Abstract
This study investigates the complex relationships between health literacy, patient safety perception, and patient experience, which are critical indicators of healthcare quality. While previous research has focused primarily on large hospitals, this study fills a significant gap by focusing on inpatients in small- and medium-sized hospitals in South Korea. A key hypothesis was that patient safety perception would act as a crucial mediator in the relationship between health literacy and patient experience. A cross-sectional survey was conducted with 300 inpatients across three small- and medium-sized hospitals. Data were collected using validated questionnaires and analyzed with SPSS and the PROCESS Macro (Model 4) to test for mediation effects. The results confirmed that health literacy significantly and positively impacts both patient safety perception and patient experience. These findings suggest that improving patient safety perception may enhance the positive impact of health literacy on patient experience. Healthcare providers should consider implementing educational and organizational strategies to strengthen patient health literacy and safety awareness. Such initiatives may contribute to more patient-centered care and better-quality outcomes.
Plain Language Summary
Patient experience—how patients feel about the care they receive—is an important way to measure the quality of healthcare. This study looked at how two important factors, health literacy and patient safety perception, affect the experience of patients in small- and medium-sized hospitals in South Korea. The study found that patients who had higher health literacy were more likely to feel safe, and also reported better overall hospital experiences. It also found that patient safety perception played a partial mediating role—in other words, health literacy made patients feel safer, and that sense of safety helped improve their overall experience. These findings show that helping patients better understand health information and creating safer hospital environments can significantly improve how patients experience care.
Introduction
Patient-centeredness, which values patient preferences, values, and respect for patients, has emerged as a core element of the quality of medical care (Institute of Medicine, 2001). As part of efforts to realize patient-centeredness and improve the quality of medical care, patient experience evaluation has been introduced (Health Insurance Review & Assessment Service [HIRA], 2023). Patient experience evaluation, first implemented by the HIRA in 2017, is used as an indicator to evaluate the performance of healthcare, to expand patient-centered medical culture and improve the quality of medical care that the public can feel. According to the HIRA’s 2023 statistics, among the sub-areas of the evaluation, the nursing area was evaluated the highest at 85.03 points, while patient rights guarantee received the lowest score at 80.02 points. The scores for each area increased as institutions continued to participate in the evaluation (HIRA, 2023).
Patient experience evaluation is a way to determine the satisfaction level of the quality of medical care provided by medical professionals in medical institutions and environmental evaluation; it can provide direct information for identifying problems by identifying the sub-factors of medical services and establishing coping strategies related to them (Her et al., 2019). Additionally, patient experience can include not only the treatment procedures that patients encounter during the treatment process, but also everything related to interactions with medical staff, and anything that a patient experiences in a medical institution can be a patient experience (Han & Kim, 2019). Patient experience is a complex social phenomenon that goes beyond simple service satisfaction and is formed by relationships within the healthcare system, opportunities for patient participation, and institutional controls (Ocloo et al., 2020). Therefore, a system-wide approach is needed to improve patient-centeredness between medical staff and patients, within organizations, and at the policy level. Previous studies have shown that positive patient experience can alleviate symptoms, increase treatment compliance, and reduce unnecessary tests, all of which positively affect patient safety (Prang et al., 2019). In addition, medical institutions with higher patient experience scores showed higher profitability, and a correlation was found between good patient experience and reduced medical errors (Betts et al., 2016). Medical institutions strive to establish systematic measures to actively involve patients in treatment to improve their experience (Bastemeijer et al., 2019). However, patients do not actively participate in patient safety because of a lack of patient safety perception. It has been emphasized that it is important for patients to perceive patient safety and participate in medical care on their own (Van der Voorden et al., 2023).
