Abstract
Introduction
In surgeries for unstable AO/OTA 31A3.3 fractures, surgeons use various lengths of intramedullary nails (IMNs). However, there is insufficient evidence regarding the appropriate nail length for these fractures. This study compared the biomechanical properties of IMNs of different lengths for AO/OTA 31A3.3 fractures.
Methods
30 synthetic femora of AO/OTA 31A3.3 fracture model were randomly assigned to the following three groups: short- (170 mm), mid- (235 mm), and long-length (300 mm) nail groups, and were performed fixation surgery. The translation patterns of the constructs were examined by cyclic testing and compared among three groups. Additionally, changes in the neck–shaft and shaft–nail angles after cyclic testing were evaluated using radiological images.
Results
The translation patterns during cyclic loading did not differ among the groups. Conversely, one-way analysis of variance (ANOVA) revealed a significant difference in the neck–shaft angle change (5.8° ± 1.8°, 2.8° ± 1.3°, and 1.9° ± .9° in the short-, mid-, and long-length groups, respectively; P < .001), and post-hoc analysis revealed that the change was greater in the short-length group than in the mid- and long-length groups (P < .001 and P < .001, respectively). Furthermore, one-way ANOVA revealed a significant difference in the shaft–nail angle change (3.1° ± 2.1°, 1.4° ± 1.4°, and .1° ± .6° in the short-, mid-, and long-length groups, respectively; P < .001), and post-hoc analysis revealed that the change was greater in the short-length group than in the mid- and long-length groups (P = .044 and P < .001, respectively).
Conclusions
Short-length nails were associated with relevant changes in the neck–shaft and shaft–nail angles in our AO/OTA 31A3.3 fracture model. Thus, the selection of mid- or long-length nails instead of short-length nails might be better in IMN surgery for these fractures to prevent postoperative varus deformity.
Introduction
Femoral intertrochanteric fractures of class 31A3.3 according to the Arbeitsgemeinschaft fur Osteosynthesefragen Foundation/Orthopaedic Trauma Association (AO/OTA) classification are unstable proximal femoral fractures and are some of the challenging fractures to treat.1-5 In surgery for these unstable fractures, surgeons use intramedullary nails (IMNs) of various lengths.5-7 Several studies have reported on which IMN length provides better clinical outcomes for intertrochanteric fractures6,7; however, there is insufficient evidence regarding the appropriate IMN length for unstable fractures, such as AO/OTA 31A3.3 fractures.
There have been several biomechanical studies on the proper nail length for IMN surgery in stable trochanteric fracture models (AO/OTA 31A1 or A2).8,9 A previous study performed a biomechanical comparison among the short-length (170 mm), mid-length (235 mm), and long-length (300 mm) TFN-ADVANCED Proximal Femoral Nailing System (TFNA) (DePuySynthes, Zuchwil, Switzerland) for fixation in a stable trochanteric fracture model (AO/OTA 31A1.2) involving synthetic femora and demonstrated the biomechanical inferiority of short-length nails compared with mid- and long-length nails. 8 To the best of our knowledge, no biomechanical studies have investigated the proper length of IMNs for unstable intertrochanteric fractures (AO/OTA 31A3.3).
We hypothesized that even in unstable AO/OTA 31A3.3 fractures, short-length IMN fixation will have greater reduction loss after cyclic loading tests than mid- and long-length IMN fixations, and short-length IMN fixation will be biomechanically inferior to mid- and long-length IMN fixations. To clarify these hypotheses, we compared the biomechanical properties of short-, mid-, and long-length IMN fixations for AO/OTA 31A3.3 fractures.
Material and Methods
Nail Implantation and Fracture Simulation
The Clinical Research Ethics Committee of our institution waived the requirement for ethical approval because this biomechanical study used synthetic bone and IMNs. Thirty synthetic femora (Sawbones Worldwide, Vashon, WA) were used to biomechanically evaluate the construct lateral angular movements of three different lengths of IMN (TFNA 170, 235, and 300 mm) constructs for the fixation of intertrochanteric fractures.8,9 The study procedures were based on those reported in previous studies.8,9 We could not obtain a synthetic femur model similar to that in the study by Marmor et al (polyurethane made) 9 owing to non-availability in our country. The inner cancellous material of the femora from Sawbones Worldwide was reamed using a 15-mm-diameter drill. The procedure was performed as a surrogate preparation for a stovepipe femur. The femora were randomly assigned to the following three groups (10 per group) according to the length of the IMN implanted: short-length nail group (TFNA 170 mm), mid-length nail group (TFNA 235 mm), and long-length nail group (TFNA 300 mm). All implants were inserted into the femora by one trauma surgeon based on official surgical instructions. All constructs consisted of a 9-mm-distal-diameter nail with a 125° neck angle and a 90-mm-length lag screw. As the distal interlocking screw, one 36-mm screw was inserted in the static hole.
