Abstract
The integration of digital technologies is transforming healthcare, with telemedicine emerging as a pivotal solution. However, its adoption remains uneven, particularly in developing countries. This study examines the factors influencing telemedicine adoption among healthcare professionals in Malaysia, with a specific focus on technology readiness and technology acceptance. The findings reveal that optimism and perceived ease of use significantly influence adoption intent, while perceived usefulness serves as a critical mediator. Additionally, age moderates these relationships, indicating that older healthcare professionals may demonstrate greater reluctance towards telemedicine adoption. By identifying the interplay between technological and demographic factors, this study provides valuable insights into the barriers and enablers of telemedicine adoption, contributing to a more targeted approach in facilitating digital healthcare integration, particularly in resource-constrained settings.
Keywords
Introduction
The expansion of telemedicine during public health crises has been extensively examined in recent research (Cavallone & Palumbo, 2020, Jimenez et al., 2020; Mishra & Sharma, 2022). Anthony (2024), for instance, applied the Technology-Organisation-Environment (TOE) framework to assess telehealth adoption during public health emergencies, identifying regulatory support and digital infrastructure readiness as key enablers. These findings reinforce the role of external environmental factors in shaping healthcare digital transformation. However, the successful implementation of telemedicine depends not only on technological progress but also on organisational readiness and structured digital transformation frameworks (Binci et al., 2022). Mishra and Sharma (2022) further highlight the importance of digital maturity and convergence models in facilitating a structured transition towards digital healthcare ecosystems. These insights underscore the necessity of proactive digital strategies to optimise remote healthcare solutions.
Telemedicine is increasingly recognised as a viable response to these challenges. Traditionally, patients seek medical advice when symptoms arise, requiring in-person visits to healthcare facilities. In contrast, telemedicine enables the remote exchange of health information and facilitates online consultations, offering greater accessibility and convenience for both healthcare professionals and patients. Despite its potential benefits—such as improved prevention, education, and treatment—telemedicine adoption remains influenced by various individual and systemic barriers. Factors such as high implementation costs and inadequate reimbursement policies contribute to resistance among healthcare professionals (Garavand et al., 2022). Meanwhile, Abushaar and Ismail (2018) observed that while doctors generally perceive telemedicine as useful, overall acceptance rates remain moderate, with concerns about workflow integration and technological proficiency acting as key impediments.
The healthcare industry is undergoing rapid digital transformation, driven by innovations in e-consultations, digital health platforms, real-time diagnostics, and artificial intelligence-driven decision support. The adoption of big data, cloud computing, the Internet of Things (IoT), and social media is reshaping healthcare operations, enabling fundamental changes in business processes and service delivery models (Matarazzo et al., 2021; Vial, 2019). These advancements enhance the efficiency of health services, improving patient outcomes while reducing operational inefficiencies (Mettler & Pinto, 2018). However, in Malaysia, the adoption of telemedicine remains relatively low despite early efforts by the Ministry of Health (MOH), which launched a national telemedicine initiative in 1997. While this IT-based innovation has the potential to enhance healthcare quality and generate cost savings, its utilisation remains limited. Given the highly specialised nature of medical expertise and the competitive nature of the healthcare sector, healthcare professionals play a critical role as both end-users and facilitators of digital health technologies.
The COVID-19 pandemic has further highlighted the relevance of telemedicine in bridging the gap between patients, doctors, and health systems. Its ability to facilitate remote consultations and chronic disease management has become increasingly apparent (Au-Yong-Oliveira et al., 2021). However, pre-pandemic legal and regulatory barriers often restricted the implementation of telemedicine, limiting its widespread adoption (Khodadad-Saryazdi, 2021). The effectiveness of telemedicine adoption is contingent on healthcare professionals’ willingness to integrate digital tools into clinical practice. Understanding their attitudes and behavioural patterns is crucial, as technology acceptance is shaped by behavioural, social, and psychological factors (Granić, 2022).
While research on telemedicine has traditionally focused on technological advancements and clinical applications, increasing attention is being given to factors influencing user adoption and acceptance. The Technology Acceptance Model (TAM; Davis et al., 1989) remains one of the most widely used frameworks for predicting technology adoption. Initially developed for workplace technology adoption, its applicability in healthcare settings—where technology use is often voluntary rather than mandated—raises important questions about its generalisability.
An important extension of TAM is the Technology Readiness and Acceptance Model (TRAM), which integrates the Technology Readiness Index (TRI) and TAM to account for both personality-driven predispositions and system-specific adoption behaviours (Lin et al., 2007). According to TRAM, technology readiness traits, such as optimism, serve as precursors to perceived usefulness (PU) and perceived ease of use (PEOU), which in turn influence adoption intent (Parasuraman, 2000; Parasuraman & Colby, 2015). This study builds upon TRAM by examining the specific roles of optimism and perceived ease of use in telemedicine adoption.
In addition to technological factors, this study investigates the moderating role of age in telemedicine adoption. Previous research suggests that age influences digital engagement, shaping perceptions of ease of use and usefulness in technology adoption (Chawla & Joshi, 2018; Porter & Donthu, 2006). Accordingly, this study categories participants into three distinct age groups to capture generational differences in technology interaction patterns. The inclusion of age as a moderating factor is supported by prior research on demographic influences in technology adoption, providing a theoretically grounded approach to understanding variations in healthcare professionals’ acceptance of telemedicine (Blut & Wang, 2020; Sergelles-Calvo et al, 2017).
