Abstract
Primary health care (PHC) holds great potentials to improve maternal, newborn, and child health (MNCH) outcomes. However, there has been limited documentation of its effects on increasing universal access to maternal, newborn, and child health services in sub-Saharan Africa. Also, not adequately known are the most effective interventions to improve the delivery of PHC services in the region. The objective of this study was to conduct a systematic review of empirical evidence of interventions that improved access and quality of PHC services for maternal, newborn, and child health in sub-Saharan Africa. The protocol was registered on Prospero (Registration number CRD42019126029). Using terms related to primary health care and MNCH, we searched African Journals Online (AJOL), PubMed/Medline, Popline, ScienceDirect, Google Scholar, WHO Repository (IRIS), Directory of Open Access Journals (DOAJ), Cochrane Library, and reference lists for studies published in English between 2000 and 2019. Studies were included in the search if they reported interventions, and strategies implemented to improve quality and access to primary health care for maternal, newborn, and child health in sub-Saharan Africa. A total of 25 studies were included in the review. Effective interventions included financial incentives, task-shifting, community-directed engagements, training of providers, mobile health, cost-sharing, and supportive supervision among others. The result of this review contributes useful insight to guide the reformation, and development of new policies and programs for improving access and quality of primary health care delivery in sub-Saharan Africa, particularly to improve maternal and child health in the region. However, strategies to scale and sustain the successes need to be in place.
Keywords
Introduction
The high rate of maternal, neonatal, and child mortality continues to be a major public health concern in many sub-Saharan African countries (Kinney et al., 2010; World Health Organization, 2010). For instance, the highest estimated maternal mortality ratio (MMR) worldwide is in Sierra Leone (1,360/100,000 live births), and 18 other countries in sub-Saharan Africa are estimated to have very high MMR ranging from 500 to 999 per 100,000 live births (World Health Organization, 2015). Weak health systems made worse by conflicts, disasters, and forced displacement among other factors in the region increase exposure to the risk of death for mothers and children. Many of these deaths occur in hard-to-reach and underserved rural communities in the region, especially among illiterate and poorly educated women (Black et al., 2003; World Health Organization, 2016). It is increasingly evident that poor access to quality health care by socially disadvantaged women is at the root of the high rate of maternal and child mortality in many parts of sub-Saharan Africa. Evidence from Demographic and Health Surveys in sub-Saharan African countries suggests that a high proportion of pregnant women who have no formal education and those with only primary-level education deliver with unskilled traditional birth attendants rather than with skilled attendants in the formal health system, exposing them to higher risks of maternal and neonatal morbidity and mortality (ICF International, 2015).
To address this, the World Health Organization has recommended Primary Health Care (PHC) as capable of increasing women’s access to the level of care needed to attend to the majority of the minor conditions that lead to avoidable maternal, newborn, and child morbidity and mortality (World Health Organization, 1978). Primary health care is a form of accessible, affordable, and effective health care that enables citizens to enter the formal health system to receive evidence-based promotive, preventive and curative care necessary to avert morbidity and mortality. It includes, at least, the education of women on prevailing health problems and the methods of preventing and controlling them, promotion of food supply and proper nutrition, an adequate supply of safe water and basic sanitation, maternal and child health care including family planning, immunization against the major infectious diseases, prevention and control of locally endemic diseases, appropriate treatment of common diseases and injuries, and the provision of essential drugs. Consequently, most countries in sub-Saharan Africa have adopted PHC as the foundation of their health care systems in efforts to reach the most vulnerable persons (World Health Organization, 2008). A country like Ethiopia has made impressive progress in providing primary health care across the country, particularly to rural communities through an elaborate health extension program with a notable impact on maternal and child health (African Union, 2013; Memirie et al., 2016). In the Gambia, Hill et al. (2000) documented evidence of a significant decline in childhood mortality in communities with a primary health care facility compared to communities without a PHC in the 1980s. However, the gain in childhood mortality in the Gambia waned when PHC program began to receive reduced governmental support after 1994. Nigeria recently revitalized its PHC approach by recommending the creation of Primary Health Care Development Agencies in its 36 States and identifying nine indicators to measure their successful performances (Federal Government of Nigeria, 2013; National Primary Health Care Development Agency, 2012). The policy referred to as “Primary Health Care Under One Roof (PHCUOR),” if well implemented promises to strongly position PHC for effective delivery of maternal and child health care to under-served communities in Nigeria.
However, despite the promise of PHC, there has been limited documentation of its effectiveness in improving maternal, newborn, and child health in sub-Saharan Africa, a region with the highest burden of maternal and child mortality and morbidity. Also, not adequately known are the best approaches for developing and implementing policies on PHC to enable them to respond to the health needs of women and children. However, a few systematic reviews have been conducted on best practices in effective PHC delivery in sub-Saharan Africa but they are limited in focus. For instance, Christopher et al. (2011) reviewed studies on the effectiveness of Community Health Workers in sub-Saharan Africa. Their study was limited in its coverage, focusing only on child health and three countries in the region (Gambia, Ghana, and Benin).
