Abstract
Age-associated physical musculoskeletal alterations increase elder adults’ (age 55 and older) risk for injury. Research has demonstrated that on-the-job injuries result in increased absenteeism, and fatalities are more common for the elder adult population. Older adults aged above 65 years comprise the fastest-growing segment of the U.S. population, growing from 40.2 million in 2010 to 88.5 million projected by 2050; this population shift will generate challenges for occupational health nurses providing care for older workers. A paucity of evidence-based “best practices” exists in which occupational health nurses can assess the physical status of older workers, evaluate their risk for age-related musculoskeletal injuries, and educate these workers on injury prevention. This article provides a critical synthesis of research on age-related physical and cognitive changes and their impact on safety, providing “best practice” evidence for occupational health nurses to examine and apply.
The percentage of elder adults is predicted to double and re-double in another 10 years (Keller & Burns, 2010). According to Loeppke et al. (2013), “older workers are defined as individuals who are 55 years or older employed in any capacity” (p. 501). The increase in older adults employed in the workforce is mainly due to workers delaying retirement, training for alternate careers, and increasing their longevity due to health care advances (Canning & Bloom, 2012; Harvey, & Thurnwald, 2009; Leggert, 2007). To address the issue of older workers in the workplace, research on musculoskeletal injuries and disorders (MSDs) were reviewed using the definition provided by da Costa and Vieira (2010): “Injuries or dysfunctions affecting muscles, bones, nerves, tendons, ligaments, joints, cartilages and spinal discs. These disorders included sprains, strains, tears, soreness, pain, carpal tunnel syndrome, hernias, and connective tissue injuries of the structures previously mentioned” (p. 286).
The intent of this review was to critique and synthesize current research findings to increase occupational health nurses’ knowledge of age-related physical changes that increase older workers’ risk of occupational injury. Research has shown that the safety of older adults in the workplace is an occupational priority for employers, occupational health nurses, and safety experts (Canning & Bloom, 2012; Loeppke et al., 2013). Current knowledge reflects the literature on age-related physical changes but gaps exist in research on effective in-place strategies to assist companies and occupational health nurses provide adaptations for older workers. Gaining knowledge in this area could improve nurses’ abilities to properly identify risk factors for older adult workers and prevent serious injuries.
Slavin’s method of conducting literature reviews, known as
Age-related physical changes often cause occupational injuries and restrict activity (Lee et al, 2012). Research has shown many older employees suffer from some type of MSD with the most significant changes seen in joints (Tugman, 2013; United States Bone and Joint Initiative, 2011). These changes may result in arthritis; the incidence of arthritis has been found to increase dramatically after age 45 (United States Bone and Joint Initiative, 2011). Research has also shown that age-related physical changes, including acute and chronic disease and MSDs, can negatively affect job performance and consequently contribute to an increased risk of injury (Silverstein, 2008).
The global population is also aging and 20% of the population in the United States will become age 65 over the next 35 years (Canning & Bloom, 2012). Many companies do not employ appropriate safety approaches and procedures to protect and promote healthy behavior in older employees (Canning & Bloom, 2012; Loeppke et al., 2013). Based on these trends, occupational health nurses must be prepared to provide care for a large number of older adults employed worldwide in all types of organizational settings.
Method
Articles for this review were drawn from electronic bibliographic databases and hand searches of published literature. The electronic databases, MEDLINE, CINAHL, Business Source Primer, and Google Scholar were searched from January, 2005, through May, 2014, using the search term “work-related injury” to identify the target population. The keyword “illness” was not used, so as to narrow the search to specific evidence on musculoskeletal injury. The keywords “age-related changes” and “safety” were used in tandem to assess how much research has been done on this emerging global issue. The term “older adult” was not used because authors do not use a single term across studies. Inclusion criteria were as follows: articles published in English and those that reviewed age-related changes and ergonomic impact. Exclusion criteria were as follows: data published before January 2005, publications focusing on chronic disease, unpublished works, participants below the age of 55, and emphasis on psychosocial impact of occupational injury rather than musculoskeletal issues. Thirty-two articles were reviewed. Twenty-seven articles were rejected because they did not meet the inclusion and exclusion criteria.