By addressing these factors, this study makes both theoretical and practical contributions. Theoretically, it extends existing models of technology adoption by incorporating individual-level traits and demographic factors specific to healthcare professionals. Practically, the findings provide actionable insights for healthcare providers, policymakers, and technology developers seeking to enhance telemedicine adoption in a competitive and rapidly evolving healthcare landscape.
Literature Review and Hypothesis Development
The Technology Readiness and Acceptance Model (TRAM) serves as the foundation of this research. Within TRAM, Technology Readiness (TR) plays a crucial role in shaping individuals’ perceptions of perceived ease of use (PEOU) and perceived usefulness (PU), which subsequently influence technology acceptance and adoption (Lin et al., 2007). However, scholars have debated the precise relationship between TR and TAM constructs, particularly regarding the extent to which TR functions as a higher-order factor influencing PEOU and PU (T. Kim & Chiu, 2019).
This study extends the Technology Readiness Index (TRI) and the TAM framework by identifying specific technology readiness motivators—innovativeness (INN) and optimism (OPT)—and examining their effects on PU, PEOU, and ultimately, telemedicine adoption intent (INT). Additionally, age (AGE) is introduced as a moderating factor to assess its influence on the adoption process.
To establish key readiness factors influencing behavioural intent and perceived usefulness in telemedicine adoption, this study conducted an extensive review of the literature on technology readiness, technology acceptance, and behavioural intention. Based on TRAM theory (Lin et al., 2007), the central hypothesis asserts that technology readiness motivators positively influence telemedicine adoption, mediated by PU and PEOU. Furthermore, the study hypothesises that age negatively moderates the relationships between motivators (INN and OPT), PU, PEOU, and telemedicine adoption intent.
Technology Readiness Motivators and Telemedicine Adoption Intent
This study draws its independent variables from the Technology Readiness framework, focusing on innovativeness and optimism. Traditionally, these dimensions have been treated as independent constructs, reflecting distinct psychological processes. However, recent research suggests that their influence may vary across different contexts. Parasuraman and Colby (2015) conceptualised the Technology Readiness Index (TRI) as comprising two primary categories—motivators and inhibitors. Given the post-pandemic context, this study focuses exclusively on motivators, excluding inhibitors such as discomfort and insecurity.
Healthcare organisations navigating digital transformation face challenges related to resource constraints and evolving operational demands, particularly during crises. Amran et al. (2023) explored how social enterprises adapted to the COVID-19 pandemic, underscoring the critical role of strategic resilience and resource allocation in ensuring digital transformation success. These insights are directly applicable to telemedicine adoption, where aligning technological resources with strategic objectives is essential.
M. J. Kim et al. (2020) investigated technology readiness as a predictor of technology adoption, demonstrating that optimism and innovativeness significantly influence users’ adoption patterns across essential and emerging technologies. Similarly, Y. Wang et al. (2017) examined the impact of technology readiness in the travel industry, finding that optimism and innovativeness enhance perceived service quality and user satisfaction. These findings suggest that individuals with a strong inclination towards technological innovation are more likely to engage with digital health solutions such as telemedicine.
Building upon these perspectives, this study examines how technology readiness motivators drive telemedicine adoption within the broader context of technology acceptance.
Innovativeness and Telemedicine Adoption Intent
Innovativeness reflects an individual’s inclination to adopt and experiment with emerging technologies. Those with high innovativeness demonstrate a proactive approach to digital solutions, driven by curiosity and a belief in technology’s transformative potential (Prodanova et al., 2021). Such individuals are early adopters, embracing telemedicine as an opportunity to enhance healthcare delivery and patient engagement. Their willingness to explore untested digital solutions positions them as key facilitators in accelerating telemedicine adoption.
Optimism and Telemedicine Adoption Intent
Optimism refers to a positive disposition towards technology, characterised by the belief that digital innovations enhance efficiency, flexibility, and control (Qasem, 2021). Optimistic users tend to view new technologies as trustworthy and beneficial, fostering a greater willingness to engage with telemedicine. This outlook encourages healthcare professionals to explore telemedicine solutions, driven by expectations of improved service delivery and patient-centred care.
Technology Acceptance and Telemedicine Adoption Intent
Within the Technology Acceptance Model (TAM), both perceived usefulness (PU) and perceived ease of use (PEOU) are recognised as key determinants of behavioural intention in technology adoption (T. Kim & Chiu, 2019). Multiple meta-analyses have consistently reinforced their significant roles in influencing user adoption across diverse technological domains (Chiu & Cho, 2021).
Perceived Usefulness (PU) and Telemedicine Adoption
Perceived usefulness (PU), as defined by Davis et al. (1989), refers to the extent to which an individual believes that using a system enhances their performance. In the context of telemedicine, PU represents how users evaluate the effectiveness of telemedicine in improving healthcare access, service efficiency, and clinical outcomes. A strong perception of usefulness positively correlates with the likelihood of adoption.
Extensive research underscores PU as a primary driver of technology acceptance. When users recognise telemedicine as a tool that enhances healthcare delivery, facilitates remote consultations, and improves patient management, they are more inclined to integrate it into their professional practice. As such, clear communication of telemedicine’s tangible benefits is essential to fostering its acceptance.
