to older adults. A sound educational foundation of how aging affects individuals’ risk of injury is extremely important for nurses in the workplace. Having this knowledge should lower workers’ risk of musculoskeletal injury. Occupational health nurses care for employees who have been injured on and off the job. For this reason, they are essential members of the health care team.
The need for a musculoskeletal safety guideline as a resource for occupational health nurses was identified by the author after participating in informal discussions with New Jersey occupational health nurses. The author conducted a series of 12 face-to-face or teleconference interviews with musculoskeletal experts from physical therapy, occupational therapy, ergonomics, workplace design, safety, and advanced practice nursing to understand content that should be included in the development of a safety guideline.
To evaluate the prevalence of musculoskeletal disorders, particularly overexertion injuries, a survey was sent to New Jersey occupational health nurses to determine the three most common types of injuries the nurses identified in their offices. The survey included questions to determine whether any policies or musculoskeletal safety guidelines were used in New Jersey organizations and the types of charting procedures occupational health nurses were using. To search for strong evidence to support the guideline, an extensive review of the literature using key words (e.g., international aging workforce, safety, and age-related changes) was completed. To identify if a gap existed in this area of research, three national occupational health nurse experts used the Agree 2 evaluation tool to compare the strengths and weaknesses of three national guidelines. This instrument is used to evaluate the quality of an existing guideline and newly developed guidelines being considered for clinical practice (Brouwers et al., 2010).
Method
The search engines for the literature review were Medline, CINAHL, Business Source Primer and Google Scholar. Thirty-two articles were reviewed. Five studies were rejected because they did not meet the inclusion criteria (i.e., publications in English and articles that reviewed age-related changes and ergonomic impact) and exclusion criteria (i.e., data published before January 2005, publications focusing on chronic disease, unpublished works, individuals aged 55 or younger, and emphasis on the psychosocial impact of occupational injury rather than musculoskeletal disorders or injuries).