Literature Synthesis
According to Culp, Tonelli, and Ramey (2011), “the average life span has increased for individuals from 68.9 years (during the 1950s) to 79 years (in 2009)” (p. 87). Increasing longevity and advances in health care are two reasons why many individuals continue to work into their 80s (Canning & Bloom, 2012). Concurrently, fertility rates have decreased, resulting in fewer younger workers in the U.S. workforce (Loeppke et al., 2013). Globally, more contingent workers report poorer health than non-contingent workers. Contingent workers’ health status is probably due to less access to safety and health education at work. Consequently, their risk of workplace injury increases (Bohle, Pitts, & Quinlan, 2010). To respond to these trends, occupational health nurses, critical members of the interprofessional team, are charged with reducing work-related injuries among older workers.
Significance of the Problem
In 2011, more than 3 million severe occupational injuries and more than 4,000 deaths were recorded in the United States (U.S. Bureau of Labor Statistics, 2011). According to the 2010 Liberty Workplace Safety Index, the most severe workers’ compensation injuries cost a total of US$51.1 billion (Liberty Mutual Institute for Safety [LMIS], 2012). Overall, overexertion injuries led the Liberty Workplace Safety Index. “Overexertion is defined as injuries occurring from individuals pushing, holding, lifting, throwing, carrying, and pulling objects” (LMIS, 2012, p. 6). In 2010, overexertion injuries cost corporations a total of US$13.61 billion in direct cost expenses (LMIS, 2012). According to Cheng and Chan (2009), injuries due to lifting or carrying accounted for 19% of the total occupational injuries in Hong Kong. A study by Hoonakker and van Duivenbooden (2010) found that Dutch construction workers, age 55 and older, who engage in awkward postures were at risk of musculoskeletal injuries. Employees in the United Kingdom experiencing work-related back pain lose almost 6 million workdays (Cheng & Chan, 2009). In addition to overexertion injuries, falls on the same floor level as the worker cost companies US$6.6 billion (LMIS, 2012).
Economic Cost–Benefit Considerations
Because the rate of fatal work-related injuries is higher for older workers than for younger workers (Loeppke et al., 2013) and older workers have a slower recovery rate after an occupational injury (Silverstein, 2008), injury prevention programs are essential for this population. A study of coal miners above age 50 found an association between their age and absenteeism after sustaining an occupational injury (Margolis, 2010). According to the Occupational Safety and Health Administration (OSHA; OSHA and U.S. Department of Labor, 2008), implementing safety programs and guidelines can reduce the financial burden caused by injury and illness for workers and companies.
Other Considerations
The number of workers above age 55 requiring chronic disease care has increased by more than 2% during the last 10 years (United States Bone and Joint Initiative, 2011). Much of this care is required for MSDs (United States Bone and Joint Initiative, 2011). MSDs and resulting chronic pain have been shown to be expensive health problems for health insurance companies and the workers’ compensation system (Gaskin & Richard, 2012). In order of occurrence, the areas of musculoskeletal pain most encountered by older adults are low back, shoulder, neck, and knee (Foster, Hartvigsen, & Croft, 2012). The risk of workplace injury is higher for individuals with pain and MSDs than those with other types of injuries and resulting pain.
Individuals diagnosed with MSDs experience the highest occurrence of arthritic and joint pain symptoms (United States Bone and Joint Initiative, 2011). It is projected that 67 million adults above age 18 will be diagnosed with arthritis by 2030 (Caban-Martinez et al., 2011). As baby boomers age, many will be diagnosed with arthritic disease by age 55. This increased prevalence of MSDs will place additional older employees at risk of musculoskeletal injury. Both blue-collar and older employees have a higher risk of developing arthritis and losing their jobs due to this disease (Caban-Martinez et al., 2011). In reviewing the literature, a systematic review and meta-analysis found that above age 50, workers experience an increased prevalence of knee osteoarthritis (Blagojevic, Jinks, Jeffrey, & Jordan, 2010). These findings are significant for older adults whose job requires them to squat or kneel. A limitation of this meta-analysis review was the small number (82) of risk-factor studies included. However, the systematic review in this article included case control studies that demonstrate a larger effect size.