Patients’ abilities to understand health information must be supported to increase their active participation in providing medical services (Ghalenow et al., 2022). However, according to a survey of 1,002 adults in Korea 2020, only 29.1% had adequate health literacy (Choi et al., 2020). Health literacy refers to the ability to use the information necessary to manage one’s health to make appropriate decisions and take care of one’s health (Aaby et al., 2020) and acts as a major factor in patient participation in healthcare (Brabers et al., 2017). Health literacy is not merely an individual capacity but is shaped by various social determinants such as educational level, socioeconomic status, cultural background, and access to healthcare. Previous studies have shown that socially vulnerable groups tend to have lower health literacy (Choi et al., 2020), which can be a significant cause of health disparities. Individuals with low health literacy are less likely to ask questions about medical issues or seek out new information (Aboumatar et al., 2013). Therefore, health literacy is recognized as a public health issue influenced by social inequality and structural factors, necessitating systematic policies and interventions at the national level (Schillinger, 2021). On the other hand, patients with high health literacy have demonstrated higher engagement in health-promoting behaviors and self-management, leading to more active participation in disease prevention and treatment decision-making processes (Kim, 2018; Zou et al., 2024). Furthermore, health literacy plays a crucial role in enhancing patient safety during treatment and encouraging active participation in treatment decisions (Won et al., 2024). Therefore, patients need to acquire information and practice healthy lifestyle habits to improve their medical treatment effectiveness, and it is necessary to identify and improve the health literacy of inpatients.
Patient safety perception refers to the extent to which patients believe their safety is not at risk within a medical environment (Kim et al., 2018). Previous studies have shown that the higher the perception of patient safety among inpatients, the greater their willingness to participate in patient safety (Kang & Park, 2019), and that patient safety perception is positively correlated with the performance of patient safety activities (Kim & Park, 2021). Recent empirical studies have repeatedly confirmed that patient safety perception serves as a key mediating variable in the relationship between patient experience and safety behavior (Baek & Shin, 2021; Won et al., 2024). Factors such as patients’ health literacy, safety knowledge, and the hospital environment have been empirically verified to play a crucial role in interacting with patient safety perception to promote patients’ safety behavior and active participation (Baek & Kim, 2025). These results strongly suggest that expanding patient safety education, improving health literacy, and fostering a patient-centered hospital environment are essential strategies for improving the quality of patient experience and promoting active patient safety participation. Many Korean medical institutions are establishing systematic patient safety activities through a certification system, but in Small and medium-sized hospitals show significant differences from large hospitals in terms of personnel, organization, and safety culture (Park, 2019). The incidence rate of root cause analysis for patient safety incidents in large hospitals reaches 90%, while in small and medium hospitals, it is only 27% (Gu, 2016). This can be interpreted in light of South Korea’s healthcare system, where, under a competitive medical market structure, small and medium hospitals face greater difficulties than large medical institutions in securing resources and training specialized personnel. Furthermore, small and medium hospitals lack sufficient education and support necessary for patient safety activities, whereas large hospitals benefit from strengthened regulations and support following government accreditation and evaluations, enabling them to build differentiated safety management capabilities (Han & Kim, 2019; Park, 2019; Seo & Choi, 2023). Therefore, to improve patient safety in small- and medium-sized hospitals, it is necessary to form patient safety perceptions that encourage the active participation of inpatients and conduct effective patient safety education.
Previous studies have primarily conducted patient experience evaluations on inpatients at general hospitals or higher-level institutions (Her et al., 2019), while only a few have targeted inpatients at small- and medium-sized hospitals. In addition, an examination of the relationship between health literacy, patient safety perception, and patient experience revealed that inpatients’ health literacy had a positive effect on patient safety perception (Won et al., 2024), and a positive correlation between patient safety perception and patient experience has been reported (Baek & Shin, 2021). However, no studies have explicitly verified the relationship between health literacy and patient experience. A qualitative study targeting patients undergoing cardiac surgery, health literacy was found to positively affect patients’ discharge experience (Dimech et al., 2023). Health literacy can be inferred as a factor affecting patient experience. Therefore, based on previous studies, a research model was established in which health literacy affected patient experience through the mediating variable of patient safety perception.
Accordingly, this study provides the basic data necessary for developing strategies to improve patient experience and patient safety by analyzing the mediating effect of patient safety perception on the relationship between health literacy and patient experience of inpatients.
This study identifies the relationship between health literacy, patient safety perception, and patient experience among inpatients. The specific objectives of this study are as follows: First, the levels of health literacy, patient safety perception, and patient experience among inpatients were examined. Second, the mediating effect of patient safety perception on the relationship between health literacy and patient experience was analyzed.
Methods
Study Design
This descriptive research study analyzed the mediating effect of patient safety perception on the relationship between health literacy and the patient experience of inpatients.
Participants and Data Collection
The study participants were inpatients in three small- and medium-sized hospitals located in Seoul and Gyeonggi-do, and were selected through convenience sampling. The selection criteria for the participants were adults aged 19 to 65 years who fulfilled the purpose of the study, voluntarily agreed to participate, and could read and answer the questionnaire independently.