Next, a doctoral committee was assembled to guide the project. The committee members were chosen for their expert knowledge needed for the development and implementation of the project. Because “older adults” were the target population, an expert in adult and gerontology nursing was selected to review the disease content and chair the committee. The guideline was meant to be used by occupational health nurses in all types of organizational settings. So, a nurse expert in leadership was chosen to provide organizational management of the project. The final committee member was a statistical expert to assist in data analysis.
The external reviewers were three individuals considered experts in the field of occupational health nursing. One university professor in the group is well recognized as a musculoskeletal injury researcher. The second reviewer is a university professor and expert reviewer of scholarly publications for peer-reviewed journals. The third reviewer is a university clinical professor in the field of community health.
The Agree 2 evaluation was applied to national guidelines by two of the three occupational health nurse experts. The musculoskeletal injury researcher reviewed the initial draft of the musculoskeletal safety guideline later developed by the author. This instrument was used to appraise the
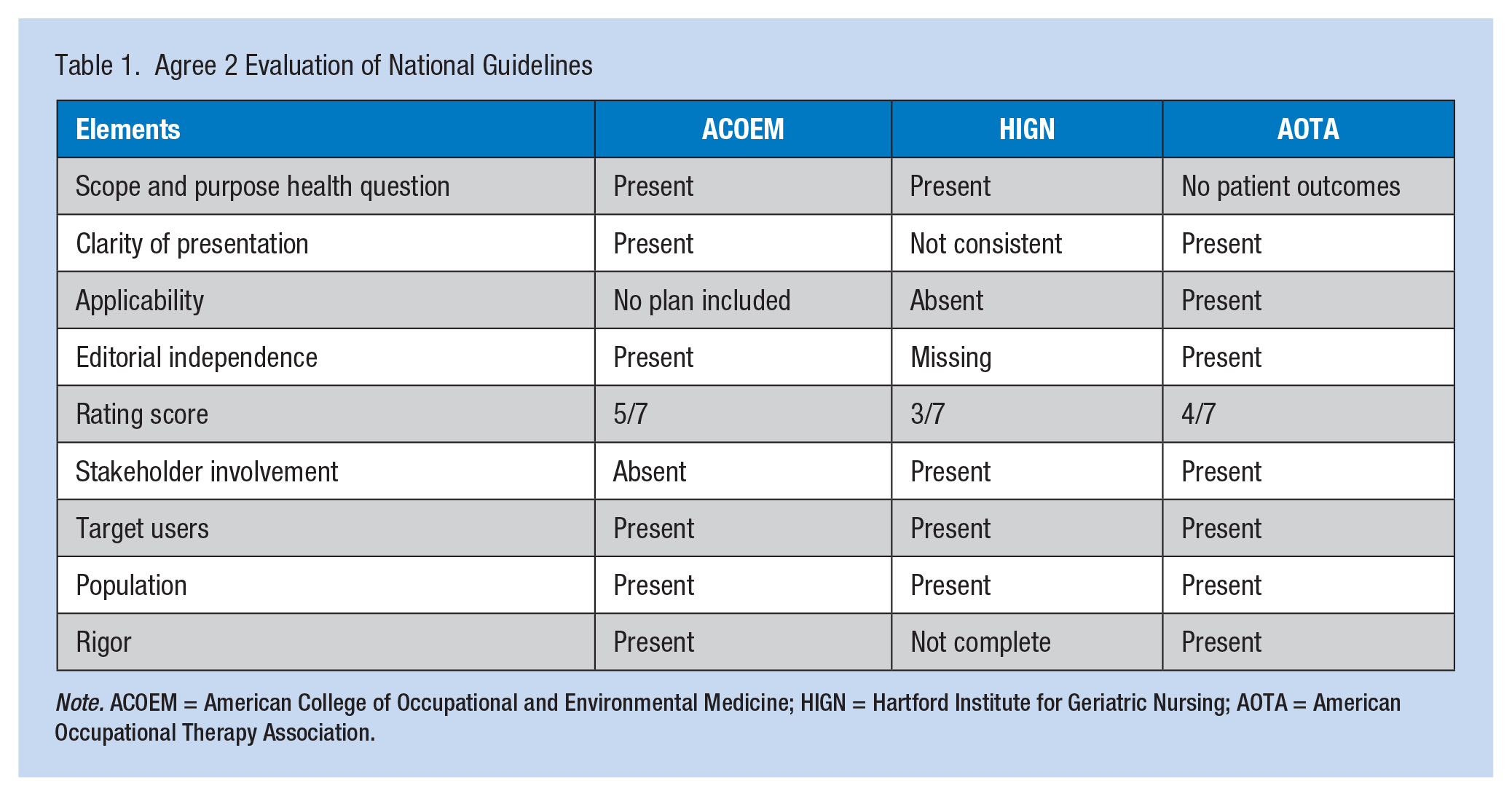
After the Agree 2 evaluations were completed, a comparison table was developed by the author to identify key elements that should definitely be included in the musculoskeletal safety guideline (Table 1). The rigorous evaluations demonstrated that no quality nursing guidelines were available for nurses to identify age-related risk factors. The highest Agree 2 rating was given to a medical guideline. These evaluations further supported the need for a standardized nursing guideline. The Center of Evidence-Based Medicine (CEBM) levels of evidence were used for rating all five main articles included in the evidence table (Phillips et al., 2009). The guideline was further supported by the use of additional relevant articles.