Therefore, through a review of the existing literature, we specifically focused on how effective primary health care has been positioned using different interventions to improve maternal, newborn, and child health care, including family planning and the prevention of related morbidity and mortality in sub-Saharan Africa. We solicited information on community, outreach, and facility-based interventions, strategies, and approaches that have been applied to improve access and quality of services for MNCH at the primary health care level. We believe this review of existing studies will be useful for developing policies and programs for improving the quality of delivery of primary maternal and child health services in the region.
Methods
Search Strategy
The Preferred Reporting Items for Systematic Review and Meta-Analysis (PRISMA) statement was followed in conducting this review and the protocol was registered on Prospero (Registration number CRD42019126029). PRISMA is a set of minimum items for reporting systematic review and meta-analysis. Its focus is primarily on reporting reviews of randomized control trials; however, it is also used to report reviews of other types of research particularly those that involve the assessment of interventions. The literature search targeted peer-reviewed and published journal articles. We searched bibliographic databases including African Journals Online (AJOL), PubMed/Medline, Popline, ScienceDirect, Google Scholar, WHO Repository (IRIS), Directory of Open Access Journals (DOAJ), and Cochrane Library. Also, searched were reference lists of relevant systematic reviews and other articles. Keywords used in the systematic search of the literature included keywords drawn from the WHO recommended interventions for pregnancy, childbirth, postpartum, newborn, infant and child care, and family planning at the community and first-level facility (World Health Organization, 2010). Also included were synonyms and Medical Subject Headings (MeSH) of each database (Medline/PubMed).
Inclusion Criteria
The evidence for this review was drawn from intervention studies that were PHC facility-based, community-based, and related to the functions of a PHC, with outcomes designed to improve quality and access to PHC services for maternal, newborn, and child health care. Quality of service was defined in terms of improvement in self-reported or otherwise tested competence of providers in providing PHC functions for MNCH. Access was defined as improvement in the utilization of PHC facility, community, and outreach services by women for MNCH. Studies were included if they used quantitative design, were written in English, conducted in sub-Saharan Africa between 2000 and 2019, and published in a peer-reviewed journal. The review period was limited to 2000 and 2019 to assess the progress made in sub-Saharan Africa in achieving health for all through primary health care before the Alma Ata deadline in 2000 and efforts made toward the attainment of the Millennium Development Goals. The search using the various terms generated 2,055 articles (Figure 1). After removing duplicates, 119 potentially relevant articles were retrieved for full-text review, and 25 met our inclusion criteria. Articles were retrieved and screened by two authors (LFCN and SA).

Flow diagram of study selection according to PRISMA flow chart.
Data Extraction, Synthesis, and Analysis
Using a data extraction form we extracted the following information from each study: authors, date of publication, setting, data source, research design, intervention/strategy implemented, follow-up period, desired outcome measured, and major findings. The information extracted from the studies was qualitatively analyzed and organized into thematic areas on types of interventions or strategies for improved quality of care and utilization of primary health care services. Improvement in quality and access to PHC for MNCH care was our primary outcome of interest. Thus, interventions, strategies, and approaches were assessed to be effective if the reported outcome was statistically significant, resulted in quantified or self-reported improvement in the quality of care provided and in the utilization of services for MNCH care.
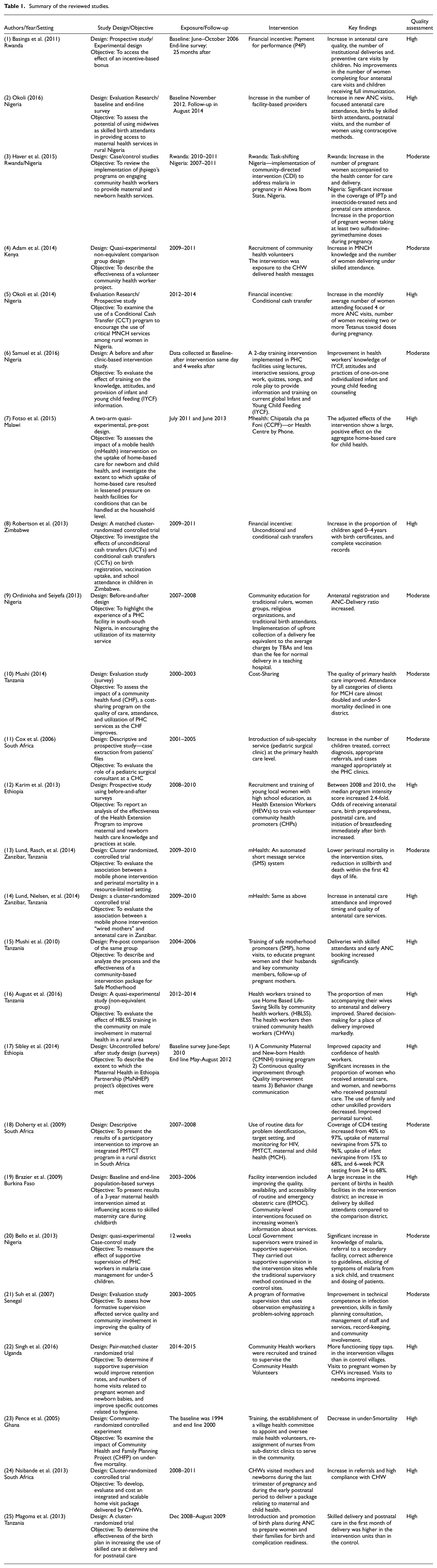
