Abstract
Background
Owing to the increasing number of arthroplasty cases performed annually and an aging population with longer life expectancy, periprosthetic fractures have become more common. Very low distal femur periprosthetic fractures (PPDFF) are rare and still underreported. Due to the osteopenia bone quality at metaphysis and complex fracture pattern, fixation stability could decline over time especially with single-plate fixation, even with weight-bearing restriction. Dual construct, a newer fixation strategy, not only ensures the most stable fixation but also allows immediate weight bearing in this frail geriatric group. This study aims to demonstrate any change in fracture alignment 1 year after immediate weight-bearing practice post-surgery and to report the fracture union and functional outcomes with the newer dual construct technique.
Method
All Type III Su Classification very low PPDFFs with surgery performed from 2020 to 2023 were reviewed. All surgeries were performed using an extensile medial parapatellar single-incision approach. Either dual plate (DPC) or nail-plate construct (NPC) was performed. Immediate weight bearing was allowed from Day 1 post-surgery. Radiographs were assessed for malunion or non-union. Patients were evaluated for pain, stiffness, functional activity in the WOMAC score, range of knee motion and complications.
Results
Six were performed with DPC and another two with NPC. All patients had union at 8.0 weeks and consolidation at 35 weeks. The differences in LDFA and PDFA were only 1.4° and 1.2°. Post-surgery knee flexion was at a mean of 100°, with a mean WOMAC score of 32 points and Parker Mobility Score of 8. There was no change in ambulatory status and no postoperative complication despite the longer operative time, a mean of 172 min.
Conclusion
A dual construct by dual-plating or nail-plate combination in very low PPDFF ensures fracture fixation stability with early union and allows safe, immediate postoperative weight-bearing as tolerated in older adults.
Keywords
Introduction
Periprosthetic distal femur fractures (PPDFFs) are becoming increasingly common due to the advancing age of the geriatric population, their active mobility, and the increasing number of TKAs performed annually.
There is no consensus on an optimum treatment method. The problems associated with very low PPDFFs are severe comminution fracture pattern, osteopenia bone quality, and metaphysis bone loss which prevent stable screws purchase.
The first option is open reduction internal fixation (ORIF) by plate or nail. Previously, this fracture was treated by retrograde nailing or locked plate as a single fixation method. However, this was associated with varying complications directly related to the surgery itself, including non-union, malunion, fixation failure and revision surgery. Other indirect complications include knee stiffness, deep vein thrombosis and inability to regain pre-fall mobility and function. Various studies have compared these 2 techniques, and there was no specific preference in comparison.1,2
The second option is revision arthroplasty with distal femur replacement (DFR). The advantages include immediate weight bearing and obviate the possibility of non-union with ORIF. The surgery is more extensive with a larger surgical insult. It requires distal femur bone resection and tibia base plate revision with a long stem and a constrained polyethylene construct. There is a risk of refracture, infection, and implant loosening. Hence, this option should be considered carefully, depending on the patient’s life expectancy. Also, this option may not be feasible in our setting as it is more costly. A recent meta-analysis review shows similar surgical complication and reoperation rates comparing both ORIF and DFR, however, DFR is associated with a 3 times higher rate of medical complications post-surgery. In short, DFR is a suitable salvage option when the fracture is too complex to be fixed or in a failed ORIF scenario.3,4
In the geriatric group, it is imperative to give stable fixation, which allows early and immediate weight bearing to reduce morbidities. The treatment of fragility long bone fracture should be given similar attention as the treatment of geriatric hip fracture. Previous studies involved only a small number of patients due to the rarity of Su Type III very low PPDFFs. 5 The objectives of this write-up were to demonstrate any change in the alignment of the fracture at 1 year following immediate weight bear as tolerated (WBAT) practice after surgery and to report the union rate and functional outcome by performing the dual fixation technique of NPC or DPC.
Methodology
All patients with Type III Su classification very low PPDFFs who presented to our tertiary referral center from 2020 to 2023 were included. The exclusion criteria include the presence of TKA implant loosening or severe metaphysis bone loss with poor bone stock. This was a retrospective review of patients’ records. The study obtained ethical approval from the National Medical Research Register committee (NMRR ID - 24-00503-7IO).
Preoperative Preparation
All patients had standard radiographs and computed tomography (CT) scans with a 3D reconstruction view performed before surgery. Sagittal and coronal views were assessed for the configuration of the fracture pattern, bone stock remaining in the metaphysis, and loosening of femoral and tibial components. Blood investigations, especially septic parameters, were performed to exclude the possibility of infection in the TKA implant. If there was any suspicion of infection, ultrasound-guided knee aspiration was performed, with the joint fluid being sent for microbiological testing.