Perceived Ease of Use (PEOU) and Telemedicine Adoption
Perceived ease of use (PEOU) refers to the degree to which a system is regarded as effortless to use (Kamal et al., 2020). First introduced by Davis (1986), PEOU has been widely validated as a significant factor in technology adoption. The more intuitive and user-friendly a technology is, the more likely users are to engage with it.
Research highlights that healthcare professionals require training and guidance to navigate telemedicine platforms effectively. The adoption of telemedicine is strongly influenced by how easily users can integrate it into their workflow without encountering technical difficulties (Manda & Salim, 2021). If telemedicine platforms are designed to be accessible, seamless, and require minimal additional effort, users will be more inclined to adopt them.
The relationship between PEOU and adoption intent is well-documented in TAM literature, with numerous studies affirming its impact on behavioural intention (Chiu & Cho, 2021; T. Kim & Chiu, 2019). Thus, enhancing user experience and reducing operational complexity are crucial to promoting telemedicine adoption.
Mediating Effect of Perceived Usefulness, Perceived Ease of Use
Perceived Ease of Use (PEOU) is defined as “the degree to which a prospective user expects the target system to be free of effort” (Davis et al., 1989). Perceived Usefulness (PU), on the other hand, refers to “the prospective user’s subjective probability that using a specific application system will enhance their job performance within an organisational context” (Davis et al., 1989). These two constructs are central to the Technology Acceptance Model (TAM) and are widely recognised as key determinants of technology adoption, including within telemedicine.
Innovativeness and Telemedicine Adoption via Perceived Usefulness
Innovativeness reflects an individual’s propensity to embrace and experiment with emerging technologies. Highly innovative individuals tend to be early adopters, actively exploring novel digital solutions with enthusiasm and an open-minded approach (Prodanova et al., 2021). This trait makes them particularly relevant in the context of telemedicine adoption, where early engagement with digital healthcare tools can drive broader acceptance within the medical community.
Innovative individuals are more likely to perceive telemedicine as a beneficial tool that enhances healthcare accessibility, patient engagement, and clinical efficiency. Their positive assessment of telemedicine’s utility strengthens their intention to adopt it, as they recognise its potential to improve healthcare delivery and outcomes (Prodanova et al., 2021).
Innovativeness and Telemedicine Adoption via Perceived Ease of Use
In addition, their tech-savvy disposition allows them to quickly adapt to telemedicine platforms, finding them intuitive, user-friendly, and accessible. As a result, they are more likely to perceive telemedicine as easy to use, reinforcing their intent to adopt it.
Optimism and Telemedicine Adoption via Perceived Usefulness
Optimism in technology adoption refers to a positive outlook on the benefits and transformative potential of digital solutions. Optimistic individuals tend to believe that technology enhances efficiency, flexibility, and control over daily activities (Qasem, 2021). They generally perceive new technologies as reliable and valuable, with minimal concerns about potential risks (Walczuch et al., 2007).
This positive perception of technology extends to telemedicine, where optimists are more likely to recognise its value in improving healthcare delivery, remote patient monitoring, and clinical decision-making (Qasem, 2021). As a result, optimism fosters a stronger perception of telemedicine’s usefulness, which in turn increases adoption intent.
Optimism and Telemedicine Adoption via Perceived Ease of Use
Moreover, optimistic individuals tend to be more adaptable and confident in using technology, reducing potential resistance to telemedicine adoption. Their comfort with digital tools allows them to perceive telemedicine platforms as straightforward and convenient, further reinforcing their intention to adopt them.
Moderating Effect of Individual Age
The role of demographic characteristics, particularly age, in technology adoption has been extensively studied. Some researchers conceptualise age as an antecedent within the Technology Acceptance Model (TAM), while others examine it as a moderating factor influencing key TAM constructs (Porter & Donthu, 2006).
Empirical findings suggest a negative correlation between age and technology adoption, with older individuals often demonstrating greater reluctance towards adopting new technologies (Chawla & Joshi, 2018). In this study, age is expected to moderate the relationship between innovativeness and telemedicine adoption intent. Younger individuals typically exhibit lower resistance to technological change, making them more receptive to innovations in healthcare, including telemedicine (Malaquias & Hwang, 2019). Conversely, older adults may hesitate due to unfamiliarity with digital tools (T. B. Kim & Ho, 2021). However, research indicates that age-related technology adoption gaps are narrowing, as older adults increasingly engage with digital solutions, while younger generations adopt a more discerning approach to technology use.
Similarly, age may moderate the relationship between optimism and telemedicine adoption intent. Optimism, defined as a positive attitude towards technology’s potential benefits, is often linked to greater willingness to adopt digital solutions (Qasem, 2021). Younger individuals, who generally maintain a more optimistic stance on technology, are likely to embrace telemedicine as a valuable healthcare tool. In contrast, older individuals may exhibit a more cautious outlook, influencing their willingness to adopt telemedicine. However, as digital technologies become more embedded in everyday life, generational differences in optimism towards technology are evolving.
Age may also moderate the relationship between perceived usefulness (PU) and telemedicine adoption intent. PU is widely recognised as a key driver of technology adoption (Davis et al., 1989), but age-related differences may influence its effect. Younger individuals, who are typically more accustomed to digital interactions, are likely to immediately recognise telemedicine’s advantages and exhibit a stronger intention to adopt it. Conversely, older individuals may require more substantial evidence of telemedicine’s benefits before demonstrating similar adoption intent. However, as telemedicine services expand and become more prevalent, older users may increasingly acknowledge their utility.