Age-Related Physical Changes
Mobility changes
Mobility loss is found with advancing age. Research has documented the negative effects of sedentary behavior on cardiovascular health but this behavior also affects mobility by increasing the risk of future disability (American College of Sports Medicine [ACSM], 2011). “Sitting disease” affects many individuals in the work setting.
Balance changes
After age 50, many individuals experience alterations in balance increasing their risk for falls (Silverstein, 2008). These injuries are costly to both organizations and workers (Silverstein, 2008). Regular exercise may improve balance (ACSM, 2011).
Strength and overall endurance changes
Research shows that muscle strength decreases with age due to muscle fiber atrophy (Perry, 2010). Older workers experience more difficulty completing job tasks due to an imbalance between available muscle strength and muscle strength demand (Perry, 2010). Without proper nutrition and adequate exercise, muscle fiber is replaced by fat tissue leading to less endurance and productivity, which can negatively affect safety (Perry, 2010).
Sight changes
Visual acuity decreases as workers age. Dynamic visual acuity deteriorates with age, which increases the risk of injury (Perry, 2010). Perry (2010) defines “dynamic visual acuity as the ability to resolve details of a moving target” (p. 23). As a result, older adults have difficulty following visual targets, which is important if their job requires them to drive (Perry, 2010).
Pain as a Factor
Fatal falls are a major problem for workers aged 65 and older (CDC, 2009). Pain medication is a notable risk factor for falls; increased use of pain prescriptions for acute and chronic pain may be a contributing factor in falls.
Low back, neck, and shoulder pain are common areas for acute and chronic pain among American workers. Hauke, Flintrop, Brun, and Rugulies (2011) reviewed complaints of low back, neck, and shoulder pain in workers and found that pain in these areas contributed to worker absenteeism and disability. Hauke reported evidence of an association between MSDs in the low back, neck, and shoulder with physical, emotional, and social factors that had occurred at the workplace. The results showed a statistically significant relationship between workers’ low back, neck, and shoulder pain and working conditions (e.g., lack of social support, little job satisfaction, and constant job pressure).
Stress at Work
Further research indicated a triangular relationship between work-associated stress, illness and injury (Salonen, Arola, Nygard, & Huhtala, 2008). Women report occupational stress when they have little power over their own jobs (Salonen et al., 2008). A high percentage of these women have identified health issues that increase their risk of injuries (Salonen et al., 2008). Findings in this study demonstrated that prolonged symptoms associated with stress showed meaningful correlations with MSDs (Salonen et al., 2008). Assessment of stress-related symptoms is essential for reducing occupational stress (Salonen et al., 2008). Prolonged stress can predispose older workers to chronic diseases that can increase their risk of injury (Salonen et al., 2008).
A systematic review by Linton (2001) also reported strong evidence that monotonous work tasks, poor co-worker relationships, little job satisfaction, and exceptional job stress were related to the development of future back complaints and problems. Early identification of risk factors is needed to prevent long-term occupational back pain, which can become chronic and disabling.
Occupational health nurses can identify workers’ injury risk and needed ergonomic changes. da Costa and Vieira’s (2010) systematic review of recent longitudinal studies demonstrated a causal association between excessive repetition, heavy lifting, poor posture, and work-related MSDs. This study offers health care providers, ergonomists, and design specialists supporting evidence for interventions to lower MSD risk (da Costa & Vieira, 2010). The systematic review of remote and mobile workers’ health validated the need for ergonomic assessment and implementation of solutions (Crawford, MacCalman, & Jackson, 2011). The authors found that musculoskeletal symptoms among mobile workers improve with proper ergonomic interventions (Crawford et al., 2011). Strong evidence suggested that neck, shoulders, and low back were the most common areas of occupational injury (Crawford et al., 2011), validating the findings of the Hauke study.