Surgical Technique
The surgery was performed by a single consultant arthroplasty surgeon. The midline single incision extensile medial parapatellar approach was used following the previous scar. A proximal extension was made along the plane between the rectus femoris and vastus medialis muscle by identifying the fatty tissue pad in between. 6 Joint fluid was routinely aspirated and tested with the Alpha Defensin test before arthrotomy. First, the fracture site was assessed for any sign of infection and collateral ligaments were checked for their integrity. Then, femoral and tibia components were checked for loosening. The polyethylene insert was assessed for any wear damage.
The fracture was reduced with manual traction in supine and knee flexion at 45°. Multiple Kirschner Wires 2.0 mm were inserted for temporary stabilisation. Fracture reduction was performed first at the less comminuted side (Figure 1). For Dual Plate Construct (DPC), a medial locking compression plate (LCP) was inserted first. A single proximal cortical screw was inserted first after confirming the plate position, followed by the distal locking screws. The choice of the medial plate would depend on the size of bone fragments and be shorter than the lateral plate. It included distal femur LCP, proximal tibia LCP, medial distal tibia LCP, and olecranon LCP. Plate bending could be done if necessary to follow the conformity of the medial distal femur. Fracture Reduction With Double Reduction Clamp and Entry Point for Retrograde Nail Created (Left) and Extensile Medial Parapatellar Approach (Right)
Subsequently, the lateral variable angle distal femur LCP was inserted. A periarticular reduction clamp was applied to compress both plates together, which helped restore coronal alignment. 7 Distal locking screws were inserted based on fracture configuration with variable angle drill sleeves. The screws for the distal end should be long adequately to purchase until the opposite column to create an interdigitating locking configuration.
Proximally, lateral minimal invasive incisions were used for proximal screw insertion with the LISS system (Figure 2). Intraoperative Fluoroscopy was used to check for fracture alignment, plate length and screw configuration. For Nail Plate Construct (NPC), the retrograde nail was inserted first, followed by lateral variable LCP using a similar minimal invasive surgical approach (Figure 3). A surgical drain was inserted for all patients to prevent hematoma collection. Well-Healed Incision Following Previous Scar (Left) and Multiple Small Mini-Invasive Incisions at Lateral for Locking Screws Placement (Right) Dual Plate Construct (DPC) (left), Nail Plate Construct (NPC) (right)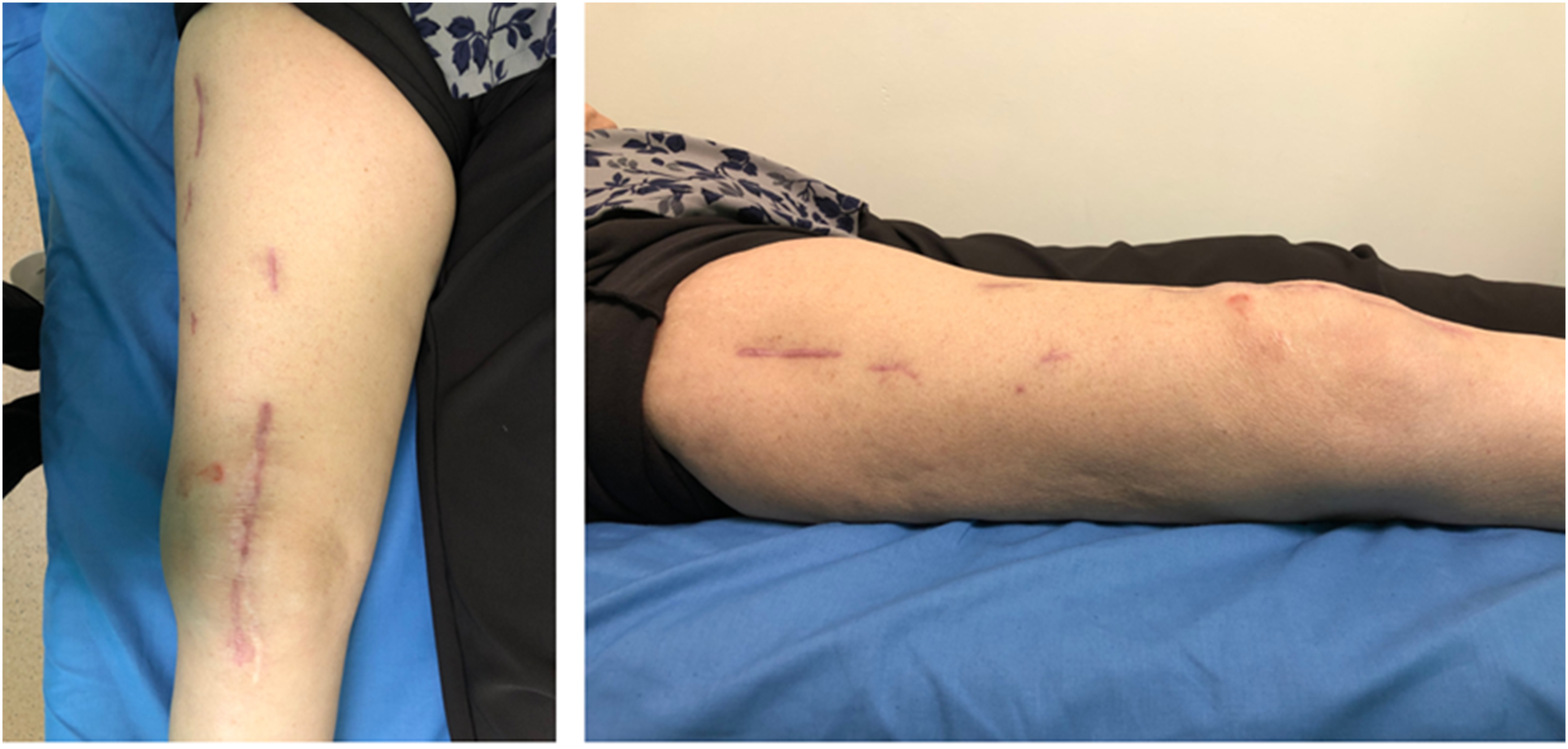

Post-Operative Protocol and Evaluation