Data were collected from 300 people for analysis based on a simple mediation model. This is based on the simulation results presented by Fritz and MacKinnon (2007). If α or β among the mediating paths has a medium or higher effect size (e.g., .26–.39), a power of .80 or higher can be secured with a sample size of about 150 to 300 people. Therefore, the sample size was considered statistically sufficient to analyze the mediation effect.
Questionnaires and Measurements
Health Literacy
To measure health literacy, the Short-Form Health Literacy 12 (HLS-SF12) developed by Van Duong et al. (2017) for the general public aged 15 years or older across Asia was used, and the Korean version of the Short-Form Health Literacy Scale (HLS-SF-K12) developed by Seo et al. (2020) was used. The HLS-SF-K12 consists of a total of 12 items, consisting of 4 items on ‘health management,’ 4 items on ‘disease prevention,’ and 4 items on ‘health promotion. ’ Each item was measured on a 4-point Likert scale from ‘very difficult’ (1 point) to ‘very easy’ (4 points), with scores ranging from 12 to 48 points. A higher total score indicates a higher level of health literacy. In the study by Seo et al. (2020), the reliability of the tool was Cronbach’s α = .89, and in this study, Cronbach’s α = .86.
Patient Safety Perception
The Patient Safety Perception Scale developed by Kim et al. (2018) was used. The patient safety perception scale consists of 24 items, including 10 items on ‘safety assurance activities,’ 10 on ‘patient safety practices,’ and 4 on ‘trust in the medical system.’ Each item is measured on a 5-point Likert scale from ‘very dissatisfied’ (1 point) to ‘very much so,’ with scores ranging from 24 to 120 points. A higher total score indicated a higher level of patient safety perception. In the study by Kim et al. (2018), the reliability of the scale was Cronbach’s α = .93, and in this study, Cronbach’s α = .94.
Patient Experience
The Patient Experience Evaluation Form produced by the Health Insurance Review and Assessment Service (HIRA, 2023) measured patient experience. The Patient Experience Evaluation Form consists of a total of 19 questions, including 4 questions on ‘nurse area,’ 4 questions on ‘doctor area,’ 5 questions on ‘medication and treatment process,’ 2 questions on ‘hospital environment,’ and 4 questions on ‘patient rights protection. ’ Each question was measured on a 4-point Likert scale from ‘not at all’ (1 point) to ‘always’ (4 points), with scores ranging from 19 to 76 points. A higher total score indicates a more positive patient experience, and this scale is publicly available for use by anyone. At the time of its development, the scale demonstrated a reliability of Cronbach’s α = .88, and in this study, Cronbach’s α = .92.
Data Collection and Ethical Considerations
This study was approved by the researcher’s University Bioethics Committee (SYU IRB 2024–07–007) before data collection. The data were collected from August 20 to September 13, 2024. The researcher visited three small- and medium-sized hospitals to request cooperation for the study and, after obtaining permission from the relevant institutions, posted recruitment documents for research participants in each ward. The research participant questionnaire for data collection included the purpose of the research, the research process and method, expected risks and benefits, withdrawal of consent, etc. The ethical aspects of the participants were considered by ensuring voluntary participation. In addition, the collected data was stored in a locked locker for 3 years, used only for research purposes, and was provided with a research explanation after specifying that the data would be destroyed directly by the researcher after the research was completed. A survey was conducted after obtaining written consent from the participants who voluntarily agreed to participate in the study. The time required to complete the questionnaire was 10 to 15 min, and all participants who participated in the survey were provided with a gift.
Data Analysis
The collected data were analyzed using the IBM SPSS/WIN 25.0 program. The participants’ general characteristics were analyzed using frequencies and percentages, and their health literacy, patient safety perceptions, and patient experiences were analyzed using means and standard deviations. Correlations among health literacy, patient safety perception, and patient experience were analyzed using Pearson’s correlation coefficients. Correlations among health literacy, patient safety perception, and patient experience were analyzed using Pearson’s correlation coefficients. The mediating effect (indirect effect) of patient safety perceptions on the relationship between health literacy and patient experience was analyzed using Process macro version 4.2 (Model 4). The significance of the mediating effect was calculated using the bootstrapping method and a 95% confidence interval (CI).