An unstable intertrochanteric fracture model (AO/OTA 31A3.3) was created for each of the implanted femora using a surgical oscillating saw and a bone rongeur (Figure 1). This model is an intertrochanteric fracture with lateral wall fracture, which is the most frequent fracture type in AO31A3 fractures.
10
The fracture model was produced based on the method in previous reports.9,11 The first osteotomy line was created from the central lateral aspect of the greater trochanter to the pinnacle of the lesser trochanter.
9
The second osteotomy line was set perpendicular to the intertrochanteric line between the distal one-third of the femur and the lateral cortex.
11
The lesser trochanter was removed via a cut through its base using a bone rongeur.
11
Unstable intertrochanteric fracture model (AO/OTA 31A3.3) was fixed using the TFN-ADVANCED Proximal Femoral Nailing System.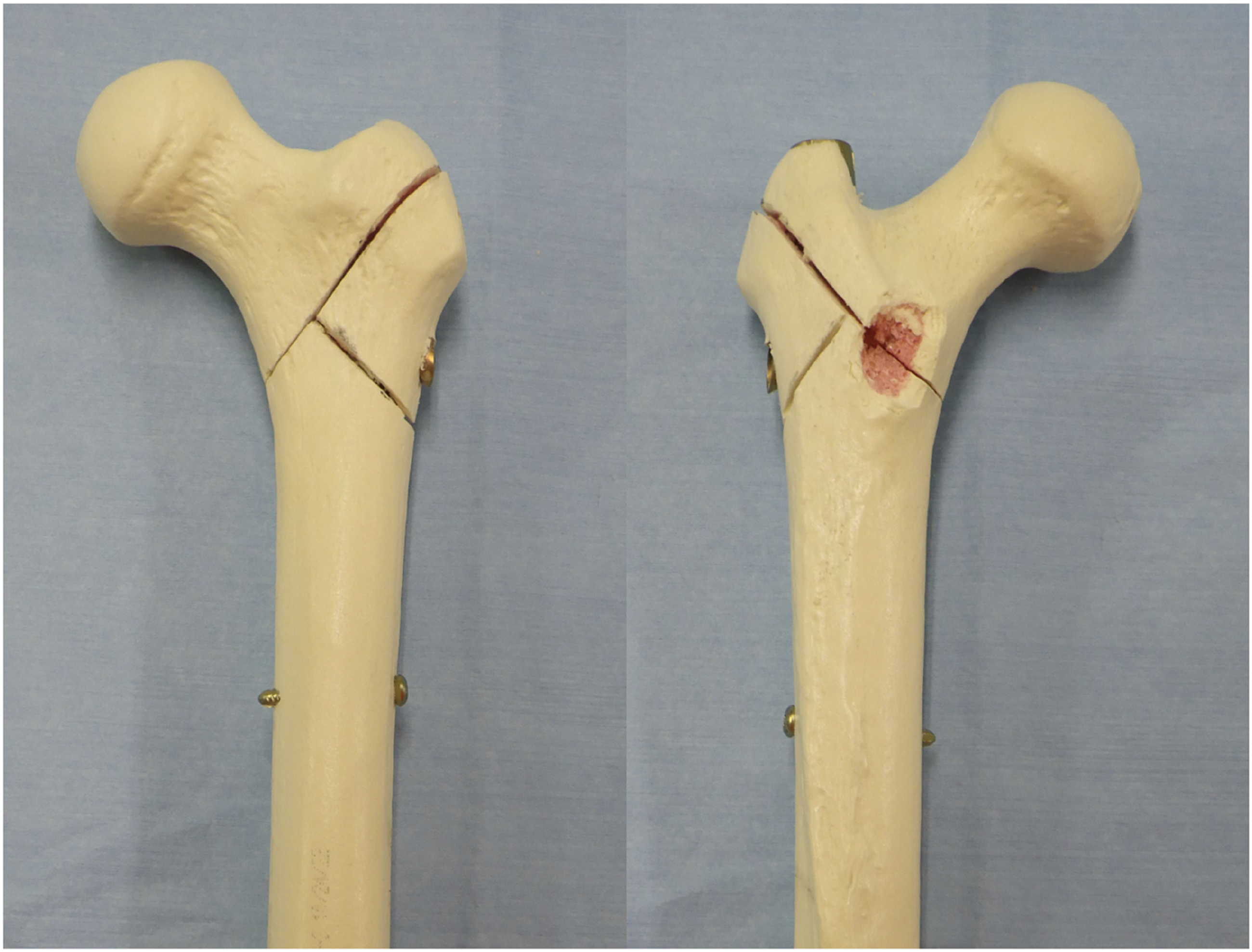
Biomechanical Evaluation
Cyclic testing was performed to investigate the translation patterns of the three types of fixation constructs. The prepared constructs were mounted on a tensile tester (Tensilon RTG 1310, Orientec Co., Ltd., Tokyo, Japan) with a set of specially designed grips (Figure 2A). As each femur was oriented, cyclic loading was applied along the mechanical axis of the femur. After cutting off 10 cm of the distal femur, the distal 4 cm of each femur was clamped using a custom-made jig. A load-displacement curve was created using specific software (Tensilon Advanced Controller for Testing, Orientec Co., Ltd., Tokyo, Japan) (Figure 2B). Then, the femora were cyclically loaded up to 750 N (2000 cycles) with reference to the pressure settings of past cyclic tests on synthetic femur models.12,13 The displacements in the machine axial direction at cycles 10-100, 100-500, 500-1000, 1000-1500, and 1500-2000 were determined through software calculations of actuator displacements during cycling. The translations of the actuator at cycles 100, 500, 1000, 1500, and 2000 were calculated and determined using software.