After surgery, patients would be co-managed by the geriatric and arthroplasty subspecialty team. Postoperatively, all patients were allowed to weight bear as tolerated (WBAT) with a walking frame from day 1 onwards. We do not specifically restrict the weight-bearing ability of the patient. Daily continuous passive motion of the knee and self-active knee motion exercises were started immediately from day 1. All patients were given subcutaneous teriparatide injections, starting from day 3 post-surgery, for a total of 3 month duration.
All patients were followed up at weeks 2, 4, 8, 16, 24, and 52, calculated from the date of surgery. Full-length lower limb anteroposterior (AP) view, whole femur AP and lateral radiographs were repeated during follow-up to investigate for fracture displacement and callus formation. Radiological measurements, including posterior distal femoral angle (PDFA) and lateral distal femoral angle (LDFA), presence of callus formation at bone cortices and clinical assessments, including pain, stiffness, range of motion (ROM), and ambulation status were performed by fellowship-trained arthroplasty surgeons (Author 1 and (2) at weeks 4, 8, 16, 24 and 52. Surgical complications, including failure of fixation, infection, hematoma, and any re-operation, were recorded.
Primary Outcome
The primary outcome is to investigate the alignment of fracture and fracture union. Malunion is defined by (1) greater than 5°of coronal malalignment compared with normal mechanical LDFA of mean 88° (range 85-90°) and (2) greater than 10° of sagittal malalignment based on anatomical PDFA of mean 83° (Range 79-87°).8,9 The angles were measured on the initial post-operative radiographs and during bone union and the angle difference was calculated to investigate for any malalignment after the weight-bearing practice. The presence of callus formation at the fracture site in 3 out of 4 cortices on the AP and lateral radiographs would be considered as fracture union. Non-union is defined by the absence of callus in 3 out of 4 bone cortices after 3 months. 10 The obliteration of the fracture line with calcified bridging callus would be considered as bone consolidation. 11 Time to union and time to consolidation were recorded.
Secondary Outcome
The secondary outcome is to assess the knee function post-surgery. The outcome measures include knee ROM, change in ambulatory status, Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) score, and Parker Mobility Score, assessed at week 24 follow-up. 12 Data analysis was performed using the student t-test with SPSS version 29.0.2 (IBM SPSS Statistics for Windows, IBM Corp., Armonk, NY, USA).
Results
Demographics of Patients a (n = 8)

aBMI = Body Mass Index, CCI = Charlson Comorbidity Index, CR = Cruciate Retaining, PS = Posterior Stabilising.