Results
Demographic Characteristics of Participants
The analysis of the general characteristics of the participants revealed that there were 113 males (37.7%) and 187 females (62.3%). The average age was 37.07 (±7.34), with 144 participants (48.0%) in their 30s, 115 cases (138.3%) over 40, and 41 cases (13.7%) in their 20s. Regarding marital status, 127 patients (42.3%) were unmarried, and 173 patients (57.7%) were married. Most participants had graduated from college (256 cases, 85.3%), and the majority of participants were employed (252 cases, 84.0%). There were 208 cases (69.3%) without underlying diseases, and 229 cases (76.3%) with experience in procedure/surgery showed a high distribution. The number of hospitalizations was two for 118 cases (39.3%), three or more times for 93 cases (31.0%), and once for 89 cases (29.7%); the department of internal medicine was the most prevalent in 201 cases (67.0%). There was a high distribution of cases with experience in patient safety education, with 216 cases (72.0%).
Differences in Health Literacy, Patient Safety Perception, and Patient Experience According to General Characteristics
There was a statistically significant difference in health literacy by sex (t = −3.50, p = .001), age (F = 12.41, p < .001), marital status (t = −6.57, p < .001), education level (t = −2.81, p = .005), occupation (t = −3.23, p = .001), operation (t = −3.29, p = .001), length of stay (t = −2.51, p = .009), and patient safety education (t = −7.98, p < .001). The post-test results for age showed that health literacy scores were significantly higher in those in their 20s and 30s than those in their 40s and older (Table 1).
Differences in Health Literacy by General Characteristics (N = 300).

Note. Superscript alphabetic notation indicates the results of the post-hoc test of Scheffé’s method.
p < .01, ***p < .001.
There were statistically significant differences in patient safety perception by sex (t = −2.66, p = .008), age (F = 17.08, p < .001), marital status (t = −6.32, p < .001), education level (t = −3.16, p = .003), occupation (t = −3.71, p < .001), operation (t = −2.46, p = .015), inpatient ward (t = −2.44, p = .015), length of stay (t = −2.18, p = .031), and patient safety education (t = −9.75, p < .001). The posttest results for age showed that patient safety perception scores were significantly higher in patients in their 20s and 30s than in those in their 40s and older (Table 2).
Differences in Patient Safety Perception by General Characteristics (N = 300).
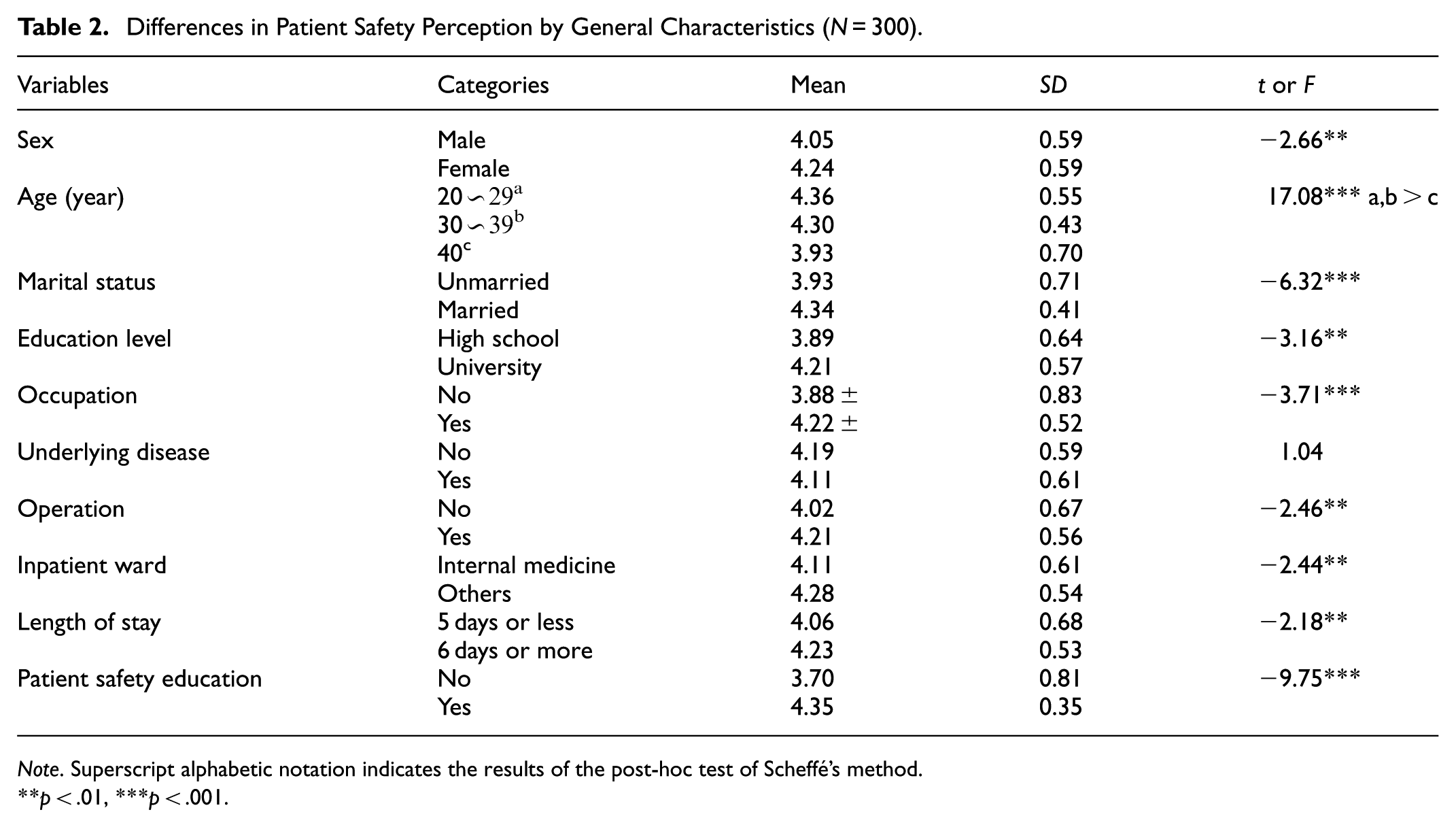
