Abstract
Introduction
Distal femur fractures are the second most common femoral fragility fractures in older adults, with postoperative mortality rates similar to or exceeding those of hip fractures. While early surgery has been shown to improve outcomes in hip fracture patients, its impact on distal femur fractures remains unclear. This study examines the relationship between surgical timing and postoperative outcomes in distal femur fracture patients.
Methods
This retrospective cohort study utilized the American College of Surgeons National Surgical Quality Improvement Program (ACS NSQIP) database to identify patients aged 65 and older who underwent surgery for distal femur fractures between 2015 and 2022. Patients were categorized into early (within 1 day), intermediate (between 1-2 days), and delayed (>2 days) surgery groups. The primary outcome was 30-day mortality. Secondary outcomes included postoperative complications, length of hospital stay (LOS), and hospital readmission rates. Multivariate logistic regression was performed to adjust for potential confounders.
Results
A total of 4500 cases met the inclusion criteria, with 67% undergoing surgery within one day, 20% within 1-2 days, and 13% after more than two days. After adjustment for baseline characteristics, early surgery was not associated with a significant reduction in 30-day mortality (OR: 1.00, 95% CI: 0.57-1.83,
Conclusions
Unlike in hip fractures, early surgery did not significantly impact mortality or most postoperative complications in distal femur fracture patients. However, it was associated with a reduced risk of UTIs. These findings suggest that surgical timing may be less critical than preoperative optimization and comprehensive perioperative care in improving outcomes for this population.
Keywords
Introduction
Fragility fractures in the lower extremities represent a major cause of morbidity and mortality among the aging population in the U.S. 1 Among elderly patients, distal femur fractures are the second most common type of femoral fragility fracture after hip fractures. 2 Typically resulting from minor trauma, such as falls from standing height, these fractures are associated with a high postoperative mortality rate, ranging from 13.4% to 35% within the first year—a rate that is often similar to or even exceeds that of hip fractures.3-12 Given these similarities, there is increasing interest in exploring whether early surgical intervention, which has shown improved outcomes in hip fracture patients, might yield comparable benefits for distal femur fracture patients.
Managing distal femur fractures presents unique challenges. These fractures often involve complex patterns, such as comminution and intra-articular extension, and occur frequently in patients with osteoporotic bone. Furthermore, the increasing rate of total knee and hip arthroplasty has led to a rise in periprosthetic and interprosthetic distal femur fractures, further complicating surgical management.8 9 While early surgery has been shown to improve outcomes in hip fracture patients,13-16 its impact on distal femur fractures remains less clear. Despite similarities in patient demographics and injury mechanisms, studies examining time to surgery in distal femur fractures have reported conflicting results. These inconsistencies may stem from differences in study design, patient populations, and institutional protocols.1,17-24 A multi-institutional analysis is therefore needed to determine whether early surgical intervention provides comparable benefits in this population.
The purpose of this study is to explore the relationship between surgical timing and postoperative outcomes in distal femur fracture patients. The primary outcome is 30-day mortality, assessing whether early surgical intervention is associated with improved survival. Secondary outcomes include the incidence of postoperative complications (such as infectious, thromboembolic, renal, cardiovascular, and pulmonary complications), length of stay (LOS), and the rates of hospital readmission and reoperation within 30 days.
By systematically analyzing these outcomes, this study aims to determine whether early surgery for distal femur fractures confers similar benefits to those observed in hip fracture management.