Clinical Outcomes and Radiological Outcomes, Statistical Analysis by Student T-test (Two-Sided) a

aROM = Range of motion, ° = Degree, WOMAC = Western Ontario and McMaster Universities Osteoarthritis Index, LDFA = Lateral Distal Femoral Angle, PDFA = Posterior Distal Femoral Angle.
The initial postoperative LDFA was 86.2°. At the time of union, LDFA was 86.9°. The mean difference was 0.7° for varus malalignment after bone healing, statistically not significant to suggest any fracture malunion despite immediate weight bearing (Table 2). For sagittal alignment, the mean PDFA at initial post-surgery was 84.8° and, at the time of union, the mean PDFA was 85.6°. The difference for PDFA after union was 0.8°. None of the patients required reoperation and neither had any surgical complications.
Discussion
The incidence of periprosthetic fracture ranges from 0.3 to 5.5% following primary surgery and up to 30% in revision knee surgery. The Scottish registry has shown that the number of periprosthetic fractures has doubled over 11 years. 13
The multicentre analysis from the Characteristics, Outcomes and Management of Periprosthetic Fracture Service Evaluation (COMPOSE) study team shows that patients with periprosthetic fractures around the knee are more frail and elderly, with a mean age of 80. Mortality of PPDFFs was reported as high as 26%, especially in those with multiple medical comorbidities and almost equal to hip fracture.14,15 The priority, hence, should be expedited surgery for frail older adults. 16 It took us 9 average days to operate for this study group due to the delay in optimizing the medical condition, waiting for COVID swab results, and the arrangement of operating theatres.
Secondly, early mobility is important in managing geriatric fractures to reduce postoperative mortality. The norm of a surgeon in prescribing reduced weight-bearing status after surgery is very difficult for frail older adults to comply with. Hence, they are prone to diminishing their mobility attempts. 17 Immediate weight bearing does not affect the union rate or increase the reoperation rate in PPDFFs with dual construct fixation while enabling a return to baseline ambulation status.18,19
A stable fixation construct is vital, which not only allows micromotion for callus formation but also eases the surgeon’s worry about the practice of early weight bearing. The difficulties posed by Su Type III distal femur fracture include osteoporotic bone quality, comminuted fracture pattern, and inadequate bone for screws anchorage with metaphysis bone loss. Previously, it was managed with a single construct, either a plate or a nail.
The single plate fixation method has a high risk of failure with limited screws anchorage in a weakened metaphysis with a tendency for varus malalignment. Even with a long working length plate and variable angle locking screws, there is still a risk of screws cut out and late displacement. If there is medial comminution in the distal femur, it is associated with a 10 times hazard ratio of reoperation 20
A single intramedullary nail fixation is also associated with mal-reduction with extension deformity, especially in a posteriorly placed box design with a poor nail entry point. Intramedullary nail fixation requires an open-box femoral design for nail entry. Its trajectory may be affected by the diameter and location of the box and could lead to fracture mal-reduction in the sagittal plane. A posteriorly placed box with a poor nail entry point potentially causes mal-reduction with extension deformity. One case series reported this extension deformity in half of their series. 21
A systematic review has shown an equivalent union rate and no difference in reoperation rate between the nailing and plating methods. However, nailing is associated with less non-union and infection.2,22,23 Another systematic review also shows similar union rates of up to 80% for both methods, but nailing was 18% higher in malunion and required revision. 24 Plating was associated with non-union, while malunion was seen in nailing. 25
The latest update in managing this complex fracture was the use of dual construct fixation, which was either dual plate construct (DPC) or nail-plate construct (NPC) as shown in Figure 3.
A biomechanic study has shown that DPC has at least 2.6 times better torsional stiffness and higher load to failure than single-plate26,27 DPC reduced fracture gap motion to 0.13 mm under bending and compression, which is only 4.3% of the fracture gap in contrast to the single plate with 0.6 mm gap motion, equivalent to 20% of the fracture gap. 28 It also reduced the incidence of varus collapse to 2.6% compared to 26% in single plate, and fracture is more likely to be anatomically reduced. 29 29 The addition of a short medial plate is safe, with a study showing that the femoral artery’s average distance from the adductor tubercle is within 16-18.8 cm. 30 To sum up, a medial plate is added as a buttress to prevent varus collapse and increase construct stiffness, which is beneficial for distal periprosthetic fracture. 31
Another biomechanic study shows that either NPC or DPC construct improves stiffness, survival and cycles to failure. 32 The NPC survives 100% maximum loading in the test compared to 70% in the DP. This would be beneficial in a short and weakened distal fracture segment. NPC method is affected by nail diameter. An 11 mm NPC is 1.6 times stiffer than a 9 mm NPC, and a higher overall construct stiffness allows immediate post-op weight bearing. 27 NPC provides a better union rate and prevents varus collapse compared to the single lateral plate fixation method.33,34 With the above-mentioned biomechanics studies, a dual construct with plates or nail plates would be preferred, as the overall construct would have more stability and stiffness.