8
In addition, the number of test abandonments due to material failures (femoral head fragment fracture, diaphyseal fracture, and implant breakage), number of proximal femoral fractures other than at the osteotomy site after cyclic testing, and number of distal locking screw breakage and backout events were counted. Photograph of a specimen in the tensile testing machine (A) and schematic image of the load-displacement curve generated during cyclic testing with software (B). The specimens are set into the special testing machine. Axial load is applied to the femoral head. The axial load is 750 N, and 2000 cycles are applied.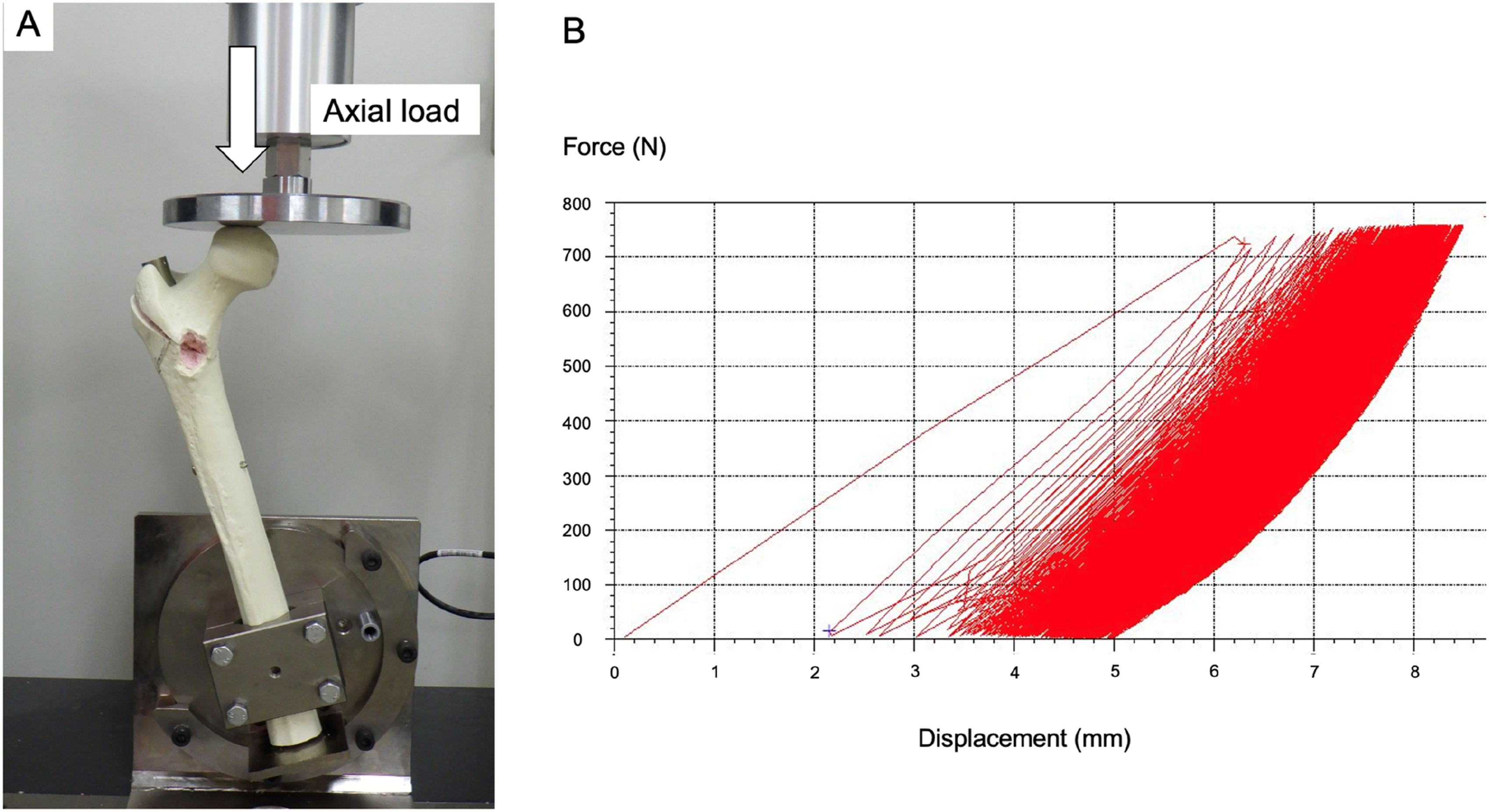
Radiological Evaluation
Anteroposterior and lateral radiography images of all femora were obtained before and after cyclic testing, and the tip–apex distance (TAD) before cyclic testing,
14
change in the neck–shaft angle after cyclic testing,15,16 and change in the angle between the femoral shaft axis and distal nail axis (shaft–nail angle) after cyclic testing
8
were evaluated using the Picture Archiving and Communicating System monitor (GE Healthcare, Barrington, IL, USA) (Figure 3). Angle change before and after cyclic testing was defined as a positive value in the varus direction. Anteroposterior radiography of the specimen before and after the cyclic test. (a) Tip–apex distance; (b) Neck–shaft angle; and (c) Shaft–nail angle.
Statistical Analysis
A one-way analysis of variance (ANOVA) with Tukey post-hoc analysis was used to evaluate between-group differences in displacement and translation during the cyclic tests and evaluate the radiological findings among the three study groups. The numbers of material failures and proximal femur fractures other than at the osteotomy site among the three groups were compared using the Fisher exact test. All data are presented as mean ± standard deviation. A priori power analysis was performed using G* Power 3.1 (Franz Paul, Kiel, Germany). 