Materials and Methods
Data Collection and Patient Selection
This study used a retrospective cohort design, drawing data from the American College of Surgeons National Surgical Quality Improvement Program (ACS NSQIP) database. The ACS NSQIP is a national registry that includes patient demographics, comorbidities, surgical details, and 30-day postoperative outcomes from over 600 hospitals across the United States. ACS NSQIP includes a diverse mix of public and private hospitals of varying sizes, which enhances the generalizability of our findings. For this study, we utilized ACS NSQIP data to construct a comprehensive dataset of patients who underwent distal femur fracture surgery between January 1, 2015, and December 31, 2022. Patient identification was based on specific procedural codes, including CPT 27509, 27511, 27513, and 27 514. These codes correspond to the following procedures: 27 509 – open treatment of a distal femoral fracture involving the medial or lateral condyle with internal fixation; 27 511 – open treatment of a femoral supracondylar fracture without intercondylar extension, including internal fixation; 27 513 – open treatment of a femoral supracondylar fracture with intercondylar extension, including internal fixation; and 27 514 – percutaneous skeletal fixation of a femoral supracondylar fracture, with or without intercondylar extension. It is worth nothing that this study included all surgically treated distal femur fractures without distinguishing between native and periprosthetic fractures, as the ACS NSQIP dataset does not differentiate between these categories. However, patients who underwent distal femoral replacement were excluded, as this procedure could differ in patient population, perioperative management compared to open reduction and internal fixation (ORIF) or intramedullary nailing, and could introduce confounding effects on the early postoperative outcomes. We excluded patients younger than 65 and those with missing time-to-surgery data.
Patient, Demographic, and Perioperative Variables
Baseline Clinical Characteristics
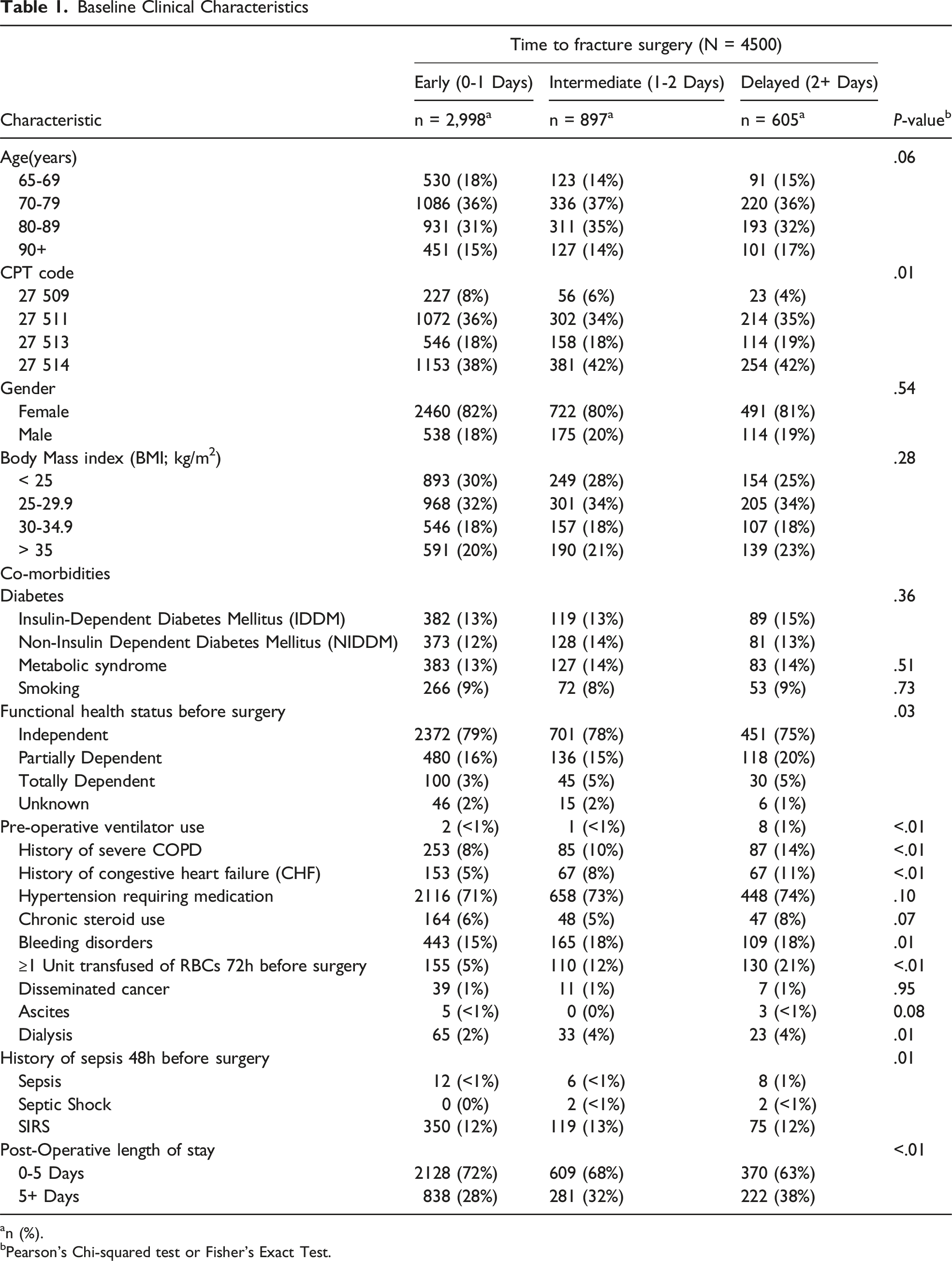
an (%).