An assessment of the quality of evidence was conducted using the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) approach (Atkins et al., 2004; Guyatt et al., 2008). The quality of evidence was classified into high, moderate, and low. In the GRADE approach, high quality means that further research is very unlikely to change the confidence in the estimate of effect; moderate quality indicates further research is likely to have an important impact on our confidence in the estimate of effect and may change the estimate. Low quality entails further research is very likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate. Studies were ranked on a scale of 3-1 (3 = high quality, 2 = moderate quality, and 1 is low quality) on eight criteria: Study design, an adequate description of the intervention, an adequate description of the outcome measures before and after the intervention, the period between the intervention and outcome more than 1 year, the analysis involved inferential statistics and control of potential confounders, the results are clearly reported, reported positive results, and limitations/biases reported. The highest obtainable score was 24. The cumulative quality score of each study was converted to a percentage. Scores ≥70% were classified as high quality (3), moderate quality score was from 50% to <70% (2), and low-quality score was <50% (1). For the study design, randomized control trials were rated as high quality except where there were inconsistencies in the results, and reporting bias, case-control studies, pre-post or before and after without control were rated moderate; cross-sectional and descriptive studies were rated low. The summary of the reviewed literature is presented in Table 1.
Summary of the reviewed studies.
Results
The included studies differed in terms of study design, method of data collection, type of data collected, and analytical strategies. Thus, the articles were grouped according to similar interventions for narrative synthesis.
Characteristics of the Included Studies
The included articles are relatively a good representation of studies across sub-Saharan Africa as the studies covered all the regions except Central Africa. Studies from Eastern Africa were the highest (n = 12): Tanzania (August et al., 2016; Lund, Nielsen et al., 2014; Lund, Rasch et al., 2014; Magoma et al., 2013; Mushi, 2014; Mushi et al., 2010), Rwanda (Basinga et al., 2011; Haver et al., 2015), Ethiopia (Karim et al., 2013; Sibley et al., 2014), Kenya (Adam et al., 2014), and Uganda (Singh et al., 2016). There were five studies from Southern Africa: South Africa (Cox et al., 2006; Doherty et al., 2009; Nsibande et al., 2013), Malawi (Fotso et al., 2015), and Zimbabwe (Robertson et al., 2013). Studies conducted in Western Africa were 9: Nigeria (Bello et al., 2013; Haver et al., 2015; Okoli, 2016; Okoli et al., 2014; Ordinioha & Seiyefa, 2013; Samuel et al., 2016), Burkina Faso (Brazier et al., 2009), Senegal (Suh et al., 2007), and Ghana (Pence et al., 2005). No study that met the inclusion criteria was found for 2017 to 2019. The majority of the studies used quasi-experimental designs (n = 16); seven studies were cluster/community randomized trials, and three were prospective studies that engaged descriptive and mixed methods. The subject in the three studies was financial incentives in the form of results-based payments, conditional and unconditional cash transfers. One study evaluated the effect of increasing the number of facility-based providers; another study evaluated task-shifting. Community-directed interventions were the subject of 10 studies, and in some cases, the community-based interventions were implemented with improvements in facility-based activities. In three studies, interventions were focused on upgrading the skills of facility-based providers but in one of the three studies, a community-based intervention was also implemented alongside providers’ training. Other themes were mobile health (n = 3), cost-sharing (n = 1), introduction of a sub-specialty (n = 1) and supportive supervision (n = 3). Assessment of the quality of evidence showed that 15 studies were of high quality (≥70%), particularly the randomized control trials, 11 were assessed moderate in quality of evidence and none was of low quality.
Interventions and Their Effect on Maternal, New-born and Child Health
Included in this review were studies that examined facility and community-based interventions and strategies implemented to improve the quality of care and utilization of primary health care services for maternal, newborn, and child health in sub-Saharan Africa. The results are presented qualitatively using themes that describe the types of intervention. The interventions and strategies and their outcomes were described under each theme.