Note. Superscript alphabetic notation indicates the results of the post-hoc test of Scheffé’s method.
p < .01, ***p < .001.
There were statistically significant differences in patient experience by sex (t = −3.71, p = .001), age (F = 18.16, p < .001), marital status (t = −6.09, p < .001), education level (t = −2.98, p = .004), occupation (t = −2.99, p = .003), operation (t = −3.65, p < .001), inpatient ward (t = −3.63, p < .001), and patient safety education (t = −10.66, p < .001). The post hoc test results on age showed that patient experience scores were significantly higher in those in their 20s and 30s than in those over 40 years (Table 3).
Differences in Patient Experience by General Characteristics (N = 300).

Note. Superscript alphabetic notation indicates the results of the post-hoc test of Scheffé’s method.
p < .01, ***p < .001.
Correlation Between Health Literacy, Patient Safety Perception, and Patient Experience
The results of the correlations between participants’ health literacy, patient safety perception, and patient experience are shown in Table 4. Health literacy was significantly and positively correlated with patient safety perceptions (r = .85, p < .001). Patient experience was significantly and positively correlated with health literacy (r = .82, p < .001) and patient safety perception (r = .90, p < .001).
Correlation of Health Literacy, Patients Safety Perception and Patient Experience (N = 300).

p < .001.
The Mediating Effect of Patient Safety Perception in the Relationship Between Health Literacy and Patient Experience
The skewness and kurtosis of health literacy, patient safety perception, and patient experience were −1.67 to −1.42, and kurtosis was 1.31 to 2.64, assuming normality (Table 4). Additionally, the Durbin-Watson value was 2.07, indicating no autocorrelation and that the observations were independent. The variance inflation factor (VIF) was less than 10, indicating no problem with multicollinearity, thus satisfying the assumption of regression analysis. The mediating effect was analyzed using the PROCESS Macro program (Model 4), and among the general characteristics, sex, age, marital status, education, occupation, operation, inpatient ward, and patient safety education, which showed significant differences in patient experience, were entered as control variables. The results confirming the mediating effect of patient safety perception on the relationship between health literacy and patient experience are presented in Table 5.
Results of Mediating Effect Analysis (N = 300).

Note. PS = patient safety.
p < .001.