bPearson’s Chi-squared test or Fisher’s Exact Test.
Outcome Measures
Surgical timing was defined using the NSQIP ‘Days from Hospital Admission to Operation’ variable, which categorizes time as 0 days, 1 day, 2 days, etc. This variable provides a standardized approach for assessing surgical timing within NSQIP. 25 Based on this classification, we categorized patients into three groups: early group (within 1 day), intermediate group (between 1-2 days), and delayed group (more than 2 days). The primary outcome is 30-day mortality, assessing whether early surgical intervention is associated with improved survival. Secondary outcomes include the odds of postoperative complications and LOS. The complications assessed included surgical site infections (categorized as superficial, deep, or organ/space), pneumonia, pulmonary embolism (PE), acute renal failure, urinary tract infection (UTI), stroke/cerebrovascular accident, cardiac arrest, myocardial infarction, deep vein thrombosis (DVT), septic shock, sepsis, reoperation, and hospital readmission.
Statistical Analyses
Statistical analyses were conducted using R statistical software. Relevant demographic and clinical characteristics were compared between the three time-to-surgery cohorts using Chi-Square Tests or Fisher’s Exact Test.
To identify the most relevant covariates for each outcome, we employed a two-step variable selection process combining stepwise selection and LASSO (Least Absolute Shrinkage and Selection Operator) methods. 26 This approach was chosen to balance traditional statistical significance (stepwise) with modern regularization techniques (LASSO) for robust variable selection. For each outcome, stepwise selection was performed using both forward and backward elimination, with the Akaike Information Criterion (AIC) as the selection criterion. 27 Then, LASSO selection was conducted using cross-validation to determine the optimal regularization parameter. This process was repeated for each of the 16 outcomes studied. The final set of covariates for each outcome was determined by taking the variables selected by both methods. In cases where there were no shared variables, unique variables from each outcome were selected.
After covariate selection, multivariate logistic regression analysis was used to examine the association between time to surgery and each outcome, with the delayed time-to-surgery cohort (2+ days) serving as the reference group. Each model included the selected covariates specific to that outcome for parsimonious and comprehensive adjustment of potential confounders. Results were presented as adjusted odds ratios with 95% confidence intervals and
Results
A total of 4500 cases met the inclusion criteria and were included in this study (Figure 1). The majority of patients were female (81.6%), with 78.3% being independent before surgery, and 36.5% falling within the 70-79 age group. Among these cases, 67% underwent surgery within 1 day of admission (early group), 20% had surgery between 1-2 days (intermediate group), and 13% had surgery after more than 2 days (delayed group). (Table 1) Patients with significant medical comorbidities, such as severe COPD, congestive heart failure, dialysis dependency, bleeding disorders, the need for preoperative transfusion, or preoperative sepsis, were more likely to experience delayed surgery (Table 1). Overall time to surgery, 30-day mortality, postoperative complications, and length of hospital stay for the study cohort are summarized in Table 2. Flow diagram of case selection. Time to Distal Femur Fracture Surgery, Overall 30-Day Mortality, and Complications an (%).