Financial intervention
Financial incentives in the forms of payment for performance and conditional and unconditional cash transfers to households and women increased the quality of care and access to primary health care facilities for MNCH preventive and curative services, albeit, there were variations across the different outcome indicators. For instance, in a prospective study conducted by Basinga et al. (2011) the potential of payment for performance scheme to increase the use and quality of MNCH services was assessed using antenatal care visits and institutional deliveries, quality of antenatal care, and child preventive care visits and immunization as outcome measures. Facilities in the intervention group experienced a 23% increase in the number of institutional deliveries and 56% increase in the number of preventive care visits by children aged 23 months or younger and a 132% rise in visits for children aged between 24and 59 months (132%) and a significant increase in antenatal care quality (0.157 standard deviations -95% CI 0.026–0.289). Although antenatal quality reportedly increased, there was no improvement in the number of women who completed four or more antenatal visits and the number of children who received full immunization. In Zimbabwe (Robertson et al., 2013), conditional cash transfer (CCT) and unconditional cash transfer (UCT) was associated with better outcome in the intervention sites than in the control clusters where no cash transfer was implemented. Compared with the control group, the number of children aged 0 to 4 with birth certificates increased by 16.4% (95% CI 7.8–25.0) in the CCT group and 1.5% (95% CI -7.1–10.1) in the UCT group, but the difference was only significant in the CCT group. For complete vaccination of children aged 0 to 4, there was an increase of 3.1% in the UCT group and 1.8% in the CCT group but there was no difference with the control group. Similar to Zimbabwe, conditional cash transfer intervention in a pilot study conducted in 37 PHC facilities in 9 Nigerian States improved maternal health. Compared to the control sites, CCT was associated with a statistically significant increase in the monthly average number of women who completed four or more antenatal care visits by 15.11 visits per 100,000 catchment population (95% CI: 7.38–22.85), and the number of women receiving two or more tetanus toxoid doses during pregnancy by 21.66 cases per 100,000 catchment population (95% CI: 9.23–34.08) (Okoli, 2016).
Cost-sharing in the form of a Community Health Fund (CHF) was another form of a financial intervention. Mushi (2014) assessed the impact in Tanzania on the quality of care, attendance, and utilization of PHC services as the CHF improves. The program presented two options for paying medical bills to households—over-the-counter cash payment on receipt of services or pre-payment through the CHF. Under the CHF, participating households pay a fixed amount per year to cover their medical expenses in public PHC facilities within the district. All the revenues are kept in a common district account that is managed by the District Medical Officer. The government increased the regular inflow of medical supplies to PHC facilities. With increased regular supply, revenue from the CHF was used mainly for minor renovations, extensions of health facility premises, and occasional purchase of medical supplies when there is a shortage. The program resulted in improvement in the quality of primary health care services, attendance by all categories of clients for MCH care almost doubled by the year 2005, and under-5 mortality declined in one district.
Human resource intervention
One of the challenges of the effective functioning of PHC in sub-Saharan Africa is the dearth of skilled health providers. Interventions addressing this barrier revolved around increasing the number of nurses/midwives, community health workers (CHWs), task shifting, and recruitment of community health volunteers with or without the assistance and involvement of the target communities (Adam et al., 2014; Haver et al., 2015; Karim et al., 2013; Mushi et al., 2010; Okoli, 2016). The volunteers are trained in diverse target components of MNCH for outreach to individuals, families, households, small groups, and communities. In a few settings they received a stipend, and in many cases, they were not given any stipends. In Kenya, the volunteers were trained to deliver reproductive health messages one-on-one and with small groups, and they received no stipends. The effect of the human resource intervention in Kenya was a significant increase in knowledge of maternal and child health and facility delivery for women who were exposed to the health message (Adam et al., 2014). In a Nigerian study (Okoli, 2016), recruitment of more midwives between 2012 and 2014 reportedly resulted in a 42% increase in new antenatal care visits, 56% in skilled birth attendance, 33% in postnatal visits, and 66% in the use of contraceptives. The recruitment of young local women as Health Extension Workers and the “model family” strategy in Ethiopia (Karim et al., 2013) was associated with increased program intensity which increased the odds of antenatal care (OR 1.13 CI: 1.03–1.23), receiving iron supplement (OR 1.14 CI: 1.02–1.26), receiving at least 2 Tetanus Toxoid injections (OR 1.09 CI: 1.00–1.18), birth preparedness (OR 1.31 CI: 1.19–1.44), postnatal care (OR 1.60 CI 1.34–1.91) and initiation of breastfeeding immediately after birth (OR 1.10 CI: 1.02–1.20), knowledge of danger sign during childbirth (β = .06 CI: 0.02–0.10), postnatal period (β = .04 CI: 0.00–0.07) and neonatal danger sign (β = .04 CI: 0.00–0.07). In Tanzania (Mushi et al., 2010), the use of safe motherhood promoters (men and women) who were married, literate, and accepted by the community resulted in a significant improvement in skilled deliveries (34%–51.4% p < .05), early booking for antenatal care (18%−56.9% p < .01) and four or more antenatal care visits (42.2%−51.3%) for primigravid mothers. Increasing the number of professionally trained providers in a PHC facility as in the Nigerian study or trained volunteers as in Kenya, Ethiopia, and Tanzania who provide community-based PHC services is germane for improved quality and access to PHC services for MNCH.