Loeppke et al. (2013) found that “by utilizing the principles of safe design, musculoskeletal injuries on the job can be decreased when preventive interventions are correctly implemented” (p. 503). Ergonomists should assess universal design and human factors when implementing appropriate strategies for changes in senses, balance, and strength as workers advance in age to ensure the safety and increased productivity of elder employees (Loeppke et al., 2013; Perry, 2010).
This review may not have identified all articles related to the area of study. Synthesis reviews can be affected by author bias, so single studies were added. It was not the authors’ intent to include a rigorous search of articles about the psychosocial impact on injury; this should be investigated in another literature review.
Nursing Implications and Recommendations
These findings provide occupational health nurses with a synthesis of the available evidence to translate into practice. The risk of musculoskeletal injuries can be reduced when occupational health nurses assess physical alterations due to aging through the use of evidence-based nursing safety guidelines (see Table 1).
Suggested Evidence-Based Practices for Occupational Health Nurses to Reduce the Risk of Older Worker Musculoskeletal Injury
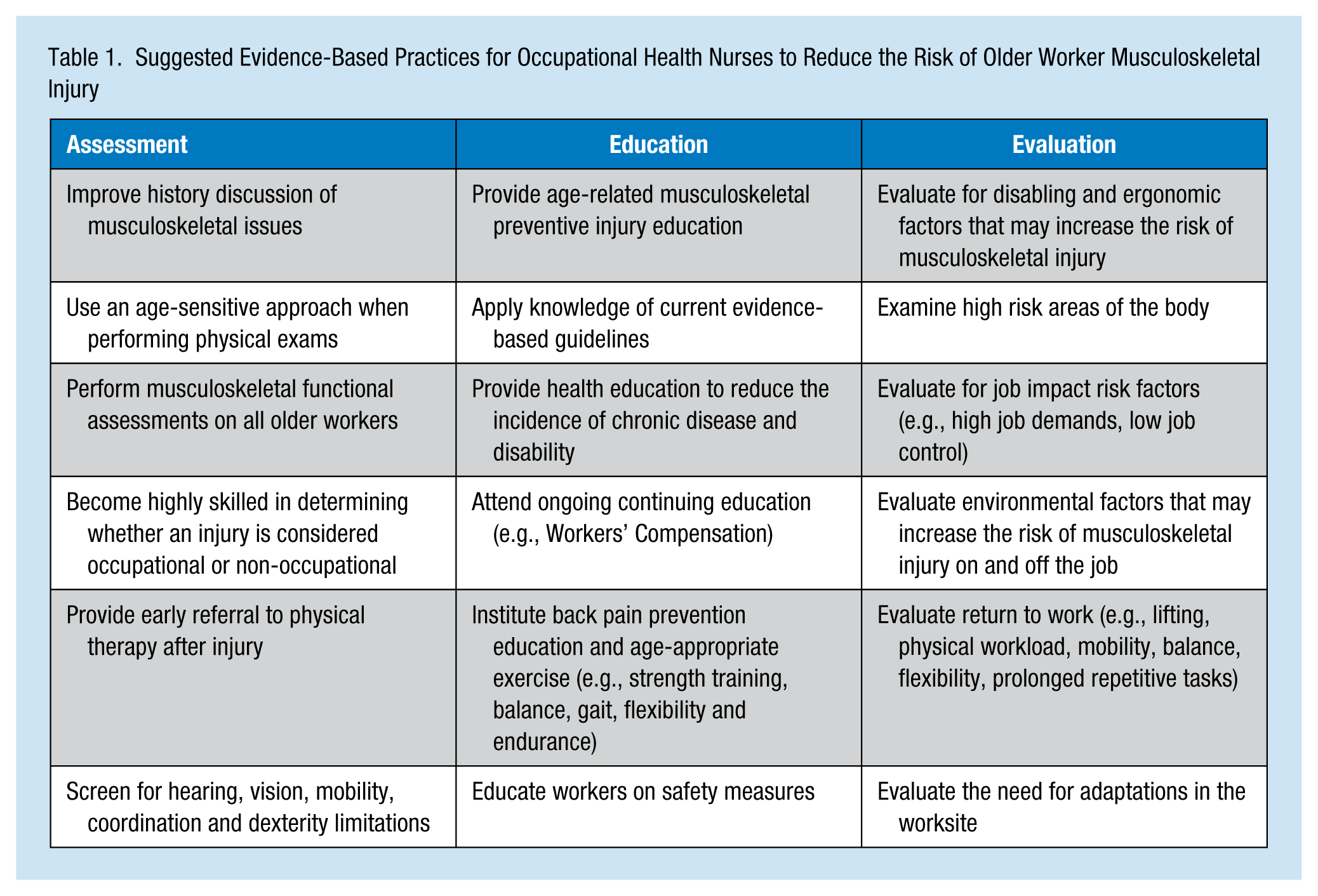
The extent of age-related physical changes experienced by older workers is significantly influenced by chronic illnesses (Bohle et al., 2010). Improving lifestyles could reduce organizational costs (American College of Occupational and Environmental Medicine [ACOEM], 2012). Reducing costs is important because although older worker statistics report lower work-related injury rates, their recovery is slower and lost work time is longer (Loeppke et al., 2013).