Agree 2 Evaluation of National Guidelines
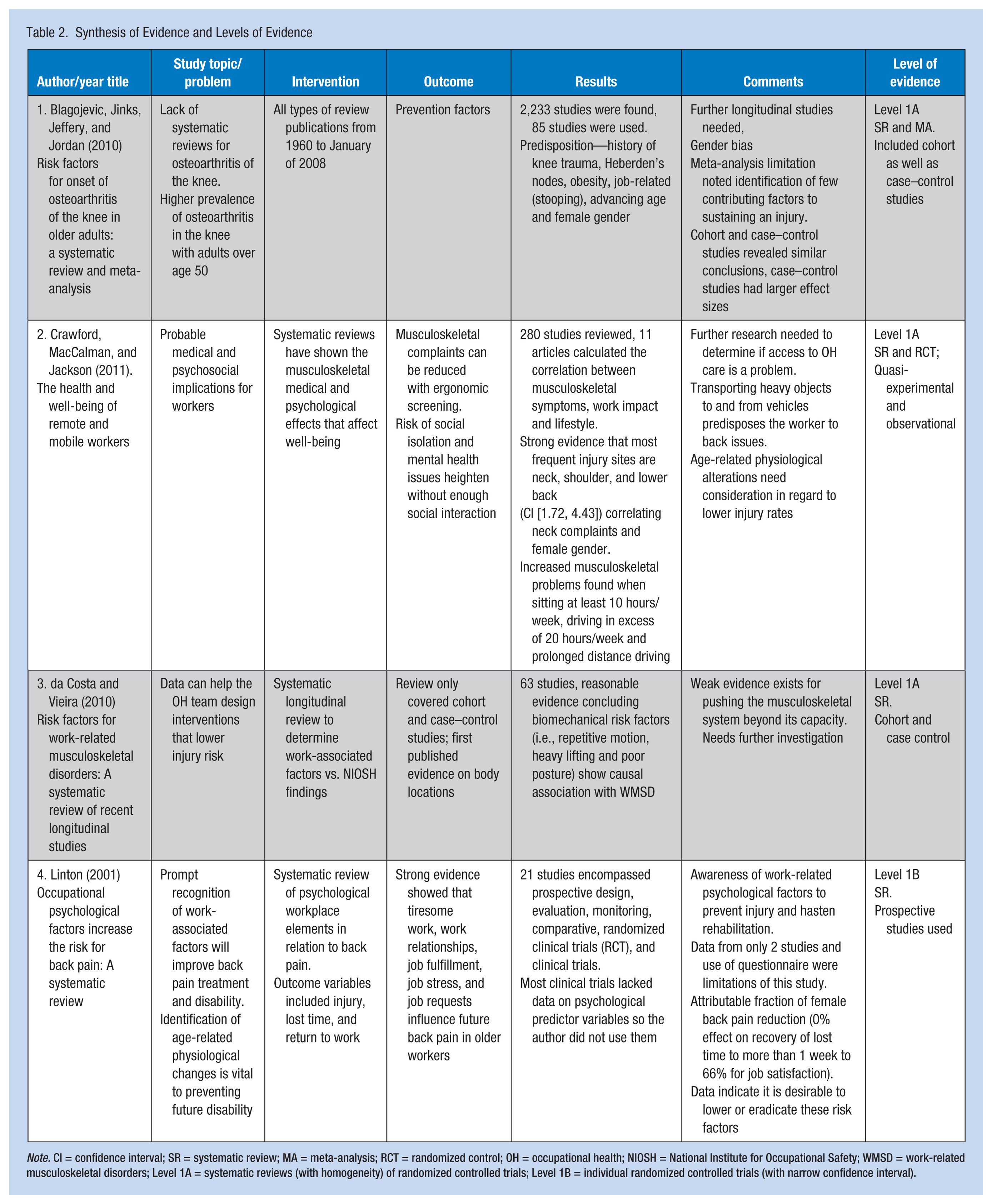
Synthesis of Evidence and Levels of Evidence
Additional Research Supporting Development of Evidence-Based Safety Guideline/Educational Program
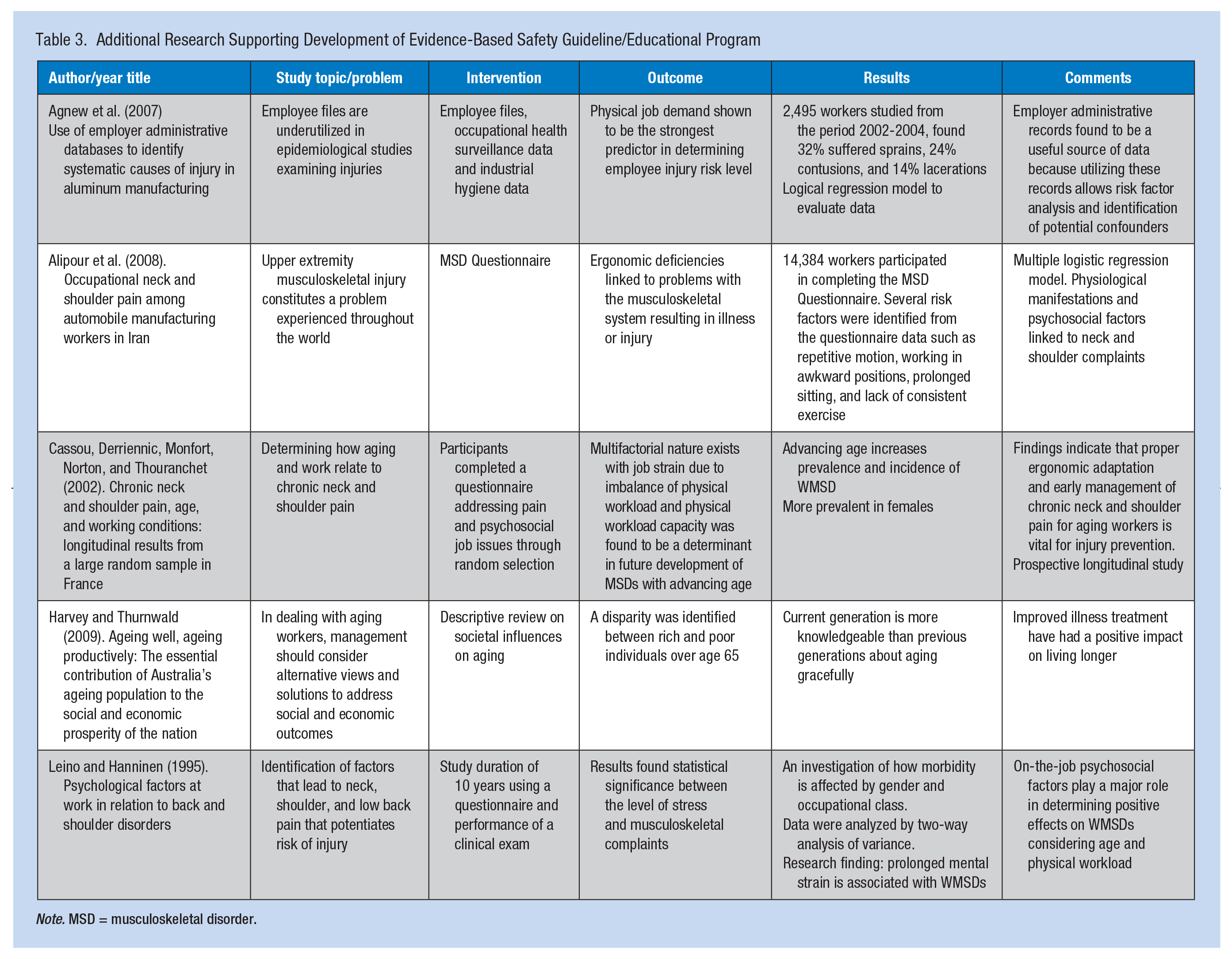
After the previous steps were completed, a comprehensive evidence-based safety guideline to lower the risk of musculoskeletal injuries was developed from an in-depth literature review, expert reviewers, and evaluation of three national guidelines using the results of the Agree 2 evaluations. The intended users of this guideline are occupational health nurses and advanced practice nurses. The recommendations below are intended to increase occupational health nurses’ knowledge of assessment, education, and evaluation of age-related risk factors for musculoskeletal injuries.
The following is a synopsis of the recommendations from the comprehensive guideline:
Age-related musculoskeletal changes increase injury risk for older adults (Bohle, Pitts, & Quinlan, 2010; Centers for Disease Control and Prevention, 2009; da Costa & Vierira, 2010; Foster, Hartvigsen, & Croft, 2012; Hush, Cameron, & Mackey, 2013; Perry, 2010). Prompt detection of musculoskeletal symptoms is paramount to improving injury rates and recurrent injuries.