Another component of human resource intervention was capacity-building through training and retraining of providers. In a community-directed intervention in Nigeria (Haver et al., 2015), PHC staff were trained on malaria and malaria in pregnancy and they reached out to community leaders and volunteers. The program significantly increased the coverage of intermittent preventive treatment (IPTp) and insecticide-treated nets and prenatal care attendance in the intervention communities compared to the control communities. The proportion of pregnant women taking at least two sulfadoxine-pyrimethamine doses during pregnancy was five times in the experiment communities compared with three times in the control group (p < .001). In another Nigerian study, 2-day training in 10 PHCs on child feeding resulted in improved health providers’ knowledge, attitude, and practices of one-on-one individualized infant and young child feeding counseling in line with global Infant and Young Child Feeding recommendations (Samuel et al., 2016). A capacity building intervention in KwaZulu-Natal, South Africa (Doherty et al., 2009) with a focus on using routine data for problem identification, target setting, and monitoring for HIV, PMTCT, maternal and child health (MCH) increased the coverage of CD4 testing from 40% to 97%; uptake of maternal nevirapine increased from 57% to 96%; uptake of infant nevirapine increased from 15% to 68%; while 6 weeks PCR testing increased from 24% to 68%.
Noteworthy is that although the human resource interventions were primarily aimed to improve maternal and newborn health, the capacity of the providers (professionals and volunteers) is also built as an intended or unintended consequence. For instance, in Ethiopia, a home-visit package reportedly improved the capacity and confidence of the home-visit team of Health Extension Workers, Community Health Development Agents, and Traditional Births Attendants to provide better maternal and newborn care (Sibley et al., 2014). In Tanzania, 94% of the SMPs reported that the training was useful to themselves and their work (Mushi et al., 2010).
Home-visits intervention
Some of the studies reported specialized packages of home visits to increase the utilization of PHCs services for maternal, newborn, and child care (August et al., 2016; Nsibande et al., 2013; Sibley et al., 2014). The specialized home visits were particularly useful for the recognition of danger signs by mothers, improvement in child health, male involvement, and adequate antenatal and postnatal care. In Kwazulu-Natal, South Africa, CHWs delivered a package of home visits, Good Start Saving Newborn Lives, which involved the provision of essential maternal and newborn care to pregnant and postnatal women and their newborn to prevent mother to child transmission of HIV. Mothers were counseled and referred to a PHC where necessary. Referrals to PHC clinics increased and compliance with the referrals was reported to be 95% among mothers who completed the referral forms. Also, compared to none of the mothers who did not complete the referral forms, 51% of mothers who completed the referral forms recognized danger signs and reported improved infant health (Nsibande et al., 2013). Specialized visits by CHW who were trained in Home-Based Life-Saving Skills (HBLSS), to visit identified pregnant women and their husbands four times to provide education in two districts of Tanzania (August et al., 2016) was associated with a statistically significant improvement in male involvement in the intervention sites (39.2%–80.9% CI: 28.5–53.8). In the intervention sites, there was a statistically significant net intervention effect (NIE) in women’s knowledge of at least three danger signs during pregnancy (NIE 21.3%, 95% CI: 13.7–28.9), childbirth (NIE 13.9%, 95% CI: 10.5–17.4) and postpartum (NIE 15.1%, 95% CI: 9.2–21); the proportion of men who accompanied their wives to antenatal care visits (NIE 16.4%, CI: 5.6–27.2), childbirth (NIE 33.1%, 95% CI: 24.1–42.1), and joint decision between wife and husband about the place of delivery (NIE 38.5%, 95% CI: 28.0–49.1). The proportion of men who mentioned at least three danger signs during pregnancy, childbirth and postpartum significantly improved in the intervention relative to the control sites (NIE 27%, 95% CI: 15.3–38.5), took at least three birth preparation and complications readiness actions (NIE 26.8%, 95% CI: 15.3–38.2). In Ethiopia, the home visit strategy was conducted by a team comprising a Health Extension Worker, Community Health Development Agent, and Traditional Birth Attendant trained in HBLSS who taught skills to women and their care givers in their second and third trimester of pregnancy. Behavior change communication tools such as films and drama among others were also used. This intervention significantly increased the number of women who received four or more antenatal care visits, use of skilled providers for childbirth, and postnatal care for mothers and new-borns.