More interprofessional collaboration is needed among occupational health care experts to keep older workers safe (Culp et al., 2011). Occupational health nurse leaders must critique research and translate available evidence to safety guidelines for older workers. Strategies to enhance occupational health nursing education will improve nurses’ ability to conduct comprehensive musculoskeletal and ergonomic assessments. This skill set is critical for preserving employee functionality and productivity (Tugman, 2013). Occupational health nurses should provide employee education on the primary prevention of chronic disease (Dickerson, Brookham, & Chopp, 2010). This education may lower the incidence of chronic disease and co-morbidities as well as improve the overall health of older workers. To decrease chronic pain and loss of balance and strength, older employees should be taught by occupational health nurses to maintain joint flexibility through regular exercise (Perry, 2010). Older office workers should walk regularly to improve energy levels and functional ability. Workers should also be aware that exercise can lower their risk for injuries. These interventions should be encouraged by occupational health nurses and practiced by workers both in and outside the workplace (Schrack, Simonsick, & Ferrucci, 2010). Occupational health nurses, key members of the interprofessional team, educate workers about and reinforce health and safety daily practices to lower injury risk.
Other recommendations include the need to further investigate the impact of psychosocial factors on musculoskeletal safety, a current area of concern internationally (Loeppke et al., 2013). For example, negative workplace relationships may be a risk factor for MSDs and workplace injuries. Not addressing psychosocial factors can place older workers at increased risk of musculoskeletal injuries and reduced productivity. Occupational health nurses must merge the concepts of safety protection and health promotion to produce better employee health and safety outcomes (Hymel et al., 2011)
Conclusion
It is clear from the evidence generated that age-related physical changes among older workers is accompanied by a higher prevalence of MSDs and other chronic illnesses (Caban-Martinez et al., 2011; Canning & Bloom, 2012; Loeppke et al., 2013). This demographic change will create challenges in care delivery for occupational health nurses and occupational health nurse practitioners. By using evidence-based guidelines for employee care and developing strong evidence-based policies for changing workplaces to assist older workers in adapting, occupational health nurses can reduce workers’ risk factors for musculoskeletal injury. These strategies will require further research to evaluate their efficacy in preventing injuries in this age group. The quality of research in this area has improved by becoming more inclusive; research today focuses on not only ergonomics but also the prevention of chronic disease and MSDs to reduce injuries. New research on this issue is vital to further development of cost-effective, national, and international policies for older workers.
Footnotes
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Biography
Nancy Delloiacono completed a post-masters certificate in Primary Care of the Adult/Aged in January 2012 from Rutgers, the State University School of Nursing, and graduated with a Doctor of Nursing Practice degree from Rutgers, The State University School of Nursing, in May 2014. She has past experience as a visiting nurse, health department nurse, and occupational health nurse. Currently, she is a Nursing Resource Center coordinator at Rutgers, The State University School of Nursing, and an APN-BC employed in homecare at Universal Health Care Navigators.