To date, 3 retrospective clinical studies reported only a low number of patients with Su III PPDFFs (n = 215, n = 97, n = 1310) however, showed excellent radiographic and functional outcomes with dual plate fixation. In a comparison study, Kriechling et al 29 reported that none of the DPC patients (n = 7 with Su III fracture) underwent revision, compared to 6.7% in the DFR group and 14% in the single plate construct group. Similarly, our study shows that with immediate weight-bearing practice, there is no significant displacement or malunion (Table 2).
A meticulous preoperative surgical planning includes a whole-length femur radiograph, a CT scan with 3D reconstruction to assess the remaining bone stock and to check on the box’s location and width corresponding to the diameter of the nail reamer and rehearsal of wire trajectory placement to prevent fracture mal-reduction. Preparing the armamentarium for various plates, bone grafts, polyethylene inserts, and revision arthroplasty sets before surgery is tedious but vital for ensuring the success of the surgery.
Our practice is an extensile medial parapatellar approach with a single midline incision following the previous scar (Figures 1 and 2). This approach is more than adequate for visualization of both the medial and lateral distal femur circumferentially.6,35 It reduces the risk of patella avascular necrosis compared to the double incision. This approach allows direct inspection of femur or tibia component loosening and polyethylene damage. In unexpected infection, thorough debridement and implant removal can be performed without the need for a second incision. 36 The infection rate reported was low, 1.7% for this surgical approach. 20
Lastly, attention should be given to the management of osteoporosis which is one of the main risk factors in periprosthetic fracture. 37 All patients in our case series received teriparatide injection for only 3 months, followed by alendronate therapy. The teriparatide was started immediately post-surgery, before discharge, and after consultation with the geriatric consultant. Notably, teriparatide therapy was recommended only for the treatment of osteoporosis as per FDA approval. Kim et al. reported abundant callus formation at 2 months and earlier fracture healing with the clinical union at 5.7 months with teriparatide injection in femur fractures, including periprosthetic fracture. 38 The latest systematic review, published in 2023, reported that subcutaneous teriparatide was safe and effective in inducing callus formation and treating delayed unions. 39 As discussed above, our 4 management principles involve early surgery, immediate mobility, stable fixation, and osteoporosis management.
There were a few limitations of the study. First, the small number of patients was included because the Su III fracture pattern was rare compared to the Su I and II fracture patterns. Due to the small sample size, a power analysis for sample size calculation was not done. Also, there is no comparison group to the single plate fixation method as this was not practiced in our center, particularly the Su III fracture pattern, for the reasons explained above. The early good result of this case series would prompt us to continue the same treatment principles and strategy with the hope of a larger study in the future. Next, not all patients receive bone density scans as they would be performed on an appointment basis due to the busy tertiary hospital setting. Osteoporosis management is started immediately post-surgery without delay and without waiting for the DEXA scan appointment. Most patients were given only a short 3 month duration of teriparatide due to expensive cost and ‘off-license’ use to stimulate callus formation without the suggested length of treatment.
Conclusion
A dual construct by double plating or nail-plate combination in Su III periprosthetic distal femur fracture ensures fracture fixation stability with early union and allows immediate postoperative weight bearing in the geriatric population.
Footnotes
Acknowledgement
We would like to thank Director General of Health, Ministry of Health Malaysia for his permission to publish this article.
Ethical Approval
This study was conducted in accordance with Declaration of Helsinki and has received ethical approval from National Medical Research Register (NMRR) committee with protocol number of (NMRR ID-24-00503-7IO).
Informed Consent
Written informed consent was obtained from all patients.
Author Contributions
Author 1: Conceptualization, Methodology, Writing original draft and editing. Author 2/3: Reviewing and Editing. Author 3/4: Supervision.
Funding
The research did not receive any specific funding or grants.
Declarations of Conflicting Interests
The authors declare that they have no relevant financial or non-financial interests to report
Data Availability Statement
The data of this study is available from the corresponding author, Wei Cheong Eu, upon reasonable request.