Multivariate Regression Analysis on the Effect of Time of Distal Femur Fracture Surgery on 30-Day Post-operative Patient Outcomes
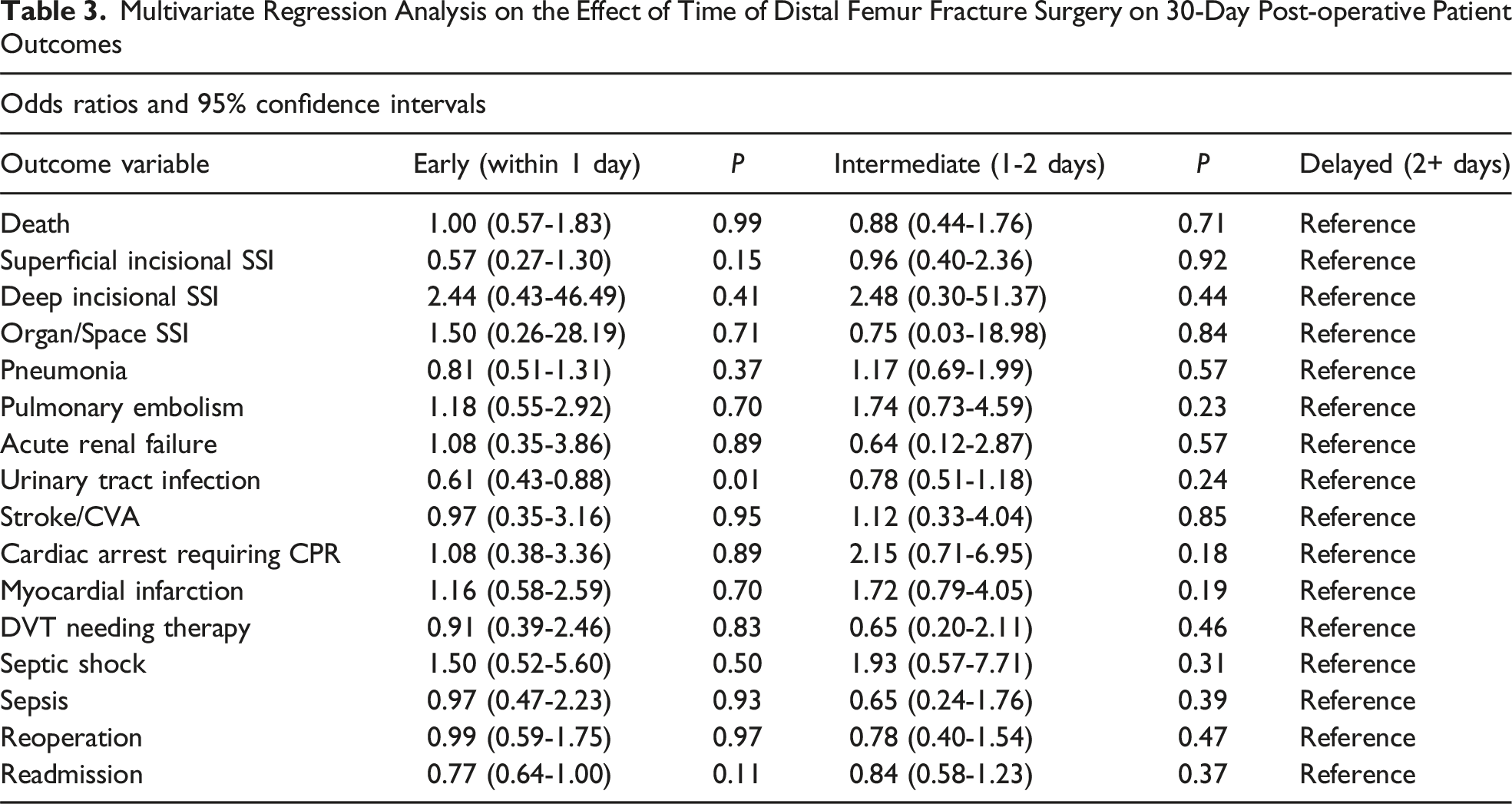
Selected Variables for Each Outcome in Multivariate Regression Analysis

Discussion
This study examined the impact of surgical timing on postoperative outcomes in distal femur fractures and found that early surgery (within one day) was not associated with a reduction in 30-day mortality or major complications, although it was linked to a lower incidence of UTI. Unlike hip fractures, where expedited surgery has demonstrated improved survival and reduced complications, our findings suggest that surgical timing may be less critical in distal femur fractures. Instead, patient comorbidities and overall health status likely play a more significant role in determining outcomes.
