Abstract
Background
Patients with geriatric neck of femur (NOF) fractures often have multiple medical conditions and compromised baseline nutrition, impacting arthroplasty outcomes. Indicators like BMI, albumin, hemoglobin, urea, creatinine, CRP, and HbA1c influence nutritional status and postoperative results. This study evaluates the impact of preoperative nutrition on surgical outcomes, including postoperative complications, mobility, and pain scores in geriatric femoral neck fractures.
Methods
A retrospective study of 141 geriatric patients with NOF fractures admitted to Kuala Lumpur General Hospital between 2022-2023, treated operatively, was conducted. Associations of age, gender, ethnicity, BMI, education, smoking status, comorbidity, pre-fracture mobility, American Society of Anesthesiologists (ASA) level, and perioperative nutritional parameters with post-surgical complications, mobility, and WOMAC scores 1-year post-surgery were analyzed using logistic regression.
Results
Higher BMI (AOR = 1.21, 95% CI: 1.07-1.42, P = 0.03) and ASA levels ≥2 (AOR = 2.53, 95% CI: 1.30-4.91, P = 0.01) were significant predictors of post-surgical complications. Abnormal hematological variables, including hemoglobin (AOR = 1.78, 95% CI: 1.45-2.45, P < 0.001), urea (AOR = 1.35, 95% CI: 1.15-1.60, P = 0.002), creatinine (AOR = 1.20, 95% CI: 1.00-1.52, P = 0.04), and HbA1c (AOR = 1.40, 95% CI: 1.25-1.67, P = 0.004), were also associated with complications. BMI (AOR = 1.12, 95% CI: 1.06-1.30, P = 0.049) and abnormal hematological variables, including hemoglobin (AOR = 1.99, 95% CI: 1.05-2.70, P = 0.003), urea (AOR = 1.58, 95% CI: 1.06-1.95, P = 0.006), creatinine (AOR = 1.21, 95% CI: 1.09-1.38, P = 0.048), and HbA1c (AOR = 1.98, 95% CI: 1.25-2.57, P = 0.002), were significant predictors of reduced post-surgical mobility. No significant factors were associated with WOMAC scores at 1 year.
Conclusion
Preoperative nutritional status significantly impacts outcomes in geriatric patients undergoing arthroplasty for femoral neck fractures. Comprehensive preoperative nutritional assessments are essential for improving postoperative outcomes.
Introduction
Nutrition plays a crucial role in the overall success of an arthroplasty surgery. Body mass index (BMI) and albumin (ALB), hemoglobin (HB), urea, creatinine (CRET), C-reactive protein (CRP), and Glycosylated hemoglobin (HbA1c) levels are important preoperative clinical indicators that play a significant role in preventing post-arthroplasty surgery complications such as prosthetic joint infections (PJIs), decreased mobility, and pain. For example, ALB, a serum protein, plays a crucial role in maintaining osmotic pressure in the blood, transporting various substances, and supporting immune function. Hypoalbuminemia states are associated with impaired wound healing, reduced immune response, and increased risk of infection. 1 In addition, adequate HB levels are crucial for tissue oxygenation and wound healing. Low HB levels result in anemia, leading to tissue hypoxia, impairing the body’s ability to fight infections and heal properly after surgery. 2
Urea and creatinine levels reflect the patient’s kidney function, wherein impaired kidney function would result in chronic inflammation and anemia, negatively affecting wound healing. The risk of PJI is higher in patients with chronic kidney disease. 3 CRP is an acute inflammatory marker that increases at the sites of inflammation or infection. Although the prevalence of elevated preoperative CRP is low, elevated CRP levels are associated with PJI. 4 BMI is a measure of body fat based on height and weight. It indicates overall nutritional status and can be an important predictor of postoperative complications. Both underweight and obese patients have a higher risk of complications, including infections, after Total Joint Arthroplasty (TJA). 5 HbA1c is a crucial marker for long-term blood glucose control, reflecting the average blood sugar level over the past 3 months. Elevated HbA1c levels indicate poor blood sugar control that can impair wound healing. High blood glucose levels can lead to decreased tissue perfusion, impaired immune function, and delayed wound closure, all of which increase the risk for PJI. 6 There is ongoing research to determine the optimal HbA1c threshold for safe elective surgery. Many experts suggest aiming for an HbA1c level below 7% to minimize the risk of postoperative complications, including PJI. 7
Rakutt et al, 7 concluded that despite multiple recommendations, nutritional laboratory studies are infrequently ordered before arthroplasty. Rao et al, 8 surveyed 819 patients in the USA to determine the role of routine preoperative nutritional screening in all primary Total Joint Arthroplasty (TJA) cases. Abnormal preoperative nutritional values were albumin <3.5 g/dL, transferrin <200 mg/dL, and TLC <1500 cells/mm3. Their study suggested that routine testing of healthy patients is not warranted before TJA. Alfargieny et al, 9 examined nutritional status as a predictive marker for surgical site infection (SSI) in TJA in 135 Libyan patients. They concluded that serum albumin level was the only significant predictor of SSI and should be used as a screening tool to avoid SSI. Eu et al, 10 conducted a study on 85 Malaysian patients with soft tissue and bone sarcomas of the upper and lower limbs and concluded that malnutrition is a significant independent factor related to infectious and non-infectious complications, leading to unplanned readmission and prolonged stay.