Birth preparedness and complications readiness intervention
A birth preparedness plan between a provider and a pregnant woman was reported in only one study conducted in Tanzania and was associated with an increase in skilled delivery, uptake, and early initiation of postnatal care. In Ngorongoro district, Arusha region, Tanzania, the intervention consisted of the introduction and promotion of birth plans during antenatal care visit to prepare women and their families for birth and complication readiness was implemented (Magoma et al., 2013). Health providers at the intervention sites were given a birth plan implementation guide and instructions on how to assist women to develop a birth plan. They discussed with women on the planned place of delivery, the importance of skilled delivery care, transport arrangement to the health facility during delivery or an emergency, funding arrangements for delivery or emergency, identification of possible blood donors, identification of a birth companion if desired, and appropriate, and support in looking after the household while the woman is at the facility. Also discussed were strategies for accessing skilled care, and recognition of danger signs during pregnancy, labor, and postpartum. Women were asked about their choice of place of delivery (dispensary or hospital) and with their consent, their male partners or any other persons they identified as a carer were invited for subsequent discussion. The birth plans were written, one copy for the woman and a second copy retained at the dispensary. Relative to the control sites, skilled delivery care was 16.8%, higher in the intervention sites [95% CI 2.6–31.0; p = .02] postnatal care utilization in the first month of delivery was higher (difference in proportions: 30.0% [95% CI 11.3–46.7; p < .01]) and was also initiated earlier (mean duration 6.6 ± 1.7 days vs. 20.9 ± 4.4 days at the control, p < .01).
Mobile Health (mHealth) intervention
Mobile health was shown to facilitate emergency medical responses, point-of-care support, improvement in access and adoption of maternal, prenatal, and neonatal services. An assessment of the impact of using mHealth (Chipatala cha pa Foni) in Malawi (Fotso et al., 2015) showed a large, positive effect of the project on the aggregate home-based care for child health (p < .01), and a sharp, negative impact on facility-based care-seeking for fever among children whose mothers/caretakers used the services offered by the intervention. A cluster randomized controlled trial conducted in primary health care facilities in Zanzibar, Tanzania demonstrated that an intervention using mobile phones with a voucher component for the wired women resulted in a 50% significant reduction in perinatal mortality (odds ratio 0.50, 95% CI 0.27–0.93) in the intervention clusters. The mobile phone intervention was associated with an increase in the uptake of four and more antenatal care visits. In the intervention group, 44% of the women received four or more antenatal care visits versus 31% in the control group (OR, 2.39; 95% CI, 1.03–5.55) (Lund, Nielsen et al., 2014; Lund, Rasch et al., 2014).
Introduction of a sub-specialty
The intervention reported by Cox et al. (2006) was the introduction of sub-specialty service (pediatric surgical clinic) at the primary health care level in Western Cape, South Africa. Over 58 months, 1,171 children aged 0 to 19 were seen, the largest group being under 1 year. The correct diagnosis was established by the nurse practitioners in 255 children (71%). In total, 597 patients were referred directly to an appropriate care facility, while 574 patients could be managed entirely at the clinic level. The clinic allowed for timely surgical intervention in 65% of surgical cases, thereby decreasing inappropriate tertiary referrals. The introduction of a subspecialty in primary health care facilities in Western Cape, South Africa improved accuracy in diagnosis and appropriate diagnosis and highlights the preventative and cost-effective role of a surgical clinic at the primary health care level.
Supportive supervision intervention
Contrary to the top-down supervision approach which tends to concentrate more on administrative functions and emphasizes fault-finding, supportive supervision emphasizes mentoring, joint problem-solving, and two-way communication between the supervisor and supervisee. A significant improvement in the quality and access to sexual and reproductive health services was reported after implementing supportive supervision in different settings. Suh et al. (2007) reported improvement in technical competence in infection prevention improved by 28% and 32% in Theies and Louga, respectively. Skills in family planning consultation improved by 16% in Louga region and 10% in Tivaoune. The management of staff and services, record-keeping, and community involvement also improved considerably. A facility-based intervention to measure the effect of supportive supervision of PHC workers in malaria case management for under-5 children was implemented in Jos, Nigeria (Bello et al., 2013). Using the WHO guidelines, training in supportive supervision was conducted in the intervention sites (PHCs) while the traditional supervisory method continued in the control sites. The mean score on knowledge of malaria significantly increased from a pre-intervention score of 10.3 ± 1.4 to 113 ± 1.5 post-intervention, whereas it decreased in the control group from 10.6 ± 1.7 to 10.5 ± 2.3 (t = 3.57 p < .0015). The malaria management practices mean score for the intervention group increased from 5.8 ± 1.7 before intervention to 7.1 ± 6.4 post-intervention. Scores for the control group decreased from 6.2 ± 1.7 pre-intervention to 5.7 ± 1.6 post-intervention, but the difference was not statistically significant. A statistically significant increase in the percentage of workers who would refer to a secondary facility following a poor response to treatment increased from 47.3% to 84.3% post-intervention for the experiment group. In Uganda, after 1 year of the intervention, significantly more functioning tippy taps (p < .002) were present in the intervention villages (47%) than in control villages (35%). Visits to pregnant women by CHVs increased from 2% of pregnant women visited once before the study to 33% of pregnant women visiting 2.3 times during the study for the control sites. At the intervention, the visits increased from 9% once pre-intervention to 46%. Visits to newborns improved from 28% once visit to 44% 1.8 times visit at the control sites; at the intervention sites, it increased from 9% once visit to 67% an average of two visits (Singh et al., 2016).