First, the independent variable, health literacy, was found to have a significant positive effect on the mediating variable, patient safety perception (β = .74, p < .001), and the explanatory amount of the model was 76.7% (adjusted R2 = .767, F = 106.29, p < .001). As a result of analyzing the mediating effect by inputting patient safety perception, it was confirmed that health literacy had a significant positive effect on patient experience (β = .19, p < .001), and the mediating variable, patient safety perception, also had a significant effect on patient experience (β = .65, p < .001). The final model explained 84.0% of the variance (adjusted R2 = .840, F = 152.43, p < .001). As a result of confirming the significance of the mediating effect of patient safety perception, the indirect effect was found to be statistically significant because the 95% confidence interval did not include 0 (B = 0.46, Boot SE = 0.05, 95% CI (0.36, 0.56); Table 6). Thus, patient safety perception was confirmed to mediate the relationship between health literacy and patient experience. The results of this research model are shown in Figure 1.
Significance Test of Mediating Effects of Patient Safety Perception (N = 300).
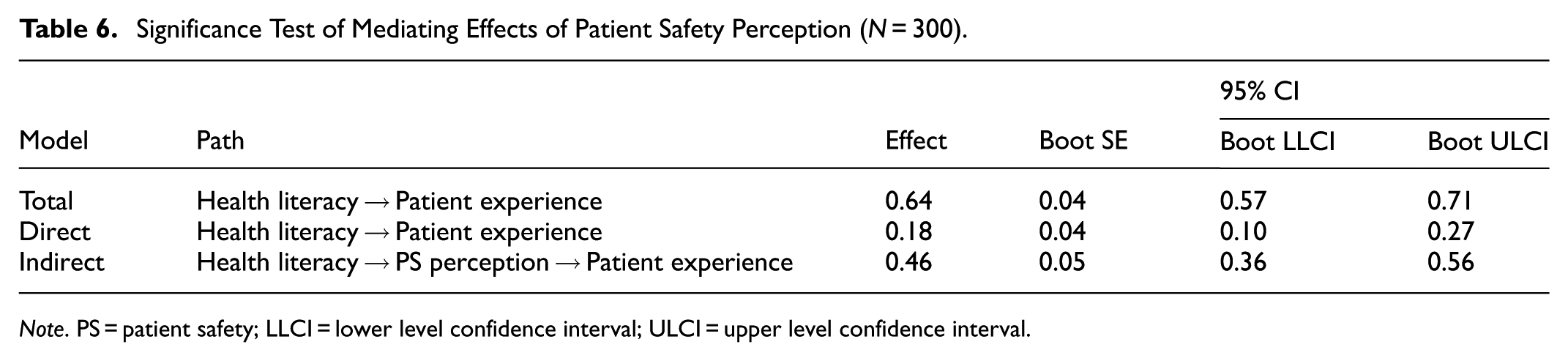
Note. PS = patient safety; LLCI = lower level confidence interval; ULCI = upper level confidence interval.

The mediation effect of patient safety perception in the relationship between health literacy and patient experience.
Discussion
The patient experience score among inpatients was 63.48 out of 76, indicating an above-average level. In a previous study, the average patient experience of inpatients with hospitals was 61.02 points (Seo & Choi, 2023), which was lower than that of inpatients with small- and medium-sized hospitals in this study. In a previous study on patient experience in small- and medium-sized hospitals, hospitals that received high evaluations for communication with medical staff and pain management had lower readmission rates (Chen et al., 2020), and the more positive patients experienced, the lower the mortality and complication rates after discharge (Dottino et al., 2019). However, a lower patient experience score was associated with an increased readmission rate (Wong et al., 2022), confirming that positively improving patient experiences is an important factor in reducing readmission rates. In a previous study, clinical quality, hospital size, and the type of medical institution were reported as significant determinants of patient experience. In other words, hospitals with a nursing grade of one were found to have higher overall patient experience scores than hospitals with a nursing grade of two or lower, more beds, and cleaner hospital environments (Seo & Choi, 2023). In another study, a higher ratio of advanced wards, more beds for integrated nursing care services, and better results in evaluating the appropriateness of long-term care benefits significantly impacted patient experience. In particular, when medical staff provided detailed explanations and showed an empathetic attitude toward patients, patients felt respected, positively affecting patient experience (Kim & Nam, 2025; Moudatsou et al., 2020). Additionally, the absence of patient-related treatment information exchange between nurses and doctors can lead to medication errors, delayed diagnosis, and unplanned treatments, all of which threaten patient safety. Furthermore, healthcare provider shortages may cause safety issues such as delayed emergency responses and increased infection rates (Gonçalves et al., 2016). Therefore, medical institutions must establish a systematic and standardized information delivery system between nurses and doctors to prevent shift work and information omissions regarding patient treatment plans. To support this, the government should implement institutional measures such as expanding the medical workforce and promoting educational programs aimed at strengthening the stability of the medical environment (Aseeri et al., 2024). Patient experience showed significant differences in sex, age, whether surgery or other procedures were performed, and patient safety experience. According to previous studies, age, education level, and health status were the major factors influencing patient experience, which is consistent with the results of this study, in which younger patients, higher education levels, and better health status reported more positive patient experiences (Guan et al., 2024) In another study, hospital type was shown to be a major factor influencing patient experience, with patient experiences in small hospitals being more positive than in general hospitals (Schiaffino et al., 2020). This is because small hospitals have shorter waiting times for treatment than general hospitals and provide a more intimate environment with medical staff, while large hospitals have abundant resources and provide specialized medical services, but their complex structure and large patient volumes often result in less positive patient experience (McFarland et al., 2017; Schiaffino et al., 2020). However, there is a paucity of research on patient experiences in small- and medium-sized hospitals. Therefore, it is necessary to compare research results and conduct in-depth research through various future studies.