Time to Surgery (TTS)
Our study observed a median time to surgery of just one day, with 67% of patients undergoing surgery within 1 day. This finding is shorter compared to previous research. For example, Mubark et al
9
reported that surgery for distal femur fractures was significantly delayed compared to proximal femur fractures, with a mean time to surgery of 49.1 hours vs 34.1 hours (
Impact of Surgical Timing on Outcomes
Previous studies have reported inconsistent results. Some studies have suggested that delayed surgery is associated with increased mortality. Gutbrod et al and Cheng et al reported that longer time to surgery was linked to higher in-hospital mortality rates.19 20 Streubel et al also found that surgery more than four days after injury was associated with significantly higher 6-month and 1-year mortality rates. 21
In contrast, other studies have reported no significant association between surgical timing and survival. For example, Wulbrand et al found that surgical delays beyond 24 hours in peri-implant distal femur fractures did not lead to increased complication or mortality rates. 22 Similarly, Delgadillo et al reported no significant association between surgical timing and mortality outcomes, although their analysis was limited by a small patient sample. 23 A large-scale study in Japan found that surgery within two days of admission was associated with fewer postoperative complications, shorter hospital stays, and lower hospitalization costs, but not with reduced 30-day mortality. 24 Our findings align with the latter group, as we observed no significant difference in 30-day mortality between early and delayed surgery groups after adjusting for confounders.
Our study also found no significant differences in most major complications between early and delayed surgery groups—except for a lower incidence of UTI in the early surgery cohort. Although UTIs may be considered a minor complication, they can contribute to delirium, delayed recovery and increased healthcare utilization, particularly in frail, older adults. 28
The comparable mortality and complication rates between early and delayed surgery groups—despite differences in surgical timing—suggest that patient health status and comorbidities may have a greater influence on outcomes than surgical timing alone. The delayed surgery group had a higher burden of comorbidities, which likely influenced both the decision to delay surgery and the overall recovery process. This indicates that surgical postponement was more often driven by medical necessity rather than system-related delays, meaning that sicker patients were more likely to undergo delayed surgery. Despite this, outcomes remained similar between early and delayed surgery groups, reinforcing the idea that preoperative optimization may be more important than the timing of surgery itself. Stabilizing medically complex patients before surgery could help mitigate the risks associated with delayed intervention, underscoring the need for individualized surgical planning rather than rigid adherence to timing benchmarks.
Why Surgical Timing May Be Less Important in Distal Femur Fractures
One possible explanation for the reduced impact of surgical timing in distal femur fractures compared to hip fractures is the greater complexity of distal femur fracture patterns and surgical management. Hip fractures are typically treated with relatively standardized procedures such as hemiarthroplasty or intramedullary nailing, which can be performed rapidly with minimal variation in technique. In contrast, distal femur fractures present greater variability in fracture morphology and fixation strategies. Distal femur fractures can involve comminution, intra-articular extension, or periprosthetic involvement, often necessitating more extensive preoperative planning, specialized implants, and subspecialist input, which may not be feasible within a strict 24-hour window. 29
Length of Stay and Recovery
Patients in the delayed surgery group had longer postoperative hospital stays, likely due to greater medical complexity, which may have slowed their recovery. However, since this study is retrospective, it is unclear whether surgical delays directly caused the longer hospital stays or if they were primarily driven by the patients’ underlying health conditions. Notably, the relatively short hospital stays observed in our cohort likely reflect standard practice in the U.S., where patients are often discharged to post-acute care facilities such as transitional care units and skilled nursing facilities. 30 This difference in healthcare systems should be considered when interpreting these findings, as countries with different post-acute care infrastructure or discharge practices may report longer hospital stays due to limited access to rehabilitation facilities or differing care models.