Finally, age could moderate the relationship between perceived ease of use (PEOU) and telemedicine adoption intent. PEOU significantly influences technology adoption (Davis et al., 1989), but its impact may vary across different age groups. Younger individuals, more familiar with digital interfaces, are likely to find telemedicine platforms intuitive, reinforcing their adoption intent. In contrast, older individuals may experience greater difficulty navigating digital healthcare tools, potentially hindering their adoption. Nonetheless, ongoing advancements in user-friendly design and digital literacy initiatives are expected to bridge these generational disparities.
We summarise the conceptual model and hypotheses in Figure 1.

Research model and hypotheses development.
Research Method
This study examines telemedicine adoption in Malaysia, a subject that has received limited academic attention within ASEAN countries. The research focuses specifically on private hospitals, addressing a critical gap in understanding telemedicine’s underutilisation in this sector. The healthcare industry plays a pivotal role in Malaysia’s economy, contributing significantly to GDP, with revenue reaching RM0.6 billion (Malaysia Department of Statistics, 2022). Given its economic importance, advancing telemedicine adoption within private healthcare settings could have substantial implications for both healthcare delivery and national growth.
The target population consists of healthcare professionals employed in private hospitals, including doctors, nurses, healthcare administrators, and other medical practitioners. While the study originally aimed to examine doctors’ perspectives, the final sample reflects a diverse range of respondents, acknowledging the multidisciplinary nature of telemedicine adoption. The sample includes physicians, surgeons, dentists, psychiatrists, paediatricians, radiologists, psychologists/counsellors, general practitioners, nurses, and administrative personnel. Since the successful implementation of telemedicine depends on collaboration across various healthcare roles, the study adopts an individual-level unit of analysis, examining how different healthcare professionals perceive and intend to use telemedicine. This broad inclusion offers a more comprehensive understanding of telemedicine adoption within Malaysia’s private healthcare sector.
Data Collection and Sampling
Data were collected through a web-based questionnaire, which was emailed directly to healthcare professionals. The data collection period spanned from January 2023 to April 2023, yielding 140 responses. To maximise participation, reminder emails were sent to non-respondents 3 days after the initial invitation. A total of 126 valid responses were retained for analysis. Notably, 14 respondents who were already using telemedicine were excluded, as the study focused on factors influencing readiness and acceptance rather than adoption among existing users.
A G*Power analysis (Cohen, 1992) was conducted to determine the minimum required sample size. For an effect size of 0.15, a significance level of .05, and a power of 0.80, the analysis indicated a requirement of 114 respondents. The final sample of 126 responses exceeds this threshold, ensuring statistical robustness.
Ensuring Sample Diversity and Representativeness
To mitigate organisation-specific bias, respondents were drawn from multiple private hospitals across various Malaysian regions, ensuring institutional diversity. Additionally, hospital size (measured by bed capacity) was included as a control variable in the PLS-SEM analysis, accounting for potential variations in organisational infrastructure and resources.
The study ensured national representativeness by incorporating respondents from diverse geographical locations, covering both urban centres (Kuala Lumpur, Selangor) and rural regions (Sabah, Sarawak, Kedah, Perak). A post hoc subgroup analysis comparing urban and rural respondents revealed no significant differences in telemedicine adoption intent. Furthermore, geographical region was incorporated as a categorical control variable, ensuring that regional factors were statistically accounted for.
Demographic Profile of Respondents
Table 1 presents the demographic breakdown of the 126 respondents. Male participants constituted 61.9%, while females accounted for 38.1%. Geographically, responses were received from across Malaysia, with the highest representation from Penang (38.10%), followed by Selangor (24.6%) and Kuala Lumpur (14.29%). Other notable contributions came from Johor (7.13%), Kedah (5.56%), Perak (4.76%), Sabah (2.38%), Sarawak (1.59%), and Malacca (1.59%).
Respondents’ Profile (Total Responses:140; Valid Responses:126).