However, to date, no specific studies have been conducted on nutrition in geriatric patients with NOF fractures undergoing arthroplasty in Malaysia. Therefore, generalizing the findings of international studies in the local context may be inaccurate because of variations in sociodemographic, economic, and healthcare characteristics. Hence, this study aims to determine the effects of preoperative nutritional levels on the outcomes of arthroplasty surgery among geriatric patients with NOF fractures.
Materials and Methods
A retrospective study of geriatric patients who sustained NOF fractures admitted to Kuala Lumpur General Hospital between 2022-2023 was included in this study. Inclusion criteria were patients aged 60 years and above with NOF fractures that were treated with arthroplasty. Patients with underlying renal and liver impairment were included in this study. The World Health Organization (WHO) often uses 60 years as the threshold for older populations, as significant health decline and increased healthcare needs typically begin at this age. Furthermore, in Malaysia, where this study was conducted, retirement and senior benefits also started at age 60, making it a practical and culturally relevant choice. The surgeries performed in this study included Bipolar Hemiarthroplasty and Total Hip Replacement (THR) procedures. The implants used in this study were the Exeter V40 System, Trident Acetabular System, and Rimfit System (Stryker, Mahwah, New Jersey, USA). All femoral stems were cemented. Acetabular cup fixation was performed using cement in patients with osteopenic bone, whereas those with better bone density received a cementless acetabular cup. The exclusion criteria were patients who underwent revision arthroplasty surgeries for periprosthetic joint infections, aseptic loosening, and periprosthetic fractures or patients with intertrochanteric femur fractures (Figure 1).The independent variables were age, gender, ethnicity, BMI, education level, smoking status, comorbidity, pre-fracture mobility, American Society of Anesthesiologists (ASA) level, surgical timing and several perioperative nutritional parameters. Study flow.
The preoperative parameter results were obtained on the first day of admission, which included ALB, HB, urea, CRET, CRP, and HbA1c. Serum ALB readings <35 g/L were considered clinical indicators of protein-energy malnutrition. 8 Anemia was defined as an HB reading below 10 g/dL. 2 The normal range for urea was 3.2-7.4 mmol/L and for creatinine was 64-111 μmol/L. A moderate elevation of CRP was defined as more than 10 mg/L. 4 A normal HbA1c level was defined as below 7% and an elevated HbA1c level was above 8%. 6 Surgical timing were also included and was categorized as less or more than 48 hours post fracture.
Surgical outcomes included the presence of complications (i.e Hypotension, cardiac arrhythmia, acute coronary syndrome, delirium, acute kidney injury, constipation, vascular thromboembolism, pressure ulcer, prosthetic joint infection, dislocation and neurovascular injury), mobility, and Western Ontario and McMaster Universities Osteoarthritis Index Questionnaire (WOMAC) scores 1-year post-surgery, which were collected from the patient’s medical records and were treated as binary categorical variables. The overall WOMAC score was categorized into no or mild symptoms (0-39) and moderate to severe symptoms (40-96). 11
The sample size for this study was calculated to meet the study objectives, with the largest estimated sample used as the final study sample. The estimation was conducted using Open Epi software version 3.01 for a cohort study design (available at https://www.openepi.com/Menu/OE_Menu.htm). The parameters were defined as follows: α = 0.05, power = 80%, a 1:1 ratio of unexposed (normal nutritional status) to exposed (malnutrition) individuals, 2% incidence of infections post-arthroplasty surgery in patients with normal nutritional status (unexposed), and an Odds Ratio (OR) of 13 based on a study by Eu et al
10
The total estimated sample size was 108 as depicted in Figure 2, which was inflated by 30% to reach a final sample size of 140, which is compatible with similar previous studies.