Combined interventions
In some of the studies, more than one strategy was employed to achieve the expected outcomes (Brazier et al., 2009; Ordinioha & Seiyefa, 2013; Pence et al., 2005). For instance, to increase delivery in a primary health care facility, a community education program for traditional rulers, women groups, religious organizations, and traditional birth attendants was implemented in Port-Harcourt, Nigeria. Also, the delivery fee was collected upfront with the antenatal care fee at the time of registration for antenatal care. The amount was equivalent to the average charge by TBAs in the community, and less than the fee for normal delivery in a teaching hospital. The effect was assessed 1 year after. Antenatal registration increased by 15.04% after the program. The ANC-Delivery ratio of the health center increased by 3.09%, p-value > .05 (Ordinioha & Seiyefa, 2013). In Burkina Faso, Brazier et al. (2009) reported a combination of facility and community-based interventions. The intervention package at the facilities (primarily focused on primary health centers) included activities to improve the quality, availability, and accessibility of routine and emergency obstetric care (EMOC): upgrading the skills of all maternity care providers through training in routine and emergency obstetric care; addressing gaps in essential obstetric equipment and supplies; strengthening the referral system; introducing a quality assurance methodology for maternal health services; and improving management systems. Community-level interventions focused on increasing women’s information about services. There was a large increase in the per cent of births in health facilities in the intervention district from 29% at baseline to 57% at end line (Chi2 = 185.3, p < .001); increase in delivery by skilled attendants from 24% to 56% (Chi2 = 256.4, p < .001). In the comparison district, there was no significant increase in the number of births at a health facility between the baseline and end line, but there was a slight increase in the proportion of births assisted by a skilled attendant from 32% to 36% (Chi2 = 6.2, p < .005).
Discussion
The objective of this review was to document the interventions aimed at addressing the improvement of PHC service delivery for reducing maternal, newborn, and child morbidity and mortality in sub-Saharan Africa. Specific evidence was sought for interventions, strategies, and approaches that have been implemented to improve quality and access to primary health care for maternal, newborn, and child health in sub-Saharan Africa. Strategies that resulted in improvement in the outcome of interest included financial incentives, increasing the number of providers, home visits, birth plan during antenatal care, cost-sharing, task shifting, capacity-building training of providers, mobile health, the introduction of a sub-specialty, and supportive supervision. All the studies reported some improvement in the quality of care and utilization of primary health care for maternal, newborn, and child health. The outcome indicators observed included effective management of malaria in pregnant women and infants, accurate diagnosis of childhood morbidity, timely and appropriate referrals from PHC facilities, effective service delivery for PMTCT of HIV, increase in the utilization of PHC facilities for pregnancy care, delivery, and postnatal care, increased male involvement in maternal health, improved capacity of PHC providers to provide better services, reduction in maternal and child mortality, and reduction in facility-based workload among others.
The successes recorded in the reviewed studies point to the essential role of primary health care in achieving better maternal, newborn, and child health outcomes in the region (African Union, 2013; World Health Organization, 1978, 2008). Studies in other countries confirm the important role of primary health care and the place of appropriate interventions in scaling access and quality of care at this level (Fischer et al., 2015; Ghimire et al., 2010; Macinko et al., 2006; Setiawan et al., 2016; Shei et al., 2014; Soofi et al., 2012). An appraisal of community health workers program in Malawi, Uganda, and Ethiopia in 2009 showed that effective delivery of care at the primary health level is constrained by issues such as inadequate remuneration which leads to loss of workers from time to time, insufficient attention to quality supervision and continuous training (Hermann et al., 2009). The results presented in the current review suggest that these constraints among others can be overcome with the appropriate design of interventions. Analysis of the effect of applying appropriate interventions in sub-Saharan Africa shows that over 4 million deaths of mothers, newborns, and children will be averted if known effective interventions reach 90% of targeted populations (Friberg et al., 2010).
Although the reviewed articles reported improvements in primary health care for MNCH, some gaps were identified. For instance, most of the studies did not report on confounders that may have influenced the reported results such as alternative public and private health care outreaches, improvement in economic status, better transportation, and access to health care and environmental factors among others. None of the studies focused specifically on PHC policy. The involvement of government and non-governmental agencies in Ethiopia (African Union, 2013; Memirie et al., 2016), for instance, strengthened PHC in that country, suggesting the critical role of PHC policy. There is a need for more proactive involvement of governments in enhancing quality and access to PHC for MNCH care and in reforming PHC policies to suit prevailing demographic social and economic changes in the country. Results from an analysis of the 2014 PHC reform in Poland suggest the importance of regular revision and scale-up of PHC operation and services to reflect changing health needs attuned to the current and future demographic structure of a country (Mokrzycka et al., 2016). Another major recommendation from the case of Poland is the need for the voice of the beneficiaries to be taken into account in policymaking and decision-making processes.