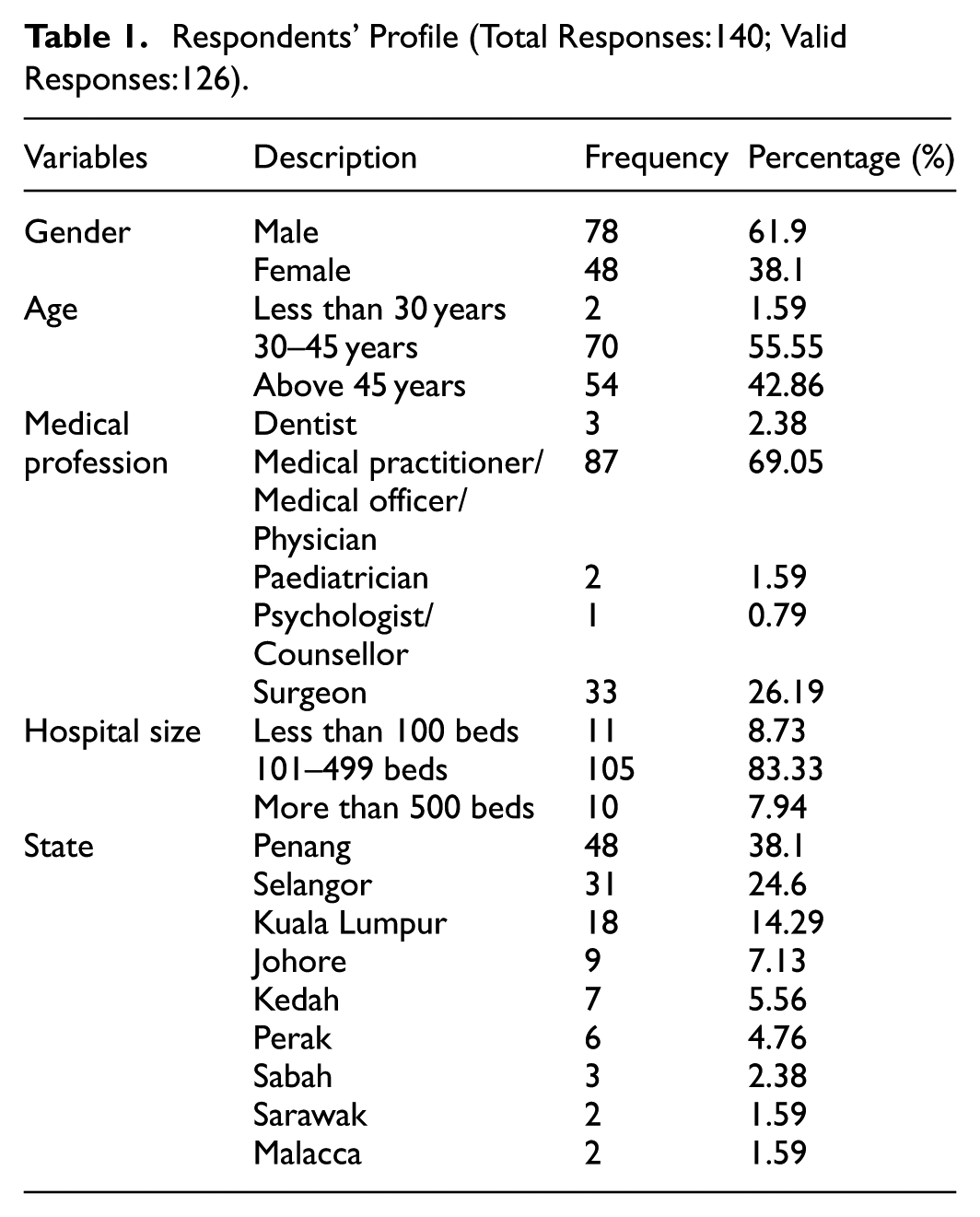
In terms of professional background, the largest group consisted of general practitioners/physicians/medical officers (69.05%), followed by surgeons (26.19%). The remaining 4.76% included three dentists, two paediatricians, and one psychologist. Regarding age distribution, 55.55% of respondents were aged 30 to 45 years, while almost 43% were above 45 years. Only two respondents (1.59%) were under 30 years old, which aligns with expectations, given the high representation of senior medical professionals, particularly surgeons (over 25% of the sample).
Measurement and Analytical Techniques
This study employed validated measurement scales to ensure reliability and validity in assessing key constructs. Telemedicine adoption intent (INT) was measured using an adapted scale from Y. Kim et al. (2017), demonstrating high internal consistency (Cronbach’s alpha = .867), surpassing the recommended threshold of 0.700 (Hair et al., 2020).
The Technology Readiness constructs—optimism (OPT) and innovativeness (INN)—were measured using scales from Parasuraman and Colby (2015), yielding Cronbach’s alpha values of .782 and .792, respectively, indicating acceptable reliability. Similarly, perceived usefulness (PU) and perceived ease of use (PEOU) were assessed using Davis et al.’s (1989) measurement items, with Cronbach’s alpha values of .954 and .913, confirming high reliability. All multi-item constructs were measured using a 5-point Likert scale, ranging from 1 (strongly disagree) to 5 (strongly agree). To examine the moderating role of age (AGE), respondents were categorised into three age groups: Group 1: Under 30 years; Group 2: 30 to 45 years; Group 3: Above 45 years. This classification enables a structured analysis of age-related differences in telemedicine adoption intent, ensuring a robust examination of demographic influences.
For data analysis, this study employed Partial Least Squares-Structural Equation Modelling (PLS-SEM), a widely used technique in social science and behavioural research. PLS-SEM is particularly suitable for complex models with multiple constructs, as it facilitates causal analysis while accommodating smaller sample sizes (Hair et al., 2014). Additionally, PLS-SEM does not require normally distributed data, making it an appropriate analytical method for this study (Hair et al., 2019). The measurement model was assessed to ensure construct validity and reliability, verifying that all indicators accurately reflected their respective constructs. These methodological choices enhance the rigour and robustness of the study, enabling meaningful insights into telemedicine adoption.
Goodness of Measurement Model
To ensure measurement validity and reliability, this study applied Partial Least Squares-Structural Equation Modelling (PLS-SEM), a recognised approach in behavioural research. The following validity tests were conducted: Convergent validity (AVE > 0.50); Discriminant validity (HTMT < 0.85); Composite reliability (CR > 0.70). These assessments followed best practices in quantitative research (Hair et al., 2020). Additionally, Variance Inflation Factor (VIF) diagnostics confirmed that multicollinearity was not a concern in the model. The survey instrument was adapted from validated measurement scales, ensuring its relevance to telemedicine adoption. To address potential common method bias (Podsakoff et al., 2012), a full collinearity test was conducted, confirming that all inner VIF values were equal to or below 5, indicating no significant bias (Hair et al., 2020).