10
Sample size calculation.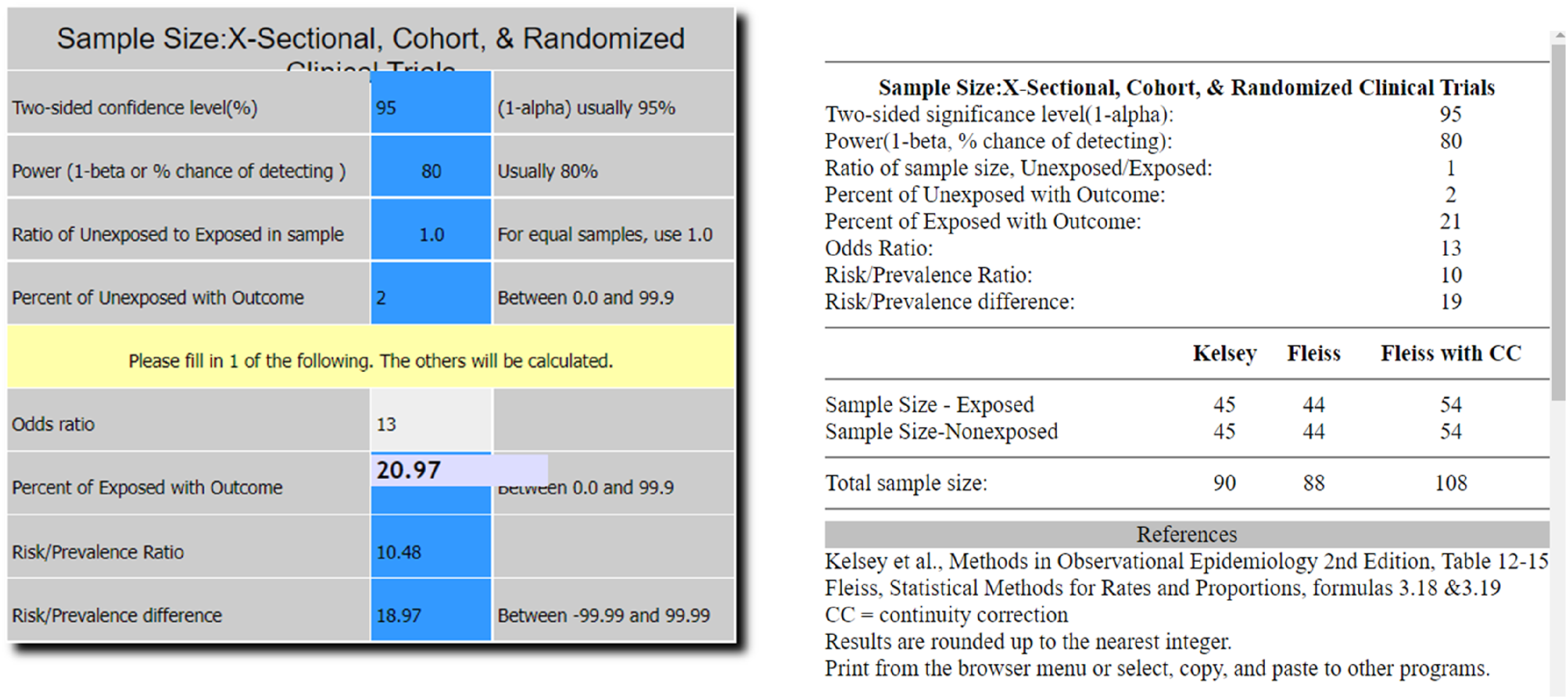
Data were analyzed using the Statistical Package for the Social Sciences (SPSS) version 26.0 by International Business Machines, IBM Corp., released in 2019 from Armonk, NY, United States of America. Data were analyzed descriptively using percentages and frequencies for categorical variables and mean, and standard deviation (SD) for continuous variables. To examine the association of nutritional factors and post-surgical outcomes, univariate and multivariate binary logistic regression analysis were performed for each surgical outcome, namely post-operative complication, mobility, and WOMAC score. Odds ratio (OR), Adjusted odds ratio (AOR), 95% confidence intervals, and P-values were reported. Variables significant at 0.25 were entered into the multivariate model to determine the adjusted OR
Results
Characteristics of Study Population (N = 141).