None of the studies focused on maternal mental health, perhaps indicating a paucity of research on mental health and a weak health system attention to mental health in sub-Saharan Africa (Jenkins et al., 2013). Maternal mental health affects child care (Harpham et al., 2005; Koutra et al., 2013; Patel et al., 2004). There is a need to scale up the scope of PHC services to include maternal mental health where it does not exist in sub-Saharan Africa. A study conducted in Australia showed the importance of scaling up the scope of PHC services for maternal health to include maternal mental health 4 years postpartum (Woolhouse et al., 2015). In this Australian study, almost one in three women reported depressive symptoms at least once in the first 4 years after birth. The prevalence of depressive symptoms at 4 years postpartum was 14.5% and was higher than at any time point in the first 12 months postpartum. More studies on maternal mental health are needed in sub-Saharan Africa.
Of note in this review is the fact that despite the positive results reported in the 25 articles, MNCH indicators in many of the countries have not improved substantially. For instance, at the termination of the MDGs in 2015, no progress was made in the reduction of MMR in Malawi, Kenya, and Nigeria but Tanzania and Ethiopia were reported to have achieved a level of change that was viewed as progress (World Health Organization, 2015). This suggests the need to scale up the successful interventions to sustainable dimensions using various novel approaches including knowledge transfer and community ownership. Most interventions in the region are sponsored by development partners from outside Africa. When the sponsorship ends, the programs inevitably suffer setbacks in many cases, especially when there is insufficient governmental or community commitment to sustain the gains. Although there were reports of community involvement in the reviewed articles particularly in recruiting community health volunteers, there is a need to strengthen sustained community ownership, including leveraging private sector support. Primary health care facilities in many countries in sub-Saharan Africa are more likely to be used by the lower socioeconomic groups than the more privileged groups (Memirie et al., 2016) and many communities in the region have high levels of poverty. Thus, communities alone cannot sustain the gains of successful intervention programs in primary health facilities, and as such political commitments from the governmental sector would be required.
The mhealth strategy is imperative given the increasing use of mobile telecommunication in many countries in sub-Saharan Africa. The mhealth in Malawi reduced the burden of care-seeking in health facilities for childhood illnesses, particularly fever (Fotso et al., 2015). This indicates that mhealth strategy would reduce the facility-level workload of PHC workers. A previous study points to the adverse effect of a large workload on providers’ efficiency in service delivery (Ogu et al., 2017). Evidence from the reviewed studies and findings from other studies show that mhealth adapted to suit the local peculiarities of the served community would increase the quality of care given by primary health care providers, and promote access to facility-based maternity care (Anstey Watkins et al., 2018; Chen et al., 2018; Ngabo et al., 2012; Tamrat & Kachnowski, 2012; Watterson et al., 2015).
In some countries such as Uganda, Ethiopia, and Nigeria, the outcomes of interventions about skilled attendance during delivery were not statistically significant. Yet, it is evident that skilled attendance at delivery is one of the most important components that can substantially improve maternal health and reduce maternal and perinatal mortality in many African countries. This is an indication that more needs to be done with respect to promoting the use of facility delivery. In addition to training more skilled MNCH providers and strengthening PHC facilities, there is a need for projects that will improve providers’ attitudes to clients and reduce long waiting times. Many studies across sub-Saharan Africa point to these as major deterrents to health facility utilization for delivery and maternal, newborn, and child care (Balde et al., 2017; Bamidele et al., 2011; Bohren et al., 2017). In addition, evidence from studies indicates that there still exists deep-seated confidence in traditional forms of maternal care in many countries in sub-Saharan Africa (Doctor & Dahiru, 2010; Sialubanje et al., 2015). This points to the need for strategies that will involve traditional birth attendants such as the “guide team” in Ethiopia (Sibley et al., 2014) to encourage skilled delivery care.
Conclusion
The results of this systematic review suggest the need for implementation research to determine how to scale up effective interventions for improving women’s access to maternal, newborn, and child health care at the primary health care level in sub-Saharan African countries. Universal access to maternal health care premised on primary health care to reach the most vulnerable and poor communities hold the key to reducing the current high burden of maternal and child mortality in the region. A knowledge transfer component should always be integrated into any intervention that is designed to improve the delivery of primary maternal health care in Africa to ensure that any knowledge gained is transferred into over-arching policies and programs. A strong political will backed by accountability mechanisms through political leadership and ownership would be critical to ensure the adoption and scaling of the best practices in primary maternal health care in the region any time soon.
A limitation of the review is the exclusion of studies published in other languages which may have accounted for the absence of articles from central Africa. Other limitations are the exclusion of articles published before 2000, gray literature, and published reports which may contain useful information on effective intervention on access and use of primary health care for maternal and child in sub-Saharan Africa. Given these limitations, the result, recommendations, and conclusions of this review are limited to the covered scope. Despite these limitations, this review revealed a large number of existing information in sub-Saharan African countries on innovative practices that can be adopted to increase women’s access to primary maternal health care for preventing maternal, newborn, and child morbidity and mortality. However, the challenge remains in identifying ways to scale such interventions to reach the most vulnerable citizens for greater impact in all parts of the continent. We recommend future reviews that will involve meta-analysis and those that will include or focus only on qualitative studies.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