17 There were 30 total specimens, 10 in each group. A power analysis calculated α error of .05, and β error of .20 (i.e., the power was .80), with effect size of .60. All statistical analyses were performed using EZR software. 18 A P-value of <.05 was considered statistically significant.
Results
Displacement and Translation During Cyclic Loading
Mean Displacement During Cyclic Loading in Each Group.

Note: Data are expressed as mean (standard deviation).
Mean Translation During Cyclic Loading in Each Group.

Note: Data are expressed as mean (standard deviation).
Complications After Cyclic Loading
There were no specimens that needed abandonment of the test due to material failure. Two short-length specimens experienced fracture of the femoral head (Fisher exact test, P = .31) and one short-length specimen showed distal locking screw backout (Fisher exact test, P = 1) (Figure 4 Radiography of a specimen with a short-length intramedullary nail showing distal screw backout after cyclic testing. Radiography after cyclic testing of a specimen in the short-length nail group. Varus changes in the neck–shaft angle and shaft–nail angle. Additionally, there is distal interlocking screw backout (white arrow). We speculate that repeated nail movement inside the femoral shaft canal caused the screw to back out.
Radiological Evaluation
Radiological Evaluation Among the Three Groups.

Note: Data are expressed as mean (standard deviation).

Changes in the neck–shaft angle and shaft–nail angle before and after cyclic testing among short-, mid-, and long-length nails (A) Neck–shaft angle change and (B) Shaft–nail angle change.