Before evaluating the structural paths in the model, several critical tests were performed to ensure the quality of the measurement model. These included: Convergent validity assessment (Average Variance Extracted, AVE); Internal consistency reliability (Composite Reliability, CR); Discriminant validity testing. As shown in Table 2, all variables exhibited AVE scores above the recommended 0.50 threshold, consistent with Hair et al.’s (2017) criteria. The AVE values ranged from 0.672 to 0.815, demonstrating strong convergent validity. Additionally, all factor loadings exceeded the recommended threshold of 0.708, with values ranging from 0.760 to 0.945, further confirming strong content validity (Hair et al., 2017).
Reliability and Validity measures.

Composite reliability (CR) values exceeded the recommended threshold of .70, ranging from .891 to .963, reinforcing the reliability of the measurement model. These results validate the study’s measurement framework, ensuring robust statistical inferences.
Discriminant Validity Assessment
To assess discriminant validity, the Heterotrait-Monotrait Ratio (HTMT) was examined. Following Henseler et al. (2015), HTMT values should remain below 0.85 to confirm that the constructs measure distinct concepts. In this study, HTMT ratios ranged from 0.449 to 0.679, demonstrating sufficient discriminant validity (see Table 3). These results confirm that each construct effectively captures a unique dimension of telemedicine adoption, reinforcing the validity of the measurement model.
Heterotrait-Monotrait Ratio (HTMT).

Note. Threshold value <0.85 (Henseler et al., 2015).
Structural Model Assessment
Following confirmation of reliability and validity, the structural model was examined to determine the significance and relevance of the path coefficients in PLS-SEM. To ensure statistical robustness and minimise Type I errors, hypothesis testing adhered to a stringent threefold acceptance criterion: (a) t-statistic: >1.65 (one-tailed test) and >1.96 (two-tailed test); (b) confidence interval (LL/UL): must exclude zero; (c) p-value: <.05. A hypothesis was accepted only if all three conditions were met, ensuring that the findings were statistically sound and minimised the risk of false positives. Additionally, to enhance interpretive depth, the study applied significance levels of: p < .05 (*); p < .01 ()**; p < .001 (*)**. These thresholds followed the standard criteria outlined by Hair et al. (2017). The statistical tests included: (a) t-statistics for one-tailed (t > 1.65) and two-tailed (t > 1.96) tests; (b) bootstrap confidence intervals (CIs) excluding zero.
To further reinforce statistical validity, bootstrapping with 5,000 resamples was applied, a widely recommended method in PLS-SEM (Hair et al., 2017). This approach enhances the stability of parameter estimates, ensuring that hypothesis testing remains robust despite sample size limitations. These methodological choices strengthen the rigour of statistical inferences, ensuring that the findings reliably capture the relationships between telemedicine adoption drivers.
Results
The study findings provide a clear distinction between significant and non-significant relationships among the tested hypotheses. Table 4 summarises the results, highlighting that optimism (OPT) and perceived usefulness (PU) positively influence adoption intent (INT), supporting H2 and H4. In contrast, innovativeness (INN) and perceived ease of use (PEOU) were not significant predictors, leading to the rejection of H1 and H3. Additionally, PU mediates the relationship between OPT and INT, confirming H6a, whereas other mediation effects were non-significant. Age (AGE) was found to moderate the relationship between PU and INT (supporting H7c) but did not significantly influence other hypothesised moderating effects (H7a, H7b, H7d). These results underscore the critical role of perceived usefulness in telemedicine adoption and suggest that optimism fosters adoption intent primarily through its influence on perceived usefulness.
Path Coefficient Testing.
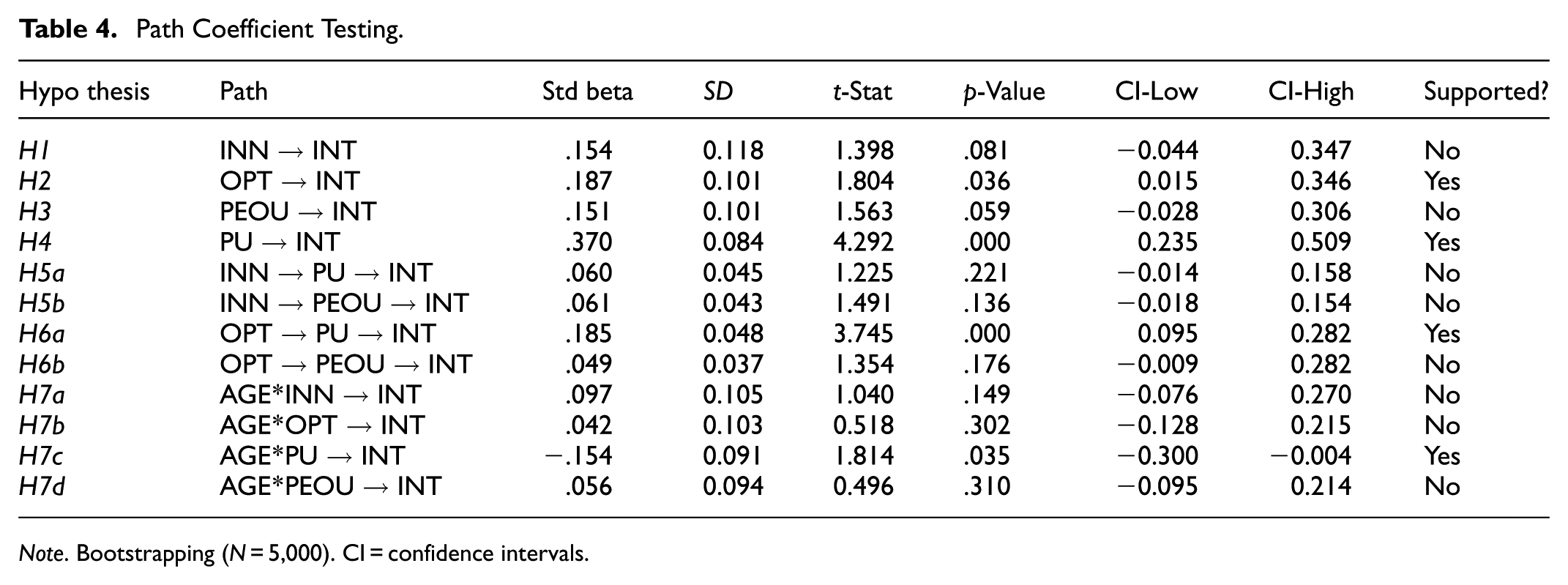
Note. Bootstrapping (N = 5,000). CI = confidence intervals.