Clinical Implications
Our findings suggest that the emphasis on early surgery for distal femur fractures may be less critical than in hip fractures. Instead, a patient-centered approach that balances timely surgical intervention with appropriate preoperative optimization may be more beneficial. While unnecessary surgical delays should be avoided, particularly in stable patients, forcing early surgery in medically complex cases may not yield significant improvements in outcomes.
For clinical practice, these results highlight the importance of assessing each patient individually, considering factors such as preoperative mobility, frailty, comorbidities, and baseline functional status when determining the optimal timing for surgery. Furthermore, our findings reinforce the importance of comprehensive perioperative care, including strategies to reduce infection risk, improve early mobilization, and address medical comorbidities preoperatively.
Limitations
This study has several limitations that may affect the interpretation of the findings. First, the retrospective design limits our ability to establish causality between surgical timing and outcomes. Second, ACS NSQIP data is restricted to the initial 30 days after surgery, which may overlook essential information on long-term outcomes, functional recovery, and quality of life in older patients. This limitation prevents an analysis of whether surgical timing influences longer-term morbidity and mortality. Third, reliance on ACS NSQIP data may introduce selection bias, limiting the generalizability of our findings to all institutions treating distal femur fractures. The dataset does not distinguish between native and periprosthetic distal femur fractures, which introduces heterogeneity in the study population and makes it difficult to determine whether fracture type modifies the relationship between surgical timing and outcomes. Additionally, identifying patients based on procedural codes may contribute to selection bias due to variability in coding practices across institutions. Fourth, patients in the delayed surgery group had a higher burden of comorbidities, suggesting that their allocation to delayed surgery was primarily driven by medical necessity rather than system-level delays or random variation. This baseline difference in patient characteristics may have influenced outcomes, although we attempted to account for this using multivariate logistic regression with covariate adjustment. Matching the cohorts using propensity score matching or similar techniques could have provided better balance in patient characteristics, but we opted not to pursue this approach due to concerns about significantly reducing the sample size, which could have limited statistical power and generalizability. Fifth, the dataset lacks fracture classification data (e.g., AO/OTA classification), which could have provided more detailed insights into whether fracture morphology influences the effect of surgical timing. Distal femur fractures are complex injuries with varying patterns of comminution, intra-articular extension, and periprosthetic involvement, all of which may affect surgical decision-making and outcomes. Without this information, it is difficult to determine whether the complexity of the fracture influenced the relationship between surgical timing and outcomes.
Future Directions
Future research should focus on prospective studies with longer follow-up periods to assess long-term functional outcomes, complications, and mortality beyond the 30-day postoperative window. Incorporating fracture classification and functional outcomes would help clarify the optimal timing for surgery in different types of distal femur fractures.
Conclusion
In contrast to hip fractures, early surgery did not significantly reduce 30-day mortality or major complications in distal femur fractures, though it was associated with a lower risk of UTI. These findings suggest that surgical timing may not be the most critical factor influencing outcomes in this population. Instead, patient comorbidities, preoperative health status, and perioperative care strategies may play a larger role in recovery and survival. This study underscores the need for an individualized approach to surgical timing, where patient optimization and comprehensive care take precedence over rigid time-based benchmarks.
Footnotes
Author Contribution
NO contributed to study conceptualization, manuscript composition, and manuscript final revision. GA contributed to data collection and analysis, manuscript composition, and final revision approval. SF contributed manuscript composition and final manuscript revision approval. CYQ contributed to manuscript editing and final manuscript revision approval. CQ contributed to study conceptualization, manuscript editing, and final revision approval.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Institute on Aging under the Paul B. Beeson Emerging Leaders Career Development Award in Aging (K76AG068435) and the authors also acknowledge funding from OREF Mentored Clinician Scientist Grant GR134534 (Quatman).
Declaration of Conflicting Interest
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr. Carmen Quatman is a committee member for IGFS. For the remaining authors none were declared. The remaining authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