Discussion
This study evaluated the biomechanical properties of short-, mid-, and long-length IMNs for AO/OTA 31A3.3 fractures. The study found that changes in the neck–shaft angle and shaft–nail angle between before and after cyclic testing were significantly greater in the short-length nail group than in the mid- and long-length nail groups.
In this study, the change in the neck–shaft angle was greater in the short-length nail group than in the mid- and long-length nail groups, and the femora in the short-length nail group showed more varus angular deformity at the fracture site. Additionally, the change in the shaft–nail angle was greater in the short-length nail group than in the mid- and long-length nail groups, and the medial angular deviation of the IMN from the femoral shaft axis inside the femoral canal was greater in the short-length nail group than in the other groups. From these results, we speculate that the coverage of a longer area in the canal by the mid- and long-length nails would restrain the movement of the nails and reduce the medial angular deformation of the nails from the femoral shaft axis, resulting in less varus deformity at the fracture site. Previous studies have reported that IMN surgery for femoral intertrochanteric fractures with varus reduction increases the risk of fixation failure and implant failure, such as cut-outs, and that varus reduction should be avoided.19-22 To reduce postoperative varus deformity and postoperative complications for AO/OTA 31A3.3 fractures, it may be useful to choose mid- or long-length IMNs instead of short-length IMNs in clinical practice. Additionally, in this study, complications, such as femoral head fracture and distal screw backout, occurred only in the short-length nail group. These complications may be caused by varus deformity,19-22 and short-length nails may not be an appropriate choice for AO/OTA 31A3.3 fractures.
This study also compared each parameter between the mid-length and long-length nail groups, but there were no significant differences, and the superiority of these implants could not be determined. The mid-length nail, in contrast to the long-length nail, could be inserted by using conventional surgical instruments without any need to insert distal screws by using a radiolucent drill, and this surgical simplification might help prevent prolonged operative time and achieve less blood loss. 23 Although further biomechanical validation and clinical studies are needed, if there is no significant difference in the biomechanical stability between the mid- and long-length nails, this convenience might be a reason for nail length selection in IMN surgery.
In the past, studies have compared nail lengths, especially short-length vs long-length nails, in clinical practice for femoral intertrochanteric fractures and have reported increased blood loss and prolonged operative time with long-length nail fixation, arguing for the superiority or non-inferiority of short-length nails.5-7,24,25 However, many of these studies did not adequately adjust for fracture type or were not limited to AO/OTA 31A3.3 fractures and may have selected longer IMNs owing to unstable and difficult fractures, which may have resulted in modified outcomes and complications.5-7,24,25 To determine the appropriate nail length for unstable intertrochanteric fractures like AO/OTA 31A3.3 fractures, more strictly designed clinical studies are required.
This study provides biomechanical evidence to help surgeons determine the nail length in IMN surgery for AO/OTA 31A3.3 fractures. In clinical practice, among nails with different lengths and the same diameter, mid- and long-length nails may be better for AO/OTA 31A3.3 fractures to prevent postoperative varus deformity. If surgeons choose to use short-length nails, additional adjustments may be needed to increase the stability between the shaft, such as enlarging the nail diameter or using two distal interlocking screws; however, a further study is needed to investigate the implications of these adjustments.
Limitations
Our study has several limitations. First, we did not use human cadaveric femora, and instead, we used synthetic femora in this study. Thus, the results may vary owing to material effects. Second, we set the cyclic testing at a load of 750 N for 2000 cycles. In our pilot study, we tried cyclic loading tests between 1000 and 2000 N, but the synthetic femur model broke, and we were unable to complete the testing. Therefore, we chose a cyclic load of 750 N with reference to the pressure settings of past cyclic tests on synthetic femur models,12,13 and chose 2000 cycles according to the setting in a previous report that assumed the value in a sedentary patient with proximal femoral fracture. 8
Conclusion
This study compared the biomechanical properties of short-, mid-, and long-length IMNs for AO/OTA 31A3.3 fractures. Mid- and long-length nails showed limited changes in neck–shaft and shaft–nail angles, while short-length nails showed relevant changes in these angles in our AO/OTA 31A3.3 fracture model. Thus, the selection of mid- or long-length nails instead of short-length nails might be better in IMN surgery for AO/OTA 31A3.3 fractures to prevent postoperative varus deformity in clinical practice.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