While gathering a musculoskeletal history, concentrate on symptomology that can precipitate overexertion injuries or result in falls.
Conduct a fall risk evaluation of older workers by using the Hendrich 11 Fall Risk Model (retrieved from http://consultgerirn.org/uploads/File/try_this_8.pdf)
When documenting health histories, record the onset of chronic conditions to calculate workers’ injury risks. Health issues that lower physical activity increase the risk of musculoskeletal injury (Linton, 2001).
“When taking a psycho-social history, factors such as self-imagined age, work\home balance, social support, work breaks, job satisfaction, supervisor and employee working relationship, socialization, relaxation methods and sleep patterns can increase risk of injury” (Hauke, Flintrop, Brun, & Rugulies, 2011; Linton, 2001, pp. 56-57).
Assess for adverse medication reactions that occur with advancing age that can lead to increased risk of work-related injury.
When documenting occupational histories, the time workers have been functioning in an ergonomically demanding environment is important to identifying injury risk (Agnew et al., 2007; Cassou, Derriennic, Monfort, Norton, & Touranchet, 2002).
Use an age-sensitive manner when examining older employees (Leggert, 2007).
When examining older workers for musculoskeletal issues, focus on the areas of the body where injury tends to occur: “eye, low back, shoulder, neck, hand, wrist, ankle and foot” (Crawford, MacCalman, & Jackson, 2011; da Costa & Vieira, 2010, pp. 32-33).
Assess the areas where workers perform job functions, and observe workers engaged in daily activities. This process will determine how much ergonomic factors influence workers’ risk and complaints.
Refer workers as soon as possible to physical therapy and occupational therapy to lower absenteeism rates (Foster et al., 2012).
Increase workers’ knowledge of low back risk factors: bending, twisting, pulling, pushing, reaching, climbing, and prolonged sitting (da Costa & Vieira, 2010; Leino & Hanninen, 1995).
Encourage rotation of sitting and standing while completing job tasks (Alipour, Ghaffari, Shariati, Jensen & Vingard, 2008).
The glenohumeral joint should be examined. This is the most unstable joint when engaged in hand-operated workplace activities (Seidel et al., 2011).
Older workers can suffer loss of consciousness from postural hypotensive changes (Harvey & Thurwald, 2009; Perry, 2010). Instruct older workers to move slowly when standing and sitting.
Encourage older workers to walk. Instruct employees that not enough exercise can interfere with coordination, balance, flexibility, and strength. These areas are already compromised with advancing age (Kravitz & ACOSM, 2011; ACOEM Clinical Practice and Guideline Center, 2012).
Cardiovascular disease negatively affects older workers with slower healing after suffering work-related musculoskeletal injuries. Therefore, instruct older workers not to sit for extended periods of time at their desks (American College of Sports Medicine, 2011; Goff et al., 2014).
Instruct workers that “lifting 35 pounds or more and lifting more than the horizontal distance of 20 inches from the person’s ankle, increases the risk of injury” (Chaffin & Park, 1973, p. 516).
In positions requiring repetitive motion, encourage sufficient time for muscle and tendon recovery by participating in adequate rest breaks.
Conclusion
When developing an evidence-based guideline, the author must be immersed in the process using a structured organized approach for the assessment, education, and prevention of the problem. The approach used in this article to design a musculoskeletal guideline can be used as a springboard for occupational health nurses and other nurse specialties to improve their practice. Due to the shortage of evidence-based “best practices” available for registered nurses and advanced practice nurses working in occupational health and safety, these guideline recommendations will assist nurses caring for older workers to prevent musculoskeletal injuries.
Footnotes
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Biography
Nancy Delloiacono received a Doctor of Nursing Practice degree, and a Post-Masters Certificate, Primary Care of the Adult and Aged Nurse Practitioner Post Master’s Program from Rutgers, The State University of New Jersey School of Nursing. She is employed at Rutgers School of Nursing as the nursing resource center coordinator and also employed as an APN-BC in home care at Universal Health Care Navigators. She has 7 years of experience as an occupational health nurse.