BMI: Body mass index. ASA: American Society of Anesthesiologists. ALB: Albumin. HB: Hemoglobin. CRET: Creatine. CRP: C reactive protein. HbA1c: Glycosylated hemoglobin. WOMAC: Western Ontario and McMaster Universities Osteoarthritis Index Questionnaire.
aHypotension, cardiac arrhythmia, acute coronary syndrome, delirium, acute kidney injury, constipation, pressure ulcer, prosthetic joint infection, dislocation and neurovascular injury.
Factors Associated With Post-surgical Complication.
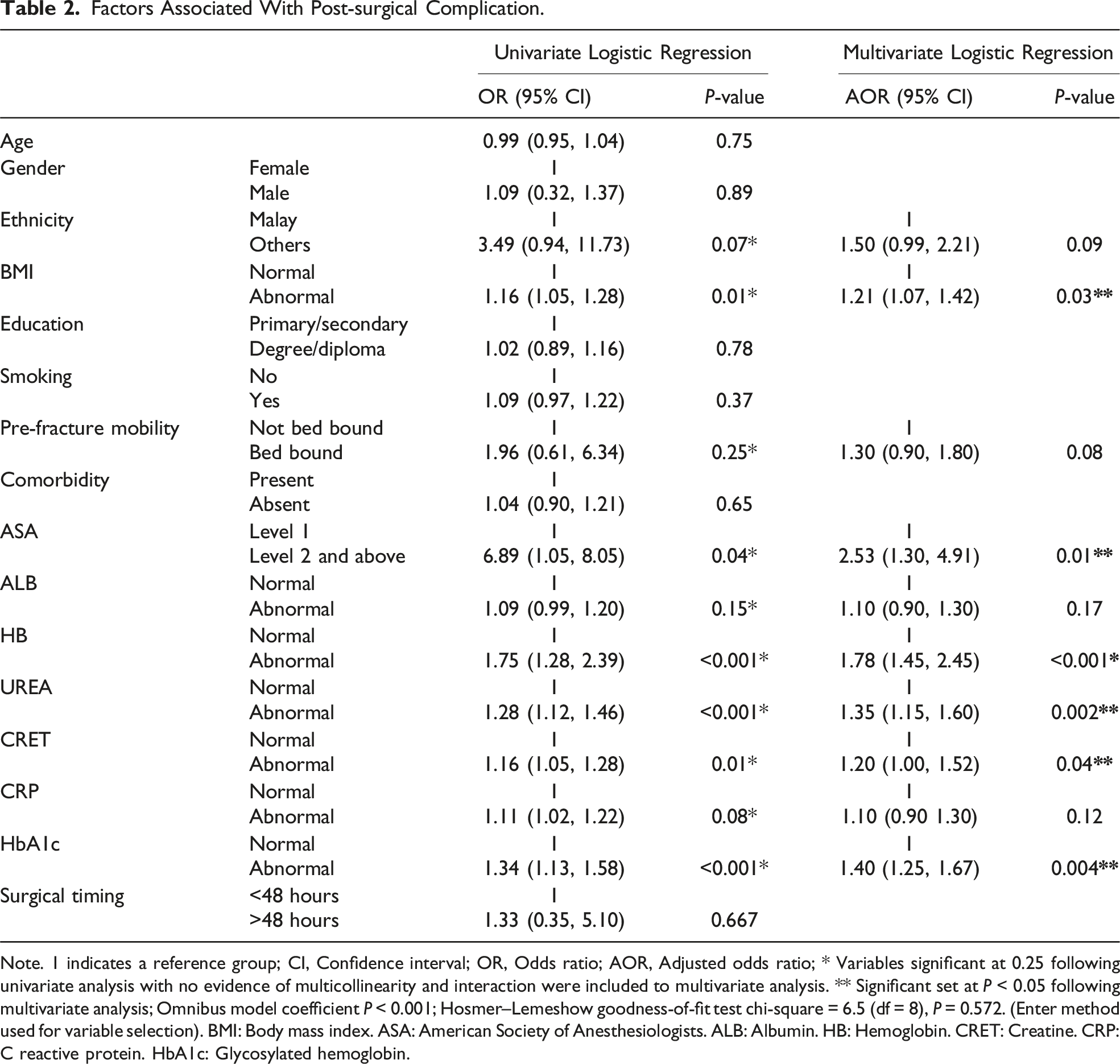
Note. 1 indicates a reference group; CI, Confidence interval; OR, Odds ratio; AOR, Adjusted odds ratio; * Variables significant at 0.25 following univariate analysis with no evidence of multicollinearity and interaction were included to multivariate analysis. ** Significant set at P < 0.05 following multivariate analysis; Omnibus model coefficient P < 0.001; Hosmer–Lemeshow goodness-of-fit test chi-square = 6.5 (df = 8), P = 0.572. (Enter method used for variable selection). BMI: Body mass index. ASA: American Society of Anesthesiologists. ALB: Albumin. HB: Hemoglobin. CRET: Creatine. CRP: C reactive protein. HbA1c: Glycosylated hemoglobin.