Predictive Strength of the Model
The model’s predictive capability was evaluated using the coefficient of determination (R2). The R2 value for Telemedicine Adoption Intent (INT) was 0.505 (50.5%), indicating that the predictors account for a substantial proportion of the variance in INT, exceeding the 26% threshold recommended by Cohen (1992). This result highlights the model’s strong explanatory power in predicting telemedicine adoption intent. Figure 2 depicts the summary findings of the structural model.

Summary of structural model findings.
Discussion
The study’s findings provide key insights into the factors influencing telemedicine adoption within private healthcare settings in Malaysia. The results highlight the importance of optimism and perceived usefulness as primary drivers of adoption intent, while innovativeness and perceived ease of use were not significant predictors. These findings suggest that healthcare professionals are more likely to adopt telemedicine when they perceive it as beneficial rather than simply easy to use.
The impact of technology readiness motivators on telemedicine adoption produced mixed results. Optimism significantly influenced telemedicine adoption (H2 supported), whereas innovativeness did not (H1 rejected). This finding can be explained by the differing nature of these traits. Optimism fosters a positive perception of telemedicine’s benefits, making individuals more receptive to its adoption. In contrast, innovativeness, which is often associated with risk-taking and experimentation, does not necessarily lead to a stronger intention to adopt telemedicine. This suggests that while being innovative may drive early exploration of technology, it does not guarantee a positive perception of telemedicine’s benefits in a healthcare setting.
The role of perceived usefulness (PU) and perceived ease of use (PEOU) also yielded notable findings. PU significantly influenced adoption intent (H4 supported), while PEOU did not (H3 rejected). This deviates from the traditional Technology Acceptance Model (TAM), where PEOU is typically expected to enhance adoption intent. One possible explanation is that post-pandemic regulatory changes, evolving patient expectations, and the urgency of telemedicine implementation may have shifted healthcare professionals’ priorities. In this context, ease of use may be less critical than the perceived benefits telemedicine offers in improving healthcare access, efficiency, and patient outcomes.
The study also examined the indirect effects of innovativeness and optimism through perceived usefulness and perceived ease of use. The results indicate that innovative individuals did not perceive telemedicine as particularly useful or easy to use (H5a, H5b rejected). This reinforces the idea that innovation alone does not translate into a strong intention to adopt telemedicine unless clear benefits are recognised. However, optimism had a significant indirect effect through perceived usefulness (H6a supported), though not through perceived ease of use (H6b rejected). This suggests that optimistic individuals are more likely to acknowledge the benefits of telemedicine, yet their positive outlook does not necessarily make them perceive telemedicine as easier to use.
The moderating effect of age also produced interesting findings. Age negatively moderated the relationship between perceived usefulness and adoption intent (H7c supported), suggesting that older healthcare professionals are more critical when assessing telemedicine’s usefulness. This aligns with prior research indicating that more experienced practitioners may be sceptical of new technologies and require stronger evidence of their value before adoption. However, age did not significantly moderate the relationships involving innovativeness, optimism, or perceived ease of use (H7a, H7b, H7d rejected). This suggests that age does not significantly alter an individual’s predisposition towards innovation, optimism, or perceived ease of use, but it does affect how they evaluate the practical benefits of telemedicine.
Overall, these findings contribute to the growing body of research on telemedicine adoption by providing empirical evidence on the role of technology readiness, technology acceptance, and demographic factors. The study highlights the importance of fostering a positive perception of telemedicine’s benefits rather than focusing solely on ease of use. Moreover, the findings suggest that targeted strategies should be implemented to address the concerns of older healthcare professionals, ensuring that telemedicine’s value is effectively communicated to encourage widespread adoption.
Conclusion
This study provides valuable insights into the key determinants of telemedicine adoption, particularly in the Malaysian private healthcare sector. The findings reinforce the importance of optimism and perceived usefulness, while also challenging conventional assumptions about the roles of innovativeness and perceived ease of use. The moderating effect of age further suggests that older healthcare professionals may require additional reassurance regarding telemedicine’s benefits before adopting it into their practice.