The health literacy of inpatients to small- and medium-sized hospitals was found to have a significant positive effect on patient experience. Although a direct comparison is difficult due to the lack of previous studies verifying the relationship between health literacy and patient experience, it was confirmed that health literacy has a positive effect on patient experience by enabling patients to participate in appropriate decision-making by utilizing the necessary information for health management. Previous studies have also demonstrated that patients with high health literacy have higher self-management for health promotion (Kim, 2018; Zou et al., 2024) and that health literacy positively affects patient experience (Park, 2022), which supports the results of this study. Additionally, patients with high health literacy showed higher patient experience evaluations through smooth communication with medical providers and compliance with treatment plans, consistent with the results of the present study (Martin, 2019). Health literacy was 3.27 out of 4 points on average, lower than the 3.91 (±0.58) points of inpatients in general hospitals in a previous study (Jang & Park, 2023). Patients with high health literacy recognized medication information regarding the efficacy and side effects of the drugs they were taking and knew about providing drug information to the medical staff (Jang & Park, 2023). However, patients with low health literacy may not follow prescribed drug instructions because of a lack of understanding of medication information, which may threaten patient safety (Rahman et al., 2020). Groups with high health literacy have easier access to medical information through education, job stability, and social support networks, and they feel confident and proactive in communicating with healthcare providers. This organizational and relational environment promote patient engagement in medical decision-making and treatment processes, and help patients feel safer within the healthcare environment (Jang & Park, 2023). Patients who are highly educated, employed, or married demonstrate superior skills in searching, evaluating, and applying health information, as well as better information access and utilization through social interaction and support (Papi et al., 2021). Therefore, healthcare providers should offer information using simple, clear language and employ strategies such as ‘Teach back’ in order to effectively assess patients’ understanding of health information (Glick, 2019). It is also essential to select patient education materials customized to the characteristics of inpatients and systematically evaluate patients’ comprehension. However, if efforts to enhance health literacy focus excessively on individual responsibility, there is a risk of overlooking the roles of healthcare institutions and society in improving information accessibility, support systems, and the care environment. Therefore, strategies to improve health literacy must be accompanied by not only the empowerment of individual inpatients, but also organizational and social support structures and improved communication capacity among healthcare providers.