Factors Associated With Post-surgical Mobility.

Note. 1 indicates a reference group; CI, Confidence interval; OR, Odds ratio; AOR, Adjusted odds ratio; * Variables significant at 0.25 following univariate analysis with no evidence of multicollinearity and interaction were included to multivariate analysis. ** Significant set at P < 0.05 following multivariate analysis; Omnibus model coefficient P < 0.001; Hosmer–Lemeshow goodness-of-fit test chi-square = 5.2 (df = 8), P = 0.772. (Enter method used for variable selection). BMI: Body mass index. ASA: American Society of Anesthesiologists. ALB: Albumin. HB: Hemoglobin. CRET: Creatine. CRP: C reactive protein. HbA1c: Glycosylated hemoglobin.
Factors Associated With Post-surgical WOMAC Pain Score.

Note. 1 indicates a reference group; CI, Confidence interval; OR, Odds ratio; AOR, Adjusted odds ratio; Analysis performed Univariate Logistic Regression with significance set at P < 0.05; * indicates variables significant at P < 0.05; since only one variable were significant at 0.25 following univariate analysis, hence multivariate analysis was not performed. BMI: Body mass index. ASA: American Society of Anesthesiologists. ALB: Albumin. HB: Hemoglobin. CRET: Creatine. CRP: C reactive protein. HbA1c: Glycosylated hemoglobin. WOMAC: Western Ontario and McMaster Universities Osteoarthritis Index Questionnaire.
Discussion
This study aimed to elucidate the influence of preoperative nutritional status on surgical outcomes of arthroplasty in geriatric patients with NOF. The results highlight the significant impact of nutritional parameters on post-surgical complications, mobility, and WOMAC pain scores, emphasizing the critical need for thorough preoperative nutritional assessments in this elderly population.
Our findings revealed that higher BMI was significantly associated with both increased post-surgical complications and decreased post-surgical mobility. This underscores the multifaceted role of obesity in surgical outcomes, where excessive adiposity not only complicates the surgical procedure but also contributes to a pro-inflammatory state that hinders recovery. This is consistent with previous literature, which has established the adverse effects of obesity on surgical morbidity and recovery.12,13 Interestingly, the significance of BMI in our study suggests that even moderate deviations in BMI can have profound effects on the elderly, highlighting the need for weight management strategies pre-surgery.
Abnormal HB levels emerged as a robust predictor for both increased complications and reduced mobility post-surgery. This finding aligns with Musallam et al, 14 who demonstrated that preoperative anemia substantially increases postoperative morbidity. Anemia compromises tissue oxygenation and immune function, leading to poorer wound healing and higher infection rates. 15 This reinforces the importance of managing anemia preoperatively to improve surgical outcomes, a recommendation that should be integrated into preoperative protocols.
The impact of renal function on surgical outcomes was also evident in our study, with abnormal urea and creatinine levels significantly predicting adverse outcomes. Renal impairment exacerbates fluid and electrolyte imbalances, increasing the risk of perioperative complications. 1 The significant association between renal biomarkers and surgical outcomes in our study underscores the need for meticulous renal function monitoring and optimization before surgery. This finding is particularly pertinent in the geriatric population, where renal impairment is more prevalent and can have more severe consequences.