These findings have significant implications for healthcare providers, policymakers, and technology developers. To drive higher telemedicine adoption, stakeholders should prioritise demonstrating its tangible benefits while addressing age-related differences in technology perception. Future research could explore longitudinal trends in telemedicine adoption, assessing how evolving digital healthcare policies and technological advancements influence adoption patterns over time.
Theoretical Implications
This study, grounded in the Technology Readiness and Acceptance Model (TRAM), addresses the limited research on telemedicine adoption compared to other technological domains. Its significance lies in its novel integration of technology readiness, technology acceptance, and socio-demographic factors within a single research framework. By incorporating elements from both Technology Readiness (TR) Theory and Technology Acceptance Model (TAM) Theory, TRAM provides a comprehensive framework for understanding individuals’ intentions to use telemedicine.
A key contribution of this study is its inclusion of age as a moderating factor, which enhances the understanding of cognitive evaluations and decision-making processes specific to telemedicine adoption. Recognising the influence of socio-demographic factors on technology adoption is essential, as perceptions of telemedicine vary across different age groups and professional backgrounds. This study underscores the importance of contextualising telemedicine adoption within a broader socio-technological landscape, offering valuable theoretical insights that extend beyond traditional TAM applications.
Practical Implications
This study provides valuable insights for both healthcare practitioners and researchers, particularly in understanding the interplay between user characteristics, technological factors, and telemedicine adoption intent. By focusing on healthcare professionals’ perspectives, the study offers practical guidance for hospitals and policymakers evaluating the challenges and benefits of telemedicine integration.
A key takeaway is the need to address barriers associated with doctors’ reluctance to adopt telemedicine, including fears of workflow disruption and technological unfamiliarity (Tabaeeian et al., 2022). Targeted training programmes, aligned with medical industry standards, can help mitigate resistance by equipping healthcare professionals with clear operational guidelines for telemedicine use. Digitalisation offers opportunities for virtual skill enhancement through personalised and group training modules, thereby increasing confidence and competency in telemedicine applications.
Furthermore, certification programmes focusing on telemedicine service provision, legal-ethical considerations, and data security compliance could incentivise adoption while ensuring adherence to data protection regulations (Pool et al., 2022). Policymakers must prioritise investments in digital infrastructure, as technological accessibility remains a significant barrier to telemedicine expansion. In addition, AI-driven healthcare models present opportunities to enhance telemedicine platforms by integrating machine learning and predictive analytics, improving patient engagement and clinical decision-making. Future policy initiatives should focus not only on expanding telemedicine access but also on incorporating intelligent automation to enhance its long-term effectiveness.
Limitations and Future Research
This study presents an exploratory investigation of telemedicine adoption among healthcare professionals across multiple regions in Malaysia. While the findings offer valuable insights, they should be interpreted within the study’s methodological constraints, as the sample representation may not fully reflect national-level adoption trends. Future research should aim for broader, more representative sampling to strengthen external validity.
Despite achieving a 28% response rate, which aligns with expectations for studies involving healthcare professionals with demanding schedules, the sample size remains a potential limitation. To improve generalisation, future research should include larger and more diverse samples, particularly incorporating healthcare professionals from public and rural healthcare settings. This is especially relevant given that public healthcare providers face distinct challenges, such as higher patient volumes and resource constraints, which may shape telemedicine adoption differently from experiences in the private sector.
Another limitation is the study’s focus on private healthcare professionals, which may introduce self-selection bias, as respondents more open to telemedicine adoption may have been more inclined to participate. Expanding future research to include public sector healthcare workers would offer a broader perspective on telemedicine challenges and opportunities, particularly in regions where healthcare accessibility and patient congestion are pressing concerns.
Additionally, the study does not explicitly account for prior professional development and telemedicine-related training, which could influence technology adoption behaviour. Future research should consider training exposure as a moderating or control variable to better understand how prior education shapes telemedicine adoption intent. Furthermore, this study primarily involved medical disciplines requiring in-person physical examinations, potentially underrepresenting fields where telemedicine is better suited, such as radiology and mental health services. To gain a more comprehensive understanding of telemedicine adoption, future studies should incorporate a wider range of medical disciplines.
Beyond the scope of technology acceptance, organisational factors such as corporate social responsibility (CSR) strategies may play a role in digital transformation and telemedicine adoption. Research by Cheah & Lim (2024) suggests that CSR initiatives enhance job satisfaction and organisational resilience, indicating that healthcare providers should integrate employee-driven CSR policies to support telemedicine implementation. Additionally, sustainability is an emerging priority in digital healthcare transformation. Cheah et al. (2024) highlight green innovation as a strategic driver of sustainable business performance, underscoring the importance of environmentally responsible telehealth solutions that balance technological advancements with sustainability goals. Future research should explore how sustainability-driven healthcare policies influence the adoption and long-term viability of telemedicine platforms.
Footnotes
Ethical Considerations
Ethical review and approval were not required for this study in accordance with institutional and national requirements.
Consent to Participate
Participants were informed about the purpose of the study and provided consent prior to participation.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported the External Grant Universiti Sains Malaysia, through a funding provided by TM Technology Services Sdn. Bhd. (Formerly Known as Webe Digital Sdn. Bhd.), USM Account Grant Number: 304/PPAMC/6501218/W110 and Universitas Airlangga for International Research Consortium Grant Number: 185/UN3.LPPM/PT.01.03/2024.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data will be provided upon reasonable request to the corresponding author.