The health literacy of inpatients significantly and positively affected patient safety perception, which acted as a mediating factor in the relationship between health literacy and patient experience. In other words, it was confirmed that health literacy positively affected patient experience through patient safety perception. Thus, patient safety perception played a crucial role in mediating the effect of inpatients’ health literacy on patient experience. Previous studies have shown that health literacy among general hospital inpatients positively affects patient safety perception (Won et al., 2024), and that patient safety perception is positively correlated with patient experience (Baek & Shin, 2021), supporting the results of this study. Patient safety perception was 4.17 out of 5 points on average, lower than the 4.25 points of inpatients in general hospitals in a previous study (Kang & Park, 2019). Patient safety perception of inpatients was higher in women than in men in their 20s and 30s than in their 40s, showing differences by sex and age. A previous study targeting inpatients at general hospitals also showed differences in patient safety perceptions according to sex and age, which is consistent with the results of this study (Alsulami et al., 2022). Patient safety perception varies individually and is shaped by complex factors including disparities in communication with healthcare providers based on age and sex, individuals’ sociocultural backgrounds, health literacy, and the hospital safety culture and trust relationships. In particular, hospital safety culture, teamwork among healthcare providers, and institutional environment that encourage patient participation play significant roles in shaping patient safety perceptions. Active promotion of patient safety activities by healthcare institutions is essential to heighten patient safety perception and sensitivity (Alsulami et al., 2022; Won et al., 2024). This study found differences in patient safety perception associated with medical department, length of stay, and surgical/procedure experiences. This finding is consistent with research indicating that patients in surgical departments, such as surgery, are more exposed to safety activities, which tends to increase their safety (Kim & Nam, 2025). Patients admitted to specific departments, those with longer hospital stays, and those with surgical or procedural experience tend to have greater exposure to safety activities, correlating with enhanced patient safety perception (Kim & Nam, 2025; Vikan, 2025). Based on this finding, medical institutions should not simply provide uniform patient safety activities to all patients, but rather increase perception and sensitivity to patient safety by expanding opportunities for customized communication and participation tailored to the characteristics and needs of each patient group. Furthermore, fostering a patient safety culture that encourages inpatients to ask questions of healthcare providers and encourages their active participation in creating safe medical environment is essential.
Based on the limitations of this study, the following suggestions are made. Because this study was conducted on patients admitted to three medium-sized hospitals, there are limitations to generalizing the results. Therefore, future studies should be conducted repeatedly to ensure the sample is representative by including more medium-sized hospitals and various regions. In addition, this study may have a limited theoretical foundation because there is a lack of previous research on the relationship between health literacy and the evaluation of inpatients’ experience. Accordingly, it is necessary to ensure the validity of the structural relationships between related variables through future research. In addition, this study collected data cross-sectionally through convenience sampling; therefore, there are limitations in clearly identifying causal relationships. Consequently, longitudinal and experimental studies are recommended to apply an intervention program reflecting health literacy and to verify its effectiveness. In addition, further studies should be conducted to develop patient-customized programs aimed at enhancing health literacy and patient safety perception among inpatients and to evaluate their effectiveness.
Practical Implication
It is crucial for medical institutions to develop customized education and engagement strategies customized to hospital size and the patient’s treatment characteristics, aiming to simultaneously enhance patient-centered safety culture and improved service quality. This study reaffirmed the lack of patient experience studies targeting small and medium-sized hospitals and highlights the need for future comparative and in-depth studies encompassing a variety of medical institutions. Therefore, It is essential to develop educational tools that support health information comprehension customized to the diverse characteristics and circumstances of inpatients and to implement systematic approaches to assess their understanding. Providing customized patient safety education programs, especially targeting long-term inpatients and patients in specific departments such as surgery, is crucial for effectively enhancing patient safety perception. Furthermore, fostering open communication between healthcare providers and patients and encouraging patients’ active questioning and participation in safety contribute significantly to cultivating safety culture. These strategies are key to building a safe healthcare environment, improving patient experience, enhancing health literacy, and ultimately advancing patient safety.
Conclusion
This study confirmed the partial mediating effect of patient safety perception on the relationship between health literacy and patient experience in small- and medium-sized hospital patients in South Korea, thereby providing theoretical grounds for the relationship between major concepts. While previous studies have primarily explored the relationship between patient experience, patient safety perception, and health literacy in large or general hospitals, this study differs from previous studies in that it empirically analyzed the relationship between patient experience and patient safety perception, focusing on patients in small and medium-sized hospitals. Specifically, it empirically analyzed the impact of health literacy and patient safety perception on patient experience within the unique healthcare environment and resource constraints of small and medium-sized hospitals. This study provides a practical basis for developing customized patient safety and health information education policies for patients in small and medium-sized hospitals. Finally, in future studies, continuous attention and institutional support are needed to expand the scope of research beyond existing research centered on large hospitals to include small- and medium-sized hospitals so that patient safety research for improving the quality of medical services can be conducted more actively.
Footnotes
Ethical Considerations
Ethical approval was sought and granted from the Institutional Review Board of Sahmyook University (SYU IRB 2024-07-007).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data sharing not applicable to this article as no datasets were generated or analyzed during the current study.