Moreover, our study found that poor glycemic control, as indicated by abnormal HbA1c levels, was significantly associated with both increased complications and reduced mobility. This finding is consistent with Dronge et al, 16 and Marchant et al, 17 who reported that uncontrolled diabetes increases the risk of postoperative infections and impairs wound healing. These results suggest that stringent glycemic control should be a priority in the preoperative management of diabetic patients undergoing arthroplasty.
The ASA classification, which considers overall physical status and comorbidities, was another significant predictor of post-surgical complications. The high OR for ASA level 2 and above indicates that a comprehensive evaluation of comorbid conditions is crucial in predicting surgical risks and planning perioperative care. 18
Our study revealed a significant relationship between advancing age and increasing WOMAC scores post-surgery, indicating that older patients tend to experience more pain, stiffness, and functional limitations following arthroplasty. This finding aligns with existing literature, which consistently reports that age influences recovery outcomes in geriatric populations undergoing orthopedic surgeries.19,20 The increase in WOMAC scores with age can be attributed to several factors, including a higher burden of comorbidities, such as cardiovascular diseases and diabetes, which complicate postoperative recovery and prolonged rehabilitation. 21 Additionally, physiological declines associated with aging, such as decreased muscle mass and strength (sarcopenia), reduced bone density, and impaired proprioception, adversely affect outcomes.22,23 Older patients’ lower baseline physical activity and fitness levels, coupled with potential cognitive decline, can impede effective engagement in and benefit from postoperative rehabilitation programs.22,23 These factors highlight the need for tailored perioperative and postoperative care strategies for older patients undergoing arthroplasty.
The limitations of this study were that it was a retrospective study, meaning it could not establish cause-and-effect relationships. The small sample size and short duration of follow-up (1 year) might be limited to definitive conclusions on some comparisons. Future prospective research should explore the impact of preoperative nutritional interventions on postoperative outcomes and the mechanisms behind the observed associations between preoperative factors and nutritional markers. Despite implementing strict inclusion and exclusion criteria, some variability remained within the study population. To address this, a multivariate analysis was conducted to adjust for potential confounders.
Conclusion
This study underscores the critical influence of preoperative nutritional status on surgical outcomes in geriatric patients who underwent arthroplasty for femoral neck fractures. Key markers, including albumin, hemoglobin, urea, creatinine, and HbA1c levels, were significantly correlated with postoperative complications, mobility, and pain outcomes. These findings emphasize the importance of incorporating comprehensive nutritional assessments and tailored interventions into preoperative protocols to optimize surgical success and recovery. Moreover, this study highlights the multifaceted role of BMI and systemic health factors in shaping surgical risks and outcomes in an aging population. Future research should explore the longitudinal effects of targeted nutritional optimization and other modifiable risk factors to enhance surgical care for this vulnerable population.
Footnotes
Acknowledgments
We thank the Director General of Health Malaysia for his permission to publish this article.
Author Contributions
The authors contributed to the manuscript as follows: Conceptualization: S.S.L.S., J.P.Y.H., K.G., K.D.T.; Methodology: J.P.Y.H., K.D.T., S.P.P., S.R.S.; Software: J.P.Y.H., K.D.T., S.S.L.S.; Validation and Formal Analysis: S.P.P., J.P.Y.H., K.G.; Investigation: K.D.T., S.P.P., S.R.S.; Resources: S.S.L.S., S.P.P., S.R.S., S.S.L.S., K.D.T.; Data Curation: S.S.L.S., K.D.T., S.R.S.; Writing - Original Draft Preparation: S.S.L.S., K.D.T., S.R.S.; Writing - Review & Editing: S.S.L.S., J.P.Y.H., K.G.; Visualization: J.P.Y.H., K.G., S.P.P.; Supervision: S.S.L.S., J.P.Y.H., S.S.L.S., K.G.; Project Administration: S.S.L.S., J.P.Y.H., S.S.L.S, K.G. All authors have read and agreed to the published version of the manuscript. All authors contributed to the study conception and design, material preparation, data collection, and analysis. The first draft of the manuscript was written by Sarbhjit Singh, and all authors commented on previous versions. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. The final version of the manuscript has been read and approved by all authors.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Statement
Data Availability Statement
The data for this study is available upon request from the authors.
